Objective: To investigate blood pressure (BP) changes within the first 3 days after initiating antipsychotic medication in psychiatric inpatients.
Methods: Through retrospective chart review using a repeated measures design, vital signs data were collected on 60 adult psychiatric inpatients who were psychiatrically hospitalized May 26, 2011, through September 4, 2012, at 9 time points within 3 days of initiation of 1 of 6 different antipsychotic medications. The random sample included patients with the following DSM-IV-TR diagnoses: schizophrenia (n = 25), schizoaffective disorder (either type; n = 19), and bipolar I disorder (n = 16). Data were analyzed using mixed-effects repeated measures analysis of variance to evaluate associations between the antipsychotic initiated and subsequent changes in BP. The main outcome variable was change in BP from baseline, and independent variables included age, sex, psychiatric diagnosis, and type of antipsychotic medication. Logistic regression was used to assess the relationship between each type of antipsychotic and hypotension (BP < 90/60 mm Hg) and hypertension (BP ≥ 140/90 mm Hg).
Results: Olanzapine (P < .01) and risperidone (P = .01) raised systolic BP to a statistically significant degree during the first 3 days after initiation. Clozapine, on the other hand, significantly reduced systolic BP (P = .02) and was associated with hypotension on linear regression. No statistically significant associations were found between the other antipsychotics and acute systolic BP changes or between any of the 6 antipsychotics and diastolic BP changes.
Conclusions: Initiation of certain antipsychotic medications may be associated with statistically significant acute BP changes. These findings require further evaluation in well-designed prospective studies.
Acute Blood Pressure Changes Associated With
Antipsychotic Administration to Psychiatric Inpatients
ABSTRACT
Objective: To investigate blood pressure (BP) changes within the first 3 days after initiating antipsychotic medication in psychiatric inpatients.
Methods: Through retrospective chart review using a repeated measures design, vital signs data were collected on 60 adult psychiatric inpatients who were psychiatrically hospitalized May 26, 2011, through September 4, 2012, at 9 time points within 3 days of initiation of 1 of 6 different antipsychotic medications. The random sample included patients with the following DSM-IV-TR diagnoses: schizophrenia (n = 25), schizoaffective disorder (either type; n = 19), and bipolar I disorder (n = 16). Data were analyzed using mixed-effects repeated measures analysis of variance to evaluate associations between the antipsychotic initiated and subsequent changes in BP. The main outcome variable was change in BP from baseline, and independent variables included age, sex, psychiatric diagnosis, and type of antipsychotic medication. Logistic regression was used to assess the relationship between each type of antipsychotic and hypotension (BP < 90/60 mm Hg) and hypertension (BP ≥ 140/90 mm Hg).
Results: Olanzapine (P < .01) and risperidone (P = .01) raised systolic BP to a statistically significant degree during the first 3 days after initiation. Clozapine, on the other hand, significantly reduced systolic BP (P = .02) and was associated with hypotension on linear regression. No statistically significant associations were found between the other antipsychotics and acute systolic BP changes or between any of the 6 antipsychotics and diastolic BP changes.
Conclusions: Initiation of certain antipsychotic medications may be associated with statistically significant acute BP changes. These findings require further evaluation in well-designed prospective studies.
Prim Care Companion CNS Disord 2018;20(4):18m02299
To cite: Parks KA, Parks CG, Yost JP, et al. Acute blood pressure changes associated with antipsychotic administration to psychiatric inpatients. Prim Care Companion CNS Disord. 2018;20(4):18m02299.
To share: https://doi.org/10.4088/PCC.18m02299
© Copyright 2018 Physicians Postgraduate Press, Inc.
aDivision of Medicine/Psychiatry, Southern Illinois University School of Medicine, Springfield, Illinois
bDepartment of Psychiatry, Sarah Bush Lincoln Hospital, Mattoon, Illinois
cDepartment of Psychiatry, Southern Illinois University School of Medicine, Springfield, Illinois
*Corresponding author: Obiora E. Onwuameze, MD, PhD, Department of Psychiatry, Southern Illinois University School of Medicine, Mail Code 9636, PO Box 19636, Springfield, IL 62794-9636 ([email protected]).
