Objective: To investigate the relationship between gabapentin use and dose with substance use disorders (SUDs) prior to inpatient mental health treatment.
Methods: A cross-sectional study was performed in current gabapentin users admitted to inpatient psychiatry services from December 2015 through January 2017 in a large urban teaching hospital. The primary analysis examined rates and doses of gabapentin use in relation to SUD. A multinomial logistic regression was performed to assess a predictive model for SUD in gabapentin users. The secondary analysis examined trends of off-label gabapentin use.
Results: Of 1,483 admissions to inpatient psychiatry services, 345 subjects (23.1%) were prescribed gabapentin as an outpatient prior to admission. Current SUD was identified in 88.1% of the sample, with 65.2% identified as polysubstance positive. Mean daily doses of gabapentin were higher in subjects with positive SUD than in those with no history of SUD. Gabapentin doses ≥ 1,800 mg/d were associated with opiate misuse (P < .001), need for detoxification (P = .004), and positive hepatitis C status (P = .001). Multinomial linear regression revealed that use of gabapentin doses ≥ 1,800 mg/d was predictive of opiate misuse and positive hepatitis C status, with 68.7% positive predictive value.
Conclusion: High-dose gabapentin use can be predictive of opiate misuse disorder. Requests for high-dose gabapentin from patients may signal potential opioid misuse.
The Association of Gabapentin Use and Dose With Substance Use Disorders Prior to Inpatient Mental Health Treatment:
A Cross-Sectional Study
ABSTRACT
Objective: To investigate the relationship between gabapentin use and dose with substance use disorders (SUDs) prior to inpatient mental health treatment.
Methods: A cross-sectional study was performed in current gabapentin users admitted to inpatient psychiatry services from December 2015 through January 2017 in a large urban teaching hospital. The primary analysis examined rates and doses of gabapentin use in relation to SUD. A multinomial logistic regression was performed to assess a predictive model for SUD in gabapentin users. The secondary analysis examined trends of off-label gabapentin use.
Results: Of 1,483 admissions to inpatient psychiatry services, 345 subjects (23.1%) were prescribed gabapentin as an outpatient prior to admission. Current SUD was identified in 88.1% of the sample, with 65.2% identified as polysubstance positive. Mean daily doses of gabapentin were higher in subjects with positive SUD than in those with no history of SUD. Gabapentin doses ≥ 1,800 mg/d were associated with opiate misuse (P < .001), need for detoxification (P = .004), and positive hepatitis C status (P = .001). Multinomial linear regression revealed that use of gabapentin doses ≥ 1,800 mg/d was predictive of opiate misuse and positive hepatitis C status, with 68.7% positive predictive value.
Conclusion: High-dose gabapentin use can be predictive of opiate misuse disorder. Requests for high-dose gabapentin from patients may signal potential opioid misuse.
Prim Care Companion CNS Disord 2018;20(4):18m02291
To cite: Tomko JR, Prasad KM, Kubas S, et al. The association of gabapentin use and dose with substance use disorders prior to inpatient mental health treatment: a cross-sectional study. Prim Care Companion CNS Disord. 2018;20(4):18m02291.
To share: https://doi.org/10.4088/PCC.18m02291
© Copyright 2018 Physicians Postgraduate Press, Inc.
aClinical Pharmacy, UPMC Mercy, Pittsburgh, Pennsylvania
bPharmacy Practice, Duquesne University School of Pharmacy, Pittsburgh, Pennsylvania
cDepartment of Psychiatry, University of Pittsburgh School of Medicine, Pittsburgh, Pennsylvania
dDuquesne University School of Pharmacy, Pittsburgh, Pennsylvania
*Corresponding author: John R. Tomko, PharmD, Duquesne University School of Pharmacy, 212 Bayer, 600 Forbes Ave, Pittsburgh, PA 15282 ([email protected]).
Gabapentin is a medication that was originally approved by the US Food and Drug Administration (FDA) in 1993 as an adjunct treatment for partial seizure disorder, with a subsequent approval for postherpetic neuralgia in 2004.1 The mechanism of action of gabapentin is not definitively understood; however, it is believed to interact with α2δ-1 subunits of voltage-gated calcium channels.2 It is also theorized that gabapentin may activate γ-aminobutyric acid (GABA)ergic neurons in the spinal dorsal horn through the increased release of norepinephrine, with subsequent increases in spinal GABA release.3 Although structurally similar to GABA, gabapentin does not bind to GABA receptors, is not metabolized to GABA or a GABA agonist, and does not inhibit the reuptake of GABA or its degradation.1
Gabapentin has been used for many off-label uses with varying degrees of success.4,5 The evidence behind off-label use has been published in systematic reviews and small clinical trials.4–18 Use at doses up to 1,800 mg/d in conditions such as chronic neuropathic pain6 and in alcoholism maintenance treatment7 yields only moderate evidence of effectiveness. Gabapentin has also been studied in such conditions as fibromyalgia,8 migraine prophylaxis,9 complex regional pain syndrome,10 hot flashes in women treated for breast cancer,11,12 bipolar disorder,13 anxiety disorders,13,14 restless legs syndrome,15,16 and chronic back pain17 at doses up to 1,200 mg/d. The evidence behind its use in these conditions has been considered low to equivocal.4,5 Gabapentin exhibits saturable absorption via l-amino acid transporters; therefore, serum drug levels obtained at doses from 100 mg to 1,600 mg are not proportional.18 Thus, high doses of gabapentin may be unnecessary when treating various disorders, both approved and off-label.
