Objective: To study possible psychiatric and criminological risk factors of intimate partner femicide (IPF) as well as the bereaved offspring’s psychiatric morbidity and premature death.
Method: We conducted a nested case-control study, based on Swedish national registries, including all perpetrators of IPF. We computed risk estimates relative to matched population controls, which were compared to those of non-IPF homicide offenders. Exposed children were matched to population controls and followed longitudinally up to 37 years. Offspring outcomes were psychiatric and substance use disorders (according to ICD) self-harm; violent crime; suicide; and premature, all-cause death.
Results: We identified 261 male IPF perpetrators and 494 bereaved children from 1973 through 2009. Multivariable logistic regression suggested that major mental disorder (adjusted odds ratio [OR] = 5.9; 95% CI, 3.3-10.6) and violent crime convictions (adjusted OR = 4.4; 95% CI, 2.7-7.2) were independent risk factors of IPF, but substance use disorders were not (aOR = 0.4; 95% CI, 0.2-1.0). Children exposed to IPF before age 18 years had elevated risks of major mental disorder (adjusted hazard ratio [HR] = 5.7; 95% Cl, 3.0-10.6), substance use disorders (adjusted HR = 5.8; 95% CI, 2.8-11.9) and self-harm (adjusted HR = 5.7; 95% CI, 3.0-11.1). Offspring 18 years or older at the IPF had an increased risk of completed suicide (adjusted HR = 4.3; 95% CI, 1.3-14.5).
Conclusions: Previous major mental disorder and violent behavior were strong independent risk factors for IPF. Bereavement caused by IPF had significant associations with the offspring’s future life, especially for those below 18 years of age at exposure. Our findings demonstrate the need of direct support to the exposed offspring by health care providers and social services.
Killing the Mother of One’s Child:
Psychiatric Risk Factors Among Male Perpetrators and Offspring
Health Consequences
ABSTRACT
Objective: To study possible psychiatric and criminological risk factors of intimate partner femicide (IPF) as well as the bereaved offspring’s psychiatric morbidity and premature death.
Method: We conducted a nested case-control study, based on Swedish national registries, including all perpetrators of IPF. We computed risk estimates relative to matched population controls, which were compared to those of non-IPF homicide offenders. Exposed children were matched to population controls and followed longitudinally up to 37 years. Offspring outcomes were psychiatric and substance use disorders (according to ICD) self-harm; violent crime; suicide; and premature, all-cause death.
Results: We identified 261 male IPF perpetrators and 494 bereaved children from 1973 through 2009. Multivariable logistic regression suggested that major mental disorder (adjusted odds ratio [OR] = 5.9; 95% CI, 3.3–10.6) and violent crime convictions (adjusted OR = 4.4; 95% CI, 2.7–7.2) were independent risk factors of IPF, but substance use disorders were not (aOR = 0.4; 95% CI, 0.2–1.0). Children exposed to IPF before age 18 years had elevated risks of major mental disorder (adjusted hazard ratio [HR] = 5.7; 95% Cl, 3.0–10.6), substance use disorders (adjusted HR = 5.8; 95% CI, 2.8–11.9) and self-harm (adjusted HR = 5.7; 95% CI, 3.0–11.1). Offspring 18 years or older at the IPF had an increased risk of completed suicide (adjusted HR = 4.3; 95% CI, 1.3–14.5).
Conclusions: Previous major mental disorder and violent behavior were strong independent risk factors for IPF. Bereavement caused by IPF had significant associations with the offspring’s future life, especially for those below 18 years of age at exposure. Our findings demonstrate the need of direct support to the exposed offspring by health care providers and social services.
J Clin Psychiatry
dx.doi.org/10.4088/JCP.15m09564
© Copyright 2016 Physicians Postgraduate Press, Inc.
aDepartment of Clinical Neuroscience, Karolinska Institutet, Centre for Psychiatry Research, Stockholm, Sweden
bDepartment of Medical Epidemiology and Biostatistics, Karolinska Institutet, Stockholm, Sweden
*Corresponding author: Henrik Lysell, MD, Karolinska Institutet, Department of Clinical Neuroscience/Stockholm County Council, Centre for Psychiatry Research, St Göran’s Hospital, SE-112 81 Stockholm, Sweden ([email protected]).
The most severe form of violence in intimate relationships is the killing of a partner; when that occurs, the victim is most commonly a woman.1 If children are left behind, exposure to such trauma might be associated with long-term adverse effects on health and well-being. Globally, 39% to 47% of all homicides with female victims are committed by an intimate partner, and estimates are higher in high-income countries1—49% in Sweden and 40% to 50% in the United States.2,3 In 90% of the intimate partner homicides in which the perpetrator also commits suicide, the homicide victim is female.4
Perpetrator Risk Factors
A history of threats and violence—most importantly interfamilial,5 but also extrafamilial3—are risk factors for intimate partner femicide (IPF). Further, perpetrator history of mental disorders, such as depression,6 psychosis,7 personality disorders,8 and substance use disorders,7,9 and also migration/acculturation,10 race (in American studies),5 and access to guns5 are identified risk factors. Perpetrators who also commit suicide, ie, IPF-suicide cases, are older, and concurrent depression is a known risk factor.11,12 These cases, however, are often not included in studies of intimate partner homicide, since they are lost to further investigation.
