Service members from Iraq and Afghanistan are returning home and reintegrating into civilian life, but many were exposed to terrifying events that can cause posttraumatic stress disorder (PTSD) and other mental health problems. Military culture, which upholds strength and resilience, can create a barrier to veterans in seeking help for PTSD. Many veterans do not receive health care available through the Department of Veterans Affairs (VA) and, instead, get health care in the private sector. Non-VA care providers need to be aware that they should ask patients about any military service, be prepared to assess veteran patients for PTSD and other mental health conditions, and provide support and education to them and their families. This Commentary features a discussion among experts in medicine and government who want to address the challenges that returning veterans face in receiving comprehensive mental and medical health care, improve the transition from active duty to veteran life, and involve family members, peers, employers, and communities in supporting veterans.
From the Behavioral Science Division, National Center for PTSD, US Department of Veterans Affairs, Washington, DC, and the Department of Psychiatry, Boston University School of Medicine, Bos-ton, Massachusetts (Dr Keane); IBM Research, San Jose, California (Dr Chaudhry); Department of Psychiatry, Weill Cornell Medical College, and New York-Presbyterian Hospital, New York (Dr Do-cherty); US Department of Veterans Affairs, Washington, DC (Drs Jesse and Lee); Serving Together, Mental Health Association of Montgomery County, Rockville, Maryland (Ms McNurlen); and Suicide Prevention Branch, Center for Mental Health Services, Substance Abuse and Mental Health Services Administration (SAMHSA), Rockville, Maryland (Ms Zeller).
Find more articles on this and other psychiatry and CNS topics:
The Journal of Clinical Psychiatry
The Primary Care Companion for CNS Disorders

On April 4, 2012, the Aspen Institute, in partnership with the CME Institute of Physicians Postgraduate Press, Inc., convened experts to identify the needs of returning combat veterans with posttraumatic stress disorder and other mental illnesses and to suggest community-based solutions to respond to those needs. The experts replicated that discussion on August 27, 2012, in the planning roundtable “Caring for Returning Veterans: Meeting Mental Health Needs.” This Commentary section of The Journal of Clinical Psychiatry presents the highlights of that planning roundtable and was prepared and independently developed by the CME Institute of Physicians Postgraduate Press, Inc.
The teleconference was chaired by Terence M. Keane, PhD, Director, Behavioral Science Division, National Center for PTSD, US Department of Veterans Affairs, Washington, DC, and Professor of Psychiatry and Assistant Dean for Research at Boston University School of Medicine, Boston, Massachusetts. The faculty were Basit Chaudhry, MD, PhD, Medical Scientist, IBM Research, Washington, DC; John P. Docherty, MD, Adjunct Professor, Department of Psychiatry, Weill Cornell Medical College, and Attending Psychiatrist, New York-Presbyterian Hospital, New York; Robert L. Jesse, MD, PhD, Principal Deputy Under Secretary for Health, US Department of Veterans Affairs, Washington, DC; Jennifer Lee, MD, Special Assistant for Community Engagement Under the Principal Deputy Under Secretary for Health, US Department of Veterans Affairs, Washington, DC; Jessica McNurlen, MA, CRC, Project Director, Serving Together, Mental Health Association of Montgomery County, Rockville, Maryland; and Eileen Zeller, MPH, Public Health Advisor, Suicide Prevention Branch, Center for Mental Health Services, Substance Abuse and Mental Health Services Administration (SAMHSA), Rockville, Maryland.
Financial disclosure: Dr Chaudhry is an employee of IBM and his spouse is a member of the speaker/advisory board for APCO International. Dr Docherty is a consultant for Comprehensive Clinical Development and Care Management Technologies and is a member of the speaker/advisory boards for AstraZeneca, Bristol-Myers Squibb, Merck, Janssen, Otsuka, and Sunovion. Drs Keane, Jesse, and Lee and Mss McNurlen and Zeller have no personal affiliations or financial relationships with any commercial interest to disclose relative to the activity.
The opinions expressed herein are those of the faculty and do not necessarily reflect the opinions of the CME provider and publisher.
J Clin Psychiatry 2013;74(1):22-28 (doi:10.4088/JCP.12071co1c)
© Copyright 2013 Physicians Postgraduate Press, Inc.
