Suicidal Thoughts and Reasons for Living in Hospitalized Patients With Severe Depression: Post-Hoc Analyses of a Double-Blind Randomized Trial of Duloxetine

ABSTRACT
Objective: To evaluate suicidal thoughts in relationship to depressive symptom severity and reasons for living in patients hospitalized for major depressive disorder (MDD).
Method: A post hoc analysis was conducted of a randomized, double-blind, parallel-group trial involving hospitalized patients with MDD (DSM-IV criteria) who received duloxetine 60 mg once daily or duloxetine 60 mg twice daily for 8 weeks. After 4 weeks, the dose for nonresponders receiving 60 mg once daily could be increased to 60 mg twice daily (double-blind). The study was conducted between February 9, 2007, and August 26, 2008 at 43 centers in 4 countries across Europe and South Africa. Suicidal thoughts were assessed with Montgomery-Asberg Depression Rating Scale (MADRS) item 10, depression severity was assessed with the 6-item Hamilton Depression Rating Scale and the Clinical Global Impressions-Severity of Illness scale, and protective factors were assessed with the patient-rated Reasons for Living Inventory (RFL) assessing 6 domains. Descriptive statistics, correlation, and linear regression analysis were performed.
Results: At baseline, patients (N = 336) had varying severity of suicidal thoughts: 18% had a score ≥ 4. The proportion of patients with a score ≥ 4 decreased to 7% at week 1 and 1% at week 8 of treatment. The RFL scores at baseline were lower in patients with higher baseline suicidal thoughts and increased significantly during treatment (P < .0001). A regression model revealed that only 16% of variance in baseline total RFL score is explained by the different MADRS items. Eight patients had suicidal behavior or ideation recorded as an adverse event during the study; no consistent pattern was found in the different psychometric scores either at baseline or at the visit preceding the suicidal behavior/ideation.
Conclusions: Suicidality rapidly decreased in hospitalized patients with severe depression treated with duloxetine. The RFL scores were low at baseline but increased during treatment, suggesting that they are at least partially state rather than trait variables. Since RFL scores are lower in depressed inpatients, these scores lose the predictive value that they have in a general population sample.
Trial Registration: ClinicalTrials.gov identifier: NCT00422162
Prim Care Companion CNS Disord 2014;16(3):doi:10.4088/PCC.13m01591
© Copyright 2014 Physicians Postgraduate Press, Inc.
Submitted: October 4, 2013; accepted December 20, 2013.
Published online: May 1, 2014.
Corresponding author: Koen Demyttenaere, MD, PhD, University Psychiatric Center-Campus Gasthuisberg, Herestraat 49, 3000 Leuven, Belgium ([email protected]).
Every year, almost 1 million people die from suicide, which is equivalent to 1 death every 40 seconds, and suicide rates increased in the last 45 years by 60% worldwide.1 The majority of studies examining variables associated with suicidal behavior focus on risk factors, and only a few evaluate possible protective factors against suicidal behavior.2
Around 15% of patients with major depressive disorder (MDD) acknowledge having made a suicide attempt, and between 2% and 12% of those with a major depressive episode end their lives by suicide.1,3,4 The ratio of completed suicides to attempts is higher in patients with affective disorders than in the general population, which suggests a high lethality of suicidal behavior in patients with this pathology and implies that particular attention must be paid to suicidal ideas and behaviors in these individuals.5 Many studies have investigated risk factors for completed suicide or suicide attempt in different populations including those with major depression. A review of prospective studies shows that past suicidal behavior, bipolar depression, psychotic depression, recurrence or failure to achieve remission, comorbid borderline personality disorder, comorbid alcohol or substance abuse including cigarette smoking, traits of impulsivity-aggression-hostility, hopelessness, and personal debt have all been suggested as risk factors in patients with depression.6 Further, hopelessness has been reported as one of the major risk factors for committing suicide.7-9 The period of highest risk seems to be the months following hospitalization.6
It has been suggested by Malone and colleagues10 that “a seldom-posed but important question is not why patients with depression want to commit suicide, but why they want to live.”(p1,084) Indeed, few studies have investigated the protective factors against suicidal acts, but family connectedness and family and peer support, as well as moral or religious objections, have been repeatedly described as protecting against suicide.11-13 Additional protective factors include religious/spiritual coping,14,15 assertiveness and perceived social support,15 and parent connectedness and academic achievement.16,17 The Reasons for Living Inventory (RFL)18 is a self-report instrument that measures “reasons for staying alive when you are thinking of killing yourself” and is composed of 48 items covering 6 domains: survival and coping beliefs, responsibility to family, child-related concerns, fear of (committing) suicide, fear of social disapproval, and moral objections to suicide. Scores on the 6 subscales of the RFL were found to be lower in patients with major depression who had made a suicide attempt than in those who had not (with the exception of child-related concerns),10 and scores were found to be lower in patients with MDD with near-lethal suicidal behavior than in those with parasuicidal behavior or suicidal ideation only.19
The severity of depression is best conceived as a dimensional concept, and the frequently reported categorical definitions mild, moderate, severe, or very severe are based on artificial cutoffs.20 There is no real consensus on the definition of severe depression, but the following have all been proposed: a higher number of positive DSM diagnostic criteria, a higher score on the Hamilton Depression Rating Scale (HDRS)21 or on the Montgomery-Asberg Depression Rating Scale (MADRS),22 an episode with longer duration, the presence of comorbid conditions, the presence of psychotic features, and the presence of suicidal ideation. The fact that suicidality is included as an item in the DSM criteria and in the most frequently used depression scales assessing change during treatment indicates that more pronounced suicidality is by definition associated with a higher depression severity, but the exact relationship between suicidality and depression severity (excluding the suicidality item) is not sufficiently known.23
Antidepressants, overall, reduce suicidal ideation in patients with depression. An analysis of the Veterans Health Administration data sets (including 226,866 veterans who received a diagnosis of depression)24 showed that suicide attempt rates were lower among patients who were treated with antidepressants than among those who were not, and that suicide attempt rates were also higher prior to treatment than after the start of treatment. Another naturalistic study investigating 1,014 inpatients with depression25 showed that emergence (baseline HDRS item 3 score changing from 0 or 1 at baseline to 3 or 4 at any time during the observational period), worsening (any increase of the item 3 score from baseline during the whole observational period), and improvement of suicidal ideation (any decrease of the item 3 score from baseline during the whole observational period) occurred in 3.2%, 14.7%, and 90.8% of patients, respectively. Beasley et al26 found improvement in suicidal ideation in 72.2% of patients treated with fluoxetine, in 69.8% of patients treated with tricyclic antidepressants, and in 54.8% of patients treated with placebo. A meta-analysis published by Acharya et al27 found that suicidality improved more often in patients treated with duloxetine (74.5%) than in placebo-treated patients (64.5%). On the other hand, increased suicidal ideation in the initial days of treatment with antidepressants has been reported in adolescents and in young adults and resulted in a warning for all antidepressants in patients under age 25 years.28-30
Therefore, this post hoc analysis of the data from a previously published study was conducted to evaluate the evolution of suicidal thoughts in relationship to depressive symptom severity and to reasons for living in patients hospitalized for severe MDD and treated with duloxetine.31

- Suicide is a common phenomenon but difficult to study, and patients with suicidal thoughts are often excluded from clinical studies; therefore, a systematic approach is helpful in clinical practice.
