Objective: To determine if the use of mindfulness-based cognitive therapy (MBCT) in patients with a history of 2 or more episodes of major depressive disorder and other mood disorders will decrease the need for medication management and other interventions and will also decrease the need for outpatient services and the overall cost of treatment.
Methods: The study patients completed MBCT group sessions between January 1, 2010, and December 31, 2013. Patients who had 2 or more episodes of major depressive disorder (recurrent MDD) were categorized into a group. The remaining patients with other mood disorders were placed in a comparison group. The mean differences in drug treatments and hospital utilizations between the recurrent MDD and nonrecurrent MDD group were compared. Wald P values and 95% CIs were obtained for both adjusted and unadjusted estimated mean differences. Covariates were adjusted for age at start of MBCT, gender, and race/ethnicity.
Results: The final sample consisted of 142 patients (93 recurrent MDD and 49 others). There was no significant difference in the effect of MBCT on medication changes between recurrent MDD patients and nonrecurrent MDD patients. Recurrent MDD patients who participated in MBCT experienced reduction in all calls and visits (P = .0068) and less psychiatric visits (P = .0026) in the year after MBCT when compared with the visits before the intervention.
Conclusions: This study evaluated the effectiveness of MBCT in reducing the need for additional psychiatric services. The study evaluated patients who received MBCT over 3 years and demonstrated that MBCT decreased the need for care regardless of medication changes. The results raise the question of whether MBCT allows patients to respond to situations more skillfully or if MBCT itself decreases depressive symptoms. The limitations of this study include a small sample size, patient selection, and its design as a retrospective study. However, this study may have implications as a treatment strategy that may be generalizable to other clinics and patient populations.
Mindfulness-Based Cognitive Therapy for Patients With Depression Decreases the Need for Outpatient Visits

ABSTRACT
Objective: To determine if the use of mindfulness-based cognitive therapy (MBCT) in patients with a history of 2 or more episodes of major depressive disorder and other mood disorders will decrease the need for medication management and other interventions and will also decrease the need for outpatient services and the overall cost of treatment.
Methods: The study patients completed MBCT group sessions between January 1, 2010, and December 31, 2013. Patients who had 2 or more episodes of major depressive disorder (recurrent MDD) were categorized into a group. The remaining patients with other mood disorders were placed in a comparison group. The mean differences in drug treatments and hospital utilizations between the recurrent MDD and nonrecurrent MDD group were compared. Wald P values and 95% CIs were obtained for both adjusted and unadjusted estimated mean differences. Covariates were adjusted for age at start of MBCT, gender, and race/ethnicity.
Results: The final sample consisted of 142 patients (93 recurrent MDD and 49 others). There was no significant difference in the effect of MBCT on medication changes between recurrent MDD patients and nonrecurrent MDD patients. Recurrent MDD patients who participated in MBCT experienced reduction in all calls and visits (P = .0068) and less psychiatric visits (P = .0026) in the year after MBCT when compared with the visits before the intervention.
Conclusions: This study evaluated the effectiveness of MBCT in reducing the need for additional psychiatric services. The study evaluated patients who received MBCT over 3 years and demonstrated that MBCT decreased the need for care regardless of medication changes. The results raise the question of whether MBCT allows patients to respond to situations more skillfully or if MBCT itself decreases depressive symptoms. The limitations of this study include a small sample size, patient selection, and its design as a retrospective study. However, this study may have implications as a treatment strategy that may be generalizable to other clinics and patient populations.
Prim Care Companion CNS Disord 2016;18(4):doi:10.4088/PCC.16m01985
© Copyright 2016 Physicians Postgraduate Press, Inc.
aDepartment of Psychiatry, University of California Irvine, Orange
bKaiser Permanente, Riverside, California
cRegional Research Statistical Support, Kaiser Permanente Southern California
*Corresponding author: Robert G. Bota, MD, University of California Irvine, 101 City Drive, Orange, CA ([email protected]).