The Aspen Institute is pleased to partner with The Journal of Clinical Psychiatry to foster discussion among clinicians on meeting the challenges to society related to the mental health of veterans returning from Iraq and Afghanistan. In April 2012, the Aspen Institute and Physicians Postgraduate Press, Inc., publisher of The Journal, brought together a group of experts from the Veterans Administration, Department of Defense, Department of Health and Human Services, several think tanks, and community organizations devoted to helping combat veterans returning from Iraq and Afghanistan reintegrate into civilian life. The experts identified needs of veterans, gaps in services, and potential solutions. They agreed that the civilian population is generally unaware of the needs of returning combat veterans and veterans with mental health issues are often reluctant to seek treatment because of perceived stigma. At the end of the day-long meeting, the experts called for a national public relations effort to raise awareness among front-line health providers about the psychological needs of returning combat veterans.
The accompanying Commentary is the first step in the public relations effort of the newly formed Aspen Veterans Initiative. It suggests that health professionals routinely query patients about military service, become familiar with veteran resources and eligibility requirements locally and nationally, and equip veterans and their families with education, counseling, and coping mechanisms to deal with mental health issues, including the symptoms of PTSD.
The partnership arises from the Aspen Veterans Initiative of the Aspen Institute intended to spur discussions about challenges and solutions related to the well-being of returning combat veterans. The Aspen Institute is an educational and policy studies organization based in Washington, DC. Its mission is to foster leadership based on enduring values and to provide a nonpartisan venue for dealing with critical issues. The Institute is based in Washington, DC; Aspen, Colorado; and on the Wye River on Maryland’s Eastern Shore. It also has offices in New York City and an international network of partners. For more information, visit www.aspeninstitute.org.
By working together, the Aspen Institute and Physicians Postgraduate Press, Inc., hope to provide resources for health care professionals to improve the mental health of returning Iraq and Afghanistan veterans.
Since 2001, 2.3 million Americans have served in a war zone,1 and many of those service members have returned or are returning from deployment. Among military personnel who have served in Operation Iraqi Freedom (OIF), Operation Enduring Freedom (OEF), and New Dawn, over 6,500 service members have died, close to 50,000 have been physically wounded, and an estimated 400,000 have mental illnesses, such as posttraumatic stress disorder (PTSD).2
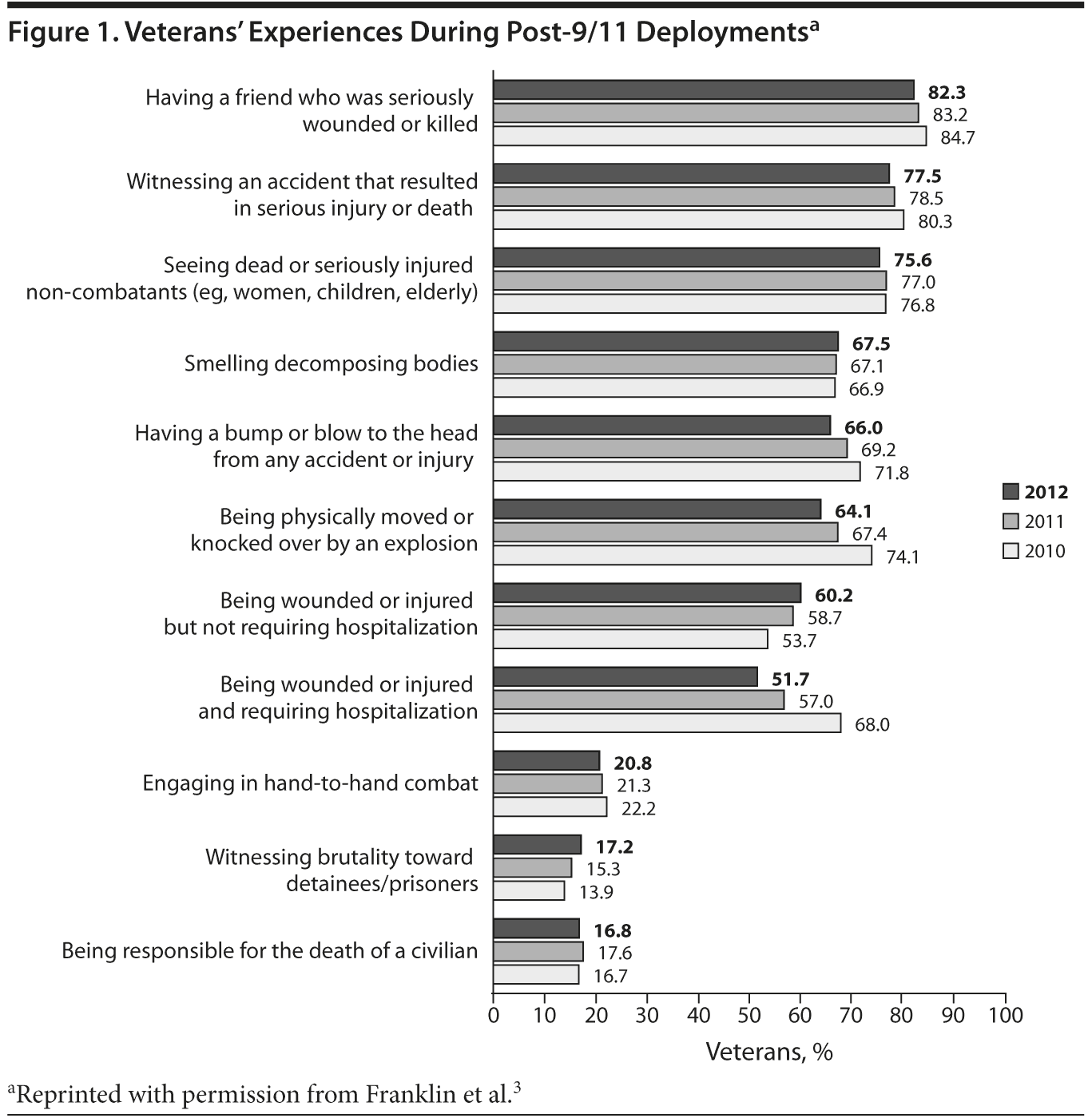
PTSD can occur after people experience trauma from combat, assault, or disaster. For service members, traumatic experiences can include having a friend die, smelling dead bodies, and physically feeling the impact of an explosion (Figure 1).3 If PTSD develops, the service member will experience intrusive recollections, avoidant/numbing symptoms, and/or hyperarousal symptoms.4