It has been argued that men who kill their partners deviate less from the “normal” than do other homicide offenders. Mental disorders, previous convictions,9 and substance use disorders13 seem to be more common among the latter. There is still a scarcity of studies within this field, and research from different cultural settings with representative samples is needed to further inform of specific psychiatric and criminal risk factors among men who kill a female intimate partner.
Offspring Consequences
Children who become deprived of their mother by IPF—or of both parents by IPF-suicide—are exposed to significant trauma, which is likely to affect them in the future. Research in offspring’s bereavement of a parent caused by homicide is sparse,14 and the few studies that are published are based on small samples.15 It is known, however, that a parent’s unnatural death, and particularly suicide, increases the risk of violent behavior, substance use disorders, serious mental disorders, and suicide in bereaved children.16,17 Younger age at such exposure is associated with a higher risk of later suicide.17 The risk of suicide and adverse events in children after the loss of one or both parents by IPF or IPF-suicide has, to our knowledge, not been studied.
We aimed to identify psychiatric and criminal risk factors that distinguish male perpetrators of IPF from other male homicide offenders. Further, we investigated the risk among IPF-exposed children of developing mental disorders, engaging in suicidal and criminal behavior, or facing premature death, with regard to their age at the time of trauma.
METHOD
Study Setting
We conducted a case-control study, nested within the Swedish population and identified through Swedish national registries, including all cases of femicide from 1973 through 2009, in which the perpetrator and the victim had mutual children (biological or adopted); these cases were defined as intimate partner femicide (IPF). Children were included in a matched cohort study with regard to the outcomes of mental disorder, suicidal/violent criminal behavior, and death by suicide or other cause. Identification was possible through the linkage of longitudinal, nationwide population-based registries by use of the unique personal identity numbers.18
Identification of Perpetrators and Controls
We first identified deceased women whose cause of death was recorded as deadly violence inflicted by another person (International Classification of Diseases [ICD]-8, -9: E96; ICD-10: X85–Y09) (the Cause of Death Register). Deaths with uncertain intent were not included. Second, we identified a partner on the condition of a mutual child (the Multi-Generation Register). This procedure enabled identification of events in which a child was affected. Intimate partner femicide was considered when a partner had been convicted of murder, manslaughter, or involuntary manslaughter (the National Crime Register) or committed suicide (the Cause of Death Register) within 3 days of the death of the female victim. For each case, 10 controls, matched by birth year and gender, were randomly drawn from the population (the Total Population Register).
We also identified all male non-IPF homicide perpetrators (convicted for homicide or manslaughter) during the study period, who were likewise matched to general population controls.
Identification of Children
Children of the killed woman and the perpetrating male were identified by the Multi-Generation Register and constituted the child cohort. To each child proband, we matched 10 population controls (the Total Population Register) on birth year and gender. Children were followed until outcome, emigration, or end of follow-up (December 31, 2009), whichever came first.
Psychiatric Morbidity
Diagnoses were extracted from the National Patient Register from January 1, 1973, through December 31, 2009. The National Patient Register contains ICD codes from all inpatient care in Sweden, including the few private hospitals. Coverage and validity of diagnoses are fair to excellent.19–21 The principal psychiatric diagnosis (except substance use disorders and personality disorders, which were included in any position) was recorded for cases and controls. Major mental disorder included psychotic disorders, affective disorders, and personality disorders. Substance use disorders included alcohol and other drugs. Any mental disorder comprised all of the above-mentioned disorders, and, in addition, phobic disorder, anxiety disorder, obsessive-compulsive disorder, eating disorder, and adjustment disorder. Categorization followed previous work on intrafamilial violence.22
Previous self-harm was defined as hospitalization due to self-inflicted harm of determined and undetermined intent (ICD-8, -9: E950–E959, E980–E989; ICD-10: X60–X84, Y10–Y34). Completed suicide was obtained from the Cause of Death Register by similar diagnostic coding. We included both certain and uncertain suicides, consistent with many other studies, to avoid underestimation.23
Criminal Offending
Conviction data were obtained from 1973 through 2009 from the National Crime Register. This register contains all convictions committed by perpetrators aged 15 years and older in Sweden regardless of the sentence; fines; or custodial, noncustodial, or compulsory forensic psychiatric care. Any crime comprised all convictions; violent crime included convictions for homicide, assault, robbery, illegal threats or intimidation, and sexual offenses (not including prostitution, the hiring of prostitutes, or possession of child pornography).24 Convictions of attempted and aggravated forms of these offenses were included whenever applicable.
Sociodemographic Factors
The highest level of education was collected from the Education Register and the National Census (Statistics Sweden). Information was available from 1970 and 1990–2009. Low education was defined as ≤ 9 years of completed education. Immigrant status was defined as being born outside of Sweden (the Total Population Register).
Statistical Analyses
We used Student t test for means and χ2 test or Fisher exact test for comparison of proportions between groups. Perpetrators of IPF and non-IPF homicide were compared to controls in separate analyses; we used conditional logistic regression analyses to take into account the dependence between cases and controls due to matching, which yielded odds ratios (ORs) with 95% confidence intervals (CIs) as estimates of risk for the studied factors for each perpetrator group compared to their controls. We initially performed bivariate analyses, then we adjusted for education and immigrant status; in the final models, all variables were included. All covariates in the analyses were extracted as occurrences before the index event. Statistical analyses were performed using SAS software, version 9.4 (SAS Institute, Cary, North Carolina) with the proc logistic command for conditional logistic regression.