Chronic recurrent depression constitutes a major social and financial burden in society. Lifetime prevalence of depression ranges from 17% to 19%,1 and the recurrence rate is 50%-80% for individuals suffering from major depression.2 Mindfulness-based cognitive therapy (MBCT) has emerged as a valuable treatment modality for major depression.3 MBCT has been found to decrease depressive recurrences in patients with chronic mood disorders.4 Furthermore, patients with 3 or more recurrences are particularly responsive to this treatment modality.5
MBCT is a group-based, manualized program intended to teach patients skills that will reduce the recurrence of depressive symptoms. The program is designed to teach participants how to recognize the physical sensations, feelings, and thoughts that are associated with a relapse. It is based on the theory that returning to previous automatic thoughts and behaviors associated with depression will result in the recurrence of depressive symptoms. The premise of MBCT is that it teaches people to become aware of these thoughts and sensations and trains them to create plans or provides strategies for how to cope with these distressing thoughts, feelings, and sensations.
Patients with recurrent major depressive disorder (MDD) have a very high rate of relapse. There are many variables determining the relapse rate, including but not limited to, noncompliance (with treatment in general, not attending therapy sessions, medication management visits, and noncompliance with medication treatment) and natural course of the illness.6 In subsequent episodes of MDD, the relationship between psychological stress and depressive relapse changes. Early episodes are often preceded by significant negative events. When depression remits, the patient’s view of the world does not differ from people who never had a depressive episode. However, with subsequent episodes, stressful events play a progressively less important role.7
Mindfulness can offer tools by which patients’ tolerance to stress, including normal stressors, increases, and, therefore, it can decrease the rate of relapse and increase one’s quality of life. From another pragmatic standpoint, decreased relapse rate will also lead to a decrease in loss of productivity at work, decreased cost of hospitalizations, decreased risk of suicide, and decreased need for services.
MBCT trains people to consciously pay attention to the present moment and to observe and accept thoughts and perceptions in a nonjudgemental manner. This allows one to value his or her thoughts as mental concepts and not as an immovable reality, and it can free people from the distorted reality that they often create and can allow for more clear-sightedness and a greater sense of manageability in life. MBCT is a group type of psychotherapy that is easily administered in the long term.
Previous studies3 have pointed to the effectiveness of MBCT in depression relief and preventing further depressive episodes. The association between MBCT and reduction in depressive symptoms is a large effect size. MBCT significantly reduced the risk of relapse in individuals with 3 or more previous episodes of depression.4 Patients with recurrent depressive episodes demonstrated an increased response to MBCT if they had experienced 3 or more previous episodes of depression.5 Finally, MBCT was shown to provide additional treatment benefits to usual care. For instance, in a study by Kuyken et al,8 MBCT was more effective than maintenance antidepressants in reducing residual depressive symptoms and psychiatric comorbidity and in improving quality of life in physical and psychological domains.
The purpose of this retrospective study was to determine if the use of MBCT in patients with a history of 2 or more episodes of MDD and other mood disorders will decrease the need for medication management and other interventions and outpatient services as well as the overall cost of treatment.

- Mindfulness-based cognitive therapy (MBCT) is a valuable treatment modality for depression.
- Patients with major depressive disorder have a high relapse rate.
- MBCT is a manualized group type of psychotherapy that is easily administered in the long term.
METHOD
Cohort Selection
We examined a cohort of patients who completed MBCT group sessions between January 1, 2010, and December 31, 2013. The patients were referred by psychiatrists from the same clinic. Patients were assigned to several available groups, one of them being MBCT.
Patients who had 2 or more episodes of MDD (recurrent MDD) were included into 1 group. The comparison group was composed of all other patients (patients with mood disorder, bipolar disorder, depressive disorder, but no patients with single-episode MDD). Patients with psychotic disorders and substance use disorder at that time were not referred to the MBCT group. Patients who received MBCT after December 31, 2013 were excluded. We reviewed service utilization 1 year before and 1 year after the MBCT participation.
Statistical Methods
We describe the sample using means with standard deviations or medians with interquartile regions for continuous variables. For discrete variables, we used percentages and counts. P values were obtained using the Fisher exact test for proportions and Wilcoxon test for continuous variables.
