Objective: This study assessed mental and health functioning in full versus partial posttraumatic stress disorder (PTSD) among newly returning veterans from Iraq (Operation Iraqi Freedom [OIF]) and Afghanistan (Operation Enduring Freedom [OEF]) who were referred by primary care providers for a behavioral health assessment and reported an emotional trauma.
Method: Participants included OEF/OIF veterans receiving care in 2 veterans’ affairs medical centers and affiliated community-based outpatient clinics who reported behavioral health issues to their primary care providers. All veterans underwent a clinical behavioral health assessment of Axis I disorders and functioning via telephone between June 2007 and April 2008. Functioning was measured using the 12-item Short-Form Health Survey (SF-12). Those reporting a previous emotional trauma were subsequently assessed for PTSD using the PTSD Patient Checklist (PCL).
Results: The final sample (N = 201) was 88.1% male with a mean age of 34.2 years (SD = 10.1). Individuals with full PTSD (n = 120, 59.7%) reported worse mental health functioning compared to those with partial PTSD (n = 37, 18.4%). Individuals with partial PTSD reported worse mental health functioning scores than the trauma exposed-only group (n = 44, 21.9%). Compared to national norms, patients with partial PTSD reported mental health functioning scores that were worse than 75% of individuals within a similar age range. After controlling for other psychiatric factors, there was no difference between partial PTSD and the trauma-only group.
Conclusion: OEF/OIF veterans with partial PTSD referred for a behavioral health assessment may incur significant problems with functioning. These complaints may be better attributed to psychiatric comorbidity as opposed to symptoms specifically related to trauma.
Submitted: April 6, 2009; accepted August 4, 2009.
Published online: May 27, 2010.
Corresponding author: Les A. Gellis, PhD, Philadelphia Veterans Medical Center, MIRECC (116, 2nd floor), University & Woodland Avenues, Philadelphia, PA 19104 ([email protected]).
Functional Quality of Life in Full Versus Partial
Posttraumatic Stress Disorder Among Veterans
Returning From Iraq and Afghanistan
Objective: This study assessed mental and health functioning in full versus partial posttraumatic stress disorder (PTSD) among newly returning veterans from Iraq (Operation Iraqi Freedom [OIF]) and Afghanistan (Operation Enduring Freedom [OEF]) who were referred by primary care providers for a behavioral health assessment and reported an emotional trauma.
Method: Participants included OEF/OIF veterans receiving care in 2 veterans’ affairs medical centers and affiliated community-based outpatient clinics who reported behavioral health issues to their primary care providers. All veterans underwent a clinical behavioral health assessment of Axis I disorders and functioning via telephone between June 2007 and April 2008. Functioning was measured using the 12-item Short-Form Health Survey (SF-12). Those reporting a previous emotional trauma were subsequently assessed for PTSD using the PTSD Patient Checklist (PCL).
Results: The final sample (N = 201) was 88.1% male with a mean age of 34.2 years (SD = 10.1). Individuals with full PTSD (n = 120, 59.7%) reported worse mental health functioning compared to those with partial PTSD (n = 37, 18.4%). Individuals with partial PTSD reported worse mental health functioning scores than the trauma exposed–only group (n = 44, 21.9%). Compared to national norms, patients with partial PTSD reported mental health functioning scores that were worse than 75% of individuals within a similar age range. After controlling for other psychiatric factors, there was no difference between partial PTSD and the trauma-only group.
Conclusion: OEF/OIF veterans with partial PTSD referred for a behavioral health assessment may incur significant problems with functioning. These complaints may be better attributed to psychiatric comorbidity as opposed to symptoms specifically related to trauma.
Prim Care Companion J Clin Psychiatry 2010;12(3):e1–e6
© Copyright 2010 Physicians Postgraduate Press, Inc.
Submitted: April 6, 2009; accepted August 4, 2009.
Published online: May 27, 2010 (doi:10.4088/PCC.09m00823blu).
Corresponding author: Les A. Gellis, PhD, Philadelphia Veterans Medical Center, MIRECC (116, 2nd floor), University & Woodland Avenues, Philadelphia, PA 19104 ([email protected]).