In the offspring cohort, we stratified analyses by age at exposure according to the Swedish age of majority (0–17 years, ≥18 years). We used Cox regression to compute hazard ratios (HRs) with 95% CIs for the outcomes of major mental disorder, substance use disorders, self-harm, conviction of a violent crime, suicide, and nonsuicidal death after exposure to IPF. Different covariates were entered in the adjusted models; for suicide, we used a history of self-harm in parent and child prior to exposure. For the remaining outcomes, we controlled for preexposure history of each outcome aspect present in the child and/or the child’s parents. For the outcome of nonsuicidal death, we controlled for immigrant status and education in parents. SAS software, version 9.4 (SAS Institute), was used with the PROC PHREG command for conditional Cox regression.
RESULTS
Perpetrators
We identified 261 instances of IPF during the study period (1973–2009); thus, 261 men had killed a woman with whom they had children. Of these events, 80 (30.7%) were IPF-suicides. The mean age of perpetrators of IPF was 45.8 years (SD = 14.0). Previous hospitalization records for mental disorders were present among 44 (16.9%) of the perpetrators. The most common diagnoses among those hospitalized due to a mental disorder were affective disorder (n = 15, 5.7%) and substance use disorders (n = 15, 5.7%). Previous self-harm requiring inpatient observation and treatment was detected in 13 subjects (5.0%), and 43 (16.5%) had been convicted of a violent crime prior to the index event. The proportions of all studied variables differed between perpetrators and controls (Table 1). IPF-suicide offenders were significantly older (53.3 vs 42.5 years, t = 6.17, P < .001) but less often born outside Sweden (20.0% vs 53.0%, χ2 = 24.7, P < .001) or convicted of a violent crime (1.2% vs 23.2%, χ2 = 19.4, P < .001), compared to IPF offenders who did not commit suicide (data not shown in table).
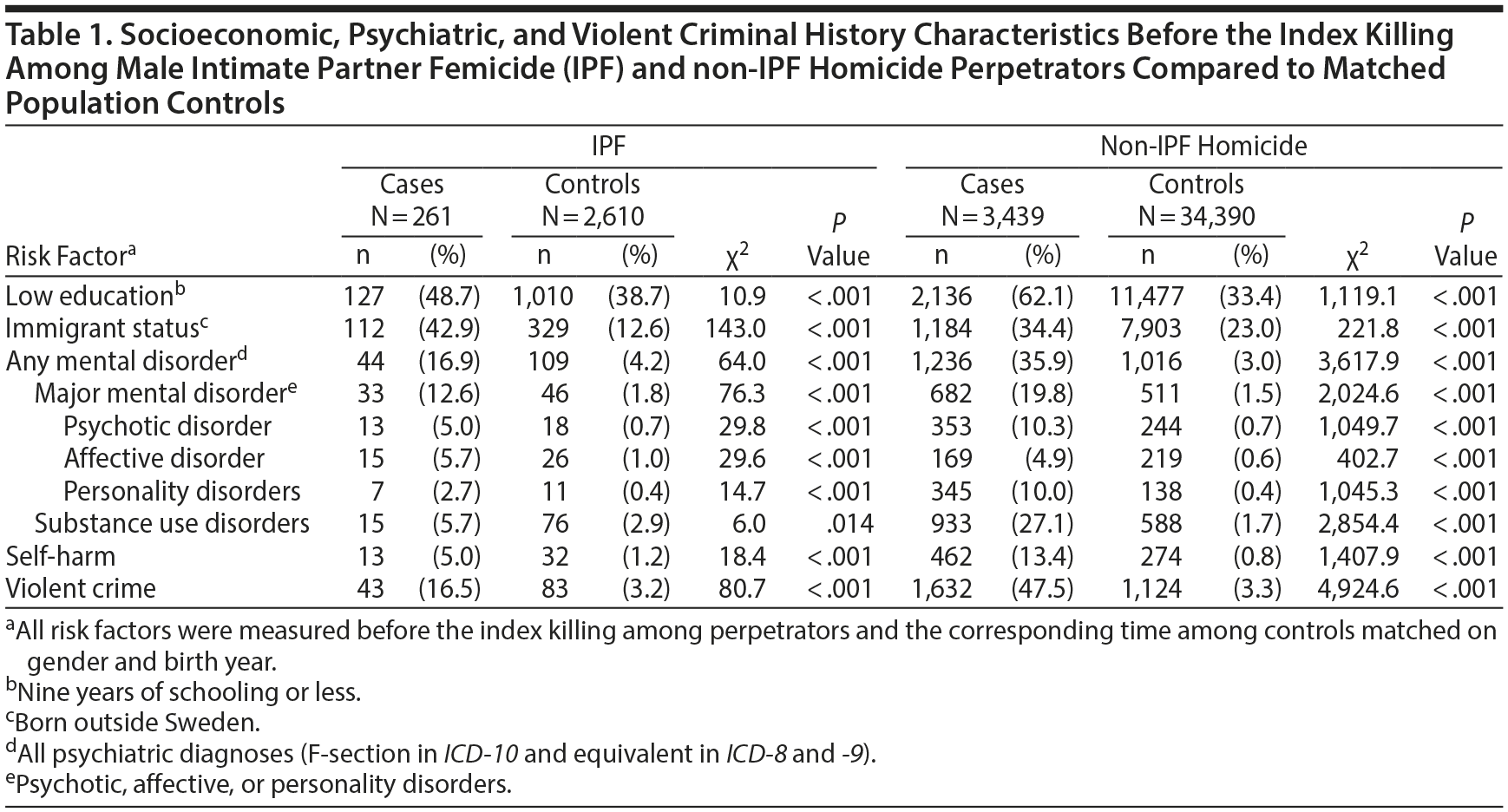
Among non-IPF homicide offenders, more than a third had a psychiatric history, with substance use disorders being the most common (n = 933, 27.1%). Almost half had a previous conviction for violent crime (Table 1).
