Variations in the Probability of Depression Screening at Community-Based Physician Practice Visits
Donald L. Harrison, PhD; Michael J. Miller, DrPH; Michael R. Schmitt, PharmD; and Bryan K. Touchet, MD
Background: Despite depression screening being a US Preventive Services Task Force-recommended practice in primary care, little is known about the degree to which it is performed and the factors associated with its conduct.
Method: Using a nationally representative sample (National Ambulatory Medical Care Survey) of adult, community-based physician practice visits during the survey years 2005 to 2007 (total = 55,143; representing approximately 1.7 billion visits nationally), we estimated the probability of depression screening and variation by visit characteristics.
Results: Depression screening occurred at 2.29% of adult, community-based physician practice visits. Visits with primary care physicians were more likely to include depression screening (AOR = 2.19; 95% CI, 1.31-3.65), as were visits for preventive (AOR = 4.09; 95% CI, 2.55-6.57) and chronic care (AOR = 2.00; 95% CI, 1.44-2.80) compared to visits for acute care. Compared to the Northeast, visits in the West were less likely to include depression screening (AOR = 0.27; 95% CI, 0.13-0.57), as were visits for patients having ≥ 6 visits within the past 12 months (AOR = 0.65; 95% CI, 0.42-1.00) when compared to visits for new patients. Depression screening was more common at visits for patients with ICD-9-diagnosed depression (AOR = 7.51; 95% CI, 5.38-10.50) and for females (AOR = 1.26; 95% CI, 1.00-1.57). Bivariate analyses revealed that depression screening was more common at visits for patients with hyperlipidemia (3.21% vs 2.09%, P = .0086), obesity (4.59% vs 2.08%, P < .0001), and osteoporosis (4.46% vs 2.21%, P = .0002) and less common at visits for patients with diabetes (1.58% vs 2.39%, P = .0102).
Conclusions: Depression screening at community-based physician practice visits in the United States appears to be low (2.29%) and may reflect an undefined optimal screening interval or strategy in published guidelines, lack of reimbursement incentives, or incomplete documentation in the medical record. Opportunities exist to improve depression screening in males, patients with chronic disease (especially diabetes), and the western region of the United States.
Prim Care Companion J Clin Psychiatry 2010;12(5):e1-e8
© Copyright 2010 Physicians Postgraduate Press, Inc.
Submitted: October 8, 2009; accepted January 4, 2010.
Published online: October 7, 2010 (doi:10.4088/PCC.09m00911blu).
Corresponding author: Donald L. Harrison, PhD, University of Oklahoma, College of Pharmacy, 1110 N Stonewall Ave, Oklahoma City, OK 73117 ([email protected]).
Major depressive disorder (MDD) is a chronic illness, with most recent evidence suggesting 12-month prevalence in the United States ranging from 5.28%1 to 6.6%2 for adults 18 years of age or older. Moreover, 13.23%1 to 16.2%2 of adults will experience a major depressive episode during their lifetime. Additionally, it has been estimated that the lifetime prevalence of depression symptoms is approximately 23%.3 Depression was recognized by the World Health Organization as the “leading cause of disability”4 worldwide and “the fourth leading contributor to the global burden of disease”4 in the year 2000.
Lifetime prevalence of MDD is higher among females; individuals less than 65 years of age; those who have been widowed, separated, or divorced; and those at the lowest income levels.1 With the exception of Native Americans, those who belong to a minority racial or ethnic group (black, Hispanic, and Asian) have lower prevalence of MDD compared to white persons.1 Depression is more common in patients with chronic diseases (eg, diabetes, cardiovascular and cerebrovascular disease, cancer, pain, and obesity)5 and is associated with increased physical symptoms, functional disability and impairment, poor adherence to medical treatment and self-care, and increased medical costs, compared to the general population.6
Clinical Points
- The overall extent of depression screening appears to be low.
- Primary care physicians play an important role in depression screening.
- Depression screening appears to be underutilized in diabetics and males.
