Objective: Persons with schizophrenia often receive suboptimal physical health care, but the reasons are poorly understood. Vignettes have been used to examine how a patient’s race, gender, or physical health influences a provider’s practice; in this study, we used vignettes to examine the effect of a mental health diagnosis (schizophrenia) on providers’ clinical expectations and decision making regarding physical health care.
Method: A cross-sectional survey was administered from August 2011 to April 2012 to 275 primary care and mental health providers in 5 US Department of Veterans Affairs medical centers. Vignettes described identical scenarios for patients with and without schizophrenia. The survey assessed providers’ clinical expectations of patients (adherence, competence, ability to read and understand health education materials) and practice behaviors (referrals to weight reduction, pain management, and sleep study).
Results: Clinicians expected persons with schizophrenia would be less adherent to treatment (P = .04), less able to read and understand educational materials (P = .03), and less capable of managing their health and personal affairs (P < .01). Providers were less likely to refer a patient with schizophrenia to a weight-reduction program (P = .03). Other types of referral decisions (for pain management and sleep study) were not influenced by a schizophrenia diagnosis.
Conclusions: For both mental health and primary care providers, a history of schizophrenia was found to negatively affect provider expectations of patients’ adherence to treatment, ability to understand educational materials, and capacity to manage their treatment and financial affairs as well as some treatment decisions, such as referral to a weight-reduction program.

ABSTRACT
Objective: Persons with schizophrenia often receive suboptimal physical health care, but the reasons are poorly understood. Vignettes have been used to examine how a patient’s race, gender, or physical health influences a provider’s practice; in this study, we used vignettes to examine the effect of a mental health diagnosis (schizophrenia) on providers’ clinical expectations and decision making regarding physical health care.
Method: A cross-sectional survey was administered from August 2011 to April 2012 to 275 primary care and mental health providers in 5 US Department of Veterans Affairs medical centers. Vignettes described identical scenarios for patients with and without schizophrenia. The survey assessed providers’ clinical expectations of patients (adherence, competence, ability to read and understand health education materials) and practice behaviors (referrals to weight reduction, pain management, and sleep study).
Results: Clinicians expected persons with schizophrenia would be less adherent to treatment (P = .04), less able to read and understand educational materials (P = .03), and less capable of managing their health and personal affairs (P < .01). Providers were less likely to refer a patient with schizophrenia to a weight-reduction program (P = .03). Other types of referral decisions (for pain management and sleep study) were not influenced by a schizophrenia diagnosis.
Conclusions: For both mental health and primary care providers, a history of schizophrenia was found to negatively affect provider expectations of patients’ adherence to treatment, ability to understand educational materials, and capacity to manage their treatment and financial affairs as well as some treatment decisions, such as referral to a weight-reduction program.
J Clin Psychiatry 2015;76(8):1068-1074
dx.doi.org/10.4088/JCP.14m09465
© Copyright 2015 Physicians Postgraduate Press, Inc.
aVA South Central (VISN 16) Mental Illness Research, Education, and Clinical Center, Central Arkansas Veterans Healthcare System (CAVHS), North Little Rock
bTranslational Research Institute and cDepartment of Psychiatry Division of Health Services Research, University of Arkansas for Medical Sciences, Little Rock
dDivision of Evaluation and Research, Louisiana Public Health Institute, New Orleans
eCollege of Psychology, Illinois Institute of Technology, Chicago
fMichael E. DeBakey VA Medical Center, Houston, Texas and Menninger Department of Psychiatry and Behavioral Sciences, and Department of Neurology, Baylor College of Medicine, Houston, Texas
gSchool of Medicine, University of California, Riverside (current affiliation)
*Corresponding author: Dinesh Mittal, MD, Center for Mental Healthcare and Outcomes Research, Central Arkansas Veterans Healthcare System, Bldg 58 (152/NLR), North Little Rock, AR 72114 ([email protected]).
Persons with schizophrenia are at high risk for chronic medical conditions1-3 and premature death.4-6 Some studies,1,2,4,5,7-10 but not all,11 report that persons with schizophrenia, relative to those without mental illness, receive suboptimal medical, preventive, and specialty health care. While the reasons for this pattern are complex, a patient’s mental illness diagnosis potentially affects clinicians’ clinical expectations and choices.9 For example, different approaches to treatment may ensue according to whether the provider expects a patient to be nonadherent to treatment or lacking the capacity to manage his or her own health.