In the early part of the 21st century, gabapentin was marketed off-label with little to no evidence supporting its use. Many studies used as evidence in the promotion of off-label gabapentin use were fraught with study design issues or various biases.19–21 In 2004, the manufacturer was found liable for these questionable marketing practices, resulting in numerous legal and monetary sanctions.22 As an ongoing consequence of this marketing strategy, the rate of off-label use of gabapentin continued to escalate. In a study23 of off-label prescribing by physicians conducted after the court case, 83% of prescribed gabapentin was found to be off-label, the highest proportion of any of the medications included in the study. A survey of physician knowledge conducted after the court case found that many physicians lacked knowledge about FDA-approved uses and the scarcity of evidence behind many of the off-label uses of gabapentin.24 Additionally, many clinical decisions involving the prescription of gabapentin for off-label use among psychiatrists, neurologists, and pain management specialists may have been founded on anecdotal or personal testimony of evidence.25
Gabapentin has recently been reported26,27 as an emerging drug of abuse. Due to the lack of controlled substance restrictions, as well as the aforementioned off-label promotion, gabapentin may be relatively easy to obtain for illicit use. Possible illicit uses could be for enhancement of other illicit substances or as a cutting agent for heroin.28 Gabapentin has been abused singularly as a euphoric agent, similar to the physiologic effects of marijuana and alcohol.29 In a 2014 study30 from Scotland, the number of gabapentin prescriptions was found to be escalating at a much higher rate than that of reports of neuropathic pain. Mean doses documented in this study30 were found to be higher than in most published literature (1,343 mg/d), and those prescribed gabapentin were 3 times more likely to admit to analgesic misuse. This report30 is consistent with reports31 that the drug is being used in conjunction with other drugs of abuse and even with opioid replacement therapies to enhance the opioid effect. A 2015 study32 estimated that while 30% of opioid-dependent patients undergoing detoxification were positive for other illicit substances, gabapentin was misused by 22% of the cohort. Gabapentin has also been reported to be concurrently abused along with opiates among clients in a dual-diagnosis correctional population.33
The primary objective of this study was to examine substance misuse and rates of abuse in patients admitted to a hospital psychiatric unit who were taking prescription gabapentin during the month prior to admission. We studied the relationship of gabapentin use and dose to various substances of abuse and polysubstance misuse. From this information, we hoped to develop a predictive model for gabapentin use and dose with various substance use disorders (SUDs) and comorbid conditions seen in SUD. Secondarily, we examined gabapentin dose trends in off-label diagnoses and the need for detoxification at hospital admission in gabapentin users.
METHODS
A cross-sectional study was performed from December 2015 through January 2017 for adult patients aged ≥ 18 years admitted to inpatient psychiatry services with any psychiatric diagnosis in a large urban teaching hospital. Inclusion criteria included prescription and outpatient self-administration of gabapentin continually during the month prior to admission to inpatient psychiatry. Subjects admitted to the separate medical-psychiatry detoxification unit were excluded from the study since SUD detoxification was the primary reason for hospital admission in these patients.
Sample Size Determination
A published finding32 of 30% incidence of polysubstance misuse in the opioid-dependent population was the basis for power calculation. In that work,32 22% of subjects were concurrently using gabapentin. We chose the higher 30% incidence rate for power calculations to provide a more stringent estimate of potential misuse. The study was powered at 80% with 2-tailed α = .05 to detect a 10% higher rate of SUD in our gabapentin-prescribed subjects compared to published results.32 The 10% difference would require greater subject recruitment. Thus, an a priori sample size of 172 subjects was required.
Data Collection
Data were collected from all subjects admitted to the adult psychiatric unit who were taking gabapentin during the month prior to admission. Gabapentin doses were collected from patient medication reconciliation and outpatient pharmacy records. Medical or psychiatric indications for gabapentin use were recorded and categorized into FDA-approved or off-label use. Admission urine drug analysis results were collected for drugs of abuse and alcohol using a 12-drug panel (Bio-Rad Laboratories, Hercules, California). Further collected data included the need for medical detoxification at admission and the number of and specific substances present in the urine drug screening (if any). Controlled substances prescribed in the month prior to admission were counted as a negative urine test result for illicit substance misuse. Positive screen results for buprenorphine or methadone were confirmed with the outpatient provider of these opiate replacement services and, if confirmed, counted as a negative result.
Statistical Analysis
Demographic data were analyzed descriptively. Mean daily doses of gabapentin were analyzed overall and by concurrent use of each observed substance of abuse, subject history of SUD, polysubstance misuse, reported gabapentin indication (approved or off-label), need for detoxification at hospital admission, detoxification protocol(s) used, and opiate replacement therapy.
Gabapentin dose ranges were coded as high dose: ≥ 1,800 mg/d and low dose: 0–1,799 mg/d. Chi-square testing was performed comparing gabapentin dose range use to demographics, comorbid conditions, and positive illicit drugs. As a secondary analysis and to validate the use of categorical high and low dose ranges, the dose range 0–1,799 mg/d was further recoded into 900–1,799 mg/d and 0–899 mg/d to examine any differences within these dose ranges.
To determine if a predictive model could be derived describing high-dose gabapentin use in the presence of SUD, significant factors identified from the previous analysis were entered into a multinomial logistic regression model, controlling for demographics. The study was approved by the hospital institutional review board to ensure protection of human subjects in accordance with the Declaration of Helsinki. All statistical analyses were performed using SPSS 24.0 (IBM Corporation, Armonk, New York).
