Prediction of Trauma-Related Disorders: A Proposed Cutoff Score for the Peritraumatic Distress Inventory
In the month following a motor vehicle accident, the rate of posttraumatic stress disorder (PTSD) and other trauma-related disorders (ie, mood, other anxiety disorders, and substance use disorders) may reach 30%.1 From a clinical perspective, there is an unmet need to develop screening tools that can help identify individuals at risk of developing such disorders. The Peritraumatic Distress Inventory (PDI) is a 13-item self-report measure—validated in several languages—that has been shown in several studies to predict the development of posttraumatic stress symptoms or disorder.2-4 In a prospective study of 79 motor vehicle accident victims, Nishi et al5 proposed an optimum cutoff point of 23 for the PDI to predict acute PTSD 1 month after the accident. However, to this day, the measure has not been used to predict the full spectrum of trauma-related disorders. The aim of this study was to fill that gap.
Method. The study, approved by an independent ethics committee, included 211 subjects consecutively hospitalized in a Trauma Center following a motor vehicle accident from January 2003 to July 2006. The PDI was administered within 5 days of admission after written informed consent was obtained. Six weeks after the accident, the patients underwent a semistructured PTSD diagnostic interview6 as well as the Mood, Anxiety, and Substance Use Disorders sections of a structured psychiatric interview7 by trained psychiatrists. Partial PTSD as described by Blanchard et al8 was also screened for. Subjects with a history of posttraumatic amnesia were excluded. Nineteen subjects were lost at the 6-week follow-up and therefore dropped from the analyses.
Results. The final cohort consisted of 192 subjects, 137 adult men and 55 women. The mean age of subjects was 35.14 years (SD = 15.39). Injury severity was classified as mild (10%), moderate (49%), or severe (41%). In the final cohort, 154 subjects fulfilled DSM-IV-TR criteria A1 and A2 for trauma exposure. The mean PDI total score was 15.68 (SD = 8.71). At the follow-up, 66 patients fulfilled criteria for partial (n = 31) or full (n = 35) PTSD, 19 for major depressive disorder, 10 for at least 1 anxiety disorder, and 3 for a psychoactive substance disorder. No association was found between injury severity and PTSD (χ2 = 0.96, df = 1, NS). The PDI score was, however, significantly associated with an increased risk of acute PTSD (χ2 = 5.15, df = 1, P = .02).
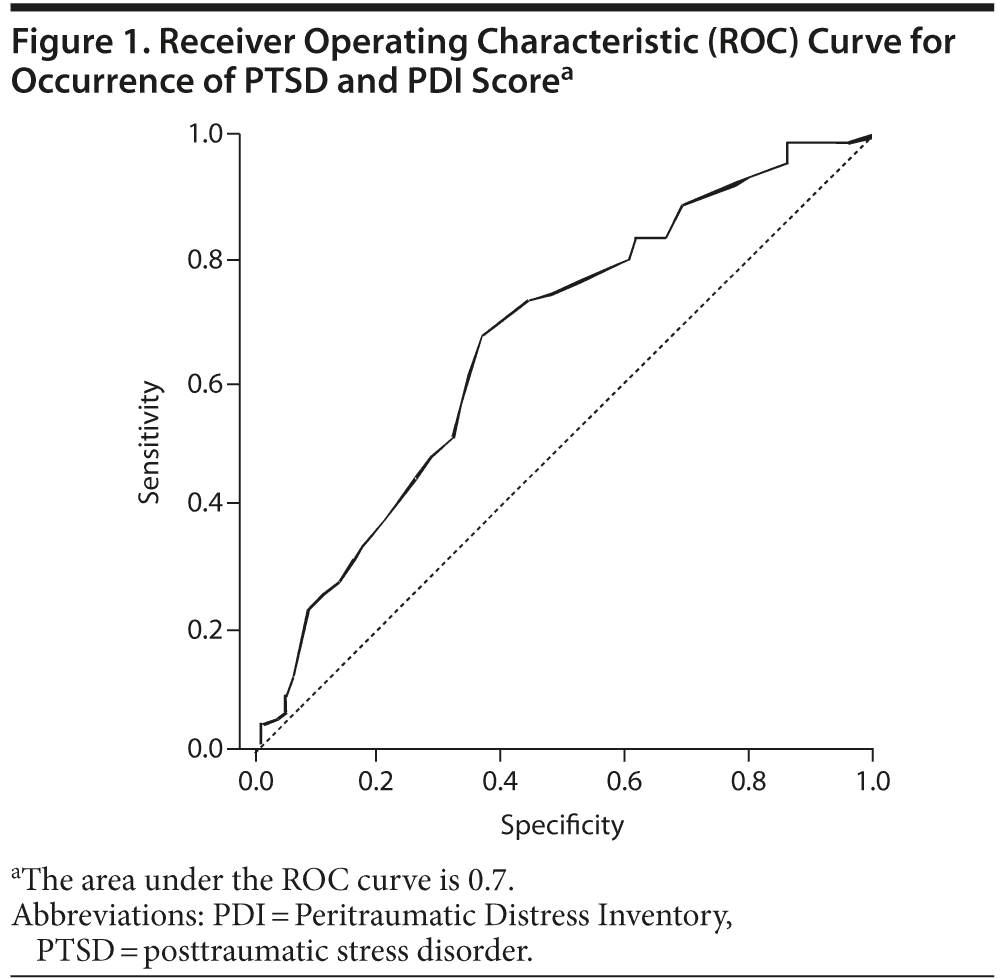
According to the occurrence of traumatic events, receiver operating characteristic curve analysis showed an area under the curve (AUC) of 0.7 (Figure 1). The optimum predictive cutoff point of the PDI was a score of 14 (sensitivity 68%, specificity 61%). On the one hand, 90% of the victims with a PDI score > 28 developed PTSD or partial PTSD at follow-up. On the other hand, 90% of those with a score < 7 did not develop PTSD. In order to detect PTSD or partial PTSD 6 weeks later, we propose a cutoff score of 14 (PTSD: sensitivity 84% and specificity 47%, AUC 0.6; partial PTSD: sensitivity 73% and specificity 60%, AUC 0.7).