Clinicians resemble the general public in terms of holding negative views of persons with mental illness.12-14,15 Research comparing the attitudes of primary care providers with those of mental health professionals is sparse but suggests that primary care providers have a more negative view (especially about prognosis and likelihood of dangerousness) of persons with schizophrenia.16-19 Previous studies13,20-22 primarily examined how mental illness influences providers’ attitudes (such as a desire for personal social distance) rather than how mental illness directly affects clinical expectations or practice. This study, part of a larger study of provider stigma,23 explored the influence of a diagnosis of schizophrenia on clinical expectations and practice. Vignettes, often employed in studies to investigate situations involving bias, were used to reduce the likelihood that respondents endorsed socially desirable answers. Previous research with clinicians has used vignettes to investigate bias related to gender,24 race,25 age,26 and socioeconomic status.27 In this study, vignettes described patients with and without schizophrenia who otherwise had exactly the same demographic characteristics, job, physical health conditions, and level of functioning. In this article, we compare clinicians’ responses to hypothetical vignette patients. Specifically, we asked clinicians about expectations of the patient’s medication adherence, capacity to manage his or her own health, and ability to read and understand educational materials; and we asked whether clinicians would choose to refer the patient to specialty services such as weight reduction, a sleep study, or pain management. We examined the effect of vignette type on providers’ expectations and referral practices. We also compared whether primary care and mental health providers’ responses were influenced by vignette type.
METHOD
Primary care and mental health nurses and physicians employed at 5 US Department of Veterans Affairs (VA) hospitals in the southeast and southwest areas of the United States participated in a cross-sectional survey from August 2011 to April 2012. Research staff attended regularly scheduled clinician staff meetings, explained the study, and distributed surveys. The study was approved by the VA Central Institutional Review Board (IRB). The IRB allowed waiver of the informed consent documentation to maximize participant privacy. Providers who volunteered to complete the survey were given an information sheet describing all aspects of the informed consent. No incentive was offered.
Surveys were distributed during regularly scheduled staff meetings, some with one provider type (eg, nurses only) and others attended by both physicians and nurses. Research assistants from each site requested surveys from the coordinating site based on an estimated number of attendees at these staff meetings. Surveys were returned anonymously to the site study coordinator using preaddressed, postage-paid envelopes.
Each provider responded to one vignette. To ensure adequate distribution of equal numbers of each survey version, the coordinating site sent packages of alternating versions of the different vignettes to the site research coordinator, who was instructed to distribute surveys systematically from the packaged stack in order to ensure distribution of roughly equal numbers of each survey version. When unequal numbers of one survey version versus another were returned from a site, the next set of surveys sent to the site was adjusted such that equal numbers of vignettes (depicting patients with and without schizophrenia) were distributed. In all, 574 surveys were distributed to meeting attendees, and 282 surveys were returned. The final analysis included 275 surveys, as 7 were missing provider type information. Since minimal deception was required (participants were told this was a study of clinical decision making, not specifically a study of the influence of schizophrenia on decision making), researchers visited each site to explain the need for deception after data collection was completed. Study results were presented at a second site visit.

- Previous studies indicate that clinicians resemble the general public in terms of holding negative views of persons with mental illness. This study explored the influence of a diagnosis of schizophrenia on providers’ clinical expectations and referral practices.
- Both primary care and mental health providers’ perspectives of the abilities and competence of high-functioning patients with schizophrenia are likely more negative than warranted.
- Clinicians should be aware that such negative perspectives have the potential to influence their clinical decision making with these patients.
To develop vignettes and inform survey questions, researchers conducted focus groups with patients with serious mental illness (n = 6), family members of patients (n = 5), psychiatrists (n = 6), mental health nurses (n = 6), primary care physicians (n = 5), and primary care nurses (n = 5) at 1 of the 5 study sites. Researchers then used cognitive interviewing with 3 volunteers (a nurse, a psychiatrist, and a primary care physician) to ensure that the clinical vignette and survey questions were clear and understandable.
Focus-group participants identified provider expectations they thought would be influenced by mental illness. Specifically, focus-group members believed providers would expect poor treatment adherence, poor understanding of educational materials, incompetence to manage one’s own health and personal affairs, and lower levels of social and vocational functioning. Focus groups also provided information about common clinical scenarios potentially faced by each provider type in routine care situations in which a patient may or may not have schizophrenia.
Because focus groups identified arthritis as a common condition and the provider focus group expressed the concern that individuals with mental illness might be more likely to become addicted to pain medications, we created a scenario involving a patient with chronic arthritis and back pain. The vignette was intended to depict a relatively high-functioning person with a steady job who had been psychiatrically stable over several years and who routinely engaged in social and recreational activities.
Two versions of the vignette were used, 1 including the information shown here in brackets (vignette patient with schizophrenia) and 1 without that information (vignette patient without schizophrenia).
