Psychiatric Care of the Patient With Hepatitis C: A Review of the Literature
Context: Approximately 1.8% of the US population is chronically infected with the hepatitis C virus (HCV). The prevalence rates of psychiatric illness in patients with HCV infection are higher than those rates in the general US population, and the prevalence of HCV infection in patients with severe mental illness may be as high as 9 times that of the general US population. Primary care physicians and psychiatrists are on the forefront of identifying patients with psychiatric illness who are at risk for HCV infection and can screen for HCV infection. This review summarizes the psychiatric implications of HCV infection and strategies for the management of interferon alfa-induced neuropsychiatric adverse effects.
Evidence Acquisition: English-language studies were identified by computerized searches using the term hepatitis C psychiatric between 1972 and 2009, and further references were obtained from bibliographies of the reviewed articles. Relevant references were reviewed by the authors and included the basis of significance and applicability to practicing psychiatrists and internists.
Results: Since primary care physicians and psychiatrists are sometimes the only medical link for patients with psychiatric illness, they are expected to provide posttest counseling for their patients with HCV and psychiatric illness. The task of conducting a psychiatric and psychosocial pretreatment risk-benefit assessment to determine whether or not to treat HCV infection is increasingly delegated to primary care providers as well as psychiatrists. The use of interferon alfa-based therapies to eradicate HCV has been associated with frequent neuropsychiatric adverse effects (eg, affective, anxiety, cognitive, and psychotic symptoms) that compromise the management of HCV patients with and without a preexisting history of psychiatric illness. Primary care physicians and psychiatrists are frequently asked to assist in the management of these neuropsychiatric adverse effects and evaluate the risks and benefits of using prophylactic psychotropics.
Conclusions: Despite the clinical challenge that interferon alfa treatment for patients with comorbid HCV and psychiatric illness presents, recent research indicates that interferon alfa can be safely administered to HCV-infected patients with psychiatric disorders provided there is a comprehensive pretreatment assessment, a risk-benefit analysis, and intensive ongoing medical and psychiatric follow-up.
Prim Care Companion J Clin Psychiatry 2010;12(6):e1-e13
© Copyright 2010 Physicians Postgraduate Press, Inc.
Submitted: August 29, 2009; accepted May 7, 2010.
Published online: December 16, 2010 (doi:10.4088/PCC.09r00877whi).
Corresponding author: Muhamad Aly Rifai, MD, Lehigh Valley Health Network, 2545 Schoenersville Rd, 5th Floor, Bethlehem, PA 18017 ([email protected]).
In 1972, Alter and colleagues1 first identified non-A, non-B transfusion-associated hepatitis, which became known in 1989 as the hepatitis C virus (HCV) infection.2,3 Hoofnagle et al4 described in 1986 the use of interferon alfa to correct liver function abnormalities in patients with non-A, non-B hepatitis, even before the actual causative agent was discovered. The neuropsychiatric implications of HCV infection and its treatments were also apparent before the identification of HCV. In 1987, Renault, a psychiatrist at the National Institute of Mental Health (NIMH), along with Hoofnagle and others described interferon alfa-associated neuropsychiatric adverse effects when treating patients with non-A, non-B hepatitis.5,6 Several case reports were published afterward detailing the use of psychotropics to treat interferon alfa-associated neuropsychiatric adverse effects.7,8 Yet, it was not until 2001 that the high association between HCV infection and psychiatric illness was established and documented,9-11 and, in 2002, the seminal trials evaluating the utility of antidepressants in treating interferon alfa-induced depression in patients with HCV infection were published.12,13
Clinical Points
- Primary care physicians and psychiatrists are on the forefront of identifying patients with psychiatric illness who are at risk for hepatitis C virus (HCV) infection and can screen for HCV.
- Preexisting psychiatric disorders complicate HCV treatment, as HCV treatment may cause the emergence, exacerbation, or acceleration of psychiatric disorders.
- Primary physicians and psychiatrists can help detect, manage, and ameliorate the neuropsychiatric adverse effects associated with HCV treatment.
In this review, we describe the epidemiology of HCV infection in psychiatric populations, introduce the concept of HCV as a disease of the liver and the central nervous system (CNS), and present new emerging evidence suggesting that HCV invades the CNS. Additionally, we review the current literature on response rates resulting from the use of antiviral treatments to eradicate HCV infection in patients with psychiatric disorders and present the current knowledge on interferon alfa-associated neuropsychiatric adverse effects. We then review the pretreatment assessment process for interferon alfa and ribavirin treatment. Finally, we discuss the available treatment options and prophylactic modalities to prevent interferon alfa and ribavirin-associated neuropsychiatric adverse effects and discuss future research directions.
English-language studies were identified by computerized searches using the term hepatitis C psychiatric between 1972 and 2009, and further references were obtained from bibliographies of the reviewed articles. Relevant references were reviewed by the authors and included the basis of significance and applicability to practicing psychiatrists and internists.
HCV and Its Epidemiology
HCV is a neuropathic ribonucleic acid (RNA)-based virus from the Flaviviridae family (which includes among other neurotoxic viruses the West Nile virus and the encephalitis viruses).14 HCV has 6 different viral genotypes (1-6) and possesses a very primitive enzymatic replication system that has an error rate of 1/100,000 (ie, an error in replication in 1 viral copy out of every 100,000 produced).15 This high error rate along with the genetic heterogeneity of HCV may explain the inability of innate immunity to clear HCV in the majority of those infected. Chronicity of HCV infection occurs in about 75%-85% of those infected. This primitive replication machinery helps explain the resistance of HCV to antiviral therapies and difficulties in developing a vaccine against HCV infection.
The HCV genotypes, which have about 65% genetic homology, are geographically distributed. Genotypes 1, 2, and 3 are most common in North America and the Far East (Japan, Korea, Taiwan).16 Type 4 is found mostly in the Middle East (specifically Egypt). Genotype 5 is predominately found in South Africa, while genotype 6 is found almost exclusively in Southeast Asia.16
Among US patients with HCV infection, approximately 70% have genotype 1, while genotypes 2 and 3 together account for the remaining 20%-30% of US HCV patients.17 Although HCV genotypes do not correlate with disease severity, response rates to interferon alfa-based therapies are substantially higher among patients infected with genotype 2 or 3 compared with patients infected with genotype 1 (75%-85% vs 50%-60%).17 Furthermore, patients infected with these more responsive HCV genotypes can be treated with a shorter course of interferon alfa and ribavirin therapy (24 weeks for genotypes 2 and 3 vs 48 weeks for genotype 1).18
HCV Transmission and Risk Factors
Well-established HCV risk factors include intravenous (IV) drug use, blood or blood product transfusions prior to 1992, and hemodialysis.19 Targeted screening for HCV infection in patients with 1 or more of these risk factors has been recommended by the Centers for Disease Control (CDC) and is clearly warranted.20 However, evidence is beginning to emerge that other patient groups also may be at a higher risk for HCV infection when compared with the general US population.21 These groups include non-IV drug users,22,23,24 patients with high-risk sexual practices (eg, men having sex with men), and patients admitted to psychiatric hospitals.25-27 Two distinct demographic groups that have an elevated prevalence of HCV infection include patients followed at the Department of Veterans Affairs hospitals (prevalence is around 6%)28,29 and incarcerated individuals (prevalence as high as 20%).30 HCV is not considered a sexually transmitted disease; however, having multiple sexual partners is a risk factor.19 The potential transmission of HCV infection through tattooing and body piercing remains a controversial issue; there are insufficient data to consider patients with tattoos and body piercing at an elevated risk for HCV infection.19
Is HCV a Disease of the Liver Only?
There is growing interest in the concept of HCV infection as a disease of the liver and the CNS since patients with HCV infection suffer from cognitive impairment and an excess prevalence of psychiatric illness when compared with the general US population.31 So far, demonstrating an association between HCV infection and the CNS has been a clinical phenomenon, with a large evidence of neuropsychological and biochemical findings, but illusive histochemical evidence.32-34
Several researchers found that, in comparison to healthy controls, patients with HCV infection showed evidence of cognitive impairment, primarily in attention and higher executive functions.32,35-37 Patients with HCV infection were found to suffer from higher levels of anxiety and depression and impairment of quality of life.38,39 The cerebral cortex of patients with HCV infection showed a significant decrease of the N-acetyl-aspartate/creatine ratio on 1H magnetic resonance spectroscopy coupled with electroencephalogram waves being slowed in a majority of such patients. These deficits were more marked in the patients with moderate rather than mild fatigue.34
The task of locating HCV in the CNS has proven very difficult. The hypothesis that HCV-induced neuropsychiatric symptoms are related to HCV invasion of the CNS has been examined by studying cerebrospinal fluid (CSF) from a small series of patients with HCV infection.40-43 The presence of negative strands of HCV (viral replication intermediate) in the CSF has suggested active HCV replication.40-43 Forton et al44 examined the CSF, serum, and peripheral blood mononuclear cells searching for different strains of HCV, as determined by phylogenetic analysis. CSF-derived strains were more closely related to those found in peripheral blood mononuclear cells than in serum. The researchers44 hypothesized that peripheral blood mononuclear cells could carry the virus into the CNS and provide a mechanism for HCV neuroinvasion. In a follow-up study, Forton et al45,46 were able to identify brain-specific variants of HCV from brain tissue of HCV-infected individuals collected at autopsy, and these variants had discrete genomic mutations in the internal-ribosomal entry site region of the HCV genome, suggesting that this region may be important in promoting replication of the virus in cells other than hepatocytes.