RESULTS
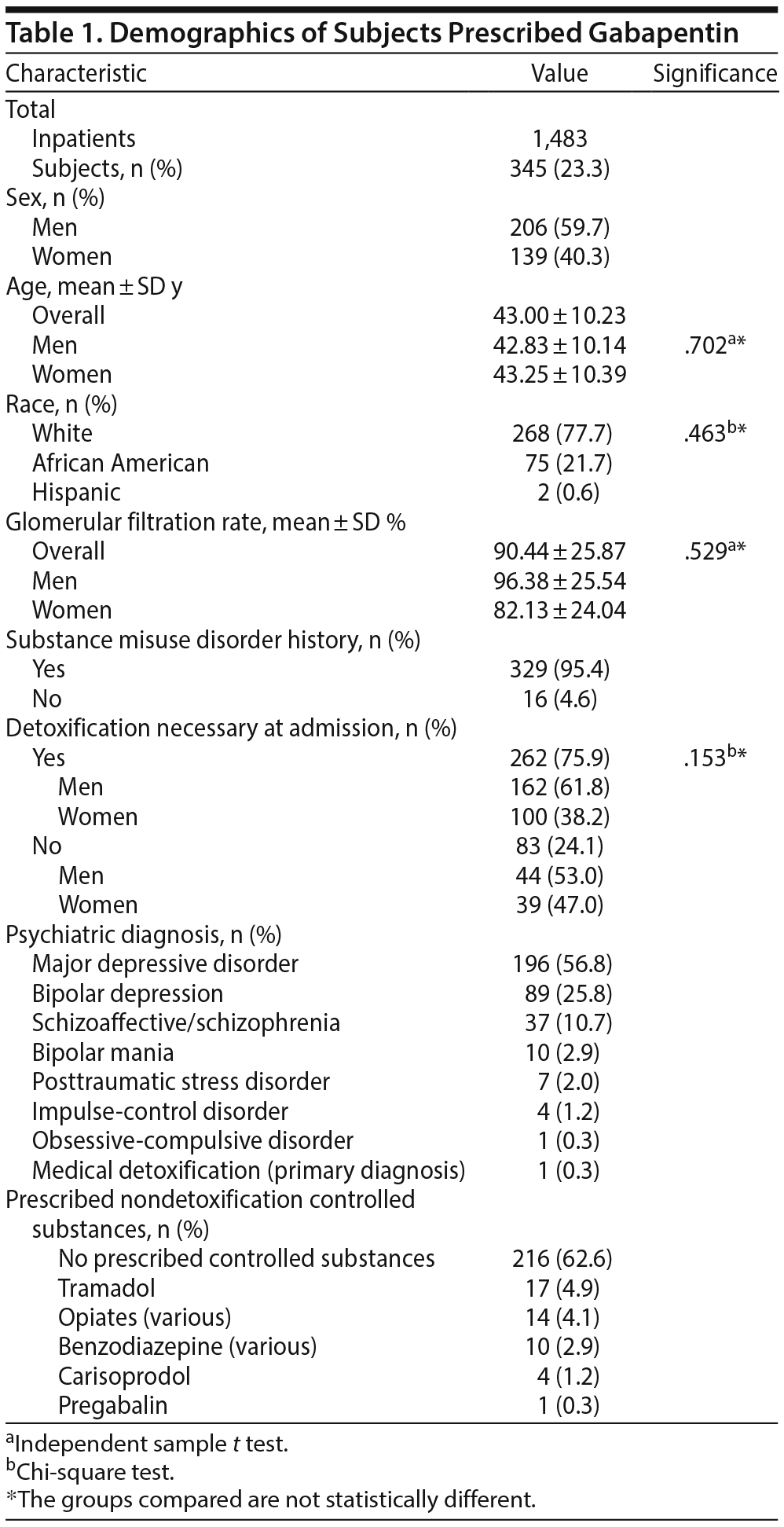
There were 1,483 admissions to the adult psychiatric unit during the 14-month study period. Of these, 345 subjects (23.3%) met inclusion criteria for gabapentin use at the time of hospital presentation, with 329 subjects positive for SUD history (95.4% of the gabapentin users). Positive illicit urine drug analyses were found in 304 subjects (88.1%), while polysubstance misuse was identified in 225 subjects (65.2%). Medical detoxification from drugs of abuse was warranted in 75.9% of gabapentin users. Subject demographics, diagnoses, and concurrent prescribed controlled substances are summarized in Table 1.