Case 1
Mr A is a 34-year-old male with [schizophrenia], hypertension, obesity, and chronic low back pain. His X-ray shows evidence of arthritis. He has been coming to your clinic for about 6 months, and this is his third visit. His current medications include lisinopril 40 mg daily, naproxen 500 mg twice a day, fluoxetine 20 mg per day [and risperidone 3 mg at bedtime]. He comes to his appointment today 15 minutes late and states that he has already used up all of the naproxen for the month in 25 days and would like to have his prescription filled early or get “something else that works better.” He has tolerated naproxen well. His height is 5′ 5″ and he weighs 201 lb. Three months ago he weighed 195 lb. His blood pressure today is 150/98, and 3 months ago it was 148/92. Mr A says that his back pain is “worse than ever” and that he is having a great deal of trouble sleeping. He looks more disheveled than usual [but reports no changes in his mental status]. Mr A grew up in Manchester, New Hampshire, and completed high school there. He has no history of substance abuse. He lives with his brother and has worked in food services at the VA for 3 years. His job performance has been above average. He attends church and church functions frequently and enjoys reading magazines. Occasionally he goes fishing with his brother.
After reading the vignette, providers completed a survey that included 26 questions about their clinical expectations and treatment decisions relative to the patient described in the vignette. These questions addressed specific issues identified by the focus groups and also asked about whether or not the provider would refer the patient for additional services or tests (sleep study and weight-reduction and pain-management programs).
Measures
In the absence of established scales to assess clinical expectations and treatment decisions relative to a given vignette, we generated these 26 items ourselves. For each item, providers were asked to rate the patient in the vignette on a scale of 1-10 in terms of their expectations or their decisions about referral. We then used factor analyses to guide the creation of 3 scales. Three items were used to assess expected treatment adherence (3 items, α = .89), 4 items assessed whether or not the patient could read and understand health education materials (4 items, α = .88), and 2 items assessed the patient’s competence to manage his or her own health care and personal finances (2 items, α = .86). We also included 3 single items: referral to a weight-reduction program, to a pain-management program, and to a sleep study. The provider’s expectation of the patient’s competence was assessed using 2 items, and participants rated them on a scale of 1-4. The measure was dichotomized because the majority (around 66%) selected 8 (from a range of 2-8). The measure created indicated high competence (8) versus low competence (< 8). The questions for the measures are presented in Table 1.
Data Analysis
Most study variables, except vignette type and site, had missing values, with the amount of missing data ranging from 2% to 13%. Where possible, missing values were replaced based on corresponding nonmissing related variables. For the remaining variables, we used the multiple imputation method of missing values.28,29 Five imputed datasets were generated with the SAS (SAS Inc) MI procedure using regression method or Markov chain Monte Carlo method when appropriate. The analysis was done for each imputed dataset separately, and then the SAS MIANALYZE procedure was used to combine the statistics from the 5 imputed datasets.
Descriptive statistics were calculated for all variables in the analysis. We used general or generalized linear regression models to examine the relationship between the independent variable vignette type (with or without schizophrenia) and each of the 6 dependent variables: (1) adherence to treatment; (2) ability to read and understand written educational materials; (3) competence; and whether the provider would refer the patient for additional services, such as (4) weight reduction, (5) pain management, and (6) sleep studies, while controlling for covariates, which included provider demographic characteristics (gender, age, and race), provider years in clinical practice, site, provider type (nurses, physicians), and provider specialty (mental health, primary care). The interaction between vignette type and provider specialty was also tested and excluded if not significant. For dependent variables with a skewed distribution (eg, patient’s adherence), we tried both generalized linear models and general linear models. Since results were similar in terms of significance, we chose the general linear model approach. A logistic regression model was used for patient competence.