These clinical, behavioral, biochemical, and histologic findings provide preliminary evidence of CNS involvement in patients with HCV infection. These findings coupled with the fact that HCV belongs to a family of neuropathic viruses that affect the CNS add credence to the notion of HCV infection being a disease of both the liver and the CNS. Future advancement in histochemical and viral detection technology, viral cultures, and imaging techniques may help answer and clarify the link between HCV infection and the CNS.34
HCV and Psychiatric Illness
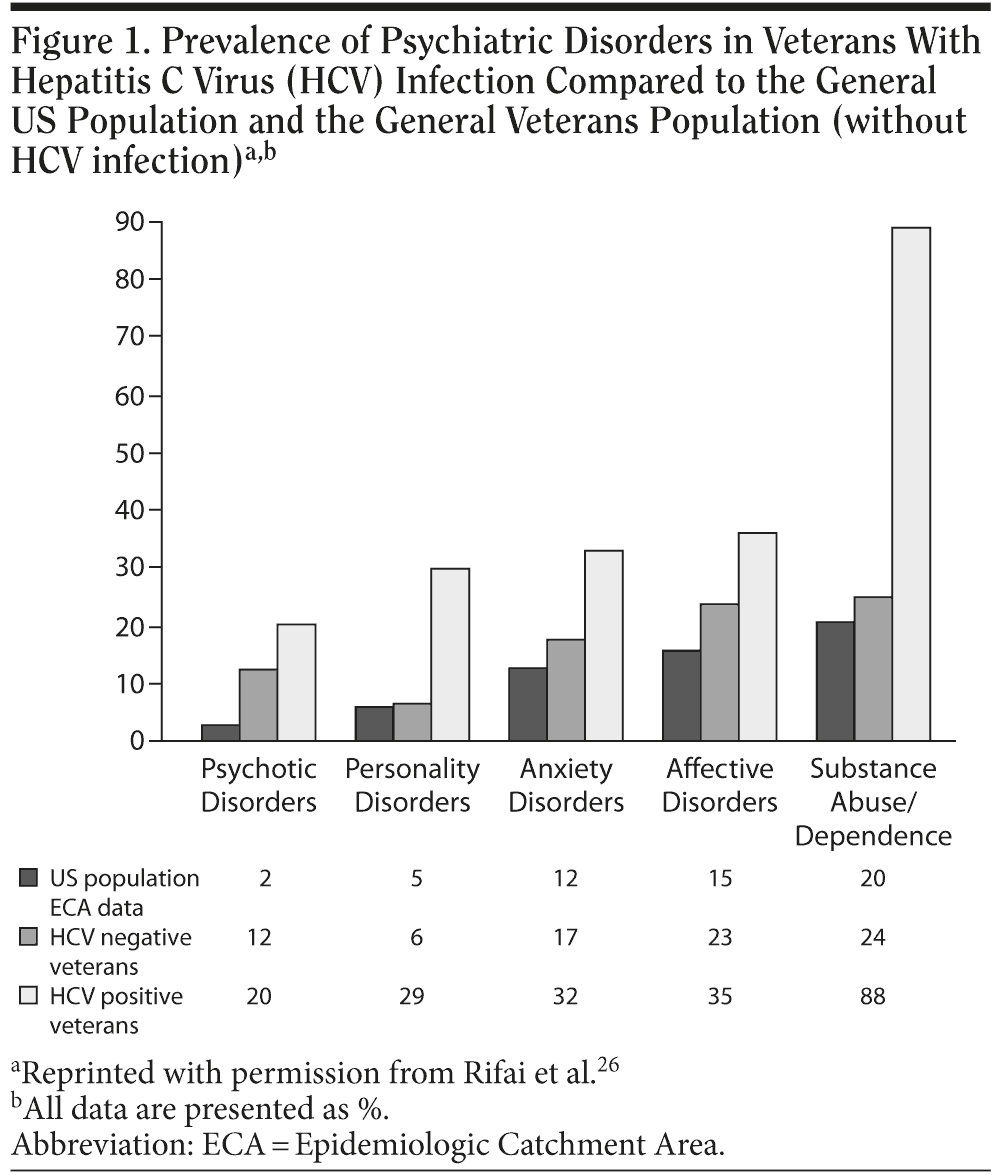
A growing body of evidence indicates that patients infected with HCV have a high prevalence of psychiatric disorders, irrespective of HCV antiviral treatments.10,47,48 At least 50% of patients infected with HCV suffer from a psychiatric illness, and the lifetime prevalences of psychotic, anxiety, affective, personality, and substance use disorders are all higher among patients with HCV,10,47 as compared to the general US population studied in the Epidemiologic Catchment Area study.49,50 Most of the studies on the prevalence of psychiatric disorders among patients with HCV infection, however, have surveyed veterans followed at the US Department of Veterans Affairs hospitals. Nonetheless, even when correcting for the higher prevalence of psychiatric disorders among the veteran population, patients with HCV infection have a higher prevalence of psychiatric disorders. Studies on the prevalence of psychiatric illness in other patient populations with HCV infection have yielded similar results to those found in the veteran population, indicating the increased association between psychiatric illness and HCV infection even when antiviral treatments are taken into account. Figure 1 illustrates the prevalence rates of psychiatric disorders among patients with HCV infection.
The Prevalence of HCV in Psychiatric Populations
The prevalence of HCV among US patients with severe mental illness is 4-9 (8%-18%) times that of the general US population (2%). A 5-site health and risk study found the prevalence of HCV infection among patients in psychiatric hospitals to be 18%.22 In a separate report, the prevalence of HCV infection among patients admitted to the state psychiatric hospitals in Illinois was found to be 8.5%.25 We and others have found the prevalence of HCV infection among veterans admitted to inpatient psychiatric services in Virginia to be 12.7% (443/3,470).31,51,52
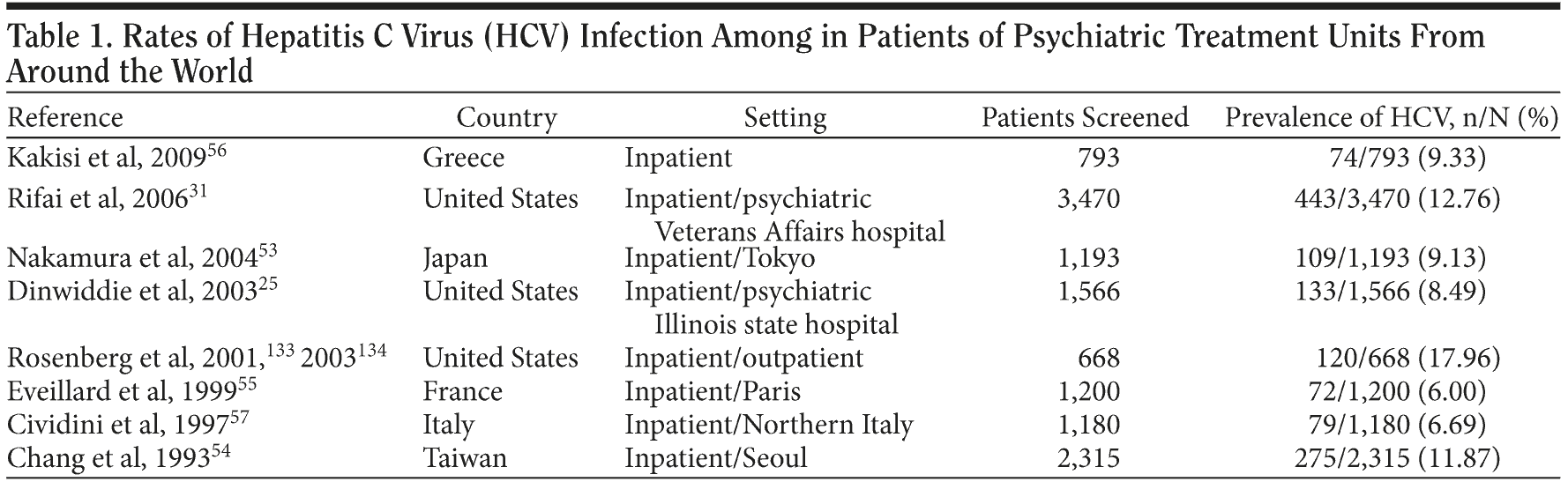
The high prevalence of HCV infection is not a phenomenon that is unique to psychiatric institutions in the United States. In fact, the prevalence of HCV infection among patients admitted to psychiatric institutions in different countries around the world is significantly higher than the prevalence of HCV among the general populations of those countries. For example, in a study of patients hospitalized in psychiatric hospitals in central Japan,53 the prevalence of HCV infection was found to be 9.1%, several times the prevalence of HCV infection in the general Japanese population (1%-2%). A similar survey in Taiwan indicated the prevalence rate of HCV infection to be 11.87% among patients admitted to psychiatric institutions, while the prevalence of HCV infection among the general Taiwanese population was 1%.54
Case-controlled studies investigating the prevalence of HCV infection in psychiatric institutions conducted on the European continent (France, Italy, Greece) also have demonstrated that the prevalence of HCV infection among psychiatric populations is higher than that of the general European population.55,56 Cividini et al57 found the prevalence of HCV among psychiatric patients in northern Italy to be 6.69%, compared with the prevalence of 1.5% among the general Italian population. Table 1 lists the prevalence of HCV in different inpatient and outpatient psychiatric settings in the United States and around the world.