- The Reasons for Living Inventory was utilized in this analysis of relevant social and clinical dimensions.
- Patient management with antidepressant therapy improved depression severity and the reasons for living became prominent.
- Antidepressants, in general, are suspected to trigger suicidal behavior, but this study has data in support of suicide-related adverse events and also the improvement of reasons for living domains with antidepressant therapy.
METHOD
Study Design
These post hoc analyses were carried out with the data from a previously published clinical trial.29 Briefly, the study was a randomized, double-blind, parallel-group trial involving hospitalized patients with severe depression. The study was conducted between February 9, 2007, and August 26, 2008 at 43 centers in 4 countries across Europe and South Africa. The patients were randomized to either duloxetine 60 mg once daily or duloxetine 60 mg twice daily for 8 weeks. After 4 weeks, the dose for nonresponders who were receiving 60 mg once daily could be increased to 60 mg twice daily (double-blind). The primary objective of this study was to test whether duloxetine 120 mg per day provides a better response to treatment than duloxetine 60 mg per day after 4 weeks in patients with severe MDD.
Each clinical study site’s institutional review board approved the protocol, which was developed in accordance with the ethical standards of Good Clinical Practice and the Declaration of Helsinki. All patients provided written informed consent before the commencement of any study procedures. Additional operational information about this study is disclosed under ClinicalTrials.gov identifier: NCT00422162.
Patients
Male or female patients ≥ 18 years of age at screening who met the criteria for severe MDD, as defined by the DSM-IV,32 who had their diagnoses confirmed by the Mini-International Neuropsychiatric Interview (MINI),33 and who had a total score ≥ 30 on the MADRS, a score ≥ 12 on the 6-item HDRS (HDRS-6), and a score ≥ 4 on the Clinical Global Impressions-Severity of Illness scale (CGI-S)34 were included in this study.35 Patients with suicidal behavior were not excluded from this study; an initial hospitalization of at least 2 weeks was required. Additional details of patient inclusion and exclusion criteria can be found in a previous publication.31
Scales
Depression severity was assessed with the MADRS, the HDRS-6, and the CGI-S.
Suicidal thoughts were assessed with MADRS item 10, an item that assesses the feeling that life is not worth living, that a natural death would be welcome, suicidal thoughts, and preparations for suicide (suicide attempts should not in themselves influence the rating). The scoring ranges from 0 to 6: 0 = enjoys life or takes it as it comes; 2 = weary of life, only fleeting suicidal thoughts; 4 = probably better off dead, suicidal thoughts are common, and suicide is considered as a possible solution, but without specific plans or intension; and 6 = explicit plans for suicide when there is an opportunity, active preparations for suicide.
Protective factors were assessed with the patient-rated RFL. This instrument has 48 items covering 6 domains that look at the other side of hopelessness, ie, reasons for not committing suicide. Each item is rated from 1 (not at all important) to 6 (extremely important), so high scores indicate strong reasons for living. The 6 domains include the following: (1) survival and coping beliefs, (2) responsibility to family, (3) child-related concerns, (4) fear of (committing) suicide, (5) fear of social disapproval, and (6) moral objections. The full RFL was assessed at baseline and after 8 weeks; for visits in between, the short form of the RFL was used. The total and the 6 domain scores are calculated as the mean of the nonmissing items, whereby a minimum number of nonmissing items is required.
Statistical Analyses
The data obtained from patients treated daily with either 60 mg or 120 mg of duloxetine were pooled for these post hoc analyses. The analyses are primarily descriptive, but results of t tests are provided for mean change in RFL total score from baseline to endpoint, and for the correlation between individual baseline MADRS item scores and the baseline RFL total score. Linear regression analysis was used to predict total RFL score at baseline and the change in total RFL score between baseline and endpoint. The endpoint is calculated as the last value for treatment up to week 8 (last observation carried forward). The independent variables in the regression model predicting the baseline total RFL score were the 10 individual MADRS items at baseline, age, gender, and number of previous episodes. The independent variables in the regression model predicting change in total RFL score were the change in each of the 10 individual MADRS items from baseline to endpoint, age, gender, and number of previous episodes. All variables except gender were treated as continuous variables, and nonsignificant variables were removed from the regression model in a stepwise fashion to obtain the final model.