RESULTS
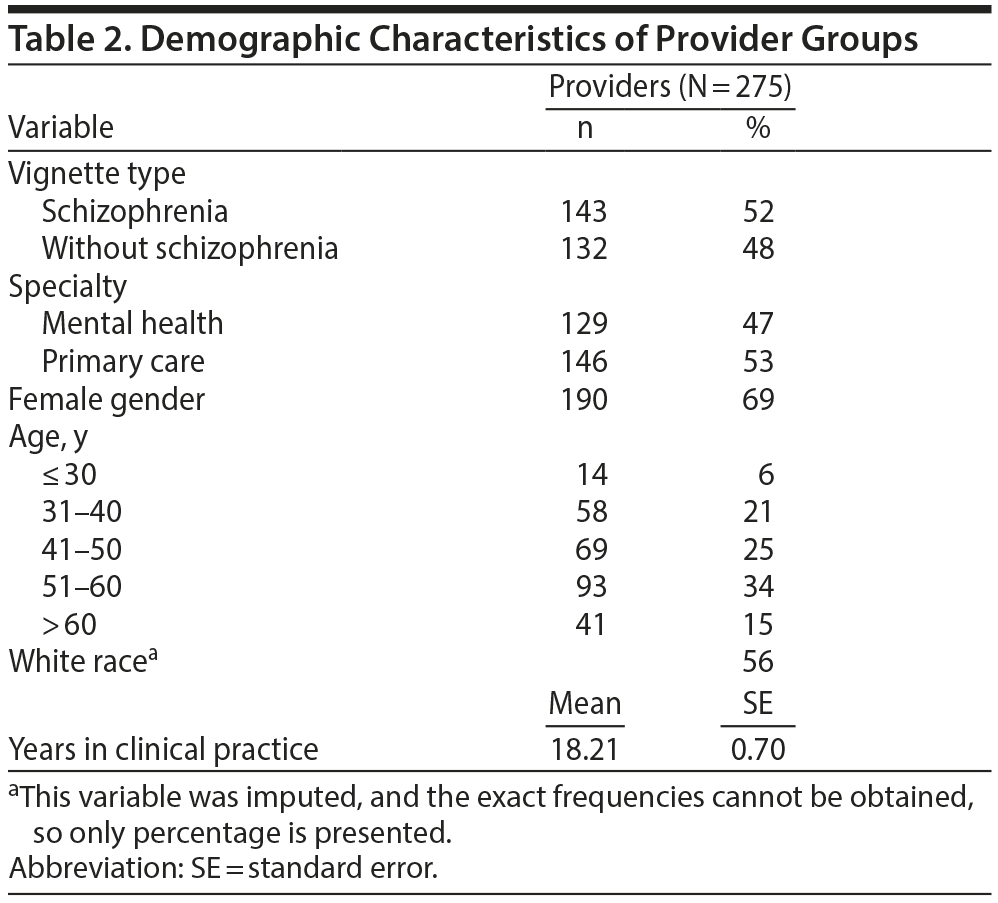
One hundred forty-three providers completed surveys about the patient having a diagnosis of schizophrenia; 132 completed surveys about the patient without schizophrenia. Most nurses were women (91%), and although the majority of physicians were men (61%), more than a third were women. Nurses were older with more years in clinical practice (on average, about 21 years), while physicians were younger with fewer years in clinical practice (on average, about 15 years). Over half (56%) of the providers were white (Table 2).
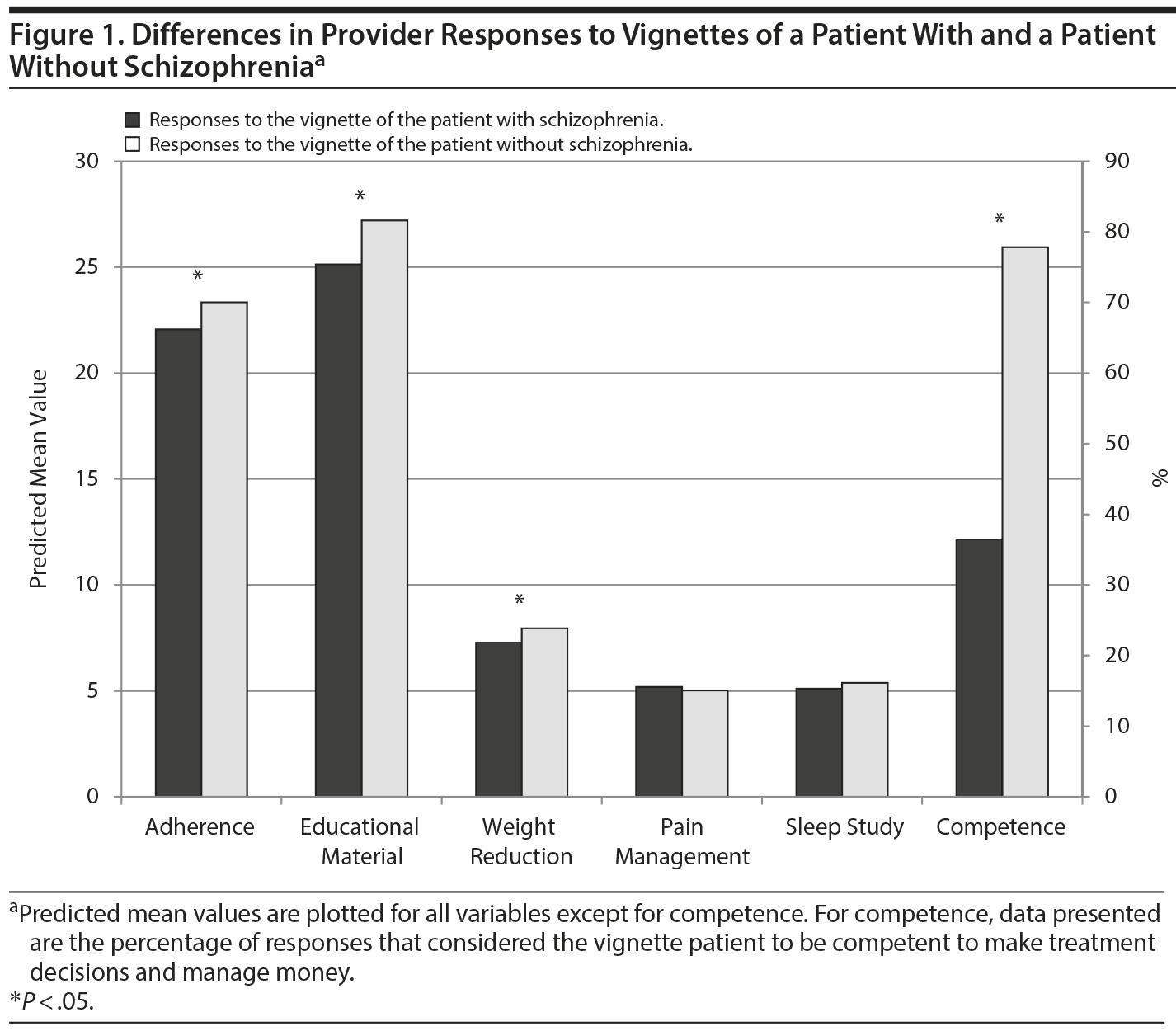
Findings from the multiple regression models for each of the 6 dependent variables indicated that the 2-way interaction between the vignette type and provider specialty was not significant for any of these models, indicating that the participants’ responses to the vignette type were not dependent on provider specialty (primary care or mental health). A significant main effect for vignette types was found for adherence (β = −1.28, t = −2.02, P = .04), competence (β = −1.81, t = −5.70, P < .01), ability to read and understand educational materials (β = −2.08, t = −2.25, P = .03), and referral to weight-reduction programs (β = −0.67, t = −2.17, P = .03). Clinicians expected persons with schizophrenia to be less likely to adhere to treatment, to be less competent to manage their own health and personal affairs, and to be less able to read and understand educational materials. Clinicians were also less likely to refer persons with schizophrenia to a weight-reduction program. The vignette type effect was not significant for referral to pain management or for a sleep study. Figure 1 depicts these findings, comparing the providers’ responses to the vignette in which the patient had schizophrenia and responses to the vignette describing the patient without schizophrenia.
DISCUSSION
We presented clinicians with vignettes describing 2 virtually identical patients with chronic physical health problems—one with and another without schizophrenia. Even though the 2 patients had the same educational background and social and vocational level of functioning, and the person with schizophrenia was clearly stable psychiatrically, a diagnosis of schizophrenia appeared to influence clinicians’ expectations related to patient competence, treatment adherence, and ability to read and understand educational materials. Further, providers were less likely to refer persons with schizophrenia for weight-reduction programs.
