Objective: The primary objective of this systematic review and meta-analyses was to summarize the impact of all reported treatments on transition to psychosis in high-risk samples.
Data Sources: PsycINFO, Embase, CINAHL, EBM, and MEDLINE online databases were searched from inception to May 2017 using the keywords psychosis, risk, and treatment with no geographical, date, or language restrictions.
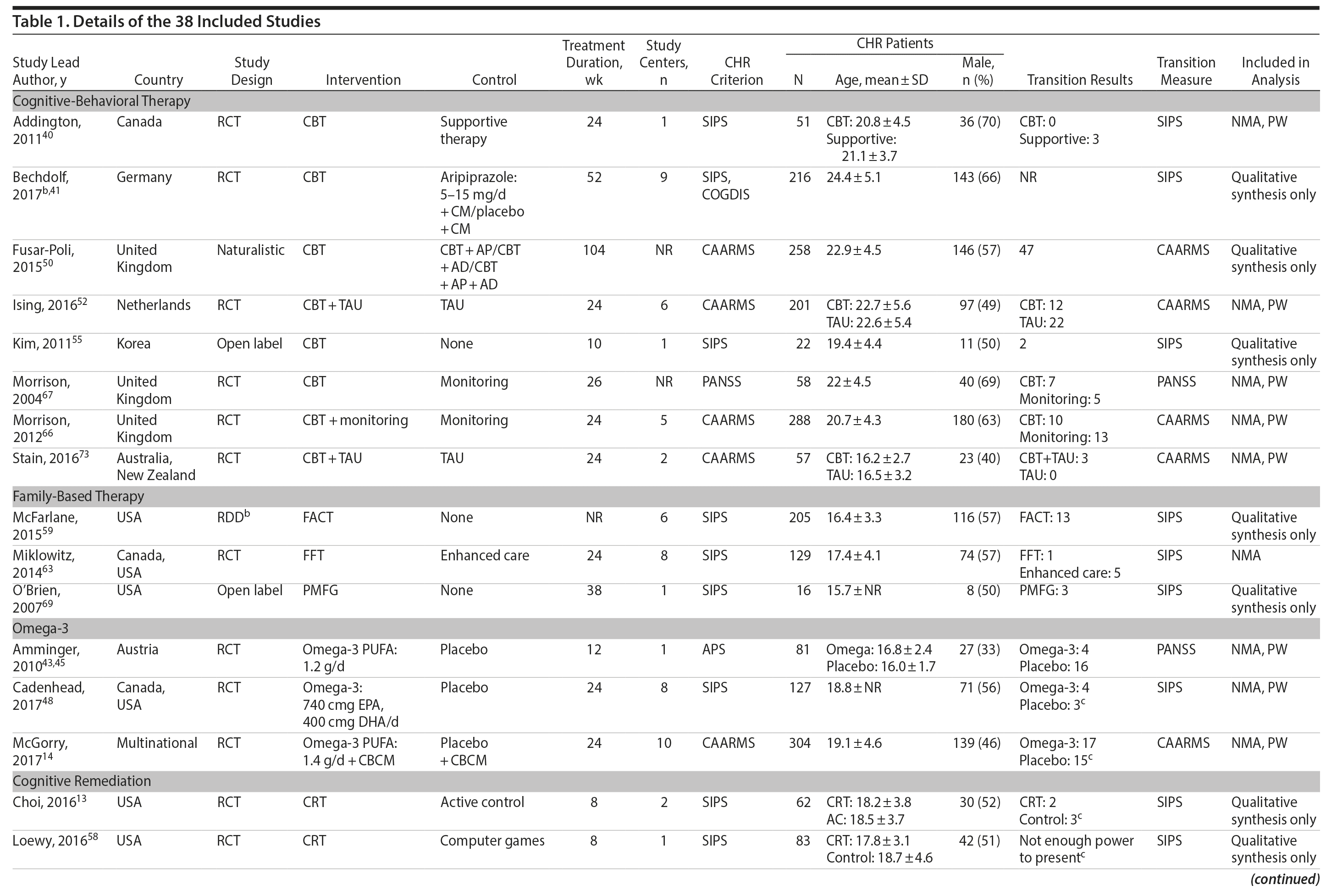
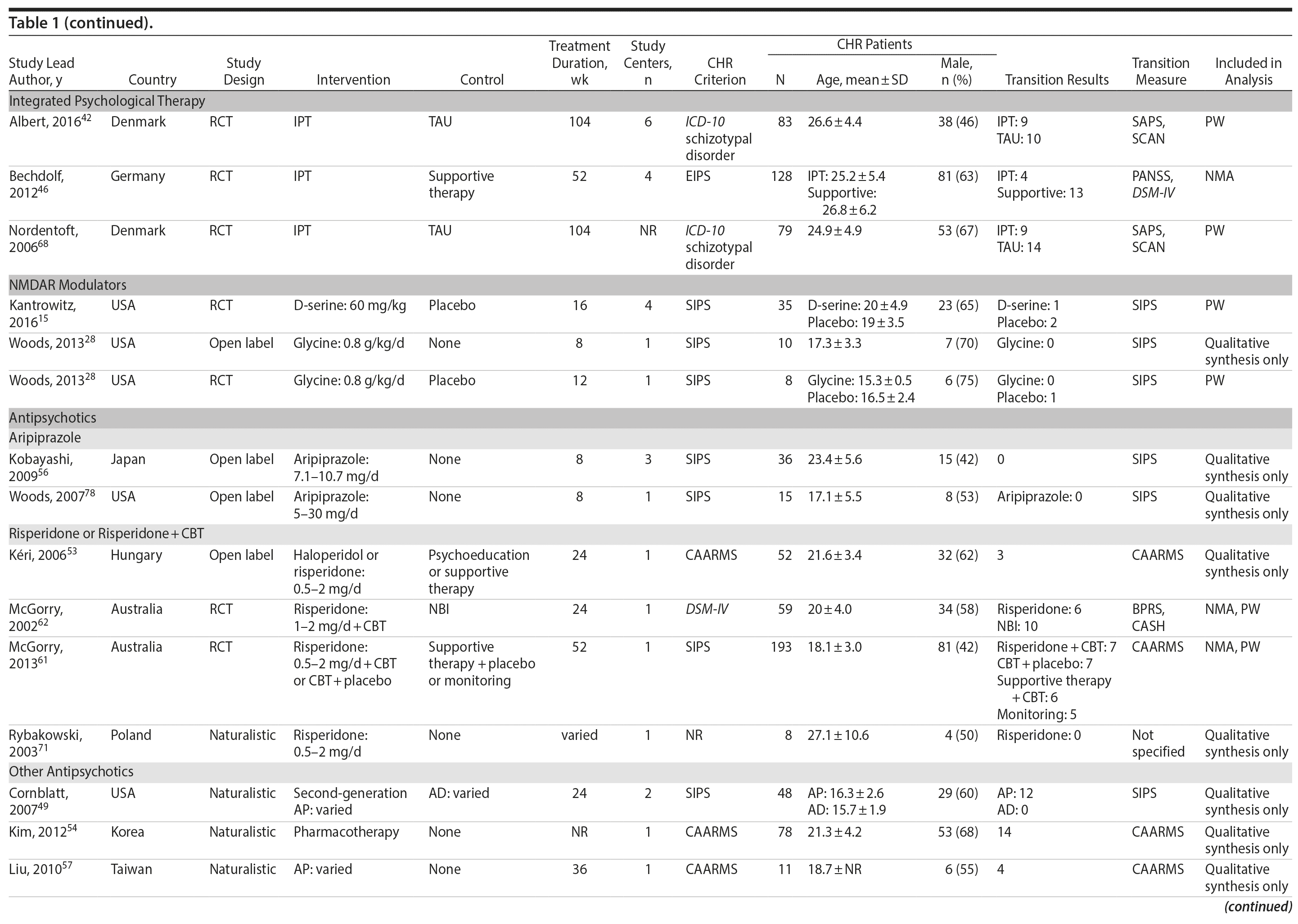
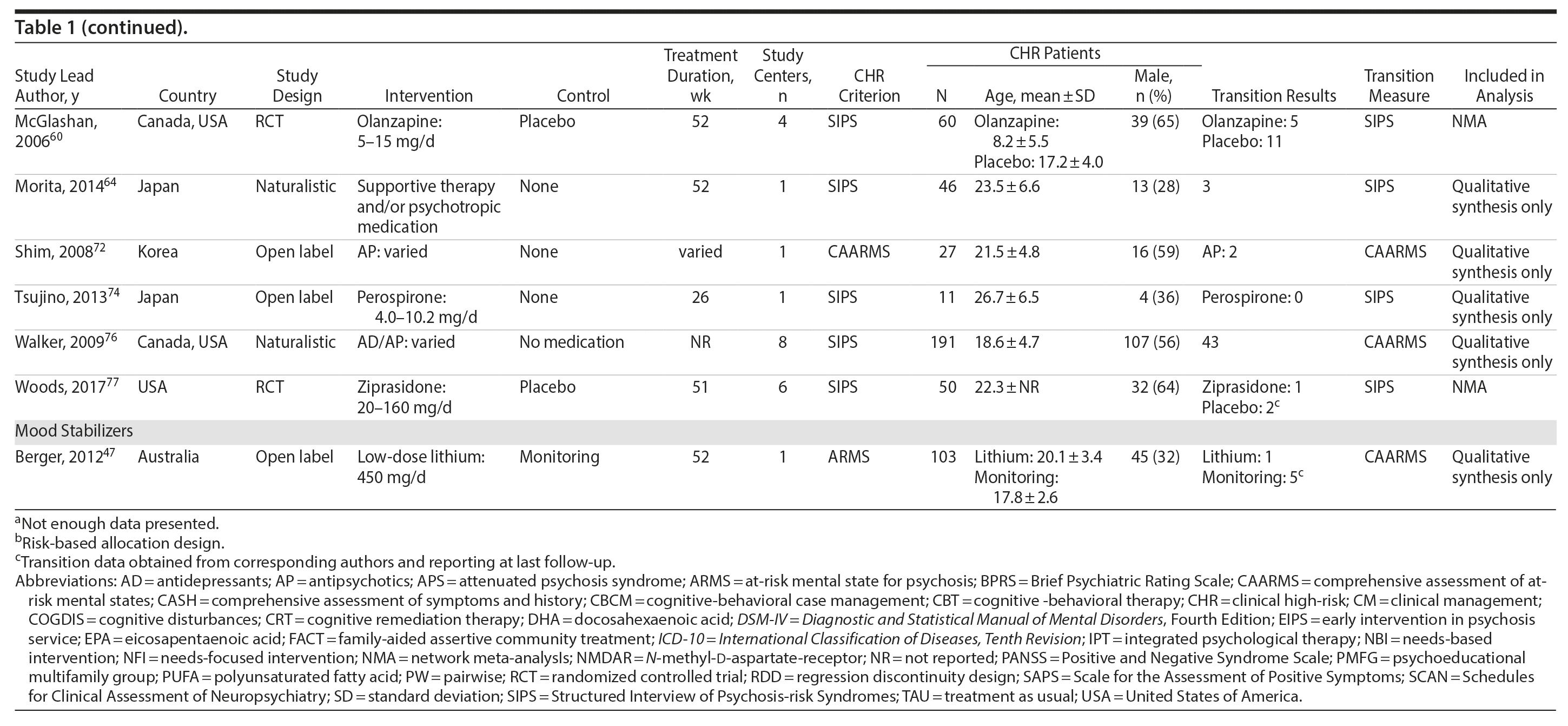
Study Selection: A total of 38 independent studies met the inclusion criteria: conducted a treatment study in a sample at high risk for psychosis and reported on transition to psychosis as an outcome.
