Objective: One of the proposed revisions for DSM-5 is to rate panic attacks as a separate dimension across all mental disorders. The idea is that panic attacks occurring outside panic disorder are a dimension predicting important clinical outcomes. The aim of this study was to validate the proposition for DSM-5 that panic attacks have predictive value for overall psychopathology onset, course, and functioning.
Method: Data were derived from the Netherlands Mental Health Survey and Incidence Study (NEMESIS), a prospective population-based study. Using the Composite International Diagnostic Interview (with classifications based on DSM-III-R), 5,571 subjects were selected who had (1) no panic history, (2) a history of panic attacks (but no panic disorder), (3) current panic attacks, or (4) current panic disorder. The impact of panic status on the prevalence of anxiety, affective, alcohol, and any mental disorders; on the onset and persistence of these disorders during 3-year follow-up; and on levels of functioning during 3-year follow-up (as assessed with the 36-Item Short-Form Health Survey) was examined.
Results: Current panic attacks outside the realm of panic disorder were associated with increased prevalence of mental disorders (χ23=490.6; P<.001), increased onset of mental disorders (hazard ratio=4.42; 95% CI, 2.88-6.80), persistence of mental disorders (odds ratio=2.72; 95% CI, 1.53-4.82), and impaired functioning during 3-year follow-up (F=69.67; P<.001). Although the impact was smaller than for panic disorder, the associations identified for panic attacks were consistent and significant and were, to a lesser extent, also found for a history of panic attacks.
Conclusions: Given the consistent impact of panic attacks on various aspects of psychopathology, the proposition to dimensionally rate panic attacks across all mental disorders may be of great value for clinical care.
J Clin Psychiatry 2012;73(9):1195-1202
© Copyright 2012 Physicians Postgraduate Press, Inc.
Submitted: February 26, 2012; accepted June 4, 2012(doi:10.4088/JCP.12m07743).
Corresponding author: Neeltje M. Batelaan, MD, PhD, Department of Psychiatry and EMGO Institute, VU University Medical Center and GGZ inGeest, A.J. Ernststraat 1187, 1081 HL Amsterdam, the Netherlands ([email protected]).
Find more articles on this and other psychiatry and CNS topics:
The Journal of Clinical Psychiatry
The Primary Care Companion for CNS Disorders
ABSTRACT
Objective: One of the proposed revisions for DSM-5 is to rate panic attacks as a separate dimension across all mental disorders. The idea is that panic attacks occurring outside panic disorder are a dimension predicting important clinical outcomes. The aim of this study was to validate the proposition for DSM-5 that panic attacks have predictive value for overall psychopathology onset, course, and functioning.
Method: Data were derived from the Netherlands Mental Health Survey and Incidence Study (NEMESIS), a prospective population-based study. Using the Composite International Diagnostic Interview (with classifications based on DSM-III-R), 5,571 subjects were selected who had (1) no panic history, (2) a history of panic attacks (but no panic disorder), (3) current panic attacks, or (4) current panic disorder. The impact of panic status on the prevalence of anxiety, affective, alcohol, and any mental disorders; on the onset and persistence of these disorders during 3-year follow-up; and on levels of functioning during 3-year follow-up (as assessed with the 36-Item Short-Form Health Survey) was examined.
Results: Current panic attacks outside the realm of panic disorder were associated with increased prevalence of mental disorders (χ23 = 490.6; P < .001), increased onset of mental disorders (hazard ratio = 4.42; 95% CI, 2.88-6.80), persistence of mental disorders (odds ratio = 2.72; 95% CI, 1.53-4.82), and impaired functioning during 3-year follow-up (F = 69.67; P < .001). Although the impact was smaller than for panic disorder, the associations identified for panic attacks were consistent and significant and were, to a lesser extent, also found for a history of panic attacks.
Conclusions: Given the consistent impact of panic attacks on various aspects of psychopathology, the proposition to dimensionally rate panic attacks across all mental disorders may be of great value for clinical care.
J Clin Psychiatry 2012;73(9):1195-1202
© Copyright 2012 Physicians Postgraduate Press, Inc.
Submitted: February 26, 2012; accepted June 4, 2012(doi:10.4088/JCP.12m07743).
Corresponding author: Neeltje M. Batelaan, MD, PhD, Department of Psychiatry and EMGO Institute, VU University Medical Center and GGZ inGeest, A.J. Ernststraat 1187, 1081 HL Amsterdam, the Netherlands ([email protected]).
One of the proposed revisions for DSM-5 is to dimensionally rate panic attacks across all mental disorders.1,2 The idea is that panic attacks occurring outside panic disorder predict the occurrence of, persistence of, and level of functioning in other disorders. Panic attacks are highly prevalent in the general population,3-9 and high rates of comorbidity with a wide range of mental disorders have been reported.3,4,6,10,11 For example, 71.9% of persons with lifetime panic attacks had a lifetime DSM-IV disorder.6 Furthermore, it was shown that panic attacks significantly increase the risk of onset of mental disorders.12-17 In addition, a few studies have reported an impact of past panic attacks on psychopathology,4,12,16 suggesting that even a history of panic attacks should raise awareness among clinicians for current and future psychopathology.
However, in a review undertaken to propose changes in DSM-5, Craske and colleagues1 concluded that a more thorough understanding of the impact of panic attacks is needed. First, it is unclear to what extent associations reported for panic attacks are driven by panic disorder, because the majority of studies did not stratify analyses to compare panic attacks versus panic disorder.1 The impact of full-blown comorbid mental disorders such as panic disorder on other mental disorders is known and would be no reason to specify panic attacks alongside mental disorders. Second, insight into the contribution of a history of panic attacks is lacking. Previous studies either did not differentiate between a history of panic attacks and current panic attacks1 or reported contradictory results.12,16 Third, the impact of confounding variables has not always been taken into account, although studies that adjust for potential confounders still report evidence for the impact of panic attacks (see Craske et al1). Fourth, most previous studies relied on cross-sectional data. Prospective data would enable examining the impact of panic attacks on course trajectories. Finally, given that little attention has been paid to the impact of panic attacks on persistence of psychopathology and on course of functioning,18,19 research addressing these aspects is needed.
The present study addresses these gaps by examining the association between panic attacks and presence of a wide range of mental disorders, the predictive value of panic attacks on onset and persistence of mental disorders, and the impact of panic attacks on current and future functioning. Effect on outcomes was compared between persons with no panic history, a history of panic attacks (but no panic disorder), current panic attacks, and current panic disorder. Our aim was to thereby empirically test the proposal for DSM-5 to dimensionally rate panic attacks across mental disorders.
