Objective: A limited number of studies have investigated QT wave dispersion (QTd) in depressive disorder. The objective of this study was to investigate whether QTd differed in patients diagnosed with depression compared to a control group and whether the difference correlated with the depression and anxiety scores.
Methods: Forty patients diagnosed with major depressive disorder (DSM-5 criteria) who did not receive their first treatment after the first episode were included in the study. Forty healthy individuals with similar sociodemographic characteristics were included in the control group. A sociodemographic and clinical data form, the Beck Depression Inventory, and the Beck Anxiety Inventory were given to all patients. Electrocardiograms were evaluated in a single-blind setting by the same cardiologist. The longest QT interval (QTmax) and the shortest QT interval (QTmin) were calculated. Heart rate-corrected QTmax (QTcmax) and QTmin (QTcmin) were calculated using the Bazett formula (QT[ms]/√R-R). The difference between QTcmax and QTcmin was accepted as the corrected QT dispersion (QTcd). The study was conducted from December 2018-March 2019.
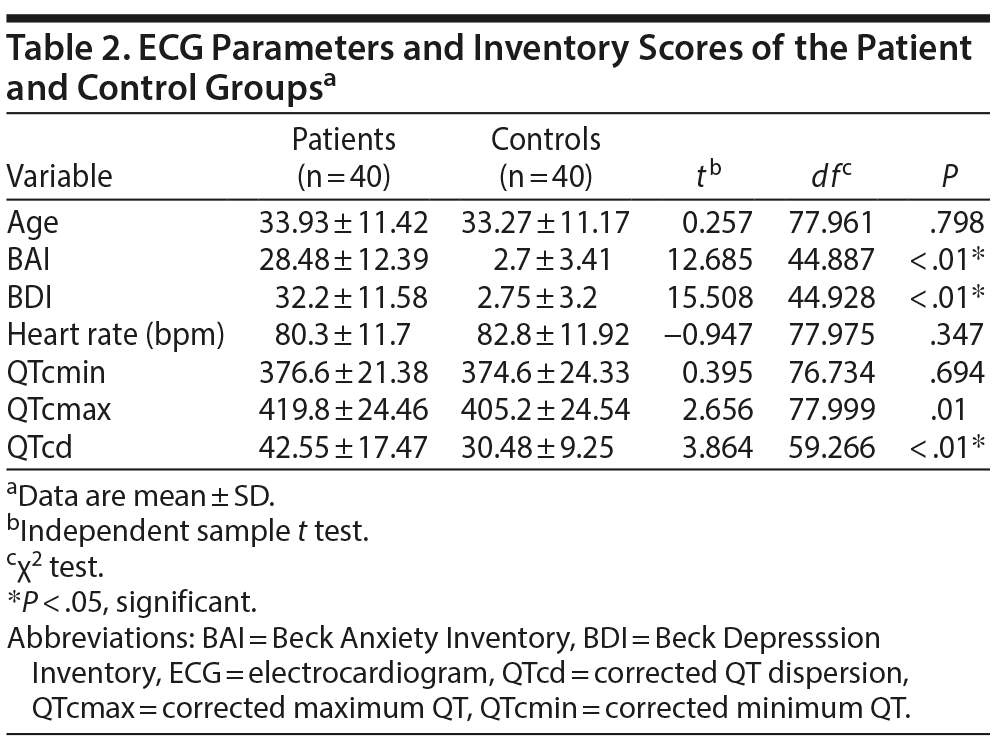
Results: No statistically significant difference was found between patient and control groups on the basis of age, sex, body mass index, or smoking. Beck Anxiety Inventory and Beck Depression Inventory scores of the patient group (28.48 ± 12.39 and 32.2 ± 11.58, respectively) were significantly higher compared to the control group (2.7 ± 3.41 and 2.75 ± 3.2, respectively). The patient group QTcmax (419.8 ± 24.46) and QTcd (42.55 ± 17.47) values were significantly higher compared to the QTcmax (405.2 ± 24.54) and QTcd (30.48 ± 9.25) values of the control group. There was a positive correlation between QTcd, QTcmax, and anxiety and depression scores.