Recent studies have shown that a significant number of veterans returning from conflicts in Iraq (Operation Iraqi Freedom [OIF]) and Afghanistan (Operation Enduring Freedom [OEF]) are struggling with recovery from trauma.1,2,3 While posttraumatic stress disorder (PTSD) has traditionally been diagnosed using Axis I criteria, understanding the impact of trauma in OEF/OIF veterans may also require an analysis of subdromal or partial PTSD, which is characterized by a constellation of PTSD symptoms without meeting full criteria for the disorder. In light of the fact that reactions to extreme stress may exist on a dimensional scale,4 it is possible that individuals on the border of meeting criteria for a formal diagnosis of PTSD (ie, partial PTSD) may be in need of mental health treatment. Community-based studies and investigations from clinical populations have documented rates of partial PTSD ranging from 50% to approximately 3 times that of full PTSD.5–8 Thus, focusing only on individuals with the full diagnosis of PTSD may significantly underestimate the number of newly returning veterans who may be in need of care.
In order to assess whether those with partial PTSD indeed exhibit meaningful symptoms that may require or warrant clinical care, a number of studies have compared functioning differences between those with partial and full PTSD. These investigations have generally revealed greater disability in individuals with full PTSD as compared to those with partial PTSD, who in turn, report greater disability than trauma-only groups who experienced a trauma with few or no symptoms.6–9 The extent of the disparities between groups, however, has been mixed, suggesting that the disability associated with partial PTSD requires greater clarification. Further, only 1 other study has assessed for functional problems in partial PTSD among veterans. In this study, Grubaugh et al9 compared older veterans (mean age = 61.4 years) with various symptom levels of PTSD on the Medical Outcomes Study 36-item Short-Form Health Survey,10 which can be used to compare disability to a healthy national sample. Although scores for partial PTSD were significantly worse than those of a trauma-only comparison group after controlling for depression, these scores were in fact better than the national average.9 This suggests that the partial PTSD among veterans did not necessarily show significant impairment. However, this study included older veterans who experienced trauma many years prior to their participation in the study. Consequently, these findings may not be representative of current OEF/OIF veterans.9 Also, because depression shares multiple symptoms with PTSD and may be subject to the same effects of trauma,11 it is possible that controlling for depression minimized the observed association between trauma/PTSD and functioning.9
In order to build upon prior work and address the relationship between functioning and partial/full PTSD diagnoses specifically among newly returning veterans, the current study compared mental and physical functioning among OEF/OIF veterans who were referred by primary care for a behavioral health assessment and reported an emotional trauma. We used a standardized measure of functioning that can be compared to national norms and assessed functioning both with and without accounting for other psychiatric factors. PTSD is consistently associated with increased disability,12–15 and it is expected that OEF/OIF veterans with PTSD will also report greater functional problems as compared to a trauma-only group who experience no or few symptoms of PTSD. If individuals with partial PTSD show functioning complaints similar to that of full PTSD, it will provide evidence that their clinical symptoms may warrant greater attention and may indicate that these individuals should be offered psychosocial and psychiatric treatment similar to those with the full disorder.
METHOD
Sample and Procedures
This project was reviewed and approved by the Philadelphia Veterans Affairs Medical Center Institutional Review Board. The sample included OEF/OIF veterans receiving primary care in the Philadelphia and Lebanon Veterans Affairs Medical Centers (Philadelphia and Lebanon, Pennsylvania, respectively) and affiliated community-based outpatient clinics. All participants were assessed by the Behavioral Health Laboratory (BHL), an evidence-based, clinical management program that focuses on the identification, screening, assessment, and triage of primary care patients who may be in need of care for behavioral health issues such as depression, anxiety, alcohol misuse, and PTSD. An overview of the procedures and components of the BHL are described in detail elsewhere16 and briefly outlined below.