METHOD
Procedures
Data were derived from the Netherlands Mental Health Survey and Incidence Study (NEMESIS), a naturalistic, prospective, general population survey (N = 7,076). Data were recorded in 3 waves: at baseline in 1996 (T0), after 12-month follow-up in 1997 (T1), and after 3 years in 1999 (T2). The mean time between T0 and T1 was 379 days (SD = 35 days) and between T1 and T2, 744 days (SD = 71 days). The sampling procedure consisted of a multistage, stratified, random sample.20 Procedures were approved by the ethics committee of the Netherlands Institute of Mental Health and Addiction, and informed consent was obtained according to the prevailing Dutch law of 1996. Participants were representative of the Dutch population with regard to gender, civil status, and level of urbanization. Only the 18-24 years age group was slightly underrepresented.20 Of the 7,076 respondents interviewed at baseline, 5,618 were followed up after 1 year (response 79.4%), and 4,848 were followed up after 3 years (response 68.5% of those participating at T0). In the current study, availability of data from the baseline assessment and at least 1 follow-up assessment was considered necessary. At both follow-up measurements, 4,796 subjects were assessed; at T0 and T1, 822 were assessed; and at T0 and T2, 52 were assessed. Those with a history of panic disorder (without current panic attacks or panic disorder) (n = 99) were excluded to prevent the possibility that associations of past panic attacks were driven by past panic disorder. This resulted in a total sample size of 5,571. Attrition between baseline and T2 was not significantly associated with any of the panic groups, after adjustment for sociodemographics and somatic disorders.
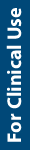
- Panic attacks occur in a wide range of psychiatric disorders; that is, their occurrence is not limited to panic disorder or anxiety disorders.
- Clinicians should be aware of the risk of onset of psychiatric disorders when patients present with panic attacks.
- In patients with panic (panic disorder, panic attacks, past panic attacks), both mental functioning and physical functioning are more impaired than in those without panic.
Characteristics
Baseline characteristics included gender, age, education (lower than versus equal to or higher than secondary school), and presence of somatic disorders. Somatic disorders were defined as the number of self-reported somatic disorders, out of a 32-item list21 used in various large-scale psychiatric cohort studies,22,23 that were treated or monitored by a doctor in the year preceding T0. This list includes the most common somatic disorders, such as chronic obstructive pulmonary disease, osteoarthritis, heart disease, stroke, peptic ulcer, and diabetes. Comparisons between self-reports of chronic physical disorders and medical records show moderate to good concordance.24-26
Assessment of Panic
Panic status was defined using the Composite International Diagnostic Interview (CIDI),27 version 1.1,28 classifying disorders according to the DSM-III-R.29 The CIDI is a fully structured interview for diagnosing mental disorders with acceptable reliability and validity.30 Most population-based studies use the CIDI as a diagnostic instrument that can be conducted by trained lay interviewers.
The “no panic” group consisted of those who reported neither past nor current panic attacks or panic disorder. The “history of panic attacks” group consisted of those who reported lifetime panic attacks, but no panic disorder, and no panic occurring in the last 12 months. The “current panic attacks” group consisted of those who reported at least 1 panic attack during the previous 12 months, not fulfilling criteria for panic disorder, and irrespective of panic history. A panic attack was defined as at least 1 sudden experience of intense fear in a situation in which most people would not be afraid. This experience may not be attributable to an organic cause and must have been accompanied by at least 4 of the 13 panic-related symptoms in DSM-III-R.29 These include the following: shortness of breath or smothering sensations; dizziness, unsteady feelings, or faintness; palpitations or accelerated heart rate; trembling or shaking; sweating; choking; nausea or abdominal distress; depersonalization or derealization; numbness or tingling sensations; flushes (hot flashes) or chills; chest pain or discomfort; fear of dying; and fear of going crazy or doing something uncontrolled. According to this definition, the occurrence of “unexpected” panic attacks was not required, thereby also allowing for situationally bound or situationally predisposed panic attacks.
The “current panic disorder” group consisted of those fulfilling DSM-III-R criteria for panic disorder during the previous 12 months, irrespective of panic history.
Assessment of Mental Disorders
A range of mental disorders were assessed with the CIDI. Anxiety disorders consisted of 12-month agoraphobia, simple phobia, social phobia, generalized anxiety disorder, or obsessive-compulsive disorder, but not panic disorder. Affective disorder consisted of 12-month major affective disorder, dysthymic disorder, or bipolar disorder. Alcohol disorder consisted of 12-month alcohol dependence. Given the small numbers of subjects with 12-month schizophrenia (n = 11), eating disorder (n = 13), and drug disorders (n = 54), these disorders could not be analyzed separately. These diagnoses, as well as anxiety, affective, and alcohol disorders, were included in the category “any disorder.”
Assessment of Functioning
Functioning was assessed with the 36-Item Short-Form Health Survey (SF-36)31 at all 3 waves. The SF-36 is a widely applied questionnaire involving 8 subscales. Scoring was performed on a 0-100 scale, with 100 defined as maximum functioning. In this study, total scores were computed. Good reliability and validity of this instrument have been shown elsewhere.32-35 Sufficient internal reliability was also demonstrated in NEMESIS (total scores: T0, Cronbach α = 0.83; T1, α = 0.82; T2, α = 0.81).
Statistics
The distribution of characteristics of participants across panic groups was compared using 2-tailed χ2 statistics for categorical variables and 1-way analysis of variance statistics for continuous variables. Differences between panic groups were calculated in separate analyses.
The prevalence of psychopathology (ie, any disorder) and the prevalence of anxiety disorders, affective disorders, and alcohol disorders were compared across panic groups using 2-tailed χ2 statistics. In addition, differences in prevalence of separate mental disorders across panic groups were calculated in separate analyses.
To examine whether panic predicts onset of psychopathology in a sample at risk, ie, without psychopathology at baseline, incidence densities were calculated, which took into account differences in sample sizes between the panic groups and possible differences in length of follow-up period. Incidence density was defined as the number of onsets per 100 observed person-years. The observation period was calculated per person. Onset of the disorder was estimated halfway between T0 and T1 if a subject fulfilled criteria for a new disorder at T1, and halfway between T1 and T2 if a subject fulfilled criteria for a new disorder at T2 only. Both first-ever incidence and recurrent incidence disorders were taken into account. Cox regression analyses were conducted to examine the association between panic groups and time to onset of psychopathology.
The association between panic groups and persistence of psychopathology during 3 years of follow-up was examined using logistic regression analyses. Persistence was defined as a 12-month diagnosis at T1 and/or any 2-year diagnosis at T2 among those with a diagnosis at baseline. Subsequently, similar analyses were conducted for the persistence of each specific disorder separately, ie, anxiety, affective, and alcohol disorders.