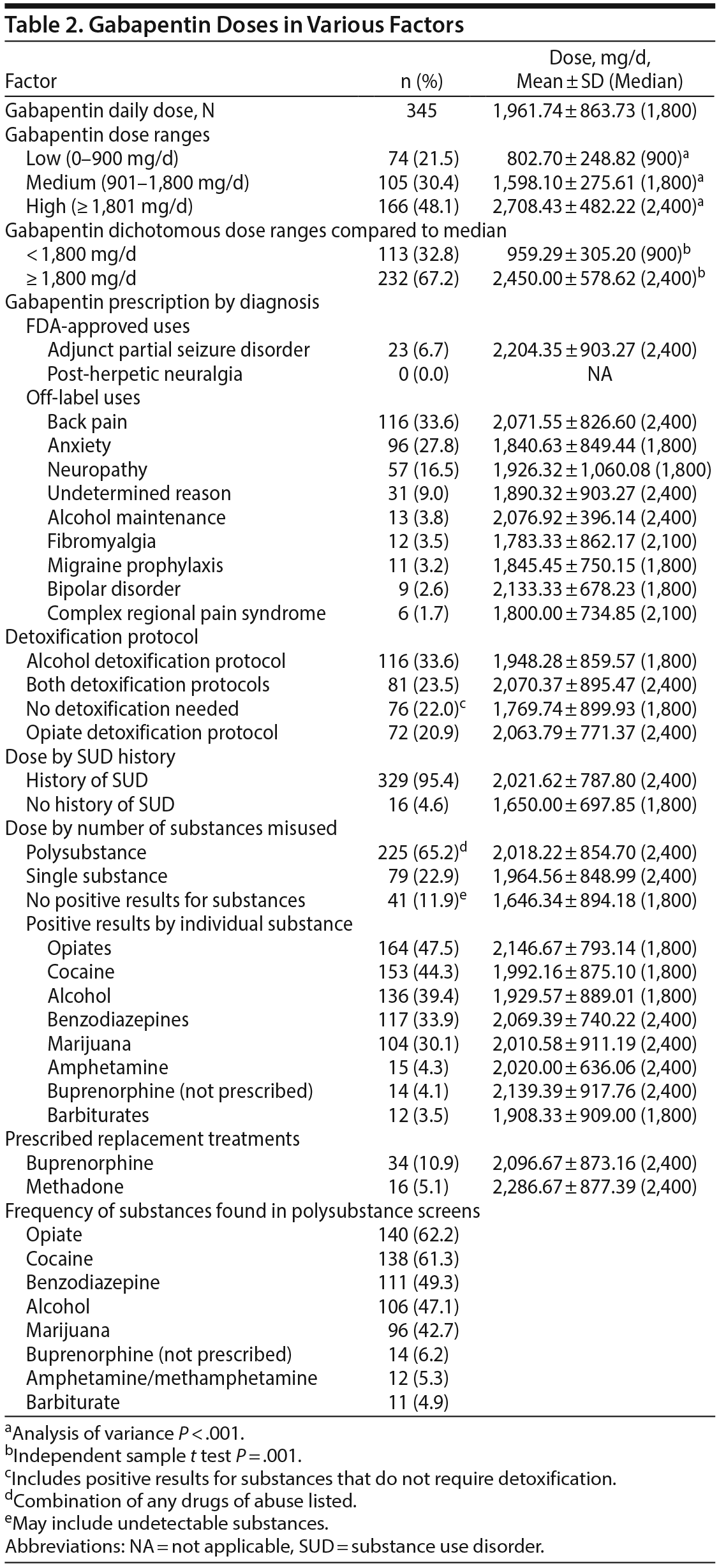
Gabapentin mean doses in various diagnoses and concurrent illicit substance use are presented in Table 2. The lowest mean daily gabapentin dose was found among subjects with no SUD history (16 subjects; 1,650.00 ± 697.85 mg/d). When considering all reasons for gabapentin use, the highest mean daily dose was among those who took gabapentin for the FDA-approved use of adjunct partial seizure disorder. For subjects with a SUD history, the highest mean daily dose was among patients receiving methadone maintenance treatment (20 subjects; 2,286.67 ± 877.39 mg/d). Mean doses of gabapentin were also higher in subjects taking illicit compared to prescribed buprenorphine. Illicit opiate misuse, either as a single agent or as part of polysubstance misuse, was identified in 47.5% of urine drug screens. This subgroup used a mean gabapentin dose of 2,146.67 ± 793.14 mg/d, the highest mean dose for any positive illicit substance group.
Factor Identification and Analysis
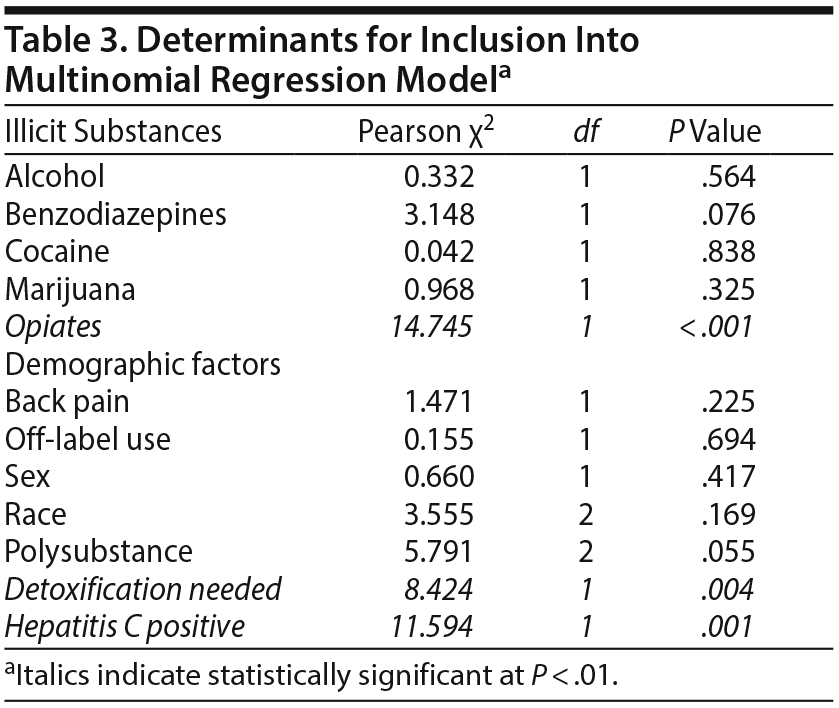
Chi-square analysis of each drug of abuse and demographic factors compared to gabapentin dose determined that subjects who were illicit opiate positive (P < .001), required detoxification at hospital admission (P = .004), or were hepatitis C positive (P = .001) were more likely to be taking gabapentin doses ≥ 1,800 mg/d. Doses in polysubstance misuse versus single-substance or no substance misuse trended toward significance (P = .055). No other drugs of abuse were significantly different between dose ranges. The secondary analysis of the same drugs and factors comparing low- (0–899 mg/d) and medium-dose (900–1,799 mg/d) gabapentin use showed no significant difference with any drug or factor. Results are presented in Table 3.