Patients were identified by the BHL through 3 main mechanisms: (1) referral of the patient to the BHL following a positive screen for PTSD, alcohol misuse, and/or depression in primary care; (2) providers’ referral of patients to the BHL for assessment independent of screening and on the basis of clinical judgment; or (3) after initiation of an antidepressant. Upon receipt of patient names, BHL health technicians contacted patients by telephone and conducted an initial 20- to 30-minute behavioral health screening assessment covering Axis I psychiatric disorders, sociodemographic characteristics, and functioning.
Data for the current set of analyses were extracted from the parent BHL clinical sample. Participants were selected according to the following criteria: (1) completion of the initial screening interview from June 2007 to April 2008, (2) serving in the Iraqi or Afghanistan conflicts, and (3) reporting having experienced an event that was “unusually or especially frightening, horrible, or traumatic.” Patients reporting a traumatic event were subsequently assessed for PTSD. There were 2,023 completed interviews from the above time period, which included 245 OEF/OIF veterans. Of the 245 veterans, 201 (82.0%) recalled a traumatic event. The final sample included 201 participants. Table 1 presents a summary of the sociodemographic characteristics of the study sample.

Measures
MINI-International Neuropsychiatric Interview. The MINI-International Neuropsychiatric Interview (MINI)17 is a valid and reliable structured diagnostic instrument that assesses the presence of DSM-IV diagnoses. The MINI was used to assess for a psychotic disorder, panic disorder, alcohol abuse/dependence, and bipolar disorder.
Patient Health Questionnaire-9. The Patient Health Questionnaire-9 (PHQ-9)18 is a valid measure of depression severity. Patients reported how often they experienced each of the 9 symptoms for a major depressive episode (0 = not at all, 3 = nearly every day) during the previous 2 weeks. The scale was used as a continuous variable (total summed score; range, 0–27) in analyses.
PTSD Patient Checklist. The PTSD Patient Checklist (PCL)19 was used to assess for PTSD. The PCL is a standardized rating scale for PTSD that measures the extent to which individuals are bothered in the past month by the 17 PTSD symptoms on a 5-point ordinal scale ranging from “not at all” to “extremely.” Several studies have demonstrated the reliability and validity of the PCL.20,21
On the basis of scores from the PCL, participants were assigned to 1 of 3 groups: (1) full PTSD, (2) partial PTSD, and (3) trauma exposure only. Those in the full PTSD group reported being at least “moderately bothered” by at least 1 item from the “reexperiencing” category, 3 items on the “avoidance or numbing” category, and 2 items from the “hyperarousal” category. The definition of partial PTSD for the purposes of this study was based on the criteria as described by Blanchard et al5 and used by Grubaugh et al.9 We adapted this definition using the PCL, and these criteria were chosen to allow for comparisons across studies. Veterans in the partial PTSD group reported being at least moderately bothered by no less than 1 item from the reexperiencing category and either 3 items from criterion C or 2 items from criterion D. All other individuals were assigned to the trauma exposure–only group.
Mental and physical functioning. Functional ability was assessed with the 12-item Short-Form Health Survey (SF-12) from the Medical Outcomes Study,22 a widely used standardized measure of functional status. The SF-12 has a mean of 50 and standard deviation of 10, with lower scores indicating worse functioning. Two composite scores, the mental component score (MCS) and physical component score (PCS), were generated. Scores from the SF-12 were evaluated against norms from the SF-36,23 and these 2 measures offer highly reliable comparisons.24,25 The SF-12 has been shown to be a useful measure of disability in those with anxiety disorders.26
Sociodemographic and background factors. Age, gender, race, income, and traumatic brain injury were assessed during the BHL interview. To assess for traumatic brain injury, individuals were asked if they had ever experienced a significant head injury and whether this injury led to a loss of consciousness. They were also asked to report the length of time they were unconscious (< 20 minutes, 20 minutes to 1 hour, or > 1 hour). Because few participants reported experiencing a loss of consciousness greater than 20 minutes (n = 10), we did not have the necessary power to classify participants according to mild, moderate, and severe traumatic brain injury, and participants were categorized into 1 of 2 groups. One group included individuals with a significant head injury who lost consciousness, and the other group included individuals who did not have a significant head injury or did not lose consciousness from any injury.