Despite its significant contribution to medical care burden, MDD is underrecognized in the primary care setting. One study noted that only 64% of patients with a confirmed diagnosis of major depression were identified by their primary care provider as being psychologically distressed and that up to 50% of depressed patients remain undiagnosed.7
In 2002, the US Preventive Services Task Force (USPSTF) updated their 1996 report, recommending “screening adults for depression in clinical practices that have systems in place to assure accurate diagnosis, effective treatment, and follow-up.”8(p760) Although depression screening is recommended, the USPSTF guidelines do not specify an optimal screening interval. Although screening for depression remains a critical first step in identifying individuals suffering with or at risk for depression, a review of the literature revealed a dearth of research describing the probability of depression screening at community-based physician practice visits. Moreover, little is known about variations in depression screening as it relates to key patient and physician characteristics. Therefore, this research sought to (1) estimate the probability of depression screening in a nationally representative sample of community-based physician practice visits and (2) describe variations in the probability of depression screening by patient and physician visit characteristics.
METHOD
Study Design Overview
This research used cross-sectional data from the 2005-2007 National Ambulatory Medical Care Survey (NAMCS)9,10 to assess the proportion of adult, community-based, physician practice visits in which depression screening was performed and to evaluate variations in screening based on patient and physician visit characteristics. This study was granted exempt from review status by the University of Oklahoma Institutional Review Board because it used publicly available, deidentified data.
Data Source
The NAMCS is an annual, nationwide, multistage, probability-based sample survey of ambulatory physician office visits performed by the National Center for Health Statistics. The sampling design and data collection methods are described in detail elsewhere,9,10 and the data are publicly available (http://www.cdc.gov/nchs/ahcd.htm). Each record in the NAMCS is assigned a patient weight (ie, inflation factor) that is a mathematical adjustment provided by the National Center for Health Statistics to account for complex sampling design and allow for estimation of national population parameters from the number of sampled visits.
Data Inclusion and Exclusion Criteria
Together, the raw NAMCS data files for 2005 to 2007 contained 87,835 unique visits. The USPSTF guidelines recommend routine depression screening only in adults, as there are inadequate data to support or recommend against depression screening in children. Therefore, only visits for patients ≥ 18 years of age were used. Also excluded were patient visits with a primary reason for visit related to injuries, adverse effects, test results, administrative codes (eg, examinations required for employment, licensing, Social Security disability), and uncodable items (eg, insufficient information), as it is unlikely that depression screening would occur at these types of visits. Additionally, only visits with complete data on all variables of interest were used in multivariable analyses, leaving a final analytic sample of 55,143 visits that represented a population of 1,741,090,686 community-based physician visits.
Study Variables
Variable selection for this research was guided by the framework for the study of access to medical care.11,12 The dependent variable in this research was the order for or provision of depression screening as recorded in the medical record. Data abstractors use a defined response set of yes or no to document depression screening on the NAMCS patient record form. Detail about the type and intensity of screening is not known. Independent variables included predisposing immutable characteristics, perceived and evaluated need characteristics, and mutable and immutable enabling characteristics of the population at risk.
Predisposing immutable characteristics included patient sex, age group, and race/ethnicity. Sex was defined as male or female. A 3-level age variable was defined as 18 to 39 years, 40 to 64 years, or ≥ 65 years. Race and ethnicity were defined as white (non-Hispanic), black (non-Hispanic), Hispanic, or other (ie, Asian, Native Hawaiian/Other Pacific Islander, American Indian/Alaska Native, multiple races).
Perceived and evaluated need characteristics of the population at risk included major reason for visit, presence of chronic disease, established patient status, and visit history. Major reasons for visit included acute care, chronic care (ie, routine or flare-up), or preventive care. Visit history was defined as a 5-level variable including patients who were new to the practice or established patients with 0, 1-2, 3-5, or 6 or more prior visits within the previous 12 months.
Chronic disease was conceptualized in a number of ways. The NAMCS dataset contains indicator variables for 14 common, chronic conditions (arthritis, asthma, cancer, cerebrovascular disease, congestive heart failure, chronic renal failure, chronic obstructive pulmonary disease, depression, diabetes mellitus, hyperlipidemia, hypertension, ischemic heart disease, obesity, and osteoporosis). To examine bivariate relationships between depression screening and each chronic disease, individual indicator variables for each of the chronic conditions were used, with the exception of chronic renal failure due to insufficient sample size. Also, vascular-related diseases, including cerebrovascular disease, ischemic heart disease, and congestive heart failure, were combined into a single disease indicator variable due to limited sample size. In addition, a unique, dichotomous indicator variable was defined as the presence or absence of at least 1 of 13 common, chronic conditions, excluding a diagnosis of depression. Finally, a 4-level indicator variable combining the presence or absence of depression and presence or absence of all other chronic conditions was created to describe each patient visit encounter as having no chronic disease, depression only, any chronic diseases without depression, and any chronic diseases with depression.
