Objective: To compare prevalence rates of alcohol, nicotine, and other drug use and major psychiatric disorders (major depressive disorder, persistent depression, bipolar I disorder, agoraphobia, social and specific phobias, and antisocial, schizotypal, and borderline personality disorders) between US-born and foreign-born Mexican Americans and non-Hispanic whites and between early entry versus later-entry foreign-born Mexican Americans and non-Hispanic whites.
Methods: Data were derived from face-to-face interviews in the 2012-2013 National Epidemiologic Survey on Alcohol and Related Conditions-III (N = 36,309).
Results: US-born Mexican Americans and US-born non-Hispanic whites were at greater risk (P < .05) of alcohol, nicotine, and any drug use and their associated disorders and other DSM-5 psychiatric disorders relative to their foreign-born counterparts. US-born non-Hispanic whites were more likely (P < .05) to use substances and develop many psychiatric disorders relative to US-born Mexican Americans. Foreign-born Mexican Americans < 18 years old at immigration were at greater risk of drug use, drug use disorders, and nicotine use disorder compared with foreign-born Mexican Americans ≥ 18 years old at immigration. Foreign-born non-Hispanic whites < 18 years old at immigration were more likely to use substances and to develop many psychiatric disorders relative to foreign-born non-Hispanic whites ≥ 18 years old at immigration.
Conclusions: Taken together, the findings of this study support the healthy immigrant hypothesis and adverse role of acculturation for US-born and foreign-born Mexican Americans and non-Hispanic whites. Further research is warranted on immigration status and age at arrival into the United States and those processes underlying differential exposure to substances and development of psychiatric conditions. An understanding of these processes can be invaluable to clinicians in guiding culturally sensitive and informed prevention and intervention efforts.
Substance Use and Psychiatric Disorders Among Mexican Americans and Non-Hispanic Whites by Immigration Status
ABSTRACT
Objective: To compare prevalence rates of alcohol, nicotine, and other drug use and major psychiatric disorders (major depressive disorder, persistent depression, bipolar I disorder, agoraphobia, social and specific phobias, and antisocial, schizotypal, and borderline personality disorders) between US-born and foreign-born Mexican Americans and non-Hispanic whites and between early entry versus later-entry foreign-born Mexican Americans and non-Hispanic whites.
Methods: Data were derived from face-to-face interviews in the 2012–2013 National Epidemiologic Survey on Alcohol and Related Conditions-III (N = 36,309).
Results: US-born Mexican Americans and US-born non-Hispanic whites were at greater risk (P < .05) of alcohol, nicotine, and any drug use and their associated disorders and other DSM-5 psychiatric disorders relative to their foreign-born counterparts. US-born non-Hispanic whites were more likely (P < .05) to use substances and develop many psychiatric disorders relative to US-born Mexican Americans. Foreign-born Mexican Americans < 18 years old at immigration were at greater risk of drug use, drug use disorders, and nicotine use disorder compared with foreign-born Mexican Americans ≥ 18 years old at immigration. Foreign-born non-Hispanic whites < 18 years old at immigration were more likely to use substances and to develop many psychiatric disorders relative to foreign-born non-Hispanic whites ≥ 18 years old at immigration.
Conclusions: Taken together, the findings of this study support the healthy immigrant hypothesis and adverse role of acculturation for US-born and foreign-born Mexican Americans and non-Hispanic whites. Further research is warranted on immigration status and age at arrival into the United States and those processes underlying differential exposure to substances and development of psychiatric conditions. An understanding of these processes can be invaluable to clinicians in guiding culturally sensitive and informed prevention and intervention efforts.
Prim Care Companion CNS Disord 2019;21(1):18m02359
To cite: Kerridge BT, Chou SP, Pickering RP. Substance use and psychiatric disorders among Mexican Americans and non-Hispanic whites by immigration status. Prim Care Companion CNS Disord. 2019;21(1):18m02359.
To share: https://doi.org/10.4088/PCC.18m02359
© Copyright 2019 Physicians Postgraduate Press, Inc.
aEpidemiology and Biometry Branch, National Institute on Alcohol Abuse and Alcoholism, Rockville, Maryland
*Corresponding author: Bradley T. Kerridge, PhD, Epidemiology and Biometry Branch, National Institute on Alcohol Abuse and Alcoholism, 5635 Fishers Lane, Room 3075, Rockville, MD 20852 ([email protected]).
Hispanics are the largest ethnic minority in the United States, representing 55.4 million Americans.1 Current population projections predict a doubling of the Hispanic population by 2060 to 119 million.1 Mexican Americans are the largest Hispanic subgroup today, constituting about 63% of the US Hispanic population.2 Considering the size and projected increases in the population of Mexican Americans in the United States, current knowledge of substance use and psychiatric morbidity among them is of public health and clinical care importance. Central to this knowledge is whether immigration status and age at entry into the United States affect the risk of substance use and psychiatric disorders.
Early large-scale epidemiologic surveys3–8 have compared foreign-born Mexican Americans with their US-born counterparts and non-Hispanic whites. In general, these studies found that for most psychiatric disorders (1) US-born Mexican Americans had greater rates than foreign-born Mexican Americans and (2) rates among US-born Mexican Americans were comparable to US-born non-Hispanic whites. Similar results have also been found for alcohol and other drug use.9–13
Some of these studies4,7,8 compared US-born and foreign-born Mexican Americans with the entire non-Hispanic white population with no regard to immigration status, thereby confounding race-ethnicity with immigration status. Only 1 study6 used a US-born non-Hispanic white comparison group, and 1 study compared US-born and foreign-born Mexican Americans with US-born and foreign-born non-Hispanic whites.5 The latter comparison group is important in determining if lower rates of substance use and psychiatric disorders found among foreign-born Mexican Americans generalize to foreign-born non-Hispanic whites.