We adjusted both longitudinal analyses for gender, age, education, and somatic disorders. Because current mental disorders may impact upon onset or persistence of psychopathology, we additionally adjusted for current mental disorders (other than the group under consideration). Thus, when investigating onset or persistence of anxiety disorders, we additionally adjusted for current mood disorders, alcohol disorders, eating disorders, drug disorders, and schizophrenia. All analyses were conducted using SPSS version 15.0.36
Finally, to examine the association of panic groups (as compared to subjects without panic) and level of functioning during 3 years of follow-up, linear mixed models were used. Estimated mean scores were calculated for the total SF-36 scores. All variables were entered in the model as fixed factors. The only random factor entered in the model was the subject. A panic-by-time interaction term was entered to investigate whether the course of functioning over the 3-year follow-up period differed between the panic groups.
RESULTS
Sample
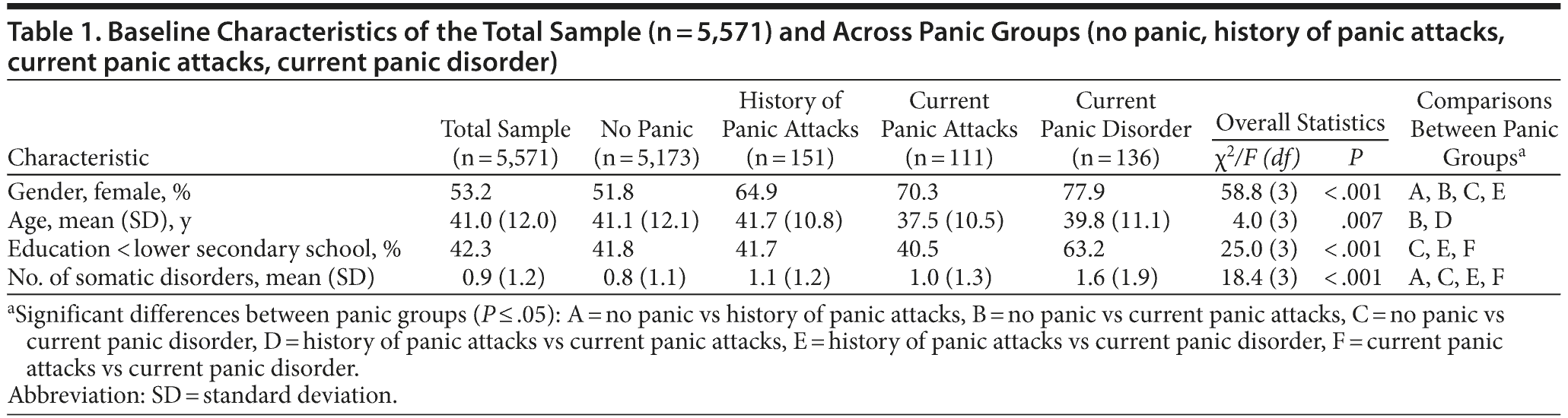
Of the total sample (n = 5,571), a large majority, 91.9% (n = 5,173), had no current or past panic at T0 (NoPan). A history of panic attacks (HisPA) was present in 2.7% (n = 151) of the sample. Current panic attacks (PA) were present in 2.0% (n = 111) of the sample, and current panic disorder (PD) was present in 2.4% (n = 136) of the sample. The baseline characteristics of the total sample and across panic groups are displayed in Table 1.
Panic and the Association With Psychopathology
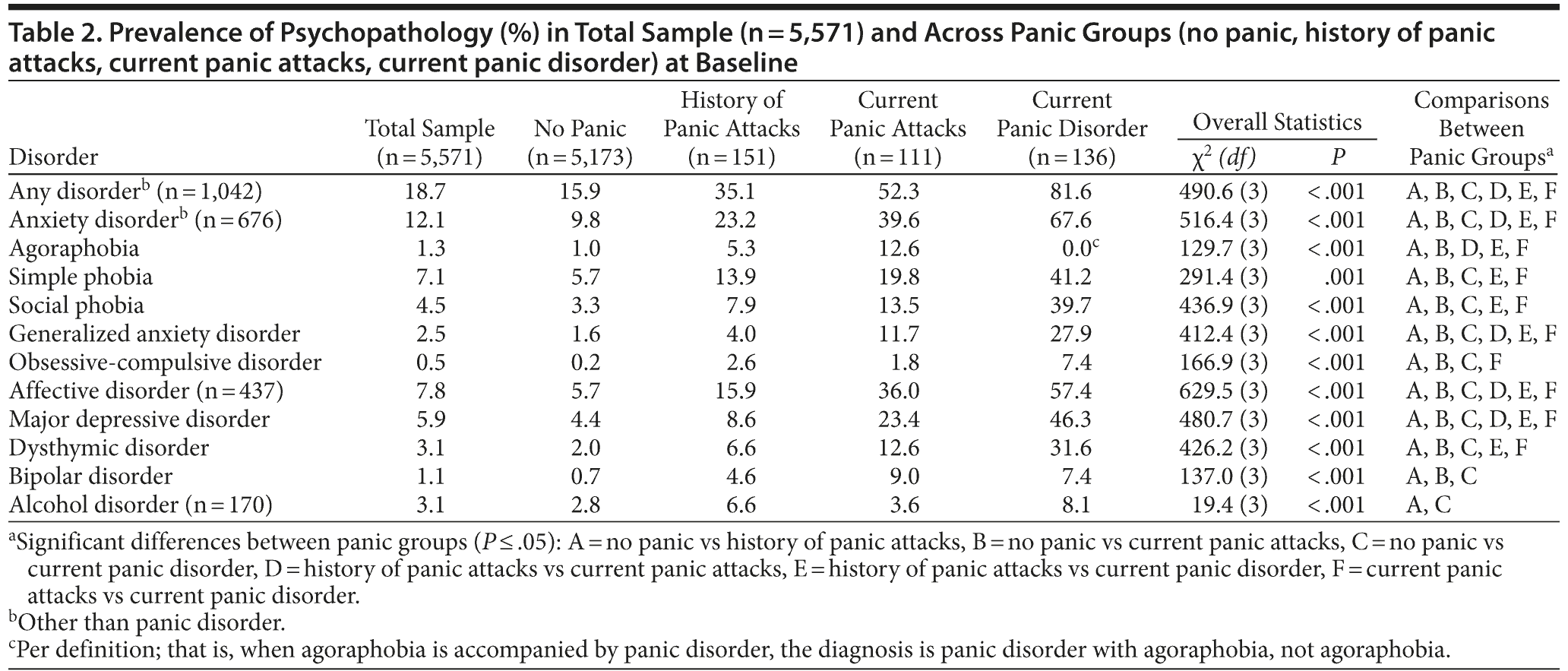
As illustrated in Table 2, rates of comorbid disorders were significantly higher in all panic groups compared to NoPan: 15.9% of NoPan, 35.1% of HisPA, 52.3% of PA, and 81.6% of PD had any mental disorder (other than panic disorder) (P < .001). Associations were strongest for PD, but also significant for PA and, to a lesser extent, HisPA. A higher prevalence of comorbid disorders in PA was also found when investigating anxiety disorders and affective disorders, and in HisPA when investigating anxiety disorders, affective disorders, and alcohol disorders. Again, in general, associations were strongest for PD, followed by PA, and finally HisPA.