Mutable and immutable enabling characteristics included primary care provider status, expected payment type, geographic region, and metropolitan statistical area status. Visits were defined as seeing either a primary care or nonprimary care physician. Expected payment types included private insurance, Medicare, Medicaid, and other (ie, worker’s compensation, self-pay, no charge, other payment type, or unknown payment type). Geographic regions were defined as Northeast, Midwest, South, or West. To control for physician visits in both rural and urban settings, visits were defined as whether or not they occurred within a metropolitan statistical area.
Analysis
Univariate statistics were computed to profile the study population. Bivariate and multivariable associations between depression screening and predisposing, need, and enabling variables were evaluated. For bivariate analyses, a design-based F statistic for complex samples was used.
Ideally, it would be best to stratify the analytic sample by visits with and without patients with a diagnosis of depression to allow for an evaluation of the differences in physician-reported screening for each of the sample subgroups. However, the reported International Classification of Diseases, Ninth Revision (ICD-9) codes are not sufficiently specific to differentiate between a patient with a reported diagnosis of depression who was both screened and diagnosed at the sampled visit or a patient whose diagnosis of depression was ongoing, suggesting disease monitoring rather than screening. In addition, stratification of the sample by diagnosis of depression reduces the sample in each of the strata so as to create unstable estimates for some study covariates, especially with respect to subgroup analyses by physician type. In the absence of an ideal method to accurately remove patients with a prior depression diagnosis and to preserve sample size and external validity, visits with a diagnosis of depression were retained. An indicator variable for the depression comorbidity was included in all multivariable analyses to help control for the diagnosis of depression and allow for independent interpretation of study covariates.