The frequency of antipsychotic medication use continues to rise worldwide.1–3 Off-label use of antipsychotics has also been increasing,4 and these medications are not infrequently prescribed to geriatric patients with psychiatric and major neurocognitive disorders.5 Despite concerns over the safety of antipsychotic treatment in older adults, long-term use is common.5 Potential adverse effects associated with antipsychotics include extrapyramidal symptoms (eg, dystonia, akathisia, parkinsonism, tardive dyskinesia), cardiovascular events (eg, tachycardia, orthostatic hypotension, QTc interval prolongation, and sudden death), neuroleptic malignant syndrome, seizures, central nervous system depression and respiratory failure (mostly in overdose), and metabolic effects (eg, obesity, dyslipidemia, insulin resistance).1,2,6–11 Orthostatic hypotension has most commonly been reported with chlorpromazine, thioridazine, clozapine, and quetiapine9,12; other agents have not been associated with development of hypotension. Although hypertension often occurs in patients maintained on long-term antipsychotic therapy as a consequence of metabolic syndrome,13,14 acute changes in blood pressure (BP) following initiation of antipsychotics have not been widely reported. Such BP fluctuations could precipitate adverse events and may, therefore, require closer monitoring during the early stages of antipsychotic therapy. Indeed, cases in which acute hypertension occurring after the initiation of second-generation antipsychotic therapy was accompanied by diminished consciousness, syncope, and rigidity have been reported.15 Such symptoms are features of catatonia and neuroleptic malignant syndrome, further lending importance to their prompt recognition.
Antipsychotics, which produce significant orthostatic hypotension, are thought to do so via α1-receptor antagonism, resulting in peripheral vasodilation and associated reflex tachycardia.9 Another mechanism reported in the literature16 is the antagonism of the histamine type 1 receptor common to clozapine and olanzapine both of which have been associated with acute onset of hypotension. Interestingly, clozapine administration has been associated with both hypotension and hypertension in different clinical scenarios.10,11,17–20 In 1 retrospective study21 comparing acute BP changes in Korean patients with schizophrenia treated with either clozapine or olanzapine, the investigators found that clozapine significantly increased both systolic and diastolic BP (SBP and DBP, respectively) within 8 weeks of initiation, while olanzapine did not.
During routine screening of the data from New Zealand’s Intensive Medicines Monitoring Program, Coulter15 found several cases of acute hypertension following second-generation antipsychotic initiation. In these cases, risk factors for hypertension included age greater than 50 years and concurrent use of selective serotonin reuptake inhibitor or tricyclic antidepressant medication.15 Aripiprazole has also been associated with clinically significant acute hypertension in several case studies.22,23 These antipsychotics all appear to exhibit antagonism at the postsynaptic α1– and presynaptic α2-receptors, and the overall balance of each drug’s activity at these receptors may be responsible for the clinically significant effect on BP.24–28
Overall, there is a paucity of evidence-based literature exploring the link between antipsychotic initiation and acute fluctuations in BP. The few reports8,9 of clinically significant BP changes associated with antipsychotic administration indicate that it is plausible that these medications may sometimes be associated with acute hypertension or hypotension. Therefore, we conducted a retrospective chart review to better elucidate this relationship.
METHODS
We performed a retrospective review of the electronic medical record using a repeated measures design. Institutional review board approval was obtained from the Springfield Committee for Research Involving Human Subjects at the institution wherein the data were collected. The project was deemed exempt due to its retrospective chart review design and did not require informed consent from participants or their families. We collected de-identified data from 60 randomly selected adult patients who were psychiatrically hospitalized May 26, 2011, through September 4, 2012, and started on an antipsychotic medication. Inclusion criteria included age 18–65 years and 1 of the following DSM-IV-TR diagnoses: schizophrenia, schizoaffective disorder (either bipolar or depressive type), or bipolar I disorder. In addition, patients must not have been taking any antipsychotic medications prior to hospital admission.