The extent to which psychiatric illness and inpatient psychiatric hospitalization predisposes individuals to HCV infection and conversely that HCV infection contributes to psychiatric illness is not currently known. For example, 1 study found that razor-sharing is associated with increased transmission of HCV among psychiatric populations in the inpatient setting in Japan.58 In opposition, researchers in northern Italy followed 499 psychiatric patients hospitalized for up to 7.5 years and found no increase in transmission of HCV during the inpatient psychiatric hospitalization.59
For some patients with preexisting mental illness (psychotic, substance use disorders), their high-risk behavior (behavioral dyscontrol, particularly the sharing of needles, intranasal paraphernalia during drug use, or high-risk unprotected sexual activity) clearly increases the likelihood of contracting HCV infection.52,60,61 However, for other patients (eg, those with anxiety and affective disorders), the distinction between cause and effect is less clear.62,63 In any event, for 25%-40% of patients with HCV, there is no clear identifiable mode of transmission.64
The Role of Primary Care Physicians and Psychiatrists in Screening for HCV
Despite the association between HCV and psychiatric illness, screening for HCV has not been a routine practice in patients with psychiatric illness. These patients are at risk for contracting HCV by engaging in risky sexual behaviors (multiple partners, men having sex with men) and intranasal drug use but may not be forthcoming about these activities.65 Therefore, the only reliable way to rule out HCV infection would be to screen these at-risk populations. The CDC has recommended routine screening of incarcerated individuals in correctional facilities for HCV.66 Routine HCV screening is also recommended for all patients who are found to be infected with HIV.65 The Department of Veterans Affairs conducts routine HCV screening for all veterans being treated at Veterans Affairs hospitals.31,67,68
However, the US Preventive Services Task Force in 2004 recommended against routine screening for HCV in high-risk individuals because it found no data to support the efficacy of interferon alfa and ribavirin treatment in reducing morbidity and mortality from HCV infection despite 2 decades of research on the utility of interferon alfa-based therapies in achieving viral clearance.69 Therefore, interferon alfa and ribavirin treatment for patients with HCV infection continues to be considered a therapeutic modality with an intuitive value but no evidence-based efficacy in reducing the overall morbidity and mortality associated with HCV.70
The care of patients with HCV and comorbid psychiatric illness is challenging, since most psychotropic drugs (antidepressants, antipsychotics, mood stabilizers) are metabolized by the liver and are associated with significant hepatotoxicity. The combination of HCV-induced liver disease and psychotropic drug use (not to mention alcohol use) may hasten the progression to cirrhosis.71,72 Several researchers, including our group, have found increased rates of all-cause mortality as well as mortality rates specifically from liver disease in patients with HCV infection and psychiatric disorders.31,73 Furthermore, patients with HCV and psychiatric illness also may be less likely to receive a liver transplant due to the perceived difficulties they might have in complying with the rigorous posttransplant regimen.62,63,74
Given the steep trajectory of HCV-induced liver disease among patients with psychiatric illness and the role alcohol, psychotropics, and decreased compliance play in accelerating HCV-induced liver and CNS consequences,31,62,63,71-74 we believe that the argument about the lack of sufficient data supporting the utility of HCV antiviral treatments in reducing morbidity and mortality from cirrhosis and primary liver cancer needs to be balanced by the additional risks for poor outcomes in the HCV population with psychiatric illness. We therefore contend that screening for HCV in patients with psychiatric illness is clinically appropriate and prudent.75
Posttest Counseling of Patients With Psychiatric Illness and HCV Infection
Patients who are found to be infected with HCV should be counseled regarding prevention of the spread of the virus to others.19,76 HIV testing should be offered given the comorbidity of HIV/AIDS and HCV (approximately 5% of HCV patients are coinfected with HIV).77 HCV can be transmitted through shared use of common household objects such as toothbrushes, shaving utensils, and other personal items, and patient and family counseling should emphasize not sharing such personal items. Although HCV infection has a low rate of sexual transmission (particularly very low rates of transmission among long-term monogamous partners), patients should still be advised to practice safe sex and use barrier protection to further reduce transmission risks of HCV and other sexually transmitted diseases.
Recent emerging research suggests that the most important component of posttest counseling for a patient with newly diagnosed HCV infection should be a candid discussion about alcohol use. An accumulating body of evidence suggests that alcohol use even in moderation can accelerate the progression of HCV-induced liver disease78; consequently, HCV patients should be advised to eliminate all alcohol use.79,80
Research in veterans with HCV infection and alcohol use disorders suggests that candid counseling about the need to eliminate alcohol use may be a motivator toward improved rates of abstinence from alcohol use and actually may yield a better eligibility for interferon treatment and improved treatment outcomes.79,80
HCV Pretreatment Assessment: The Role of Integrated Multidisciplinary Care
Primary care physicians and psychiatrists along with gastroenterologists are increasingly taking the lead role in deciding whether to offer interferon alfa and ribavirin treatment to patients with HCV.81 This decision is more frequently undertaken in a multidisciplinary fashion and is based on a comprehensive pretreatment risk-benefit assessment that incorporates not only predictors of viral clearance and the likelihood of interferon alfa and ribavirin-induced neuropsychiatric adverse effects, but also the patient’s treatment preferences and available psychosocial resources.82
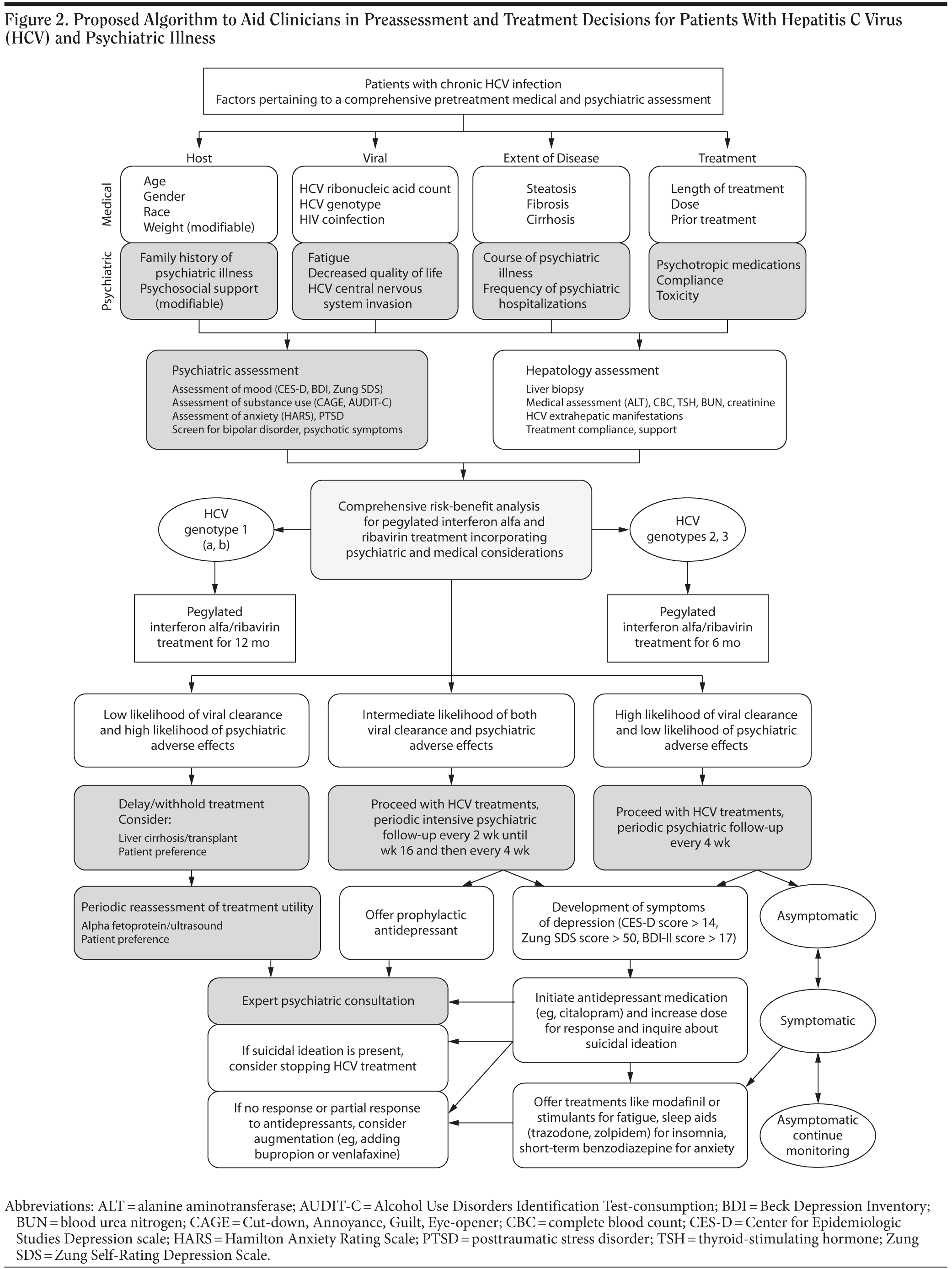
We propose an update of an algorithm that we previously developed to assist clinicians caring for patients with HCV who are being considered for interferon alfa and ribavirin treatment (Figure 2).83 The first part of the algorithm lists prognostic factors that are both static and modifiable that can be incorporated into the decision whether to proceed with interferon alfa and ribavirin treatment in a particular patient.18 Gastroenterologists and hepatologists rely on consensus guidelines to navigate through a multitude of cumulative and prognostic factors (HCV genotype, HCV RNA viral load, race, gender, age, body mass index). These prognostic factors may foretell the likelihood of response to treatment. The multidisciplinary assessment should incorporate results from liver pathology and the course of HCV-induced liver disease to formulate individualized treatment recommendations for patients with HCV and psychiatric illness.70,76 Expert consultant psychiatrists can add to this decision and advise on the likelihood of neuropsychiatric adverse effects with HCV treatments.52,81,84,85
Several researchers have reported that the use of a multidisciplinary approach led to improved rates of patient engagement in the evaluation process for HCV treatment and enhanced compliance rates as well as superior HCV viral clearance rates compared to those reported in the literature.86,87 The broad aims of integrated multidisciplinary care models include reducing fragmentation and improving continuity and coordination of care. Components of a primary care practice or HCV clinic incorporating these principles include routine screening of all patients for psychiatric and substance use disorder risk factors, collaboration with mental health providers, following a defined integrated medical/psychiatric clinical protocol, provision of ongoing integrated support during antiviral treatment or retreatment, and educating patients on principles of chronic disease self-management.86,87
There is an absence of consensus regarding when interferon alfa and ribavirin treatment should be withheld or delayed (either due to the low estimated likelihood of viral clearance or the high probability of neuropsychiatric adverse effects).68,82 Nonetheless, primary care physicians, psychiatrists, and gastroenterologists should collaborate to make an individualized and balanced risk-benefit analysis incorporating HCV disease-specific factors as well as the potential for neuropsychiatric adverse effects prior to offering interferon alfa treatment to a patient.84,88