Even though research has indicated that persons with schizophrenia are no less adherent to medication or treatment than other patients with chronic mental or physical conditions,30 established beliefs about schizophrenia may affect practitioner behavior. In terms of competence to make treatment decisions, both persons who were not mentally ill and those with schizophrenia demonstrate substantial heterogeneity in decision-making capacity.31 High-functioning persons with schizophrenia are capable of making decisions regarding their health and personal affairs and “only patients at the very bottom of the performance curve” should be considered incompetent.32 In addition, persons with schizophrenia are reasonably successful in weight-loss programs relative to those without schizophrenia.33-36 Finally, there is no reason to expect a person with schizophrenia to have less ability to read or understand educational materials than a person with similar educational achievement who does not have schizophrenia, unless of course he is floridly psychotic or his symptoms are not well controlled, which was clearly not true in this case. It is likely that providers are responding to prevailing beliefs or stereotypes rather than to scientific evidence.
One potential explanation could be clinicians’ experience with persons with schizophrenia and other psychiatric diagnoses. Often, clinicians, especially those working in inpatient settings, are exposed to more severely ill individuals. They may attribute the characteristics and illness course of more severely ill patients to all patients with the same diagnosis, a phenomenon referred to by Cohen and Cohen37 as the “clinician’s illusion.” Accordingly, all individuals with schizophrenia are more likely to be regarded as limited, even high-functioning individuals with well-managed symptoms. Such low expectations related to adherence, ability to read and understand instructions, and competency could influence referral to noninvasive procedures (eg, weight-loss program) and could have an even greater influence on provider decisions about more invasive procedures, such as revascularization.
Clinicians who treat persons with schizophrenia are in powerful positions. For example, they may or may not choose to refer patients for rehabilitation services. To be effective, the recovery model clearly requires providers to focus on strengths rather than deficits and to involve individual patients in goal setting and decision making. Providers with low expectations of high-functioning persons with schizophrenia may well be limiting their patients’ recovery and may also undermine the patient’s own confidence and belief in his or her abilities and potential.
