Residual Symptoms and Relapse: Mood, Cognitive Symptoms, and Sleep Disturbances
Remission is the standard of care in major depressive disorder (MDD). However, even in patients who respond to treatment and achieve remission, residual symptoms significantly inhibit functionality and increase the risk of relapse and recurrence. The most common residual symptoms are fatigue, sleep problems, and cognitive dysfunction. Clinicians should be cognizant of these potential residual symptoms and the unique ways in which they present in patients with MDD. Treating these symptoms as target symptoms from baseline increases the patient’s chances of an asymptomatic remission. Making use of clinically practical screening instruments and monitoring these target symptoms throughout the course of treatment can improve patients’ functional recovery.
(J Clin Psychiatry 2013;74[suppl 2]:9-13)
From the Department of Psychiatry, Rush University Medical Center, Chicago, Illinois.
This article is derived from the planning teleconference series "Depression: Managing the Full Range of Symptoms to Achieve Lasting Remission," which was held in May and June 2013 and supported by an educational grant from Takeda Pharmaceuticals International, Inc., US Region and Lundbeck.
Dr Zajecka has received grants/research support from AstraZeneca, Cyberonics, Euthymics, Hoffmann-LaRoche, the National Institute of Mental Health, Otsuka, Shire, and Takeda and has served as a consultant for Abbott, Eli Lilly, Otsuka, Pamlab, Shire, and Takeda.
Corresponding author: John M. Zajecka, MD, 1700 W Van Buren St, 5th Floor, Chicago, IL 60612 ([email protected]).
doi:10.4088/JCP.12084su1c.02
© Copyright 2013 Physicians Postgraduate Press, Inc.
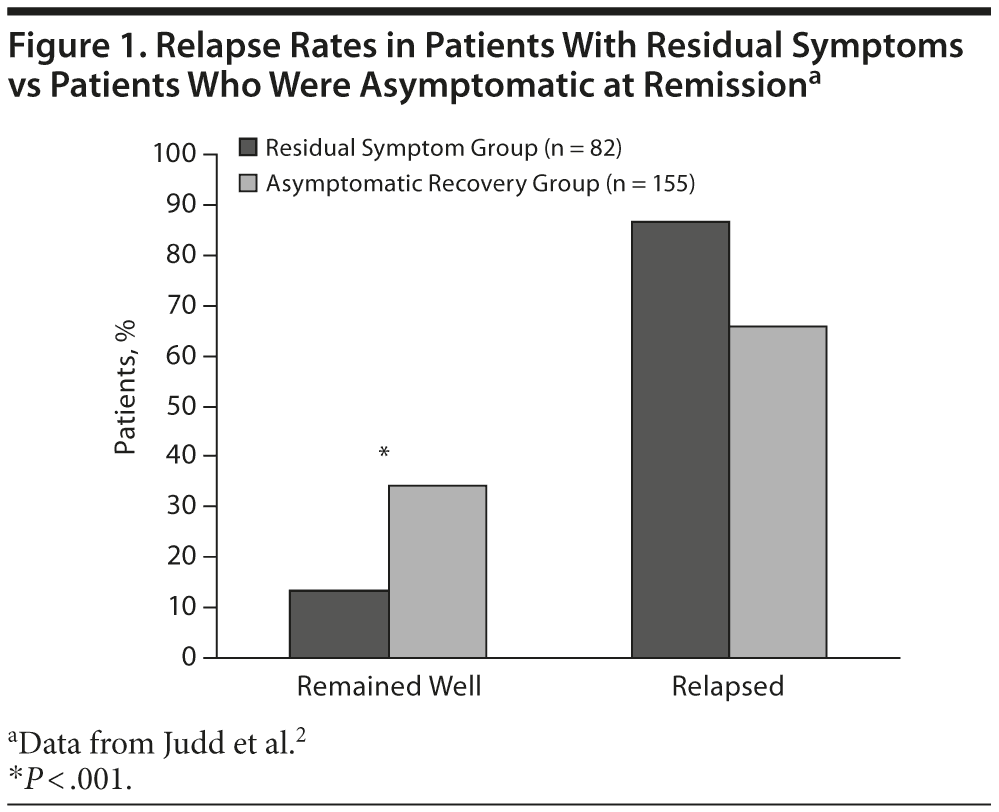
Although remission has become the standard of care in treating major depressive disorder (MDD), remission is difficult to define consistently.1 Full remission should mean that the patient has experienced the resolution of all symptoms of depression and the restoration of occupational, educational, interpersonal, and psychosocial functioning to a premorbid state. Clinical studies, however, often allow patients to have some remaining (or residual) symptoms and still be considered to be in remission. When patients achieve and sustain asymptomatic remission, they have a lower risk of relapse than patients who are considered to be in remission but have residual symptoms (Figure 1).2,3 In fact, versus having a history of