We separated patients who completed MBCT into 2 groups: those who had 2 or more episodes of MDD (recurrent MDD) and all others with mood disorders. All patients with MDD were administered the 9-item Patient Health Questionnaire (PHQ-9)9 before and after the intervention. Our group compared the mean differences in drug treatments and hospital utilizations between the MDD and non-MDD group 1 year before the MBCT group therapy and 1 year after. Wald P values and 95% CIs were obtained for both adjusted and unadjusted estimated mean differences. Covariates adjusted for were age at start of MBCT, gender, and race/ethnicity. The study was approved by Kaiser Permanente Regional Institutional Review Board.
RESULTS
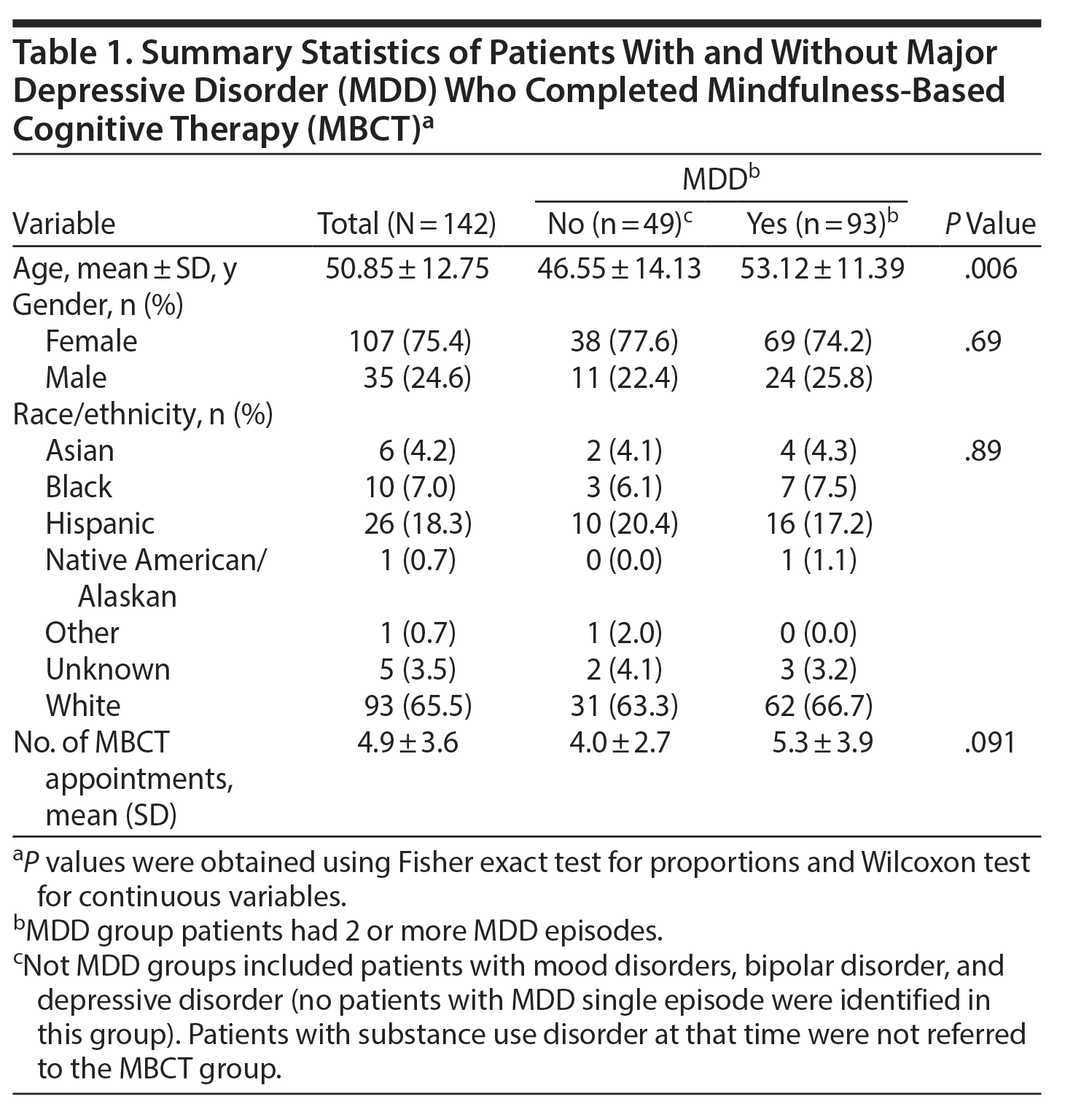
The final sample consisted of 142 patients (93 with recurrent MDD and 49 others). Table 1 shows the characteristics of subjects with and without MDD.