Many military personnel who served in Iraq and Afghanistan are not receiving health care from the Veterans Health Administration, a division of the Department of Veterans Affairs (VA). About 40% of eligible people are signing up for health care from the VA, but the other 60% are getting their health care in places where their veteran status may go undetected.5 Clinicians in the private sector need to be knowledgeable about PTSD and other mental health conditions so that they can successfully assess, triage, and support veteran patients (Table 1).6
Terence M. Keane, PhD, chaired a discussion among experts about the challenges that returning veterans face in receiving treatment for mental health conditions, the services needed to help veterans’ family members, the information sharing that should occur between the VA and Department of Defense (DoD), and the ways that employers and communities can help returning veterans.
What Challenges Do Veterans Face in Receiving Appropriate Treatment for PTSD and Other Mental Disorders?
Dr Keane: When you consider that over 2 million people have served in the most recent military operations,1 and they have spouses, children, and parents, you realize that a significant part of the American population is affected by what has happened in these war zones. Many of those deployed are suffering from the invisible wounds of war: PTSD, traumatic brain injury (TBI), and/or chronic pain. As of 2010, veterans comprised about 7% of the US population.1 Many people believe that veterans get their health care at VA facilities, but often that is untrue. When service members return to civilian life, what barriers do they face in getting mental health care?
Ms McNurlen: One challenge we have experienced in Montgomery County, Maryland, is the need for increased awareness among private practitioners and nonmilitary serving organizations on military culture and how they can provide a safety net of services to our local military, veterans, and their families. In May 2012, Serving Together, a project of Mental Health Association of Montgomery County, hosted an education event for mental health professionals and providers on behavioral health and substance abuse issues among recently returning veterans. The goal of the seminar was to increase the knowledge of best practices for treating military and veteran consumers in the community. We believe that, as we increase the level of awareness in our community, more practitioners will understand how they can better serve our military and veterans.
Dr Docherty: Of what specific aspects of military culture should care providers be aware?
Ms McNurlen: From what we have seen locally in Montgomery County, it would be helpful for providers to have a better sense of VA services and eligibility. We understand it can be a daunting task, and we do not want to make everyone subject matter experts, but understanding even just a small bit of the services provided by the VA can be a huge help.

- Ask patients about their military service and veteran status.
- Become familiar with veteran resources and eligibility requirements locally and nationally.