recurrent depressive episodes, residual symptoms are associated with a greater risk of relapse.2 In the Sequenced Treatment Alternatives to Relieve Depression trials (STAR*D), greater number of residual symptom domains was associated with an increased probability of relapse.4 As with treating chronic medical conditions such as hypertension and diabetes, clinicians treating MDD should be cognizant of and assess for any risk factors that may contribute to relapse and recurrence, including residual symptoms.
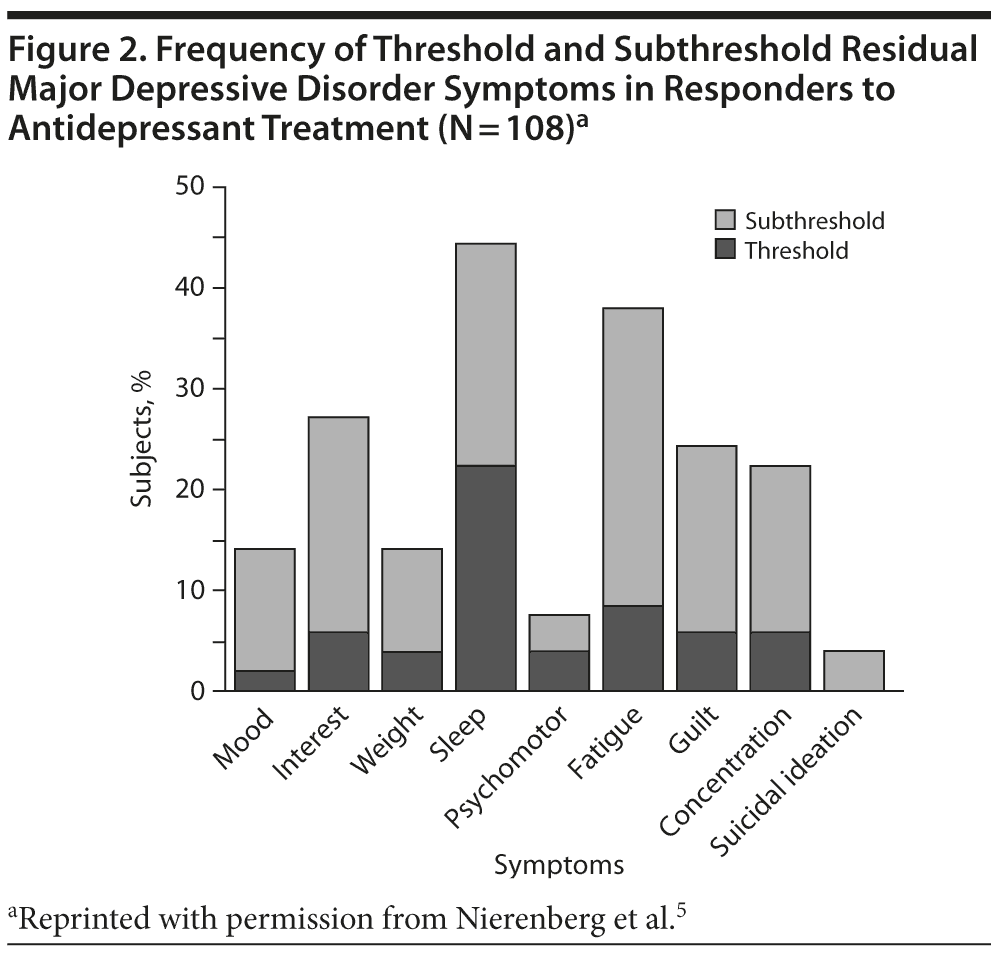
Certain types of residual symptoms are more common than others. For example, in a study by Nierenberg et al,5 the most common residual symptoms among patients who had technically achieved remission (defined as a Hamilton Depression Rating Scale [HDRS] score ≤ 7) were sleep problems (44%) and fatigue (38%), followed by lack of interest, guilt, and concentration problems (Figure 2). A number of studies6-9 have reported the persistence of fatigue or sleep problems and impairment in cognitive functioning in continuation and maintenance treatment phases.8 Because distinguishing residual symptoms from side effects of medication can be challenging, physicians must work with patients before beginning treatment to systematically identify the target symptoms that should be assessed throughout all stages of treatment.
Residual Fatigue and Sleep Symptoms
Patients who have MDD often complain of sustained fatigue without any physical exertion. They may find it difficult to perform even basic minor tasks, feeling that those tasks require more energy than they have. These patients may subsequently complain that they take longer than others to complete ordinary activities of daily living. In fact, in a 3-year prospective study of depressed primary care patients, Conradi et al9 found that lack of energy and sleep disturbances accounted for 2 of the 3 most common symptoms that persisted throughout the study. Patients experiencing a major depressive episode (MDE) reported lack of energy 90% of the time and sleep problems 85% of the time. In patients who remitted, lack of energy persisted 35% of the time and sleep problems persisted 39% of the time, while the core symptoms of depression were present only 21% of the time.

- Identify target symptoms before initiating treatment to distinguish residual symptoms from other factors that might produce new-onset symptoms.
