Background: The Diagnostic and Statistical Manual of Mental Disorders, Fourth Edition (DSM-IV), is a categorical system that provides descriptive diagnostic criteria for psychiatric syndromes. These syndrome descriptions are imperfect representations of an underlying behavioral, psychological, or biological dysfunction; thus, the criteria could be conceptualized as a type of test for the etiologically defined illnesses. Accordingly, as with any other diagnostic test, diagnoses based on DSM-IV criteria produce some false positive and some false negative results. That is, some patients who meet the criteria will not have the illness (ie, false positives), and some who do not meet the criteria because their symptoms fall below the diagnostic threshold will have the illness and incorrectly not receive the diagnosis (ie, false negatives). In this context, I consider the controversy over whether the diagnostic threshold for bipolar disorder should be lowered.
Method: Longitudinal studies of the prognostic significance of subthreshold bipolar disorder are considered.
Results: Subthreshold bipolarity is a risk factor for the future emergence of bipolar disorder, but the majority of individuals with subthreshold bipolarity do not develop a future manic or hypomanic episode.
Conclusions: The diagnostic threshold for bipolar disorder should not be lowered for 4 reasons: (1) the results of longitudinal studies suggest that lowering the diagnostic threshold for bipolar disorder will result in a greater increase in false positive than true positive diagnoses; (2) there are no controlled studies demonstrating the efficacy of mood stabilizers in treating subthreshold bipolar disorder; (3) if a false negative diagnosis occurs and bipolar disorder is underdiagnosed, diagnosis and treatment can be changed when a manic/hypomanic episode emerges; and (4) if bipolar disorder is overdiagnosed and patients are inappropriately prescribed a mood stabilizer, the absence of a future manic/hypomanic episode would incorrectly be considered evidence of the efficacy of treatment, and the unnecessary medications that might cause medically significant side effects would not be discontinued.
J Clin Psychiatry 2012;Â 73(4): 437-443
© Copyright 2012 Physicians Postgraduate Press, Inc.
Would Broadening the Diagnostic Criteria for Bipolar Disorder Do More Harm Than Good? Implications From Longitudinal Studies of Subthreshold Conditions
ABSTRACT
Background: The Diagnostic and Statistical Manual of Mental Disorders, Fourth Edition (DSM-IV), is a categorical system that provides descriptive diagnostic criteria for psychiatric syndromes. These syndrome descriptions are imperfect representations of an underlying behavioral, psychological, or biological dysfunction; thus, the criteria could be conceptualized as a type of test for the etiologically defined illnesses. Accordingly, as with any other diagnostic test, diagnoses based on DSM-IV criteria produce some false positive and some false negative results. That is, some patients who meet the criteria will not have the illness (ie, false positives), and some who do not meet the criteria because their symptoms fall below the diagnostic threshold will have the illness and incorrectly not receive the diagnosis (ie, false negatives). In this context, I consider the controversy over whether the diagnostic threshold for bipolar disorder should be lowered.
Method: Longitudinal studies of the prognostic significance of subthreshold bipolar disorder are considered.
Results: Subthreshold bipolarity is a risk factor for the future emergence of bipolar disorder, but the majority of individuals with subthreshold bipolarity do not develop a future manic or hypomanic episode.
Conclusions: The diagnostic threshold for bipolar disorder should not be lowered for 4 reasons: (1) the results of longitudinal studies suggest that lowering the diagnostic threshold for bipolar disorder will result in a greater increase in false positive than true positive diagnoses; (2) there are no controlled studies demonstrating the efficacy of mood stabilizers in treating subthreshold bipolar disorder; (3) if a false negative diagnosis occurs and bipolar disorder is underdiagnosed, diagnosis and treatment can be changed when a manic/hypomanic episode emerges; and (4) if bipolar disorder is overdiagnosed and patients are inappropriately prescribed a mood stabilizer, the absence of a future manic/hypomanic episode would incorrectly be considered evidence of the efficacy of treatment, and the unnecessary medications that might cause medically significant side effects would not be discontinued.
J Clin Psychiatry 2012;73(4):437–443
© Copyright 2012 Physicians Postgraduate Press, Inc.
See Commentary on page 443.
Submitted: July 22, 2011; accepted November 8, 2011 (doi:10.4088/JCP.11com07288).
Corresponding author: Mark Zimmerman, MD, Bayside Medical Center, 235 Plain St, Providence, RI 02905 ([email protected]).
Bipolar disorder, like most disorders defined in the Diagnostic and Statistical Manual of Mental Disorders, Fourth Edition (DSM-IV), is a symptom-based diagnosis. A biological test for bipolar disorder does not yet exist. The absence of a diagnostic test means that the DSM-IV diagnostic criteria for bipolar disorder represent a probabilistic estimate of the presence of a disease whose underlying pathophysiology we hope to one day understand and identify with a valid test.