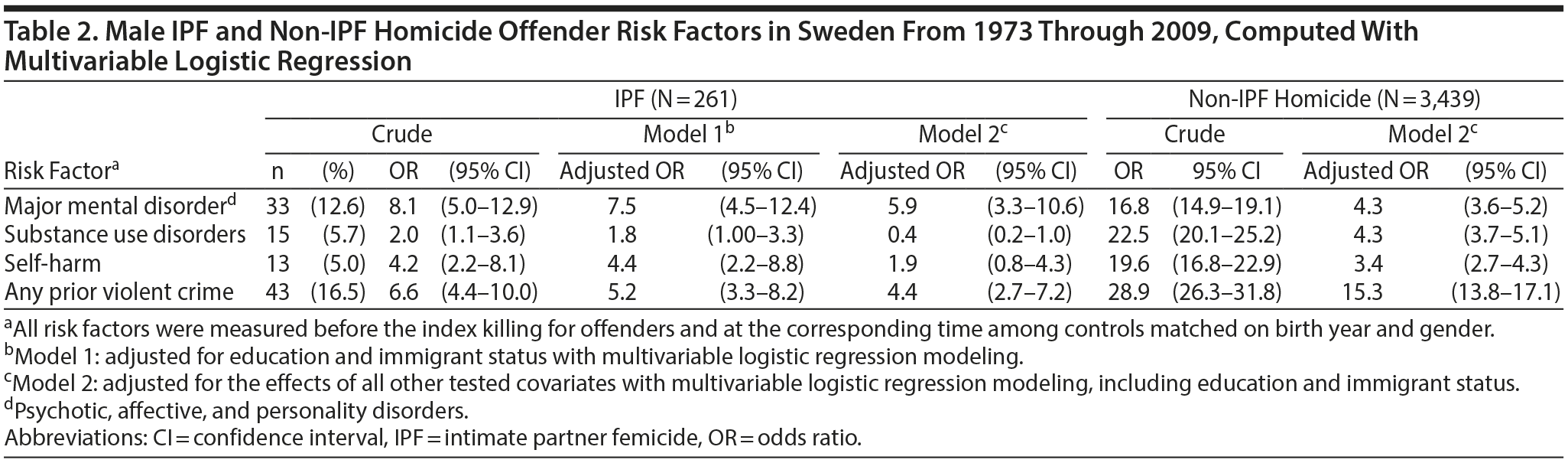
Adjustment for educational level and immigrant status did not alter the associations substantially in any of the groups (data not shown for homicide offenders). In the full regression models, the strongest independent risk factor for being an IPF offender was major mental disorder (adjusted OR = 5.9; 95% CI, 3.3–10.6). Substance use disorders and previous self-harm did not remain as independent risk factors of IPF (Table 2). For non-IPF homicide offenders, prior conviction for a violent crime was the strongest independent risk factor, and psychiatric risk factors had independent associations with adjusted ORs ranging from 3.4 to 4.3
Offspring
We identified 494 individuals deprived of their mother from IPF and included them in the offspring cohort. Another 32 children were killed in the same incident as their mother and, thus, were not included. The cohort was followed for 0.25 to 37 years (mean age = 18.2 years, SD = 10.8). Mean age at the time of bereavement was 8.6 years (SD = 5.1; range, 0–17 years) in the younger group (n = 308) and 31.0 years (SD = 9.8; range, 18–59 years) in the older group (n = 186). Offspring who lost both parents in IPF-suicide were older (n = 136, mean age = 26.4 years, SD = 12.0) than those whose father did not commit suicide (n = 358, mean age = 13.5 years, SD = 12.3, P < .001).