- Consult patients when identifying target symptoms. Because patients often present with MDD in different ways, think beyond DSM criteria when listening to patients.
- Intervene early when new-onset symptoms or side effects arise during treatment.
Even though fatigue is common, it can be difficult to assign a diagnosis to it. In an observational cohort study of 571 patients, Nijrolder et al10 found that a wide range of diagnoses were associated with fatigue in primary care. Psychological disorders were the second most common diagnostic category in the cohort and accounted for 16.5% of diagnoses. The researchers concluded that, since at least half of the patients in the cohort did not receive a diagnosis that explained their fatigue during the presentation or the 1-year follow-up, this symptom is a complex problem that deserves more attention.
Clinical Challenges
Various clinical challenges are associated with characterizing fatigue in general. First, no universally accepted definition of fatigue exists in medicine, and its presentation may vary over time within individuals.10,11 Second, few standardized ways to measure or assess fatigue are available, although sleep problems are fairly well defined and able to be assessed by objective measures.11 Third, patients may use language to describe their symptoms that does not fit clinicians’ ideas of fatigue-related symptoms described in diagnostic criteria such as the Diagnostic and Statistical Manual of Mental Disorders (DSM).
Even after fatigue has been identified, its cause can be difficult to pinpoint. One cause of fatigue and sleep problems may be side effects of medication. However, the clinician who identifies fatigue or sleep disruption before beginning depression treatment will be better able to rule out medication side effect as the cause. One study5 reported that 91.7% of those who had posttreatment symptoms of insomnia and 92.7% of those who had posttreatment symptoms of fatigue had pretreatment insomnia and fatigue, respectively.
Fatigue may be associated with stress and a variety of medical and psychiatric disorders, so it may not be necessarily identified by the patient or the clinician as one of the patient’s core depressive symptoms. A study by Fuhrer and Wessely12 found that, among 3,784 people who were seen by general practitioners, 41.2% of the patients had symptoms of persistent fatigue, but only 7.6% actually reported fatigue to their doctor. The investigators reported a strong relationship between fatigue and depression in this sample.