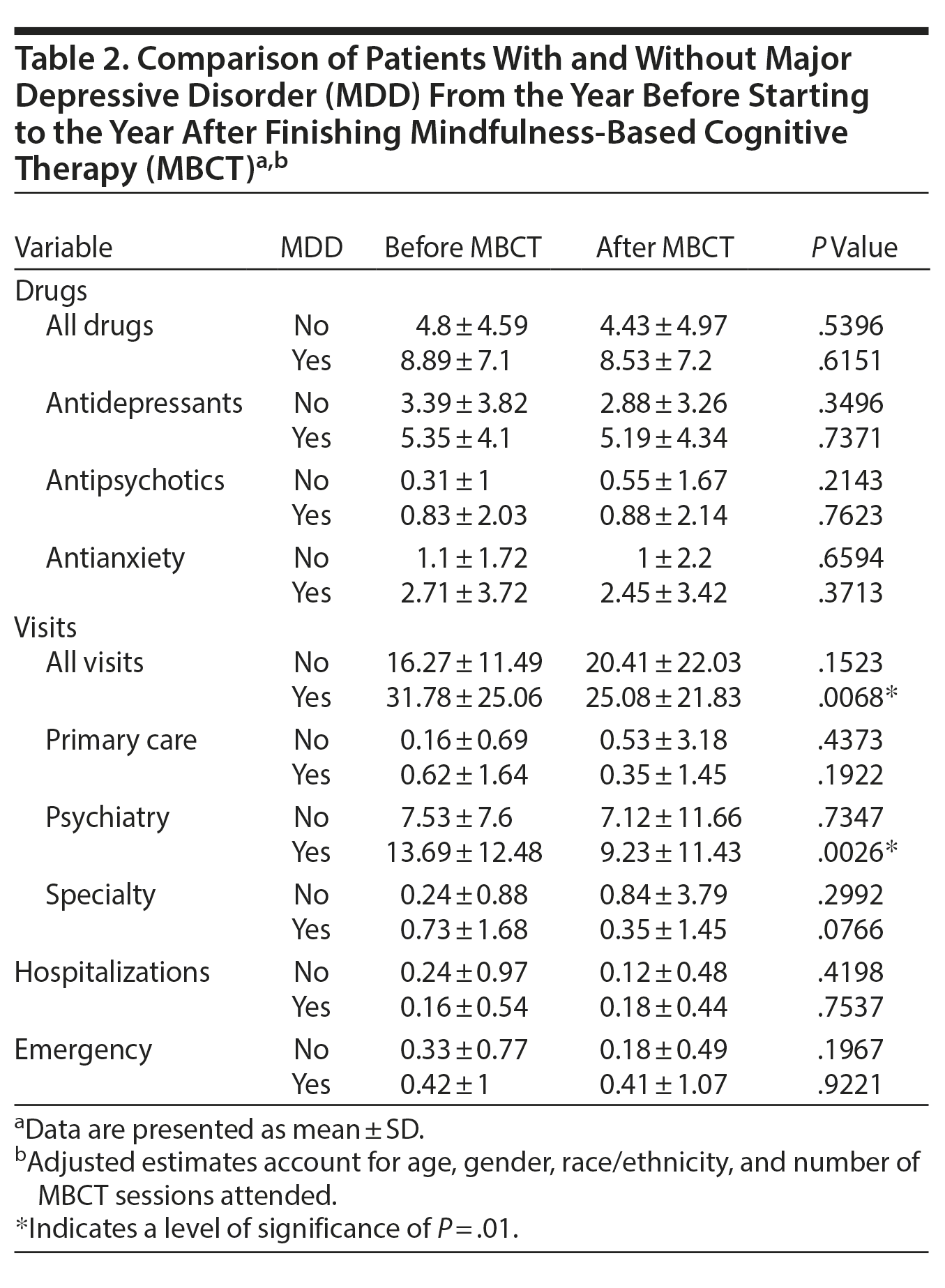
The patients with recurrent MDD had a mean of 6.5 visits (all specialties) less in the year after MBCT than the year before (P < .0068). Specifically, there were 4 fewer psychiatric contacts in the year following MBCT (P = .0026). Patients with recurrent MDD had a PHQ-9 score decreased from 10.15 to 6.3, and difficulties caused by the symptoms decreased to approximately half reported pre-MBCT (odds ratio of 1.09 with a P value of .0013). However, there were no differences in the number of hospitalizations, emergency room visits, primary care visits, or specialty visits in the MDD group before or after MBCT.