Data Analyses
Statistical analyses were performed using SPSS, version 15 (SPSS Inc, Chicago, Illinois). Bivariate tests of significance included analysis of variance assessing for the equality of means for continuous outcomes and χ2 tests for dichotomous outcomes. These bivariate tests were used to determine the covariates to be used in a multivariate model, and variables meeting a criterion of P < .05 were retained in multivariate analyses. Analysis of variance with Tukey post hoc testing was used to compare MCS and PCS scores across the 3 PTSD groups. A 1-way analysis of covariance (ANCOVA) with least significant difference post hoc testing was conducted to compare mental health functioning by PTSD group after controlling for demographic variables and other psychiatric factors.
RESULTS
Demographic and Behavioral Health Characteristics by PTSD Group
The final sample (N = 201) included 120 (59.7%) individuals with full PTSD, 37 (18.4%) individuals with partial PTSD, and 44 (21.9%)individuals reporting a trauma with few or no symptoms of PTSD. Participants were mostly male (88.1%) and white (58.2%) and had a mean age of 34.2 years (SD = 10.1). Table 1 provides comparisons of demographics and psychiatric characteristics by PTSD group. With respect to health and sociodemographic/background characteristics, analyses revealed no significant differences between PTSD groups on age, gender, financial situation, traumatic brain injury, or current psychosis. Panic disorder (χ22 = 7.5, P = .023), bipolar disorder (χ22 = 10.3, P = .006), and race (χ22 = 14.1, P = .001) were related to PTSD group. Depression severity (PHQ-9 total score) also differed by PTSD group (F2,198 = 25.9, P < .001). Individuals with full PTSD reported greater depression severity than those with partial PTSD, who showed greater depression severity than the trauma-only group.
PTSD Group Differences in Mental
and Physical Health Functioning
Mental health functioning (MCS) differed by PTSD group (F2,198 = 39.3, P < .001) (Table 2 provides MCS scores by PTSD group). Post hoc testing revealed that OEF/OIF veterans with full PTSD reported significantly worse MCS scores as compared to those with partial PTSD (P < .001). Further, individuals with partial PTSD reported significantly worse MCS scores than the trauma exposed–only group (P < .018). There were no differences among PTSD groups in regard to physical health functioning.
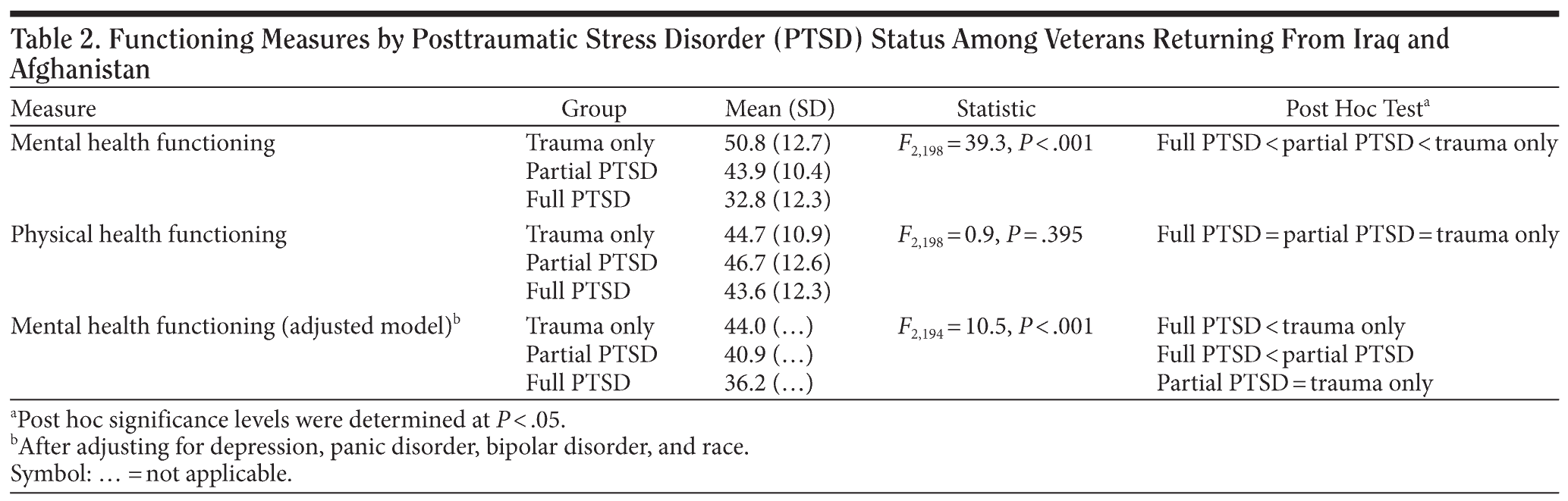
Depression severity (r = –0.76, P < .001), panic disorder (F1,199 = 14.2, P < .001), bipolar disorder (F1,199 = 8.0, P = .005), and race (F1,199 = 12.3, P = .001) were related to MCS. Given that these variables could potentially confound the relationship between PTSD group and mental health functioning, we adjusted for them in a multivariate ANCOVA model. Post hoc testing showed that after controlling for these factors, MCS scores for full PTSD remained significantly worse than partial PTSD (P = .009) and trauma only (P < .001), and partial PTSD was no longer significantly greater than the trauma exposed–only group (P = .074).
Functioning Status of PTSD Groups in Relation to National Norms
In the national sample, the median mental health functioning score for individuals aged 24–34 years was 51.88.23 To put this score in perspective, the 25th percentile comprised a score of 45.09. In our sample of OEF/OIF veterans referred for a behavioral health assessment, scores for partial PTSD were less than the scores for the 25th percentile. The relevance of these findings is further highlighted by the fact that a decrease in 3 points on the mental health component of the SF-36 is associated with a 13% greater likelihood of being unable to work, a 16% greater chance of 1-year job loss, and a 30% increased chance of using mental health services.