A secondary, multivariable logistic regression was also performed using a subsample of physician visits restricted to primary care specialties of family, general, and internal medicine. The subset analysis was conducted to describe variations in depression screening for the specific physician subgroups to which the USPSTF depression screening guidelines are targeted. For the subset analysis, race/ethnicity categories of black non-Hispanic and Hispanic were combined due to sample size limitations.
For all analyses, the a priori α level was .05. All data management and analyses were performed in Stata version 10.1,13 using complex survey commands with Taylor-linearized variance estimation, sampling weights, and masked sampling design variables provided in the NAMCS dataset.
RESULTS
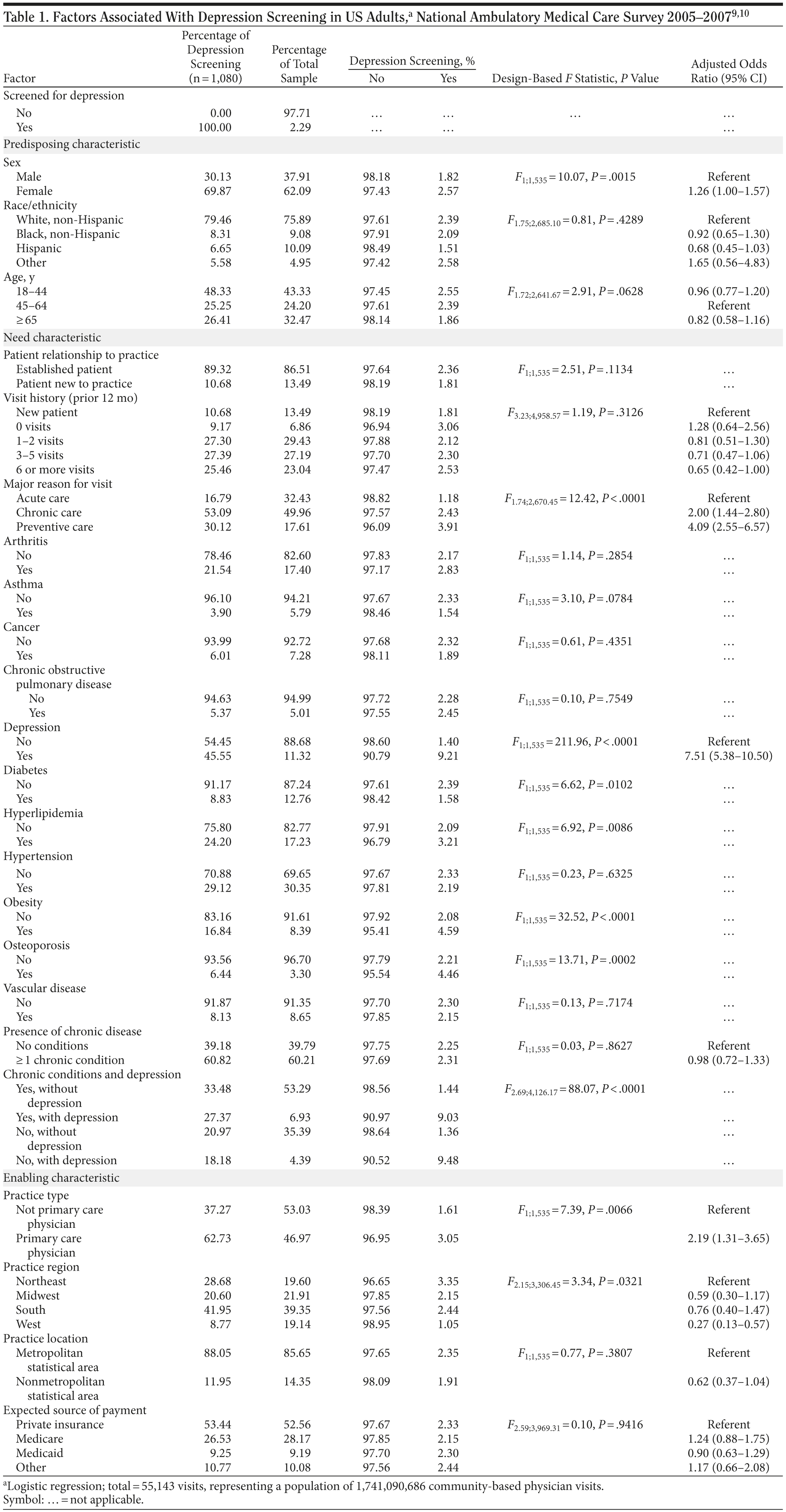
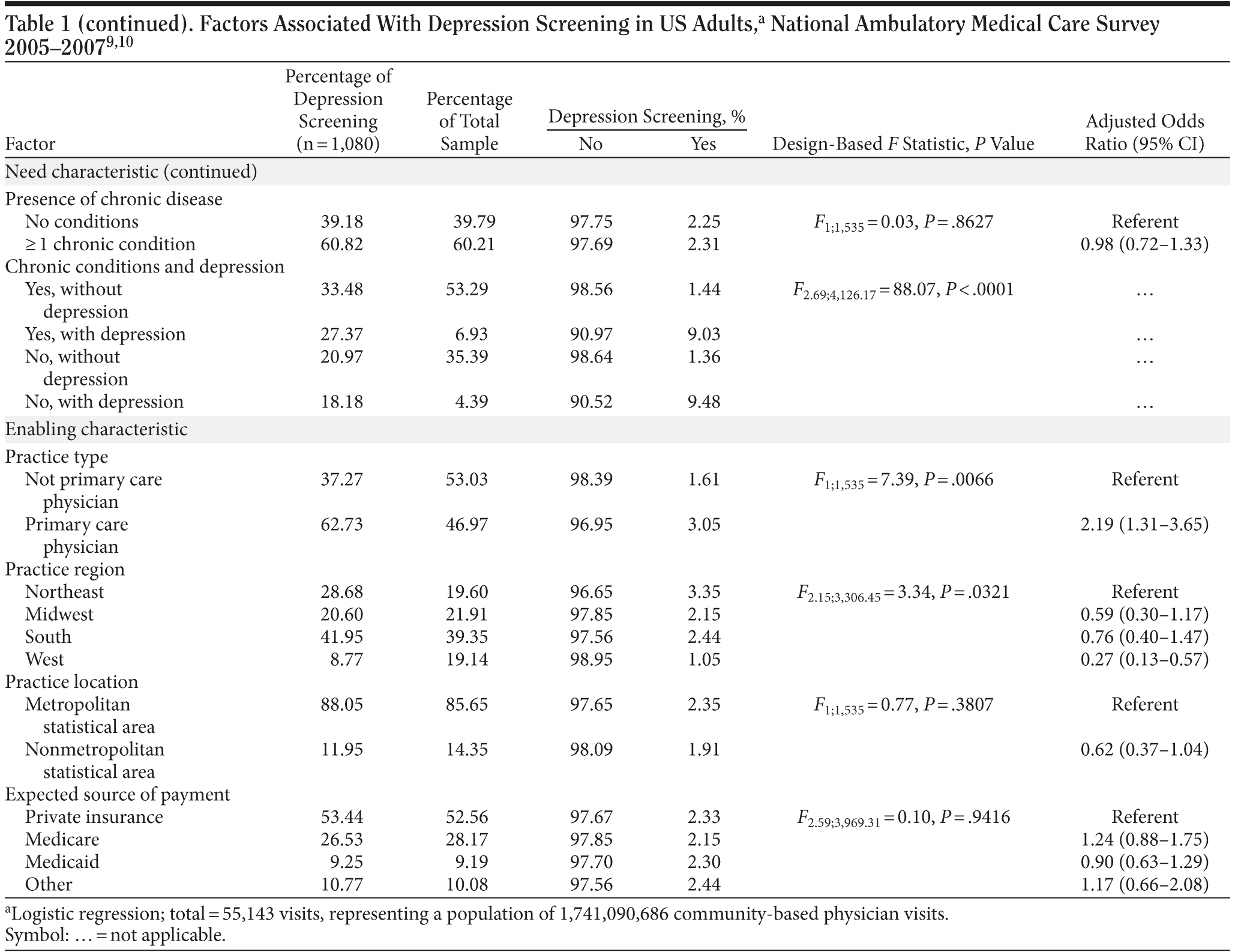
The 2005-2007 NAMCS dataset included 87,835 visits, representing almost 2.9 billion (2,859,892,874) community-based physician practice visits. After exclusion criteria were applied, the analytic sample size was 55,143 community-based physician practice visits, which represents the study population of 1.7 billion (1,741,090,686) office visits by US adult (aged ≥ 18 years) patients. Henceforth, the results are presented and discussed at the population level. Table 1 describes the distribution of predisposing, need, and enabling characteristics of the study population; the probability of depression screening; and variation of depression screening by these characteristics. Physician visits involved patients who were predominantly female (62.09%), white (75.89%), and less than 65 years of age (67.53%). The majority of visits (60.21%) included patients with a chronic condition (excluding depression) and involved established patients (86.51%) with 3 or more visits during the previous year (50.23%). Depression was reported at 11.32% of visits. Depression screening occurred at 2.29% of the community-based physician practice visits.