Several prior studies8,9,11,13–15 also examined the additional effect of age at immigration (or years of residence in the United States) on prevalence of alcohol and drug use and psychiatric disorders among foreign-born Mexican Americans. In these studies,8,9,11,13–15 prevalence rates of alcohol and drug use and psychiatric disorders were greater among foreign-born Mexican Americans who arrived earlier (or resided longer) in the United States relative to those who arrived later (or resided for a shorter time). However, in these studies, rates among early versus late-entry foreign-born Mexican Americans were not directly compared, with US-born Mexican Americans consistently serving as the reference group. Further, no study to date has compared earlier- versus later-entry foreign-born Mexican Americans with earlier- versus later-entry foreign-born non-Hispanic whites. This comparison is needed to determine whether risk incurred among earlier-entry foreign-born Mexican Americans generalizes to early entry for foreign-born non-Hispanic whites.
The relationship of immigration status and age at entry to the United States and substance use and psychiatric disorders is critical, both in terms of policy and need for services. Given that Mexican Americans constitute 60% of the US Hispanic population, focus on this group is timely and important. Further, most of the previous literature in this area, including recently published articles, is based on data that are at least a decade old. This study presents current information on the prevalence of alcohol, nicotine, and other drug use and DSM-5 psychiatric disorders among US-born and foreign-born Mexican Americans and US-born and foreign-born non-Hispanic whites, along with direct comparisons between earlier- versus later-arrival foreign-born Mexican Americans and foreign-born non-Hispanic whites. Data for this study were derived from the National Epidemiologic Survey on Alcohol and Related Conditions-III (NESARC-III).16
METHODS
Sample
The 2012–2013 NESARC-III is a nationally representative, face-to-face interview survey of 36,309 adults aged 18 years and older residing in households and selected group quarters, with respondents selected through multistage probability sampling. Primary sampling units were counties or groups of census-defined blocks, and tertiary sampling units were households within sampled secondary sampling units, within which eligible adult respondents were selected. Hispanic, black, and Asian individuals were oversampled. The household response rate was 72%, the person-level response rate was 84%, and the overall response rate was 60.1%, which were comparable with other current US national surveys.17,18 Data were adjusted for nonresponse and weighted to represent the US civilian population based on the 2012 American Community Survey.19 The National Institutes of Health and Westat Institutional Review Boards approved the protocol and consent procedures.
Immigration Status
Race and ethnicity were identified by self-identification of the respondent’s origin and descent, while immigration status was determined as US born or foreign born. For the purposes of the present study, race-ethnicity and nativity were classified into 4 groups: (1) US-born Mexican Americans, (2) foreign-born Mexican Americans, (3) US-born non-Hispanic whites, and (4) foreign-born non-Hispanic whites. The non-Hispanic white subgroup in this study did not include other Hispanic subgroups (eg, Puerto Ricans, South Americans) or blacks. Foreign-born Mexican Americans and foreign-born non-Hispanic whites were further classified by age at entry into the United States before and after age 18 years.
Substance Use and Psychiatric Disorders
Substance use was defined as any lifetime use of alcohol, nicotine, or other drugs (sedatives/tranquilizers, opioids other than heroin, heroin, stimulants, hallucinogens, cannabis, cocaine, inhalants/solvents, and other drugs). Consistent with the DSM-5, lifetime alcohol use disorder (AUD), nicotine use disorder (NUD), and other drug use disorder (DUD) diagnoses required at least 2 of 11 criteria associated with each substance within the last 12 months or prior to the last 12 months. Specific drug use diagnoses were aggregated to form an overall diagnosis of any DUD.
DSM-5 lifetime mood disorder included major depressive disorder (MDD), persistent depression, and bipolar I disorder. DSM-5 lifetime anxiety disorders included panic, agoraphobia, social and specific phobia, and generalized anxiety. Consistent with DSM-5, mood and anxiety disorders excluded substance-induced and medical-illness–induced disorders. Lifetime posttraumatic stress disorder (PTSD) and schizotypal, borderline, and antisocial personality disorders (PDs) were also assessed. PTSD diagnosis generally followed the DSM-5 definition, but criteria C and D more strictly required ≥ 3 positive, rather than ≥ 2 positive, to be met.
Test-retest reliability of alcohol, nicotine, and other drug use was good to excellent.20–22 Reliability and validity of DSM-5 psychiatric disorders examined here were fair to moderate.23,24
Sociodemographic Characteristics
Sociodemographic characteristics included sex (male, female), age (18–29, 30–44, 45–64, ≥ 65 years), marital status (married or cohabitating; widowed, separated, or divorced; never married), education (< high school, high school, some college or higher), family income ($0–$19,999, $20,000–$34,999, $35,000–$69,999, ≥ $70,000), urbanicity (urban, rural), and region (Northeast, Midwest, South, West).
Statistical Analyses
Weighted cross-tabulations were used to calculate lifetime prevalence of alcohol, nicotine, and other drug use and psychiatric disorders for all comparison groups (foreign-born and US-born Mexican American and non-Hispanic whites) across sociodemographic characteristics. Differences between foreign-born and US-born Mexican Americans and non-Hispanic whites were assessed using χ2 statistics. Odds ratios derived from logistic regressions were then used to examine associations between the 4 comparison groups and lifetime alcohol, nicotine, and other drug use and specific psychiatric disorders, controlling for a broad array of sociodemographic characteristics. Prevalence rates and similar logistic regressions were used to compare foreign-born Mexican Americans and foreign-born non-Hispanic whites by age at entry to the United States (< 18 vs ≥ 18 years). All statistical analyses used SUDAAN25 to account for the complex design of the NESARC-III.
RESULTS
Sociodemographic Characteristics Among
Mexican Americans and Non-Hispanic Whites
by Immigration Status
Table 1 shows the distribution of sociodemographic characteristics among Mexican Americans and non-Hispanic whites by immigration status. There were 3,657 respondents who self-identified with Mexican-American descent of whom 1,670 were US born and 1,987 were foreign born. Of the 19,189 non-Hispanic white respondents, 18,265 were US born and 924 were foreign born.