It is very important that patients considering HCV antiviral treatment understand the process and plan for it; they will need to commit to a venture that may be difficult and long in duration while ultimately not achieving its goal.68,89 Those patients with unrealistic views of treatment may not make the necessary plans for accommodation and may prematurely withdraw from treatment when faced with medical or neuropsychiatric adverse effects of the antiviral treatment regimen, or may take an emotional down spiral upon learning of their treatment’s failure.31,67 The interferon alfa and ribavirin pretreatment evaluation offers multiple opportunities to reinforce patients’ knowledge of HCV infection and its treatment; therefore, all physicians conducting such assessments should be conversant with the basic facts of interferon alfa and ribavirin treatments.90,91
Treatment Rates of HCV in Patients With Psychiatric Illness
The HCV clearance rates in response to antiviral treatment that are reported in the literature may not be applicable to the entire HCV-infected population because they were derived from clinical trials that excluded patients with preexisting psychiatric and substance use disorders.92,93 In contrast to these large pivotal HCV treatment trials, early reports detailing the clinical experience with HCV antiviral treatments describe reduced rates of patient engagement in the evaluation process leading to HCV treatment.92,93 These reports also cite psychiatric illness and substance use as reasons for HCV treatment ineligibility in at least half of the HCV patients being evaluated.92,93 Additionally, patients who were eligible for treatment had poorer HCV clearance rates (10%-15%).92,93
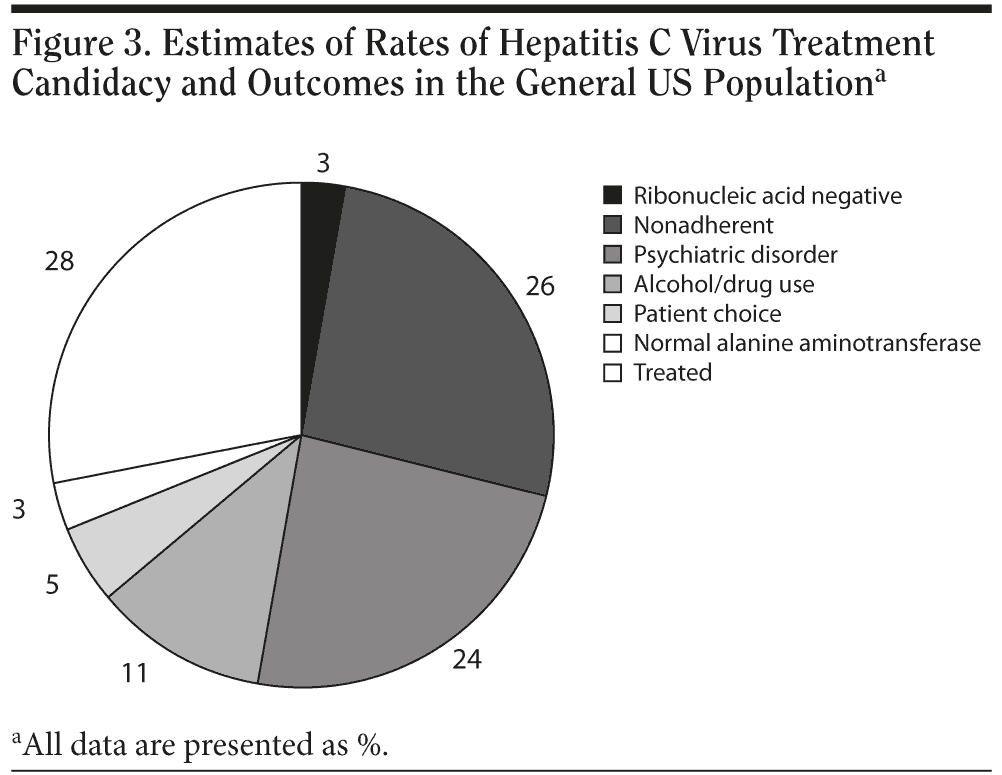
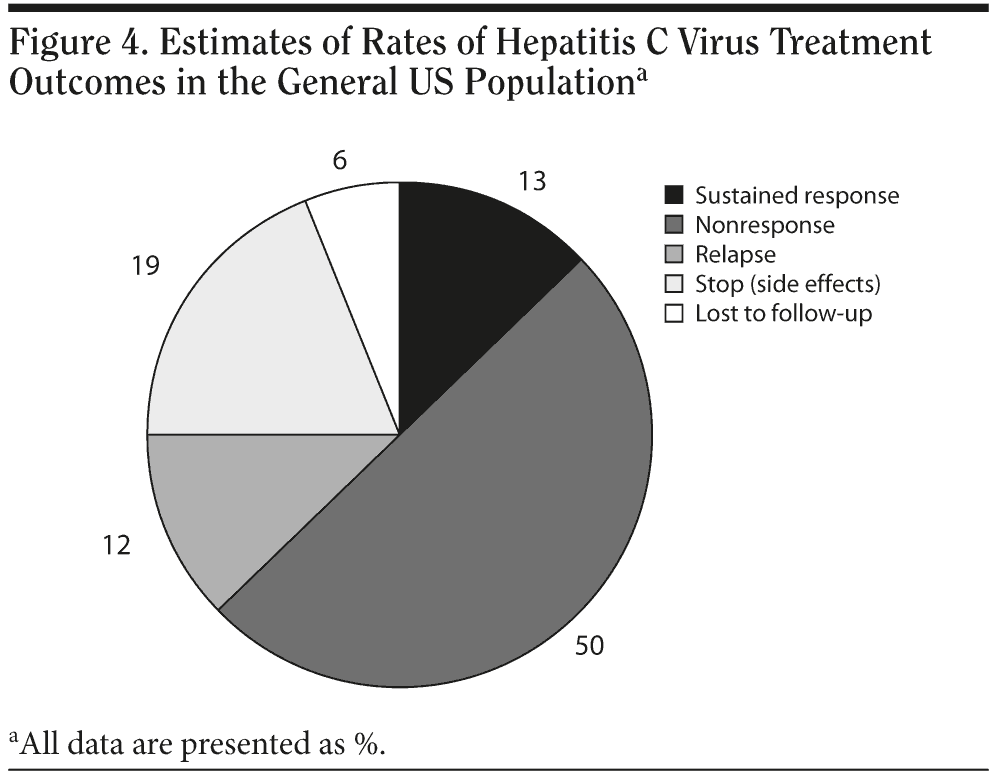
However, we and others reported more recently and in multiple populations with HCV and psychiatric disorders that HCV antiviral treatments can be safely completed and that compliance rates and viral clearance rates and outcomes in these patients are similar to those in patients with HCV infection but without psychiatric or substance abuse histories.31,85,89,94 These findings about improved compliance and safety of HCV antiviral treatment have led to an increase in the rates of initiating HCV antiviral treatment in patients with HCV and psychiatric disorders.18,95 Figures 3 and 4 illustrate realistic rates of HCV treatment candidacy and HCV treatment outcomes.
HCV Treatment Outcomes: The Effect of Psychiatric Illness
Despite the emerging evidence that patients with HCV infection and preexisting or current psychiatric illness and/or history of substance abuse can be safely treated with antiviral treatments, these patients continue to be routinely excluded from interferon alfa and ribavirin therapy for HCV due to concerns about interferon alfa and ribavirin-induced neuropsychiatric adverse effects.96-98 Nonetheless, several researchers have observed similar rates of neuropsychiatric adverse effects of interferon alfa and ribavirin treatment in those with and without preexisting psychiatric illness.99-101
Schaefer and colleagues99,102-104 prospectively examined the treatment outcomes of different groups of patients with HCV and comorbid psychiatric and substance abuse risk factors who received pegylated interferon alfa and ribavirin. Seventy patients were divided into 4 groups: (1) controls, those with no history of psychiatric illness or substance abuse; (2) psychiatric group, patients with a history of mental illness, but without history of prior substance use disorders; (3) methadone maintenance group, patients active in a methadone maintenance program, with or without history of psychiatric illness (83.3% had psychiatric comorbidity); and (4) former drug abusers group, with or without history of psychiatric illness (92.4% had psychiatric comorbidity).
Several important findings were observed in this series of studies by Schaefer et al99,102-104 examining the treatment of patients with HCV and comorbid psychiatric and substance abuse disorders. First, sustained virologic response rates in patients with prior psychiatric histories and prior substance use disorders were similar to response rates seen in the control group (50%, 53.8%, and 58.8%, respectively). Second, subjects with prior psychiatric histories and drug use disorders did not experience increased psychiatric side effects from the antiviral therapy, despite being considered a high-risk group. Finally, surprisingly, the patients who received methadone maintenance therapy had sustained virologic response (HCV-RNA negative status after 6 months) rates higher than all other groups, including the control group, at 72.2%.
Alvarez-Uria et al105 conducted an observational study of patients with HCV genotypes 2 and 3 that compared HCV antiviral treatment response rates of patients with current and prior psychiatric and substance abuse histories to patients without such histories. Patients with a history of depression, but who were not being treated with an antidepressant at the onset of antiviral therapy, had the highest interferon alfa treatment dropout rate, and patients who were actively using intravenous drugs were found to have the highest rate of relapse of HCV infection.105 However, patients with chronic psychotic disorders and those with prior histories of intravenous drug use, but not currently using, had similar treatment response rates as patients without such histories.105
Although much of the research examining psychiatric illness and HCV has focused on depression, the first author reported on 5 patients with HCV and comorbid bipolar disorder during combination interferon alfa and ribavirin therapy.106 In this small series, 3 of the patients were able to successfully complete antiviral therapy, 1 without psychiatric adverse effects and 2 with psychiatric adverse effects that were carefully managed throughout the course of treatment. The remaining 2 patients had to discontinue interferon alfa and ribavirin therapy due to mania and suicidal ideation. Prior to treatment initiation, comprehensive psychiatric histories were obtained on all patients, and all were required to maintain frequent psychiatric follow-up. The 3 patients who were able to complete interferon therapy all had histories of several years of mood stability and were without report of significant substance use disorders. Two were treated with lithium carbonate and the third patient received lithium carbonate during interferon therapy to treat emergent manic symptoms. The 2 individuals who did not successfully complete treatment had more complicated psychiatric histories with several prior psychiatric hospitalizations, prior substance use disorders, and prior difficulties with recurrent suicidal ideation. This descriptive information might be useful to physicians making clinical decisions about whether or not a patient with bipolar disorder should undergo treatment with interferon alfa and ribavirin. The author cautions physicians about treating patients with bipolar disorder due to the potential apparent fragility of the disorder when exposed to HCV antiviral treatment.106
Neuropsychiatric Adverse Effects of Interferon Alfa and Ribavirin in Patients With HCV
Neuropsychiatric side effects are common during interferon alfa and ribavirin therapy for HCV, ranging from 24% to 49% of patients experiencing such symptoms.47,107 Neuropsychiatric adverse effects can include fatigue, irritability, depression, anhedonia, relapse in alcohol or drug abuse, anxiety, anger, hostility, cognitive disturbances, manic symptoms, delirium, psychosis, and suicidal ideation.99,108-111
During clinical trials conducted to gain US Food and Drug Administration approval of peginterferon alfa-2a and -2b, psychiatric adverse effects were among the most commonly reported adverse effects, occurring in 77% of patients.18 The most common psychiatric adverse effects were depression (ranging from 25%-34%), irritability, and insomnia. The observance of high rates of insomnia and irritability in these early trials is interesting given that recent reports in the literature indicate that mania and hypomania are also common adverse effects of interferon alfa and ribavirin therapy for HCV.101,106,112,113 Suicidal ideation, suicide attempts, and actual suicides occurred in 2% of all patients studied during initial drug approval.114,115 Furthermore, psychiatric adverse effects have been among the most common reasons for therapy discontinuation, along with systemic (eg, fatigue, headache) and gastrointestinal effects.