Conclusions: QTcd values of depressed patients were higher than those of the healthy controls, and there was a positive correlation between QTcd and depression and anxiety scores.
QT Wave Dispersion in Patients With Major Depressive Disorder
ABSTRACT
Objective: A limited number of studies have investigated QT wave dispersion (QTd) in depressive disorder. The objective of this study was to investigate whether QTd differed in patients diagnosed with depression compared to a control group and whether the difference correlated with the depression and anxiety scores.
Methods: Forty patients diagnosed with major depressive disorder (DSM-5 criteria) who did not receive their first treatment after the first episode were included in the study. Forty healthy individuals with similar sociodemographic characteristics were included in the control group. A sociodemographic and clinical data form, the Beck Depression Inventory, and the Beck Anxiety Inventory were given to all patients. Electrocardiograms were evaluated in a single-blind setting by the same cardiologist. The longest QT interval (QTmax) and the shortest QT interval (QTmin) were calculated. Heart rate-corrected QTmax (QTcmax) and QTmin (QTcmin) were calculated using the Bazett formula (QT[ms]/√R-R). The difference between QTcmax and QTcmin was accepted as the corrected QT dispersion (QTcd). The study was conducted from December 2018-March 2019.
Results: No statistically significant difference was found between patient and control groups on the basis of age, sex, body mass index, or smoking. Beck Anxiety Inventory and Beck Depression Inventory scores of the patient group (28.48 ± 12.39 and 32.2 ± 11.58, respectively) were significantly higher compared to the control group (2.7 ± 3.41 and 2.75 ± 3.2, respectively). The patient group QTcmax (419.8 ± 24.46) and QTcd (42.55 ± 17.47) values were significantly higher compared to the QTcmax (405.2 ± 24.54) and QTcd (30.48 ± 9.25) values of the control group. There was a positive correlation between QTcd, QTcmax, and anxiety and depression scores.
Conclusions: QTcd values of depressed patients were higher than those of the healthy controls, and there was a positive correlation between QTcd and depression and anxiety scores.
Prim Care Companion CNS Disord 2020;22(1):19m02512
To cite: Korkmaz S, Aksoy DB, Çakar M, et al. QT wave dispersion in patients with major depressive disorder. Prim Care Companion CNS Disord. 2020;22(1):19m02512.
To share: https://doi.org/10.4088/PCC.19m02512
© Copyright 2020 Physicians Postgraduate Press, Inc.
aDepartment of Psychiatry, Firat University, Faculty of Medicine, Elazig, Turkey
bDepartment of Cardiovascular Surgery, Firat University, Faculty of Medicine, Elazig, Turkey
cDepartment of Cardiology, Malatya State Hospital, Malatya, Turkey
dDepartment of Cardiology, Firat University Faculty of Medicine, Elazig, Turkey
*Corresponding author: Sevda Korkmaz, MD, Department of Psychiatry, Firat University Faculty of Medicine, Elazig, Turkey ([email protected]).
There is a significant correlation between depressive disorder symptoms and the incidence of cardiac events.1 Cardiovascular diseases are observed more frequently in depressed individuals, which reduces their quality of life by worsening their clinical symptoms. Depression is considered to lead to cardiac events through psychophysiologic mechanisms such as platelet activity, hypothalamic-pituitary-adrenal axis function imbalances, abnormal autonomous nervous system functions, and changes in immune functions, inflammation, and biobehavioral mechanisms such as risky health behavior.2,3
Electrocardiogram (ECG) is one of the most commonly used methods to diagnose cardiovascular disease. QT wave dispersion (QTd) is obtained by measuring the difference between the maximum and minimum QT wave distance on the ECG. QTd could lead to severe ventricular arrhythmia and sudden cardiac death due to various mechanisms such as nonhomogeneous conduction velocities in different ventricular regions or repolarization.4 Thus, QTd is considered a useful parameter in predicting ventricular arrhythmias in individuals with elongated QT wave distance.5 It is important to identify QTd in at-risk patient groups to prevent future complications and control the follow-up and treatment of the primary disease. QTd has been investigated in several psychiatric disorders with significant anxiety symptoms.6,7 However, a limited number of studies8,9 have investigated QTd in depression. The present study aimed to investigate the difference in QTd between patients diagnosed with major depressive disorder and a control group to determine the correlations between QTd and depression and anxiety scores.