Controversy exists regarding the diagnostic boundary for bipolar disorder. Critics of the existing DSM-IV criteria note that the choice of the minimum number of features and minimum duration used to define a manic or hypomanic episode are arbitrary, not based on empirical study, and overly narrow.1,2 It has been suggested that the current DSM-IV symptom and duration thresholds should be lowered to include individuals with bipolar disorder who are currently excluded from the diagnosis.1–7 In support of this recommendation, both clinical and general population epidemiologic studies have found that individuals with subthreshold levels of bipolar pathology (ie, fewer than the DSM-IV–required number of symptoms or briefer than the DSM-IV-required number of days) differed from depressed subjects without subthreshold levels of bipolar symptoms in comorbidity, personality, family history, and longitudinal course.8–11 More research has examined lowering the duration than the symptom number threshold, and the DSM-5 Mood Disorders Work Group is considering expanding the definition of bipolar disorder by reducing the duration required to define a hypomanic episode.12 Expansion of the definition of bipolar disorder by lowering the minimum number of symptoms required for a diagnosis of mania or hypomania is apparently not under consideration.12
In the present commentary, I consider the possible risks and benefits of expanding the diagnostic criteria for bipolar disorder. While most of the literature on expanding the bipolar definition has examined the impact of reducing the duration threshold, the ensuing discussion applies to expanding the definition by lowering either the duration or symptom count threshold. I begin by discussing the problem of diagnosis based on reports of past episodes and how, despite the best efforts of clinicians and researchers, diagnostic clarity may remain elusive. Then I suggest that, rather than considering the DSM-IV symptom criteria for bipolar disorder as definitive, they should be considered as a test for the undiscovered underlying etiologically defined illness. From this perspective, diagnoses based on the symptom criteria are associated with some false positive and some false negative results, and changing the diagnostic threshold simply changes the relative rate of each of these errors. In light of this conceptualization of the diagnostic criteria for bipolar disorder, I consider recent studies of the prognostic significance of “subthreshold” bipolar disorder for predicting future “threshold” episodes of mania or hypomania. Finally, I consider studies of the treatment of subthreshold bipolar disorder and discuss the process of treatment decision-making while following patients longitudinally.
DETECTING PAST EPISODES OF HYPOMANIA
IN DEPRESSED PATIENTS AND THE ELUSIVENESS
OF DIAGNOSTIC CERTAINTY
The underrecognition of bipolar disorder in patients presenting for the treatment of depression has been identified as a significant clinical problem.13–22 For patients diagnosed with bipolar disorder, the lag between initial treatment-seeking and the correct diagnosis is often more than 10 years.23,24 The treatment and clinical implications of the failure to recognize bipolar disorder in depressed patients include the underprescription of mood stabilizing medications, an increased risk of rapid cycling, and increased costs of care.16,25–27
When diagnosis is based on the presence of symptom episodes that occurred in the past, as is the case with bipolar disorder in currently depressed patients, diagnostic clarity is sometimes elusive. Wherever the boundary of bipolar disorder is drawn, there will be some false negative as well as false positive diagnoses. Some patients diagnosed with major depressive disorder will turn out to have bipolar disorder when they manifest a hypomanic or manic episode during prospective follow-up. For some patients, this will be the initial emergence of manic/hypomanic symptomatology, whereas for others it will represent the latest in a number of episodes, and only then will it have become apparent that a prior history of hypomanic or manic episodes had not been identified. A number of studies have found that the rate of missed diagnoses of bipolar disorder is fairly high, especially when a broader definition of hypomania is used than the one specified in DSM-IV.15,16,21,28–30
As a clinician, it is often the case that early in the course of treatment I am not sure if a currently depressed patient has bipolar disorder. This uncertainty occurs despite an extensive evaluation that includes the administration of a semistructured interview, a review of prior records, and an interview with an informant. Did the 42-year-old depressed businessman previously experience a hypomanic episode when his mood was elevated at the initiation of a new venture during which time he slept only 2 to 3 hours and did not feel tired (described as an “unthrottled expenditure of energy”), reportedly worked 16 to 18 hours per day, felt much more confident than usual, asserted that his creativity and clarity of thought were enhanced, and described his thoughts as going much faster than usual? He reported 2 such episodes of a few months’ duration, each time coinciding with a new business initiative and associated with enhanced productivity. Both episodes were followed by periods of major depression. While the reports of these episodes met DSM-IV criteria for hypomania, and I made a diagnosis of bipolar II disorder, it was unclear to me if these symptoms represented a hypomanic phenocopy in a driven, successful businessman or true bipolar illness. Because of the implications of possible lifetime treatment if this were considered bipolar illness, we agreed to treat his condition as nonbipolar depression. In the decade since the initial evaluation, he has not had another hypomanic (or subthreshold hypomanic) episode and has been in remission for the past 7 years since he was started on a dual reuptake inhibitor. I have seen a number of other patients who describe what sounds like 1 or 2 hypomanic episodes at the initial evaluation but, when followed longitudinally, never experienced a recurrence despite being treated only with antidepressant medication. What is the valid diagnosis in these patients?
CONCEPTUALIZING DSM CRITERIA
AS A DIAGNOSTIC TEST
The Diagnostic and Statistical Manual of Mental Disorders, Fourth Edition, is a categorical system that provides descriptive diagnostic criteria of psychiatric syndromes. The definition of mental disorder in DSM-IV notes that these syndrome descriptions represent underlying behavioral, psychological, or biological dysfunction, albeit imperfect representations of the potentially unknown, underlying core dysfunction. This definition suggests that the descriptive diagnostic criteria should not be reified and considered the last word on whether a patient has the illness in question, but instead the criteria should be conceptualized as a type of test for the underlying, etiologically defined illness. Accordingly, as with any other diagnostic test, diagnoses based on the DSM-IV criteria produce some false positive and some false negative results (Figure 1). That is, some patients who meet the DSM-IV diagnostic criteria will not have the illness (ie, false positives), and some who do not meet the criteria because their symptoms fall below the DSM-IV diagnostic threshold will have the illness and incorrectly not receive the diagnosis (ie, false negatives). According to this conceptualization, the gold-standard to which DSM-IV diagnoses are being compared is a not-yet-discovered index of illness such as a biomarker.