Constant et al112,113 carefully assessed and followed 93 interferon-naive patients and found higher than expected rates of interferon-induced hypomania and mania. Psychosocial assessments were completed at baseline, at 4 weeks, and again at 12 weeks. In this group, there was a 32% incidence of interferon-induced mood disorders. Sixty percent of subjects with interferon-induced mood disorders presented with mania (10%) or hypomania (50%), and the remaining 40% were described as having “depressive mixed states” defined as depressive episodes combined with hypomanic symptoms such as racing thoughts, irritability, psychomotor agitation, and aggression. Among patients who developed interferon-induced mood disorders, the majority (63%) had a past history of a psychiatric disorder. Thirty-five percent had a prior history of depression and 29% had a prior history of substance abuse.
The majority of the literature has focused on interferon alfa and ribavirin-induced depression, and efforts have been made to identify the risk factors for the development of interferon alfa and ribavirin-induced depression. Suspected risk factors have included polymorphisms of the serotonin transporter gene, the interferon alfa receptor gene, and apolipoprotein E ε4.89,116-119 Other studies have found that levels of the inflammatory marker interleukin (IL-6) predict levels of depressive symptoms during interferon therapy.120
Dell’ Osso et al101 found that patients without a past psychiatric history were at increased risk for developing interferon alfa-induced depression if they had a lifetime history of hypomanic symptoms, but not depression. Dan et al111 found that the emergence of anger during interferon therapy was associated with increased scores on depression rating scales and poorer scores on health-related quality of life scales. Anger and irritability also might be symptoms of mania or hypomania, so gathering a complete history is important to distinguish between depression and manic symptoms, which require different forms of treatment. If a patient had interferon-induced mania, rather than depression, a mood-stabilizing agent would be indicated instead of monotherapy with antidepressants to avoid the development of antidepressant-induced mania. There also have been several case reports of interferon-induced psychosis, most of which occurred during treatment; but, there have been a few reports of the emergence of psychosis after interferon alfa discontinuation.121-123
Prophylactic Treatment of Interferon Alfa and Ribavirin-Induced Neuropsychiatric Adverse Effects
Whether or not patients with a history of psychiatric illness can complete a full course of treatment with interferon alfa and ribavirin is an important clinical question. It is frequently asked whether a patient presenting with HCV, who reports a history of psychiatric illness, but who is not currently experiencing psychiatric symptoms, can complete an HCV antiviral treatment regimen without interruption and with minimal neuropsychiatric adverse effects. It is recommended that high-risk patients, those with current psychiatric disorder or history of psychiatric illness, receive a psychiatric assessment prior to initiation of HCV antiviral treatment. Several studies have examined the usefulness of prophylactic treatment of depression in patients undergoing antiviral therapy for HCV with mixed results.124-127
Gleason and colleagues124 conducted an open-label study that examined the prophylactic treatment of depression in patients with a history of major depression in remission at the time of presentation for treatment for HCV. This study investigated whether such patients could complete a course of pegylated interferon alfa-2a and ribavirin for HCV if first pretreated with escitalopram. All patients were treated with escitalopram 10 mg daily for 1 month prior to the initiation of interferon alfa and ribavirin therapy. Escitalopram was continued during antiviral therapy, and dose adjustments were made as clinically indicated. Hamilton Depression Rating Scale scores did not change significantly during the course of treatment compared to scores obtained at baseline.124 Six of the 10 patients completed the antiviral therapy course. The 4 who did not were discontinued for reasons other than relapse of depression. The results of this small study suggest that pretreatment with escitalopram may be useful in helping patients with a history of major depression complete a course of treatment with interferon alfa and ribavirin.124
Schaefer et al126 conducted an open-label study examining the usefulness of citalopram in preventing the development of major depression during combination interferon alfa and ribavirin therapy of 14 patients. Patients who endorsed mild to moderate depressive symptoms were pretreated with citalopram 20 mg for 2 weeks prior to initiation of antiviral therapy. Major depression rates were compared over a 6-month treatment period. Subjects in the pretreatment group developed significantly fewer depressive episodes than did subjects in the control groups who did not receive citalopram.126 Kraus et al128 studied the efficacy of selective serotonin reuptake inhibitor (SSRI) prophylaxis in 8 subjects with history of prior unsuccessful treatment with interferon alfa and ribavirin who had developed major depression on such treatment. Depression rating scale scores were compared to a group of patients who were not treated with SSRI prophylaxis but who also had prior unsuccessful antiviral therapy trials, some with prior episodes of interferon-induced depression. In this study, depression scores were significantly lower during interferon alfa retrial.128
In contrast to these reports,124,126,128 in a double-blind placebo-controlled trial, Morasco and colleagues125 found that paroxetine did not prevent depression during HCV antiviral therapy in a sample of 33 patients. They did find, however, that paroxetine decreased the severity of depressive symptoms in those treated with paroxetine. Raison and colleagues,127 in a larger placebo-controlled double-blind trial including 67 patients, found that paroxetine did not prevent depression during HCV antiviral therapy. Similar to the findings by Morasco et al,125 Raison and colleagues127 found that paroxetine did reduce the intensity of depressive symptoms and depressive scores.
In addition to the lack of efficacy in preventing depression during HCV antiviral treatment, there are several concerns with wide use of antidepressant prophylaxis prior to HCV antiviral therapy. Given that an estimated 30%-35% of patients receiving interferon therapy are likely to develop interferon-induced depression,47 if all patients were treated, this would result in unnecessary antidepressant treatment in up to 70% of patients. Most available antidepressants are hepatically metabolized, which presents potential concerns with regard to drug metabolism and potential hepatotoxicity. Nonetheless, the newly approved antidepressant desvenlafaxine may prove helpful in this population due to very little appreciable hepatic metabolism.
Consideration of prophylactic treatment must take into account the potential risks of pharmacologic therapy with antidepressants (eg, nausea, vomiting, sexual dysfunction, drug interactions, paradoxical reactions, serotonin syndrome, and withdrawal symptoms upon discontinuation).124 The safety of using SSRIs in patients with HCV has been questioned, particularly with regard to potential for increased risk of bleeding and retinopathy.129,130 Examples of other antidepressants that present safety concerns include mirtazapine, which is associated with increased risk of bone marrow suppression and agranulocytosis, potentially placing a patient being treated with interferon at increased risk for infection given the potential for bone marrow suppression from interferon alfa as well.131 Another example is nefazodone, which has been shown to induce hepatotoxicity and is contraindicated in patients with liver disease.63,132
Antidepressant therapy may be very beneficial to those patients at risk for, or who develop depression during, HCV antiviral therapy, but it is important to weigh the potential benefits against the potential risks in this group and engage in dialogue with the patient about the value and utility of antidepressant treatment to reduce the severity of depressive symptoms during HCV antiviral therapy specifically for those at risk of developing interferon alfa and ribavirin-induced depression.
CONCLUSION
HCV infection is a disease of the liver that is likely to also affect the CNS and is associated with significant neuropsychiatric morbidity. The management of psychiatric disorders associated with HCV infection is complex. These preexisting psychiatric disorders complicate HCV treatment as HCV treatments may cause the emergence, exacerbation, or acceleration of psychiatric disorders. Primary care physicians and psychiatrists can assist fellow liver specialists in HCV pretreatment evaluation and can help detect, manage, and ameliorate the neuropsychiatric adverse effects associated with HCV treatments.
Drug names: citalopram (Celexa and others), desvenlafaxine (Pristiq), escitalopram (Lexapro and others), lithium (Lithobid and others), mirtazapine (Remeron and others), paroxetine (Paxil, Pexeva, and others).
Author affiliations: Department of Psychiatry, Lehigh Valley Health Network, Penn State College of Medicine, Bethlehem, Pennsylvania (Dr Rifai); Department of Psychiatry, University of Oklahoma School of Community Medicine, Tulsa (Dr Gleason); and St Joesph Regional Medical Center, Patterson, New Jersey (Dr Sabouni).
Potential conflicts of interest: None reported.
Funding/support: None reported.
Previous presentation: This article is a summary of the yearly continuing medical education course “Psychiatric Care of the Hepatitis C Patient” presented at the Annual American Psychiatric Association Annual meetings from 2005 to 2009 (158th: May 25, 2005, Atlanta, Georgia; 159th: May 24, 2006, Toronto, Canada; 160th: May 23, 2007, San Diego, California; 161st: May 6, 2008, Washington, DC; and 162nd: May 19, 2009, San Francisco, California).
REFERENCES
1. Alter HJ, Holland PV, Purcell RH, et al. Posttransfusion hepatitis after exclusion of commercial and hepatitis-B antigen-positive donors. Ann Intern Med. 1972;77(5):691-699. PubMed
2. Alter HJ. Descartes before the horse: I clone, therefore I am: the hepatitis C virus in current perspective. Ann Intern Med. 1991;115(8):644-649. PubMed
3. Alter H. Discovery of non-A, non-B hepatitis and identification of its etiology. Am J Med. 1999;107(suppl 2):16-20. doi:10.1016/S0002-9343(99)00375-7
4. Hoofnagle JH, Mullen KD, Jones DB, et al. Treatment of chronic non-A, non-B hepatitis with recombinant human alpha interferon: a preliminary report. N Engl J Med. 1986;315(25):1575-1578. PubMed
5. Renault PF, Hoofnagle JH, Park Y, et al. Psychiatric complications of long-term interferon alfa therapy. Arch Intern Med. 1987;147(9):1577-1580. PubMed doi:10.1001/archinte.147.9.1577
6. Renault PF, Hoofnagle JH. Side effects of alpha interferon. Semin Liver Dis. 1989;9(4):273-277. PubMed doi:10.1055/s-2008-1040523
7. Gleason OC, Yates WR. Five cases of interferon-alpha-induced depression treated with antidepressant therapy. Psychosomatics. 1999;40(6):510-512. PubMed
8. Hauser P, Soler R, Reed S, et al. Prophylactic treatment of depression induced by interferon-alpha. Psychosomatics. 2000;41(5):439-441. PubMed doi:10.1176/appi.psy.41.5.439
9. Yovtcheva SP, Rifai MA, Moles JK, et al. Psychiatric co-morbidities in veterans with hepatitis C at the Salem Veterans Affairs Medical Center. Med Psychiatry. 2001;4(1):42.