Fatigue and MDD
Fatigue has been studied as a predictor and residual symptom of MDD, as well as a symptom of MDE, and has been associated with other factors and conditions related to depression. The Baltimore Epidemiologic Catchment Area follow-up study13 found that both baseline and new-onset fatigue during the 13-year period were associated with a 28-fold greater risk of new-onset MDD compared with those without fatigue. Kroenke et al14 found that, among patients in 2 primary care clinics who identified fatigue as a major problem, 80% screened positive for MDD and/or somatic anxiety compared with 12% of those without fatigue.
Functional status is particularly affected when fatigue and depression co-occur.15 The impact of fatigue on function is related to but somewhat distinct from the severity (ie, experience) of fatigue.11,16 In patients with cancer, a pattern in which functional interference from fatigue was greater than the severity of fatigue helped predict which patients had MDD.17 Fatigue is cited as one of the symptoms of MDD most likely to cause occupational interference.18
Residual Cognitive Symptoms
Cognitive dysfunction is another common residual symptom in patients with MDD.8,9 As with fatigue and sleep problems, cognitive symptoms need to be distinguished from medication side effects. One study by Bolling et al6 examined the side effects of selective serotonin reuptake inhibitors (SSRIs) as factors in patients’ decisions to quit treatment. Of 161 patients, 30 (18.6%) reported apathy, 28 (17.4%) reported being unable to concentrate, and 21 (13.0%) reported memory loss. Iatrogenically induced cognitive problems could also occur with antihypertensive medications, chemotherapy, and many other medications.
Cognitive symptoms associated with depression tend to develop over a brief time unlike the more gradual decline in dementia. The clinician and the patient should work together to identify a temporal relationship. Systematically assessing symptoms before starting treatment makes it easier to identify target symptoms and determine whether they are truly a residual symptom of depression.
McClintock et al8 discovered that, among 428 patients whose depression responded but did not remit after 12 weeks of antidepressant treatment, 70.6% reported decreased concentration/reasoning as a symptom that persisted from baseline to exit. Cognitive impairment is an important treatment target in MDD because it is strongly correlated with physical, mental, and functional disability,19 as well as incomplete remission.20 Jaeger et al20 reported that deficits in neurocognitive domains were predictive of lack of functional recovery. Patients whose neurocognitive performance showed impairment at baseline and at 6-month follow-up had lower ratings of function at follow-up than those without cognitive deficits, independent of mood ratings. Naismith et al19 found that cognitive impairment was equally strongly predictive of physical impairment as depression severity was.
Cognitive symptoms are particularly problematic for patients whose work requires strong cognitive skills, such as academically or occupationally challenging roles.21 Cognitive symptoms such as concentration and memory problems (along with fatigue, low energy, and insomnia) are perceived to interfere most with occupational functioning in patients with MDD.18 For patients who begin psychotherapy for their depression, cognitive problems can keep them from becoming completely immersed in the psychotherapeutic process.
Cognitive symptoms can present in a wide variety of ways in patients with MDD, making them difficult to identify.7,21 As with fatigue, many patients may not recognize that these cognitive problems are related to their depression, so reports from significant others may be helpful in identifying these symptoms.21
Assessing Symptoms and Functioning
Identify Target Symptoms With Patients
Presentations of MDD vary from one patient to another. Each person has an individual expression of the illness. When evaluating the patient, clinicians should think beyond the DSM criteria, because many patients do not use DSM language and may describe symptoms outside of DSM criteria. Clinicians must ask patients to describe emotional, physical, and cognitive problems that they would like to target and see improve during treatment. These target symptoms should be assessed throughout the course of treatment. This approach allows patients to express in their own words how they experience depression and how they experience improvement over time. Identifying the patient’s full range of symptomatology at baseline also helps the clinician to track improvement of symptoms, be cognizant of any residual symptoms, and recognize new-onset symptoms during treatment.