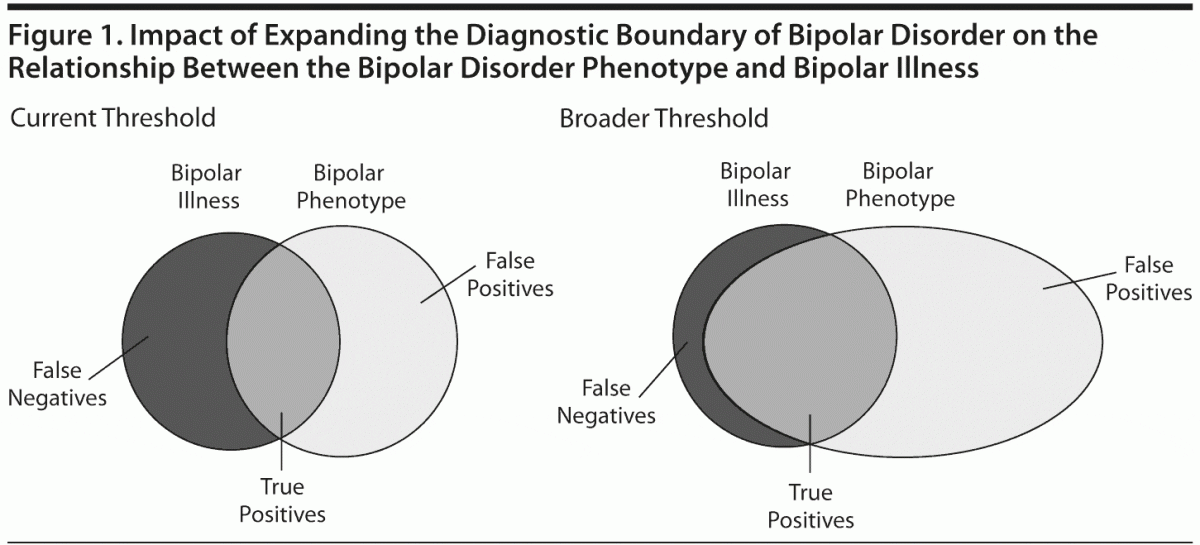
The lack of congruence between phenomenological diagnosis and underlying pathophysiology is only one cause of diagnostic error. A second cause of diagnostic error is related to assessment methodology. There are limits to the accuracy of retrospective recall of prior hypomanic and manic episodes. Despite appropriate inquiry, patients might not recall or report prior episodes, thus resulting in false negative diagnoses. Or false negative diagnoses could result from the failure to make inquiry or the failure to make appropriate inquiry.31–33 False positive diagnoses may also be a problem. It is sometimes difficult to determine if prior hypomanic/manic episodes occurred independent of substance use, thereby resulting in false positive diagnoses.34,35 Transient episodes of affective instability and emotional lability associated with borderline personality disorder might be confused with hypomanic episodes, thereby resulting in false positive diagnoses.36,37 This is not to suggest that affective instability is pathognomonic for borderline personality disorder but rather to illustrate how phenomenological similarities might result in diagnostic error. In fact, recent research has suggested differences in the type of affective instability experienced by patients with bipolar disorder and borderline personality disorder.38
In sum, wherever the lower boundary of bipolar disorder is drawn, diagnostic error is inherent in a system in which diagnoses are based on retrospective recall of symptom episodes.
The question is not whether diagnostic error exists, but rather which type of error predominates, and how much will shifting the diagnostic threshold impact the number of each of these diagnostic errors. Also important to consider are the clinical consequences of each type of error, and which error is more difficult to undo after it has been made.
THE UNCERTAIN IMPACT OF LOWERING THE DIAGNOSTIC THRESHOLD FOR BIPOLAR DISORDER
Supporting the recommendation to lower the diagnostic boundary, some studies have found that individuals with subthreshold levels of bipolar pathology differed from depressed subjects without subthreshold levels of bipolar symptoms in comorbidity, personality, family history, and longitudinal course.8–11,39 However, no studies have examined the potential impact this change would have on diagnosis and outcome in real-world clinical practice. With the existing DSM-IV diagnostic criteria, which require a minimum 4-day duration for hypomania, overdiagnosis (ie, false positives) is already a problem.40 If the duration diagnostic threshold is lowered, how many more patients will be overdiagnosed with bipolar disorder because the brief periods of affective instability, behavioral impulsivity, or irritability and anger characteristic of cluster B personality pathology will be incorrectly considered indicative of hypomania?36 The frequency of overdiagnosis due to lowering the diagnostic threshold must be contrasted against the frequency of underdiagnosing “true” bipolar disorder because the observed or recently occurring hypomanic syndrome did not last long enough to qualify as a DSM-IV hypomanic episode. While underdiagnosis due to insufficient duration is a possibility, there is evidence that clinicians are not rigid in the application of the DSM-IV diagnostic thresholds.41 Thus, it is likely that patients who manifest recurrent hypomanic episodes of presumably insufficient duration during the course of treatment will be diagnosed with bipolar disorder and treated accordingly.
Both false positive and false negative diagnoses are associated with adverse consequences. Unrecognized bipolar disorder is associated with underprescription of mood stabilizing medications, an increased risk of rapid cycling, and increased costs of care.16,25,27 Overdiagnosed bipolar disorder is associated with overtreatment with unneeded medications and consequent exposure to potential side effects and medical risk as well as the potential failure to offer more appropriate treatments. In trying to decide where to set the threshold for diagnosing bipolar disorder and minimize diagnostic errors of all types, another question is whether one type of diagnostic error is likely to be more long-lasting and difficult to undo than another.