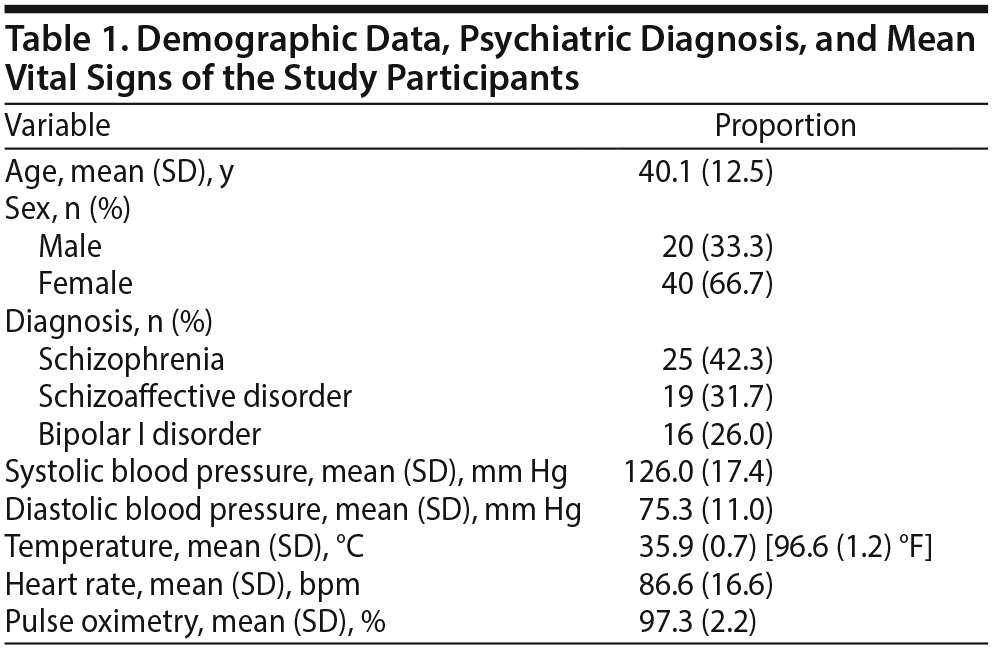
The participants included 60 patients with diagnoses of schizophrenia (n = 25), schizoaffective disorder (n = 19), and bipolar I disorder (n = 16). Data collected from each participant included demographic information, psychiatric diagnosis, and vital signs, including SBP and DBP, temperature, heart rate, and pulse oximetry measured at 9 time points within 3 days of antipsychotic initiation (Table 1). The type of antipsychotic medication each patient received was also noted and included haloperidol, olanzapine, clozapine, risperidone, ziprasidone, and quetiapine. At least 10% of the 60 patients had to be taking a particular antipsychotic for it to be included in the study analysis.
Data analysis was performed with Statistical Analysis Software version 9.4 (SAS Institute, Cary, North Carolina) using the mixed-effects repeated measures analysis of variance procedure to evaluate associations between the type of antipsychotic initiated and subsequent changes in BP. The frequency distribution and means and proportion analysis were calculated using the frequency and means procedure, respectively. To account for missing BP values, likelihood-based mixed-effects analyses were employed, as these have been shown to be more accurate in compensating for missing data compared to a last-observation-carried-forward approach.29 Independent (predictor) variables included age analyzed as continuous, sex analyzed as dichotomous, psychiatric diagnosis analyzed as categorical (ie, schizophrenia, schizoaffective disorder, or bipolar I disorder), and administration of each type of antipsychotic medication analyzed as dichotomous (ie, yes or no for haloperidol, olanzapine, clozapine, risperidone, ziprasidone, and quetiapine). Our main outcome variable was change in SBP and DBP from baseline. Secondary outcome variables, investigated for each type of antipsychotic using logistic regression analysis, included the occurrence of hypotension (defined as SBP < 90 mm Hg or DBP < 60 mm Hg) and the occurrence of hypertension (defined as SBP ≥ 140 mm Hg or DBP ≥ 90 mm Hg). In all cases, we used the criterion of medication initiation within the past 72 hours to explore the immediate effects on BP as well as to control for potential confounding factors that would be expected to arise with longer time periods of measurement.