Panic as Predictor of Onset of Psychopathology
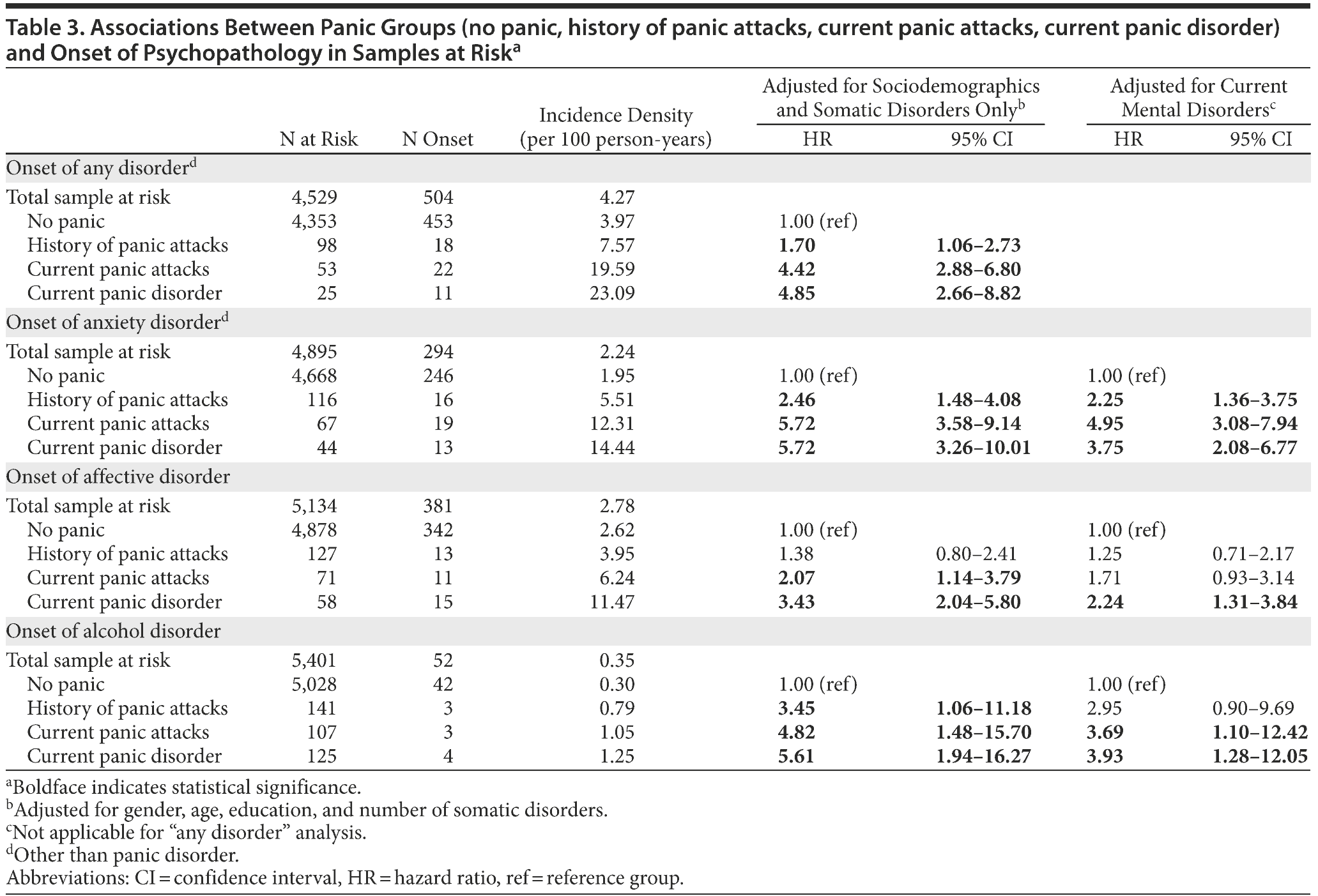
Of the total sample, 4,529 subjects (81.3%) had no mental disorder at baseline. Of these, 504 (11.1%) developed a disorder during follow-up. In total, 11,814.4 person-years of follow-up time were observed; hence, the incidence density was 4.27 per 100 person-years for the total sample (Table 3). In the NoPan group, the incidence density was 3.97; in HisPA, the incidence density almost doubled (7.57); and in PA and PD, it rose to 19.59 and 23.09, respectively. As shown by the hazard ratios (HRs), onset of psychopathology was associated with all panic groups. Associations could not be explained by sociodemographics and somatic disorders. Likewise, onset of anxiety disorders, affective disorders, and alcohol disorders was increased for panic groups. Associations were least strong for those with HisPA and did not reach significance when onset of affective disorders was investigated. Although most associations were stronger for PD compared to PA, associations between PA and onset of psychopathology were quite strong, with HRs varying between 2.07 (onset of affective disorder) and 5.72 (onset of anxiety disorder). When we adjusted for current mental disorders as a potential confounder in the association between panic attacks and onset of psychopathology, HRs diminished, but remained higher as compared to HRs for those without panic. Thus, although current mental disorders had an impact on onset of psychopathology, they did not explain the reported associations for panic attacks.