At the beginning of treatment, clinicians should also ask their patients to define a premorbid time point by which they can gauge whether they have reached remission. That is, can they imagine a time when they did not have symptoms of depression and were fully functional in interpersonal relationships, work, and school? They will recognize remission by symptom control and full functionality in comparison with this previous time point.
Use Screening Instruments
When identifying target symptoms with patients at baseline and assessing them at follow-up, clinicians will benefit from a routine, systematic way of listing possible symptoms so that nothing is missed. A number of screening instruments have been developed for use in research and clinical practice. Current outcome measures, however, may fail to ascertain many common residual symptoms of treated MDD during acute and long-term treatment.
The Patient’s Health Questionnaire (PHQ)22 is a self-administered questionnaire that assesses common threshold and subthreshold DSM-IV disorders. The PHQ-9 is a 9-item depression module of the PHQ that determines whether symptoms of depression have been present over a 2-week period. This self-report questionnaire allows patients to take part in their symptom assessment, and, for the clinician, is quick (requires less than 3 minutes to review) and reliable. The PHQ-9 does not cover all aspects of MDD (including functional impairments), but it identifies symptoms that can prompt the clinician to ask about other symptoms as well as functioning.
Some depression scales that are widely used in clinical research may not be practical to use in clinical practice, such as the clinician-rated Hamilton Depression Rating Scale (HDRS),23 the Montgomery-Asberg Depression Rating Scale (MADRS),24 and the Inventory of Depressive Symptomatology (IDS).25 However, the self-rated version of the IDS, the 16-item Quick Inventory of Depressive Symptomatology-Self Report (QIDS-SR),26 is more suitable for clinical practice.
One scale that is helpful for assessing functional impairment is the Sheehan Disability Scale (SDS).27 The SDS is a 3-item tool that assesses the functioning of the patient in work/school, family, and social domains.
The Massachusetts General Hospital Cognitive and Physical Functioning Questionnaire (CPFQ)28 is helpful in assessing cognitive and executive function, physical symptoms, and fatigue in patients with mood and anxiety disorders. The CPFQ, a 7-item, self-rated scale with high reliability, is sensitive to symptomatic changes throughout the course of treatment.
While the HDRS, MADRS, and IDS may not be practical to use in clinical settings, they, like the DSM, can provide a framework for clinicians to elicit information from patients about a range of depressive symptoms. Clinically practical measurements like the SDS and the CPFQ can help clinicians and patients identify target symptoms at baseline and track those symptoms over time, identifying residual symptoms and their impact on the patients’ ability to achieve full remission and functional recovery.
Differential Diagnosis of Residual and new-Onset Symptoms
When faced with residual or new-onset symptoms, clinicians need to use a differential diagnostic approach to assess causes of these symptoms so that they can be addressed and the symptoms can be resolved. Various factors have the potential to cause new-onset or residual symptoms (Table 1).29
Antidepressant Tachyphylaxis
Patients who respond or remit with an SSRI or a serotonin-norepinephrine reuptake inhibitor (SNRI) may complain weeks or months later that they do not feel the same as when they first responded to the treatment. They may have developed apathy, decreased motivation, fatigue, sleepiness, dullness in cognitive function, and a feeling that it is difficult to laugh or cry.30 This phenomenon, known as antidepressant tachyphylaxis, increases the risk of recurrence in patient with MDD. Tachyphylaxis may be associated with a compensatory decrease of norepinephrine or dopamine due to the increase of serotonin in the brain. Both clinicians and patients commonly confuse iatrogenic effects of medication with antidepressant tachyphylaxis. Good questions to ask patients who begin to present with such symptoms are, "Do you feel blah?" and "When did this start?" If these symptoms are present, clinicians may consider switching to a broad-spectrum antidepressant that may prevent diminished norepinephrine and dopamine modulation in the brain.29,30 Additional options to manage this phenomenon are lowering the dose, as long as it is not at the cost of losing efficacy, or adding adjunctive treatment.