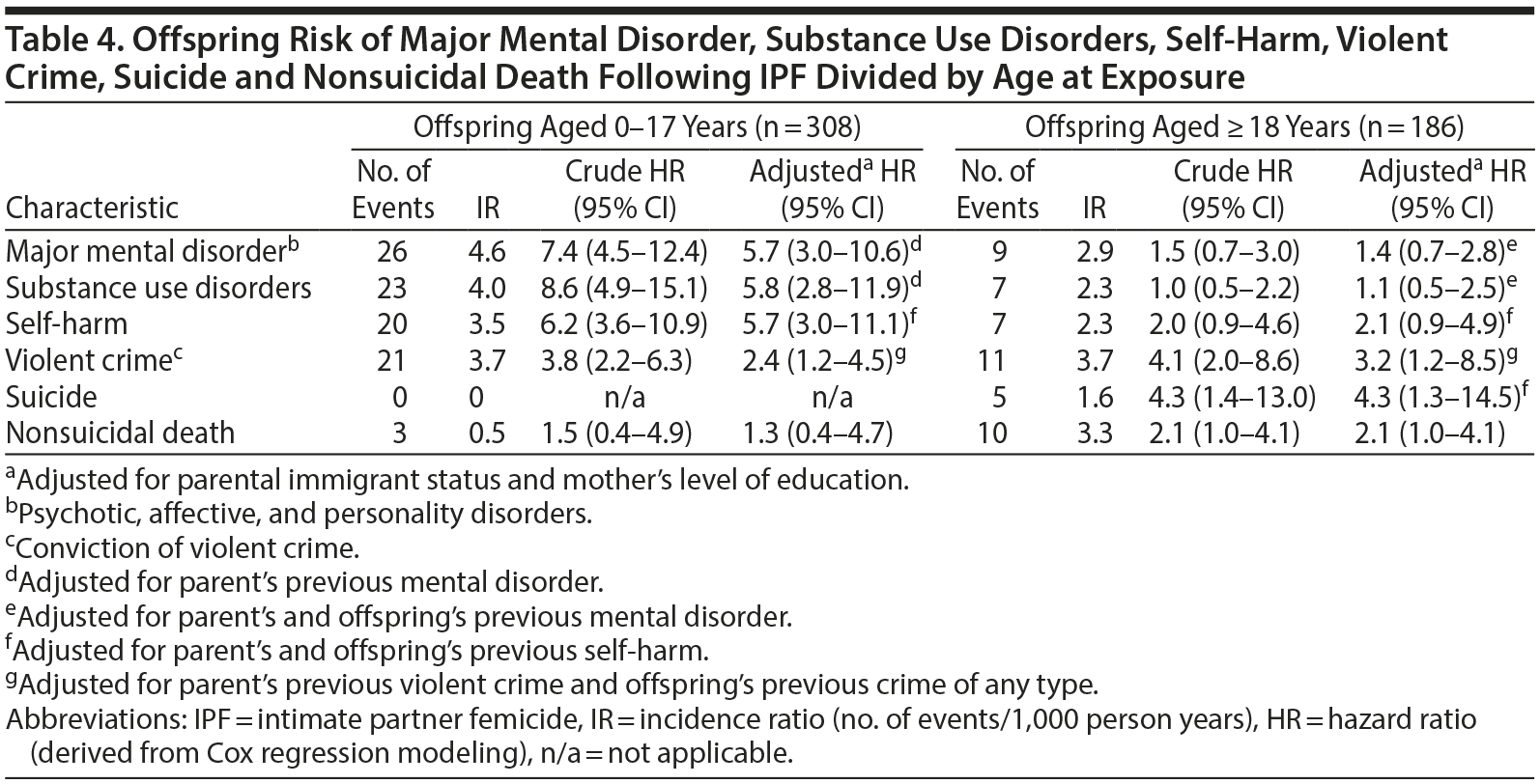
Offspring exposed to IPF under age 18 years had a significantly higher incidence of mental disorders, substance use disorders, violent crime, and self-harm than did comparison children during follow-up (Table 3). The risk of developing a major mental disorder was more than 7-fold compared to controls (HR = 7.4; 95% CI, 4.5–12.4) and remained essentially unchanged after adjustment (adjusted HR = 5.7; 95% CI, 3.0–10.6). Risk of substance use disorders was almost 6-fold (adjusted HR = 5.8; 95% CI, 2.8–11.9), and the same held for self-harm (adjusted HR = 5.7; 95% CI, 3.0–11.1) (Table 4).
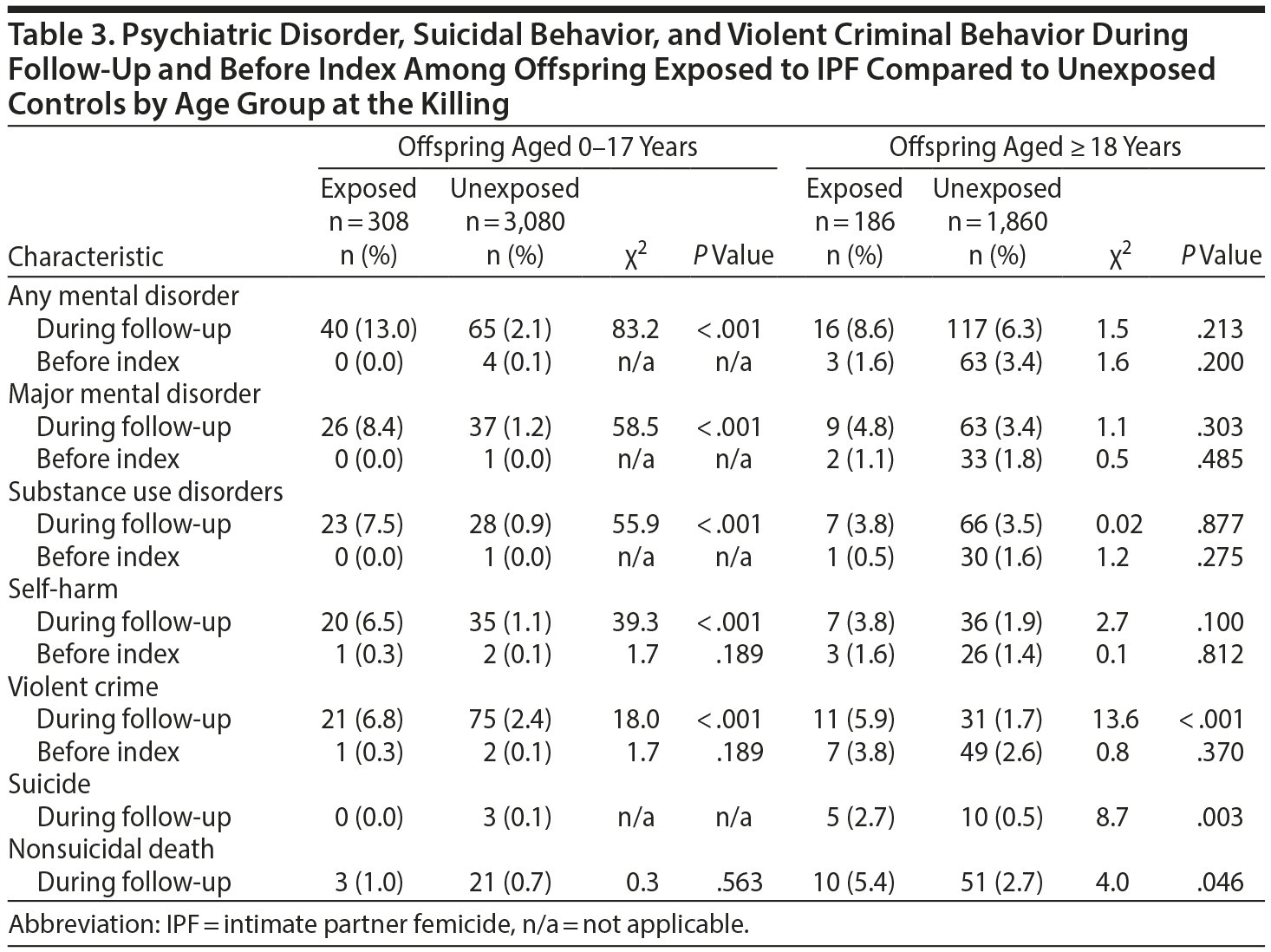
For offspring who were 18 years of age or older at exposure, convictions for violent crime, death by suicide, and premature nonsuicidal death were more common than among unexposed controls during follow-up (Table 3); suicide risk was 4 times higher, with no difference between crude and adjusted point estimates (adjusted HR = 4.3, 95% CI 1.3–14.5). The adjusted risk of nonsuicidal death was 2.1 (95% CI, 1.0–4.1) (Table 4).
DISCUSSION
We conducted a nationwide, nested case-control study of men who had killed a woman with whom they had 1 or more children; and, to our knowledge, this is the first large-scale study of offspring outcomes following such a killing. Previous hospitalization for mental disorder and convictions of violent crime were independent offender risk factors of IPF perpetration in multivariable analyses. In contrast, previous hospitalizations for self-harm or substance use disorders increased the risk for non-IPF homicide perpetration but were not significantly associated with IPF. Offspring younger than 18 years at the killing of their mother had clearly elevated risks to develop mental and substance use disorders, exhibit self-harming behavior, and be convicted of violent crime during follow-up. Offspring aged 18 years and above when exposed had elevated risks of violent crime, suicide, and premature death from other causes.
Our primary finding was that major psychiatric morbidity was an independent risk factor of IPF and non-IPF homicide. Previous studies confirm that perpetrators of deadly violence often suffer from mental disorders.22,25 We found that a history of affective disorder was particularly common among IPF offenders, which may be considered in line with previous findings that depression is of particular importance to femicide in intimate relationships.4,26 The prevalence of mental disorders among perpetrators varies in the literature7 and is often higher than the prevalence in the present study; the same holds for previous self-harm.3 These differences may be explained by our use of hospitalization-based diagnoses only. A history of substance use disorders was more common among IPF offenders than controls, as previously found,7 but we found that substance use disorders were not an independent risk factor for IPF. Drug use is usually strongly correlated to violent crime in both correctional and psychiatric cohort studies,27–29 and