10. Yovtcheva SP, Rifai MA, Moles JK, et al. Psychiatric comorbidity among hepatitis C-positive patients. Psychosomatics. 2001;42(5):411-415. PubMed doi:10.1176/appi.psy.42.5.411
11. Yovtcheva SP, Rifai MA, Moles JK, et al. Psychiatric comorbidity among hepatitis C-positive patients. Focus. 2005;3(2):261-265.
12. Hauser P, Khosla J, Aurora H, et al. A prospective study of the incidence and open-label treatment of interferon-induced major depressive disorder in patients with hepatitis C. Mol Psychiatry. 2002;7(9):942-947. PubMed doi:10.1038/sj.mp.4001119
13. Gleason OC, Yates WR, Isbell MD, et al. An open-label trial of citalopram for major depression in patients with hepatitis C. J Clin Psychiatry. 2002;63(3):194-198. PubMed
14. Seeff LB. Natural history of hepatitis C. Am J Med. 1999;107(suppl 2):10-15. doi:10.1016/S0002-9343(99)00374-5
15. Alter MJ. Epidemiology of hepatitis C. Hepatology. 1997;26(suppl 1):62S-65S. PubMed doi:10.1002/hep.510260711
16. Armstrong GL, Alter MJ, McQuillan GM, et al. The past incidence of hepatitis C virus infection: implications for the future burden of chronic liver disease in the United States. Hepatology. 2000;31(3):777-782. PubMed doi:10.1002/hep.510310332
17. Armstrong GL, Wasley A, Simard EP, et al. The prevalence of hepatitis C virus infection in the United States, 1999 through 2002. Ann Intern Med. 2006;144(10):705-714. PubMed
18. Ghany MG, Strader DB, Thomas DL, et al. American Association for the Study of Liver Diseases. Diagnosis, management, and treatment of hepatitis C: an update. Hepatology. 2009;49(4):1335-1374. PubMed doi:10.1002/hep.22759
19. Alter MJ. Prevention of spread of hepatitis C. Hepatology. 2002;36(suppl 1):S93-S98. PubMed doi:10.1002/hep.1840360712
20. Alter MJ, Seeff LB, Bacon BR, et al. Testing for hepatitis C virus infection should be routine for persons at increased risk for infection. Ann Intern Med. 2004;141(9):715-717. PubMed
21. Poynard T, Yuen M-F, Ratziu V, et al. Viral hepatitis C. Lancet. 2003;362(9401):2095-2100. PubMed doi:10.1016/S0140-6736(03)15109-4
22. Osher FC, Goldberg RW, McNary SW, et al. Five-Site Health and Risk Study Research Committee. Substance abuse and the transmission of hepatitis C among persons with severe mental illness. Psychiatr Serv. 2003;54(6):842-847. PubMed doi:10.1176/appi.ps.54.6.842
23. McMahon JM, Tortu S. A potential hidden source of hepatitis C infection among noninjecting drug users. J Psychoactive Drugs. 2003;35(4):455-460. PubMed
24. Rifai MA, Moles JK, Van Der Linden BJ. Hepatitis C screening in patients with substance abuse/dependence disorders. Psychosomatics. 2004;45(2):159-160.
25. Dinwiddie SH, Shicker L, Newman T. Prevalence of hepatitis C among psychiatric patients in the public sector. Am J Psychiatry. 2003;160(1):172-174. PubMed doi:10.1176/appi.ajp.160.1.172
26. Rifai MA, Van Der Linden BJ, Moles JK. Abstracts From the 2001 Annual Meeting of the Association of Medicine and Psychiatry. The prevalence of psychiatric disorders in veterans with chronic hepatitis C infection: impact on screening [abstract]. Prim Care Companion J Clin Psychiatry. 2002;4(4):163.
27. Rifai MA, Moles JK, Van Der Linden BJ. The prevalence of psychiatric disorders in patients with chronic hepatitis C. Psychosomatics. 2003;44(2):142-143.
28. Sloan KL, Straits-Tröster KA, Dominitz JA, et al. Hepatitis C tested prevalence and comorbidities among veterans in the US Northwest. J Clin Gastroenterol. 2004;38(3):279-284. PubMed doi:10.1097/00004836-200403000-00016
29. Cheung RC. Epidemiology of hepatitis C virus infection in American veterans. Am J Gastroenterol. 2000;95(3):740-747. PubMed doi:10.1111/j.1572-0241.2000.01854.x
30. Weinbaum C, Lyerla R, Margolis HS. Centers for Disease Control and Prevention. Prevention and control of infections with hepatitis viruses in correctional settings. MMWR Recomm Rep. 2003;52(RR-1):1-36, quiz CE1-CE4. PubMed
31. Rifai MA, Moles JK, Short DD. Hepatitis C treatment eligibility and outcomes among patients with psychiatric illness. Psychiatr Serv. 2006;57(4):570-572. PubMed doi:10.1176/appi.ps.57.4.570
32. Forton DM, Taylor-Robinson SD, Thomas HC. Cerebral dysfunction in chronic hepatitis C infection. J Viral Hepat. 2003;10(2):81-86. PubMed doi:10.1046/j.1365-2893.2003.00416.x
33. Forton DM, Thomas HC, Taylor-Robinson SD. Central nervous system involvement in hepatitis C virus infection. Metab Brain Dis. 2004;19(3-4):383-391. PubMed doi:10.1023/B:MEBR.0000043983.42843.ac
34. Weissenborn K, Tryc AB, Heeren M, et al. Hepatitis C virus infection and the brain. Metab Brain Dis. 2009;24(1):197-210. PubMed doi:10.1007/s11011-008-9130-5
35. Poynard T, Cacoub P, Ratziu V, et al. Multivirc group. Fatigue in patients with chronic hepatitis C. J Viral Hepat. 2002;9(4):295-303. PubMed doi:10.1046/j.1365-2893.2002.00364.x
36. Huckans M, Seelye A, Parcel T, et al. The cognitive effects of hepatitis C in the presence and absence of a history of substance use disorder. J Int Neuropsychol Soc. 2009;15(1):69-82. PubMed doi:10.1017/S1355617708090085
37. Forton DM, Thomas HC, Murphy CA, et al. Hepatitis C and cognitive impairment in a cohort of patients with mild liver disease. Hepatology. 2002;35(2):433-439. PubMed doi:10.1053/jhep.2002.30688
38. Weissenborn K, Krause J, Bokemeyer M, et al. Hepatitis C virus infection affects the brain-evidence from psychometric studies and magnetic resonance spectroscopy. J Hepatol. 2004;41(5):845-851. PubMed doi:10.1016/j.jhep.2004.07.022
39. Lowry D, Coughlan B, McCarthy O, et al. Investigating health-related quality of life, mood and neuropsychological test performance in a homogeneous cohort of Irish female hepatitis C patients. J Viral Hepat. 2010;17(5):352-359. PubMed doi:10.1111/j.1365-2893.2009.01188.x
40. Radkowski M, Gallegos-Orozco JF, Jablonska J, et al. Persistence of hepatitis C virus in patients successfully treated for chronic hepatitis C. Hepatology. 2005;41(1):106-114. PubMed doi:10.1002/hep.20518
41. Vargas HE, Laskus T, Radkowski M, et al. Detection of hepatitis C virus sequences in brain tissue obtained in recurrent hepatitis C after liver transplantation. Liver Transpl. 2002;8(11):1014-1019. PubMed doi:10.1053/jlts.2002.36393
42. Radkowski M, Wilkinson J, Nowicki M, et al. Search for hepatitis C virus negative-strand RNA sequences and analysis of viral sequences in the central nervous system: evidence of replication. J Virol. 2002;76(2):600-608. PubMed doi:10.1128/JVI.76.2.600-608.2002
43. Laskus T, Radkowski M, Bednarska A, et al. Detection and analysis of hepatitis C virus sequences in cerebrospinal fluid. J Virol. 2002;76(19):10064-10068. PubMed doi:10.1128/JVI.76.19.10064-10068.2002
44. Forton DM, Karayiannis P, Mahmud N, et al. Identification of unique hepatitis C virus quasispecies in the central nervous system and comparative analysis of internal translational efficiency of brain, liver, and serum variants. J Virol. 2004;78(10):5170-5183. PubMed doi:10.1128/JVI.78.10.5170-5183.2004
45. Forton DM, Allsop JM, Main J, et al. Evidence for a cerebral effect of the hepatitis C virus. Lancet. 2001;358(9275):38-39. PubMed doi:10.1016/S0140-6736(00)05270-3
46. Forton DM, Wright M, Knapp S, et al. New insights into hepatitis C. Clin Med. 2002;2(6):554-559. PubMed
47. el-Serag HB, Kunik M, Richardson P, et al. Psychiatric disorders among veterans with hepatitis C infection. Gastroenterology. 2002;123(2):476-482. PubMed doi:10.1053/gast.2002.34750