Inaccurate Diagnosis
Clinicians should always evaluate the accuracy of the diagnosis. For example, patients with bipolar disorder may be misdiagnosed with MDD, because a patient in a depressed stage of bipolar disorder may present with the same symptoms as a patient with unipolar major depression.29
Comorbid Disorders
Patients with depression are often treated on a long-term or lifelong basis. Therefore, clinicians need to also watch for the development of new-onset medical disorders, such as endocrine disorders (including thyroid abnormalities), rheumatologic disorders, neurologic conditions, cancer, and dementia. These medical disorders, rather than MDD, may be responsible for new-onset or residual symptoms.
In addition, fatigue and cognitive problems may be signs of comorbid psychiatric disorders.29 Clinicians should remain alert for substance use or withdrawal as the cause of any new-onset or residual symptoms. MDD also commonly co-occurs with anxiety disorders, attention-deficit/hyperactivity disorder, and sleep disorders, but the comorbidity may not have been apparent until the depression was treated. The treatment of a comorbid illness may also exacerbate antidepressant side effects.
Side Effects or Drug Interactions
A new-onset or residual symptom may also be a result of a drug interaction with other medications that the patient may be taking, including over-the-counter medications or medications prescribed by other clinicians. Clinicians should ask patients at each visit what medications they are taking along with their antidepressant medication.
Psychosocial Variables
Another differential diagnostic consideration for new-onset or residual symptom causes is psychosocial variables.29 When depression improves, patients may resume activities, such as returning to work or school, which can produce new life stressors. Clinicians should assess for these psychosocial variables throughout treatment.
Adherence Issues
Most importantly, clinicians should regularly assess patients for lack of adherence. When patients begin to feel better, they may decide to cut back on their medications, especially if cost is an issue. Patients who miss doses or stop their antidepressants abruptly could experience discontinuation phenomena. These physical symptoms, such as fatigue and flu-like symptoms, can easily be confused with residual symptoms of depression.31 Patients may also experience cognitive symptoms and mood symptoms, such as dysphoria or irritability. All of these can be easily misinterpreted as a new-onset depressive symptom or a relapse, so it is important to make sure that the symptoms are not a result of decreasing or stopping the pharmacologic treatment.
Managing Residual Symptoms
For patients to achieve and sustain asymptomatic remission, clinicians must help them manage residual symptoms (Table 2). Identifying baseline target symptoms with the patient is the most important component of managing residual symptoms because this allows the clinician to distinguish new symptoms from residual symptoms. Tools such as laboratory work and neuropsychological testing can be used in the differential diagnosis of symptoms such as fatigue and cognitive impairment, and assessment tools should be used to monitor treatment effectiveness over time. Clinicians should intervene early when new-onset symptoms or side effects arise during treatment. If medication may be contributing to the symptoms, consider reducing the dose of the medication or adding an adjunctive therapy, whether that is pharmacologic therapy or psychotherapy. Clinicians should also consider switching to a different pharmacologic class of antidepressants for patients who present with residual symptoms.
Reconceptualizing the Approach to Depression Treatment
Not all symptoms of depression respond the same way to treatment. For example, why do symptoms of fatigue linger in many patients when their mood improves during treatment for MDD? Why do cognitive problems often not respond to conventional treatments like the other core depressive symptoms? The acute treatment of depression can result in an early improvement of core symptoms of depression, such as mood, appetite, helplessness, and guilt. However, symptoms such as fatigue, cognitive problems, and sleep problems are commonly experienced even after remission of the other core depressive symptoms. Incomplete remission can hinder functional recovery and contribute to relapse. Therefore, clinicians must modify their approach to achieving remission from MDD to include all symptoms and restoration of functioning.