METHODS
This case-control study was conducted from December 2018 to March 2019 in accordance with the Declaration of Helsinki after approval by the local ethics committee. The study included 40 patients diagnosed in the psychiatry outpatient clinic with major depressive disorder based on DSM-5 diagnostic criteria who did not receive treatment after the first episode (within the first 6 months after ethics committee approval). The patients were required to have no previous vasoactive or psychotropic agent use, no diagnosis of heart disease or hypertension, and no alcohol or substance use. Forty healthy individuals with similar sociodemographic characteristics were included in the control group. All participants completed a sociodemographic and clinical data form developed by the authors based on the study objectives, the Beck Depression Inventory (BDI),10 and the Beck Anxiety Inventory (BAI).11 All ECGs were administered in the morning after the participant rested for 10 minutes in the supine position in a quiet room using a 12-lead ECG set at 50 mm/second. ECGs were analyzed by the same cardiologist in a single-blind setting. The QT interval was measured as the distance from the beginning of the Q wave to the end of the T wave (the point where it reached the T-P line). The maximum QT interval (QTmax) and the minimum QT interval (QTmin) were calculated. Heart rate-corrected QTmax (QTcmax) and QTmin (QTcmin) were calculated using the Bazett formula (QT[ms]/√R-R). The difference between QTcmax and QTcmin was accepted as heart rate-corrected QT dispersion (QTcd). Measurements were not conducted for the leads when the end of the T wave was not identified. For corrected QT dispersion (QTcd) measurement, the criteria included the presence of at least 7 leads, 3 of which had to be precordial leads. All ECG parameters were measured in milliseconds.
Analysis
Sociodemographic and clinical data form. A sociodemographic and clinical data form was developed in accordance with clinical experience and information obtained from the reviewed literature and based on the study objectives. The semistructured form included sociodemographic information such as age, sex, marital status, educational status, occupation, place of residence, income level, and family structure and clinical data such as duration of the disease and presence of psychosocial stress factors at the onset of the disease.

- Increased QT dispersion is considered a predisposing factor in the development of sudden cardiac death from ventricular arrhythmia.
- It is important to identify arrhythmias in high-risk patient groups and take necessary precautions without causing complications.
- Prediction of certain cardiac risks with an easily applicable, cost-effective, inexpensive, and practical method such as electrocardiogram may provide diagnostic and treatment convenience.
Beck Depression Inventory (BDI). The BDI was developed by Beck et al10 to determine an individual’s depression risk and to measure the level and severity of depressive symptoms. Each inventory item includes 21 questions scored between 0 and 3. The total score obtained by adding the points scored for each question can vary between 0 and 63.
Beck Anxiety Inventory (BAI). The BAI measures the frequency of anxiety symptoms experienced by an individual. This Likert-type self-assessment scale developed by Beck et al11 includes 21 items scored between 0 and 3. The higher the total score, the higher the anxiety experienced by the individual. The total score ranges from 0 to 63 points. A score between 0 and 7 indicates minimal, 8 and 15 indicates mild, 16 and 25 indicates moderate, and ≥ 26 indicates severe anxiety.
Statistics
SPSS for Windows 22.0 software (IBM Corp, Armonk, New York) was used in the statistical analysis of the study data. In the analysis, t test was used for paired comparisons and χ2 test for categorical comparisons. Correlation analyses were conducted to determine the correlations between the inventory scores and the ECG parameters, and linear regression analyses were conducted for the variables.