48. Lehman CL, Cheung RC. Depression, anxiety, post-traumatic stress, and alcohol-related problems among veterans with chronic hepatitis C. Am J Gastroenterol. 2002;97(10):2640-2646. PubMed doi:10.1111/j.1572-0241.2002.06042.x
49. Regier DA, Narrow WE, Rae DS, et al. The de facto US mental and addictive disorders service system: epidemiologic catchment area prospective 1-year prevalence rates of disorders and services. Arch Gen Psychiatry. 1993;50(2):85-94. PubMed
50. Norquist GS, Regier DA. The epidemiology of psychiatric disorders and the de facto mental health care system. Annu Rev Med. 1996;47:473-479. PubMed doi:10.1146/annurev.med.47.1.473
51. Al Jurdi RK, Burruss JW. Prevalence of hepatitis C in psychiatric institutions. Psychosomatics. 2003;44(5):439-440. PubMed doi:10.1176/appi.psy.44.5.439
52. Sabouni D, Rifai MA, Moles JK, et al. Hepatitis C treatment eligibility and outcomes in patients with psychiatric illness. Am J Gastroenterol. 2005;100(9):S117-S118. doi:10.1111/j.1572-0241.2005.001_5.x
53. Nakamura Y, Koh M, Miyoshi E, et al. High prevalence of the hepatitis C virus infection among the inpatients of schizophrenia and psychoactive substance abuse in Japan. Prog Neuropsychopharmacol Biol Psychiatry. 2004;28(3):591-597. PubMed doi:10.1016/j.pnpbp.2004.01.018
54. Chang TT, Lin H, Yen YS, et al. Hepatitis B and hepatitis C among institutionalized psychiatric patients in Taiwan. J Med Virol. 1993;40(2):170-173. PubMed doi:10.1002/jmv.1890400216
55. Eveillard M, Daroukh A, Desjardins P, et al. Seroprevalence of hepatitis B and C viruses in a psychiatric institution. Pathol Biol (Paris). 1999;47(5):543-548. PubMed
56. Kakisi OK, Grammatikos AA, Karageorgopoulos DE, et al. Prevalence of hepatitis B, hepatitis C, and HIV infections among patients in a psychiatric hospital in Greece. Psychiatr Serv. 2009;60(9):1269-1272. PubMed doi:10.1176/appi.ps.60.9.1269
57. Cividini A, Pistorio A, Regazzetti A, et al. Hepatitis C virus infection among institutionalised psychiatric patients: a regression analysis of indicators of risk. J Hepatol. 1997;27(3):455-463. PubMed doi:10.1016/S0168-8278(97)80348-0
58. Sawayama Y, Hayashi J, Kakuda K, et al. Hepatitis C virus infection in institutionalized psychiatric patients: possible role of transmission by razor sharing. Dig Dis Sci. 2000;45(2):351-356. PubMed doi:10.1023/A:1005472812403
59. Stroffolini T, Marchi L, Brunetti E, et al. Lack of hepatitis C transmission among institutionalized psychiatric patients. J Hepatol. 2003;38(2):244. PubMed doi:10.1016/S0168-8278(02)00355-0
60. Huckans MS, Blackwell AD, Harms TA, et al. Management of hepatitis C disease among VA patients with schizophrenia and substance use disorders. Psychiatr Serv. 2006;57(3):403-406. PubMed doi:10.1176/appi.ps.57.3.403
61. Huckans M, Mitchell A, Ruimy S, et al. Antiviral therapy completion and response rates among hepatitis C patients with and without schizophrenia. Schizophr Bull. 2010;36(1):165-172. PubMed doi:10.1093/schbul/sbn065
62. Crone CC, Gabriel GM, Wise TN. Managing the neuropsychiatric side effects of interferon-based therapy for hepatitis C. Cleve Clin J Med. 2004;71(suppl 3):S27-S32. PubMed doi:10.3949/ccjm.71.Suppl_3.S27
63. Crone C, Gabriel GM. Comprehensive review of hepatitis C for psychiatrists: risks, screening, diagnosis, treatment, and interferon-based therapy complications. J Psychiatr Pract. 2003;9(2):93-110. PubMed doi:10.1097/00131746-200303000-00002
64. Flamm SL. Chronic hepatitis C virus infection. JAMA. 2003;289(18):2413-2417. PubMed doi:10.1001/jama.289.18.2413
65. Alter MJ, Kuhnert WL, Finelli L. Centers for Disease Control and Prevention. Guidelines for laboratory testing and result reporting of antibody to hepatitis C virus. MMWR Recomm Rep. 2003;52(RR-3):1-13, 15, quiz CE1-CE4. PubMed
66. Allen SA, Spaulding AC, Osei AM, et al. Treatment of chronic hepatitis C in a state correctional facility. Ann Intern Med. 2003;138(3):187-190. PubMed
67. Rifai MA, Moles JK, Lehman LP, et al. Hepatitis C screening and treatment outcomes in patients with substance use/dependence disorders. Psychosomatics. 2006;47(2):112-121. PubMed doi:10.1176/appi.psy.47.2.112
68. Rifai MA, Loftis JM, Hauser P. Hepatitis C treatment of veterans with psychiatric illness. Am J Gastroenterol. 2006;101(3):673-674, author reply 674-675. PubMed doi:10.1111/j.1572-0241.2006.473_3.x
69. Chou R, Clark EC, Helfand M. US Preventive Services Task Force. Screening for hepatitis C virus infection: a review of the evidence for the US Preventive Services Task Force. Ann Intern Med. 2004;140(6):465-479. PubMed
70. Strader DB, Wright T, Thomas DL, et al. American Association for the Study of Liver Diseases. Diagnosis, management, and treatment of hepatitis C. Hepatology. 2004;39(4):1147-1171. PubMed doi:10.1002/hep.20119
71. Wong JB, McQuillan GM, McHutchison JG, et al. Estimating future hepatitis C morbidity, mortality, and costs in the United States. Am J Public Health. 2000;90(10):1562-1569. PubMed doi:10.2105/AJPH.90.10.1562
72. Duberg AS, Törner A, Davidsdóttir L, et al. Cause of death in individuals with chronic HBV and/or HCV infection, a nationwide community-based register study. J Viral Hepat. 2008;15(7):538-550. PubMed doi:10.1111/j.1365-2893.2008.00982.x
73. Rifai MA, Moles JK, Van der Linden BJ. Hepatitis C and post-traumatic stress disorder in US veterans. Am J Gastroenterol. 98(9 suppl 1):S99-S100.
74. Dan AA, Martin LM, Crone C, et al. Depression,anemia and health-related quality of life in chronic hepatitis C. J Hepatol. 2006;44(3):491-498. PubMed doi:10.1016/j.jhep.2005.11.046
75. Rifai MA. To screen or not to screen for hepatitis C. Psychiatr Serv. 2010;61(3):325-326
76. National Institutes of Health. National Institutes of Health Consensus Development Conference Statement: Management of hepatitis C: 2002: June 10-12, 2002. Hepatology. 2002;36(suppl 1):S3-S20. PubMed doi:10.1002/hep.1840360703
77. Sulkowski MS, Thomas DL. Hepatitis C in the HIV-infected person. Ann Intern Med. 2003;138(3):197-207. PubMed
78. Peters MG, Terrault NA. Alcohol use and hepatitis C. Hepatology. 2002;36(suppl 1):S220-S225. PubMed doi:10.1002/hep.1840360728
79. Lieber CS. Hepatitis C and alcohol. J Clin Gastroenterol. 2003;36(2):100-102. PubMed doi:10.1097/00004836-200302000-00003
80. Anand BS, Currie S, Dieperink E, et al. VA-HCV-001 Study Group. Alcohol use and treatment of hepatitis C virus: results of a national multicenter study. Gastroenterology. 2006;130(6):1607-1616. PubMed doi:10.1053/j.gastro.2006.02.023
81. Rifai MA, Rosestein DL. Interferon treatment of hepatitis C patients with psychiatric disorders: evidence-based, risk-benefit assessment. Psychosomatics. 2005;46(2):165-166.
82. Rifai MA, Bozorg B, Rosenstein DL. Interferon for hepatitis C patients with psychiatric disorders. Am J Psychiatry. 2004;161(12):2331-2332, author reply 2332-2334. PubMed doi:10.1176/appi.ajp.161.12.2331
83. Rifai MA, Loftis JM, Hauser P. Interferon-alpha treatment of patients with Hepatitis C: the role of a comprehensive risk-benefit assessment. CNS Drugs. 2005;19(8):719-721, author reply 721-722. PubMed doi:10.2165/00023210-200519080-00009
84. Rifai MA. Ethical impasses in the care of patients with hepatitis C. Psychosomatics. 2006;47(6):540-541. PubMed doi:10.1176/appi.psy.47.6.540