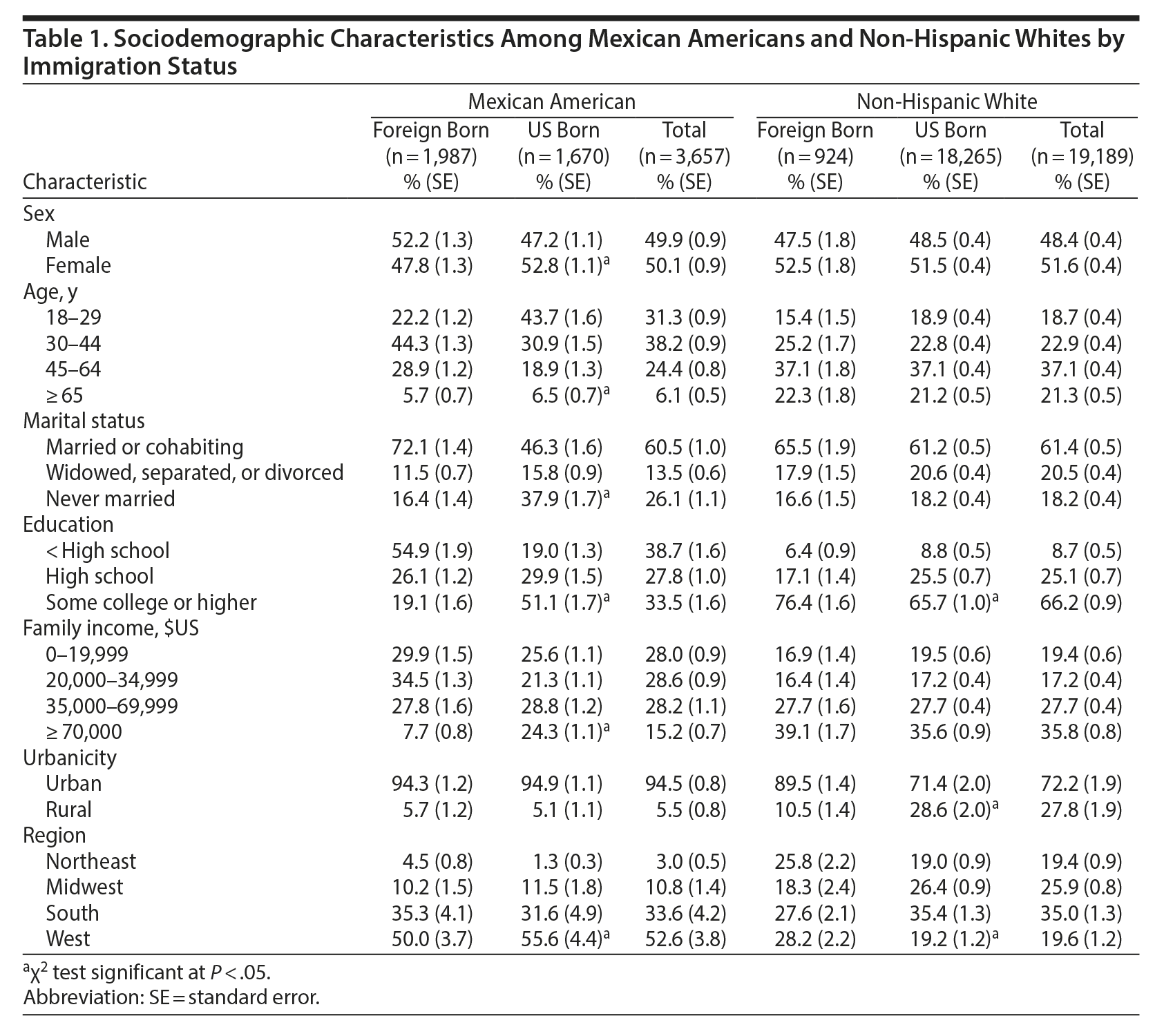
Compared to foreign-born Mexican Americans, US-born Mexican Americans were more likely to be female, younger, and never married; to have some college or higher education and greater income; and to reside in the West (χ2 P < .05). Relative to foreign-born non-Hispanic whites, US-born non-Hispanic whites were more likely to have a high school education and to reside in rural areas and in the Midwest and South (χ2 P < .05).
Substance Use and DSM-5 Psychiatric Disorders Among Mexican Americans and Non-Hispanic
Whites by Immigration Status
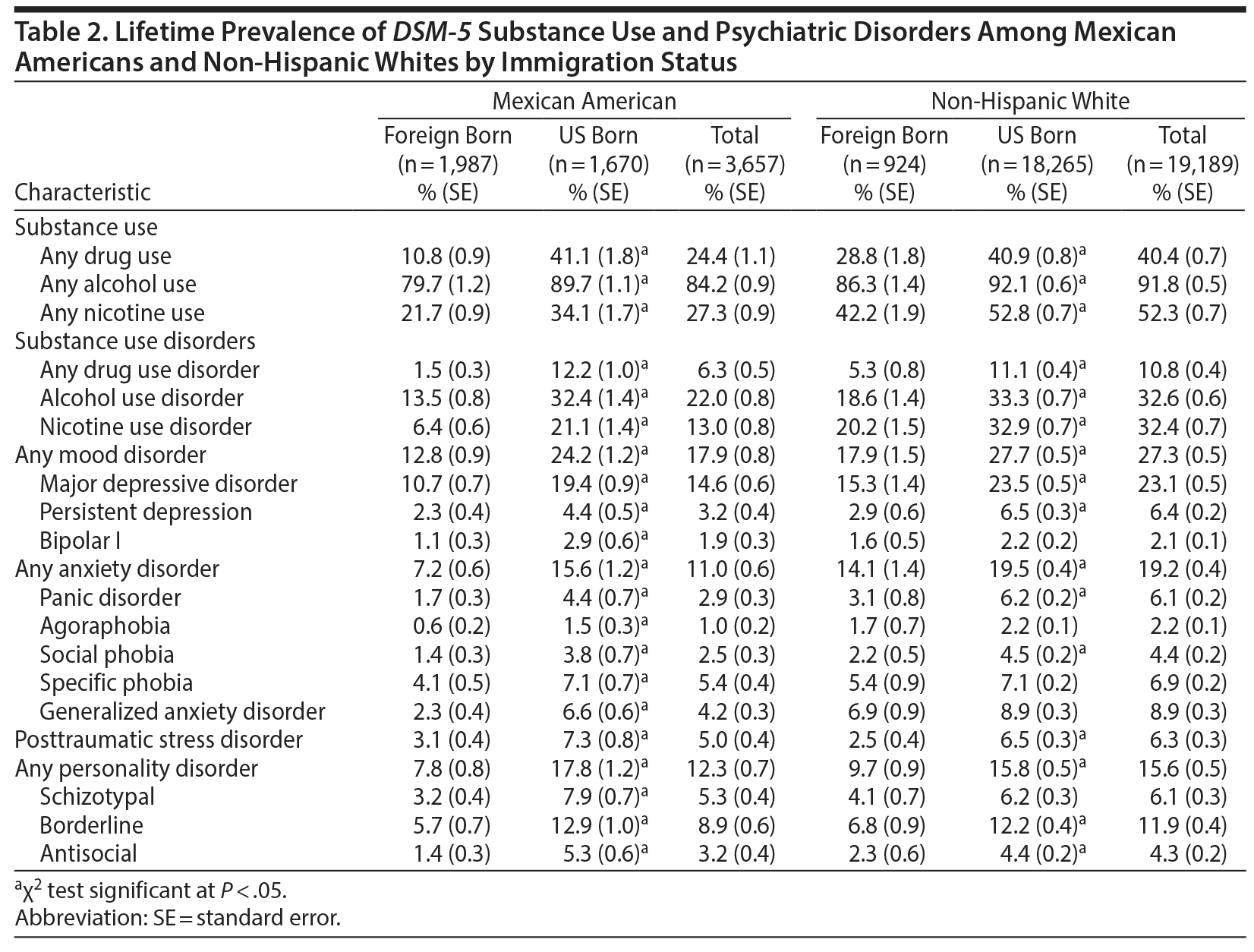
Lifetime prevalence rates of drug, alcohol, and nicotine use and all mood and anxiety disorders, PTSD, and PDs were greater among US-born Mexican Americans compared with foreign-born Mexican Americans (χ2 P < .05) (Table 2). Similarly, rates of drug, nicotine, and alcohol use and all psychiatric disorders except bipolar I disorder, agoraphobia, specific phobia, and generalized anxiety disorder (GAD) were greater among US-born non-Hispanic whites relative to foreign-born non-Hispanic whites.
Odds Ratios of Substance Use and Psychiatric Disorders Among Mexican Americans and Non-Hispanic Whites by Immigration Status