Multinomial Logistic Regression
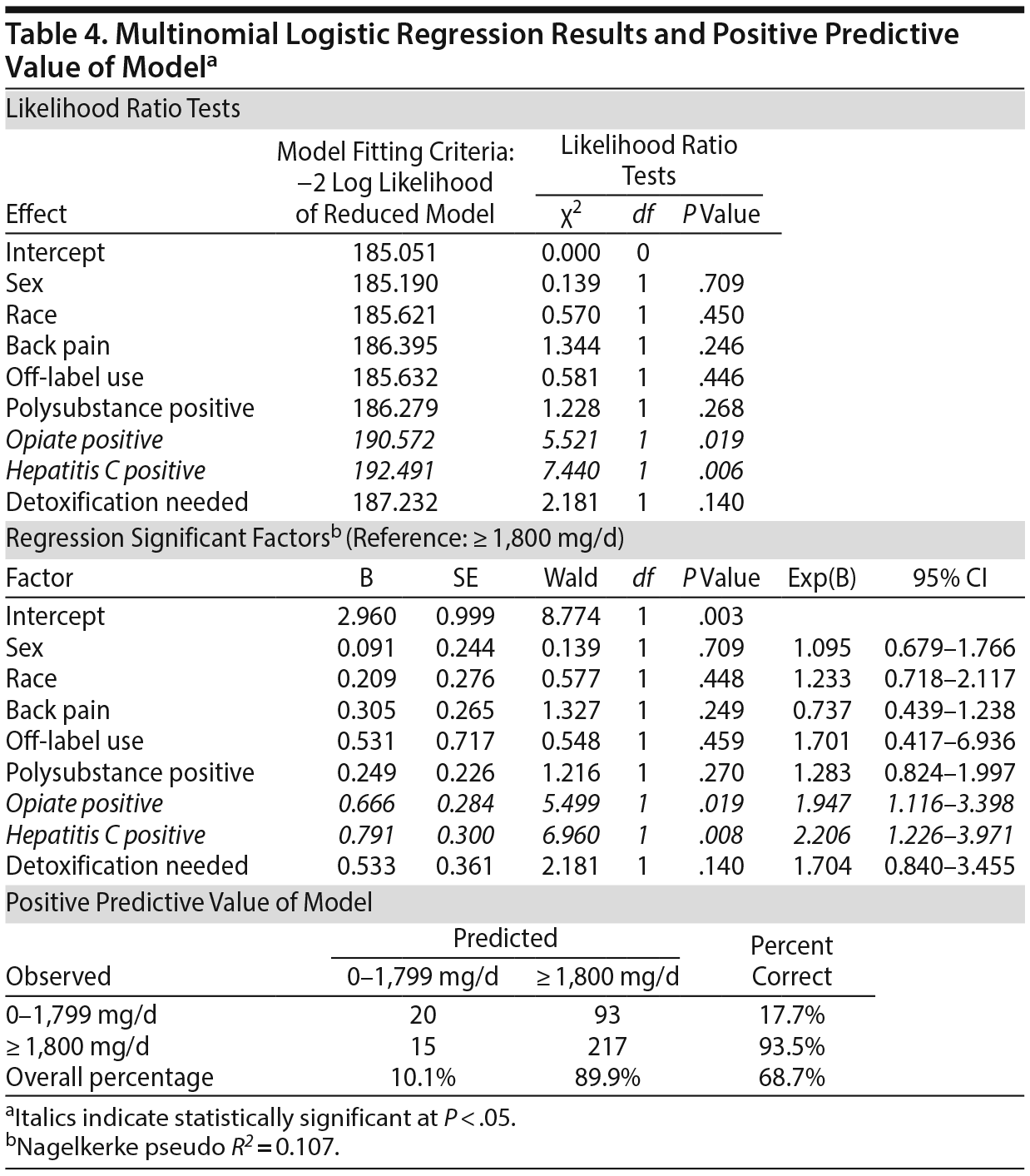
Statistically significant drugs and factors were entered into a multinomial logistic regression to determine the predictability of these factors in signaling high-dose gabapentin. Opiate misuse, positive hepatitis C status, and need for detoxification at admission were analyzed, controlling for demographics and off-label use. Results suggest that high-dose gabapentin users may be nearly twice as likely to be illicit opiate positive (odds ratio [OR]=1.947; 95% CI, 1.116–3.398; P = .019). Further, these subjects are also more than twice as likely to be hepatitis C positive (OR = 2.206; 95% CI, 1.226–3.971; P = .008). The model yielded a 68.7% positive predictive value. Results of the model are presented in Table 4.