Diagnosis is a dynamic, fluid process that is (hopefully) reconsidered as additional clinical material becomes available. However, when diagnosis is based, in part, on the presence of past episodes, it is more difficult to take away the diagnosis once it has been established than to add the diagnosis once an episode occurs. Once a depressed patient is diagnosed with bipolar disorder, the reoccurrence of a hypomanic or manic episode is not necessary to retain the diagnosis. In fact, the lack of recurrence could be viewed as treatment success. The patient with a false positive diagnosis of bipolar disorder who is doing well on an antidepressant and a mood stabilizer is unlikely to have the mood stabilizer discontinued or the diagnosis corrected. On the other hand, a patient with a false negative diagnosis is more likely to have it changed from major depressive disorder to bipolar disorder on the emergence of a hypomanic or manic episode. Thus, a false negative diagnosis of nonbipolar depression is easier to correct than a false positive diagnosis of bipolar disorder. Lowering the diagnostic boundary for bipolar disorder may or may not reduce the overall number of diagnostic errors. However, the error due to false positive diagnoses, which will increase when the diagnostic boundary is broadened, will be more likely to persist than the error due to false negative diagnoses.
THE PROGNOSTIC SIGNIFICANCE OF SUBTHRESHOLD BIPOLARITY
Up to this point, the discussion of where to set the diagnostic threshold has referred to an unknown prevalence of overall diagnostic error and an unknown relative frequency of false positive and false negative diagnoses. Strong evidence supporting the expansion of bipolar disorder’s diagnostic boundary would come from prospective follow-up studies demonstrating that individuals with subthreshold bipolarity are at high risk for developing bipolar disorder (as currently defined). If the majority of individuals with subthreshold bipolar disorder develop manic or hypomanic episodes during prospective follow-up, this would indicate that the higher threshold results in more false negative than false positive diagnoses. Recently, 4 prospective follow-up studies have examined the prognostic significance of subthreshold bipolarity (Table 1). These studies differed in their definition of subthreshold bipolarity, with some defining it according to a lower duration threshold, some defining it according to a lower symptom count threshold, and some defining it according to the lowering of both thresholds.
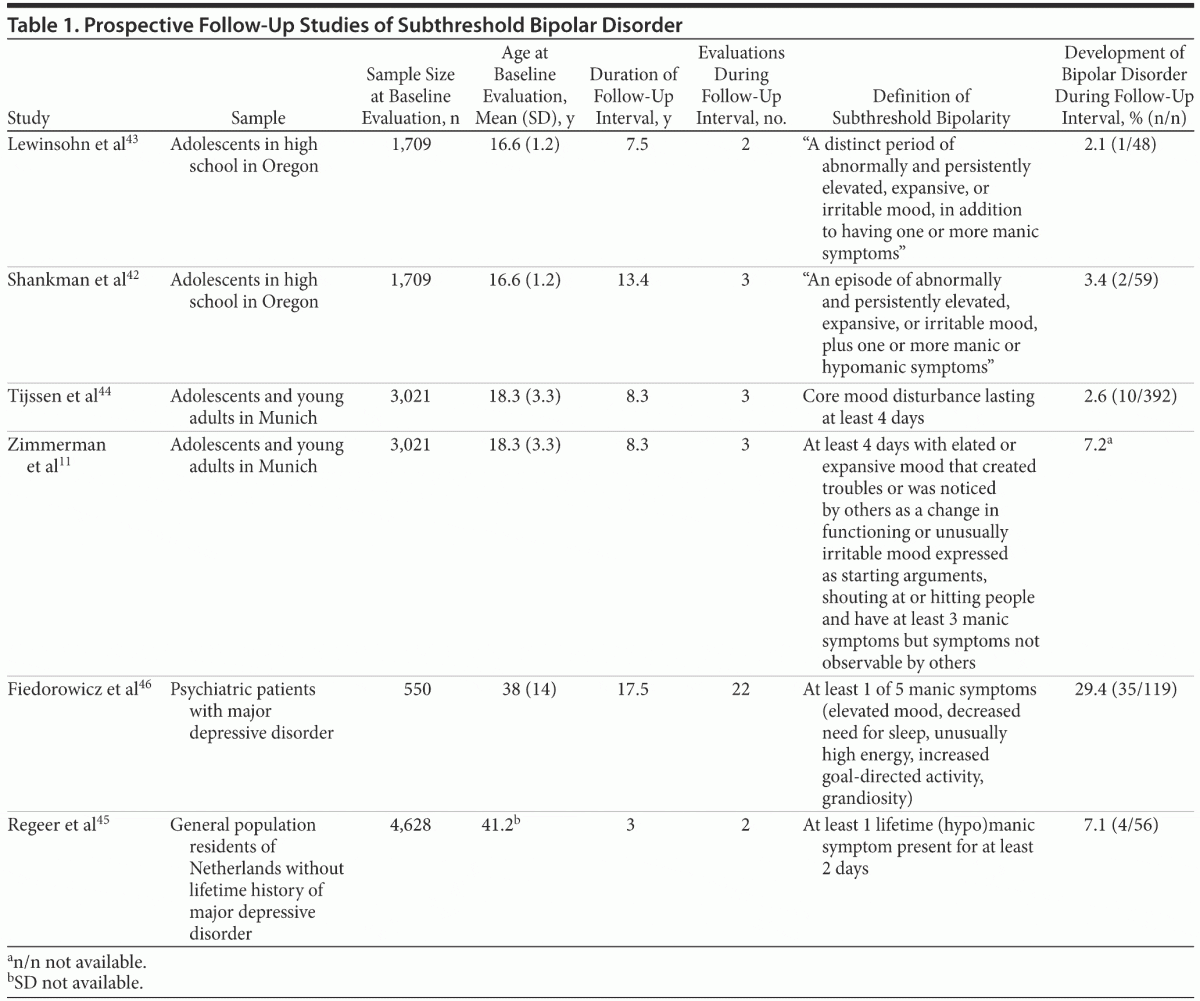
In the Oregon Adolescent Depression Project (OADP), 1,709 randomly selected high school students were followed for up to 15 years.42 Follow-up interviews were conducted approximately 1, 10, and 15 years after the initial evaluation. Subthreshold bipolarity was defined as “an episode of abnormally and persistently elevated, expansive, or irritable mood, plus one or more manic or hypomanic symptoms.” The authors did not define “persistent”; thus, it is not clear if the bipolar threshold was expanded according to symptom count and episode duration or just symptom count. Two reports from the OADP have described the frequency of bipolar disorder in individuals with subthreshold bipolar symptoms at the initial evaluation. The first report, by Lewinsohn et al,43 described the findings from the 10-year follow-up, and the second report, by Shankman et al,42 described the findings from the 15-year follow-up. The results were nearly identical. The mean age of subjects was 16.6 years at the baseline interview and 30.4 years at the final follow-up evaluation. After 15 years, 3.4% of the 59 subjects who described a history of subthreshold bipolar symptoms at the baseline interview developed bipolar disorder. Only 2 of 18 subjects who developed bipolar disorder during the follow-up period had subthreshold bipolarity at baseline; thus, the sensitivity of subthreshold bipolarity for predicting bipolar disorder was 11.1%. Subthreshold bipolar symptoms were not associated with a significantly increased risk of developing bipolar disorder during the follow-up.