The odds of alcohol, nicotine, and drug use and all psychiatric disorders were greater among US-born non-Hispanic whites relative to foreign-born Mexican Americans and generally greater among US-born non-Hispanic whites than US-born Mexican Americans except for alcohol use, bipolar I disorder, social and specific phobias, PTSD, and schizotypal and antisocial PDs (Table 3, columns 1 and 2). US-born Mexican Americans had higher odds of all drug use and psychiatric disorders except agoraphobia compared with foreign-born Mexican Americans (Table 3, column 4). In contrast, US-born Mexican Americans had greater odds of alcohol use, AUD, PTSD, and borderline and antisocial PDs relative to foreign-born non-Hispanic whites (Table 3, column 3).
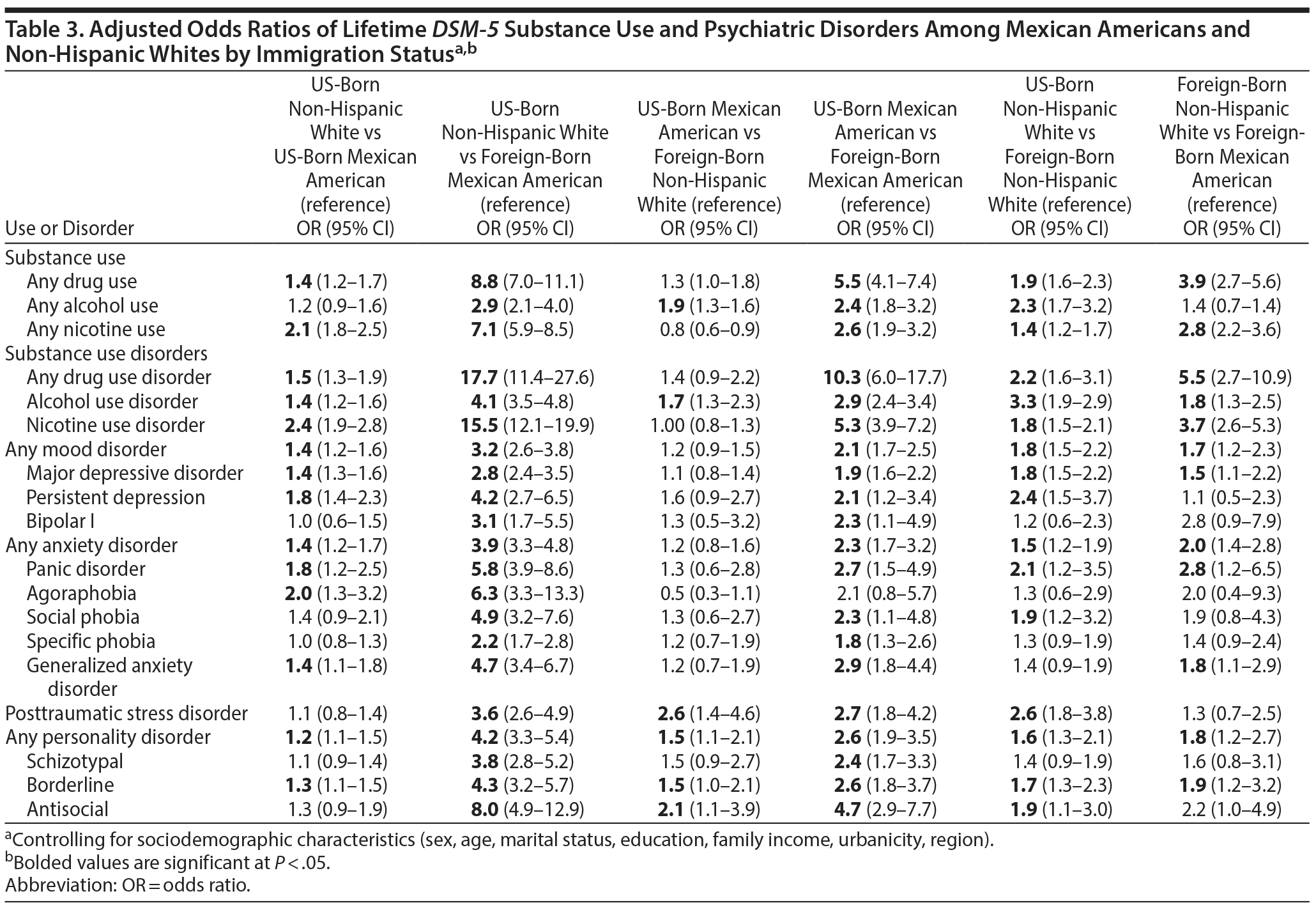
The odds of alcohol, nicotine, and drug use and associated disorders; MDD; persistent depression; panic disorder; social phobia; PTSD; and borderline and antisocial PDs were greater among US-born non-Hispanic whites compared with foreign-born non-Hispanic whites (Table 3, column 5). The odds of nicotine and drug use and DUD, AUD, NUD, MDD, panic disorder, GAD, and borderline PD were greater among foreign-born non-Hispanic whites compared with foreign-born Mexican Americans (Table 3, column 6).