Data Extraction: The following data were extracted: study characteristics (eg, sample size), participant characteristics (eg, mean age), and clinical outcome data (eg, number and percentage of patients transited for each intervention group at each time-point and transition assessment employed). Data were analyzed using random-effects pairwise meta-analysis (to explore differences between treatment and controls) and multivariate network meta-analyses (NMAs; to explore differences between treatment types on transition) and were reported as risk ratios (RR).
Results: In pairwise meta-analyses, cognitive-behavioral therapy (CBT) studies were associated with a significant reduction in transition compared with controls at 12-month and 18-month follow-up (RR = 0.57; 95% CI, 0.35-0.93; I2 = 7%; P = .02 vs RR = 0.54; 95% CI, 0.32-0.92; I2 = 0%; P = .02). In the NMAs, integrated psychological therapy, CBT, supportive therapy, family therapy, needs-based interventions, omega-3, risperidone plus CBT, ziprasidone, and olanzapine were not significantly more effective at reducing transition at 6 and 12 months relative to each other.
Conclusions: This systematic review and pairwise meta-analyses demonstrated a reduced risk for transition favoring CBT at 12 and 18 months. No interventions were significantly more effective at reducing transition compared with all other interventions in the NMAs. NMA results should be interpreted with caution due to the small sample size.

ABSTRACT
Objective: The primary objective of this systematic review and meta-analyses was to summarize the impact of all reported treatments on transition to psychosis in high-risk samples.
Data Sources: PsycINFO, Embase, CINAHL, EBM, and MEDLINE online databases were searched from inception to May 2017 using the keywords psychosis, risk, and treatment with no geographical, date, or language restrictions.
Study Selection: A total of 38 independent studies met the inclusion criteria: conducted a treatment study in a sample at high risk for psychosis and reported on transition to psychosis as an outcome.
Data Extraction: The following data were extracted: study characteristics (eg, sample size), participant characteristics (eg, mean age), and clinical outcome data (eg, number and percentage of patients transited for each intervention group at each time-point and transition assessment employed). Data were analyzed using random-effects pairwise meta-analysis (to explore differences between treatment and controls) and multivariate network meta-analyses (NMAs; to explore differences between treatment types on transition) and were reported as risk ratios (RR).
Results: In pairwise meta-analyses, cognitive-behavioral therapy (CBT) studies were associated with a significant reduction in transition compared with controls at 12-month and 18-month follow-up (RR = 0.57; 95% CI, 0.35-0.93; I2 = 7%; P = .02 vs RR = 0.54; 95% CI, 0.32-0.92; I2 = 0%; P = .02). In the NMAs, integrated psychological therapy, CBT, supportive therapy, family therapy, needs-based interventions, omega-3, risperidone plus CBT, ziprasidone, and olanzapine were not significantly more effective at reducing transition at 6 and 12 months relative to each other.
Conclusions: This systematic review and pairwise meta-analyses demonstrated a reduced risk for transition favoring CBT at 12 and 18 months. No interventions were significantly more effective at reducing transition compared with all other interventions in the NMAs. NMA results should be interpreted with caution due to the small sample size.
J Clin Psychiatry 2020;81(3):17r12053
To cite: Devoe DJ, Farris MS, Townes P, et al. Interventions and transition in youth at risk of psychosis: a systematic review and meta-analyses. J Clin Psychiatry. 2020;81(3):17r12053.
To share: https://doi.org/10.4088/JCP.17r12053
© Copyright 2020 Physicians Postgraduate Press, Inc.
aDepartment of Psychiatry, Hotchkiss Brain Institute, University of Calgary, Alberta, Canada
*Corresponding author: Jean Addington, PhD, Mathison Centre for Mental Health Research & Education, 3280 Hospital Drive NW, Calgary, Alberta T2N 4Z6 Canada ([email protected]).
Between 17% and 28% of those identified as being at clinical high risk (CHR) for psychosis will have a first psychotic episode within the first year.1 In a recent meta-analysis,2 attenuated psychotic symptoms and global functioning were 2 factors associated with transition to psychosis, followed by negative symptoms. Longer duration of untreated psychosis has also been reported to lead to poorer outcomes, including functional deficits3,4 and greater psychotic symptoms.5,6 The morbidity associated with frank psychotic illnesses is well recognized,7 with general consensus that effective interventions are necessary to prevent the onset of psychosis.8-10
Accordingly, transition to a psychotic disorder has been the primary outcome in the majority of randomized and observational intervention studies in those at CHR for psychosis. A variety of interventions (eg, antipsychotics, cognitive behavioral therapy [CBT], omega-3) have been tested, but most of these interventions have not been efficacious over control treatment or treatment as usual at reducing transition rates. There is a need for a more comprehensive search and assessment of the impact of interventions on transition to psychosis to inform both clinical practice and future trials.
Presently, to the best of our knowledge, only 2 aggregate pairwise meta-analyses have examined the impact of treatment interventions on transition to psychosis in those at CHR for psychosis. The first review11 found an effect for CBT on reducing transition at 12 months, and the latter12 found that “CBT-informed” treatment was associated with a reduced risk of transition to psychosis at 6 months, 12 months, and long-term follow-up. Both reviews focused mainly on the efficacy of CBT; however, interventional studies in CHR samples have increased considerably and encompass newer treatments such as N-methyl-d-aspartate receptor (NMDAR) modulator interventions (glycine and D-serine), cognitive remediation therapy (CRT), and omega-3.13-15 Our review expands on the previous reviews, first by systematically ascertaining more than 4 times the number of intervention studies and examining their impact on transition. Second, we performed the recommended two-step approach of first conducting a traditional pairwise meta-analysis followed by a network meta-analysis (NMA).16 The benefit of an NMA is that it allows for indirect comparisons between treatment arms that have not been compared before in a head-to-head fashion17 (eg, CBT to family therapy to antipsychotics) by using common comparators (eg, placebo, supportive therapy, needs-based interventions), and the results can offer a framework for clinical decision making.16 However, NMAs are often difficult to understand and subject to bias, which may lead to a misinterpretation of results,17 and some argue that it remains unclear whether or not NMAs improve patient care and outcomes.16 The benefit of using a traditional pairwise meta-analysis is that it allows you to compare treatments to controls and is easier to comprehend and decipher for clinicians.16
By including additional studies, new treatment interventions, a more comprehensive systematic search of the literature, and a novel analysis, the evidence base on treatment interventions and their impact on transition to psychosis in CHR youth will be enhanced.
METHODS
Protocol
A protocol was registered a priori for this systematic review and meta-analyses (PROSPERO [International Prospective Register of Systematic Reviews] number: CRD42017077963). All processes adhered to Preferred Reporting Item for Systematic Reviews and Meta-Analyses (PRISMA) guidelines and Meta-analysis of Observational Studies in Epidemiology (MOOSE) guidelines.18-21 A PRISMA checklist is available for both the pairwise meta-analyses and NMAs; see Supplementary Search 1 for details.22

- Treatments for those at clinical high risk for psychosis have been increasing, but the most effective treatment for reducing transition has not yet been established.
- In pairwise meta-analyses, cognitive-behavioral therapy (CBT) studies were associated with a significant reduction in transition compared to controls at 12-month and 18-month follow-up.
- If a patient presents with being at risk for psychosis, clinicians should consider offering CBT to help reduce the risk of a first episode.
Objective
The primary objective of this systematic review and meta-analyses was to summarize the impact of all reported interventions on transition to psychosis.
Data Sources and Search Strategy
MEDLINE, PsycINFO, Embase, CINAHL (Cumulative Index to Nursing and Allied Health Literature), and EBM (Evidence-based Medicine) online databases were systematically searched up to May 2017, using no geographical, date or language restrictions. The detailed search strategies are presented in Supplementary Search 1. Title and abstract screening were followed by a more comprehensive, full-text screening (based on inclusivity), which was performed independently and in duplication by 2 reviewers (M.S.F. and P.T.). All references lists of articles meeting the inclusion criteria were hand-searched for additional relevant articles. Further, to broaden the search, additional searches were performed as follows: (1) Scopus (http://www.scopus.com) using the keywords psychosis risk and treatment, (2) Clinicaltrials.gov registry using the keywords psychosis risk and treatment, and (3) The International Clinical Trials Registry Platform (http://apps.who.int/trialsearch/) using the keywords psychosis and risk.