DISCUSSION
Findings from this investigation suggest that mental health functioning varies according to PTSD group among OEF/OIF veterans referred for a behavioral health assessment. Those meeting full criteria for the disorder report significantly worse functioning than those with partial PTSD, who in turn, report worse functioning than individuals reporting an emotional trauma with few or no symptoms. These findings are consistent with the majority of studies comparing functioning differences in full and partial PTSD.6–9
Psychiatric factors other than PTSD symptoms may partly explain the functioning differences between these groups. After accounting for other psychiatric factors and race, full PTSD continues to show significantly worse functioning as compared to all other groups; however, partial PTSD no longer shows worse functioning than the trauma-only group. This finding suggests that psychiatric comorbidity accounts for a portion of the variability in functioning problems across patients with partial and full PTSD.
These nonsignificant differences between the partial PTSD and trauma-only groups conflict with the study by Grubaugh et al,9 which is the only other study we found that assessed partial PTSD among veterans. These discrepant findings may be explained by the lower functioning scores across the 3 groups in our study. Functioning status for both the trauma-only and partial PTSD groups were lower than the national average after adjusting for other factors. Thus, it may be important to consider functioning problems among all levels of PTSD severity in OEF/OIF veterans reporting an emotional trauma. There are unique circumstances associated with the cohort in this study that may increase disability. Newly returning veterans may potentially live with not only the apprehension of possible redeployment but also the anxiety and fear of having friends and colleagues currently at war.
There is no consensus on the definition of partial PTSD, and it is plausible that other criteria would have produced different results. For instance, this definition of partial PTSD requires a positive item on the reexperiencing category (criterion B). Those with a previous trauma, however, may engage in purposeful avoidance and may successfully prevent the reexperiencing of symptoms. Consequently, those with significant avoidance and hyperarousal symptoms may have been included in the trauma-only group, and these diagnostic criteria may have weakened differences between partial PTSD and the trauma-only group. PTSD is also commonly assessed using the total symptom severity score from the PCL as opposed to DSM-IV criteria. A score of 50 on the PCL has often been used as the ideal cutoff for assessing PTSD, though a recent review suggested that lower scores will better predict PTSD status in settings with a high prevalence of the disorder.27 Thus, it is plausible that veterans with true full PTSD in this sample were included in the partial PTSD group or even in the trauma-only group, which may have worsened functioning in those groups. Future investigations should assess how different criteria for partial PTSD are related to functioning.