Age at Immigration: Prevalence Rates and Odds Ratios
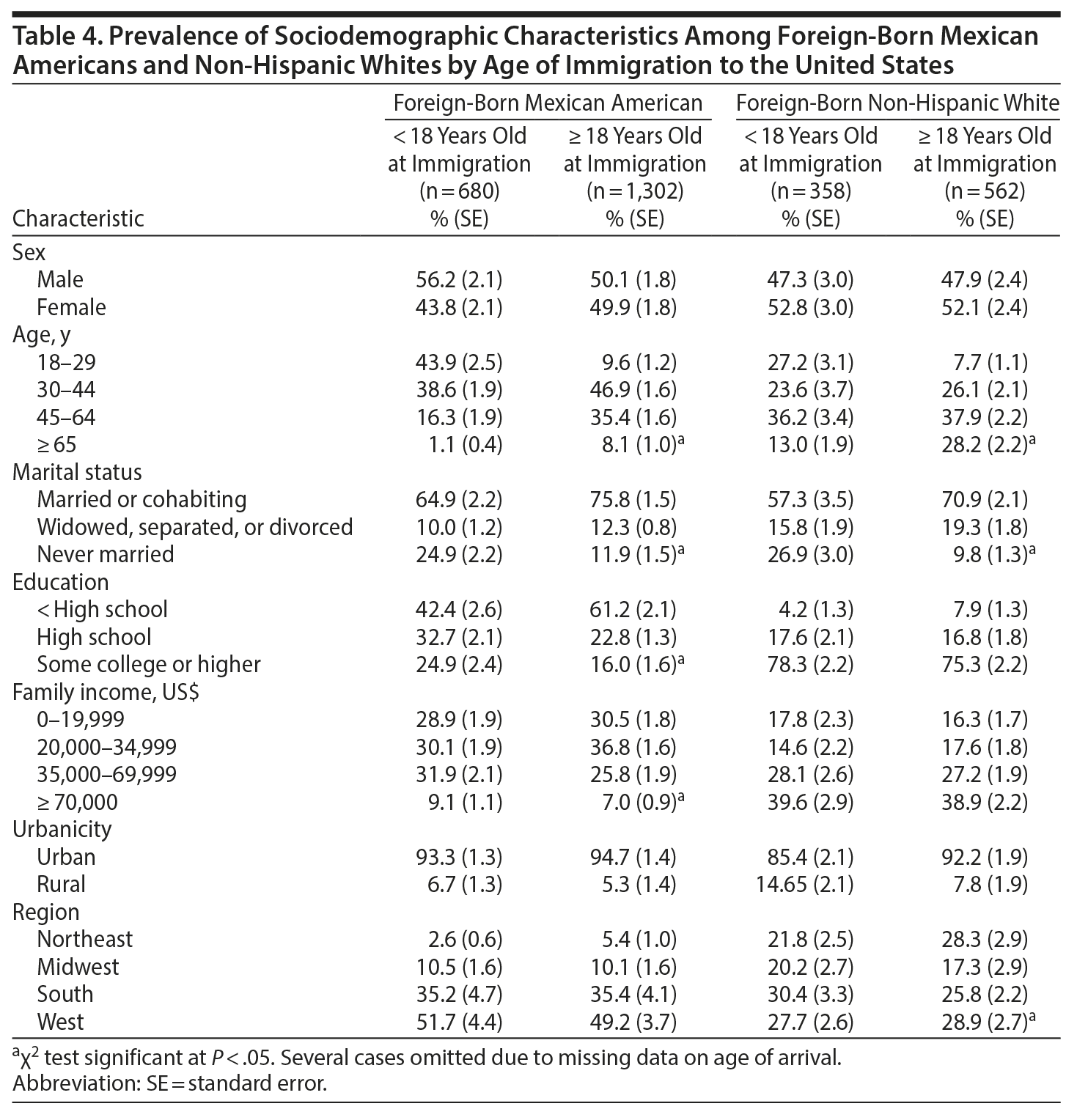
Compared to foreign-born Mexican Americans aged ≥ 18 years at immigration, foreign-born Mexican Americans < 18 years at immigration were younger and more likely to be never married and to have greater than high school education and higher incomes (Table 4). Compared to foreign-born non-Hispanic whites ≥ 18 years at immigration, foreign-born non-Hispanic whites aged < 18 years at immigration were younger and more likely to have never married and to reside in the Northeast and South (Table 4).