Selection Criteria
Inclusion criteria for this systematic review were as follows: (1) studies including participants at risk of psychosis, including attenuated psychotic symptom syndrome (requires the presence of at least 1 attenuated psychotic symptom, which has begun or worsened in the past year), genetic risk and deterioration (combination of both functional decline and genetic risk), brief intermittent psychotic syndrome (requires the presence of any 1 or more psychotic symptoms that are too brief to meet diagnostic criteria for psychosis), early initial prodromal state (requires the presence of basic symptoms or a functional decline in combination with perinatal complications or genetic risk), or schizotypy; (2) studies including treatments in an observational or experimental setting; (3) studies reporting transition or conversion to psychosis; and (4) studies reporting a mean age of participants between 12 and 30 years. Studies were excluded if they employed an unsuitable study design (eg, case reports, review articles, editorials with insufficient study information) or did not involve an intervention (eg, treatment). Reconciliation of any discrepancies were resolved by a third reviewer (D.J.D. or J.A.).
Data Extraction
Data were extracted from all included studies, completed independently and in duplication by 2 reviewers (M.S.F. and P.T.), and verified by a third reviewer (D.J.D.). The following data were extracted: study characteristics (first author, publication year, country, study design, CHR sample size, number of study centers, CHR criterion used, rate of attrition for intervention and control groups, method of imputation used, severe adverse events reported), participant characteristics (mean ± SD age, number and percentage of male patients), treatment characteristics (number of participants allocated to each intervention and control group, type of intervention, type of control, duration, study endpoint), and clinical outcome data (number and percentage of patients transited for each intervention group at each time-point and transition assessment employed). Percentage transitioned was calculated and extracted accordingly if not present in the article. Crude risk ratios (RRs) and number-needed-to-treat were derived using the percent transitioned in each intervention/control group and used in the qualitative synthesis.
Risk-of-Bias Assessment
Cochrane’s tool for assessing risk-of-bias23 for randomized studies was used to evaluate study quality, using Review Manager24 (RevMan) version 5.1 (training.cochrane.org/). Further, for nonrandomized studies, the Risk-of-Bias In Nonrandomized Studies of Interventions (ROBINS-I)25 was used to evaluate quality of evidence. In the NMAs, to assess the quality of evidence associated with comparisons, the level of bias present in most trials was estimated using the blinding of outcome assessments and weighted according to the number of studies in each comparison using colored edges (green = low risk, yellow = unclear risk, red = high risk) and the Grading of Recommendations Assessment, Development and Evaluation (GRADE) approach26 was used to evaluate the quality of evidence associated with the results in the NMAs at each time point.
Data Synthesis and Analysis
The κ statistic was used in the title/abstract screening phase to assess agreement between reviewers. Treatments were combined in both the pairwise meta-analyses and NMAs to account for similarities in design. Specifically, D-serine and glycine were combined as N-methyl-d-aspartate-receptor (NMDAR) modulators, as they are both amino acids that serve as neuromodulators acting as coagonists on the NMDAR with glutamate.27,28 Further, enhanced care, treatment as usual, community care, monitoring, and needs-focused interventions were merged as needs-based interventions (NBI). Only randomized control trials were included in meta-analyses, while observational studies were included in the qualitative synthesis. Random-effects models in the pairwise meta-analyses and NMAs were used to account for differences between studies because of study design, dose, CHR criteria, and the idiosyncratic treatment strategies. Last, the principal summary measure utilized in all analyses were RRs.
For the primary analysis, a DerSimonian and Laird29 random-effects pairwise model was used to derive pooled transition RR estimates for individual treatments types with a minimum of 2 trials (eg, 3 omega-3 trials) compared with the controls (eg, placebo). In the pairwise analysis, transition was stratified by available time points (eg, 6-months, 12-months, 18-months). Pairwise comparisons were performed in RevMan 5.1.24 Statistical heterogeneity was evaluated using the I2 statistic, where I2 ≥ 50% indicated moderate heterogeneity and I2 ≥ 75% was deemed high heterogeneity.
For the secondary analysis, the White30 and Higgins31 random-effects multivariate NMA assuming consistency, common heterogeneity across all comparisons in the network, and inverse-variance probability weighting32,33 was used to examine and directly compare treatment intervention effects in RCTs. This method was chosen to account for studies with multiple treatment arms (> 2)34 as it appropriately accounts for correlations between RRs in multiarm RCTs. Exponential format was applied for display in the forest plots produced. Due to the heterogeneity of study endpoints, only studies with transition rates reported at either 6-month, 12-month, or long-term follow-ups were included. Observational study designs and studies with additional participants not classified as CHR (eg, schizotypy) were excluded from the NMA. Both a global test for inconsistency34 and inconsistency plots assuming loop-specific heterogeneity were produced to determine if inconsistency existed in the NMA.35-38 These effects were potentially mitigated a priori with the use of inclusion criteria employed at the screening phases (eg, age). Furthermore, to investigate the most effective interventions compared with a better hypothetical treatment, surface under the cumulative ranking curve (SUCRA) was plotted. The closer the curve arches to 1, the higher the probability of efficacy.35,39 Network comparison-adjusted funnel plots35 were used to assess publication bias by ordering the interventions as active treatment versus controls. Last, a sensitivity analysis was performed in both the 6- and 12-month NMAs by dropping studies that had a high risk-of-bias for blinding of outcomes based on Cochrane’s tool for assessing risk-of-bias.23 We analyzed NMA data using Stata version 13 (StataCorp LLC: College Station, Texas), and graphical illustrations of the network evidence utilized the graphical toolset called “networkplot.”35 All statistical analyses used an α < .05 for statistical significance.
RESULTS
Search Yield
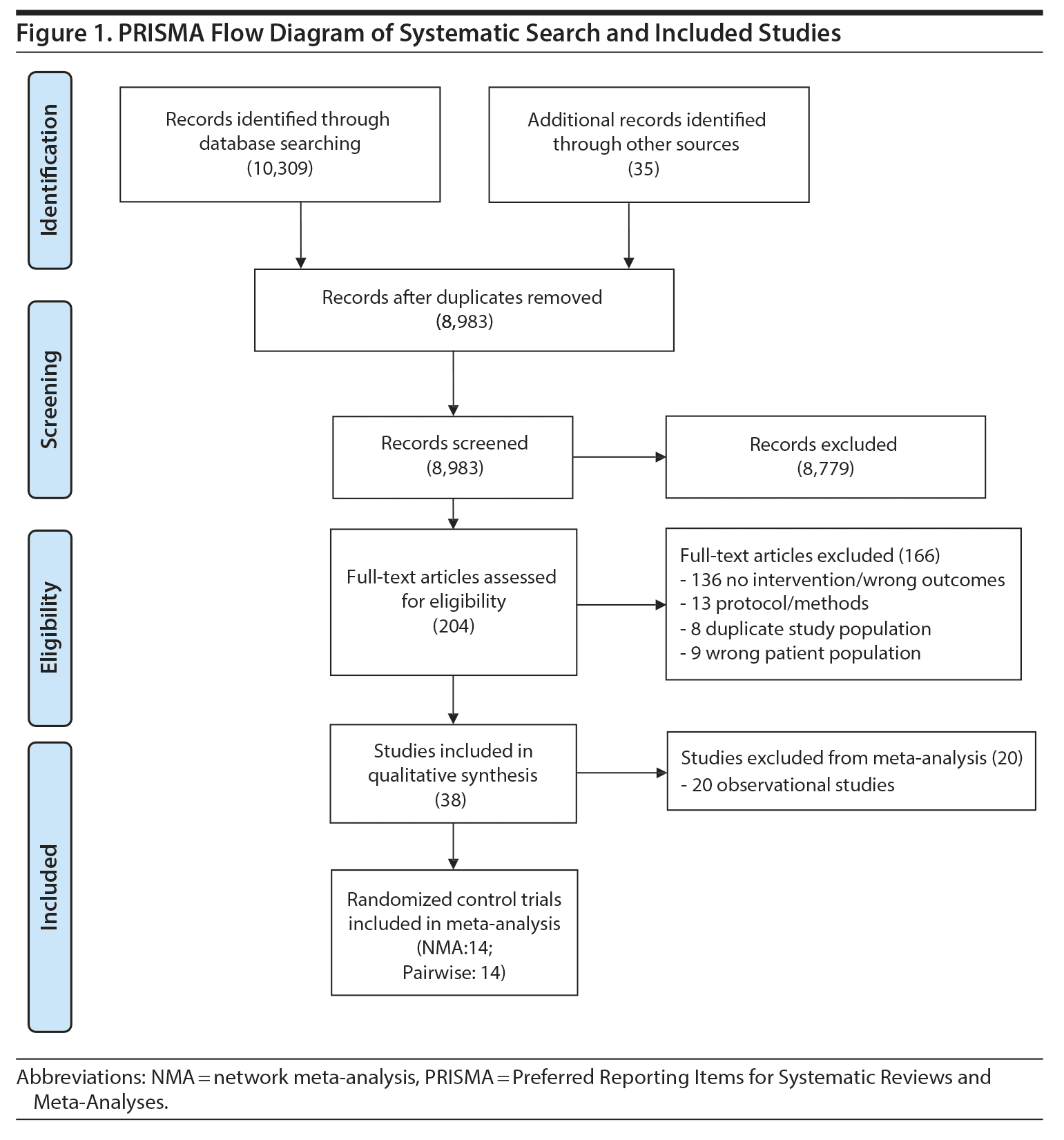
Our search strategy rendered 10,344 citations. Of those, 8,983 unique titles and abstracts were screened in duplication. Agreement between title and abstract reviewers was high for study inclusion (κ = 0.88). Overall, 204 full-text articles were screened and 45 articles13-15,28,40-80 fit our inclusion criteria for the systematic review. We identified 38 unique studies,13-15,40-43,46-50,52-64,66-69,71-74,76-78with 2 studies published in 1 article,28 and 8 articles44,45,51,65,70,75,79,80 with a duplicate study population (see Figure 1).