Off-Label Use
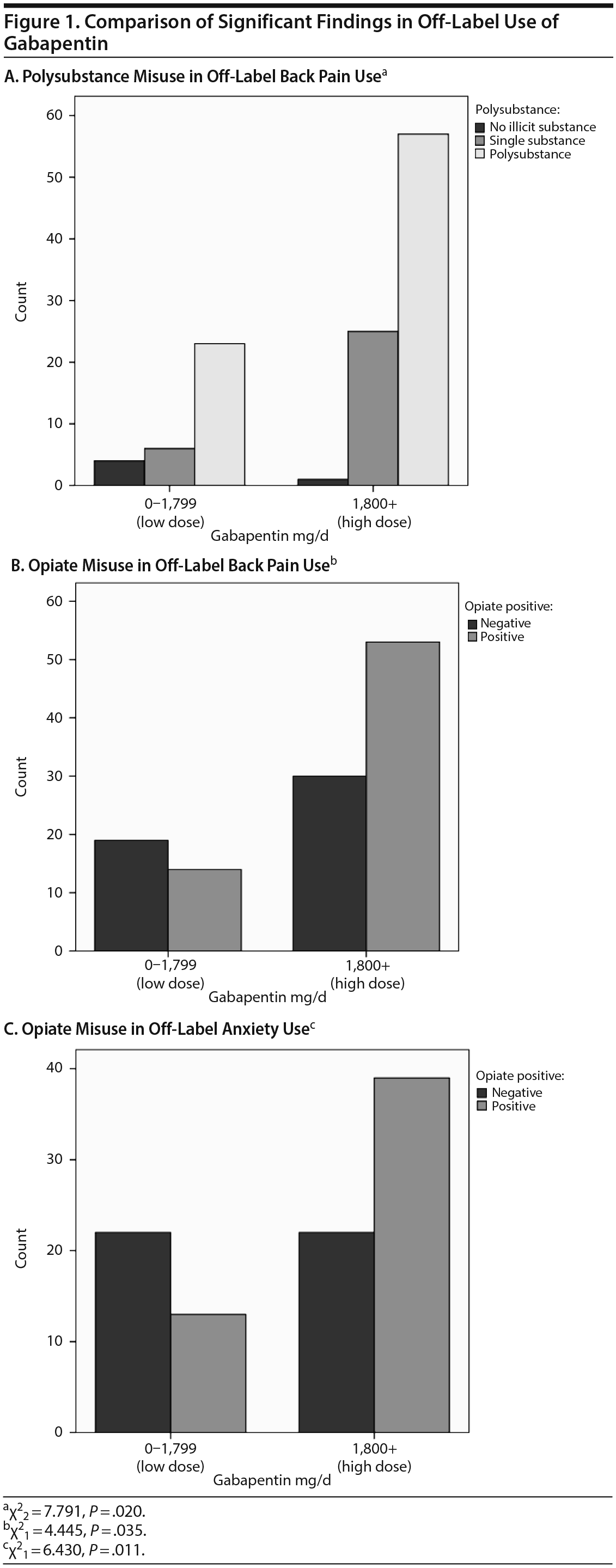
The 4 most common off-label uses (back pain, anxiety, neuropathy, and undetermined use) were analyzed as subsets comparing gabapentin doses to substances commonly used in a diagnosed category or polysubstance abuse status. High-dose gabapentin was significantly associated with illicit opiate misuse in subjects claiming back pain as the use for gabapentin (χ21 = 4.445, P = .035) (Figure 1). These subjects were also more likely to be polysubstance dependent (χ22 = 7.791, P = .020). In subjects claiming anxiety as the reason for off-label use, no difference was found in gabapentin dose range compared to illicit benzodiazepine use (χ21 = 0.083, P = .773) or polysubstance misuse (χ22 = 1.964, P = .375); however, subjects claiming anxiety were more likely to be positive for illicit opiates (χ21 = 6.430, P = .011). In subjects who claimed either neuropathy or an undetermined reason for gabapentin use, no differences in illicit substances or polysubstance misuse were found.
DISCUSSION
Mental health patients who are taking gabapentin at doses of 1,800 mg/d or higher exhibit greater probability of having a concurrent opiate misuse disorder than patients receiving less than 1,800 mg/d. Further, these patients are more likely to have a positive hepatitis C status. These findings raise a potentially clinically significant question as to whether gabapentin has addiction potential or whether use of gabapentin in conjunction with illicit substances such as opiates enhances the euphoric effects of the illicit substances.
Gabapentin use was identified in 23.1% of the total number of admissions to the mental health unit; however, 95.4% of the patients prescribed gabapentin had substance misuse history, either current or remote. Our population yielded 225 subjects who were current polysubstance misusers, comprising 65.2% of the total cohort of gabapentin recipients. These numbers were substantially higher than the published 30% polysubstance misuse estimates found by Wilens et al32 used for sample size determination. Additionally, mean daily doses used in patients with SUD history were higher than for those with no SUD history, although the difference was not statistically significant. SUD mean daily doses were also much higher than the doses studied in off-label studies, potentially signifying further illicit use of gabapentin.
Since our sample exhibited high rates of gabapentin use and potentially excessive doses in patients with SUD, especially those with illicit opiate use, model determination that could predict potential SUD in patients requesting escalating gabapentin doses was undertaken. To our knowledge, this work is the first attempt to determine a model predictive of high-dose gabapentin use in those with SUD, specifically opiate misusers. Opiate misuse may be either single-agent opiate misuse or a component of polysubstance misuse. Patients who take gabapentin doses ≥ 1,800 mg/d have nearly twice the likelihood of being illicit opiate positive and greater than double the likelihood of concurrently having hepatitis C while controlling for sex, race, off-label uses, need for detoxification at admission, and polysubstance misuse. The model yielded a 68.7% positive predictive value; therefore, it may be helpful for clinicians to consider these factors when patients request escalating doses of gabapentin. Illicit opiate use and positive hepatitis C status should be explored prior to agreeing to higher doses. Despite a statistically insignificant finding, polysubstance misuse trended toward significance and should not be ruled out in patients administering high-dose gabapentin.