Several aspects of the study limit its generalization. First, participation was relatively low and sample size was small, relative to the number of mental health and primary care providers in the United States. All providers were practicing in the VA; the VA health care system serves a large proportion of persons with chronic mental and physical illnesses who may be more ill than the general population,38 which might promote more negative expectations. Also, it is important to note that the findings were based on responses to hypothetical vignettes that may or may not represent how clinicians would actually practice.39
While some progress has been made to develop attitudinal scales for providers,40 additional work is needed in this area. Future studies could examine attitudes of providers and compare these to actual clinical decision making rather than hypothetical vignettes. If these attitudes are indeed driving decision making, interventions need to be devised to reduce stigma toward persons with serious mental illness among providers.
CONCLUSIONS
Our findings suggest that interventions for clinicians are warranted, especially to educate providers about the potential of higher functioning persons with schizophrenia. Evidence suggests that a large portion of individuals with schizophrenia should be able to achieve a substantial degree of “long-term remission and functional recovery,” meaning that they are capable of working, living independently, and sustaining long-term relationships.41,42 Interventions that promote education and bring providers into contact with persons with schizophrenia who are further along in their recovery may be particularly useful43 in ameliorating long-held beliefs about the functional limits of individuals diagnosed with schizophrenia. Further research is needed to determine the extent to which negative views of mental illness potentially influence the quality of care delivered in clinical settings.
Submitted: August 23, 2014; accepted December 15, 2014.
Drug names: fluoxetine (Prozac and others), naproxen (Naprosyn, Anaprox, and others), risperidone (Risperdal and others).
Disclosure of off-label usage: The authors have determined that, to the best of their knowledge, no investigational information about pharmaceutical agents that is outside US Food and Drug Administration-approved labeling has been presented in this article.
Financial disclosure: Drs Sullivan, Mittal, Haynes, Mukherjee, Morris, Marsh, and Corrigan and Mss Reaves and Han have no personal affiliations or financial relationships with any commercial interest to disclose relative to the article.
Funding/support: This research was supported by a grant (IIR 08-086) from the US Department of Veterans Affairs (VA) Health Services Research and Development Services through the Central Arkansas Veterans Healthcare System; the South Central Mental Illness Research, Education, and Clinical Center (MIRECC), and by the Translational Research Institute at the University of Arkansas for Medical Sciences (8 UL1 TR000039-04).
Role of the sponsor: The study sponsor had no role in the design and conduct of the study; collection, management, analysis, and interpretation of the data; and preparation, review, or approval of the manuscript.
Previous presentation: This study was presented in part at the American Psychiatric Association Annual Meeting; May 18-22, 2013; San Francisco, California.
Acknowledgments: The authors thank Lisa Dixon, MD, MPH (Columbia University Medical Center), for her very helpful comments on the manuscript; Stephen Marder, MD (University of California, Los Angeles [UCLA]), Alexander S. Young, MD, MSHS (Greater Los Angeles VA & UCLA), and Richard Owen, MD (Central Arkansas Veterans Healthcare System), who were advisors to this project; and site principal investigators Drew Helmer, MD, MS (Michael E. DeBakey VA Medical Center, Houston; Dr Helmer is now affiliated with VA New Jersey Health Care System, East Orange Campus); Amee J. Epler, PhD (G. V. [Sonny] Montgomery VA Medical Center, Jackson, Mississippi); Scott A. Cardin, PhD (VA Gulf Coast Veterans Health Care System, Biloxi, Mississippi), and Michelle D. Sherman, PhD (Oklahoma City VA Medical Center, now at University of Minnesota), and their research staff for assistance with data collection. They also thank Penny White, BS (Central Arkansas Veterans Healthcare System), for administrative assistance and Carrie Edlund, MS (VA South Central Mental Illness Research, Education and Clinical Center), for assistance with editing and manuscript preparation. None of the acknowledged individuals have any financial conflicts of interest to disclose.