RESULTS
Baseline Demographic and Clinical Characteristics
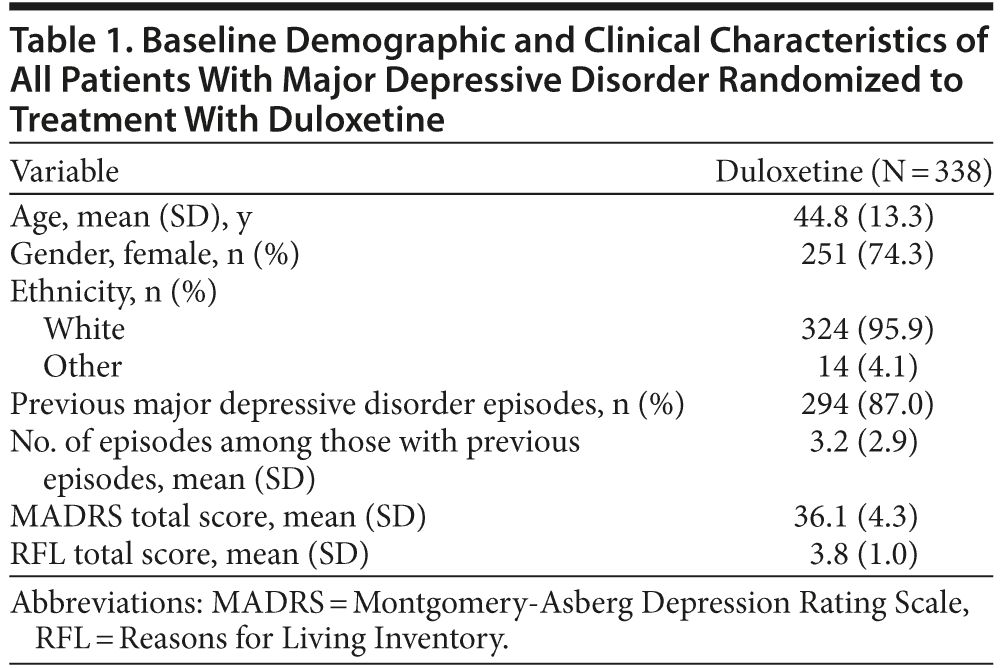
Baseline demographic and clinical characteristics are summarized for the 338 randomized patients in Table 1. All of the patients had severe MDD, and the majority were female (74%) and white (96%). The mean age was 45 years. The study design and the details of baseline characteristics have been published.31 Since 2 patients did not provide any efficacy assessment postbaseline, the full analysis set consisted of 336 patients.
Change in Suicidal Thoughts (MADRS item 10) During Treatment
These hospitalized patients with severe depression showed varying degrees of severity in suicidal thoughts at baseline as assessed with the observer-rated MADRS item 10. At baseline, 65% of the patients had a score of at least 2 (2 being defined as weary of life, only fleeting suicidal thoughts), and 18% had a score of at least 4 (4 being defined as probably better off dead, suicidal thoughts are common and suicide is considered as a possible solution, but without specific plans or intention). However, these more pronounced suicidal thoughts rapidly decreased during the treatment period. The proportion with a score ≥ 4 dropped from 18% at baseline to 7% at week 1; 2% at weeks 2, 3, 4, and 6; and 1% at week 8. Less pronounced suicidal thoughts decreased gradually but more slowly during the treatment period. The proportion with a score ≥ 2 dropped from 65% at baseline to 39% at week 1, 28% at week 2, 21% at week 3, 14% at week 4, 9% at week 6, and 6% at week 8.
Relationship Between Suicidal Thoughts (MADRS item 10) and Severity of Depression, the Other MADRS Items, and the HDRS-6
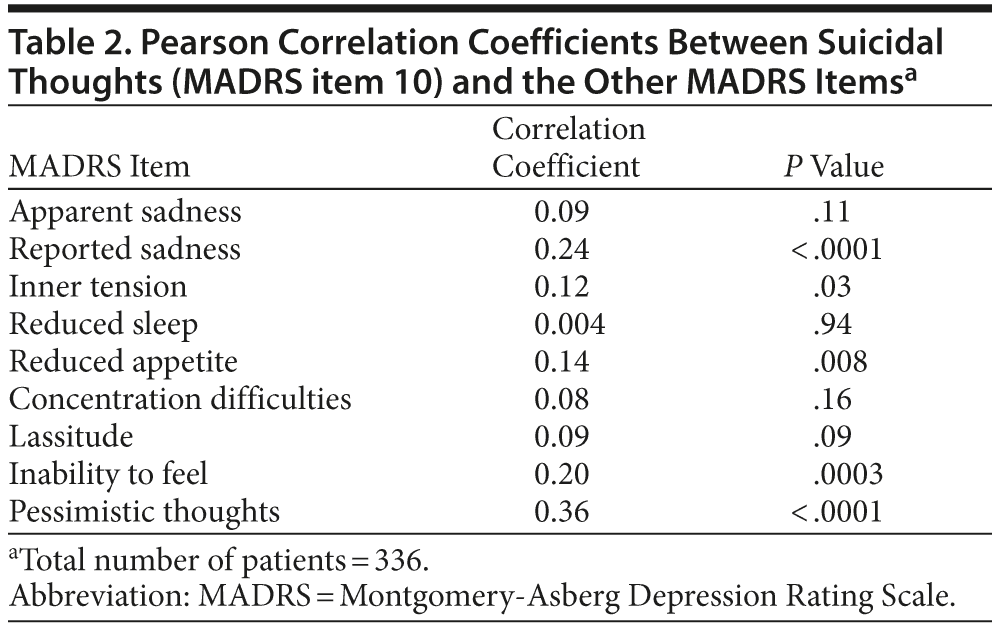
Suicidal thoughts were significantly correlated with the HDRS-6 total score and with the CGI-S (r = 0.12, p = .03 and r = 0.26, < .0001, respectively). Table 2 shows that suicidal thoughts were significantly correlated with 5 other MADRS items (reported sadness, inner tension, reduced appetite, inability to feel, and pessimistic thoughts), although all of these correlation coefficients, again, were rather low. Suicidal thoughts were significantly correlated with only 2 HDRS-6 items: depressed mood and feelings of guilt (r = 0.14, p = .008 and r = 0.18, p = .0008, respectively).