The Early Developmental Stages of Psychopathology (EDSP) study has completed a 10-year prospective study of teenage and young adult community residents of Munich, Germany.11,44 The mean age of the subjects at the baseline evaluation was 18.8 years. Subjects were evaluated at 3 time points: 1.6, 3.4, and 8.3 years after the baseline evaluation. Two reports from the EDSP described the transition from subthreshold to diagnostic status in overlapping, albeit different, samples. Tijssen et al44 focused on the 1,565 subjects who were interviewed at baseline and the second and third follow-up evaluations and who, before the last follow-up evaluation, had not been diagnosed with bipolar disorder or used mental health services. The report by Zimmerman et al11 was more inclusive and focused on all 2,210 respondents who completed the third follow-up interview. Subthreshold bipolarity required “at least 4 days with elated or expansive mood that created trouble or was noticed by others as a change in functioning or unusually irritable mood expressed as starting arguments, shouting at or hitting people and have at least 3 manic symptoms but symptoms not observable by others.” Thus, the authors examined the impact of lowering the symptom count threshold. Zimmerman et al11 found that 7.2% of the subjects with subthreshold bipolar symptoms converted to bipolar disorder, significantly higher than the 1.7% rate in subjects with major depressive disorder. The highest rate of conversion to bipolar disorder was in subjects with subthreshold bipolar symptoms causing a change in functioning observable to others (13.2%).
A third general population study examining the prognostic significance of subthreshold bipolar symptoms is the Netherlands Mental Health Survey and Incidence Study (NEMESIS).45 Hypomanic symptoms lasting for at least 2 days were counted as present, and subthreshold bipolarity included the presence of at least 1 hypomanic symptom. The analysis was based on the 4,628 subjects who had not been diagnosed with bipolar disorder or major depressive disorder at baseline. Follow-up evaluations were conducted 1 and 3 years after the baseline interview. Subjects’ mean age at baseline was 41.2 years. The risk of developing bipolar disorder during follow-up was significantly higher in the subjects with a history of subthreshold bipolar symptoms than subjects without subthreshold bipolar symptoms (7.1% vs 0.2%). The sensitivity of subthreshold bipolarity for future bipolar disorder was 28.6%, and specificity was 98.9%.
Finally, 1 study examined the risk of developing bipolar disorder in depressed patients with subthreshold symptoms.46 In the Collaborative Depression Study (CDS), 450 patients with major depressive disorder were followed a mean of 17.5 years. The follow-up was intensive, occurring every 6 months during the first 5 years of the CDS and yearly thereafter. At baseline, the presence of 5 manic/hypomanic symptoms was rated (elevated mood, decreased need for sleep, unusually high energy, increased goal-directed activity, grandiosity) on a 6-point Likert scale of severity (range, 0–5). Because of the low frequency of symptoms of clinically significant severity, the authors adopted a low threshold and included a rating of 1 as indicative of a subthreshold manic/hypomanic symptom. The minimum duration of symptom presence was not specified. Compared to patients with no subthreshold hypomanic symptoms, significantly more patients with at least 1 subthreshold hypomanic symptom developed bipolar disorder during the follow-up (29.4% vs 16.9%). The results of a receiver operating curve analysis indicated that the optimal cutoff for predicting bipolar disorder was ≥ 3 symptoms. Patients with 3 or more manic symptoms had a 42% likelihood of developing bipolar disorder during the long-term follow-up (versus 18% of the patients who had 2 or fewer manic symptoms). Based on this cutoff, the sensitivity and specificity of subthreshold bipolarity for detecting bipolar disorder were 16% and 95%, respectively.
These longitudinal studies indicate that subthreshold bipolarity is a risk factor for the future emergence of bipolar disorder. In the community-based epidemiologic samples, the conversion rate was low. In terms of diagnostic efficiency statistics, the sensitivity and positive predictive value of subthreshold bipolarity were low, whereas the specificity and negative predictive value of the absence of subthreshold bipolarity were high. However, clinicians are most interested in the clinical significance of subthreshold bipolarity in depressed patients presenting for treatment. In the CDS, the majority of patients with subthreshold bipolarity did not develop bipolar disorder during nearly 20 years of intensively monitored follow-up. Fiedorowicz et al46 concluded that the presence of subclinical hypomanic symptoms did not warrant a change in diagnosis. Rather, in light of the modest positive predictive value of subthreshold manic/hypomanic symptoms, the authors recommended careful monitoring of depressed patients during ongoing treatment to detect the emergence of manic or hypomanic episodes.