There were several significant bivariate associations between predisposing, need, and enabling characteristics and depression screening. Compared to males, females were more likely to be screened for depression (2.57% vs 1.82%, F1;1,535 = 10.07, P = .0015). Visits involving patients with hyperlipidemia (3.21% vs 2.09%, F1;1,535 = 6.92, P = .0086), obesity (4.59% vs 2.08%, F1;1,535 = 32.52, P < .0001), osteoporosis (4.46% vs 2.21%, F1;1,535 = 13.71, P = .0002), or depression (9.21% vs 1.40%, F1;1,535 = 211.96, P < .0001) were associated with an increased likelihood of depression screening. In contrast, visits with patients who had diabetes were less likely to include depression screening (1.58% vs 2.39%, F1;1,535 = 6.62, P = .0102). Depression screening was most common for preventive care visits followed by visits for chronic and acute problems, respectively (3.91% vs 2.43% vs 1.18%, F1.74;2,670.45 = 12.42, P < .0001). Additionally, primary care physicians were more likely to screen for depression than specialists (3.05% vs 1.61%, F1;1,535 = 7.39, P = .0066). Finally, physician visits in the West were less likely to include screening for depression compared to those in the Northeast (1.05% vs 3.35%, F2.15;3,306.45 = 3.34, P = .0321).
Most bivariate relationships did not change in multivariable analysis (Table 1). Females were more likely to be screened for depression (adjusted odds ratio (AOR) = 1.26; 95% CI, 1.00-1.57). Visits involving a patient with a diagnosis of depression (AOR = 7.51; 95% CI, 5.38-10.50) were more likely to include depression screening, as were visits with primary care physicians (AOR = 2.19; 95% CI, 1.31-3.65) and visits for preventive (AOR = 4.09; 95% CI, 2.55-6.57) and chronic problems (AOR = 2.00; 95% CI, 1.44-2.80) when compared to visits for acute problems. Physician visits in the West region were less likely than visits in the Northeast to include screening for depression (AOR = 0.27; 95% CI, 0.13-0.57).
The multivariable logistic regression results attained from the analysis on the subset of family, general, and internal medicine practitioners were very similar to the overall results attained, with the exception of the sex variable, which was not significantly associated with depression screening (AOR = 1.21; 95% CI, 0.95-1.54; results not shown).