RESULTS
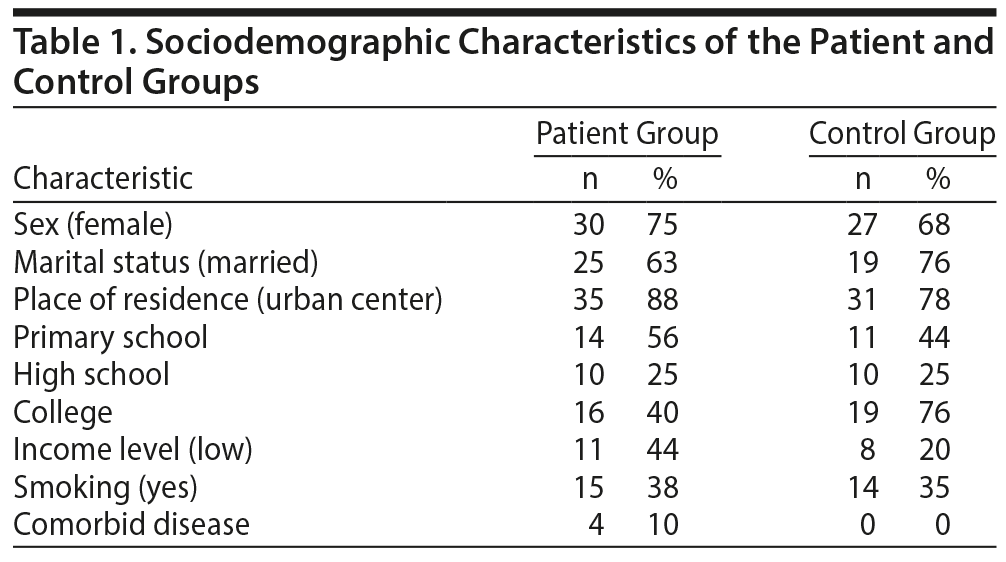
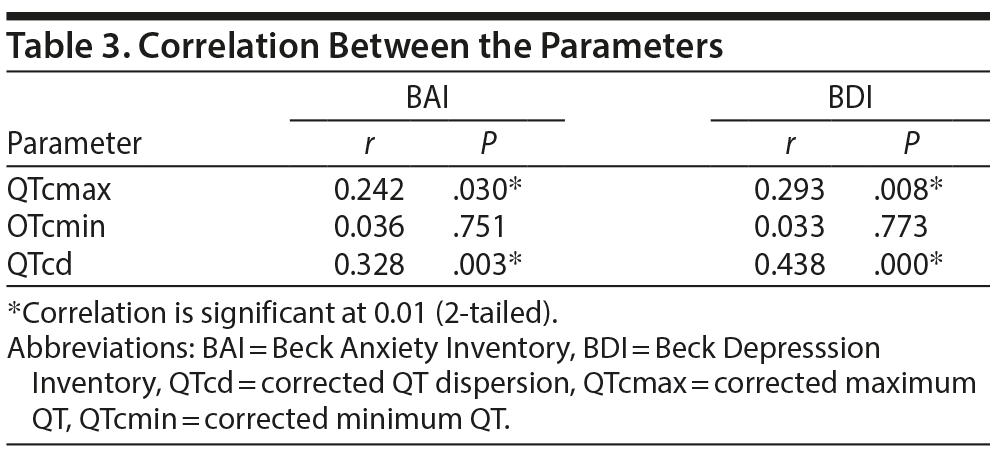
There was no statistically significant difference between the patient and control groups based on age, sex, body mass index, or smoking. Sociodemographic and clinical characteristics of the groups are presented in Table 1. The patient group mean ± SD BAI and BDI scores (28.48 ± 12.39 and 32.2 ± 11.58, respectively) were significantly higher compared to those of the control group (2.7 ± 3.41 and 2.75 ± 3.2, respectively) (Table 2). There was no significant difference between QTcmax, QTcmin, and QTcd values of smokers and nonsmokers. Patient group QTcmax (419.8 ± 24.46) and QTcd (42.55 ± 17.47) values were significantly higher than the control group QTcmax (405.2 ± 24.54) and QTcd (30.48 ± 9.25) values (Table 2). There was a positive correlation between QTcd, QTcmax, and anxiety and depression scores (Table 3). Linear regression analysis demonstrated that the effects of pre-ECG depression stress levels on QTcmax, QTcmin, QTcd, and heart rate of the cardiac patients did not have a significant effect when the regression correlation levels were examined as a whole. It was determined that the R value was 0.503, the R2 was 253.23, and the standard error predictive value was 0.444. On the basis of this information, analysis of the control group correlation values demonstrated that the correlation between QTcmax, QTcmin, QTcd, and heart rate and the regression model was weak.