Study and Participant Characteristics
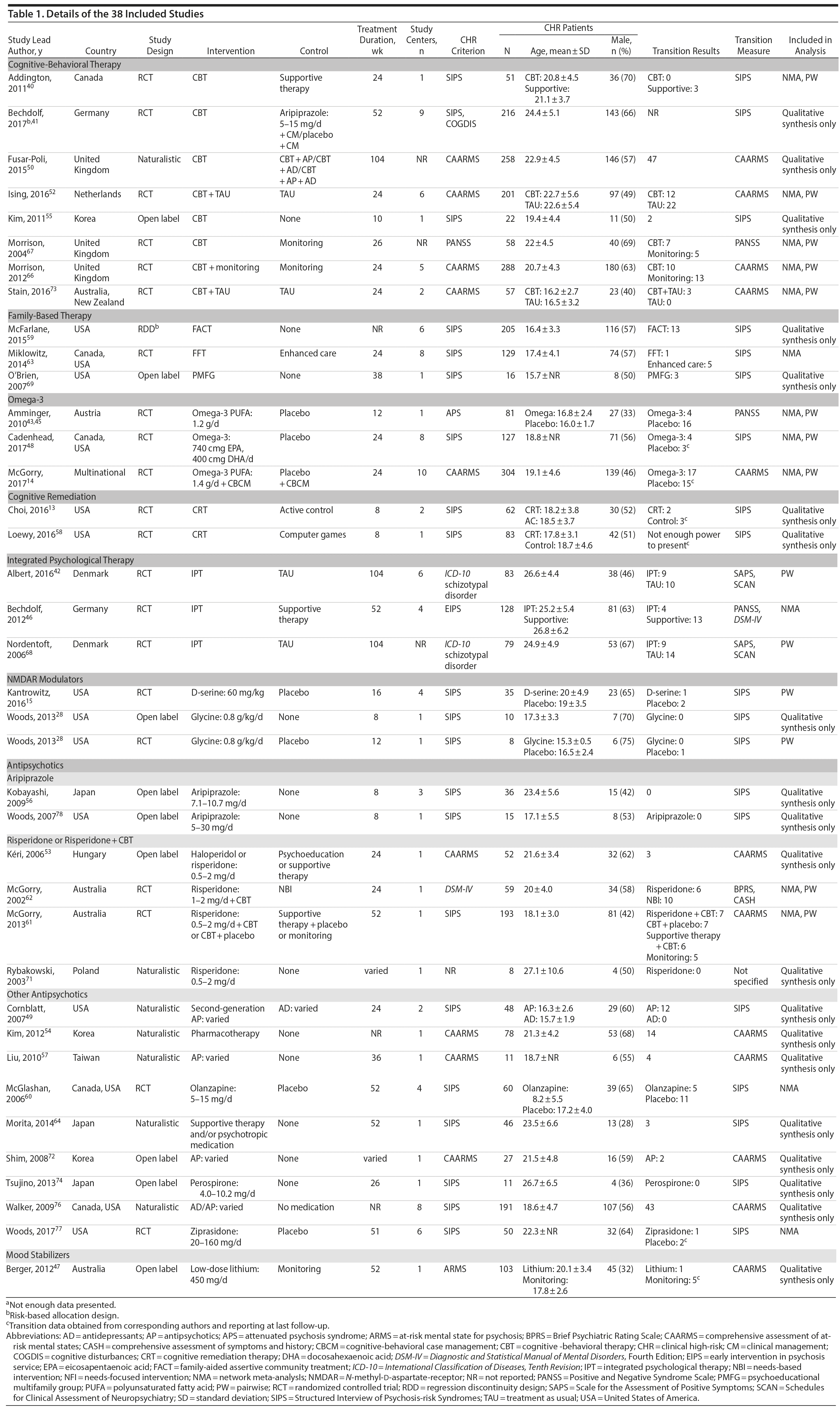
Study design varied and included 21 RCTs, 9 open-label designs, 7 naturalistic design, and 1 regression discontinuity design, all outlined in Table 1. The majority of the studies were performed in North America (15), followed by Europe (11), Asia (7), and Australia (4); one was a multinational study. This review included a total of 3,489 CHR participants with a mean age of 19.9 years, and 53.9% were male. Sample size and mean age ranged from 8 to 304 participants and 15.3 to 27.1 years, respectively. The most common measure used to identify transition to psychosis was the Structured Interview of Psychosis-risk Syndromes (SIPS) (19 studies), followed by the Comprehensive Assessment of At-risk Mental States (CAARMS) (12 studies).
Features of Treatment Interventions and Controls
Interventions were diverse: CBT,40,41,50,52,55,66,67,73 family therapy,59,63,69 omega-3,14,43,48 integrated psychological therapy (IPT),42,46,68 CRT,13,58 NMDAR modulators,15,28 mood stabilizers,47 and several types of antipsychotics such as risperidone or risperidone plus CBT,53,61,62,71 aripiprazole,56,78 olanzapine,60 perospirone,74 ziprasidone,77 and varied/unspecified.49,54,57,64,72,76
Risk-of-Bias Assessment
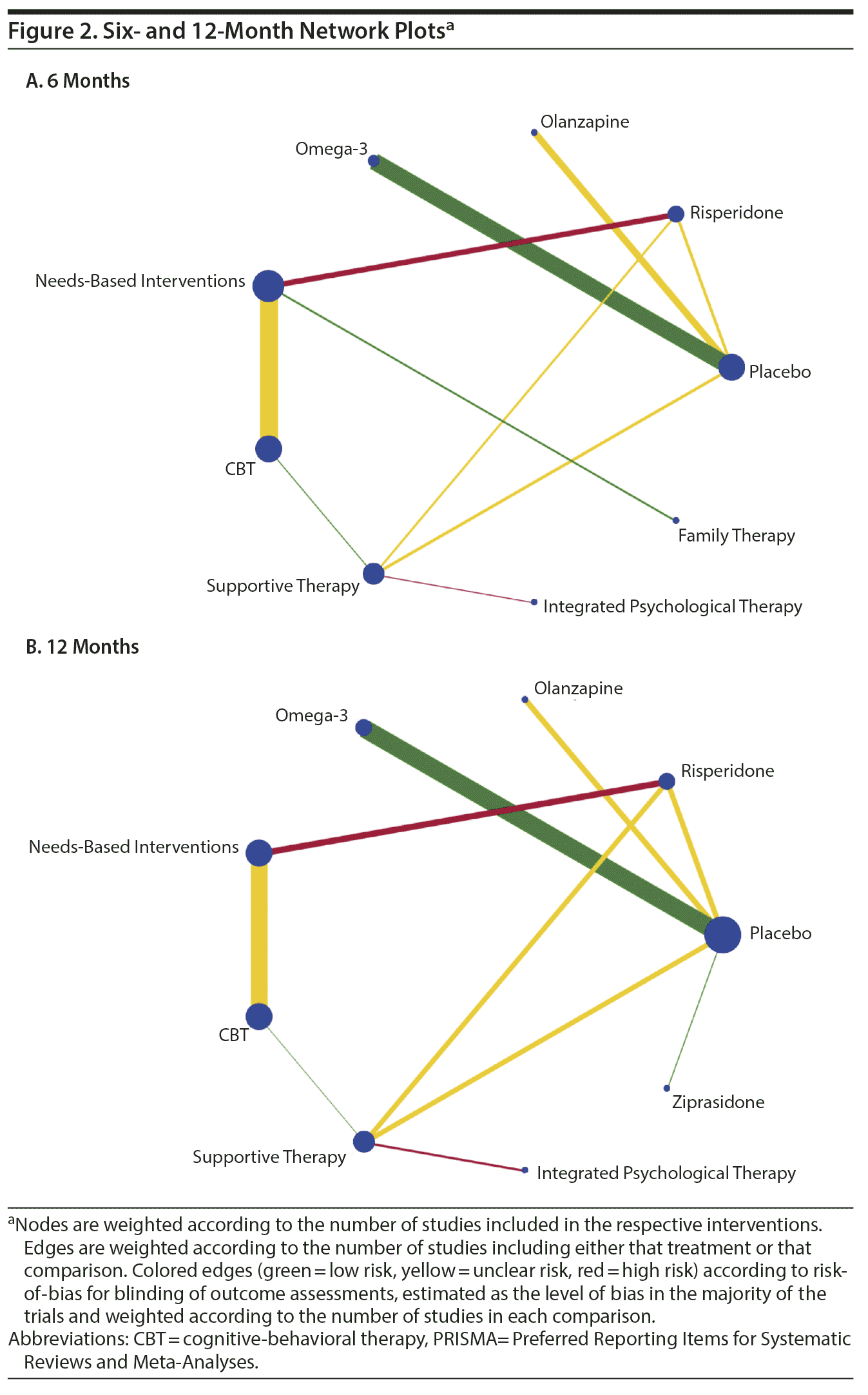
Quality assessments are reported in Supplementary Figure 1. The majority of RCTs had a low risk of bias for random sequence generation (20 studies). RCTs had a higher risk of bias for attrition bias (7 studies) and blinding of participants and personnel (8 studies). Weighted risk-of-bias assessment in the network meta-analysis plot (Figure 2) for blinding of outcome assessments revealed that 4 edges had an unclear risk-of-bias, 3 edges had a low risk-of-bias, and 2 edges had a high risk-of-bias. Quality assessment of observational studies using ROBINS-I varied from serious to low (Supplementary Table 2), and the overall quality of the NMAs using GRADE varied between very low quality to moderate quality (Supplementary Table 3); however, the majority of the evidence from the NMAs was rated as having very low quality of evidence.