REFERENCES
1. DE Hert M, Correll CU, Bobes J, et al. Physical illness in patients with severe mental disorders, 1: prevalence, impact of medications and disparities in health care. World Psychiatry. 2011;10(1):52-77. PubMed
2. Viron MJ, Stern TA. The impact of serious mental illness on health and healthcare. Psychosomatics. 2010;51(6):458-465. PubMed doi:10.1176/appi.psy.51.6.458
3. Druss BG, Bornemann TH. Improving health and health care for persons with serious mental illness: the window for US federal policy change. JAMA. 2010;303(19):1972-1973. PubMed doi:10.1001/jama.2010.615
4. Mitchell AJ, Lord O. Do deficits in cardiac care influence high mortality rates in schizophrenia? a systematic review and pooled analysis. J Psychopharmacol. 2010;24(suppl):69-80. PubMed doi:10.1177/1359786810382056
5. Saha S, Chant D, McGrath J. A systematic review of mortality in schizophrenia: is the differential mortality gap worsening over time? Arch Gen Psychiatry. 2007;64(10):1123-1131. PubMed doi:10.1001/archpsyc.64.10.1123
6. Casta×±eda SF, Holscher J, Mumman MK, et al. Dimensions of community and organizational readiness for change. Prog Community Health Partnersh. 2012;6(2):219-226. PubMed doi:10.1353/cpr.2012.0016
7. Crump C, Winkleby MA, Sundquist K, et al. Comorbidities and mortality in persons with schizophrenia: a Swedish national cohort study. Am J Psychiatry. 2013;170(3):324-333. PubMed doi:10.1176/appi.ajp.2012.12050599
8. Leung GY, Zhang J, Lin WC, et al. Behavioral health disorders and adherence to measures of diabetes care quality. Am J Manag Care. 2011;17(2):144-150. PubMed
9. Carter R, Satcher D, Coelho T. Addressing stigma through social inclusion. Am J Public Health. 2013;103(5):773. PubMed doi:10.2105/AJPH.2012.301167
10. Weisse CS, Sorum PC, Dominguez RE. The influence of gender and race on physicians’ pain management decisions. J Pain. 2003;4(9):505-510. PubMed doi:10.1016/j.jpain.2003.08.002
11. Hicks S, Duran B, Wallerstein N, et al. Evaluating community-based participatory research to improve community-partnered science and community health. Prog Community Health Partnersh. 2012;6(3):289-299. PubMed doi:10.1353/cpr.2012.0049
12. Schulze B. Stigma and mental health professionals: a review of the evidence on an intricate relationship. Int Rev Psychiatry. 2007;19(2):137-155. PubMed doi:10.1080/09540260701278929
13. Nordt C, Rössler W, Lauber C. Attitudes of mental health professionals toward people with schizophrenia and major depression. Schizophr Bull. 2006;32(4):709-714. PubMed doi:10.1093/schbul/sbj065
14. Uçok A, Polat A, Sartorius N, et al. Attitudes of psychiatrists toward patients with schizophrenia. Psychiatry Clin Neurosci. 2004;58(1):89-91. PubMed doi:10.1111/j.1440-1819.2004.01198.x
15. Link BG, Struening EL, Neese-Todd S, et al. Stigma as a barrier to recovery: the consequences of stigma for the self-esteem of people with mental illnesses. Psychiatr Serv. 2001;52(12):1621-1626. PubMed doi:10.1176/appi.ps.52.12.1621
16. Björkman T, Svensson B, Lundberg B. Experiences of stigma among people with severe mental illness: reliability, acceptability and construct validity of the Swedish versions of two stigma scales measuring devaluation/discrimination and rejection experiences. Nord J Psychiatry. 2007;61(5):332-338. PubMed doi:10.1080/08039480701642961
17. Caldwell TM, Jorm AF. Mental health nurses’ beliefs about likely outcomes for people with schizophrenia or depression: a comparison with the public and other healthcare professionals. Aust N Z J Ment Health Nurs. 2001;10(1):42-54. PubMed doi:10.1046/j.1440-0979.2001.00190.x
18. Hori H, Richards M, Kawamoto Y, et al. Attitudes toward schizophrenia in the general population, psychiatric staff, physicians, and psychiatrists: a web-based survey in Japan. Psychiatry Res. 2011;186(2-3):183-189. PubMed doi:10.1016/j.psychres.2010.08.019
19. Hugo M. Mental health professionals’ attitudes towards people who have experienced a mental health disorder. J Psychiatr Ment Health Nurs. 2001;8(5):419-425. PubMed doi:10.1046/j.1351-0126.2001.00430.x
20. Aydin N, Yigit A, Inandi T, et al. Attitudes of hospital staff toward mentally ill patients in a teaching hospital, Turkey. Int J Soc Psychiatry. 2003;49(1):17-26. PubMed doi:10.1177/0020764003049001544
21. Kua JH, Parker G, Lee C, et al. Beliefs about outcomes for mental disorders: a comparative study of primary health practitioners and psychiatrists in Singapore. Singapore Med J. 2000;41(11):542-547. PubMed
22. Wilson J, Read J. What prevents GPs from using outside resources for women experiencing depression? a New Zealand study. Fam Pract. 2001;18(1):84-86. PubMed doi:10.1093/fampra/18.1.84
23. Mittal D, Corrigan P, Sherman M, et al. Healthcare providers’ attitudes towards persons with schizophrenia. Psychiatr Rehabil J. 2014;37(4):297-303. doi:10.1037/prj0000095 PubMed
24. Maserejian NN, Link CL, Lutfey KL, et al. Disparities in physicians’ interpretations of heart disease symptoms by patient gender: results of a video vignette factorial experiment. J Womens Health (Larchmt). 2009;18(10):1661-1667. PubMed doi:10.1089/jwh.2008.1007
25. Rathore SS, Ketcham JD, Alexander GC, et al. Influence of patient race on physician prescribing decisions: a randomized on-line experiment. J Gen Intern Med. 2009;24(11):1183-1191. PubMed doi:10.1007/s11606-009-1077-7
26. Uncapher H, Areán PA. Physicians are less willing to treat suicidal ideation in older patients. J Am Geriatr Soc. 2000;48(2):188-192. PubMed doi:10.1111/j.1532-5415.2000.tb03910.x
27. van Ryn M, Burgess D, Malat J, et al. Physicians’ perceptions of patients’ social and behavioral characteristics and race disparities in treatment recommendations for men with coronary artery disease. Am J Public Health. 2006;96(2):351-357. PubMed doi:10.2105/AJPH.2004.041806