Panic as Predictor of Persistence of Psychopathology
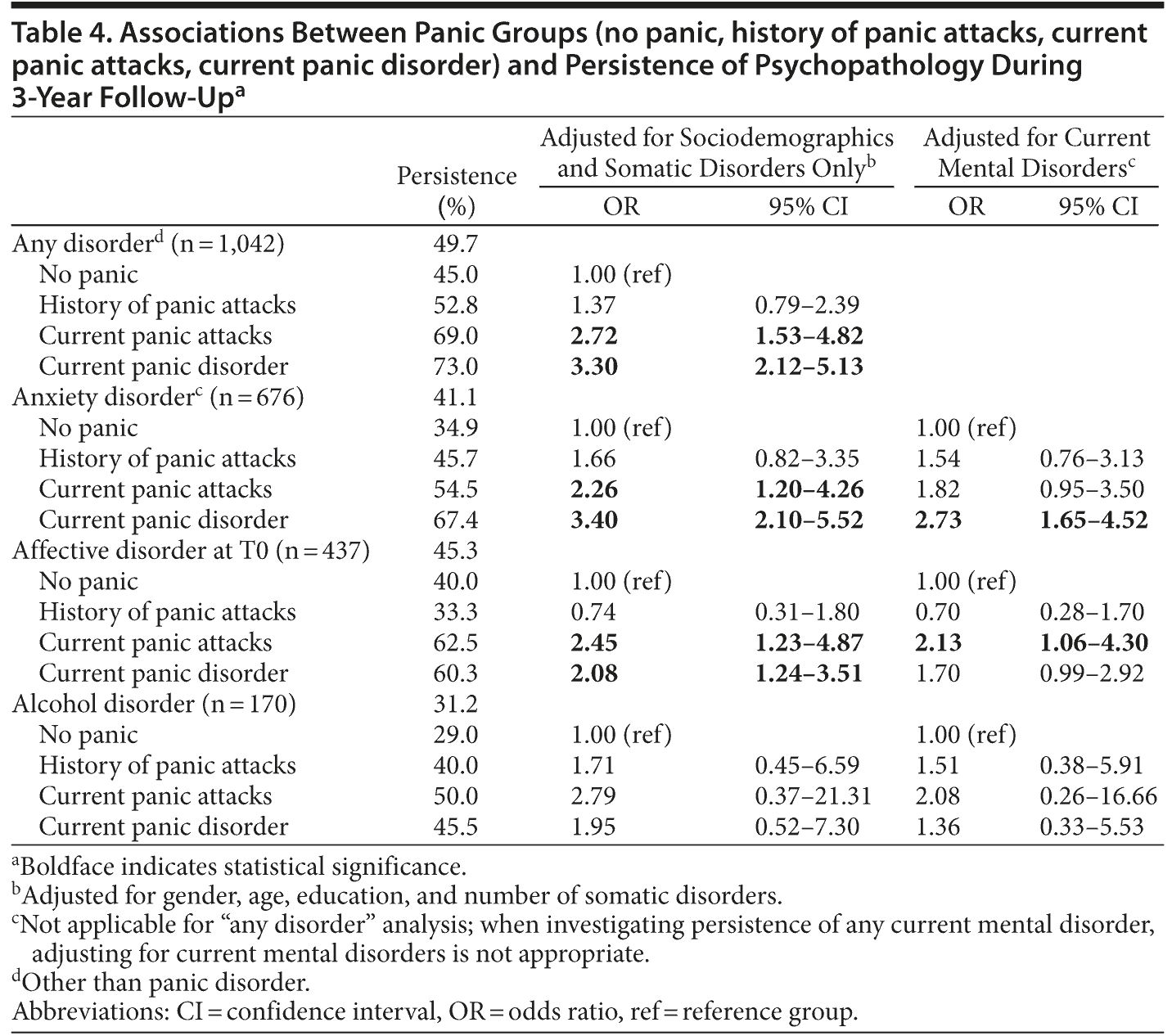
About half of the subjects with any disorder at baseline had any disorder at T1 and/or T2 (49.7%) (Table 4). Whereas in NoPan 45.0% of mental disorders persisted, psychopathology more often persisted across increasing levels of panic (HisPA, 52.8%; PA, 69.0%; PD, 73.0%). Associations were strongest for PD (OR = 3.30) and still fairly strong in PA (OR = 2.72). In HisPA, the association did not reach significance (OR = 1.37; 95% CI, 0.79-2.39). Anxiety disorders, affective disorders, and alcohol disorders also tended to persist in the presence of panic compared to NoPan. When we investigated persistence of any disorder and of anxiety disorders, estimates were somewhat higher for PD than for PA; when we investigated the persistence of affective disorders and of alcohol disorders, estimates were somewhat lower for PD compared to PA. ORs for HisPA did not reach significance in any of the comparisons, nor did ORs in alcohol disorders. Comorbid current mental disorders impacted upon persistence of psychopathology but could not fully explain the associations between panic groups and persistence of psychopathology.
Impact of Panic on Level of Functioning
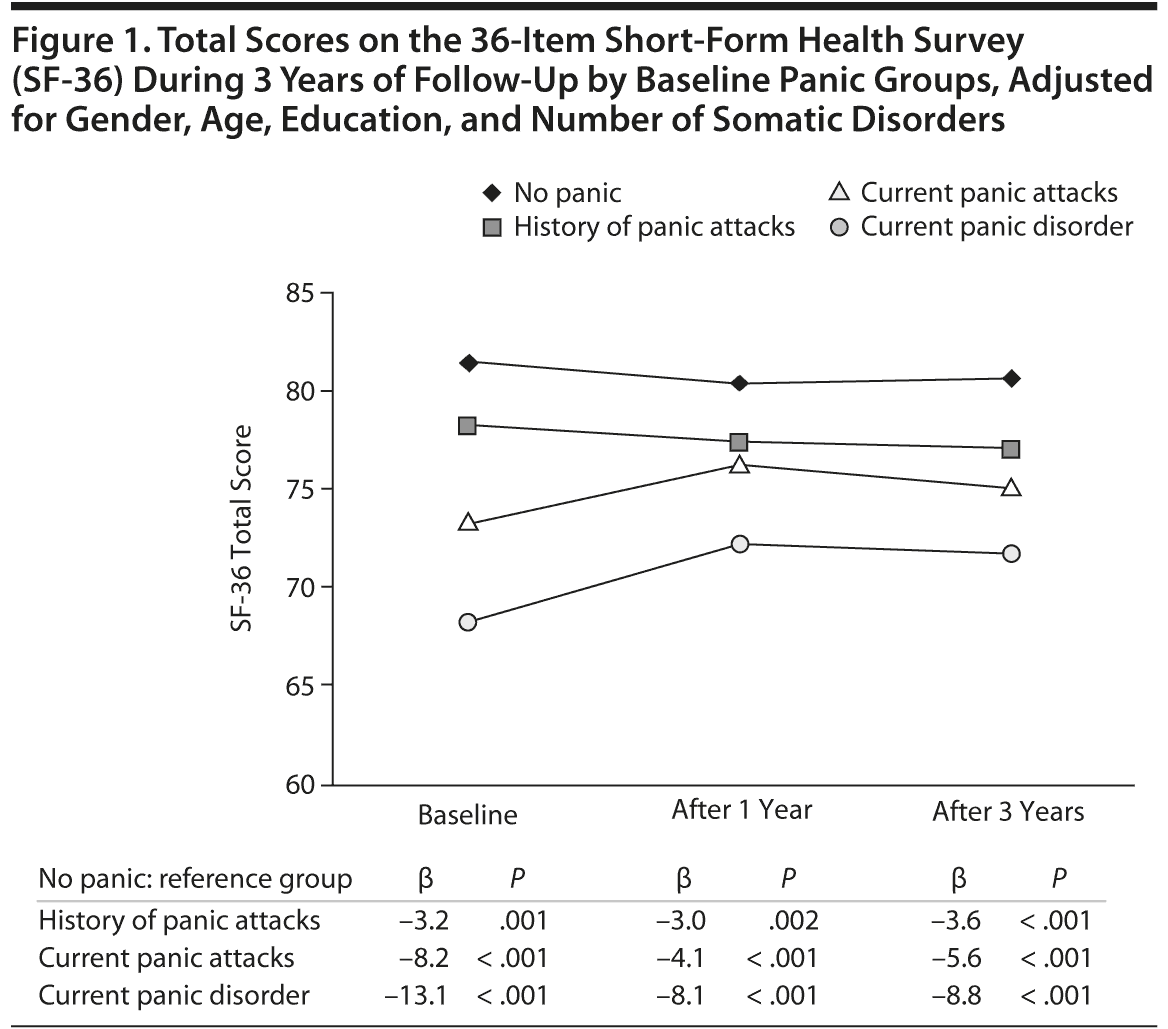
Subjects with panic had significantly lower levels of functioning compared to those without panic during 3-year follow-up in analyses that were basically adjusted for sociodemographics and somatic illnesses (F = 69.67, P < .001) (Figure 1). At T0, the level of functioning was lowest for PD (β = −13.1; P < .001), followed by PA (β = −8.2; P < .001) and HisPA (β = −3.2; P = .001) (NoPan = reference). Also at other timepoints, the level of functioning of all panic groups was significantly lower than that of NoPan. A post hoc analysis revealed that a lower level of functioning in panic groups applied for both mental functioning (F = 93.13; P < .001) and physical functioning (F = 21.59; P < .001) subdomains.