The PDI could be a useful tool for screening individuals at risk of developing trauma-related disorders. We recommend that trauma survivors with a PDI score < 7 do not require monitoring. Those with a PDI total score > 28 would need immediate care and follow-up. Finally, for those with a score of 7 through 28, we propose a checkup after a few weeks.
References
1. Shalev AY, Freedman S, Peri T, et al. Prospective study of posttraumatic stress disorder and depression following trauma. Am J Psychiatry. 1998;155(5):630-637. PubMed
2. Brunet A, Weiss DS, Metzler TJ, et al. The Peritraumatic Distress Inventory: a proposed measure of PTSD criterion A2. Am J Psychiatry. 2001;158(9):1480-1485. PubMed doi:10.1176/appi.ajp.158.9.1480
3. Jehel L, Brunet A, Paterniti S, et al. [Validation of the Peritraumatic Distress Inventory’s French translation]. Can J Psychiatry. 2005;50(1):67-71. PubMed
4. Nishi D, Matsuoka Y, Noguchi H, et al. Reliability and validity of the Japanese version of the Peritraumatic Distress Inventory. Gen Hosp Psychiatry. 2009;31(1):75-79. PubMed doi:10.1016/j.genhosppsych.2008.09.002
5. Nishi D, Matsuoka Y, Yonemoto N, et al. Peritraumatic Distress Inventory as a predictor of post-traumatic stress disorder after a severe motor vehicle accident. Psychiatry Clin Neurosci. 2010;64(2):149-156. PubMed doi:10.1111/j.1440-1819.2010.02065.x
6. Blake DD, Weathers FW, Nagy LM, et al. The development of a Clinician-Administered PTSD Scale. J Trauma Stress. 1995;8(1):75-90. PubMed doi:10.1002/jts.2490080106
7. Sheehan DV, Lecrubier Y, Sheehan KH, et al. The Mini-International Neuropsychiatric Interview (M.I.N.I.): the development and validation of a structured diagnostic psychiatric interview for DSM-IV and ICD-10. J Clin Psychiatry. 1998;59(suppl 20):22-33, quiz 34-57. PubMed
8. Blanchard EB, Hickling EJ, Taylor AE, et al. Psychological morbidity associated with motor vehicle accidents. Behav Res Ther. 1994;32(3):283-290. PubMed doi:10.1016/0005-7967(94)90123-6
Author affiliations: Centre Hospitalier Régional Universitaire de Lille (Drs Guardia, Ducrocq, and Vaiva); Université du Droit et de la Santé de Lille, EA4559 (Drs Guardia and Vaiva) and EA2694 (Dr Duhamel); and Centres d’ investigation Cliniques (Dr Demarty), Lille, France; and Douglas Mental Health University Institute and McGill University, Montreal, Quebec, Canada (Dr Brunet).
Potential conflicts of interest: Dr Brunet holds a salary award from the Fonds de recherche en santé du Québec. Dr Vaiva has been on the speakers or advisory boards for Janssen, Lundbeck, Bristol-Myers Squibb, and Servier. Drs Guardia, Duhamel, Ducrocq, and Demarty report no potential conflict of interest relevant to the subject of this letter.
Funding/support: None reported.
Published online: January 10, 2013.
Prim Care Companion CNS Disord 2013;15(1):doi:10.4088/PCC.12l01406
© Copyright 2013 Physicians Postgraduate Press, Inc.