in line with this finding, substance use disorders (also including alcohol-related diagnoses) were a risk factor for non-IPF homicide in the present study. Our different results for the 2 offender groups are in line with previous findings.30 We were not able to investigate the effects of alcohol intoxication at the time of the offense, which is a factor closely related to family violence.12 Further, our estimates of substance use disorders were, again, based on hospital diagnoses, which should indicate an underestimation of the “true” prevalence. For the risk estimates, however, inference was made with general population controls, and we have no reason to assume that detection rates should differ between perpetrators and controls and, thus, affect statistical precision.
Offspring Consequences
As expected, exposure to IPF was associated with poor long-term prognosis in offspring and significantly differed with age at the time of trauma. We found increased risks for hospitalization due to mental disorders (including substance use disorders) and self-harm and for convictions for violent crimes among those under age 18 years at exposure, but there were no suicides in this group. For those aged 18 years and older at the killing of their mother, elevated long-term risks for later suicide and conviction for a violent crime were found. We have not found any previous quantitative studies on bereavement caused by IPF, but the risk ratios might be compared to bereavement of a parent by suicide or other death. In a recent study,17 the risk of hospitalization for a suicide attempt was elevated in offspring after parental death by suicide, accident, or other cause, regardless of age at loss. The increased risks of suicide were found only in offspring aged below 18 years at loss and only after parental death by suicide or accidental death.17 This may seem contradictory to our finding that no suicides occurred during follow-up in the younger group. For children bereaved by parental suicide at an early age, however, the risk of suicidal behavior does not commence to increase until some years after the loss of the parent and then increases for decades.31 If a similar pattern would be assumed to follow bereavement by IPF or IPF-suicide, the limited follow-up time of the current study might have failed to capture late suicides. In line with our findings, the risk of being convicted for a violent crime is also elevated for offspring bereaved of a parent by any cause and regardless of age at loss.17
Previous research has demonstrated a high level of heritability in suicidal behavior,32 and, therefore, we adjusted the analyses on suicide for earlier self-harm among parents and children. Likewise, mental disorders have a hereditary component of various degrees for different disorders.33,34 Our results were adjusted for mental disorders present in parents and children before the index event. With these adjustments, the results were relatively unchanged, which points to a significant impact of the traumatic event and its immediate consequences.