During the first year of follow-up, the level of functioning of both PD and PA improved significantly more compared to NoPan, as is indicated by significant interaction with time (PD ×— time: t = 4.65, P < .001; PA ×— time: t = 3.39, P = .001). HisPA subjects did not show any significant improvement of functioning during the first year of follow-up. Results are similar for the 3-year follow-up (PD ×— time: t = 3.72, P < .001; PA ×— time: t = 2.05, P = .04; HisPA ×— time = NS). Between T1 and T2, interaction with time was not significant, indicating that most improvement occurred during the first year of follow-up.
Additionally adjusting for comorbid mental disorders at baseline reduced beta values, but functioning remained significantly lower in all panic groups and at all timepoints compared to those without panic (F = 30.80; P < .001), and again this applied to both mental (F = 43.20; P < .001) and physical (F = 8.34; P < .001) subdomains (results not shown).
DISCUSSION
With the DSM-5 forthcoming, the nosologic status of panic attacks has gained renewed interest. In earlier times, Freud reckoned the central position of anxiety symptoms within the full range of psychopathology.37 This view largely vanished with the introduction of DSM-III,38 in which several anxiety disorders were defined and panic attacks were described within the panic disorder section. In DSM-IV,39 the cross-cutting feature of panic attacks was partly recovered, and panic attacks were positioned outside the panic disorder section, calling attention to the finding that panic attacks may occur in association with any anxiety disorder.40,41 Taking this repositioning one step further, for DSM-5 it has been proposed that panic attacks may be a valuable specifier or dimensional rating across all mental disorders.1,2 The present study was conducted because several quite elementary aspects needed empirical testing.
By demonstrating that panic is associated with high levels of comorbid psychiatric disorders across the diagnostic spectrum, with prevalence rates increasing with each level of panic, our results are consistent with and extend prior cross-sectional findings.3,4,6,10,11
Although the impact of panic on onset of psychopathology has been demonstrated previously,12-17 clarification was needed with regard to (1) the impact of panic attacks versus panic disorder and (2) the impact of a history of panic attacks versus current panic attacks. With regard to the first, Kinley et al17 demonstrated the impact of both panic attacks and panic disorder on onset of future psychopathology in a large, longitudinal population-based study (N = 34,653). They reported only very minor differences between panic attacks and panic disorder in predicting psychopathology. Risk estimates in our study were somewhat higher in those with panic disorder compared to panic attacks. With regard to comparing a history of panic attacks and of current panic attacks, previous research is inconsistent. Whereas Kessler et al16 suggested, on the basis of cross-sectional data, that persons with a history of panic attacks are at equal risk of a subsequent depression as persons with current panic attacks, Baillie and Rapee12 found a stronger association between 12-month panic attacks and depressive disorders (as well as anxiety disorders and substance use disorders) versus a history of panic attacks. The consistent findings of higher hazard ratios for current panic attacks versus a history of panic attacks in the present study clearly support the latter.
Previous studies examining the association of panic and persistence of psychiatric disorders are sparse.19 The present study provides evidence for an association between panic attacks and the persistence of a broad range of psychopathology.
Results on level of functioning underscore the detrimental effect of panic attacks on daily life by demonstrating that all panic groups had lower levels of functioning. It should be noted that even those with a history of panic attacks had significantly lower levels of functioning compared to those without panic. Our results are thereby in line with previous cross-sectional studies indicating the impact of panic attacks on functioning.3,6,7 Effects on functioning were larger for panic disorder compared to panic attacks, which is also in line with previous research.3,6 Results of the present study extend previous findings by showing that the lower level of functioning persisted over a 3-year follow-up. Moreover, whereas literature so far has focused on current panic attacks7 or on lifetime panic attacks without differentiating between current and past panic attacks,6 data from the present study suggested a larger impact of current panic attacks versus a history of panic attacks.
Associations could not be explained by sociodemographics and somatic disorders. As could be expected, current (comorbid) mental disorders had impact on onset and persistence of mental disorders and on level of functioning. However, it should be noted that even when the analyses were additionally adjusted for current mental disorders, the impact of panic attacks on onset, persistence, and level of functioning remained largely present.
Strengths and Limitations
Data were derived from a large and methodologically sound general population study with a longitudinal design, allowing examination of onset, persistence, and level of functioning over a 3-year period. Moreover, the data allowed the investigation of panic attacks outside the realm of panic disorder and the investigation of a history of panic attacks separate from current panic attacks. The results should be interpreted within the context of the following limitations. First, criteria for panic were derived from DSM-III-R.29 In DSM-III-R,29 panic attacks were not described separately but integrated within the criteria of panic disorder. As a result, onset of a panic attack was restricted to a “sudden onset” in our study, whereas in DSM-IV39 a crescendo criterion was also required to fulfill criteria of a panic attack. However, it is likely that using a more strict definition of a panic attack (ie, including the crescendo criterion) would only further strengthen associations between panic attacks and psychopathology.
Second, data did not allow the distinction between situationally bound panic attacks, situationally predisposed panic attacks, and spontaneous attacks. Thus, panic attacks occurring in the context of a phobic stimulus in an individual with an anxiety disorder could not be distinguished from unexpected panic attacks. This should be noted, because it can be hypothesized that only unexpected panic attacks have predictive value for course trajectories, and that anxiety responses to phobic stimuli or situations do not. However, if so, exclusion of situationally bound and predisposed panic attacks would further strengthen our findings.