Change in RFL Scores During Treatment
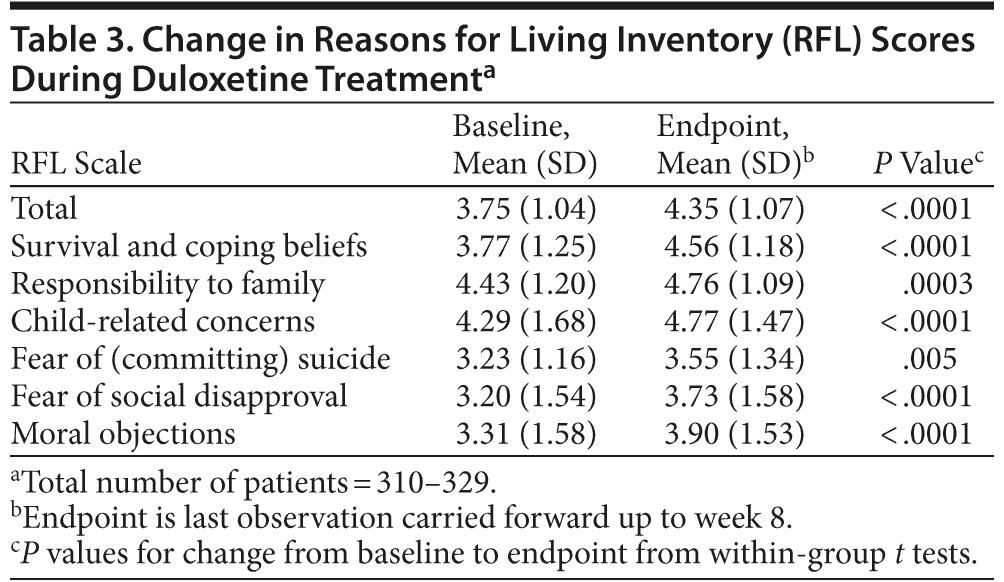
With regard to RFL domain scores, responsibility to family and child-related concerns had the highest mean (protective) scores, while fear of committing suicide, fear of social approval, and moral objections had the lowest mean (protective) scores at baseline as well as at endpoint (Table 3).
The means of the total and all 6 RFL domain scores increased significantly from baseline to endpoint.
Relationship Between Different Baseline RFL Subscores and Suicidal Thoughts (MADRS item 10)
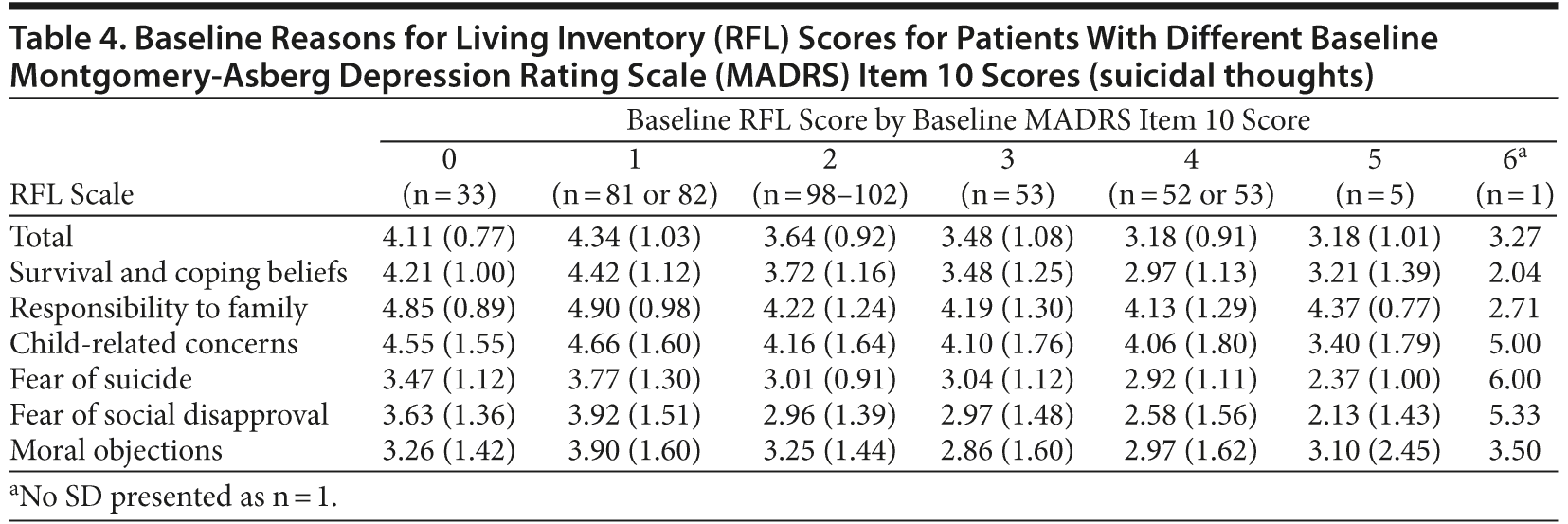
The relationships between baseline RFL scores and MADRS item 10 (suicidal thoughts) are presented in Table 4. The data show that all RFL mean scores tended to be lower with higher baseline MADRS item 10 scores, indicating that higher suicidal ideation as assessed by the physician is related to lower protection by the RFL as assessed by the patient.
Relationship Between MADRS Depressive Symptoms and Total RFL Score
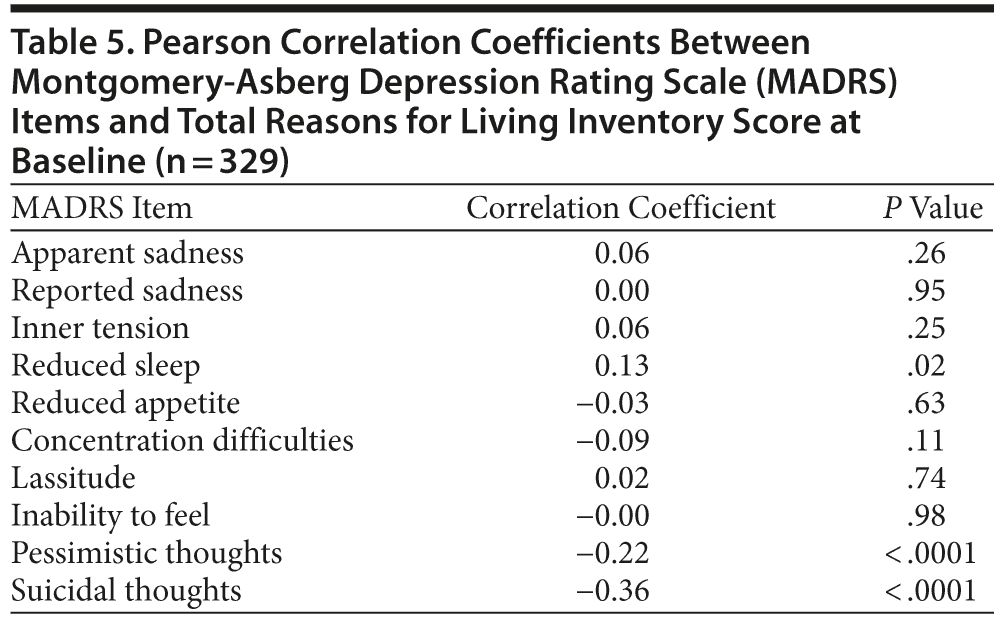
Table 5 shows that most MADRS depressive symptoms were not significantly correlated with the total RFL score. Indeed, only 2 of the 10 MADRS items showed a significantly negative correlation with the total RFL score: pessimistic thoughts and suicidal thoughts (both p < .0001), while 1 item, reduced sleep, showed a significant positive correlation (p = .02).