DISCUSSION
In this study, it was determined that QTcd values of patients with major depressive disorder were higher compared to healthy controls, and there was a positive correlation between QTcd values and depression and anxiety scores. The findings demonstrate that patients with major depressive disorder constitute an arrhythmia risk group, especially for ventricular arrhythmias, which comprise a significant portion of cardiovascular diseases.
Previous studies2,12 reported that depression was closely associated with cardiovascular diseases, and the correlation was bidirectional. In patients with heart disease, depressive symptoms may be present due to different factors such as clinical symptoms, deterioration in quality of life, anxiety due to the disease, fear of death, and adverse effects of the prescribed medications.12,13 On the other hand, in patients with major depressive disorder, increased stress molecule levels, especially cortisol levels, could induce heart disease.14 Also, in this patient group, deterioration in platelet functions, malnutrition, a sedentary lifestyle, and medication use increase the risk of heart disease.3,15
In patients with psychiatric disorders, it is important to assess risk factors for cardiovascular disease and take necessary precautions with regard to diagnosis and treatment. There are invasive as well as inexpensive and easily accessible methods for the diagnosis of heart disease. ECG, which is widely used in the clinical setting for the diagnosis of heart disease and rhythm and conduction disorders and analysis of the adverse effects of certain drugs, is the most important among these methods. The repolarization period between leads is different in ECG. QT dispersion, which is used to measure this difference, is calculated by correction with the Bazett formula since it varies with the heart rate.6 This correction prevents the variations that occur due to the heart rate and allows a more healthy analysis. Recently, ECG was used not only in the context of cardiac diseases but also in several psychiatric disorders that induce their risk, especially in studies that aimed to determine ventricular arrhythmias.16,17 A study conducted in 2013 by Tosu et al18 found that QT dispersion was higher in patients with depression compared to healthy controls. On the basis of these findings, they emphasized that QT dispersion may be an indicator of autonomous imbalance in depressed individuals and is important in cardiac mortality.18 Later, in a study19 conducted with female patients, QT dispersion was high and a positive correlation between QT dispersion rates and the severity of depression was reported. In the literature, QT dispersion was found to be significantly higher in depressed patients compared to healthy controls.18
The present study has limitations. The low patient count and absence of predisease ECG records in the patient group could be considered among these limitations. Also, since the majority of the study participants were female and the sample size was small, it was not possible to conduct a significant comparison between the sexes. Furthermore, the presence of smokers in both patient and healthy control groups may be considered a limitation in data analysis due to the negative effects of smoking on cardiac parameters. However, since the smoking rate was almost the same in both groups, it could be suggested that the present study findings were minimally affected by the presence of smokers.
CONCLUSION
Ventricular arrhythmias are induced by early stimuli at the focus of any ventricular region. When left untreated, they are known as arrhythmias with high morbidity and sudden cardiac death risk, especially in individuals with structural heart disease. Increased QT dispersion is considered a predisposing factor in the development of sudden cardiac death from ventricular arrhythmia.20 It is important to identify these arrhythmias in at-risk patient groups and take necessary precautions without causing complications. Prediction of certain risks with an easily applicable, cost-effective, inexpensive, and practical method such as ECG may provide diagnostic and treatment convenience.
Submitted: July 11, 2019; accepted September 12, 2019.
Published online: January 2, 2020.
Potential conflicts of interest: None.
Funding/support: None.