28. Rubin DB. Inference and missing data. Biometrika. 1976;63(3):581-592. doi:10.1093/biomet/63.3.581
29. Rubin DB. Multiple Imputation for Nonresponse in Surveys. New York, NY: John Wiley & Sons; 1987.
30. World Health Organization. Adherence to Long-Term Therapies: Evidence for Action. Noncomunicable Diseases and Mental Health adherence to long-term therapies project. 2003. WHO web site. http://www.who.int/chp/knowledge/publications/adherence_report/en/. Accessed April 30, 2013.
31. Jeste DV, Depp CA, Palmer BW. Magnitude of impairment in decisional capacity in people with schizophrenia compared to normal subjects: an overview. Schizophr Bull. 2006;32(1):121-128. PubMed doi:10.1093/schbul/sbj001
32. Appelbaum PS. Clinical practice: assessment of patients’ competence to consent to treatment. N Engl J Med. 2007;357(18):1834-1840. PubMed doi:10.1056/NEJMcp074045
33. Daumit GL, Dickerson FB, Wang NY, et al. A behavioral weight-loss intervention in persons with serious mental illness. N Engl J Med. 2013;368(17):1594-1602. PubMed doi:10.1056/NEJMoa1214530
34. Allison DB, Mentore JL, Heo M, et al. Antipsychotic-induced weight gain: a comprehensive research synthesis. Am J Psychiatry. 1999;156(11):1686-1696. PubMed
35. Lieberman JA. Effectiveness of antipsychotic drugs in patients with chronic schizophrenia: efficacy, safety and cost outcomes of CATIE and other trials. J Clin Psychiatry. 2007;68(2):e04. PubMed doi:10.4088/JCP.0207e04
36. Parsons B, Allison DB, Loebel A, et al. Weight effects associated with antipsychotics: a comprehensive database analysis. Schizophr Res. 2009;110(1-3):103-110. PubMed doi:10.1016/j.schres.2008.09.025
37. Cohen P, Cohen J. The clinician’s illusion. Arch Gen Psychiatry. 1984;41(12):1178-1182. PubMed doi:10.1001/archpsyc.1984.01790230064010
38. Agha Z, Lofgren RP, VanRuiswyk JV, et al. Are patients at Veterans Affairs medical centers sicker? a comparative analysis of health status and medical resource use. Arch Intern Med. 2000;160(21):3252-3257. PubMed doi:10.1001/archinte.160.21.3252
39. Goldszmidt M, Minda JP, Bordage G. Developing a unified list of physicians’ reasoning tasks during clinical encounters. Acad Med. 2013;88(3):390-397. PubMed doi:10.1097/ACM.0b013e31827fc58d
40. Kassam A, Papish A, Modgill G, et al. The development and psychometric properties of a new scale to measure mental illness related stigma by health care providers: the Opening Minds Scale for Health Care Providers (OMS-HC). BMC Psychiatry. 2012;12(1):62. PubMed doi:10.1186/1471-244X-12-62
41. Warner R. Recovery from schizophrenia and the recovery model. Curr Opin Psychiatry. 2009;22(4):374-380. PubMed doi:10.1097/YCO.0b013e32832c920b
42. Zipursky RB, Reilly TJ, Murray RM. The myth of schizophrenia as a progressive brain disease. Schizophr Bull. 2013;39(6):1363-1372. PubMed doi:10.1093/schbul/sbs135
43. Corrigan PW, Morris SB, Michaels PJ, et al. Challenging the public stigma of mental illness: a meta-analysis of outcome studies. Psychiatr Serv. 2012;63(10):963-973. PubMed doi:10.1176/appi.ps.201100529
This PDF is free for all visitors!