A regression analysis predicting baseline total RFL score revealed that lower reduced sleep, higher pessimistic thoughts, and higher suicidal ideation significantly predicted lower total RFL score (total R2 = 0.16, p < .0001; coefficients 0.13 [p = .007], −0.12 [p = .03], and −0.26 [p < .0001], respectively).
A regression analysis predicting baseline change in total RFL score from baseline to endpoint revealed that a smaller decrease in reduced sleep and a greater decrease in concentration difficulties, lassitude, and pessimistic thoughts significantly predicted a greater increase in total RFL score (total R2 = 0.20, p < .0001; coefficients 0.08 [p = .03], −0.12 [p = .002], −0.09 [p = .02], and −0.16 [p < .0001], respectively).
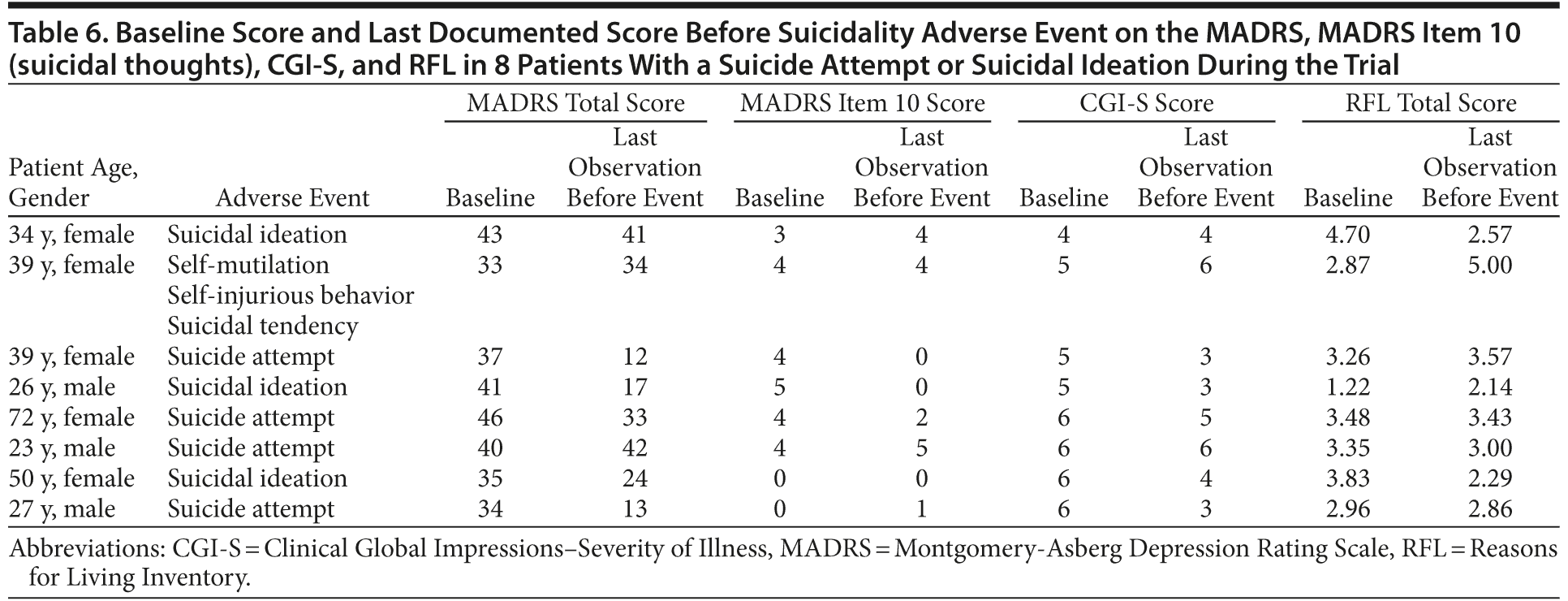
Individual Psychometric Characteristics of the 8 Patients With a Suicide Attempt or Suicidal Ideation During the Trial
Eight patients had suicidal behavior or ideation recorded as an adverse event during the study. The scores for total MADRS, MADRS item 10 (suicidal thoughts), CGI-S, and total RFL at baseline and at the last measurement prior to the adverse event are presented in Table 6. On the basis of the depression measures, these patients had an average depression severity score at baseline (including suicidal ideation) and an average RFL total score; the last assessment before the adverse event shows variable depression severity and low suicidal scores on average.
On the basis of the patient narratives, 7 of 8 cases were serious adverse events (1 case was a significant adverse event). In this study, a serious adverse event is defined as any adverse event that results in death, is immediately life threatening, results in persistent or significant disability/incapacity, requires or prolongs patient hospitalization, is a congenital anomaly/birth defect, or is to be deemed serious for any other reason representing a significant hazard, which is comparable to the aforementioned criteria (standard Council for International Organizations of Medical Sciences criteria [http://www.cioms.ch/]). For example, if a patient says “I will kill myself,” it is considered a serious adverse event per the criteria. However, if the investigator assesses the MADRS and scores item 10 without the patient expressing actively clear suicidal thoughts and therefore no hospitalization occurs, it is a MADRS scoring but not a serious adverse event. Of the 8 patients, 5 discontinued treatment, 6 with adverse events “not related to study drug” were assessed by the investigator, and 5 had a history of suicide attempt. Onset of serious or significant adverse events after study drug initiation ranged from 2 to 37 days.