Our findings reveal no differences in physical health functioning by PTSD group. These findings are inconsistent with Hoge et al,2 who showed worse physical health symptoms across a number of variables in newly returning veterans with PTSD as compared to those without PTSD. The divergent results may be explained by different methodology. Our sample was comprised of individuals presenting to primary care presumably because of a health-related problem. This sample bias may have increased pathology among all PTSD groups and minimized the differences between groups.
The individuals in this study were all referred from primary care for further assessment of behavioral health issues. Thus, the prevalence rates and functioning status of full and partial PTSD in this study cannot be generalized to the overall population of OEF/OIF veterans who were exposed to a trauma. This bias likely explains why rates of PTSD are considerably higher in this sample as compared to previous studies. This bias may also explain why there are particularly high rates of bipolar disorder in this sample. Because mood disorders and PTSD share a number of symptoms, it is possible that this additional psychopathology led to decreased functioning in those with PTSD. Because we are unable to pinpoint the primary diagnosis in these patients, it is unclear whether partial PTSD is indeed a meaningful clinical entity or whether the low functioning in this population is better attributed to other psychiatric factors.
The findings in this study should be considered along with the following limitations. First, we do not know when the particular trauma occurred for these participants, and much time may have passed between returning home and the experience of the emotional trauma(s). As a result, these data may not inform us of functioning problems that occur directly after a trauma. We also cannot be sure whether the individuals with partial PTSD instead had partial remission from full PTSD, which may have worsened functioning in this group. The chronicity of trauma-related symptoms may also influence functioning problems, and we cannot assess whether functioning problems in either group may be an artifact of the duration of problems as opposed to the severity of symptoms. We also do not know the number and type of traumas reported by the participants, and we cannot be clear whether these results generalize to any specific quality of trauma experiences.
Finally, our definition of traumatic brain injury is not validated, and we cannot be sure of the extent or accuracy of the problems related to traumatic brain injury in the population. A recent study found that focusing only on head injury may underestimate the prevalence of traumatic brain injury,28 and our definition excludes individuals who do not have a loss of consciousness yet may have incurred an event leading to a loss of memory or confusion and could be diagnosed with mild traumatic brain injury. Thus, it is possible that we have underestimated the extent of traumatic brain injury in this sample. Because traumatic brain injury is associated with mental and physical problems that could lead to worse functioning, it is possible that the degree of functioning problems were inappropriately attributed to the impact of trauma.
These results show that OEF/OIF veterans with partial PTSD may indeed be experiencing meaningful symptoms warranting care, although more studies are needed to confirm whether these problems can be attributed to trauma as opposed to other psychiatric factors. To assess this question, future studies should compare those individuals with partial PTSD to age-matched and sex-matched healthy controls who do not have a history of emotional trauma. Future studies should also further investigate the prevalence and levels of functioning in partial PTSD in newly returning veterans using a larger, more representative sample. Finally, future studies should also attempt to elucidate the relationship between the severity of functioning problems and the possible need for treatment to best identify and adequately treat individuals recovering from trauma.
Author affiliations: Philadelphia Veterans Affairs Medical Center and VISN 4 Mental Illness Research, Education, and Clinical Center, Philadelphia, Pennsylvania (Drs Gellis, Mavandadi, and Oslin).
Potential conflicts of interest: The authors report no financial or other affiliations relevant to the subject of this article.
Funding/support: This work was supported, in part, by a grant from the National Institute of Mental Health (K08MH01599 & P30 MH66270), National Institute of Alcohol Abuse and Alcoholism R01, Department of Veterans Affairs HSRD Investigator Initiated Research IIR 02-108, and the Mental Illness Research, Education, and Clinical Center at the Philadelphia Veterans Affairs Medical Center.