DISCUSSION
This research describes depression screening in community-based physician practices and explores factors that may be associated with depression screening. Given the prevalence of depression is estimated to range from 5.28% to 6.6% annually and from 13.23% to 16.2% over a lifetime,1,2 it appears that the overall probability of depression screening at a given physician visit is low, as it was documented at only 2.29% of the estimated 1.7 billion adult physician visits during 2005 to 2007. These findings may be in part due to the cyclical1,2,4 nature of depression and possibly due to the ambiguity regarding how and when to screen for depression14 as well as how to implement guidelines in practice.15 Additionally, a lack of appropriate resources specified in the 2002 screening recommendations developed by the USPSTF8 may be a potential health system barrier that may adversely affect the probability of screening in the ambulatory care setting. The need for appropriate resources is further emphasized in the newly updated USPSTF guidelines16 and may continue to play a role in the apparently low proportion of patient visits that result in depression screening. The new guidelines place an increased emphasis on screening for depression only when sufficient “staff-assisted depression care supports are in place to assure accurate diagnosis, effective treatment, and follow-up.”16(p784) Certainly, future research should seek to define the optimal depression screening interval.
In addition, other barriers that lower depression screening rates may include physician beliefs and knowledge about “depression” as well as its diagnosis and treatment, skill deficits in patient interviewing, and medicalization of depression symptoms.17 Health system barriers that may contribute to reduced depression screening rates include physician visit time constraints, competing clinical priorities, limitations in third-party coverage and treatment access, and discontinuity of care.17 Stigma and denial of depression symptoms are among the patient-level factors that may reduce depression screening rates.17
Despite research documenting significant increases in antidepressant use in the United States,18,19 depression screening remains a relatively unexplored area. Several patient and visit characteristics demonstrated significant variation with respect to depression screening in the community-based physician practice setting, even after controlling for the presence of a depression diagnosis in multivariable analysis.
Sex
Consistent with research demonstrating a higher prevalence of diagnosed depression,1 females also demonstrated significantly higher odds of being screened for depression in multivariable analysis while controlling for the presence of depression. Importantly, the potential variation may very likely contribute to underdiagnosis and, subsequently, the decreased prevalence of depression reported for men. Raising awareness of depression in men has been recognized by the National Institute for Mental Health,20 and the current findings from this research support the need for continued efforts in the area.
Age
Although depression is more prevalent in younger adults,1 depression screening does not appear to vary across age groups. This discrepancy is most likely due to presence of the depression indicator variable in the multivariable analysis. Once the depression indicator was removed from the multivariable model, those ≥ 65 years of age were significantly less likely to be screened for depression than middle-aged adults, 40-64 years old (result not shown). However, many elderly patients who have undiagnosed depression may not be screened, resulting in a missed opportunity for treatment.
Chronic Disease
Given the common depression comorbidity with chronic disease,5,17 one might suspect higher depression screening rates in patients with chronic disease. However, there was no significant difference in the odds of being screened for depression based on the presence of at least 1 chronic disease in multivariable analyses. One possible explanation for this result may be controlling for depression separately from other chronic diseases within the multivariable model, supporting the hypothesis of medicalization of depression symptoms that may be evident in chronic disease. Another explanation may be commonly shared variance among other variables in the model that explain chronic disease. For example, the likelihood of depression screening is significantly higher when the major reason for a physician visit was related to a chronic problem or preventive care as compared to acute care visits. While depression screening would be expected to more likely occur at chronic or preventive care visits compared to acute care visits, a post hoc analysis found that removal of the major reason for visit indicator for chronic conditions failed to change the significance of the chronic disease indicator (results not shown).
Individual chronic diseases were not included in the multivariable analysis to avoid model oversaturation. However, as evidenced in bivariate analyses, visits involving patients with depression were associated with increased likelihood of depression screening, as expected, along with visits involving patients with hyperlipidemia, obesity, and osteoporosis. A point of concern is that visits involving patients with diabetes were associated with a decreased likelihood of depression screening. Previous research has suggested that depression is twice as likely in patients with diabetes compared to those without diabetes,21 whereas other work has suggested that this difference is mitigated after controlling for the number of outpatient visits.22 In this research, a post hoc multivariable analysis (result not shown) confirmed that screening for depression is less likely at visits with patients who have diabetes, even while controlling for the number of visits in the previous year in multivariable analysis, suggesting a clear opportunity for increasing depression screening with diabetic patients.