DISCUSSION
Sixty-five percent of patients hospitalized with severe depression presented at least fleeting suicidal thoughts, and 18% had explicit suicidal thoughts, compared to 52% and 28%, respectively, described in a larger sample of 1,014 patients hospitalized with MDD in Germany.25 As in the German study, suicidal ideation rapidly decreased during inpatient treatment with duloxetine after 1 week of treatment; an 88% decline in patients with severe suicidal ideation (MADRS item 10 score of at least 4) was noted after 2 weeks of hospitalization, comparable with other published data (90% in a study with a variety of antidepressants, 72% in a study with fluoxetine and 70% with tricyclic antidepressants in the same study, and 74% in a meta-analysis with duloxetine).25-27
In the present study, the severity of suicidal ideation was rather poorly correlated with observer-rated depression severity. Indeed, although a significant correlation was found between suicidal thoughts and depression severity as measured by the HDRS-6 and by the CGI-S, correlations were very low (r = 0.12 and 0.26, respectively); only about 1.4% of the variance in HDRS-6 or 6.8% in CGI-S was explained by the suicidal ideation severity. Several previously published studies also found that observer-rated depression severity is poorly related to severity of suicidality. In 2 studies,10,36 no significant differences in the baseline HDRS scores were found between patients with depression who attempted suicide and patients with depression who did not attempt suicide, and no significant differences in the baseline HDRS scores were found in nonsuicidal patients and patients with (treatment-related) resolved or persistent or emergent suicidality. It is, however, interesting to note that, in 1 of the 2 studies,10 in contrast with the observer-rated HDRS, the self-rating depression score (as assessed with the Beck Depression Inventory) was found to be significantly higher in patients with depression who attempted suicide than in those who did not attempt suicide. This finding suggests that observer-rated and self-rated scales can give divergent scores. Some more specific measures such as hopelessness and decreased self-esteem are probably more closely correlated with suicidality than overall observer-rated severity of depression.10,36 Additional studies support these observations.7-9 Hostility, rather than depression severity, has been suggested to be more closely related to suicidality, but this factor was not assessed in the present study. A classic model of depression conceptualizes aggression turned inward and converted into depressive affect. So, theoretically, depressed mood is expressed inwardly, while hostility is expressed outwardly or can be turned into suicidality.37,38 When looking at the correlations between the MADRS suicidal ideation item and the other single MADRS items in the present study, the highest (but still small) correlations were found with reported sadness, inability to feel, and pessimistic thoughts and between the MADRS suicidal ideation item and items in the HDRS-6; the highest was with guilt feelings.
An important clinical finding in the present study is that protective factors against suicide and suicidal behavior were not stable; they were negatively correlated with suicidal ideation severity, and these protective factors tended to increase during the treatment. Compared to the RFL domain scores described in the original article on the RFL,18 the scores in the present study for survival and coping beliefs and for responsibility to family are comparable to original data, but the scores for child-related concerns, fear of suicide, fear of social disapproval, and moral objections were higher at baseline as well as at endpoint. The higher the baseline score for suicidal ideation (MADRS item 10), the lower the RFL domain scores tended to be, but all of the protective RFL domain scores increased significantly from baseline to endpoint. An inverse relation between the RFL responsibility for family score and suicidal ideation severity has been reported previously but only in a cross-sectional analysis of patients with depression.39 To the best of our knowledge, this longitudinal follow-up of RFL scores has not yet been reported in the literature, as most often studies compare RFL scores across groups of patients with depression and with varying degrees of suicidal ideation or look at predictive factors of suicidal acts after major depression or try to evaluate suicidality in specific racial groups.2,10,19,40,41 This is a clinically important point since traditionally accepted protective factors against suicide seem to be less effective when suicidality is pronounced. For example, religiosity (moral objections) has always been considered a protective factor against suicide; this was based on the work of Durkheim,42 who posited that religion acts as a deterrent against suicide because it enhances social integration and normalizes submission or adherence to regulation.42 It has also been suggested that religiosity is protective because religious organizations are easily accessible, provide an important source of positive affect, emphasize social ties, and enhance group cohesiveness.43 In the present study, the strength of these religious/moral beliefs was weakened in patients with higher suicidality, although they again become stronger during treatment. Total RFL scores were lower in patients with high scores on suicidal ideation and in patients with high scores for pessimistic thoughts. It should, however, be remembered that correlations were always low, suggesting that many other factors influence reasons for living and suicidality.
The analysis of the data collected in the 8 patients who had a suicidality adverse event during the study does not show a consistent pattern due to small sample size. The suicidality item score at the last visit before the suicide attempt varied between 0 (for 3 of the 8 patients) and 5 (for 1 patient); the MADRS score varied between 12 and 42, and the RFL scores were not different from the mean scores of the whole study sample. Other studies also often found that a satisfactory instrument for predicting future suicide is not available.44,45
The study limitations include that this article is based on a post hoc analysis of the data of a clinical trial.31 The restrictive nature of the Beck Depression Inventory46 precluded its use in this study, and, therefore, the CGI-S and RFL were used. The RFL was not well established for this type of clinical setting.
In conclusion, baseline suicidal thoughts in hospitalized patients with severe depression rapidly decreased during treatment with duloxetine. Baseline RFL scores tended to be lower in patients with severe suicidal ideation but increased during treatment, which suggests that reasons for living, which provide protective power against suicidality, are to some extent dependent on the affective and cognitive status of the patient at a particular point in time. Depression severity, suicidal thoughts, and reasons for living were, however, mainly independent dimensions since most correlations were low. The analysis of the 8 patients with a suicide attempt or suicidal ideation during the study shows that individual prediction of suicidal behavior remains an elusive goal.
Drug names: duloxetine (Cymbalta), fluoxetine (Prozac and others).