- Equip veterans and their families with education, counseling, and coping mechanisms to deal with mental health issues, including the symptoms of PTSD.
In addition to being more aware of the VA and its services, Serving Together would like to see local community organizations be better connected with each other—both military and nonmilitary specific. A 2008 study conducted by the Community Foundation for Montgomery County7 found that “local nonprofits may not have the outreach apparatus or procedures to accommodate the special circumstances of military families, but likely have the expertise and capacity to address some immediate and short-term concerns of those in greatest need.” Through increased coordination, veterans, service members, and their families can get the resources they want and need at the end of the day.7
We also see the value in having service providers and practitioners with a better understanding of military culture and how it differs from the civilian sector. Whether it be acronyms, rank structure, or how veteran is defined—understanding the culture can help the provider better recognize where veterans have been and what they may have experienced. Again, we are not asking that people become subject matter experts but, rather, asking that they understand what it means to have served in the military.
Ms Zeller: I agree. In general, civilians who have had little contact with the military do not understand that a military culture exists. The Substance Abuse and Mental Health Services Administration (SAMHSA) has long been grappling with discrimination against military personnel who seek mental health services. How do we encourage veterans with PTSD to actually seek treatment despite their reluctance? One answer lies in facilitating more peer support among veterans. Any combat veteran will feel a sense of camaraderie and trust with other combat veterans, and it helps if another veteran urges a peer to seek help for a mental health problem such as PTSD. When a spouse suggests getting help, the veteran may believe that the problem lies with the spouse, who does not understand what the veteran has experienced, whereas another veteran does understand. The Wounded Warrior Project Survey3 found that about 60% of veteran participants listed talking with another OEF or OIF veteran as a top resource that they used for addressing their mental health concerns.
Dr Lee: Service members and veterans may not only view mental health problems as a sign of weakness but may also be skeptical about the effectiveness of treatment. They may misunderstand the types of treatment that are available. They may also worry about the impact of mental health treatment disclosure on their security clearances or future career prospects.
Question 21 on the Standard Form 86, Questionnaire for National Security Positions, asks about history of health care for emotional or mental health conditions. Because service members perceive that answering “yes” to mental health treatment leads to security clearance denial, the question is being reexamined.8 The Secretary of Defense9 has issued new guidance on this topic, stating that recognizing and proactively seeking help for a mental health problem is viewed favorably rather than negatively.
Dr Chaudhry: Facilitating access to care and dealing with stigma are issues that we often view as being outside of the health care system proper—that is, they may be seen as ancillary to the care delivery process rather than central to it. I think part of improving the care system is to construct more organic ways for providing mental health care to veterans. Although this is a complex coordination and construction task, a key step is to acknowledge at the front end that stigma is a major issue and that certain people are central to providing access to care.10
To access a toolkit for community mental health providers, visit the VA Web site at: www.mentalhealth.va.gov/communityproviders.
What Services Are Needed for the Family Members of Returning Combat Veterans With PTSD and Other Mental Disorders?
Dr Keane: What would help the families of veterans in terms of promoting the veterans’ reintegration into civilian life and recovery from the experiences of being in war? I know the use of technology is crucial for getting resources organized, linked, and accessible.
Ms Zeller: One complaint that I often hear from family members is that there are so many resources out there that they do not know where to start. The amount of information on the Internet is overwhelming. Families usually end up using a resource that they hear about through word of mouth. Coordinated communication with families about what is available in their local area is needed.
Ms McNurlen: Many organizations and nonprofits have developed since 9/11 to better serve our military members, veterans, and their families, but what we have sometimes found locally is a lack of communication. In Montgomery County, Serving Together aims to coordinate community efforts, including local events, with resources at the local, regional, and national levels to create an easily accessible system of care. For instance, Serving Together plans to help residents better navigate the existing system so that service members, veterans, and their families seeking employment, benefits assistance, and/or mental health services get the resources they are looking for in a simple and efficient manner.
One way we hope to achieve this goal is through the recently launched online resource www.servingtogetherproject.org. The Web site puts quality resources, events, and local announcements in one easily accessible place. We envision that the Web site can be the home for Montgomery County resources and services available to local military members, veterans, and their families.