Visit History
The multivariable analysis did detect significantly decreased odds for a patient to be screened when the number of visits increased to 6 or more, compared to a new patient. This is to be expected. However, it is important to note the nonsignificant findings for all other levels of patient visit history. Once again, these results may be in part due to the cyclical1,2,4 nature of depression and possibly due to the ambiguity regarding how and when to screen for depression14 as well as how to implement guidelines in practice.15
Physician Specialty
One would expect, under normal circumstances, that a patient’s primary care physician would be the physician more likely to conduct depression screening, as primary care physicians are the focus of the USPSTF guidelines for depression screening. The results indicate that a visit with a primary care physician more than doubled the odds of screening for depression and supports the belief that primary care physicians fill a significant role in triaging for depression and its subsequent care management. Incentives to reinforce and further advance this practice should be considered to optimize depression screening efforts.
Geographic Region
While the prevalence of depression does not appear to vary by region of the country,1 the West region of the country had significantly lower odds of depression screening at a physician visit when compared to the Northeast region. This result may reflect variations in physician practice patterns23 and suggest an opportunity for increasing depression screening awareness, especially in the West.
Limitations
Several limitations must be considered when interpreting the results of this research. Due to the use of patient visits as the unit of analysis, the estimates may differ from a patient-based prevalence of depression screening. Additionally, this research used NAMCS data abstracted from patient records at physician practices and can be subject to interpretation, recording, and/or transcription error. The dependent variable used in this research represents a documented effort in the physician medical record to screen patients for depression. Although specific depression screening strategies used remain unknown, the NAMCS data currently represent the best national effort to quantify physician efforts to screen for depression. Future research should also strive to define the type and intensity of depression screening. It is also possible that a physician extender (eg, nurse practitioner, physician assistant) may have seen the patient in lieu of a physician. When restricting the dataset to only visits in which a physician spent time with the patient, interpretation varied only slightly, with visits including Hispanic patients and locations in nonmetropolitan statistical areas (ie, rural) significantly less likely to include screening for depression (result not shown). However, these results are expected, as physician extenders fulfill an important role in underserved communities.
CONCLUSIONS
Depression screening is an essential first step for identifying patients at risk for depression, and its implementation in primary care practice is supported by the USPSTF guidelines.16 Unfortunately, the probability of depression screening at community-based physician practice visits in the United States is low (2.29%) and may reflect the ambiguity related to the optimal screening interval for depression and/or the lack of incentives and defined implementation strategy to ideally provide depression screening. Opportunities exist to improve routine depression screening at physician visits, especially in males, in patients with chronic disease (particularly diabetes), and in the western region of the United States.
Author affiliations: Department of Pharmacy, Clinical and Administrative Sciences, College of Pharmacy, University of Oklahoma, Oklahoma City (Dr Harrison) and Tulsa (Drs Miller and Schmitt); and Department of Psychiatry, School of Community Medicine, University of Oklahoma, Tulsa (Dr Touchet).
Author contributions: Dr Harrison was responsible for primary data analysis, data synthesis, and manuscript preparation. Dr Miller was responsible for concept generation, data analysis and synthesis, and manuscript preparation. Dr Schmitt was responsible for secondary data analysis and manuscript preparation. Dr Touchet was responsible for manuscript preparation.
Potential conflicts of interest: All authors declare that they have no potential conflicts of interest, including specific financial interests and relationships and affiliations relevant to the subject matter or materials discussed in the manuscript.
Funding/support: No financial or material support or assistance was received by any of the authors in the conduct of this research or the preparation of this manuscript.
Disclaimer: All authors had full access to the publicly available National Ambulatory Medical Care Survey data and take responsibility for the integrity of the data and the accuracy of the data analysis.
REFERENCES
1. Hasin DS, Goodwin RD, Stinson FS, et al. Epidemiology of major depressive disorder: results from the National Epidemiologic Survey on Alcoholism and Related Conditions. Arch Gen Psychiatry. 2005;62(10):1097-1106.PubMed doi:10.1001/archpsyc.62.10.1097
2. Kessler RC, Berglund P, Demler O, et al. National Comorbidity Survey Replication. The epidemiology of major depressive disorder: results from the National Comorbidity Survey Replication (NCS-R). JAMA. 2003;289(23):3095-3105.PubMed doi:10.1001/jama.289.23.3095
3. Johnson J, Weissman MM, Klerman GL. Service utilization and social morbidity associated with depressive symptoms in the community. JAMA. 1992;267(11):1478-1483.PubMed doi:10.1001/jama.267.11.1478
4. World Health Organization. Depression: what is depression? http://www.who.int/mental_health/management/depression/definition/en/. Accessed April 25, 2009.