Author affiliations: University Psychiatric Center KU Leuven, Campus Gasthuisberg, Leuven, Belgium (Dr Demyttenaere); Eli Lilly and Company, Indianapolis, Indiana (Dr Desaiah); Eli Lilly and Company, Toronto, Canada (Dr Raskin); Boehringer Ingelheim GmbH (consultant statistician), Oxford, United Kingdom (Dr Cairns); and Boehringer Ingelheim GmbH, Ingelheim, Germany (Dr Brecht).
Potential conflicts of interest: Drs Desaiah and Raskin are employees of and Dr Raskin is a stock shareholder in Eli Lilly. Dr Cairns serves as a consultant to and Dr Brecht is an employee of Boehringer Ingelheim GmbH. Dr Demyttenaere reports no conflicts of interest related to the subject of this article.
Funding/support: This study was supported by Eli Lilly and Company, Indianapolis, Indiana, and Boehringer Ingelheim GmbH, Ingelheim, Germany.
Role of the sponsor: The role of the sponsor was collection of the data, logistical support for the statistical analysis, and assistance in writing the manuscript.
Previous presentation: The data were presented as a poster at the 28th World Congress of the International College of Neuropsychopharmacology; June 3-7, 2012; Stockholm, Sweden.
REFERENCES
1. The World Health Report 2001. Mental health: new understanding, new hope. World Health Organization, Geneva, Switzerland. http://www.who.int/whr/2001/en/. Accessed January 10, 2014.
2. Oquendo MA, Dragatsi D, Harkavy-Friedman J, et al. Protective factors against suicidal behavior in Latinos. J Nerv Ment Dis. 2005;193(7):438-443. PubMed doi:10.1097/01.nmd.0000168262.06163.31
3. Chen YW, Dilsaver SC. Lifetime rates of suicide attempts among subjects with bipolar and unipolar disorders relative to subjects with other Axis I disorders. Biol Psychiatry. 1996;39(10):896-899. PubMed doi:10.1016/0006-3223(95)00295-2
4. Bostwick JM, Pankratz VS. Affective disorders and suicide risk: a reexamination. Am J Psychiatry. 2000;157(12):1925-1932. PubMed doi:10.1176/appi.ajp.157.12.1925
5. Undurraga J, Baldessarini RJ, Valenti M, et al. Suicidal risk factors in bipolar I and II disorder patients. J Clin Psychiatry. 2012;73(6):778-782. PubMed doi:10.4088/JCP.11m07041
6. Oquendo MA, Currier D, Mann JJ. Prospective studies of suicidal behavior in major depressive and bipolar disorders: what is the evidence for predictive risk factors? Acta Psychiatr Scand. 2006;114(3):151-158. PubMed doi:10.1111/j.1600-0447.2006.00829.x
7. Pompili M, Innamorati M, Gonda X, et al. Affective temperaments and hopelessness as predictors of health and social functioning in mood disorder patients: a prospective follow-up study. J Affect Disord. 2013;150(2):216-222. PubMed doi:10.1016/j.jad.2013.03.026
8. Serafini G, Pompili M, Innamorati M, et al. Affective temperamental profiles are associated with white matter hyperintensity and suicidal risk in patients with mood disorders. J Affect Disord. 2011;129(1-3):47-55. PubMed doi:10.1016/j.jad.2010.07.020
9. Pompili M, Iliceto P, Luciano D, et al. Higher hopelessness and suicide risk predict lower self-deception among psychiatric patients and non-clinical individuals. Riv Psichiatr. 2011;46(1):24-30. PubMed
10. Malone KM, Oquendo MA, Haas GL, et al. Protective factors against suicidal acts in major depression: reasons for living. Am J Psychiatry. 2000;157(7):1084-1088. PubMed doi:10.1176/appi.ajp.157.7.1084
11. Molock SD, Puri R, Matlin S, et al. Relationship between religious coping and suicidal behaviors among African American adolescents. J Black Psychol. 2006;32(3):366-389. PubMed doi:10.1177/0095798406290466
12. Lizardi D, Dervic K, Grunebaum MF, et al. The role of moral objections to suicide in the assessment of suicidal patients. J Psychiatr Res. 2008;42(10):815-821. PubMed doi:10.1016/j.jpsychires.2007.09.007
13. Matlin SL, Molock SD, Tebes JK. Suicidality and depression among African American adolescents: the role of family and peer support and community connectedness. Am J Orthopsychiatry. 2011;81(1):108-117. PubMed doi:10.1111/j.1939-0025.2010.01078.x
14. Dervic K, Carballo JJ, Baca-Garcia E, et al. Moral or religious objections to suicide may protect against suicidal behavior in bipolar disorder. J Clin Psychiatry. 2011;72(10):1390-1396. PubMed doi:10.4088/JCP.09m05910gre
15. Dervic K, Grunebaum MF, Burke AK, et al. Protective factors against suicidal behavior in depressed adults reporting childhood abuse. J Nerv Ment Dis. 2006;194(12):971-974. PubMed doi:10.1097/01.nmd.0000243764.56192.9c
16. Eskin M, Ertekin K, Dereboy C, et al. Risk factors for and protective factors against adolescent suicidal behavior in Turkey. Crisis. 2007;28(3):131-139. PubMed
17. Taliaferro LA, Muehlenkamp JJ. Risk and protective factors that distinguish adolescents who attempt suicide from those who only consider suicide in the past year [published online ahead of print July 15, 2013]. Suicide Life Threat Behav. PubMed
18. Linehan MM, Goodstein JL, Nielsen SL, et al. Reasons for staying alive when you are thinking of killing yourself: the Reasons for Living Inventory. J Consult Clin Psychol. 1983;51(2):276-286. PubMed doi:10.1037/0022-006X.51.2.276
19. Blasczyk-Schiep S, Kazén M, Kuhl J, et al. Appraisal of suicidal risk among adolescents and young adults through the Rorschach test. J Pers Assess. 2011;93(5):518-526. PubMed doi:10.1080/00223891.2011.594130