Dr Docherty: Practitioners who see veterans should understand the importance of educating the families. What I have found in my work is that certain patient-specific issues often arise, which means that focused training is more pertinent than broad training. Effective interventions do not require a large commitment of the family’s or the provider’s time. What is important is to address the specific, puzzling behaviors. For example, family members often need help understanding a veteran’s explosive anger. Why does their loved one lose his or her temper so quickly? How can they help manage bouts of anger or keep conversations from escalating into arguments? Clinicians should provide these tools to veterans and their families.
Ms McNurlen: Which practitioners should we look to assist with the educating of military families?
Dr Keane: My thoughts are that the VA practitioners are more attuned to this issue than private practitioners, although many private practitioners end up treating veterans. Both groups of practitioners can offer focused interventions for veterans and their families.
Dr Chaudhry: Family members must be taught coping and counseling mechanisms. Most family members are just struggling to manage at home with different issues as they arise.
Ms Zeller: One issue of major concern is suicide: veteran suicides are about 20% of the nation’s suicides.11 Dr Jesse, could you tell us about the VA program called Stand by Them?
Dr Jesse: The VA and the DoD launched the Stand by Them campaign to enlist the help of friends, families, and communities to prevent veteran suicides. The VA provides a 24-hour Veterans Crisis Line at 1-800-273-TALK (8255), text support at 838255, or online chat support at www.veteranscrisisline.net, even for those who are not registered with the VA, including loved ones of veterans. Hopefully, signs of emotional distress in veterans can be recognized before problems reach the crisis point.
In another strategy to combat suicide, the VA is working with the military chaplain service as well as with lay chaplains to detect warning signs in current and former servicemen and women.12 In rural communities, the clergy form the frontline of mental health providers. They can create public awareness and spot veterans who need help. Marriage and relationship problems often contribute to suicide, and chaplains can help veterans and their families with these issues.
Dr Keane: The Joining Forces Initiative13 not only connects military veterans and spouses with potential employers but also reaches health care providers and medical school faculty with the message to improve awareness of PTSD, TBI, and other mental health issues.14
How Can the Flow of Health Information From the DoD to the VA System be Improved?
Dr Keane: How can information sharing between the DoD and the VA improve, as more active duty personnel are transitioning to veteran status?
Dr Jesse: These departments are trying to compile and share coherent health- and work-related data across organizational boundaries. Our respective clinical information systems are being rejuvenated as we move forward with joint electronic records, called Virtual Lifetime Electronic Records (VLER). VLER includes information such as deployment and occupation in addition to health records. The DoD can identify people at risk for behavioral problems by examining data like absenteeism and disciplinary records, but to pull the data together requires crossing organizational boundaries. The improvement process lies within the VA and DoD because outside systems cannot access this information.
Dr Keane: I think there has been an ongoing initiative from the outset of the war to guide transitioning DoD personnel into the VA system, but creating a common platform between the 2 databases remains a challenge. This is a huge initiative that is critical to successfully transitioning activeduty military to the veterans health care system.
Dr Chaudhry: The VA and DoD are going through a series of technical challenges right now, but the goal is that health information will be used productively via a meaningful and efficient care delivery process. What is the new transition process going to look like for service personnel as they leave the DoD and enter the VA?
Dr Docherty: Some recent legislation will facilitate a more thorough transition for people separating from the military and becoming veterans, including support for health-related issues as well as issues pertaining to college applications, employment or business start-up, and financial planning.15 The idea is that this process, called Transition Goals Plans Success (or Transition GPS), would take a week or longer, rather than a few hours as before. The new process should help returning veterans adjust by providing practical assistance to plan for civilian life.
How Can Employers Help Restore Mental Wellness in Veterans With PTSD?
Dr Keane: What is the role of employers in helping veterans with PTSD whom they have hired?
Dr Docherty: First, employers should give veterans with PTSD a flexible work schedule to facilitate their treatment. Second, employers should require training programs for the veterans’ supervisors to help them understand the issues faced by and accommodations needed for veterans with PTSD or any disability.16 Third, employers must communicate with veterans’ care providers. For example, a veteran I was treating had a bad day at work. He spouted off complaints in his intracompany instant messaging system, and his inflammatory words got picked up by their alert system. The company’s initial reaction would have been to expel him, but, because we had a coordinated effort in place, they called me. I saw him right away and realized that he was having a mini-meltdown but was fine, so he went back to work very successfully. Good communication with care providers can help employers manage veterans with PTSD.