RESULTS
During the time period, we analyzed 25 participants who received olanzapine, 17 who received ziprasidone, 9 who received clozapine, 10 who received quetiapine, 28 who received haloperidol, and 13 who received risperidone. Prior to the initiation of antipsychotics, 30% (18 of 60) of the sample participants were hypertensive. After initiation of antipsychotics, 5% (1 of 20) of the men, 25% (10 of 40) of the women, and 17% (11 of 60) of the total sample had hypertension. Only 2 participants had sustained hypertension throughout the time of antipsychotic administration. The mean change overall was a decrease in SBP by 4 mm Hg and DBP by 2 mm Hg. For the 16 patients who were hypertensive before but not after antipsychotic use, the mean change was a decrease in SBP by 20 mm Hg and DBP by 12 mm Hg. For the 33 individuals who were not hypertensive before or after antipsychotic administration, the mean change overall was a decrease in SBP by 3 mm Hg with no change in DBP.
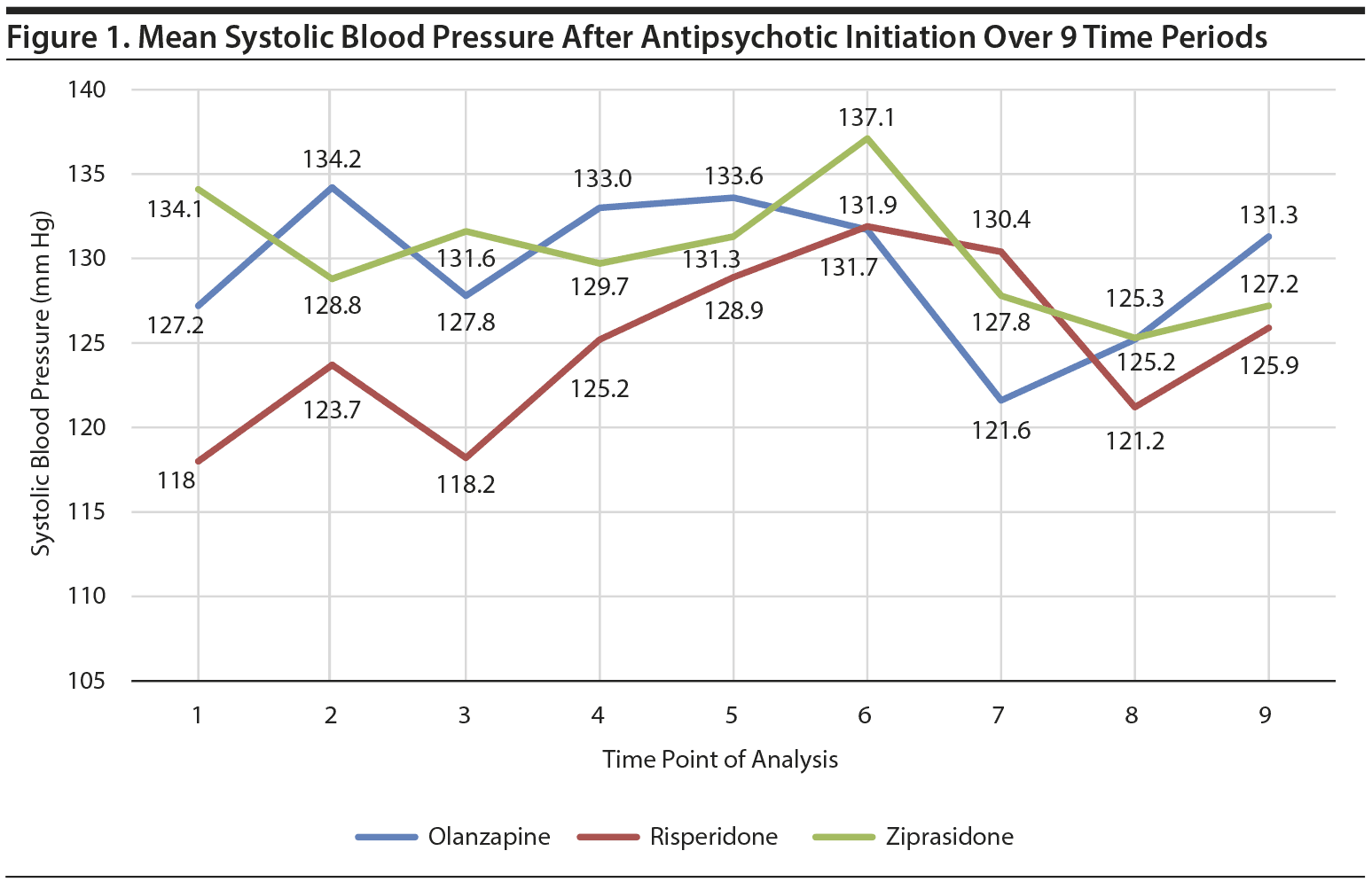
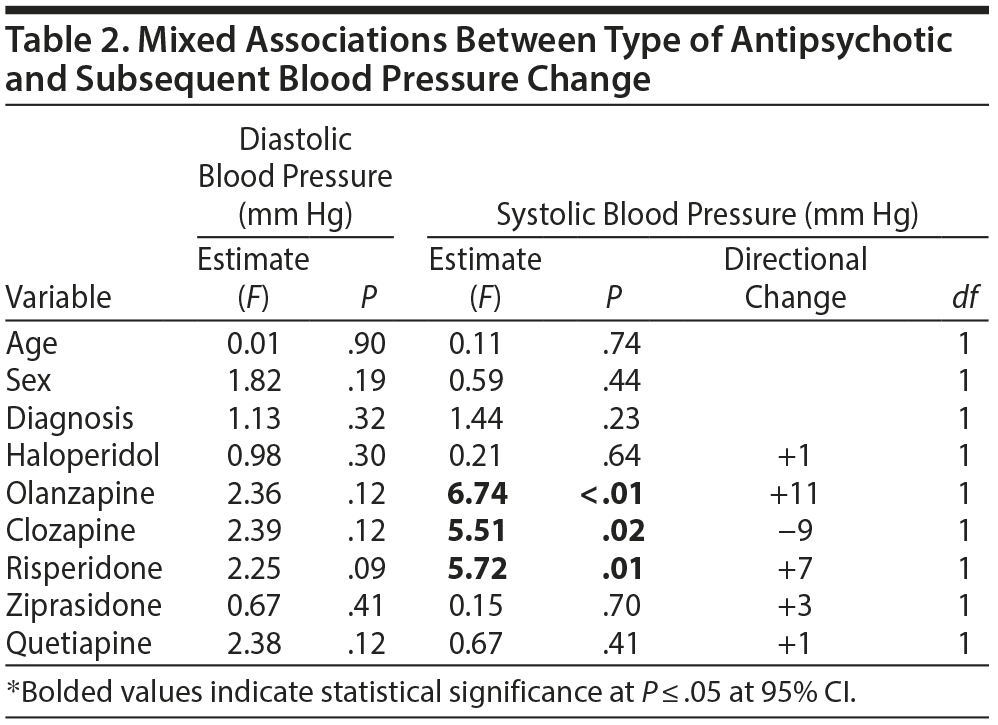
We found that olanzapine, risperidone, and ziprasidone increased SBP at some periods during the 9 times of vital sign measurement within 3 days of initiation (Figure 1). However, only olanzapine (P < .01) and risperidone (P = .01) raised SBP to a statistically significant degree (Table 2). Clozapine, however, significantly reduced SBP (Table 2) and was associated with hypotension on linear regression analysis (OR = 18.02; CI, 3.42–29.49). We found no statistically significant associations between the other antipsychotics and acute SBP changes or between any of the 6 antipsychotics and DBP changes.