Network Pattern and Network Plot
The network formed 2 complex network plots at 6 and 12 months due to having a variety of interventions (Figure 2). In addition, the network plot had some sparse connections (eg, family therapy) with NBI and placebo being the most common comparators. The long-term network plot formed a simple network between CBT, NBI, and risperidone plus CBT (Supplementary Figure 5B).
Consistency and Publication Bias
Visual inspection of the comparison-adjusted funnel plots at 6- and 12-month follow-up for symmetry demonstrated the absence of small study effects with most observations falling on the null line (Supplementary Figure 2). Global tests of inconsistency found no statistically significant evidence of inconsistency in the NMAs. In addition, inconsistency plots formed 2 quadratic loops, which found no statistically significant evidence of inconsistency in the NMAs (Supplementary Figure 3).
Psychosocial Interventions
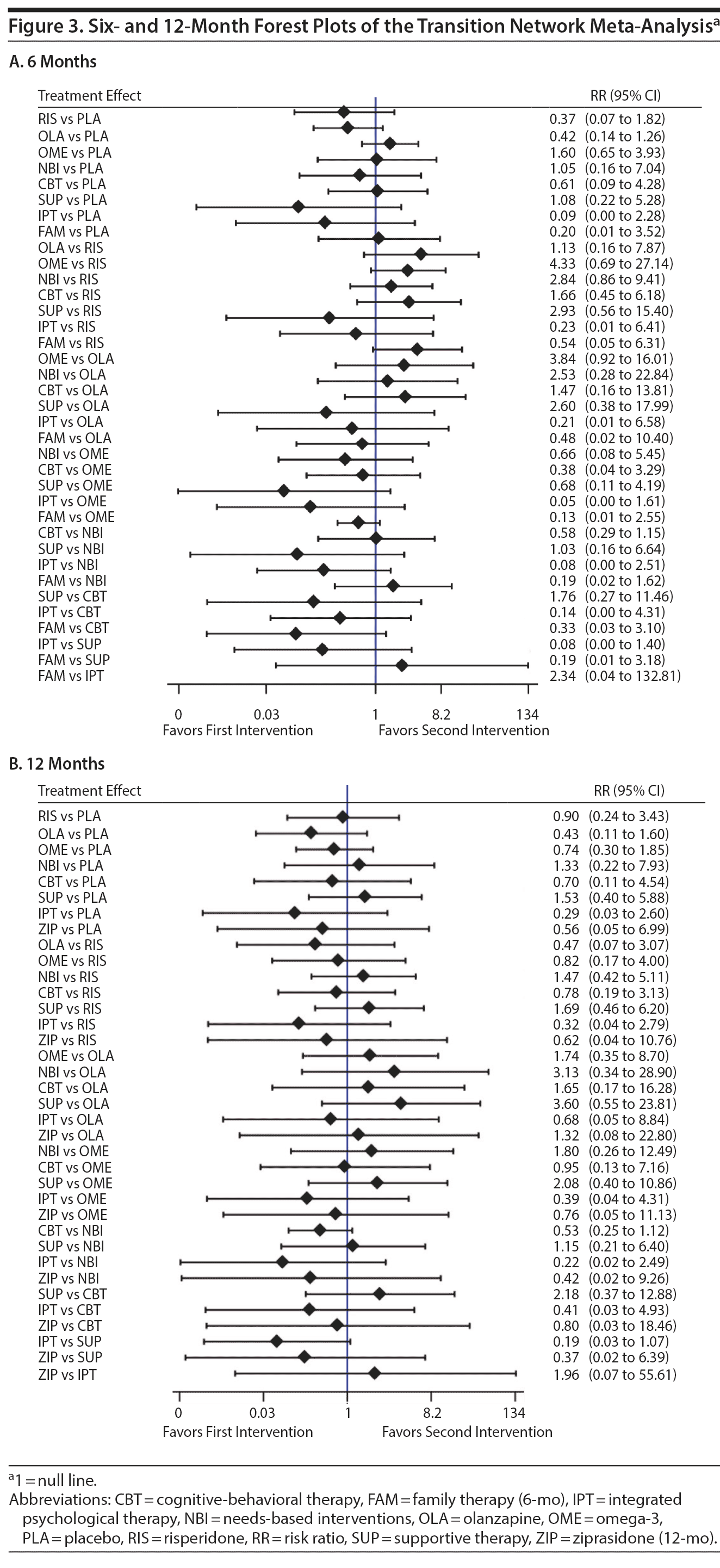
In the pairwise analyses, CBT interventions were not associated with a significant reduction in transition rates compared with controls at 6 months (RR = 0.66; 95% CI, 0.33-1.34; I2 = 19%; P = .25, 6 studies, N = 729; Supplementary Figure 7). However, CBT interventions were associated with a significant reduction in transition rates compared with controls at 12 and at 18 months (RR = 0.57; 95% CI, 0.35-0.93; I2 = 7%; P = .02, 6 studies, N = 729 vs RR = 0.54; 95% CI, 0.32-0.92; I2 = 0%; P = .02, 3 studies, N = 540). CBT trended toward statistical significance in reducing transition rates compared with controls at 24- to 48-month follow-up (RR = 0.69; 95% CI, 0.44-1.08; I2 = 0%; P = .11, 3 studies, N = 549). In the 6- and 12-month NMAs, CBT interventions were not significantly more effective at reducing transition compared with any other intervention (Figure 3).
Family therapy could be analyzed only in the 6-month NMA due to having only 1 available RCT reporting 1 time point. In the NMA, family therapy was not significantly more effective at reducing transition compared with all other interventions.
IPT could be analyzed only in the NMAs (6- and 12-month) due to having only 1 available RCT. In the NMAs, IPT was not significantly more effective at reducing transition compared with any other intervention at 6- and 12-month follow-up (Figure 3). However, in the NMAs (6- and 12-month), there was a trend favoring IPT over the majority of interventions at reducing transition, albeit not statistically significant with all CIs crossing the null line. SUCRA plots of the absolute effects and rank test among the 10 treatments indicated that IPT ranked higher than the other 10 treatments, but this is in the context of no statistically supported efficacy compared with other interventions at both 6 and 12 months (see Supplementary Figure 4).
Antipsychotics
In the pairwise analyses, risperidone plus CBT interventions were associated with a significant reduction in transition rates at 6-month follow-up (RR = 0.34; 95% CI, 0.13-0.88; I2 = 0%; P = .03, 2 studies, N = 146) but not at 12-month follow-up (RR = 0.72; 95% CI, 0.38-1.38; I2 = 0%; P = .32, 2 studies, N = 146; Supplementary Figure 8). In the 6-month and 12-month NMAs, risperidone plus CBT interventions were not significantly more effective at reducing transition compared with any other intervention. Olanzapine could be analyzed only in the 6- and 12-month NMAs due to its having only 1 available study and was not significantly more effective at reducing transition compared with any other intervention. Similarly, ziprasidone could be analyzed only in the 12-month NMA due to its having only 1 available study and was not significantly more effective at reducing transition compared with any other intervention.
Omega-3
In the pairwise analyses, omega-3 interventions were not associated with a significant reduction in transition at 6-month, 12-month, or long-term follow-up compared with placebo (6-month: RR = 1.59; 95% CI, 0.68-3.76; I2 = 0%; P = .29, 2 studies, N = 431 vs 12-month: RR = 0.69; 95% CI, 0.21-2.27; I2 = 64%; P = .54, 3 studies, N = 512 vs long-term follow-up: RR = 0.51; 95% CI, 0.10-2.55; I2 = 70%; P = .41, 2 studies, N = 208; Supplementary Figure 9). In the 6-month and 12-month NMAs, omega-3 was not significantly more effective at reducing transition compared with any other intervention.
NMDAR Modulators
In the pairwise analyses, NMDAR modulator interventions were not associated with a significant reduction in transition compared with placebo (RR = 0.48; 95% CI, 0.08-2.98; I2 = 0%; P = .43, 2 studies, N = 52; Supplementary Figure 10) at 12- to 16-week follow-up. No NMDAR modulator studies were evaluated in the NMAs due to no comparable time-point (eg, 6 or 12 months).
Cognitive Remediation Therapy
CRT was not evaluated in the pairwise meta-analyses due to having only 1 study. No CRT studies were evaluated in the NMA because it was not connected to any treatment in the network.
Integrated Treatment in Schizotypy
In the pairwise analyses, integrated treatments were not associated with a significant reduction in transition compared with standard care at long-term follow-up in studies that targeted schizotypal participants (RR = 0.74; 95% CI, 0.42-1.31; I2 = 14%; P = .30, 2 studies, N = 162; Supplementary Figure 11). Schizotypal studies were not assessed in the transition NMA because it would contravene the transitivity assumption.
Sensitivity Analyses
Sensitivity analyses were performed for both the 6- and 12-month NMAs by dropping studies that had a high risk of bias for blinding of assessments. The sensitively analyses confirmed that no interventions were significantly more effective at reducing transition compared with all other interventions in the network meta-analyses at any time point (Supplementary Figure 6).
DISCUSSION
In summary, this systematic review compared the effects of psychosocial interventions, antipsychotic medications, omega-3, and NMDAR modulators on transition to psychosis in CHR populations using both pairwise and network meta-analyses. First, pairwise meta-analyses revealed that CBT was associated with a significant reduction in transition compared with control treatments at 12- and 18-month follow-up, with a trend toward significance at long-term follow-up (24-48 months), whereas, risperidone plus CBT interventions were associated with a significant reduction in transition rates at 6-month follow-up. NMDAR modulators and omega-3 were not significantly better than placebo in pairwise analyses.