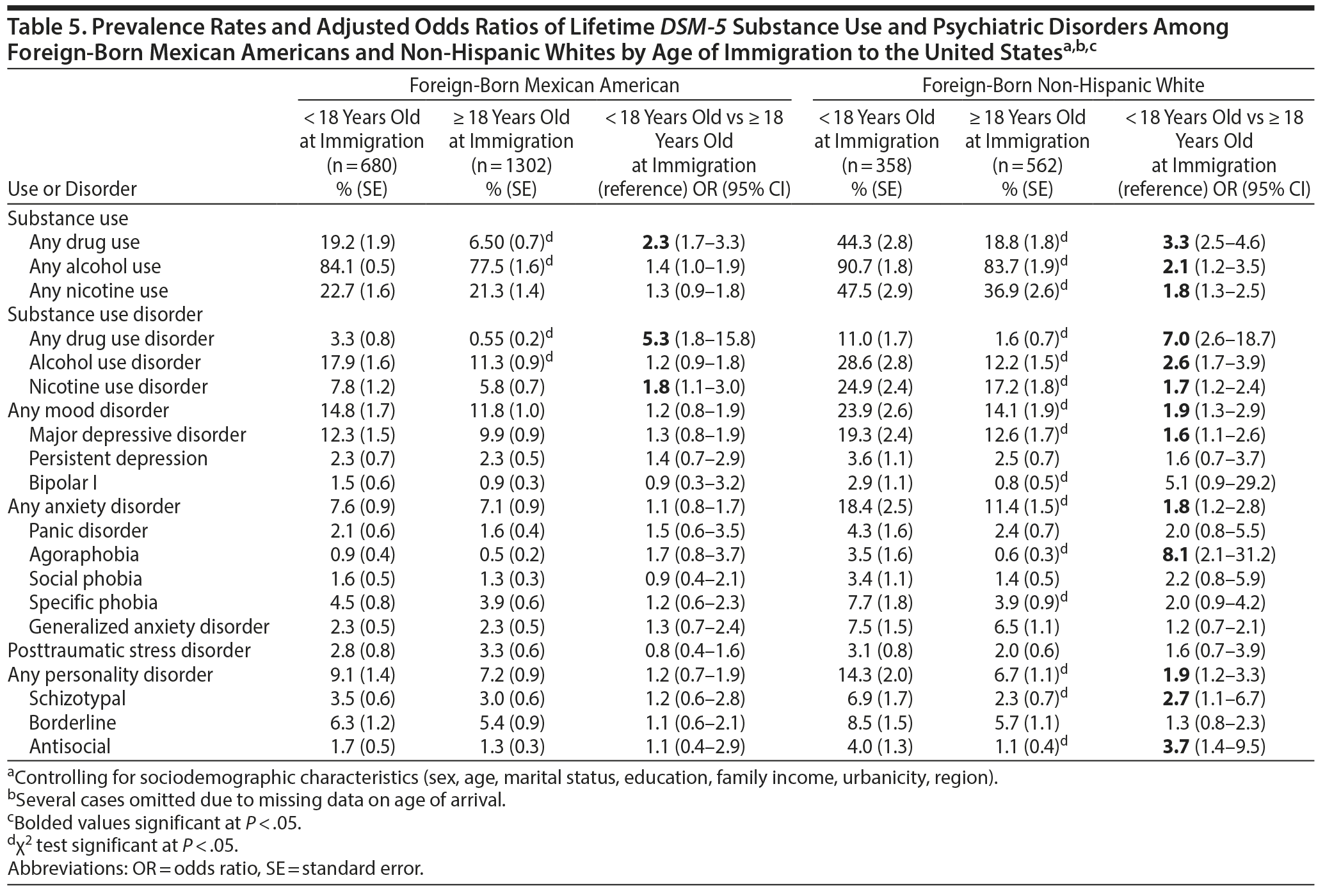
The odds of any drug use or DUD and NUD were greater among foreign-born Mexican Americans aged < 18 years at immigration compared to their counterparts aged ≥ 18 years at immigration of (Table 5). In contrast, the odds of alcohol, nicotine, and any drug use and their associated disorders, MDD, agoraphobia, and schizotypal and antisocial PDs were greater among foreign-born non-Hispanic whites < 18 years at immigration relative to those ≥ 18 years at immigration.
DISCUSSION
One major finding of this study is that foreign-born Mexican Americans and foreign-born non-Hispanic whites were at significantly lower risk of alcohol, nicotine, and other drug use and major psychiatric disorders than their US-born counterparts. Consistent with this finding was the lower risk of substance use and psychiatric disorders observed among foreign-born Mexican Americans compared with US-born non-Hispanic whites. These results are consistent with Grant et al5 but at variance with those studies3,4,6–8 that failed to differentiate between foreign-born and US-born non-Hispanic whites. It appears that results favoring foreign-born Mexican Americans in terms of substance use and mental health may generalize to foreign-born non-Hispanic whites.
Foreign-born Mexican Americans and foreign-born non-Hispanic whites had lower risk of substance use and psychiatric morbidity than their US-born counterparts despite greater stress associated with lower socioeconomic status and adjusting to a new culture.26 These results are consistent with the selection or healthy immigrant model.8,27 This model posits that individuals with good mental health are more likely to immigrate to the United States than those with poor mental health and thus are less likely to use substances and develop psychiatric disorders. However, the healthy immigrant hypothesis cannot account for the similarity in the rates of substance use and psychiatric disorders between US-born Mexican Americans and foreign-born non-Hispanic whites. This finding suggests that several processes influence the observed effect of immigration on substance use and psychiatric disorders seen in this study.28
US-born non-Hispanic whites were more likely to use substances and develop psychiatric disorders relative to US-born Mexican Americans. This finding suggests that rates of substance use and psychiatric disorders between US-born non-Hispanic whites relative to US-born Mexican Americans might be tied to their subjective assessment of social status having been born in the United States.28 That is, social and economic status expectations of US-born Mexican Americans may be more strongly associated with perceived status among their peers. Status expectations may vary depending on whether the network of peers among US-born Mexican Americans is US-born or foreign-born Mexican Americans, each with differing expectations regarding status. In close enclaves of Latino communities (eg, Miami), in which perceived status attainment is equated with the reference group rather than the actual US standard, US-born Mexican Americans might integrate into US society with greater success.