DISCUSSION
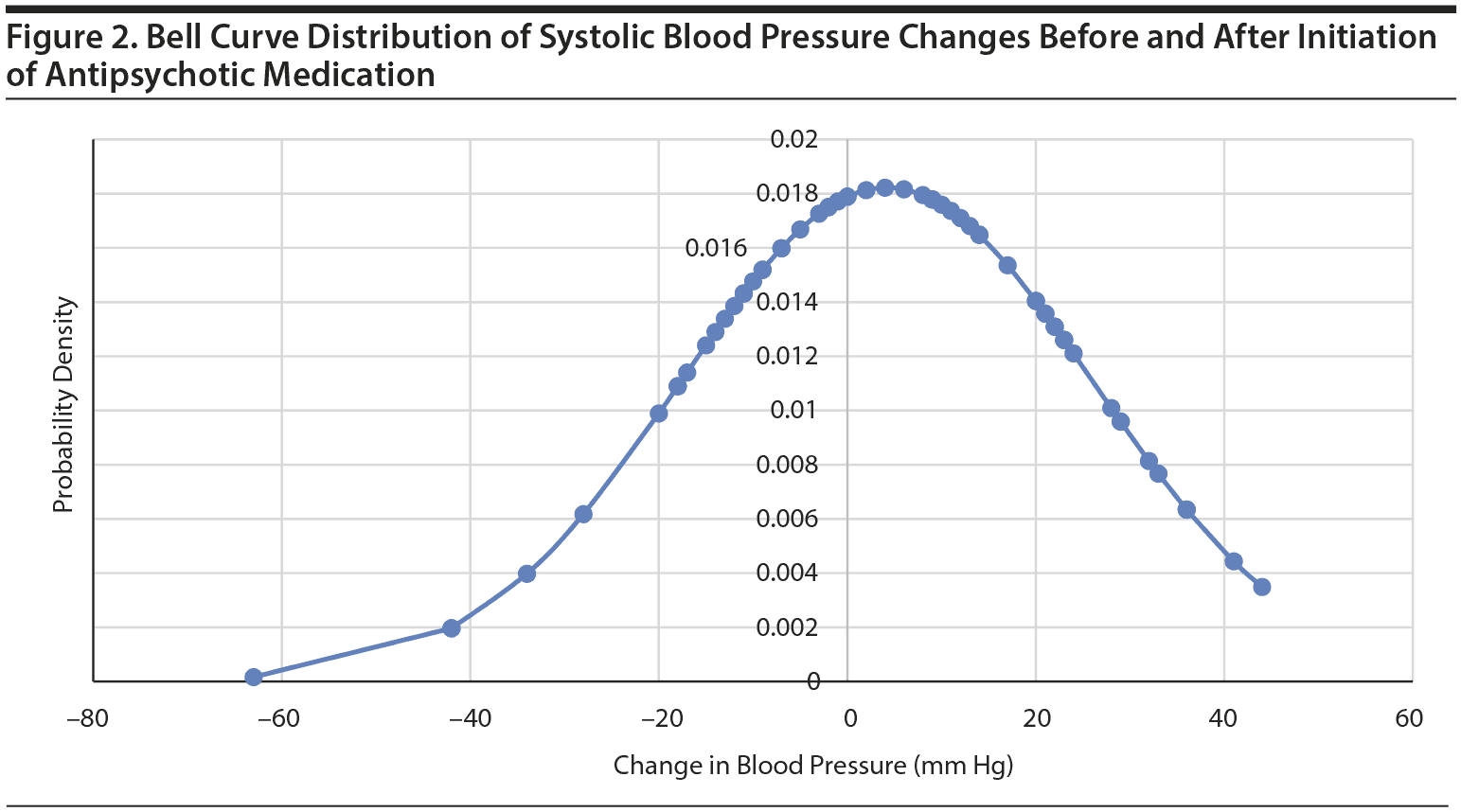
The results of this study support the previous findings of case studies reporting clinically significant BP alterations with clozapine10,11 and risperidone.15 Studies22,23 have also found aripiprazole to be associated with significant BP changes in the acute setting, but we did not have enough participants taking aripiprazole to be able to evaluate the acute BP effects of this agent. Risperidone, clozapine, and olanzapine were found to be associated with statistically significant SBP changes in the acute setting. When the data are viewed in aggregate, a bell curve distribution for SBP response emerges (Figure 2). Although SBP fluctuations for most participants were modest, the increases and decreases in SBP exhibited by the individuals in the outlier group were substantial and require further exploration in future studies, preferably with a prospective design and larger sample size.