Third, the total sample of the present study was large. As a result, statistical power was sufficient in most analyses. However, for specific subsamples and specific outcomes (especially regarding alcohol disorders), sample sizes were smaller, resulting in wider confidence intervals in these analyses. In these analyses, nonsignificant findings may therefore reflect insufficient statistical power, since it is important to note that risk estimates were generally increased in these smaller subgroups.
Fourth, given that part of our sample had only 1 follow-up assessment, the onset and persistence rates of disorders may be underestimated. Differential bias across panic groups is not likely, because attrition was not associated with any of the panic groups.
Fifth, the prospective associations between panic attacks and psychopathology shown in this study are useful in clinical practice. However, the reported associations may not be causal; that is, the possibility that panic attacks represent an underlying construct that causes the associations cannot be ruled out. Given that the construct of anxiety sensitivity is associated with panic attacks,42-44 it would have been worthwhile to assess anxiety sensitivity and adjust analyses for anxiety sensitivity. This was not possible, as the construct of anxiety sensitivity was not assessed in NEMESIS.
Sixth, posttraumatic stress disorder (PTSD) has not been assessed in NEMESIS. Including PTSD would have been interesting, given that in PTSD the occurrence of panic attacks is common and associated with adverse consequences.45
CONCLUSION
Given the consistent impact of panic attacks, and to a lesser extent a history of panic attacks, on various aspects of psychopathology, dimensionally rating panic attacks across mental disorders may be of great value for clinical care. Further work is needed to unravel the nature of the association between panic attacks and psychopathology and to examine beneficial effects of treating panic attacks.
Disclosure of off-label usage: The authors have determined that, to the best of their knowledge, no investigational information about pharmaceutical agents that is outside US Food and Drug Administration-approved labeling has been presented in this article.
Author affiliations: Department of Psychiatry and EMGO Institute, VU University Medical Center Amsterdam and GGZ inGeest, Amsterdam (Drs Batelaan, Rhebergen, Beekman, and Penninx); Netherlands Institute of Mental Health and Addiction, Utrecht (Drs de Graaf and Spijker); and Propersona, Ede (Dr Spijker), the Netherlands.
Financial disclosure: Dr Batelaan received speakers honoraria from Lundbeck. Dr Spijker received speakers honoraria from Eli Lilly, Lundbeck, AstraZeneca, GlaxoSmithKline, and Servier. Dr Beekman received grants from Eli Lilly, Shire, Janssen, and AstraZeneca and speakers honoraria from Eli Lilly and Lundbeck. Drs Rhebergen, de Graaf, and Penninx have no personal affiliations or financial relationships with any commercial interest to disclose relative to the article.
Funding/support: None reported.
Additional information: The NEMESIS database is owned by the Netherlands Institute of Mental Health and Addiction, Utrecht, the Netherlands. For information on accessing the database, contact Ron de Graaf ([email protected]) or Margreet ten Have ([email protected]).
REFERENCES
1. Craske MG, Kircanski K, Epstein A, et al; Posttraumatic and Dissociative Disorder Work Group. Panic disorder: a review of DSM-IV panic disorder and proposals for DSM-V. Depress Anxiety. 2010;27(2):93-112. PubMed doi:10.1002/da.20654
2. American Psychiatric Association. Panic attack: proposed revision. http://www.dsm5.org/ProposedRevision/Pages/proposedrevision.aspx?rid=404. Accessed Jan 12, 2012
3. Batelaan N, De Graaf R, Van Balkom A, et al. Thresholds for health and thresholds for illness: panic disorder versus subthreshold panic disorder. Psychol Med. 2007;37(2):247-256. PubMed doi:10.1017/S0033291706009007
4. Bystritsky A, Kerwin L, Niv N, et al. Clinical and subthreshold panic disorder. Depress Anxiety. 2010;27(4):381-389. PubMed doi:10.1002/da.20622
5. Eaton WW, Kessler RC, Wittchen HU, et al. Panic and panic disorder in the United States. Am J Psychiatry. 1994;151(3):413-420. PubMed
6. Kessler RC, Chiu WT, Jin R, et al. The epidemiology of panic attacks, panic disorder, and agoraphobia in the National Comorbidity Survey Replication. Arch Gen Psychiatry. 2006;63(4):415-424. PubMed doi:10.1001/archpsyc.63.4.415
7. Kinley DJ, Cox BJ, Clara I, et al. Panic attacks and their relation to psychological and physical functioning in Canadians: results from a nationally representative sample. Can J Psychiatry. 2009;54(2):113-122. PubMed
8. Reed V, Wittchen HU. DSM-IV panic attacks and panic disorder in a community sample of adolescents and young adults: how specific are panic attacks? J Psychiatr Res. 1998;32(6):335-345. PubMed doi:10.1016/S0022-3956(98)00014-4
9. Wittchen HU. Epidemiology of panic attacks and panic disorders. In: Hand I, Wittchen HU, eds. Panic and Phobias: Empirical Evidence of Theoretical Models and Longterm Effects of Behavioral Treatments. Berlin, Germany: Springer; 1986:18-28. doi:10.1007/978-3-642-71165-7_3
10. Goodwin R, Lyons JS, McNally RJ. Panic attacks in schizophrenia. Schizophr Res. 2002;58(2-3):213-220. PubMed doi:10.1016/S0920-9964(01)00373-5
11. Merikangas KR, Akiskal HS, Angst J, et al. Lifetime and 12-month prevalence of bipolar spectrum disorder in the National Comorbidity Survey Replication. Arch Gen Psychiatry. 2007;64(5):543-552. PubMed doi:10.1001/archpsyc.64.5.543
12. Baillie AJ, Rapee RM. Panic attacks as risk markers for mental disorders. Soc Psychiatry Psychiatr Epidemiol. 2005;40(3):240-244. PubMed doi:10.1007/s00127-005-0892-3
13. Batelaan NM, Smit F, de Graaf R, et al. Identifying target groups for the prevention of anxiety disorders in the general population. Acta Psychiatr Scand. 2010;122(1):56-65. PubMed doi:10.1111/j.1600-0447.2009.01488.x
14. Goodwin RD, Lieb R, Hoefler M, et al. Panic attack as a risk factor for severe psychopathology. Am J Psychiatry. 2004;161(12):2207-2214. PubMed doi:10.1176/appi.ajp.161.12.2207
15. Goodwin RD, Fergusson DM, Horwood LJ. Panic attacks and the risk of depression among young adults in the community. Psychother Psychosom. 2004;73(3):158-165. PubMed doi:10.1159/000076453
16. Kessler RC, Stang PE, Wittchen HU, et al. Lifetime panic-depression comorbidity in the National Comorbidity Survey. Arch Gen Psychiatry. 1998;55(9):801-808. PubMed doi:10.1001/archpsyc.55.9.801
17. Kinley DJ, Walker JR, Enns MW, et al. Panic attacks as a risk for later psychopathology: results from a nationally representative survey. Depress Anxiety. 2011;28(5):412-419. PubMed doi:10.1002/da.20809
18. Coryell W, Fiedorowicz JG, Solomon D, et al. Effects of anxiety on the long-term course of depressive disorders. Br J Psychiatry. 2012;200(3):210-215. PubMed
19. Frank E, Cyranowski JM, Rucci P, et al. Clinical significance of lifetime panic spectrum symptoms in the treatment of patients with bipolar I disorder. Arch Gen Psychiatry. 2002;59(10):905-911. PubMed doi:10.1001/archpsyc.59.10.905
20. Bijl RV, van Zessen G, Ravelli A, et al. The Netherlands Mental Health Survey and Incidence Study (NEMESIS): objectives and design. Soc Psychiatry Psychiatr Epidemiol. 1998;33(12):581-586. PubMed doi:10.1007/s001270050097
21. van de Berg J, van de Bos GAM. Het (meten van het) voorkomen van chronische aandoeningen 1974-1987. Mndber Gezondheid. 1989;8:4-21.