Patients with recurrent MDD had no significant difference in medication prescription patterns in general or with regard to specific classes of medications (antipsychotics, antidepressants, or antianxiety medications) before or after MBCT. Table 2 shows the mean difference in number of drug dispenses and hospital utilizations for MDD and non-MDD patients who participated in MBCT group sessions.
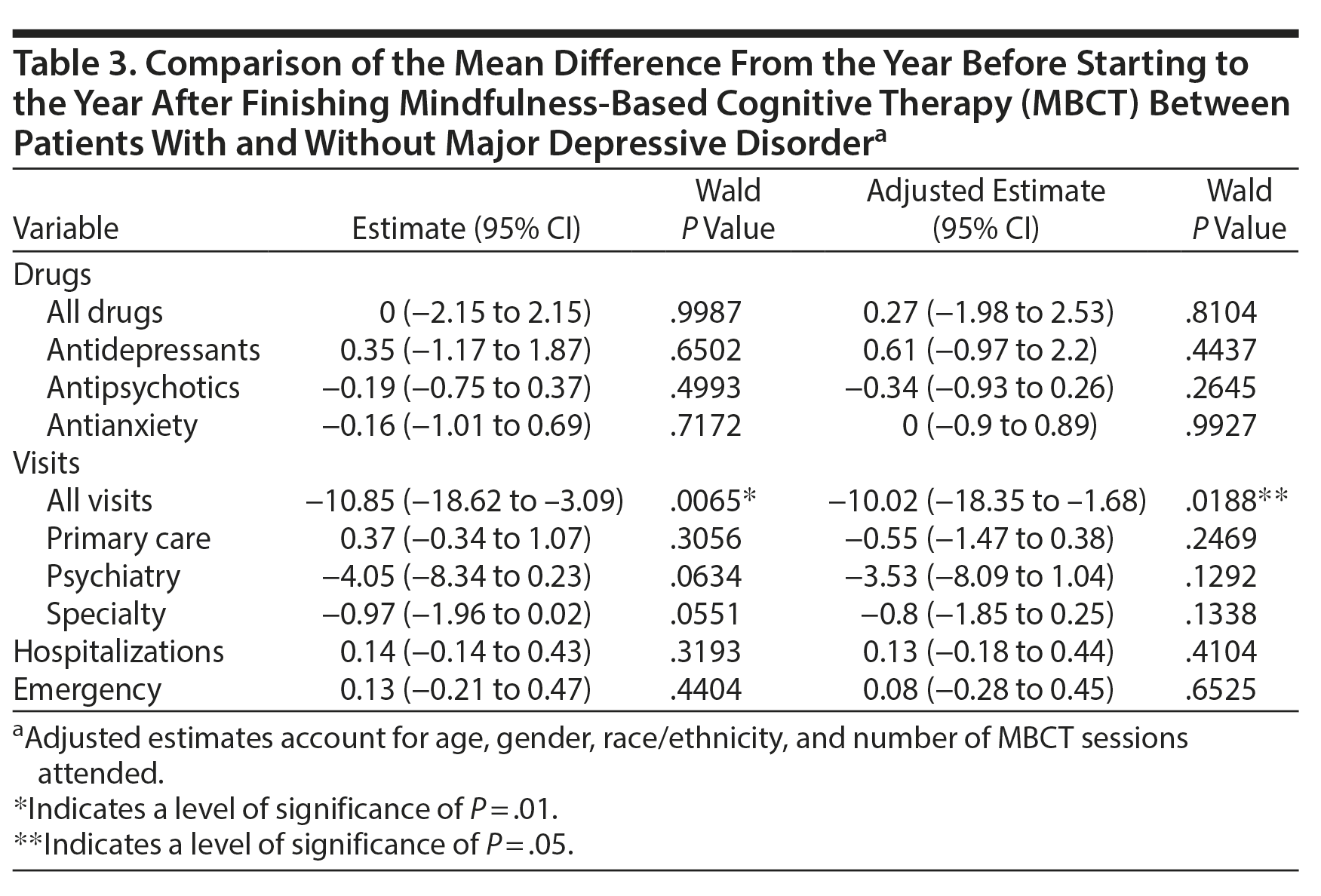
There was no significant difference in the effect of MBCT on medication changes between MDD and non-MDD patients. Recurrent MDD patients who participated in MBCT experienced a larger reduction in total physician calls and visits compared with non-MDD patients (P = .0065). The reduction in specifically psychiatric calls and visits and specialist visits was not significantly greater in recurrent MDD patients when compared with non-MDD patients (P = .0634). Table 3 shows the mean difference in number of drug dispenses and hospital utilizations between recurrent MDD patients and non-MDD patients who participated in MBCT group sessions.
DISCUSSION
Previous studies have shown the financial burden of depression. In 2010, the inflation-adjusted economic burden of depression was an estimated $210 billion,10 of which 45% have direct costs, 5% are suicide-related costs, and 50% are related to workplace costs. Thirty-eight percent of the total cost is related to MDD per se, while the rest is associated with comorbidity. Under such circumstances it is of the utmost importance to devise techniques for the prevention of relapses by a variety of methods, including MBCT. MBCT is a simple and relatively inexpensive treatment modality for relapse prevention. In addition, our study explores the impact of MBCT on utilization of care. As the findings show, patients with a history of MDD who underwent MBCT treatment were less likely to be high utilizers of follow-up psychiatric care. However, the participants in MBCT did not have statistically significant changes in the need for primary care and other specialties.