In the NMAs, there were no significant results with all CIs crossing the null line, meaning that no treatments significantly reduced transition relative to each other, although there were some trends that may be of interest. First, there was a trend favoring IPT over the majority of interventions at both 6- and 12-month follow-ups. After performing sensitivity analyses, we noted a trend emerged favoring family therapy over the majority of interventions at 6 months and favoring CBT at 12 months, compared with all other treatments.
CBT demonstrated a statistically significant benefit over control treatments at reducing transition at 12- and 18-month follow-up. This finding is somewhat contrary to a previous meta-analysis12 that reported that CBT reduced transition to psychosis at 6, 12, and 18-24 months. However, in the present review we did find a trend toward a significant reduction in transition at long-term follow-up. The discrepancy at 6 months in significance between reviews may be due to the presence of 2 additional CBT studies, both of which demonstrated no impact on transition compared with controls. In addition, the previous review included an IPT therapy at 6 months in its analysis, which may have biased results in favor of CBT.46 Nevertheless, both this current review and the previous reviews11,12 demonstrated a reduced risk for transition to psychosis for CHR participants that were randomized to CBT. Last, a trend emerged favoring CBT at reducing transition compared with all other therapies after removing studies that had a high risk of bias for blinding of outcomes at 12 months and at long-term follow-up. However, the results were not significant. CBT has the most available trials to date, and thus the results are more robust and generalizable compared with all other treatment strategies that have been tested in CHR samples.
In the NMAs, there was a trend favoring IPT over the majority of interventions at reducing transition compared with all other treatments before sensitivity analyses. Although this finding was not significant, it does merit some further discussion. As is the case with many treatment trials in CHR, there was only 1 RCT examining IPT. Consequently, the results of the NMAs should be interpreted with caution. This study was heavily weighted toward CBT (25 sessions) and included group skills training (15 sessions), cognitive remediation (12 sessions), and psychoeducational multifamily group (3 sessions). Unfortunately, due to study design, it was not possible to evaluate the different treatment strategies, making it difficult to ascertain which component(s) may have had an impact on transition. However, IPT interventions have been tested in patients with schizophrenia and have been shown to improve a variety of outcomes such as social cognition, neurocognition, psychosocial functioning, and negative symptoms compared with control treatments, as demonstrated in a recent meta-analysis.81
Finally, there was a trend favoring family therapy relative to other treatments at reducing transition in the NMA at 6 months after the sensitivity analysis was performed, albeit it was not significant. Unfortunately, there was only 1 RCT examining family therapy in CHR youth, and thus the results of the NMAs should be interpreted with caution until more RCTs investigating the impact of family therapy in CHR samples occur. However, 1 observational study59 in CHR samples has examined the impact of family therapy on transition in a CHR samples, and it reported favorable results for reducing transition compared with those at “clinically low risk.” In addition, family interventions in patients with schizophrenia are recommended by numerous international clinical guidelines and have a well-established influence at reducing psychotic symptoms.82 Finally, a recent meta-analysis83 established that family interventions decreased both relapse and readmission rates in early psychosis samples.
The strength of this review is that it included 38 unique studies examining 13 different treatment interventions with more than 3,400 CHR youth. We searched numerous databases, hand searched references to identify interventions, extracted data in duplicate, published our protocol a priori, and followed PRISMA and MOOSE guidelines, thus making this review the most comprehensive systematic review and largest meta-analysis of transition interventions in CHR to date.
However, there are important limitations to consider. First, the quality of evidence in this literature was deficient as conveyed by the high risk-of-bias for blinding of outcome assessments and may bias our findings. However, after performing sensitivity analyses by removing low-quality studies, results were minimally affected, with the exception of the removal of the 1 IPT study. Future studies should attempt to minimize risk-of-bias to strengthen the overall quality of the CHR treatment literature, which may aid future meta-analysis in the precision and quality of their conclusions. In addition, future studies may wish to undertake RCTs instead of observational studies as RCTs provide higher quality studies that can be incorporated into meta-analysis.
Second, we were unable to include all treatment strategies from the current systematic review in the NMAs, largely due to differences in when transition to psychosis rates were reported in individual treatments (eg, NMDAR modulators). Therefore, these analyses were restricted to treatments and studies reporting transition to psychosis at 6-month, 12-month, or long-term follow-up, which may have influenced our ability to detect a true difference between other treatment interventions. Moreover, the vast majority of evidence in the NMA was rated as having had a low quality as reported in GRADE, and thus the network results should be interpreted with caution. In addition, we were unable to include all treatment types in the traditional pairwise meta-analyses because some types of treatments had fewer than 2 RCTs (ie, family therapy, IPT, CRT). Due to the difference in studies included in both the pairwise meta-analyses and the NMAs, the results should be interpreted accordingly.
Third, we pooled a variety of treatments that used different criteria to define transition to a psychotic disorder, which may have important implications when interpreting the present results. The majority of studies utilized the SIPS scale for defining transition in CHR, which requires the occurrence of 1 fully psychotic symptom for at least an hour per day for an average of 4 days per week over the past month or 1 brief fully psychotic symptom that is dangerous or disorganizing. The second most common scale was the CAARMS,84 which differs in that the psychotic symptom has to have been present only for more than 1 week, and no criterion for dangerousness or disorganization is included. Interestingly, despite the differences in CHR scales utilized to determine transition, a meta-analysis85 demonstrated that transition risk remains relatively similar at multiple time-points regardless of what instrument is used. Furthermore, a recent study86 validated a conversion algorithm that demonstrated excellent diagnostic accuracy in determining conversion between the SIPS and the CAARMS.
Fourth, omega-3 pairwise meta-analyses at 12 months and long-term follow-up demonstrated significant amounts of heterogeneity, but in reviews comprising very few studies, such as in this review and meta-analyses, the I2 may not be accurate.87
Fifth, treatments included in this review had inconsistent follow-up periods, which presented a limitation when examining transition to psychosis. Due to the difference in follow-up times reported in different study types, not all studies could be included in each analysis. For example, CRT studies often reported a 3-month follow-up period whereas antipsychotics studies reported 6- and 12-month periods, thereby excluding CRT studies from the NMAs.
Another limitation in the current meta-analyses was that fidelity to treatment and comorbid diagnoses were not explored because the number of studies was too limited to perform a meta-regression. These potential mediators and moderators may impact the final outcome of interest, ie, transition rates, and may account for some of the discrepancies in transition rates in the various studies.
The findings of the current systematic review lead to a few potential areas for future research. First, IPT demonstrated a trend of reducing transition relative to other treatments, and although not significant, merits further investigation, as IPT offers a package of interventions such as family education, CBT, social skills training, and CRT, and may be an effective early intervention for other symptoms such as attenuated psychotic and negative symptoms, mood, and poor social and role functioning. Alternatively, a modular-based treatment program similar to that used in the Recovery After an Initial Schizophrenia Episode (RAISE) Early Treatment Program88,89 may be effective for those at CHR. In RAISE, through shared decision-making, participants were able to select from a range of programs that included medication management, family education, and individual resiliency training that included CBT and supported education and employment.
Next, more RCTs are needed with family therapy to support the results observed within this review. Such investigations may want to consider age of the young person, impact of expressed emotion90 and implementation.82 Moreover, family studies should investigate what specific components of the therapy are more effective at reducing transition, such as family involvement and communication training.
In conclusion, this systematic review and meta-analyses demonstrated a reduced risk for transition favoring CBT at 12 and 18 months. However, no interventions were significantly more effective at reducing transition compared with each other in the network meta-analysis. IPT and family therapy, although promising, require more clinical trials to determine a more precise and generalizable effect in CHR youth.
Submitted: December 1, 2017; accepted October 28, 2019.
Published online: May 19, 2020.
Potential conflicts of interest: The authors declare no financial or other conflicts of interest.
Funding/support: This work was supported in part by National Institutes of Health Grant RO1MH105178 awarded to Dr Addington. Mr Devoe is supported by the Alberta Innovates Graduate Studentship.
Role of the sponsor: The supporter had no role in the design, analysis, interpretation, or publication of this study.
Acknowledgments: The authors would like to thank librarian Helen Robertson, MLIS, for her assistance with running the literature search for the review; she reports no conflicts of interest.
REFERENCES
1. Fusar-Poli P, Borgwardt S, Bechdolf A, et al. The psychosis high-risk state: a comprehensive state-of-the-art review. JAMA Psychiatry. 2013;70(1):107-120. PubMed CrossRef
2. Oliver D, Reilly TJ, Baccaredda Boy O, et al. What causes the onset of psychosis in individuals at clinical high risk? a meta-analysis of risk and protective factors. Schizophr Bull. 2020;46(1):110-120. PubMed CrossRef
3. Schimmelmann BG, Huber CG, Lambert M, et al. Impact of duration of untreated psychosis on pre-treatment, baseline, and outcome characteristics in an epidemiological first-episode psychosis cohort. J Psychiatr Res. 2008;42(12):982-990. PubMed CrossRef
4. Cechnicki A, Cichocki Å, Kalisz A, et al. Duration of untreated psychosis (DUP) and the course of schizophrenia in a 20-year follow-up study. Psychiatry Res. 2014;219(3):420-425. PubMed CrossRef
5. Drake RJ, Haley CJ, Akhtar S, et al. Causes and consequences of duration of untreated psychosis in schizophrenia. Br J Psychiatry. 2000;177(6):511-515. PubMed CrossRef
6. Meagher DJ, Quinn JF, Bourke S, et al. Longitudinal assessment of psychopathological domains over late-stage schizophrenia in relation to duration of initially untreated psychosis: 3-year prospective study in a long-term inpatient population. Psychiatry Res. 2004;126(3):217-227. PubMed CrossRef
7. Beary M, Hodgson R, Wildgust HJ. A critical review of major mortality risk factors for all-cause mortality in first-episode schizophrenia: clinical and research implications. J Psychopharmacol. 2012;26(5 suppl):52-61. PubMed CrossRef
8. National Collaborating Centre for Mental Health (UK). Psychosis and Schizophrenia in Children and Young People: Recognition and Management. NICE Clinical Guidelines, No. 155. Leicester, UK: British Psychological Society; 2013.