85. Rifai MA, Rosestein DL. Hepatitis C and psychiatry. Focus. 2005;3:194-202.
86. Ho SB, Groessl E, Dollarhide A, et al. Management of chronic hepatitis C in veterans: the potential of integrated care models. Am J Gastroenterol. 2008;103(7):1810-1823. PubMed doi:10.1111/j.1572-0241.2008.01877.x
87. Knott A, Dieperink E, Willenbring ML, et al. Integrated psychiatric/medical care in a chronic hepatitis C clinic: effect on antiviral treatment evaluation and outcomes. Am J Gastroenterol. 2006;101(10):2254-2262. PubMed doi:10.1111/j.1572-0241.2006.00731.x
88. Rifai MA. Interferon-alpha treatment of hepatitis C patients with psychiatric illness: evidence-based risk-benefit assessment [letter]. Prim Care Companion J Clin Psychiatry. 2005;7(2):74-75. PubMed doi:10.4088/PCC.v07n0207b
89. Rifai MA, Indest D, Loftis J, et al. Psychiatric management of the hepatitis C patient. Curr Treat Options Gastroenterol. 2006;9(6):508-519. PubMed doi:10.1007/s11938-006-0007-6
90. Geppert CMA, Dettmer E, Jakiche A. Ethical challenges in the care of persons with hepatitis C infection: a pilot study to enhance informed consent with veterans. Psychosomatics. 2005;46(5):392-401. PubMed doi:10.1176/appi.psy.46.5.392
91. Gleason O, Fucci J, Yates W. Gastroenterologists’ perceptions of need and availability of psychiatric services for patients with hepatitis C. Psychosomatics. 2008;49(2):132-136. PubMed doi:10.1176/appi.psy.49.2.132
92. Falck-Ytter Y, Kale H, Mullen KD, et al. Surprisingly small effect of antiviral treatment in patients with hepatitis C. Ann Intern Med. 2002;136(4):288-292. PubMed
93. Cawthorne CH, Rudat KR, Burton MS, et al. Limited success of HCV antiviral therapy in United States veterans. Am J Gastroenterol. 2002;97(1):149-155. PubMed
94. Hauser P, Morasco BJ, Linke A, et al. Antiviral completion rates and sustained viral response in hepatitis C patients with and without preexisting major depressive disorder. Psychosomatics. 2009;50(5):500-505. PubMed doi:10.1176/appi.psy.50.5.500
95. Silberbogen AK, Ulloa EW, Janke EA, et al. Psychosocial issues and mental health treatment recommendations for patients with hepatitis C. Psychosomatics. 2009;50(2):114-122. PubMed doi:10.1176/appi.psy.50.2.114
96. Fleming CA, Craven DE, Thornton D, et al. Hepatitis C virus and human immunodeficiency virus coinfection in an urban population: low eligibility for interferon treatment. Clin Infect Dis. 2003;36(1):97-100. PubMed doi:10.1086/344907
97. Strader DB. Understudied populations with hepatitis C. Hepatology. 2002;36(suppl 1):S226-S236. PubMed doi:10.1002/hep.1840360729
98. Taylor LE, Costello T, Alt E, et al. Psychiatric illness and illicit drugs as barriers to hepatitis C treatment among HIV/hepatitis C virus co-infected individuals. AIDS. 2002;16(12):1700-1701. PubMed doi:10.1097/00002030-200208160-00024
99. Schaefer M, Schmidt F, Folwaczny C, et al. Adherence and mental side effects during hepatitis C treatment with interferon alfa and ribavirin in psychiatric risk groups. Hepatology. 2003;37(2):443-451. PubMed doi:10.1053/jhep.2003.50031
100. Fried R, Monnat M, Seidenberg A, et al. Swiss multicenter study evaluating the efficacy, feasibility and safety of peginterferon-alfa-2a and ribavirin in patients with chronic hepatitis C in official opiate substitution programs. Digestion. 2008;78(2-3):123-130. PubMed doi:10.1159/000173733
101. Dell’ Osso L, Pini S, Maggi L, et al. Subthreshold mania as predictor of depression during interferon treatment in HCV+ patients without current or lifetime psychiatric disorders. J Psychosom Res. 2007;62(3):349-355. PubMed doi:10.1016/j.jpsychores.2006.10.024
102. Schaefer M, Schmidt F, Horn M, et al. Depression during treatment with interferon alpha. Psychosomatics. 2004;45(2):176. PubMed doi:10.1176/appi.psy.45.2.176
103. Schaefer M, Heinz A, Backmund M. Treatment of chronic hepatitis C in patients with drug dependence: time to change the rules? Addiction. 2004;99(9):1167-1175. PubMed doi:10.1111/j.1360-0443.2004.00821.x
104. Schäfer M, Schwaiger M. Incidence, pathoetiology and treatment of interferon-alpha induced neuro-psychiatric side effects. Fortschr Neurol Psychiatr. 2003;71(9):469-476. PubMed
105. Alvarez-Uria G, Day JN, Nasir AJ, et al. Factors associated with treatment failure of patients with psychiatric diseases and injecting drug users in the treatment of genotype 2 or 3 hepatitis C chronic infection. Liver Int. 2009;29(7):1051-1055. PubMed doi:10.1111/j.1478-3231.2008.01958.x
106. Rifai MA. Hepatitis C treatment of patients with bipolar disorder: a case series. Prim Care Companion J Clin Psychiatry. 2006;8(6):361-366. PubMed doi:10.4088/PCC.v08n0607
107. Gohier B, Goeb JL, Rannou-Dubas K, et al. Hepatitis C, alpha interferon, anxiety and depression disorders: a prospective study of 71 patients. World J Biol Psychiatry. 2003;4(3):115-118. PubMed doi:10.1080/15622970310029904
108. Kraus MR, Schäfer A, Faller H, et al. Psychiatric symptoms in patients with chronic hepatitis C receiving interferon alfa-2b therapy. J Clin Psychiatry. 2003;64(6):708-714. PubMed doi:10.4088/JCP.v64n0614
109. Kraus MR, Schäfer A, Faller H, et al. Paroxetine for the treatment of interferon-alpha-induced depression in chronic hepatitis C. Aliment Pharmacol Ther. 2002;16(6):1091-1099. PubMed doi:10.1046/j.1365-2036.2002.01265.x
110. Schaefer M, Engelbrecht MA, Gut O, et al. Interferon alpha (IFNalpha) and psychiatric syndromes: a review. Prog Neuropsychopharmacol Biol Psychiatry. 2002;26(4):731-746. PubMed doi:10.1016/S0278-5846(01)00324-4
111. Dan AA, Crone C, Wise TN, et al. Anger experiences among hepatitis C patients: relationship to depressive symptoms and health-related quality of life. Psychosomatics. 2007;48(3):223-229. PubMed doi:10.1176/appi.psy.48.3.223
112. Constant A, Castera L, Quintard B, et al. Psychosocial factors associated with perceived disease severity in patients with chronic hepatitis C: relationship with information sources and attentional coping styles. Psychosomatics. 2005;46(1):25-33. PubMed doi:10.1176/appi.psy.46.1.25
113. Constant A, Castera L, Dantzer R, et al. Mood alterations during interferon-alfa therapy in patients with chronic hepatitis C: evidence for an overlap between manic/hypomanic and depressive symptoms. J Clin Psychiatry. 2005;66(8):1050-1057. PubMed doi:10.4088/JCP.v66n0814
114. Dieperink E, Ho SB, Tetrick L, et al. Suicidal ideation during interferon-alpha2b and ribavirin treatment of patients with chronic hepatitis C. Gen Hosp Psychiatry. 2004;26(3):237-240. PubMed doi:10.1016/j.genhosppsych.2004.01.003
115. Ademmer K, Beutel M, Bretzel R, et al. Suicidal ideation with IFN-alpha and ribavirin in a patient with hepatitis C. Psychosomatics. 2001;42(4):365-367. PubMed doi:10.1176/appi.psy.42.4.365
116. Gochee PA, Powell EE, Purdie DM, et al. Association between apolipoprotein E epsilon4 and neuropsychiatric symptoms during interferon alpha treatment for chronic hepatitis C. Psychosomatics. 2004;45(1):49-57. PubMed doi:10.1176/appi.psy.45.1.49
117. Lotrich FE, Ferrell RE, Rabinovitz M, et al. Risk for depression during interferon-alpha treatment is affected by the serotonin transporter polymorphism. Biol Psychiatry. 2009;65(4):344-348. PubMed doi:10.1016/j.biopsych.2008.08.009
118. Yoshida K, Alagbe O, Wang X, et al. Promoter polymorphisms of the interferon-alpha receptor gene and development of Interferon-induced depressive symptoms in patients with chronic hepatitis C: preliminary findings. Neuropsychobiology. 2005;52(2):55-61. PubMed doi:10.1159/000086605
119. Kraus MR, Al-Taie O, Schäfer A, et al. Serotonin-1A receptor gene HTR1A variation predicts interferon-induced depression in chronic hepatitis C. Gastroenterology. 2007;132(4):1279-1286. PubMed doi:10.1053/j.gastro.2007.02.053
120. Prather AA, Rabinovitz M, Pollock BG, et al. Cytokine-induced depression during IFN-alpha treatment: the role of IL-6 and sleep quality. Brain Behav Immun. 2009;23(8):1109-1116. PubMed doi:10.1016/j.bbi.2009.07.001
121. Thome J, Knopf U. Acute psychosis after injection of pegylated interferon alpha-2a. Eur Psychiatry. 2003;18(3):142-143. PubMed doi:10.1016/S0924-9338(03)00032-4
122. Quarantini LC, Cruz SC, Batista-Neves SC, et al. Psychosis during peginterferon-alpha 2a and ribavirin therapy: case report. Braz J Infect Dis. 2006;10(6):406-407. PubMed doi:10.1590/S1413-86702006000600010
123. Telio D, Sockalingam S, Stergiopoulos V. Persistent psychosis after treatment with interferon alpha: a case report. J Clin Psychopharmacol. 2006;26(4):446-447. PubMed doi:10.1097/01.jcp.0000227348.59912.5d
124. Gleason OC, Fucci JC, Yates WR, et al. Preventing relapse of major depression during interferon-alpha therapy for hepatitis C—a pilot study. Dig Dis Sci. 2007;52(10):2557-2563. PubMed doi:10.1007/s10620-006-9729-5
125. Morasco BJ, Rifai MA, Loftis JM, et al. A randomized trial of paroxetine to prevent interferon-alpha-induced depression in patients with hepatitis C. J Affect Disord. 2007;103(1-3):83-90. PubMed doi:10.1016/j.jad.2007.01.007
126. Schaefer M, Schwaiger M, Garkisch AS, et al. Prevention of interferon-alpha associated depression in psychiatric risk patients with chronic hepatitis C. J Hepatol. 2005;42(6):793-798. PubMed doi:10.1016/j.jhep.2005.01.020
127. Raison CL, Woolwine BJ, Demetrashvili MF, et al. Paroxetine for prevention of depressive symptoms induced by interferon-alpha and ribavirin for hepatitis C. Aliment Pharmacol Ther. 2007;25(10):1163-1174. PubMed
128. Kraus MR, Schäfer A, Al-Taie O, et al. Prophylactic SSRI during interferon alpha re-therapy in patients with chronic hepatitis C and a history of interferon-induced depression. J Viral Hepat. 2005;12(1):96-100. PubMed doi:10.1111/j.1365-2893.2005.00554.x
129. Hejny C, Sternberg P, Lawson DH, et al. Retinopathy associated with high-dose interferon alfa-2b therapy. Am J Ophthalmol. 2001;131(6):782-787. PubMed doi:10.1016/S0002-9394(01)00836-4
130. Loftis JM, Hauser P. Safety of the treatment of interferon-alpha-induced depression. Psychosomatics. 2003;44(6):524-526. PubMed doi:10.1176/appi.psy.44.6.524
131. Ozcanli T, Unsalver B, Ozdemir S, et al. Sertraline- and mirtazapine-induced severe neutropenia. Am J Psychiatry. 2005;162(7):1386. PubMed doi:10.1176/appi.ajp.162.7.1386
132. Choi S. Nefazodone (Serzone) withdrawn because of hepatotoxicity. CMAJ. 2003;169(11):1187. PubMed
133. Rosenberg SD, Goodman LA, Osher FC, et al. Prevalence of HIV, hepatitis B, and hepatitis C in people with severe mental illness. Am J Public Health. 2001;91(1):31-37. PubMed
134. Rosenberg SD, Swanson JW, Wolford GL, et al. Five-Site Health and Risk Study Research Committee. The five-site health and risk study of blood-borne infections among persons with severe mental illness. Psychiatr Serv. 2003;54(6):827-835. PubMed doi:10.1176/appi.ps.54.6.827