Unlike earlier studies that examined the effect of MBCT on patients with 3 or more recurrences, our cohort included patients who had 2 previous depressive recurrences. Our study demonstrates that an earlier implementation of this valuable technique is warranted for the prevention of recurrences.5
The antidepressant function of MBCT is complex and may include elements common to a variety of psychotherapeutic techniques. Often, patients with chronic depression are suffering from persistent ruminative depressive cognitive patterns that have been demonstrated to have a maintenance effect on depressed mood.11 One effect of MBCT is related to metacognitive states of mind. Previous contributions12 have shown the curative effects of a metacognitive state (the ability to contemplate one’s own thoughts). A variety of techniques have been designed on the basis of the principle of metacognitive thinking.12 This might explain why, despite there being no significant difference in medication prescription patterns in general or of specific classes of medications (antipsychotics, antidepressants, or antianxiety medications) before or after the MBCT, the patients required less visits to psychiatrists or other providers of care.
MBCT also shares common mechanisms with mindfulness meditation. Mindfulness meditation has been shown to be associated with a variety of structural and functional brain changes, evidenced by functional magnetic resonance imaging, magnetic resonance spectroscopy, and quantitative electroencephalography. In experienced meditators, Luders et al13 reported larger gray matter volumes in the right orbitofrontal cortex and larger volumes of the right hippocampus. These findings were associated with positive emotions, retained emotional stability, and ongoing engagement in mindful behavior. Johnson et al14 studied soldiers who underwent mindfulness training. The soldiers exhibited increased resiliency to stress exposure as demonstrated by enhanced recovery after stress (as measured by heart and respiration rates), a lowering of plasma neuropeptide Y concentration after stressful training, and a decrease in blood oxygen level-dependent signals in the right insula and anterior cingulate.