Despite the paucity of evidence for off-label use, 93.3% of all recipients of gabapentin were taking the drug for an off-label use. In contrast to doses (900–1,800 mg/d) in off-label studies,6–14 the high-dose users were the largest group, with a median dose of 2,400 mg/d. Interestingly, 9% of subjects received mean gabapentin doses of approximately 1,890 mg/d with no determinable diagnosis for use of the medication. On the basis of prior evidence that opiate abusers have used gabapentin to enhance opiate effects, it can be theorized that these patients may employ secondary gain or diversionary behaviors such as “doctor shopping” to obtain gabapentin, which is a noncontrolled substance. Nebulous alleged off-label use symptoms such as back pain or anxiety may be reported to obtain the drug for possible illegitimate intentions.
A descriptive finding of this study revealed that in patients who are prescribed methadone maintenance treatment for opiate misuse history, mean doses of gabapentin were found to be even higher than those used concurrently with other illicit drugs. Buprenorphine maintenance treatment also produced mean doses similar to those taken by subjects misusing illicit substances. A possible reason for these higher doses may be that after receipt of opiate replacement treatment, patients may see a separate physician who is unaware of the patient’s participation in a replacement program. Use of a noncontrolled substance such as gabapentin for claimed off-label symptoms may be perceived as a safe alternative for treatment; however, the patient’s intentions may be to enhance effects of opiate replacement therapy.
There are limitations to the application of the results of this work. All subjects were recruited from a single inpatient mental health unit within a large urban hospital, which limits generalizability to all populations. Thus, application of results to non–mental health populations should be applied with caution. Future work should make these estimations in multiple sites to improve generalizability. There were also an extraordinarily large number of subjects diagnosed with major depressive disorder. A possible explanation may have been the result of substance misusers seeking admission to the hospital for secondary gain, such as claiming suicidal thoughts to obtain short-term housing. In such cases, some subjects would be considered appropriate for the separate medical detoxification unit and would have been excluded from the study. Another limitation may be that despite subject data collection at admission through medication reconciliation and from outpatient pharmacy databases, potential limitations to the accuracy of collected data could exist. A final, yet unlikely, limitation is that gabapentin may have been prescribed as an “opioid sparing” strategy by some prescribers. Since prescribed controlled substances were counted as a negative urine drug screen, only true illicit positive results were considered.
CONCLUSION
Gabapentin, as a noncontrolled substance, has the potential for misuse in patients with a substance misuse disorder, particularly in those using illicit opiates. Physicians should consider the potential of opiate misuse and concurrent hepatitis C in their patients who request high doses of gabapentin. Regulatory agencies may consider placing gabapentin in a controlled substance status, limiting the ease of accessibility to the drug. Classification of gabapentin as a controlled substance may help to curtail illegitimate and potentially dangerous use of the drug.
Submitted: March 5, 2018; accepted May 25, 2018.
Published online: August 2, 2018.
Author contributions: All authors contributed to the study concept and design, interpretation of data, drafting of the manuscript, and critical revision of the manuscript for important intellectual content. All authors had full access to the collected de-identified data from the study and take responsibility for the integrity of the data and accuracy of the analysis. Dr Tomko was responsible for data access, and Drs Tomko and Prasad completed the data acquisition and statistical analyses.
Potential conflicts of interest: None.
Funding/support: None.
Disclaimer: Analyses, interpretations, and conclusions are solely those of the authors.
Previous presentation: Preliminary results were presented in poster format at the annual meeting of the College of Psychiatric and Neurologic Pharmacists; April 24, 2017; Phoenix, Arizona.
REFERENCES
1. Neurontin [package insert]. New York, NY: Pfizer, Inc; 2015.
2. Kukkar A, Bali A, Singh N, et al. Implications and mechanism of action of gabapentin in neuropathic pain. Arch Pharm Res. 2013;36(3):237–251. Published online Feb 24, 2013. PubMed CrossRef
3. Gassner M, Ruscheweyh R, Sandkühler J. Direct excitation of spinal GABAergic interneurons by noradrenaline. Pain. 2009;145(1–2):204–210. PubMed CrossRef
4. Gabapentin (Neurontin) Off-label uses. Missouri DUReport. 2004 Nov/Dec;9(2). Missouri Department of Social Services website. https://dss.mo.gov/mhd/cs/pharmacy/pdf/dur9-2.pdf.