It was interesting to note that a subset of the sample, 9 participants in total, who were not hypertensive prior to antipsychotic administration had BP readings in the hypertensive range following antipsychotic use. Although the small sample size in this study may have contributed to the lack of power to detect effect size, this group displayed a mean increase in SBP by 22 mm Hg and DBP by 8 mm Hg, suggesting that certain individuals, whether by virtue of their demographics, genetics, or concurrent use of other medications (eg, selective serotonin reuptake inhibitors), may be more vulnerable to acute dysautonomia resulting from introduction of antipsychotic therapy.
This study is limited in that the duration of the acute blood pressure effects of antipsychotics are unknown and may only be brief as the body adapts to the newly introduced medication. In addition, overall decreases in BP could also contribute to improvement in mental status and resolution of distress. When patients first arrive to the psychiatric unit, they are often anxious, agitated, or in a state of high sympathetic drive due to the psychiatric condition that led to their admission. With improvement in this condition over time and involvement in the therapeutic milieu, patients’ sympathetic drive would be expected to lessen, thereby leading to decreases in BP as well. Another limitation of our study involves the retrospective chart review design and that vital signs were measured using no specific protocol to ensure consistency.
Our data suggest that initiation of certain antipsychotic medications may be associated with significant acute BP changes aside from the well-established long-term relationship of some of these drugs to chronic hypertension that often occurs with metabolic syndrome. Coulter15 described cases of antipsychotic-associated severe hypertension marked by rigidity, unresponsiveness, and collapse in contrast to the findings of the present study. Such symptomatology may suggest an underlying etiology that overlaps with serotonin and neuroleptic malignant syndromes, which are life-threatening adverse events of psychiatric medication use marked by BP variability and other perturbations in neurologic function and mental status. If this were the case, acute BP changes following initiation of antipsychotics could serve as a warning to more closely monitor vital signs and de-escalate therapy if necessary. But, before further recommendations can be established, our findings require evaluation in well-designed prospective studies to better understand the relationship.
Submitted: March 14, 2018; accepted May 16, 2018.
Published online: July 19, 2018.
Potential conflicts of interest: None.
Funding/support: This study received financial support from Janssen Scientific Affairs, LLC, through their Academic Research Mentorship Program.
Role of the sponsor: The sponsor had no role in the design and conduct of the study; collection, management, analysis, and interpretation of data; or preparation, review, or approval of the manuscript.
Previous presentation: Poster presented at the American Society of Clinical Psychopharmacology annual meeting; May 29–June 2, 2017; Miami Beach, Florida.
REFERENCES
1. Comer JS, Mojtabai R, Olfson M. National trends in the antipsychotic treatment of psychiatric outpatients with anxiety disorders. Am J Psychiatry. 2011;168(10):1057–1065. PubMed CrossRef
2. Olfson M, Blanco C, Liu SM, et al. National trends in the office-based treatment of children, adolescents, and adults with antipsychotics. Arch Gen Psychiatry. 2012;69(12):1247–1256. PubMed CrossRef
3. Verdoux H, Tournier M, Bégaud B. Antipsychotic prescribing trends: a review of pharmaco-epidemiological studies. Acta Psychiatr Scand. 2010;121(1):4–10. PubMed CrossRef
4. Haw C, Stubbs J. Off-label use of antipsychotics: are we mad? Expert Opin Drug Saf. 2007;6(5):533–545. PubMed CrossRef
5. Olfson M, King M, Schoenbaum M. Antipsychotic treatment of adults in the United States. J Clin Psychiatry. 2015;76(10):1346–1353. PubMed CrossRef
6. Rummel-Kluge C, Komossa K, Schwarz S, et al. Head-to-head comparisons of metabolic side effects of second generation antipsychotics in the treatment of schizophrenia: a systematic review and meta-analysis. Schizophr Res. 2010;123(2–3):225–233. PubMed CrossRef
7. Jakubovski E, Carlson JP, Bloch MH. Prognostic subgroups for remission, response, and treatment continuation in the Clinical Antipsychotic Trials of Intervention Effectiveness (CATIE) trial. J Clin Psychiatry. 2015;76(11):1535–1545. PubMed CrossRef
8. Buckley NA, Sanders P. Cardiovascular adverse effects of antipsychotic drugs. Drug Saf. 2000;23(3):215–228. PubMed CrossRef
9. Levine M, Ruha A-M. Overdose of atypical antipsychotics: clinical presentation, mechanisms of toxicity and management. CNS Drugs. 2012;26(7):601–611. PubMed CrossRef
10. Lieberman JA. Effectiveness of antipsychotic drugs in patients with chronic schizophrenia: efficacy, safety and cost outcomes of CATIE and other trials. J Clin Psychiatry. 2007;68(2):e04. PubMed CrossRef
11. Haddad PM, Sharma SG. Adverse effects of atypical antipsychotics: differential risk and clinical implications. CNS Drugs. 2007;21(11):911–936. PubMed CrossRef