22. de Graaf R, ten Have M, van Gool C, et al. Prevalence of mental disorders and trends from 1996 to 2009: results from the Netherlands Mental Health Survey and Incidence Study-2. Soc Psychiatry Psychiatr Epidemiol. 2012;47(2):203-213. PubMed doi:10.1007/s00127-010-0334-8
23. Penninx BW, Beekman AT, Smit JH, et al; NESDA Research Consortium. The Netherlands Study of Depression and Anxiety (NESDA): rationale, objectives and methods. Int J Methods Psychiatr Res. 2008;17(3):121-140. PubMed doi:10.1002/mpr.256
24. Baker MM, Stabile M, Deri C. What Do Self-Reported, Objective Measures of Health Measure? Cambridge, UK: National Bureau of Economic Research; 2001.
25. Knight M, Stewart-Brown S, Fletcher L. Estimating health needs: the impact of a checklist of conditions and quality of life measurement on health information derived from community surveys. J Public Health Med. 2001;23(3):179-186. PubMed doi:10.1093/pubmed/23.3.179
26. National Center for Health Statistics. Vital and Health Statistics. Evaluation of National Health Interview Survey Diagnostic Reporting. Series 2: Data Evaluation and Methods Research, no 120. Hyattsville, Maryland: Department of Health and Human Services; 1994.
27. World Health Organization. Composite International Diagnostic Interview (CIDI), version 1.0. Geneva, Switzerland: World Health Organization; 1990.
28. Smeets RMW, Dingemans PMAJ. Composite International Diagnostic Interview (CIDI), version 1.1. Amsterdam, The Netherlands: World Health Organization; 1993.
29. American Psychiatric Association. Diagnostic and Statistical Manual of Mental Disorders, Third Edition, Revised. Washington, DC: American Psychiatric Association; 1987.
30. Wittchen HU. Reliability and validity studies of the WHO—Composite International Diagnostic Interview (CIDI): a critical review. J Psychiatr Res. 1994;28(1):57-84. PubMed doi:10.1016/0022-3956(94)90036-1
31. Ware JE Jr, Sherbourne CD. The MOS 36-Item Short-Form Health Survey (SF-36), 1:conceptual framework and item selection. Med Care. 1992;30(6):473-483. PubMed doi:10.1097/00005650-199206000-00002
32. Aaronson NK, Muller M, Cohen PD, et al. Translation, validation, and norming of the Dutch language version of the SF-36 Health Survey in community and chronic disease populations. J Clin Epidemiol. 1998;51(11):1055-1068. PubMed doi:10.1016/S0895-4356(98)00097-3
33. Burke JD, Burke KC, Baker JH, et al. Test-retest reliability in psychiatric patients of the SF-36 Health Survey. Int J Methods Psychiatr Res. 1995;5(3):189-194.
34. McHorney CA, Ware JE Jr, Raczek AE. The MOS 36-Item Short-Form Health Survey (SF-36), 2: psychometric and clinical tests of validity in measuring physical and mental health constructs. Med Care. 1993;31(3):247-263. PubMed doi:10.1097/00005650-199303000-00006
35. McHorney CA, Ware JE Jr, Lu JF, et al. The MOS 36-Item Short-Form Health Survey (SF-36), 3: tests of data quality, scaling assumptions, and reliability across diverse patient groups. Med Care. 1994;32(1):40-66. PubMed doi:10.1097/00005650-199401000-00004
36. SPSS. SPSS for Windows: Version 15. Chicago, IL: SPSS; 2006.
37. Freud S. Werken. Oranje W (trans). Amsterdam, Netherlands: Boom; 2006.
38. American Psychiatric Association. Diagnostic and Statistical Manual of Mental Disorders, Third Edition. Washington, DC: American Psychiatric Association; 1980.
39. American Psychiatric Association. Diagnostic and Statistical Manual of Mental Disorders, Fourth Edition. Washington, DC: American Psychiatric Association; 1994.
40. Liebowitz MR. Section III: anxiety disorders. DSM-IV Sourcebook, vol 2. 1st ed. Washington, DC: American Psychiatric Association; 1996:397-410.
41. Shear MK, Bjelland I, Beesdo K, et al. Supplementary dimensional assessment in anxiety disorders. Int J Methods Psychiatr Res. 2007;16(suppl 1):S52-S64. PubMed doi:10.1002/mpr.215
42. Ben×tez CI, Shea MT, Raffa S, et al. Anxiety sensitivity as a predictor of the clinical course of panic disorder: a 1-year follow-up study. Depress Anxiety. 2009;26(4):335-342. PubMed doi:10.1002/da.20423
43. Schmidt NB, Zvolensky MJ, Maner JK. Anxiety sensitivity: prospective prediction of panic attacks and Axis I pathology. J Psychiatr Res. 2006;40(8):691-699. PubMed doi:10.1016/j.jpsychires.2006.07.009
44. Zvolensky MJ, Schmidt NB. Introduction to anxiety sensitivity: recent findings and new directions. Behav Modif. 2007;31(2):139-144. PubMed doi:10.1177/0145445506296968
45. Cougle JR, Feldner MT, Keough ME, et al. Comorbid panic attacks among individuals with posttraumatic stress disorder: associations with traumatic event exposure history, symptoms, and impairment. J Anxiety Disord. 2010;24(2):183-188. PubMed doi:10.1016/j.janxdis.2009.10.006
This PDF is free for all visitors!