9. Carpenter WT, Buchanan RW. Early intervention: how early and with what? Schizophr Bull. 2015;41(1):4-5. PubMed CrossRef
10.Addington J, Addington D, Abidi S, et al. Canadian Treatment Guidelines for individuals at clinical high risk of psychosis. Can J Psychiatry. 2017;62(9):656-661. PubMed CrossRef
11.Stafford MR, Jackson H, Mayo-Wilson E, et al. Early interventions to prevent psychosis: systematic review and meta-analysis. BMJ. 2013;346:f185. PubMed CrossRef
12.Hutton P, Taylor PJ. Cognitive behavioural therapy for psychosis prevention: a systematic review and meta-analysis. Psychol Med. 2014;44(3):449-468. PubMed CrossRef
13.Choi J, Corcoran CM, Fiszdon JM, et al. Pupillometer-based neurofeedback cognitive training to improve processing speed and social functioning in individuals at clinical high risk for psychosis. Psychiatr Rehabil J. 2017;40(1):33-42. PubMed CrossRef
14.McGorry PD, Nelson B, Markulev C, et al. Effect of ω-3 polyunsaturated fatty acids in young people at ultrahigh risk for psychotic disorders: the NEURAPRO randomized clinical trial. JAMA Psychiatry. 2017;74(1):19-27. PubMed CrossRef
15.Kantrowitz JT, Woods SW, Petkova E, et al. D-serine for the treatment of negative symptoms in individuals at clinical high risk of schizophrenia: a pilot, double-blind, placebo-controlled, randomised parallel group mechanistic proof-of-concept trial. Lancet Psychiatry. 2015;2(5):403-412. PubMed CrossRef
16.Greco T, Biondi-Zoccai G, Saleh O, et al. The attractiveness of network meta-analysis: a comprehensive systematic and narrative review. Heart Lung Vessel. 2015;7(2):133-142. PubMed
17.Jansen JP, Naci H. Is network meta-analysis as valid as standard pairwise meta-analysis? it all depends on the distribution of effect modifiers. BMC Med. 2013;11(1):159. PubMed CrossRef
18.Liberati A, Altman DG, Tetzlaff J, et al. The PRISMA statement for reporting systematic reviews and meta-analyses of studies that evaluate healthcare interventions: explanation and elaboration. BMJ. 2009;339:b2700. PubMed CrossRef
19.Hutton B, Salanti G, Caldwell DM, et al. The PRISMA extension statement for reporting of systematic reviews incorporating network meta-analyses of health care interventions: checklist and explanations. Ann Intern Med. 2015;162(11):777-784. PubMed CrossRef
20.Moher D, Shamseer L, Clarke M, et al; PRISMA-P Group. Preferred reporting items for systematic review and meta-analysis protocols (PRISMA-P) 2015 statement. Syst Rev. 2015;4(1):1. PubMed CrossRef
21.Stroup DF, Berlin JA, Morton SC, et al. Meta-analysis of observational studies in epidemiology: a proposal for reporting: Meta-analysis of Observational Studies in Epidemiology (MOOSE) group. JAMA. 2000;283(15):2008-2012. PubMed CrossRef
22.Moher D, Liberati A, Tetzlaff J, et al. PRISMA Group. Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement. BMJ. 2009:339:b2535.
23.Higgins JPT, Green S. Cochrane Handbook for Systematic Reviews of Interventions. Chichester, UK: John Wiley & Sons; 2011.
24.Review manager (RevMan)[computer program]: Version 5.1. Copenhagen, Denmark: Cochrane Collaboration; 2011.
25.Sterne JA, Hernán MA, Reeves BC, et al. ROBINS-I: a tool for assessing risk of bias in non-randomised studies of interventions. BMJ. 2016;355:i4919. PubMed CrossRef
26.Puhan MA, Schünemann HJ, Murad MH, et al; GRADE Working Group. A GRADE Working Group approach for rating the quality of treatment effect estimates from network meta-analysis. BMJ. 2014;349:g5630. PubMed CrossRef
27.Javitt DC, Zukin SR. Recent advances in the phencyclidine model of schizophrenia. Am J Psychiatry. 1991;148(10):1301-1308. PubMed CrossRef
28.Woods SW, Walsh BC, Hawkins KA, et al. Glycine treatment of the risk syndrome for psychosis: report of two pilot studies. Eur Neuropsychopharmacol. 2013;23(8):931-940. PubMed CrossRef
29.DerSimonian R, Laird N. Meta-analysis in clinical trials. Control Clin Trials. 1986;7(3):177-188. PubMed CrossRef
30.White IR. Multivariate random-effects meta-regression: updates to mvmeta. Stata J. 2011;11(2):255-270. CrossRef
31.Higgins JP, Jackson D, Barrett JK, et al. Consistency and inconsistency in network meta-analysis: concepts and models for multi-arm studies. Res Synth Methods. 2012;3(2):98-110. PubMed CrossRef
32.Dias S, Sutton AJ, Ades AE, et al. Evidence synthesis for decision making 2: a generalized linear modeling framework for pairwise and network meta-analysis of randomized controlled trials. Med Decis Making. 2013;33(5):607-617. PubMed CrossRef
33.Caldwell DM, Ades AE, Higgins JPT. Simultaneous comparison of multiple treatments: combining direct and indirect evidence. BMJ. 2005;331(7521):897-900. PubMed CrossRef
34.White IR, Barrett JK, Jackson D, et al. Consistency and inconsistency in network meta-analysis: model estimation using multivariate meta-regression. Res Synth Methods. 2012;3(2):111-125. PubMed CrossRef
35.Chaimani A, Higgins JPT, Mavridis D, et al. Graphical tools for network meta-analysis in STATA. PLoS One. 2013;8(10):e76654. PubMed CrossRef
36.Dias S, Welton NJ, Sutton AJ, et al. Evidence synthesis for decision making 4: inconsistency in networks of evidence based on randomized controlled trials. Med Decis Making. 2013;33(5):641-656. PubMed CrossRef
37.Veroniki AA, Vasiliadis HS, Higgins JPT, et al. Evaluation of inconsistency in networks of interventions. Int J Epidemiol. 2013;42(1):332-345. PubMed CrossRef
38.Song F, Altman DG, Glenny A-M, et al. Validity of indirect comparison for estimating efficacy of competing interventions: empirical evidence from published meta-analyses. BMJ. 2003;326(7387):472. PubMed CrossRef
39.Salanti G. Indirect and mixed-treatment comparison, network, or multiple-treatments meta-analysis: many names, many benefits, many concerns for the next generation evidence synthesis tool. Res Synth Methods. 2012;3(2):80-97. PubMed CrossRef
40.Addington J, Epstein I, Liu L, et al. A randomized controlled trial of cognitive behavioral therapy for individuals at clinical high risk of psychosis. Schizophr Res. 2011;125(1):54-61. PubMed CrossRef
41.Bechdolf A, Müller H, Stützer H, et al. 108. PREVENT: A randomized controlled trial for the prevention of first-episode psychosis comparing cognitive-behavior therapy (CBT), clinical management, and aripiprazole combined and clinical management and placebo combined. Schizophr Bull. 2017;43(suppl 1):S56-S57. CrossRef
42.Albert N, Glenth׸j LB, Melau M, et al. Course of illness in a sample of patients diagnosed with a schizotypal disorder and treated in a specialized early intervention setting: findings from the 3.5 year follow-up of the OPUS II study. Schizophr Res. 2017;182:24-30. PubMed CrossRef
43.Amminger GP, Schפfer MR, Papageorgiou K, et al. Long-chain omega-3 fatty acids for indicated prevention of psychotic disorders: a randomized, placebo-controlled trial. Arch Gen Psychiatry. 2010;67(2):146-154. PubMed CrossRef
44.Amminger GP, Leicester S, Yung AR, et al. Early-onset of symptoms predicts conversion to non-affective psychosis in ultra-high risk individuals. Schizophr Res. 2006;84(1):67-76. PubMed CrossRef
45.Amminger GP, Schפfer MR, Schlögelhofer M, et al. Longer-term outcome in the prevention of psychotic disorders by the Vienna omega-3 study. Nat Commun. 2015;6(1):7934. PubMed CrossRef
46.Bechdolf A, Wagner M, Ruhrmann S, et al. Preventing progression to first-episode psychosis in early initial prodromal states. Br J Psychiatry. 2012;200(1):22-29. PubMed CrossRef
47.Berger GE, Wood SJ, Ross M, et al. Neuroprotective effects of low-dose lithium in individuals at ultra-high risk for psychosis: a longitudinal MRI/MRS study. Curr Pharm Des. 2012;18(4):570-575. PubMed CrossRef
48.Cadenhead K, Addington J, Cannon T, et al. 23. Omega-3 fatty acid versus placebo in a clinical high-risk sample from the North American Prodrome Longitudinal Studies (NAPLS) Consortium. Schizophr Bull. 2017;43(suppl 1):S16-S16. CrossRef
49.Cornblatt BA, Lencz T, Smith CW, et al. Can antidepressants be used to treat the schizophrenia prodrome? results of a prospective, naturalistic treatment study of adolescents. J Clin Psychiatry. 2007;68(4):546-557. PubMed CrossRef
50.Fusar-Poli P, Frascarelli M, Valmaggia L, et al. Antidepressant, antipsychotic and psychological interventions in subjects at high clinical risk for psychosis: OASIS 6-year naturalistic study. Psychol Med. 2015;45(6):1327-1339. PubMed CrossRef
51.Hawkins KA, Keefe RS, Christensen BK, et al. Neuropsychological course in the prodrome and first episode of psychosis: findings from the PRIME North America Double Blind Treatment Study. Schizophr Res. 2008;105(1-3):1-9. PubMed CrossRef