Previous presentation: Data were previously presented at the National Veterans Mental Health Conference; July 21–24, 2008; Washington, DC.
Acknowledgment: We would like to thank and acknowledge the many veterans of Operation Enduring Freedom and Operation Iraqi Freedom. We would also like to thank the staff of the Behavioral Health Laboratory and primary care providers at the Philadelphia Veterans Affairs Medical Center, Philadelphia, Pennsylvania.
REFERENCES
1. Hoge CW, Castro CA, Messer SC, et al. Combat duty in Iraq and Afghanistan, mental health problems, and barriers to care. N Engl J Med. 2004;351(1):13–22.doi:10.1056/NEJMoa040603 PubMed
2. Hoge CW, Terhakopian A, Castro CA, et al. Association of posttraumatic stress disorder with somatic symptoms, health care visits, and absenteeism among Iraq war veterans. Am J Psychiatry. 2007;164(1):150–153.doi:10.1176/appi.ajp.164.1.150 PubMed
3. Seal KH, Bertenthal D, Miner CR, et al. Bringing the war back home: mental health disorders among 103,788 US veterans returning from Iraq and Afghanistan seen at Department of Veterans Affairs facilities. Arch Intern Med. 2007;167(5):476–482.doi:10.1001/archinte.167.5.476 PubMed
4. Ruscio AM, Ruscio J, Keane TM. The latent structure of posttraumatic stress disorder: a taxometric investigation of reactions to extreme stress. J Abnorm Psychol. 2002;111(2):290–301.doi:10.1037/0021-843X.111.2.290 PubMed
5. Blanchard EB, Hickling EJ, Taylor AE, et al. Psychological morbidity associated with motor vehicle accidents. Behav Res Ther. 1994;32(3):283–290.doi:10.1016/0005-7967(94)90123-6 PubMed
6. Breslau N, Lucia VC, Davis GC. Partial PTSD versus full PTSD: an empirical examination of associated impairment. Psychol Med. 2004;34(7):1205–1214.doi:10.1017/S0033291704002594 PubMed
7. Stein MB, Walker JR, Hazen AL, et al. Full and partial posttraumatic stress disorder: findings from a community survey. Am J Psychiatry. 1997;154(8):1114–1119. PubMed
8. Zlotnick C, Franklin CL, Zimmerman M. Does “subthreshold” posttraumatic stress disorder have any clinical relevance? Compr Psychiatry. 2002;43(6):413–419.doi:10.1053/comp.2002.35900 PubMed
9. Grubaugh AL, Magruder KM, Waldrop AE, et al. Subthreshold PTSD in primary care: prevalence, psychiatric disorders, healthcare use, and functional status. J Nerv Ment Dis. 2005;193(10):658–664.doi:10.1097/01.nmd.0000180740.02644.ab PubMed
10. Ware JE Jr, Sherbourne CD. The MOS 36-item Short-Form Health Survey (SF-36), I: conceptual framework and item selection. Med Care. 1992;30(6):473–483.doi:10.1097/00005650-199206000-00002 PubMed
11. van der Kolk BA, Pelcovitz D, Roth S, et al. Dissociation, somatization, and affect dysregulation: the complexity of adaptation of trauma. Am J Psychiatry. 1996;153(suppl 7):83–93. PubMed
12. Magruder KM, Frueh BC, Knapp RG, et al. PTSD symptoms, demographic characteristics, and functional status among veterans treated in VA primary care clinics. J Trauma Stress. 2004;17(4):293–301.doi:10.1023/B:JOTS.0000038477.47249.c8 PubMed
13. Rapaport MH, Clary C, Fayyad R, et al. Quality-of-life impairment in depressive and anxiety disorders. Am J Psychiatry. 2005;162(6):1171–1178.doi:10.1176/appi.ajp.162.6.1171 PubMed
14. Zatzick DF, Marmar CR, Weiss DS, et al. Posttraumatic stress disorder and functioning and quality of life outcomes in a nationally representative sample of male Vietnam veterans. Am J Psychiatry. 1997;154(12):1690–1695. PubMed