Findings of a lower odds of most substance use and psychiatric disorders among foreign-born non-Hispanic whites and foreign-born Mexican Americans compared with their US-born counterparts also support the role of cultural retention as a protective factor in substance use and mental health of individuals of Mexican descent.4,8 However, foreign-born non-Hispanic whites were more vulnerable to substance use and most psychiatric disorders relative to foreign-born Mexican Americans, suggesting the role of cultural retention may be stronger among foreign-born Mexican Americans than foreign-born non-Hispanic whites. Further research is needed to examine processes involved in the effects of acculturation on foreign-born immigrants.
Foreign-born Mexican Americans aged < 18 years at entry to the United States had greater odds of any drug use, any DUD, and NUD but did not differ in the odds of other psychiatric disorders compared with foreign-born Mexican Americans aged ≥ 18 years at immigration. These results are consistent with some14 but not all of the previous literature.13,15,29 Among foreign-born non-Hispanic whites, the odds of all substance use and associated disorders and MDD, agoraphobia, and antisocial and schizotypal PD were greater among those < 18 years at immigration relative to those ≥ 18 years at entry to the United States. It appears that immigration to the United States during earlier years may lead to greater internalization of US values and places foreign-born Mexican Americans at greater risk of drug use, DUD, and NUD and foreign-born non-Hispanic whites at greater risk of substance use and disorders and several other psychiatric disorders than those arriving after age 18 to the United States.28 Earlier internalization of US values among foreign-born Mexican Americans and especially foreign-born non-Hispanic whites may also result in greater family stress and intergenerational conflict, with greater adverse mental health effects among non-Hispanic whites. Conversely, those arriving in the United States at or after age 18 may experience less acculturative stress that may serve as a protective factor for substance use and psychiatric disorders. Further, the healthy immigrant hypothesis may also, in part, explain the generally lower odds of substance use and psychiatric disorders among those entering the United States after age 18. Future research is warranted on the impact of age at arrival into the United States and the processes underlying differential exposure to substances and risk of psychiatric disorders across subgroups of the population defined by origin or descent.
Limitations of this study include methodological artifacts related to language of the instruments that may account for patterns of association observed between immigration status and substance use and psychiatric disorders. However, in the NESARC-III, respondents were interviewed in their language of choice with Spanish-translated instruments that were validated in Spanish-speaking populations.30 Recall bias may have impacted the lifetime results reported here. However, 12-month associations between immigration status and age at entry to the United States and lifetime rates of substance use and psychiatric disorders were very similar to their lifetime counterparts, but, in many cases, low sample size precluded analysis. NESARC-III does not allow us to determine whether Mexican Americans or non-Hispanic whites (especially those who were foreign-born) were in the United States with or without formal authorization. Although it is possible that authorized and unauthorized individuals may have different rates of substance use and psychiatric disorders, many federal regulations prohibit the collection of such information in national surveys like the NESARC-III.
CONCLUSION
In summary, this study points to a protective effect of immigration status and later age at entry into the United States among Mexican Americans for substance use and psychiatric disorders, and these effects appear to generalize to foreign-born non-Hispanic whites. These findings underscore a variety of selection and contextual processes that may have produced the observed results. However, these processes may differently impact substance use and mental health among Hispanics from other countries and subgroups of non-Hispanic whites, highlighting the need for further research in this area. Understanding the protective effects of cultural retention on the foreign born and the deleterious effects of acculturative stress on substance use and psychiatric disorders on Mexican Americans and non-Hispanic whites arriving in the United States prior to the age of 18 holds great promise in the development of mental health prevention and intervention strategies. An understanding of how immigration status and age at immigration contribute to substance use and psychiatric disorders among Mexican Americans and non-Hispanic whites can be invaluable to clinicians in guiding screening, prevention, and treatment efforts that are culturally sensitive and informed.
Submitted: July 27, 2018; accepted November 5, 2018.
Published online: February 28, 2019.
Potential conflicts of interest: None.
Funding/support: This study was sponsored by the National Institute on Alcohol Abuse and Alcoholism (NIAAA) with supplemental funding from the National Institute on Drug Abuse. Westat was not a sponsor of the survey but did contract work for NIAAA in various aspects of the fielding of the survey.
Role of the sponsor: The funding sources had no role in the design and conduct of the study; collection, management, analysis, and interpretation of the data; preparation, review, or approval of the manuscript; and decision to submit the manuscript for publication.
Disclaimer: The views and opinions expressed in this report are those of the authors and should not be construed to represent the views of any of the sponsoring organizations or agencies or the US government.
Additional information: The original data set for the National Epidemiologic Survey on Alcohol and Related Conditions-III (NESARC-III) can be obtained from the National Institute on Alcohol Abuse and Alcoholism (http://www.niaaa.nih.gov).
REFERENCES
1. Bureau of the Census. Projections of the Size and Composition of the US Population: Population Estimates and Projections. Washington, DC: US Bureau of the Census; 2015.
2. Bureau of the Census. Hispanic Roots: Breakdown of US Hispanic Population, by Specific Origin: 2014. Washington, DC: US Bureau of the Census; 2016.