Disclosure of off-label usage: Dr Zajecka has determined that, to the best of his knowledge, no investigational information about pharmaceutical agents that is outside US Food and Drug Administration-approved labeling has been presented in this activity.
References
1. Rush AJ, Kraemer HC, Sackeim HA, et al. Report by the ACNP Task Force on response and remission in major depressive disorder. Neuropsychopharmacology. 2006;31(9):1841-1853. PubMed doi:10.1038/sj.npp.1301131
2. Judd LL, Akiskal HS, Maser JD, et al. Major depressive disorder: a prospective study of residual subthreshold depressive symptoms as predictor of rapid relapse. J Affect Disord. 1998;50(2-3):97-108. PubMed doi:10.1016/S0165-0327(98)00138-4
3. Judd LL, Paulus MJ, Schettler PJ, et al. Does incomplete recovery from first lifetime major depressive episode herald a chronic course of illness? Am J Psychiatry. 2000;157(9):1501-1504. PubMed doi:10.1176/appi.ajp.157.9.1501
4. Nierenberg AA, Husain MM, Trivedi MH, et al. Residual symptoms after remission of major depressive disorder with citalopram and risk of relapse: a STAR*D report. Psychol Med. 2010;40(1):41-50. PubMed doi:10.1017/S0033291709006011
5. Nierenberg AA, Keefe BR, Leslie VC, et al. Residual symptoms in depressed patients who respond acutely to fluoxetine. J Clin Psychiatry. 1999;60(4):221-225. PubMed doi:10.4088/JCP.v60n0403
6. Bolling MY, Kohlenberg RJ. Reasons for quitting serotonin reuptake inhibitor therapy: paradoxical psychological side effects and patient satisfaction. Psychother Psychosom. 2004;73(6):380-385. PubMed doi:10.1159/000080392
7. Fava M, Graves LM, Benazzi F, et al. A cross-sectional study of the prevalence of cognitive and physical symptoms during long-term antidepressant treatment. J Clin Psychiatry. 2006;67(11):1754-1759. PubMed doi:10.4088/JCP.v67n1113
8. McClintock SM, Husain MM, Wisniewski SR, et al. Residual symptoms in depressed outpatients who respond by 50% but do not remit to antidepressant medication. J Clin Psychopharmacol. 2011;31(2):180-186. PubMed doi:10.1097/JCP.0b013e31820ebd2c
9. Conradi HJ, Ormel J, de Jonge P. Presence of individual (residual) symptoms during depressive episodes and periods of remission: a 3-year prospective study. Psychol Med. 2011;41(6):1165-1174. PubMed doi:10.1017/S0033291710001911
10. Nijrolder I, van der Windt D, de Vries H, et al. Diagnoses during follow-up of patients presenting with fatigue in primary care. CMAJ. 2009;181(10):683-687. PubMed
11. Neu D, Linkowski P, le Bon O. Clinical complaints of daytime sleepiness and fatigue: how to distinguish and treat them, especially when they become ‘ excessive’ or ‘ chronic’ ? Acta Neurol Belg. 2010;110(1):15-25. PubMed
12. Fuhrer R, Wessely S. The epidemiology of fatigue and depression: a French primary-care study. Psychol Med. 1995;25(5):895-905. PubMed doi:10.1017/S0033291700037387
13. Addington AM, Gallo JJ, Ford DE, et al. Epidemiology of unexplained fatigue and major depression in the community: the Baltimore ECA follow-up, 1981-1994. Psychol Med. 2001;31(6):1037-1044. PubMed doi:10.1017/S0033291701004214
14. Kroenke K, Wood DR, Mangelsdorff AD, et al. Chronic fatigue in primary care. Prevalence, patient characteristics, and outcome. JAMA. 1988;260(7):929-934. PubMed doi:10.1001/jama.1988.03410070057028
15. Leone SS. A disabling combination: fatigue and depression. Br J Psychiatry. 2010;197(2):86-87. PubMed doi:10.1192/bjp.bp.109.076604