12. DiGiacomo J. Cardiovascular effects of psychotropic drugs. Cardiovasc Rev Rep. 1989;10(5):31–47.
13. Boyda HN, Tse L, Procyshyn RM, et al. Preclinical models of antipsychotic drug-induced metabolic side effects. Trends Pharmacol Sci. 2010;31(10):484–497. PubMed CrossRef
14. Henderson DC, Daley TB, Kunkel L, et al. Clozapine and hypertension: a chart review of 82 patients. J Clin Psychiatry. 2004;65(5):686–689. PubMed CrossRef
15. Coulter D. Atypical antipsychotics may cause hypertension. Prescriber Update. 2003;24(1):4.
16. Fisher J, Taori G, Braitberg G, et al. Methylene blue used in the treatment of refractory shock resulting from drug poisoning. Clin Toxicol (Phila). 2014;52(1):63–65. PubMed CrossRef
17. Gupta S, Rajaprabhakaran R. Paradoxical hypertension associated with clozapine. Am J Psychiatry. 1994;151(1):148. PubMed
18. Ennis LM, Parker RM. Paradoxical hypertension associated with clozapine. Med J Aust. 1997;166(5):278. PubMed
19. Krentz AJ, Mikhail S, Cantrell P, et al. Drug points: pseudophaeochromocytoma syndrome associated with clozapine. BMJ. 2001;322(7296):1213. PubMed CrossRef
20. George TP, Winther LC. Hypertension after initiation of clozapine. Am J Psychiatry. 1996;153(10):1368–1369. PubMed CrossRef
21. Woo YS, Kim W, Chae J-H, et al. Blood pressure changes during clozapine or olanzapine treatment in Korean schizophrenic patients. World J Biol Psychiatry. 2009;10(4 pt 2):420–425. PubMed CrossRef
22. Borras L, Constant EL, Eytan A, et al. Hypertension and aripiprazole. Am J Psychiatry. 2005;162(12):2392. PubMed CrossRef
23. Hsiao Y-L, Chen S-J, Shen T-W, et al. Aripiprazole augmentation induced hypertension in major depressive disorder: a case report. Prog Neuropsychopharmacol Biol Psychiatry. 2011;35(1):305–306. PubMed CrossRef
24. Arnt J, Skarsfeldt T. Do novel antipsychotics have similar pharmacological characteristics? a review of the evidence. Neuropsychopharmacology. 1998;18(2):63–101. PubMed CrossRef
25. Bymaster FP, Calligaro DO, Falcone JF, et al. Radioreceptor binding profile of the atypical antipsychotic olanzapine. Neuropsychopharmacology. 1996;14(2):87–96. PubMed CrossRef
26. Paulose-Ram R, Safran MA, Jonas BS, et al. Trends in psychotropic medication use among US adults. Pharmacoepidemiol Drug Saf. 2007;16(5):560–570. PubMed CrossRef
27. Marco CA, Vaughan J. Emergency management of agitation in schizophrenia. Am J Emerg Med. 2005;23(6):767–776. PubMed CrossRef
28. Shiwach RS. Treatment of clozapine induced hypertension and possible mechanisms. Clin Neuropharmacol. 1998;21(2):139–140. PubMed
29. Mallinckrodt CH, Sanger TM, Dubé S, et al. Assessing and interpreting treatment effects in longitudinal clinical trials with missing data. Biol Psychiatry. 2003;53(8):754–760. PubMed CrossRef
Enjoy this premium PDF as part of your membership benefits!