TREATMENT OF DEPRESSED PATIENTS WITH SUBTHRESHOLD BIPOLAR SYMPTOMS
Perhaps the strongest evidence in support of expanding the DSM-IV definition of bipolar disorder would be the demonstration of the efficacy of mood stabilizers. To be sure, considering response to treatment as a diagnostic validator is not universally accepted. The approach toward diagnostic validity articulated by Robins and Guze47 more than 40 years ago did not include treatment response as one of the 5 phases of establishing validity. More recently, other researchers have included treatment response as an indicator of validity.48 It is beyond the scope of the present article to debate whether treatment response should be considered in establishing diagnostic validity. Regardless of whether treatment response is considered from the perspective of validity or clinical practice, it is noteworthy that supporters of expanding the concept of bipolar disorder to include milder variants indicate that the accurate identification of subthreshold forms of bipolar disorder is clinically important because of the treatment implications.1,3,4,6,8,18 Yet the literature reviews advocating the expansion of the diagnostic boundary have not identified a single controlled study of the efficacy of mood stabilizers in the treatment of subthreshold bipolar disorder.1,3–7 Some authors have questioned the validity of extrapolating the evidence of the efficacy of mood stabilizers in the treatment of bipolar I disorder to subthreshold bipolarity.49,50 Consideration of the above summary of the prognostic significance of subthreshold bipolarity suggests a risk of overprescribing, insofar as the majority of individuals with milder variants would never develop DSM-IV–defined bipolar disorder. Individuals with subthreshold bipolarity would therefore be prescribed such medications in the absence of controlled research establishing their efficacy.
CONCLUSIONS
First and Frances51 cautioned the developers of DSM-5 against making changes in diagnostic criteria without sufficient consideration of the unforeseen consequences of such changes. If we accept the proposition that the DSM-IV criteria are imperfect in identifying bipolar illness and conceptualize these criteria as a type of test for bipolar illness that produces some false positives and some false negatives, then shifting the diagnostic boundary downward will, to be sure, reduce the rate of underdiagnosis of true bipolar disorder (ie, reduce false negatives). However, the cost of making fewer false negative diagnoses will be an increased rate of overdiagnosing pseudobipolar disorder (ie, increase false positives).
It is important to recognize the important gaps in our current knowledge in order to determine the diagnostic significance of manic/hypomanic symptoms that do not meet the current diagnostic thresholds. In the absence of valid tests for the underlying behavioral, psychological, and biological dysfunction, the relative frequency of each type of phenomenology-based diagnostic error (ie, false positives and false negatives) is unknown. The efficacy of mood stabilizers in treating subthreshold bipolar disorder is unknown. The impact of lowering the threshold to diagnose bipolar disorder on overdiagnosing bipolar in clinical practice is unknown. The number of patients who would develop iatrogenic complications from medications that were prescribed unnecessarily is unknown. The number of patients whose bipolar disorder was not recognized at the initial evaluation but was subsequently recognized during the course of treatment is unknown. From a public health perspective, the benefit of expanding the diagnostic boundary is unknown. In the face of such critically important knowledge gaps, and in consideration of the inherent imperfect reliability and validity of diagnoses based on the retrospective application of symptom criteria, the opportunity for clinicians to change diagnosis on the emergence of a hypomanic or manic episode during the course of treatment, the low likelihood that individuals with subthreshold bipolarity will experience threshold episodes during prospective follow-up, the lack of a single controlled study demonstrating the efficacy of mood stabilizers in the treatment of subthreshold bipolarity, and the possible medically significant side effects associated with mood stabilizers, it is concluded that the risk from the potential unforeseen consequences of lowering the diagnostic threshold is too great to change bipolar disorder’s diagnostic boundary in DSM-5.
Author affiliations: The Department of Psychiatry and Human Behavior, Brown Medical School, and the Department of Psychiatry, Rhode Island Hospital, Providence.
Potential conflicts of interest: Dr Zimmerman reports no financial or other relationship relevant to the subject of the article.
Funding/support: None reported.
REFERENCES
1. Akiskal HS, Bourgeois ML, Angst J, et al. Re-evaluating the prevalence of and diagnostic composition within the broad clinical spectrum of bipolar disorders. J Affect Disord. 2000;59(suppl 1):S5–S30. doi:10.1016/S0165-0327(00)00203-2 PubMed
2. Angst J. The bipolar spectrum. Br J Psychiatry. 2007;190(3):189–191. doi:10.1192/bjp.bp.106.030957 PubMed
3. Angst J, Cassano G. The mood spectrum: improving the diagnosis
of bipolar disorder. Bipolar Disord. 2005;7(suppl 4):4–12. doi:10.1111/j.1399-5618.2005.00210.x PubMed
4. Dunner DL. Clinical consequences of under-recognized bipolar spectrum disorder. Bipolar Disord. 2003;5(6):456–463. doi:10.1046/j.1399-5618.2003.00073.x PubMed
5. Angst J, Gamma A. Prevalence of bipolar disorders: Traditional and novel approaches. Clin Appr Bipol Disord. 2002;1:10–14.