5. Evans DL, Charney DS, Lewis L, et al. Mood disorders in the medically ill: scientific review and recommendations. Biol Psychiatry. 2005;58(3):175-189.PubMed doi:10.1016/j.biopsych.2005.05.001
6. Katon W, Ciechanowski P, Katon W, et al. Impact of major depression on chronic medical illness. J Psychosom Res. 2002;53(4):859-863.PubMed doi:10.1016/S0022-3999(02)00313-6
7. Simon GE, VonKorff M. Recognition, management, and outcomes of depression in primary care. Arch Fam Med. 1995;4(2):99-105.PubMed doi:10.1001/archfami.4.2.99
8. US Preventive Services Task Force. Screening for depression: recommendations and rationale. Ann Intern Med. 2002;136(10):760-764. PubMed
9. National Center for Health Statistics. NAMCS micro-data file documentation. 2005; ftp://ftp.cdc.gov/pub/Health_Statistics/NCHS/Dataset_Documentation/NAMCS/doc05.pdf. Accessed July 7, 2009.
10. National Center for Health Statistics. NAMCS micro-data file documentation. 2006; ftp://ftp.cdc.gov/pub/Health_Statistics/NCHS/Dataset_Documentation/NAMCS/doc06.pdf. Accessed July 7, 2009.
11. Aday LA, Andersen R. A framework for the study of access to medical care. Health Serv Res. 1974;9(3):208-220. PubMed
12. Aday LA, Andersen RM. Equity of access to medical care: a conceptual and empirical overview. Med Care. 1981;19(12):4-27. doi:10.1097/00005650-198112001-00004 PubMed
13. Stata Statistical Software [computer program], version 10. College Station, TX: StataCorp LP; 2007.
14. Nease DE Jr, Maloin JM. Depression screening: a practical strategy. J Fam Pract. 2003;52(2):118-124. PubMed
15. Kilbourne AM, Daugherty B, Pincus HA. What do general medical guidelines say about depression care? depression treatment recommendations in general medical practice guidelines. Curr Opin Psychiatry. 2007;20(6):626-631.PubMed doi:10.1097/YCO.0b013e3282f0c4d3
16. US Preventive Services Task Force. Screening for depression in adults: US Preventive Services Task Force recommendation statement. Ann Intern Med. 2009;151(11):784-792. PubMed
17. Goldman LS, Nielsen NH, Champion HC. Awareness, diagnosis, and treatment of depression. J Gen Intern Med. 1999;14(9):569-580.PubMed doi:10.1046/j.1525-1497.1999.03478.x
18. Olfson M, Marcus SC. National patterns in antidepressant medication treatment. Arch Gen Psychiatry. 2009;66(8):848-856.PubMed doi:10.1001/archgenpsychiatry.2009.81
19. Compton WM, Conway KP, Stinson FS, et al. Changes in the prevalence of major depression and comorbid substance use disorders in the United States between 1991-1992 and 2001-2002. Am J Psychiatry. 2006;163(12):2141-2147.PubMed doi:10.1176/appi.ajp.163.12.2141
20. Rochlen AB, Whilde MR, Hoyer WD. The real men: real depression campaign: overview, theoretical implications, and research considerations. Psychol Men Masc. 2005;6(3):186-194. doi:10.1037/1524-9220.6.3.186
21. Anderson RJ, Freedland KE, Clouse RE, et al. The prevalence of comorbid depression in adults with diabetes: a meta-analysis. Diabetes Care. 2001;24(6):1069-1078.PubMed doi:10.2337/diacare.24.6.1069
22. O’ Connor PJ, Crain AL, Rush WA, et al. Does diabetes double the risk of depression? Ann Fam Med. 2009;7(4):328-335.PubMed doi:10.1370/afm.964
23. Kramer TL, Daniels AS, Zieman GL, et al. Psychiatric practice variations in the diagnosis and treatment of major depression. Psychiatr Serv. 2000;51(3):336-340.PubMed doi:10.1176/appi.ps.51.3.336