5. Mack A. Examination of the evidence for off-label use of gabapentin. J Manag Care Pharm. 2003;9(6):559–568. PubMed
6. Wiffen PJ, Derry S, Bell RF, et al. Gabapentin for chronic neuropathic pain in adults. Cochrane Database Syst Rev. 2017;6(6):CD007938. PubMed. CrossRef
7. Mason BJ, Quello S, Goodell V, et al. Gabapentin treatment for alcohol dependence: a randomized clinical trial. JAMA Intern Med. 2014;174(1):70–77. PubMed CrossRef
8. Cooper TE, Derry S, Wiffen PJ, et al. Gabapentin for fibromyalgia pain in adults. Cochrane Database Syst Rev. 2017;1(1):CD012188. PubMed. CrossRef
9. Linde M, Mulleners WM, Chronicle EP, et al. Gabapentin or pregabalin for the prophylaxis of episodic migraine in adults. Cochrane Database Syst Rev. 2013;(6):CD010609. PubMed. CrossRef
10. van de Vusse AC, Stomp-van den Berg SG, Kessels AH, et al. Randomized controlled trial of gabapentin in complex regional pain syndrome type 1 [ISRCTN84121379]. BMC Neurol. 2004;4(1):13. PubMed CrossRef
11. Rada G, Capurro D, Pantoja T, et al. Non-hormonal interventions for hot flushes in women with a history of breast cancer. Cochrane Database Syst Rev. 2010;(9):CD004923. PubMed. CrossRef
12. Pandya KJ, Morrow GR, Roscoe JA, et al. Gabapentin for hot flashes in 420 women with breast cancer: a randomized double-blind placebo-controlled trial. Lancet. 2005;366(9488):818–824. PubMed CrossRef
13. Berlin RK, Butler PM, Perloff MD. Gabapentin therapy in psychiatric disorders: a systematic review. Prim Care Companion CNS Disord. 2015;17(5):10.4088/PCC.15r01821. PubMed CrossRef
14. Pande AC, Pollack MH, Crockatt J, et al. Placebo-controlled study of gabapentin treatment of panic disorder. J Clin Psychopharmacol. 2000;20(4):467–471. PubMed CrossRef
15. Happe S, Sauter C, Klösch G, et al. Gabapentin versus ropinirole in the treatment of idiopathic restless legs syndrome. Neuropsychobiology. 2003;48(2):82–86. PubMed CrossRef
16. Micozkadioglu H, Ozdemir FN, Kut A, et al. Gabapentin versus levodopa for the treatment of restless legs syndrome in hemodialysis patients: an open-label study. Ren Fail. 2004;26(4):393–397. PubMed CrossRef
17. Shanthanna H, Gilron I, Rajarathinam M, et al. Benefits and safety of gabapentinoids in chronic low back pain: a systematic review and meta-analysis of randomized controlled trials. PLoS Med. 2017;14(8):e1002369. PubMed CrossRef
18. Stewart BH, Kugler AR, Thompson PR, et al. A saturable transport mechanism in the intestinal absorption of gabapentin is the underlying cause of the lack of proportionality between increasing dose and drug levels in plasma. Pharm Res. 1993;10(2):276–281. PubMed CrossRef
19. Vedula SS, Bero L, Scherer RW, et al. Outcome reporting in industry-sponsored trials of gabapentin for off-label use. N Engl J Med. 2009;361(20):1963–1971. PubMed CrossRef
20. Vedula SS, Li T, Dickersin K. Differences in reporting of analyses in internal company documents versus published trial reports: comparisons in industry-sponsored trials in off-label uses of gabapentin. PLoS Med. 2013;10(1):e1001378. Accessed Dec 14, 2015. PubMed CrossRef
21. Dickersin K. Reporting and other biases in studies of neurontin for migraine, psychiatric/bipolar disorders, nociceptive pain, and neuropathic pain. USCF website. http://dida.library.ucsf.edu/pdf/oxx18r10. Accessed January 8, 2017.
22. US Department of Justice. Warner-Lambert to pay $430 million to resolve criminal and civil health care liability relating to off-label promotion. Department of Justice website. http://www.justice.gov/opa/pr/2004/May/04_civ_322.htm. 2004.
23. Radley DC, Finkelstein SN, Stafford RS. Off-label prescribing among office-based physicians. Arch Intern Med. 2006;166(9):1021–1026. PubMed CrossRef
24. Chen DT, Wynia MK, Moloney RM, et al. US physician knowledge of the FDA-approved indications and evidence base for commonly prescribed drugs: results of a national survey. Pharmacoepidemiol Drug Saf. 2009;18(11):1094–1100. PubMed CrossRef
25. Fukada C, Kohler JC, Boon H, et al. Prescribing gabapentin off label: perspectives from psychiatry, pain and neurology specialists. Can Pharm J. 2012;145(6):280–284.e1. PubMed CrossRef
26. Schifano F. Misuse and abuse of pregabalin and gabapentin: cause for concern? CNS Drugs. 2014;28(6):491–496. PubMed CrossRef
27. Mersfelder TL, Nichols WH. Gabapentin: abuse, dependence, and withdrawal. Ann Pharmacother. 2016;50(3):229–233. PubMed CrossRef
28. Smith BH, Higgins C, Baldacchino A, et al. Substance misuse of gabapentin. Br J Gen Pract. 2012;62(601):406–407. PubMed CrossRef
29. Quintero GC. Review about gabapentin misuse, interactions, contraindications and side effects. J Exp Pharmacol. 2017;9:13–21. PubMed CrossRef
30. Baird CR, Fox P, Colvin LA. Gabapentinoid abuse in order to potentiate the effect of methadone: a survey among substance misusers. Eur Addict Res. 2014;20(3):115–118. PubMed CrossRef
31. Reeves RR, Ladner ME. Potentiation of the effect of buprenorphine/naloxone with gabapentin or quetiapine. Am J Psychiatry. 2014;171(6):691. PubMed CrossRef
32. Wilens T, Zulauf C, Ryland D, et al. Prescription medication misuse among opioid dependent patients seeking inpatient detoxification. Am J Addict. 2015;24(2):173–177. PubMed CrossRef
33. Bastiaens L, Galus J, Mazur C. Abuse of gabapentin is associated with opioid addiction. Psychiatr Q. 2016;87(4):763–767. PubMed CrossRef
Enjoy this premium PDF as part of your membership benefits!