Dr Lee: Having a champion of veterans is beneficial in the employment community, such as among human resources personnel or boards of directors. Many employers do not understand the benefits or transferable skills that working in the military provides. Veteran-hiring toolkits for employers are available from various sources such as the Society for Human Resource Management.17 Employers need standard practices to implement rather than just a vague suggestion to “help veterans.”
Dr Docherty: I think that having an internal champion of veterans is essential. The companies that I have been working with have top-level executives committed to the effort of helping veterans.
Dr Keane: Initiatives to recruit and hire more veterans in government workforces have been suggested, but both state and federal workforces are facing reductions. Tax incentives for the private sector to hire veterans are available.
Dr Docherty: Many big corporations have stepped up their hiring of veterans and military spouses.
Ms McNurlen: In addition to the larger companies, we are trying to encourage smaller companies, nonprofits, and the public sector in our community to look at the benefits of hiring veterans or offering internship and volunteer opportunities.
Ms Zeller: When urging companies to hire more veterans, we need to remind employers that not every veteran returns “broken” or violent; this is another kind of myth. The public believes that most returning veterans struggle with mental illnesses, but the reality is that about 2 in 3 service members do not have serious mental health problems. Of those who do, 88% can continue their work without changes, even while they receive treatment.14 Veterans may be changed from seeing combat, but they return with strengths gained from their experiences as well. Employers should learn what veterans can do for their companies and strive to make them successful employees.
What Can Be Done in Communities to Construct a Better Environment for Returning Veterans?
Dr Keane: How can communities offer an environment that is conducive to helping returning veterans adjust to civilian life?
Dr Docherty: Several levels of awareness must be raised in the community (Table 2).18 First, people in general must recognize the degree of sacrifice and service that veterans have provided to the country. Second, facts about veterans and what they have to offer should be shared with key community groups, such as mayors, teachers, local business leaders, and community boards. Third, a process to generate enthusiasm and provide specific discrete steps for helping and hiring veterans should be established.
Ms Zeller: I completely agree that there is not one solution, and the term community differs depending on who you are trying to target.
I am a proponent of peers speaking to peers. For example, employed veterans could speak to their coworkers on Veterans Day, and other employees could speak about their veteran or enlisted parents or grandparents near Memorial Day.
Dr Lee: Another key to community support is coordination among federal, state, and local government resources, nonprofit agencies, universities, and other stakeholders.
Dr Docherty: I recently started the nonprofit Circles of Hope Foundation in Bedford, New York, to provide support for community engagement and support for the early identification and intervention for people suffering from serious mental illness.
Dr Chaudhry: PTSD management requires a broad integration of medical care and social determinants of health, including employment, education, and housing. Merging these resources together is beyond the scope of the medical care system and beyond the scope of any one community organization. Robust networks linking resources need to be developed across communities. These networks need to span across individual organizations and provide a comprehensive range of services. Building these networks will be challenging, and community organizations will need support. A key feature of these networks would be to accurately forecast what services veterans will likely need before they reenter the community. That allows for proactive planning for each individual and also helps define what kind of support community organizations will need from funders. Drawing on systems science approaches would be a strong foundation for developing these cross-disciplinary networks of services and resources.
Ms McNurlen: In our community, Serving Together is trying to coordinate existing services and resources to make sure the system is easier to navigate. Montgomery County, which is the home of Walter Reed National Military Medical Center in Bethesda, has approximately 50,000 veterans.19 We discovered that we need to educate existing community service organizations about each other and what they all do. The goal is that, no matter where a veteran goes for services, he or she will not hear, “I’ m sorry, we don’ t do that here, and I don’ t know who does.”
Serving Together is also working with local community service providers to better define (1) who is a veteran, (2) what the difference is between National Guard and Reserve status, (3) who is an active-duty service member, (4) what benefits might be available, and (5) what resources, including the VA, are available to veterans in the community. Most importantly, providers and nonprofit organizations need to ask every person seeking services about their military experience and status so that they know who they are serving, what the person is eligible for, and how he or she can best be helped.
Conclusion
The challenges that veterans with PTSD may face in accessing evidence-based treatment include the stigma associated with seeking help and the lack of practitioners who understand military culture and veterans’ issues. Family and peer support are essential to encourage veterans to seek treatment and cope with active-duty experiences and related mental health issues, including PTSD symptoms. Government initiatives combined with business and community support will help veterans reintegrate into civilian life, get the help they need when necessary, and successfully return to the work force.