15. Zayfert C, Dums AR, Ferguson RJ, et al. Health functioning impairments associated with posttraumatic stress disorder, anxiety disorders, and depression. J Nerv Ment Dis. 2002;190(4):233–240.doi:10.1097/00005053-200204000-00004 PubMed
16. Oslin DW, Ross J, Sayers S, et al. The Behavioral Health Laboratory: screening, assessment, and management of depression in VA primary care clinics. J Gen Intern Med. 2006;21(1):46–50.doi:10.1111/j.1525-1497.2005.0267.x PubMed
17. Sheehan DV, Lecrubier Y, Sheehan KH, et al. The Mini-International Neuropsychiatric Interview (MINI): the development and validation of a structured diagnostic psychiatric interview for DSM-IV and ICD-10. J Clin Psychiatry. 1998;59(suppl 20):22–33. PubMed
18. Kroenke K, Spitzer RL, Williams JB. The PHQ-9: validity of a brief depression severity measure. J Gen Intern Med. 2001;16(9):606–613.doi:10.1046/j.1525-1497.2001.016009606.x PubMed
19. Weathers FW, Ford J. Psychometric properties of the PTSD Checklist (PCL-C, PCL-S, PCL-M, PCL-PR). In: Stamm BH, ed. Measurement of Stress, Trauma, and Adaptation. Lutherville, MD: Sidran Foundation & Press; 1996:250–252.
20. Blanchard EB, Jones-Alexander J, Buckley TC, et al. Psychometric properties of the PTSD Checklist (PCL). Behav Res Ther. 1996;34(8):669–673.doi:10.1016/0005-7967(96)00033-2 PubMed
21. Ruggiero KJ, Del Ben K, Scotti JR, et al. Psychometric properties of the PTSD checklist-civilian version. J Trauma Stress. 2003;16(5):495–502.doi:10.1023/A:1025714729117 PubMed
22. Ware J Jr, Kosinski M, Keller SD. A 12-Item Short-Form Health Survey: construction of scales and preliminary tests of reliability and validity. Med Care. 1996;34(3):220–233.doi:10.1097/00005650-199603000-00003 PubMed
23. Ware JE Jr, Kosinski M, Bjorner JB, et al. User’s Manual for the SF-36v2 Health Survey. 2nd ed. Lincoln, RI: Quality Metric Incorporated; 2007.
24. Gandek B, Ware JE, Aaronson NK, et al. Cross-validation of item selection and scoring for the SF-12 Health Survey in nine countries: results from the IQOLA Project. International Quality of Life Assessment. J Clin Epidemiol. 1998;51(11):1171–1178.doi:10.1016/S0895-4356(98)00109-7 PubMed
25. Ware JE Jr, Gandek B, Kosinski M, et al. The equivalence of SF-36 summary health scores estimated using standard and country-specific algorithms in 10 countries: results from the IQOLA Project. International Quality of Life Assessment. J Clin Epidemiol. 1998;51(11):1167–1170.doi:10.1016/S0895-4356(98)00108-5 PubMed
26. Sanderson K, Andrews G, Jelsma W. Disability measurement in the anxiety disorders: comparison of three brief measures. J Anxiety Disord. 2001;15(4):333–344.doi:10.1016/S0887-6185(01)00067-6 PubMed
27. Terhakopian A, Sinaii N, Engel CC, et al. Estimating population prevalence of posttraumatic stress disorder: an example using the PTSD checklist. J Trauma Stess. 2008;21(3):290–300. PubMed
28. Schwab KA, Ivins B, Cramer G, et al. Screening for traumatic brain injury in troops returning from deployment in Afghanistan and Iraq: initial investigation of the usefulness of a short screening tool for traumatic brain injury. J Head Trauma Rehabil. 2007;22(6):377–389.doi:10.1097/01.HTR.0000300233.98242.87 PubMed
Enjoy this premium PDF as part of your membership benefits!