Additional studies showed specific functional changes in individuals engaged in mindfulness meditation: those with prolonged practice showed sustained activation of the dorsolateral prefrontal cortex and anterior cingulate cortex correlated with increased sustained attention and better attentional error monitoring15; positive association between meditation experience and increased cortical thickness, which persists with aging16; and increased default mode network connectivity, which refers to connectivity in areas of the cortical midline structures, associated with meditation.17 Meditative states, including mindfulness, were further associated with an increased anterior frontal and midline theta synchronization as well as enhanced theta long-distant connectivity between the prefrontal and posterior association cortex, which further supports increased activity of midline brain structures.18 The regular practice of mindfulness meditation showed a decrease of age-related decline in gray matter volume, especially in the area of the putamen, a structure strongly related to attentional processing.19 In addition, intense meditation training was associated with positive psychological variables that paralleled a change in immune cell telomerase activity, pointing to the positive health effects of mindfulness meditation. All of these findings may explain the effects of mindfulness training on individuals suffering from mood disorders.
This study evaluated the effectiveness of MBCT in reducing the need for additional psychiatric services. The age in the recurrent MDD group was statistically higher than in the other group (53 vs 46, P = .006); however, other demographics and the number of completed MBCT sessions did not differ. The study evaluated patients who received MBCT over 3 years and demonstrated that MBCT decreased the need for care regardless of medication changes. The results raise the question of whether MBCT allows patients to respond to situations more skillfully or if MBCT itself decreases depressive symptoms. The limitations of this study include a small sample size, patient selection (the non-MDD group included patients with bipolar disorder and minor depression), and design as a retrospective study. This study does, however, have implications as a treatment strategy that may be generalizable to other patient populations. At first sight, the results seem relatively subtle. However, note that comparative groups are treated patients. In spite of the fact that the comparative groups had undergone treatment, additional benefits were obtained with our MBCT. The results suggest that implementation of an inexpensive intervention has an added beneficial effect in patients suffering from chronic recurrent depressive disorder.
CONCLUSION
MBCT is a safe and useful tool, and patients rated the importance of this intervention for themselves at the end of program at 9.8 out of 10 (where 1 is not important and 10 is extremely important). This intervention can be considered in patients with other diagnoses (for example, patients with anxiety disorders) with minimal increase in expense for the purpose of improving the quality of life for patients, decreasing residual symptoms, and decreasing the utilization of services and cost of care. Further prospective research is needed to understand the mechanisms of differential response and to better quantify the expected areas of improvement for patients suffering from mental illnesses.
Submitted: May 13, 2016; accepted July 6, 2016.
Published online: August 25, 2016.
Potential conflicts of interest: None.
Funding/support: The study was funded by a grant from the Regional Research Committee of Kaiser Permanente Southern California.
Role of the sponsor: The sponsor was not involved in the study design, data collection and interpretation, or preparation and review of the manuscript.