16. Matza LS, Phillips GA, Revicki DA, et al. Development and validation of a patient-report measure of fatigue associated with depression. J Affect Disord. 2011;134(1-3):294-303. PubMed doi:10.1016/j.jad.2011.06.028
17. Traeger L, Braun IM, Greer JA, et al. Parsing depression from fatigue in patients with cancer using the fatigue symptom inventory. J Pain Symptom Manage. 2011;42(1):52-59. PubMed doi:10.1016/j.jpainsymman.2010.10.262
18. Lam RW, Michalak EE, Bond DJ, et al. Which depressive symptoms and medication side effects are perceived by patients as interfering most with occupational functioning? Depress Res Treat. 2012;2012(630206). PubMed
19. Naismith SL, Longley WA, Scott EM, et al. Disability in major depression related to self-rated and objectively-measured cognitive deficits: a preliminary study. BMC Psychiatry. 2007;7(1):32. PubMed doi:10.1186/1471-244X-7-32
20. Jaeger J, Berns S, Uzelac S, et al. Neurocognitive deficits and disability in major depressive disorder. Psychiatry Res. 2006;145(1):39-48. PubMed doi:10.1016/j.psychres.2005.11.011
21. American Psychiatric Association. Diagnostic and Statistical Manual of Mental Disorders, Fourth Edition, Text Revision. Washington, DC: American Psychiatric Association; 2000.
22. Kroenke K, Spitzer RL, Williams JB. The PHQ-9: validity of a brief depression severity measure. J Gen Intern Med. 2001;16(9):606-613. PubMed doi:10.1046/j.1525-1497.2001.016009606.x
23. Hamilton M. A rating scale for depression. J Neurol Neurosurg Psychiatry. 1960;23(1):56-62. PubMed doi:10.1136/jnnp.23.1.56
24. Montgomery SA, Asberg M. A new depression scale designed to be sensitive to change. Br J Psychiatry. 1979;134(4):382-389. PubMed doi:10.1192/bjp.134.4.382
25. Rush AJ, Gullion CM, Basco MR, et al. The Inventory of Depressive Symptomatology (IDS): psychometric properties. Psychol Med. 1996;26(3):477-486. PubMed doi:10.1017/S0033291700035558
26. Rush AJ, Trivedi MH, Ibrahim HM, et al. The 16-item Quick Inventory of Depressive Symptomatology (QIDS), clinician rating (QIDS-C), and self-report (QIDS-SR): a psychometric evaluation in patients with chronic major depression. Biol Psychiatry. 2003;54(5):573-583. PubMed doi:10.1016/S0006-3223(02)01866-8
27. Leon AC, Olfson M, Portera L, et al. Assessing psychiatric impairment in primary care with the Sheehan Disability Scale. Int J Psychiatry Med. 1997;27(2):93-105. PubMed doi:10.2190/T8EM-C8YH-373N-1UWD
28. Fava M, Iosifescu DV, Pedrelli P, et al. Reliability and validity of the Massachusetts General Hospital Cognitive and Physical Functioning Questionnaire. Psychother Psychosom. 2009;78(2):91-97. PubMed doi:10.1159/000201934
29. American Psychiatric Association. Practice Guideline for the Treatment of Patients With Major Depressive Disorder, Third Edition. Washington, DC: American Psychiatric Association; 2010. http://psychiatryonline.org/content.aspx?bookid=28§ionid=1667485. Accessed July 30, 2013.
30. Rothschild AJ, Dunlop BW, Dunner DL, et al. Assessing rates and predictors of tachyphylaxis during the prevention of recurrent episodes of depression with venlafaxine ER for two years (PREVENT) study. Psychopharmacol Bull. 2009;42(3):5-20. PubMed
31. Zajecka J, Tracy KA, Mitchell S. Discontinuation symptoms after treatment with serotonin reuptake inhibitors: a literature review. J Clin Psychiatry. 1997;58(7):291-297. PubMed doi:10.4088/JCP.v58n0702