Strengths and Limitations
A major strength of this study is the national coverage, obtained by linkage of high-quality national registers. We were able to calculate unbiased estimates for risk factors of IPF perpetrators and adverse outcomes for exposed offspring by use of randomly selected controls drawn from the general population. The design enabled inclusion of IPF-suicides, an important group—quantitatively and etiologically—often absent in research within the field of IPF. A further strength is the use of an additional group of non-IPF homicide offenders in order to contextualize differences between cases and controls, which are not necessarily specific for deadly violence toward female partners.
There are several limitations. First, the modest sample size, with limited statistical power did not allow for calculations of separate estimates for IPF and IPF-suicides. Second, we had no knowledge of the status of the offender-victim relationship at the time of the killing; we were only able to identify dyads through a mutual child. By this design, the number of IPF cases was reduced, and a selection bias was introduced by which findings can be generalized to couples with children only. Further, we lacked information on possible ongoing mental disorder as well as on alcohol or drug intoxication at the time of the offense. Finally, it might have been relevant to single out offenses against women from the explaining variable “violent crime,” since such violence is a known risk factor of IPF.9 Regrettably, no information of the sex of the victim is recorded in the registry data.
CONCLUSIONS
Previous violent criminal behavior and a history of mental illness, but not substance use disorders, are independent risk factors among men who kill a female intimate partner. Children who experience such trauma at an early age run the elevated risk of future mental disorder, self-harm, and criminal behavior. For offspring older at the time of loss, the risks of criminal behavior and death, including suicide, are increased. Although further research into the effects on offspring is warranted, children of victims of IPF should be offered direct support, and their psychosocial needs should be given priority by health care providers and social services.
Submitted: October 2, 2014; accepted March 26, 2015.
Online first: January 5, 2016
Potential conflicts of interest: None of the authors report any competing interests.
Funding/support: The study was supported by grants from the National Crime Compensation Authority of Sweden and the Swedish Prison and Probation Service.
Role of the sponsor: None.
Previous presentation: Presented at the National Prison and Probation Services; February 6, 2103; Stockholm, Sweden.
Additional information: Access to the Swedish registers is restricted to those who have gained ethical approval for their study and received approval from the holder of the register.
REFERENCES
1. Stöckl H, Devries K, Rotstein A, et al. The global prevalence of intimate partner homicide: a systematic review. Lancet. 2013;382(9895):859–865. doi:10.1016/S0140-6736(13)61030-2 PubMed
2. Rying M. Utvecklingen av dödligt våld mot kvinnor i nära relationer. Stockholm, Sweden: The Swedish National Council for Crime Prevention (Brottsförebyggande rådet); 2007:6.
3. Campbell JC, Webster D, Koziol-McLain J, et al. Risk factors for femicide in abusive relationships: results from a multisite case control study. Am J Public Health. 2003;93(7):1089–1097. doi:10.2105/AJPH.93.7.1089 PubMed
4. Rosenbaum M. The role of depression in couples involved in murder-suicide and homicide. Am J Psychiatry. 1990;147(8):1036–1039. doi:10.1176/ajp.147.8.1036 PubMed
5. Campbell JC, Glass N, Sharps PW, et al. Intimate partner homicide: review and implications of research and policy. Trauma Violence Abuse. 2007;8(3):246–269. doi:10.1177/1524838007303505 PubMed
6. Boyle DJ, O’Leary KD, Rosenbaum A, et al. Differentiating between generally and partner-only violent subgroups: lifetime antisocial behavior, family of origin violence, and impulsivity. J Fam Violence. 2008;23(1):47–55. doi:10.1007/s10896-007-9133-8
7. Liem M, Hengeveld M, Koenraadt F. Domestic homicide followed by parasuicide: a comparison with homicide and parasuicide. Int J Offender Ther Comp Criminol. 2009;53(5):497–516. doi:10.1177/0306624X09334646 PubMed
8. Koziol-McLain J, Rameka M, Giddings L, et al. Partner violence prevalence among women attending a Maori health provider clinic. Aust N Z J Public Health. 2007;31(2):143–148. doi:10.1111/j.1753-6405.2007.00032.x PubMed
9. Dobash RE, Dobash RP, Cavanagh K, et al. Not an ordinary killer; just an ordinary guy: when men murder an intimate woman partner. Violence Against Women. 2004;10(6):577–605. doi:10.1177/1077801204265015
10. Edelstein A. Culture transition, acculturation and intimate partner homicide. Springerplus. 2013;2(1):338. doi:10.1186/2193-1801-2-338 PubMed