Disclosure of off-label usage: The chair has determined that, to the best of his knowledge, no investigational information about pharmaceutical agents that is outside US Food and Drug Administration-approved labeling has been presented in this article.
References
1. Martinez L, Bingham A. US veterans: by the numbers. http://abcnews.go.com/Politics/us-veterans-numbers/story?id=14928136#. Published 2011. Accessed December 4, 2012.
2. Wounded Warrior Project. Who we serve. http://www.woundedwarriorproject.org/mission.aspx. Published November 11, 2011. Accessed December 4, 2012.
3. Franklin M, Hintze W, Hornbostel M, et al. 2012 Wounded Warrior Project Survey. http://www.woundedwarriorproject.org/mission/what-our-alumni-say.aspx. Published June 29, 2012. Accessed December 4, 2012.
4. American Psychiatric Association. Diagnostic and Statistical Manual of Mental Disorders, Fourth Edition, Text Revision. Washington, DC: American Psychiatric Association; 2000.
5. Burnam MA, Meredith LS, Tanielian T, et al. Mental health care for Iraq and Afghanistan War Veterans. Health Aff (Millwood). 2009;28(3):771-782. PubMed doi:10.1377/hlthaff.28.3.771
6. US Department of Veterans Affairs. Health benefits: veteran eligibility. http://www.va.gov/healthbenefits/apply/veterans.asp. Updated September 26, 2012. Accessed December 4, 2012.
7. The Montgomery County Community Foundation. Troops and family care fund feasibility study. Silver Spring, MD; Montgomery County Community Foundation: 2008. http://www.thecommunityfoundation.org/atf/cf/%7B8C61F1DB-3FE6-435F-9B32-2D0D51A3C2EF%7D/TroopstudyFINAL.pdf. Accessed December 4, 2012.
8. Abramson L. Can counseling complicate your security clearance? http://www.npr.org/2012/09/11/160898774/question-21-a-matter-of-national-security. Published September 11, 2012. Accessed December 4, 2012.
9. Department of Defense guidance on question 21, standard form 86, questionnaire for national security positions [memorandum]. Washington, DC: Secretary of Defense; September 4, 2012. http://www.lockheedmartin.com/content/dam/lockheed/data/corporate/clearanceconnection/DoD%20Guidance%20on%20Q21.pdf. Accessed December 4, 2012.
10. Haire T. Financial problems or PTSD need not affect security clearance. http://www.ng.mil/news/archives/2009/07/071309-Clearance.aspx. Published July 8, 2009. Accessed December 4, 2012.
11. Parrish K. Battaglia calls reducing suicides a top priority. American Forces Press Service. December 12, 2011. http://www.defense.gov/news/newsarticle.aspx?id=66431. Accessed December 4, 2012.
12. Sheftick G. Chaplains step up “Strong Bonds” to halt suicides. Army News Service. September 25, 2012. http://www.army.mil/article/87980/Chaplains_step_up__Strong_Bonds__to_halt_suicides/. Accessed December 4, 2012.
13. Joining Forces: taking action to serve America’s military families. http://www.whitehouse.gov/joiningforces. Accessed December 4, 2012.
14. Cloud R. An international approach to military mental health. http://www.whitehouse.gov/blog/2012/10/03/international-approach-military-mental-health. Published October 3, 2012. Accessed December 4, 2012.
15. Cronk TM. New program aims to better help troops transition to civilian life. American Forces Press Service. August 18, 2012. http://www.defense.gov/news/newsarticle.aspx?id=117544. Accessed December 4, 2012.
16. US Equal Employment Opportunity Commission. Veterans and the Americans with Disabilities Act (ADA): a guide for employers. http://www.eeoc.gov/eeoc/publications/ada_veterans_employers.cfm. Accessed December 4, 2012.
17. Curtis SA. Support from behind enemy lines: 10 steps to becoming a military-ready employer. Alexandria, VA: Society for Human Resource Management; 2012. http://www.shrm.org/TemplatesTools/Toolkits/Documents/12-0177%20Behind_the_Lines_Toolkit_FNL.pdf. Accessed December 4, 2012.
18. US Department of Veterans Affairs. National Center for PTSD. http://www.ptsd.va.gov/. Updated October 15, 2012. Accessed December 4, 2012.
19. US Department of Veterans Affairs. Projected number of veterans in Maryland: 2010. http://www.mdlegion.org/Forms/new_vets_10.pdf. Published 2010. Accessed December 4, 2012.