6. Möller HJ, Curtis VA. The bipolar spectrum: diagnostic and pharmacologic considerations. Expert Rev Neurother. 2004;4(suppl 2):
S3–S8. doi:10.1586/14737175.4.6.S3 PubMed
7. Phelps J, Angst J, Katzow J, et al. Validity and utility of bipolar spectrum models. Bipolar Disord. 2008;10(1, pt 2):179–193. doi:10.1111/j.1399-5618.2007.00562.x PubMed
8. Angst J, Cui L, Swendsen J, et al. Major depressive disorder with subthreshold bipolarity in the National Comorbidity Survey Replication. Am J Psychiatry. 2010;167(10):1194–1201. doi:10.1176/appi.ajp.2010.09071011 PubMed
9. Angst J, Gamma A, Benazzi F, et al. Toward a re-definition of subthreshold bipolarity: epidemiology and proposed criteria for bipolar-II, minor bipolar disorders and hypomania. J Affect Disord. 2003;73(1–2):133–146. doi:10.1016/S0165-0327(02)00322-1 PubMed
10. Joyce PR, Light KJ, Rowe SL, et al. Bipolar disorder not otherwise specified: comparison with bipolar disorder I/II and major depression. Aust N Z J Psychiatry. 2007;41(10):843–849. doi:10.1080/00048670701579058 PubMed
11. Zimmermann P, Brückl T, Nocon A, et al. Heterogeneity of DSM-IV major depressive disorder as a consequence of subthreshold bipolarity. Arch Gen Psychiatry. 2009;66(12):1341–1352. doi:10.1001/archgenpsychiatry.2009.158 PubMed
12. American Psychiatric Association. Proposed criteria for hypomanic episode. DSM-5 development. 2011 http://www.dsm5.org/ProposedRevisions/Pages/proposedrevision.aspx?rid=426#.
Accessed July 20, 2011.
13. Bowden CL. Strategies to reduce misdiagnosis of bipolar depression. Psychiatr Serv. 2001;52(1):51–55. doi:10.1176/appi.ps.52.1.51 PubMed
14. Katzow JJ, Hsu DJ, Ghaemi SN. The bipolar spectrum: a clinical perspective. Bipolar Disord. 2003;5(6):436–442. doi:10.1046/j.1399-5618.2003.00068.x PubMed
15. Manning JS, Haykal RF, Connor PD, et al. On the nature of depressive
and anxious states in a family practice setting: the high prevalence of bipolar II and related disorders in a cohort followed longitudinally.
Compr Psychiatry. 1997;38(2):102–108. doi:10.1016/S0010-440X(97)90089-4 PubMed
16. Ghaemi SN, Boiman EE, Goodwin FK. Diagnosing bipolar disorder and the effect of antidepressants: a naturalistic study. J Clin Psychiatry. 2000;
61(10):804–808, quiz 809. doi:10.4088/JCP.v61n1013 PubMed
17. Ghaemi SN, Ko JY, Goodwin FK. “Cade’s disease” and beyond: misdiagnosis, antidepressant use, and a proposed definition for bipolar spectrum disorder. Can J Psychiatry. 2002;47(2):125–134. PubMed
18. Hirschfeld RM. Bipolar spectrum disorder: improving its recognition and diagnosis. J Clin Psychiatry. 2001;62(suppl 14):5–9. PubMed
19. Hirschfeld RM, Vornik LA. Recognition and diagnosis of bipolar disorder. J Clin Psychiatry. 2004;65(suppl 15):5–9. PubMed
20. Yatham LN. Diagnosis and management of patients with bipolar II disorder. J Clin Psychiatry. 2005;66(suppl 1):13–17. PubMed
21. Hantouche EG, Akiskal HS, Lancrenon S, et al. Systematic clinical methodology for validating bipolar-II disorder: data in mid-stream
from a French national multi-site study (EPIDEP). J Affect Disord. 1998;50(2–3):163–173. doi:10.1016/S0165-0327(98)00112-8 PubMed
22. Perugi G, Akiskal HS, Lattanzi L, et al. The high prevalence of “soft” bipolar (II) features in atypical depression. Compr Psychiatry. 1998;
39(2):63–71. doi:10.1016/S0010-440X(98)90080-3 PubMed
23. Hirschfeld RM, Lewis L, Vornik LA. Perceptions and impact of bipolar disorder: how far have we really come? results of the national depressive and manic-depressive association 2000 survey of individuals with bipolar disorder. J Clin Psychiatry. 2003;64(2):161–174. doi:10.4088/JCP.v64n0209 PubMed
24. Lish JD, Dime-Meenan S, Whybrow PC, et al. The National Depressive and Manic-Depressive Association (DMDA) survey of bipolar members. J Affect Disord. 1994;31(4):281–294. doi:10.1016/0165-0327(94)90104-X PubMed
25. Birnbaum HG, Shi L, Dial E, et al. Economic consequences of not recognizing bipolar disorder patients: a cross-sectional descriptive analysis. J Clin Psychiatry. 2003;64(10):1201–1209. doi:10.4088/JCP.v64n1010 PubMed
26. Shi L, Thiebaud P, McCombs JS. The impact of unrecognized bipolar disorders for patients treated for depression with antidepressants in the fee-for-services California Medicaid (Medi-Cal) program. J Affect Disord. 2004;82(3):373–383. PubMed
27. Matza LS, Rajagopalan KS, Thompson CL, et al. Misdiagnosed patients with bipolar disorder: comorbidities, treatment patterns, and direct treatment costs. J Clin Psychiatry. 2005;66(11):1432–1440. doi:10.4088/JCP.v66n1114 PubMed