11. Marzuk PM, Tardiff K, Hirsch CS. The epidemiology of murder-suicide. JAMA. 1992;267(23):3179–3183. doi:10.1001/jama.1992.03480230071031 PubMed
12. Banks L, Crandall C, Sklar D, et al. A comparison of intimate partner homicide to intimate partner homicide-suicide: one hundred and twenty-four New Mexico cases. Violence Against Women. 2008;14(9):1065–1078. doi:10.1177/1077801208321983 PubMed
13. Kivivuori J, Lehti M. Social correlates of intimate partner homicide in Finland: distinct or shared with other homicide types? Homicide Stud. 2012;16(1):60–77. doi:10.1177/1088767911428815
14. Dowdney L. Childhood bereavement following parental death. J Child Psychol Psychiatry. 2000;41(7):819–830. doi:10.1111/1469-7610.00670 PubMed
15. Steeves RH, Parker B. Adult perspectives on growing up following uxoricide. J Interpers Violence. 2007;22(10):1270–1284. doi:10.1177/0886260507305153 PubMed
16. Runeson B, Asberg M. Family history of suicide among suicide victims. Am J Psychiatry. 2003;160(8):1525–1526. doi:10.1176/appi.ajp.160.8.1525 PubMed
17. Wilcox HC, Kuramoto SJ, Lichtenstein P, et al. Psychiatric morbidity, violent crime, and suicide among children and adolescents exposed to parental death. J Am Acad Child Adolesc Psychiatry. 2010;49(5):514–523, quiz 530. PubMed
18. Ludvigsson JF, Otterblad-Olausson P, Pettersson BU, et al. The Swedish personal identity number: possibilities and pitfalls in healthcare and medical research. Eur J Epidemiol. 2009;24(11):659–667. doi:10.1007/s10654-009-9350-y PubMed
19. Dalman Ch, Broms J, Cullberg J, et al. Young cases of schizophrenia identified in a national inpatient register—are the diagnoses valid? Soc Psychiatry Psychiatr Epidemiol. 2002;37(11):527–531. doi:10.1007/s00127-002-0582-3 PubMed
20. Ludvigsson JF, Andersson E, Ekbom A, et al. External review and validation of the Swedish national inpatient register. BMC Public Health. 2011;11(1):450. doi:10.1186/1471-2458-11-450 PubMed
21. Sellgren C, Landén M, Lichtenstein P, et al. Validity of bipolar disorder hospital discharge diagnoses: file review and multiple register linkage in Sweden. Acta Psychiatr Scand. 2011;124(6):447–453. doi:10.1111/j.1600-0447.2011.01747.x PubMed
22. Lysell H, Runeson B, Lichtenstein P, et al. Risk factors for filicide and homicide: 36-year national matched cohort study. J Clin Psychiatry. 2014;75(2):127–132. doi:10.4088/JCP.13m08372 PubMed
23. Neeleman J, Wessely S. Changes in classification of suicide in England and Wales: time trends and associations with coroners’ professional backgrounds. Psychol Med. 1997;27(2):467–472. doi:10.1017/S0033291796004631 PubMed
24. Frisell T, Lichtenstein P, Långström N. Violent crime runs in families: a total population study of 12.5 million individuals. Psychol Med. 2011;41(1):97–105. doi:10.1017/S0033291710000462 PubMed
25. Fazel S, Grann M. Psychiatric morbidity among homicide offenders: a Swedish population study. Am J Psychiatry. 2004;161(11):2129–2131. doi:10.1176/appi.ajp.161.11.2129 PubMed
26. Logan J, Hill HA, Black ML, et al. Characteristics of perpetrators in homicide-followed-by-suicide incidents: National Violent Death Reporting System—17 US States, 2003–2005. Am J Epidemiol. 2008;168(9):1056–1064. doi:10.1093/aje/kwn213 PubMed
27. Parker RN, Auerhahn K. Alcohol, drugs, and violence. Annu Rev Sociol. 1998;24(1):291–311. doi:10.1146/annurev.soc.24.1.291
28. Fazel S, Lichtenstein P, Grann M, et al. Bipolar disorder and violent crime: new evidence from population-based longitudinal studies and systematic review. Arch Gen Psychiatry. 2010;67(9):931–938. doi:10.1001/archgenpsychiatry.2010.97 PubMed
29. Lundholm L, Haggård U, Möller J, et al. The triggering effect of alcohol and illicit drugs on violent crime in a remand prison population: a case crossover study. Drug Alcohol Depend. 2013;129(1–2):110–115. doi:10.1016/j.drugalcdep.2012.09.019 PubMed
30. Weizmann-Henelius G, Matti Grönroos L, Putkonen H, et al. Gender-specific risk factors for intimate partner homicide—a nationwide register-based study. J Interpers Violence. 2012;27(8):1519–1539. doi:10.1177/0886260511425793 PubMed
31. Kuramoto SJ, Runeson B, Stuart EA, et al. Time to hospitalization for suicide attempt by the timing of parental suicide during offspring early development. JAMA Psychiatry. 2013;70(2):149–157. doi:10.1001/jamapsychiatry.2013.274 PubMed
32. Tidemalm D, Runeson B, Waern M, et al. Familial clustering of suicide risk: a total population study of 11.4 million individuals. Psychol Med. 2011;41(12):2527–2534. doi:10.1017/S0033291711000833 PubMed
33. Hettema JM, Neale MC, Kendler KS. A review and meta-analysis of the genetic epidemiology of anxiety disorders. Am J Psychiatry. 2001;158(10):1568–1578. doi:10.1176/appi.ajp.158.10.1568 PubMed
34. Lichtenstein P, Yip BH, Björk C, et al. Common genetic determinants of schizophrenia and bipolar disorder in Swedish families: a population-based study. Lancet. 2009;373(9659):234–239. doi:10.1016/S0140-6736(09)60072-6 PubMed
This PDF is free for all visitors!