3. Alegría M, Canino G, Shrout PE, et al. Prevalence of mental illness in immigrant and non-immigrant US Latino groups. Am J Psychiatry. 2008;165(3):359–369. PubMed CrossRef
4. Burnam MA, Hough RL, Escobar JI, et al. Six-month prevalence of specific psychiatric disorders among Mexican Americans and non-Hispanic whites in Los Angeles. Arch Gen Psychiatry. 1987;44(8):687–694. PubMed CrossRef
5. Grant BF, Stinson FS, Hasin DS, et al. Immigration and lifetime prevalence of DSM-IV psychiatric disorders among Mexican Americans and non-Hispanic whites in the United States: results from the National Epidemiologic Survey on Alcohol and Related Conditions. Arch Gen Psychiatry. 2004;61(12):1226–1233. PubMed CrossRef
6. Karno M, Golding JM, Burnam MA, et al. Anxiety disorders among Mexican Americans and non-Hispanic whites in Los Angeles. J Nerv Ment Dis. 1989;177(4):202–209. PubMed CrossRef
7. Ortega AN, Rosenheck R, Alegría M, et al. Acculturation and the lifetime risk of psychiatric and substance use disorders among Hispanics. J Nerv Ment Dis. 2000;188(11):728–735. PubMed CrossRef
8. Vega WA, Kolody B, Aguilar-Gaxiola S, et al. Lifetime prevalence of DSM-III-R psychiatric disorders among urban and rural Mexican Americans in California. Arch Gen Psychiatry. 1998;55(9):771–778. PubMed CrossRef
9. Borges G, Breslau J, Orozco R, et al. A cross-national study on Mexico-US migration, substance use and substance use disorders. Drug Alcohol Depend. 2011;117(1):16–23. PubMed CrossRef
10. Borges G, Cherpitel CJ, Orozco R, et al. Substance use and cumulative exposure to American society: findings from both sides of the US-Mexico border region. Am J Public Health. 2016;106(1):119–127. PubMed CrossRef
11. Cherpitel CJ, Li L, Borges G, et al. Age at immigration and substance use and problems among males and females at the US-Mexico border. J Stud Alcohol Drugs. 2017;78(6):827–834. PubMed CrossRef
12. Mancini MA, Salas-Wright CP, Vaughn MG. Drug use and service utilization among Hispanics in the United States. Soc Psychiatry Psychiatr Epidemiol. 2015;50(11):1679–1689. PubMed CrossRef
13. Reingle JM, Caetano R, Mills BA, et al. The role of immigration age on alcohol and drug use among border and non-border Mexican Americans. Alcohol Clin Exp Res. 2014;38(7):2080–2086. PubMed CrossRef
14. Blanco C, Morcillo C, Alegría M, et al. Acculturation and drug use disorders among Hispanics in the US. J Psychiatr Res. 2013;47(2):226–232. PubMed CrossRef
15. Breslau J, Borges G, Hagar Y, et al. Immigration to the USA and risk for mood and anxiety disorders: variation by origin and age at immigration. Psychol Med. 2009;39(7):1117–1127. PubMed CrossRef
16. Grant BF, Chu A, Sigman R, et al. Source and Accuracy Statement: National Epidemiologic Survey on Alcohol and Related Conditions-III (NESARC-III). Bethesda, MD: National Institute on Alcohol Abuse and Alcoholism; 2014.
17. Centers for Disease Control and Prevention. 2014 National Health Interview Survey (NHIS) Public Use Data Release. Survey Description. Hyattsville, MD: Centers for Disease Control and Prevention; 2014.
18. Substance Abuse and Mental Health Services Administration. National Survey on Drugs and Health, 2013: Summary of Findings. Rockville, MD: Substance Abuse and Mental Health Services; 2014.
19. Bureau of the Census. American Community Survey, 2012. Suitland, MD: Bureau of the Census; 2013.
20. Grant BF, Harford TC, Dawson DA, et al. The Alcohol Use Disorder and Associated Disabilities Interview Schedule (AUDADIS): reliability of alcohol and drug modules in a general population sample. Drug Alcohol Depend. 1995;39(1):37–44. PubMed CrossRef
21. Grant BF, Dawson DA, Stinson FS, et al. The Alcohol Use Disorder and Associated Disabilities Interview Schedule-IV (AUDADIS-IV): reliability of alcohol consumption, tobacco use, family history of depression and psychiatric diagnostic modules in a general population sample. Drug Alcohol Depend. 2003;71(1):7–16. PubMed CrossRef
22. Grant BF, Goldstein RB, Smith SM, et al. The Alcohol Use Disorder and Associated Disabilities Interview Schedule-5 (AUDADIS-5): reliability of substance use and psychiatric disorder modules in a general population sample. Drug Alcohol Depend. 2015;148:27–33. PubMed CrossRef
23. Hasin DS, Shmulewitz D, Stohl M, et al. Procedural validity of the AUDADIS-5 depression, anxiety and post-traumatic stress disorder modules: substance abusers and others in the general population. Drug Alcohol Depend. 2015;152:246–256. PubMed CrossRef
24. Hasin DS, Greenstein E, Aivadyan C, et al. The Alcohol Use Disorder and Associated Disabilities Interview Schedule-5 (AUDADIS-5): procedural validity of substance use disorders modules through clinical re-appraisal in a general population sample. Drug Alcohol Depend. 2015;148:40–46. PubMed CrossRef
25. SUDAAN 11 [computer program]. Vol 1 and 2. Research Triangle Park, NC: Research Triangle Institute; 2012.
26. Gallo LC, Penedo FJ, Espinosa de los Monteros K, et al. Resiliency in the face of disadvantage: do Hispanic cultural characteristics protect health outcomes? J Pers. 2009;77(6):1707–1746. PubMed CrossRef
27. Kuo WH, Tsai Y-M. Social networking, hardiness and immigrant’s mental health. J Health Soc Behav. 1986;27(2):133–149. PubMed CrossRef
28. Abraído-Lanza AF, Echeverría SE, Flórez KR. Latino immigrants, acculturation, and health: promising new directions in research. Annu Rev Public Health. 2016;37(1):219–236. PubMed CrossRef
29. Vega WA, Sribney WM, Aguilar-Gaxiola S, et al. 12-month prevalence of DSM-III-R psychiatric disorders among Mexican Americans: nativity, social assimilation, and age determinants. J Nerv Ment Dis. 2004;192(8):532–541. PubMed CrossRef
30. Canino G, Bravo M, Ramírez R, et al. The Spanish Alcohol Use Disorder and Associated Disabilities Interview Schedule (AUDADIS): reliability and concordance with clinical diagnoses in a Hispanic population. J Stud Alcohol. 1999;60(6):790–799. PubMed CrossRef
Enjoy this premium PDF as part of your membership benefits!