20. Endicott J, Cohen J, Nee J, et al. Hamilton Depression Rating Scale: extracted from regular and change versions of the Schedule for Affective Disorders and Schizophrenia. Arch Gen Psychiatry. 1981;38(1):98-103. PubMed doi:10.1001/archpsyc.1981.01780260100011
21. Hamilton M. A rating scale for depression. J Neurol Neurosurg Psychiatry. 1960;23(1):56-62. PubMed doi:10.1136/jnnp.23.1.56
22. Montgomery SA, Asberg M. A new depression scale designed to be sensitive to change. Br J Psychiatry. 1979;134(4):382-389. PubMed doi:10.1192/bjp.134.4.382
23. Uebelacker LA, Strong D, Weinstock LM, et al. Likelihood of suicidality at varying levels of depression severity: a re-analysis of NESARC data. Suicide Life Threat Behav. 2010;40(6):620-627. PubMed doi:10.1521/suli.2010.40.6.620
24. Gibbons RD, Brown CH, Hur K, et al. Relationship between antidepressants and suicide attempts: an analysis of the Veterans Health Administration data sets. Am J Psychiatry. 2007;164(7):1044-1049. PubMed doi:10.1176/appi.ajp.164.7.1044
25. Seem×¼ller F, Riedel M, Obermeier M, et al. The controversial link between antidepressants and suicidality risks in adults: data from a naturalistic study on a large sample of in-patients with a major depressive episode. Int J Neuropsychopharmacol. 2009;12(2):181-189. PubMed doi:10.1017/S1461145708009139
26. Beasley CM Jr, Dornseif BE, Bosomworth JC, et al. Fluoxetine and suicide: a meta-analysis of controlled trials of treatment for depression. BMJ. 1991;303(6804):685-692. PubMed doi:10.1136/bmj.303.6804.685
27. Acharya N, Rosen AS, Polzer JP, et al. Duloxetine: meta-analyses of suicidal behaviors and ideation in clinical trials for major depressive disorder. J Clin Psychopharmacol. 2006;26(6):587-594. PubMed doi:10.1097/01.jcp.0000246216.26400.db
28. Geddes JR, Barbui C, Cipriani A. Risk of suicidal behaviour in adults taking antidepressants. BMJ. 2009;339(2):b3066. PubMed doi:10.1136/bmj.b3066
29. Barbui C, Esposito E, Cipriani A. Selective serotonin reuptake inhibitors and risk of suicide: a systematic review of observational studies. CMAJ. 2009;180(3):291-297. PubMed doi:10.1503/cmaj.081514
30. Barbui C, Cipriani A, Geddes JR. Antidepressants and suicide symptoms: compelling new insights from the FDA’s analysis of individual patient level data. Evid Based Ment Health. 2008;11(2):34-35. PubMed doi:10.1136/ebmh.11.2.34
31. Brecht S, Desaiah D, Marechal ES, et al. Efficacy and safety of duloxetine 60 mg and 120 mg daily in patients hospitalized for severe depression: a double-blind randomized trial. J Clin Psychiatry. 2011;72(8):1086-1094. PubMed doi:10.4088/JCP.09m05723blu
32. American Psychiatric Association. Diagnostic and Statistical Manual of Mental Disorders, Fourth Edition. Washington, DC: American Psychiatric Association; 1994.
33. Sheehan DV, Lecrubier Y, Sheehan KH, et al. The Mini-International Neuropsychiatric Interview (M.I.N.I.): the development and validation of a structured diagnostic psychiatric interview for DSM-IV and ICD-10. J Clin Psychiatry. 1998;59(suppl 20):22-33, quiz 34-57. PubMed
34. Guy W. Clinical Global Impressions (CGI) Scale [Modified from: Rush J, et al. Psychiatric Measures]. Washington, DC: American Psychiatric Association; 2000.
35. Bech P, Gram LF, Dein E, et al. Quantitative rating of depressive states. Acta Psychiatr Scand. 1975;51(3):161-170. PubMed doi:10.1111/j.1600-0447.1975.tb00002.x
36. Szanto K, Mulsant BH, Houck PR, et al. Emergence, persistence, and resolution of suicidal ideation during treatment of depression in old age. J Affect Disord. 2007;98(1-2):153-161. PubMed doi:10.1016/j.jad.2006.07.015
37. Akiskal HS, McKinney WT Jr. Overview of recent research in depression: integration of ten conceptual models into a comprehensive clinical frame. Arch Gen Psychiatry. 1975;32(3):285-305. PubMed doi:10.1001/archpsyc.1975.01760210019001
38. Benazzi F, Akiskal H. Irritable-hostile depression: further validation as a bipolar depressive mixed state. J Affect Disord. 2005;84(2-3):197-207. PubMed doi:10.1016/j.jad.2004.07.006
39. Britton PC, Duberstein PR, Conner KR, et al. Reasons for living, hopelessness, and suicide ideation among depressed adults 50 years or older. Am J Geriatr Psychiatry. 2008;16(9):736-741. PubMed doi:10.1097/JGP.0b013e31817b609a
40. Oquendo MA, Bongiovi-Garcia ME, Galfalvy H, et al. Sex differences in clinical predictors of suicidal acts after major depression: a prospective study. Am J Psychiatry. 2007;164(1):134-141. PubMed doi:10.1176/appi.ajp.164.1.134
41. Street JC, Taha F, Jones AD, et al. Racial identity and reasons for living in African American female suicide attempters. Cultur Divers Ethnic Minor Psychol. 2012;18(4):416-423. PubMed doi:10.1037/a0029594
42. Durkheim E. Suicide: A Study in Sociology. New York, NY: Free Press; 1951.
43. Stack S, Lester D. The effect of religion on suicide ideation. Soc Psychiatry Psychiatr Epidemiol. 1991;26(4):168-170. PubMed
44. Beck AT, Steer RA. Clinical predictors of eventual suicide: a 5- to 10-year prospective study of suicide attempters. J Affect Disord. 1989;17(3):203-209. PubMed doi:10.1016/0165-0327(89)90001-3
45. Niméus A, Träskman-Bendz L, Alsén M. Hopelessness and suicidal behavior. J Affect Disord. 1997;42(2-3):137-144. PubMed doi:10.1016/S0165-0327(96)01404-8
46. Beck AT, Ward CH, Mendelson M, et al. An inventory for measuring depression. Arch Gen Psychiatry. 1961;4(6):561-571. PubMed doi:10.1001/archpsyc.1961.01710120031004