28. Mantere O, Suominen K, Arvilommi P, et al. Clinical predictors of unrecognized bipolar I and II disorders. Bipolar Disord. 2008;10(2):
238–244. doi:10.1111/j.1399-5618.2007.00501.x PubMed
29. Nasr S, Popli A, Wendt B. Can the Mini SCID improve the detection of bipolarity in private practice? J Affect Disord. 2005;86(2–3):289–293. doi:10.1016/j.jad.2005.01.008 PubMed
30. Ghaemi SN, Sachs GS, Chiou AM, et al. Is bipolar disorder still underdiagnosed? are antidepressants overutilized? J Affect Disord. 1999;52(1–3):135–144. PubMed doi:10.1016/S0165-0327(98)00076-7
31. Benazzi F. Diagnosis of bipolar II disorder: a comparison of structured versus semistructured interviews. Prog Neuropsychopharmacol Biol Psychiatry. 2003;27(6):985–991. doi:10.1016/S0278-5846(03)00158-1 PubMed
32. Benazzi F, Akiskal HS. Refining the evaluation of bipolar II: beyond the strict SCID-CV guidelines for hypomania. J Affect Disord. 2003;73(1–2):
33–38. doi:10.1016/S0165-0327(02)00327-0 PubMed
33. Akiskal HS, Benazzi F. Optimizing the detection of bipolar II disorder in outpatient private practice: toward a systematization of clinical diagnostic wisdom. J Clin Psychiatry. 2005;66(7):914–921. doi:10.4088/JCP.v66n0715 PubMed
34. Goldberg JF, Garno JL, Callahan AM, et al. Overdiagnosis of bipolar disorder among substance use disorder inpatients with mood instability. J Clin Psychiatry. 2008;69(11):1751–1757. doi:10.4088/JCP.v69n1110 PubMed
35. Stewart C, El-Mallakh RS. Is bipolar disorder overdiagnosed among patients with substance abuse? Bipolar Disord. 2007;9(6):646–648. doi:10.1111/j.1399-5618.2007.00465.x PubMed
36. Paris J. Borderline or bipolar? distinguishing borderline personality disorder from bipolar spectrum disorders. Harv Rev Psychiatry. 2004;
12(3):140–145. doi:10.1080/10673220490472373 PubMed
37. Zimmerman M, Galione JN, Ruggero CJ, et al. Screening for bipolar disorder and finding borderline personality disorder. J Clin Psychiatry. 2010;71(9):1212–1217. doi:10.4088/JCP.09m05161yel PubMed
38. Reich DB, Zanarini MC, Fitzmaurice G. Affective lability in bipolar disorder and borderline personality disorder [published online ahead
of print May 30, 2011].Compr Psychiatry. PubMed
39. Benazzi F. Is 4 days the minimum duration of hypomania in bipolar II disorder? Eur Arch Psychiatry Clin Neurosci. 2001;251(1):32–34. doi:10.1007/s004060170065 PubMed
40. Zimmerman M, Ruggero CJ, Chelminski I, et al. Is bipolar disorder overdiagnosed? J Clin Psychiatry. 2008;69(6):935–940. doi:10.4088/JCP.v69n0608 PubMed
41. Zimmerman M, Galione J. Psychiatrists’ and nonpsychiatrist physicians’ reported use of the DSM-IV criteria for major depressive disorder.
J Clin Psychiatry. 2010;71(3):235–238. doi:10.4088/JCP.08m04940blu PubMed
42. Shankman SA, Lewinsohn PM, Klein DN, et al. Subthreshold conditions as precursors for full syndrome disorders: a 15-year longitudinal study
of multiple diagnostic classes. J Child Psychol Psychiatry. 2009;50(12):
1485–1494. doi:10.1111/j.1469-7610.2009.02117.x PubMed
43. Lewinsohn PM, Klein DN, Seeley JR. Bipolar disorder during adolescence and young adulthood in a community sample.
Bipolar Disord. 2000;2(3, pt 2):281–293. doi:10.1034/j.1399-5618.2000.20309.x PubMed
44. Tijssen MJ, van Os J, Wittchen HU, et al. Prediction of transition from common adolescent bipolar experiences to bipolar disorder: 10-year study. Br J Psychiatry. 2010;196(2):102–108. doi:10.1192/bjp.bp.109.065763 PubMed
45. Regeer EJ, Krabbendam L, de Graaf R, et al. A prospective study of the transition rates of subthreshold (hypo)mania and depression in the general population. Psychol Med. 2006;36(5):619–627. doi:10.1017/S0033291705006823 PubMed
46. Fiedorowicz JG, Endicott J, Leon AC, et al. Subthreshold hypomanic symptoms in progression from unipolar major depression to bipolar disorder. Am J Psychiatry. 2011;168(1):40–48. doi:10.1176/appi.ajp.2010.10030328 PubMed
47. Robins E, Guze SB. Establishment of diagnostic validity in psychiatric illness: its application to schizophrenia. Am J Psychiatry. 1970;126(7):
983–987. PubMed
48. Kendler KS, Kupfer DJ, Narrow WE, et al. Guidelines for
Making Changes to DSM-V. 2009. Accessed on 3/3/11 from
http://www.dsm5.org.
49. Goodwin G. Hypomania: what’s in a name? Br J Psychiatry. 2002;181:
94–95. PubMed
50. Patten SB. Does almost everybody suffer from a bipolar disorder?
Can J Psychiatry. 2006;51(1):6–8. PubMed
51. First MB, Frances A. Issues for DSM-V: unintended consequences of small changes: the case of paraphilias. Am J Psychiatry. 2008;165(10):1240–1241. doi:10.1176/appi.ajp.2008.08030361 PubMed
This PDF is free for all visitors!