REFERENCES
1.Umer H, Negash A, Birkie M, et al. Determinates of depressive disorder among adult patients with cardiovascular disease at outpatient cardiac clinic Jimma University Teaching Hospital, South West Ethiopia: cross-sectional study. Int J Ment Health Syst. 2019;13(1):13. PubMed CrossRef
2.Goldston K, Baillie AJ. Depression and coronary heart disease: a review of the epidemiological evidence, explanatory mechanisms and management approaches. Clin Psychol Rev. 2008;28(2):288-306. PubMed CrossRef
3.Kozela M, Bobak M, Besala A, et al. The association of depressive symptoms with cardiovascular and all-cause mortality in Central and Eastern Europe: prospective results of the HAPIEE study. Eur J Prev Cardiol. 2016;23(17):1839-1847. PubMed CrossRef
4.Attia J, Margetts P, Guyatt G. Diagnosis of thyroid disease in hospitalized patients: a systematic review. Arch Intern Med. 1999;159(7):658-665. PubMed CrossRef
5.Malik M, Batchvarov VN. Measurement, interpretation and clinical potential of QT dispersion. J Am Coll Cardiol. 2000;36(6):1749-1766. PubMed CrossRef
6.Somberg JC, Molnar J. Usefulness of QT dispersion as an electrocardiographically derived index. Am J Cardiol. 2002;89(3):291-294. PubMed CrossRef
7.Uyarel H, Okmen E, CobanoÄŸlu N, et al. Effects of anxiety on QT dispersion in healthy young men. Acta Cardiol. 2006;61(1):83-87. PubMed CrossRef
8.Oksuz F, Yarlioglues M, Ozturk S, et al. Atrial electromechanical delay analysed by tissue Doppler echocardiography is prolonged in patients with generalised anxiety disorders. Kardiol Pol. 2017;75(6):581-588. PubMed CrossRef
9.Nahshoni E, Aizenberg D, Strasberg B, et al. QT dispersion in the surface electrocardiogram in elderly patients with major depression. J Affect Disord. 2000;60(3):197-200. PubMed CrossRef
10.Beck AT, Ward CH, Mendelson M, et al. An inventory for measuring depression. Arch Gen Psychiatry. 1961;4(6):561-571. PubMed CrossRef
11.Beck AT, Epstein N, Brown G, et al. An inventory for measuring clinical anxiety: psychometric properties. J Consult Clin Psychol. 1988;56(6):893-897. PubMed CrossRef
12.Kyrou I, Kollia N, Panagiotakos D, et al; ATTICA Study investigators. Association of depression and anxiety status with 10-year cardiovascular disease incidence among apparently healthy Greek adults: the ATTICA Study. Eur J Prev Cardiol. 2017;24(2):145-152. PubMed CrossRef
13.Carney RM, Blumenthal JA, Catellier D, et al. Depression as a risk factor for mortality after acute myocardial infarction. Am J Cardiol. 2003;92(11):1277-1281. PubMed CrossRef
14.Holsen LM, Lee JH, Spaeth SB, et al. Brain hypoactivation, autonomic nervous system dysregulation, and gonadal hormones in depression: a preliminary study. Neurosci Lett. 2012;514(1):57-61. PubMed CrossRef
15.Seligman F, Nemeroff CB. The interface of depression and cardiovascular disease: therapeutic implications. Ann N Y Acad Sci. 2015;1345(1):25-35. PubMed CrossRef
16.Izci F, Hocagil H, Izci S, et al. P-wave and QT dispersion in patients with conversion disorder. Ther Clin Risk Manag. 2015;11:475-480. PubMed CrossRef
17.Kelmanson IA. High anxiety in clinically healthy patients and increased QT dispersion: a meta-analysis. Eur J Prev Cardiol. 2014;21(12):1568-1574. PubMed CrossRef
18.Tosu AR, Demir S, Kaya Y, et al. Increased QT dispersion and P wave dispersion in major depressive disorder. Exp Clin Cardiol. 2013;18(2):110-112. PubMed
19.Tolentino JC, Schmidt SL. Association between depression severity and cardiac autonomic modulation. J Psychosom Res. 2016;85:9-11. PubMed CrossRef
20.Padmanabhan S, Silvet H, Amin J, et al. Prognostic value of QT interval and QT dispersion in patients with left ventricular systolic dysfunction: results from a cohort of 2,265 patients with an ejection fraction of < or =40%. Am Heart J. 2003;145(1):132-138. PubMed CrossRef
Enjoy this premium PDF as part of your membership benefits!