REFERENCES
1. Kessler RC, McGonagle KA, Zhao S, et al. Lifetime and 12-month prevalence of DSM-III-R psychiatric disorders in the United States: results from the National Comorbidity Survey. Arch Gen Psychiatry. 1994;51(1):8-19. PubMed doi:10.1001/archpsyc.1994.03950010008002
2. Judd LL. The clinical course of unipolar major depressive disorders. Arch Gen Psychiatry. 1997;54(11):989-991. PubMed doi:10.1001/archpsyc.1997.01830230015002
3. Kenny MA, Williams JM. Treatment-resistant depressed patients show a good response to mindfulness-based cognitive therapy. Behav Res Ther. 2007;45(3):617-625. PubMed doi:10.1016/j.brat.2006.04.008
4. Teasdale JD, Segal ZV, Williams JM, et al. Prevention of relapse/recurrence in major depression by mindfulness-based cognitive therapy. J Consult Clin Psychol. 2000;68(4):615-623. PubMed doi:10.1037/0022-006X.68.4.615
5. Ma SH, Teasdale JD. Mindfulness-based cognitive therapy for depression: replication and exploration of differential relapse prevention effects. J Consult Clin Psychol. 2004;72(1):31-40. PubMed doi:10.1037/0022-006X.72.1.31
6. El-Hage W, Leman S, Camus V, et al. Mechanisms of antidepressant resistance. Front Pharmacol. 2013;4:146. PubMed doi:10.3389/fphar.2013.00146
7. Segal ZV, Williams JMG, Teasdale JD. Mindfulness-Based Cognitive Therapy for Depression. New York, NY: The Guildford Publications; 2013.
8. Kuyken W, Byford S, Taylor RS, et al. Mindfulness-based cognitive therapy to prevent relapse in recurrent depression. J Consult Clin Psychol. 2008;76(6):966-978. PubMed doi:10.1037/a0013786
9. Feng Y, Huang W, Tian TF, et al. The psychometric properties of the quick inventory of Depressive Symptomatology-Self-Report (QIDS-SR) and the Patient Health Questionnaire (PHQ-9) in depressed inpatients in China. Psychiatry Res. 2016;243:92-96. PubMed doi:10.1016/j.psychres.2016.06.021
10. Greenberg PE, Fournier AA, Sisitsky T, et al. The economic burden of adults with major depressive disorder in the United States (2005 and 2010). J Clin Psychiatry. 2015;76(2):155-162. PubMed doi:10.4088/JCP.14m09298
11. Mccubbin T, Dimidjian S, Kempe K, et al. Mindfulness-based stress reduction in an integrated care delivery system: one-year impacts on patient-centered outcomes and health care utilization. Perm J. 2014;18(4):4-9. PubMed doi:10.7812/TPP/14-014
12. Allen JG, Fonagy P, Bateman AW. Mentalizing in Clinical Practice. Washington, DC: American Psychiatric Publishing, Inc; 2008.
13. Luders E, Toga AW, Lepore N, et al. The underlying anatomical correlates of long-term meditation: larger hippocampal and frontal volumes of gray matter. Neuroimage. 2009;45(3):672-678. PubMed doi:10.1016/j.neuroimage.2008.12.061
14. Johnson DC, Thom NJ, Stanley EA, et al. Modifying resilience mechanisms in at-risk individuals: a controlled study of mindfulness training in Marines preparing for deployment. Am J Psychiatry. 2014;171(8):844-853. PubMed doi:10.1176/appi.ajp.2014.13040502
15. Baron Short E, Kose S, Mu Q, et al. Regional brain activation during meditation shows time and practice effects: an exploratory FMRI study. Evid Based Complement Alternat Med. 2010;7(1):121-127. PubMed doi:10.1093/ecam/nem163
16. Lazar SW, Kerr CE, Wasserman RH, et al. Meditation experience is associated with increased cortical thickness. Neuroreport. 2005;16(17):1893-1897. PubMed doi:10.1097/01.wnr.0000186598.66243.19
17. Jang JH, Jung WH, Kang DH, et al. Increased default mode network connectivity associated with meditation. Neurosci Lett. 2011;487(3):358-362. PubMed doi:10.1016/j.neulet.2010.10.056
18. Aftanas LI, Golocheikine SA. Human anterior and frontal midline theta and lower alpha reflect emotionally positive state and internalized attention: high-resolution EEG investigation of meditation. Neurosci Lett. 2001;310(1):57-60. PubMed doi:10.1016/S0304-3940(01)02094-8
19. Pagnoni G, Cekic M. Age effects on gray matter volume and attentional performance in Zen meditation. Neurobiol Aging. 2007;28(10):1623-1627. PubMed doi:10.1016/j.neurobiolaging.2007.06.008
Enjoy this premium PDF as part of your membership benefits!