52.Ising HK, Kraan TC, Rietdijk J, et al. Four-year follow-up of cognitive behavioral therapy in persons at ultra-high risk for developing psychosis: the Dutch Early Detection Intervention Evaluation (EDIE-NL) trial. Schizophr Bull. 2016;42(5):1243-1252. PubMed CrossRef
53.Kéri S, Kelemen O, Janka Z. Therapy of mental states at high risk for psychosis: preliminary results from Hungary [article in Hungarian]. Orv Hetil. 2006;147(5):201-204. PubMed
54.Kim E, Jang JH, Park H-Y, et al. Pharmacotherapy and clinical characteristics of ultra-high-risk for psychosis according to conversion status: a naturalistic observational study. Early Interv Psychiatry. 2012;6(1):30-37. PubMed CrossRef
55.Kim KR, Lee SY, Kang JI, et al. Clinical efficacy of individual cognitive therapy in reducing psychiatric symptoms in people at ultra-high risk for psychosis. Early Interv Psychiatry. 2011;5(2):174-178. PubMed CrossRef
56.Kobayashi H, Morita K, Takeshi K, et al. Effects of aripiprazole on insight and subjective experience in individuals with an at-risk mental state. J Clin Psychopharmacol. 2009;29(5):421-425. PubMed CrossRef
57.Liu CC, Sheu YH, Wu SY, et al. Rapid response to antipsychotic treatment on psychotic prodrome: implications from a case series. Psychiatry Clin Neurosci. 2010;64(2):202-206. PubMed CrossRef
58.Loewy R, Fisher M, Schlosser DA, et al. Intensive auditory cognitive training improves verbal memory in adolescents and young adults at clinical high risk for psychosis. Schizophr Bull. 2016;42(suppl 1):S118-S126. PubMed CrossRef
59.McFarlane WR, Levin B, Travis L, et al. Clinical and functional outcomes after 2 years in the early detection and intervention for the prevention of psychosis multisite effectiveness trial. Schizophr Bull. 2015;41(1):30-43. PubMed CrossRef
60.McGlashan TH, Zipursky RB, Perkins D, et al. Randomized, double-blind trial of olanzapine versus placebo in patients prodromally symptomatic for psychosis. Am J Psychiatry. 2006;163(5):790-799. PubMed CrossRef
61.McGorry PD, Nelson B, Phillips LJ, et al. Randomized controlled trial of interventions for young people at ultra-high risk of psychosis: twelve-month outcome. J Clin Psychiatry. 2013;74(4):349-356. PubMed CrossRef
62.McGorry PD, Yung AR, Phillips LJ, et al. Randomized controlled trial of interventions designed to reduce the risk of progression to first-episode psychosis in a clinical sample with subthreshold symptoms. Arch Gen Psychiatry. 2002;59(10):921-928. PubMed CrossRef
63.Miklowitz DJ, O’ Brien MP, Schlosser DA, et al. Family-focused treatment for adolescents and young adults at high risk for psychosis: results of a randomized trial. J Am Acad Child Adolesc Psychiatry. 2014;53(8):848-858. PubMed CrossRef
64.Morita K, Kobayashi H, Takeshi K, et al. Poor outcome associated with symptomatic deterioration among help-seeking individuals at risk for psychosis: a naturalistic follow-up study. Early Interv Psychiatry. 2014;8(1):24-31. PubMed CrossRef
65.Morrison AP, French P, Parker S, et al. Three-year follow-up of a randomized controlled trial of cognitive therapy for the prevention of psychosis in people at ultrahigh risk. Schizophr Bull. 2007;33(3):682-687. PubMed CrossRef
66.Morrison AP, French P, Stewart SLK, et al. Early detection and intervention evaluation for people at risk of psychosis: multisite randomised controlled trial. BMJ. 2012;344:e2233. PubMed CrossRef
67.Morrison AP, French P, Walford L, et al. Cognitive therapy for the prevention of psychosis in people at ultra-high risk: randomised controlled trial. Br J Psychiatry. 2004;185(4):291-297. PubMed CrossRef
68.Nordentoft M, Thorup A, Petersen L, et al. Transition rates from schizotypal disorder to psychotic disorder for first-contact patients included in the OPUS trial: a randomized clinical trial of integrated treatment and standard treatment. Schizophr Res. 2006;83(1):29-40. PubMed CrossRef
69.O’ Brien MP, Zinberg JL, Bearden CE, et al. Psychoeducational multi-family group treatment with adolescents at high risk for developing psychosis. Early Interv Psychiatry. 2007;1(4):325-332. PubMed CrossRef
70.Phillips LJ, McGorry PD, Yuen HP, et al. Medium term follow-up of a randomized controlled trial of interventions for young people at ultra high risk of psychosis. Schizophr Res. 2007;96(1-3):25-33. PubMed CrossRef
71.Rybakowski JK, Drózdz W, Borkowska A. Low dose risperidone in the treatment of schizophrenia-like symptoms in high-risk subjects. J Clin Psychopharmacol. 2003;23(6):674-675. PubMed CrossRef
72.Shim G, Kang D-H, Choi J-S, et al. Prospective outcome of early intervention for individuals at ultra-high-risk for psychosis. Early Interv Psychiatry. 2008;2(4):277-284. PubMed CrossRef
73.Stain HJ, Bucci S, Baker AL, et al. A randomised controlled trial of cognitive behaviour therapy versus non-directive reflective listening for young people at ultra high risk of developing psychosis: the Detection and Evaluation of Psychological Therapy (DEPTh) trial. Schizophr Res. 2016;176(2-3):212-219. PubMed CrossRef
74.Tsujino N, Nemoto T, Morita K, et al. Long-term efficacy and tolerability of perospirone for young help-seeking people at clinical high risk: a preliminary open trial. Clin Psychopharmacol Neurosci. 2013;11(3):132-136. PubMed CrossRef
75.van der Gaag M, Nieman DH, Rietdijk J, et al. Cognitive behavioral therapy for subjects at ultrahigh risk for developing psychosis: a randomized controlled clinical trial. Schizophr Bull. 2012;38(6):1180-1188. PubMed CrossRef
76.Walker EF, Cornblatt BA, Addington J, et al. The relation of antipsychotic and antidepressant medication with baseline symptoms and symptom progression: a naturalistic study of the North American Prodrome Longitudinal Sample. Schizophr Res. 2009;115(1):50-57. PubMed CrossRef
77.Woods S, Saksa J, Compton M, et al. 112. Effects of ziprasidone versus placebo in patients at clinical high risk for psychosis. Schizophr Bull. 2017;43(suppl 1):S58-S58. CrossRef
78.Woods SW, Tully EM, Walsh BC, et al. Aripiprazole in the treatment of the psychosis prodrome: an open-label pilot study. Br J Psychiatry suppl. 2007;51:s96-s101. PubMed CrossRef
79.Yung AR, Phillips LJ, Nelson B, et al. Randomized controlled trial of interventions for young people at ultra high risk for psychosis: 6-month analysis. J Clin Psychiatry. 2011;72(4):430-440. PubMed CrossRef
80.Zarafonitis S, Wagner M, Putzfeld V, et al. Psychoeducation for persons at risk of psychosis: results of a randomized controlled study. Psychotherapeut. 2012;57(4):326-334.
81.Roder V, Mueller DR, Schmidt SJ. Effectiveness of integrated psychological therapy (IPT) for schizophrenia patients: a research update. Schizophr Bull. 2011;37(suppl 2):S71-S79. PubMed CrossRef
82.Caqueo-Ur×zar A, Rus-Calafell M, Urzúa A, et al. The role of family therapy in the management of schizophrenia: challenges and solutions. Neuropsychiatr Dis Treat. 2015;11:145-151. PubMed
83.Bird V, Premkumar P, Kendall T, et al. Early intervention services, cognitive-behavioural therapy and family intervention in early psychosis: systematic review. Br J Psychiatry. 2010;197(5):350-356. PubMed CrossRef
84.Fusar-Poli P, Carpenter WT, Woods SW, et al. Attenuated psychosis syndrome: ready for DSM-5.1? Annu Rev Clin Psychol. 2014;10(1):155-192. PubMed CrossRef
85.Fusar-Poli P, Bonoldi I, Yung AR, et al. Predicting psychosis: meta-analysis of transition outcomes in individuals at high clinical risk. Arch Gen Psychiatry. 2012;69(3):220-229. PubMed CrossRef
86.Fusar-Poli P, Cappucciati M, Rutigliano G, et al. Towards a standard psychometric diagnostic interview for subjects at ultra high risk of psychosis: CAARMS versus SIPS. Psychiatry J. 2016;2016:7146341. PubMed CrossRef
87.von Hippel PT. The heterogeneity statistic I(2) can be biased in small meta-analyses. BMC Med Res Methodol. 2015;15(1):35. PubMed CrossRef
88.Kane JM, Schooler NR, Marcy P, et al. The RAISE early treatment program for first-episode psychosis: background, rationale, and study design. J Clin Psychiatry. 2015;76(3):240-246. PubMed CrossRef
89.Kane JM, Robinson DG, Schooler NR, et al. Comprehensive versus usual community care for first-episode psychosis: 2-Year outcomes from the NIMH RAISE Early Treatment Program. Am J Psychiatry. 2016;173(4):362-372. PubMed CrossRef
90.O’ Brien MP, Gordon JL, Bearden CE, et al. Positive family environment predicts improvement in symptoms and social functioning among adolescents at imminent risk for onset of psychosis. Schizophr Res. 2006;81(2-3):269-275. PubMed CrossRef
Enjoy this premium PDF as part of your membership benefits!