Objective: Recent studies document posttraumatic stress disorder (PTSD) symptoms in women following at-term deliveries with healthy baby outcomes. However, the notion that childbirth can trigger PTSD remains controversial, and the symptom clusters are mostly unknown. The objective of this study was to examine the clustering of childbirth-induced postpartum PTSD (PP-PTSD) symptoms in comparison to DSM-5 clusters.
Methods: We examined the symptom presentation of childbirth-related postpartum PTSD (PP-PTSD) in a sample of 685 women. The majority of these women delivered at term. Peritraumatic stress reactions to childbirth and PP-PTSD symptoms were assessed approximately 3 months after delivery. A hierarchical cluster analysis was used to detect grouping of the PP-PTSD symptoms.
Results: Childbirth-related peritraumatic stress was strongly and positively associated with PP-PTSD symptom severity. Cluster modeling revealed 4 distinguished symptom groups: reliving (some reexperiencing symptoms), namely nightmares and flashbacks; avoidance coupled with unwanted memories (other reexperiencing symptoms); negative cognitions and mood; and hyperarousal reactivity.
Conclusions: Our findings show that the representation of symptoms of PTSD that develops following a stressogenic childbirth experience appears, for the most part, to resemble DSM-5 symptom clusters. More research integrating descriptive symptom assessment with biological measures is warranted to better characterize the symptom presentation of this neglected posttraumatic stress syndrome.
Examining Symptom Clusters of Childbirth-Related Posttraumatic Stress Disorder
ABSTRACT
Objective: Recent studies document posttraumatic stress disorder (PTSD) symptoms in women following at-term deliveries with health baby outcomes. However, the notion that childbirth can trigger PTSD remains controversial, and the symptom clusters are mostly unknown. The objective of this study was to examine the clustering of childbirth-induced postpartum PTSD (PP-PTSD) symptoms in comparison to DSM-5 clusters.
Methods: We examined the symptom presentation of childbirth-related postpartum PTSD (PP-PTSD) in a sample of 685 women. The majority of these women delivered at term. Peritraumatic stress reactions to childbirth and PP-PTSD symptoms were assessed approximately 3 months after delivery. A hierarchical cluster analysis was used to detect grouping of the PP-PTSD symptoms.
Results: Childbirth-related peritraumatic stress was strongly and positively associated with PP-PTSD symptom severity. Cluster modeling revealed 4 distinguished symptom groups: reliving (some reexperiencing symptoms), namely nightmares and flashbacks; avoidance coupled with unwanted memories (other reexperiencing symptoms); negative cognitions and mood; and hyperarousal reactivity.
Conclusions: Our findings show that the representation of symptoms of PTSD that develops following a stressogenic childbirth experience appears, for the most part, to resemble DSM-5 symptom clusters. More research integrating descriptive symptom assessment with biological measures is warranted to better characterize the symptom presentation of this neglected posttraumatic stress syndrome.
Prim Care Companion CNS Disord 2018;20(5):18m02322
To cite: Thiel F, Ein-Dor T, Dishy G, et al. Examining symptom clusters of childbirth-related posttraumatic stress disorder. Prim Care Companion CNS Disord. 2018;20(5):18m02322.
To share: https://doi.org/10.4088/PCC.18m02322
© Copyright 2018 Physicians Postgraduate Press, Inc.
aDepartment of Psychiatry, Massachusetts General Hospital, Charlestown, Massachusetts
bUniversity of Groningen, Grote Kruisstraat 2/1, Groningen, Netherlands
cInterdisciplinary Center (IDC), Herzliya, Israel
dHarvard Medical School, Harvard University, Boston, Massachusetts
*Corresponding author: Sharon Dekel, PhD, Department of Psychiatry, Massachusetts General Hospital/Harvard Medical School, Charlestown Navy Yard, 120 2nd Ave, Charlestown, MA 02129 ([email protected]. edu).
Posttraumatic stress disorder (PTSD) is a psychiatric condition precipitated by exposure to a traumatic event and often implicated in functional impairment.1 In the face of the stressor, an acute stress (fight, flight, or freeze) response is activated to conquer or avoid the threat and achieve homeostasis.2,3 When the stress response remains, enduring symptoms of PTSD may ensue in reminders of exposure (eg, nightmares and flashbacks), activation (eg, irritability and hyperarousal), and deactivation (eg, avoidance and numbing) of trauma-related stimuli. The symptoms may, therefore, be viewed as an abnormal adaptation to the stressor4 for a period extending beyond 1 month following exposure.
Childbirth is viewed as a happy event but can also be a highly stressful experience involving an actual or perceived threat. Given that childbirth-related maternal and infant deaths are a known phenomenon around the world, some women may fear for their life or that of their child prior to and during childbirth. As research5–7 demonstrates, some women can develop a posttraumatic stress response to childbirth. Childbirth-induced postpartum PTSD (PP-PTSD) symptoms are not limited to incomplete pregnancies (eg, still birth, pregnancy loss). As much as a quarter of women report PP-PTSD symptoms at a clinical level following childbirth,8 and incidences of full-blown PTSD in the first months postpartum range between 5% and 11% in women delivering a healthy baby at the expected time.9
Nonetheless, the notion that childbirth can trigger PTSD remains controversial, and little is known about the presentation of PP-PTSD symptoms. Such knowledge is important to better characterize this traumatic stress syndrome and to compare and contrast with the typical grouping of PTSD symptoms following other potentially traumatic events such as war, assault, or disaster.
Clustering is a common modeling technique in which data are divided into groups of similar objects with the aim of identifying homogenous groups of cases.10,11 In reference to a mental condition, various symptoms of psychopathology are tied together into potential coherent syndromes. To the best of our knowledge, no study has examined the clustering of PP-PTSD symptoms on the basis of DSM-5 symptoms. The DSM-5 conceptualizes several PTSD symptom clusters, namely reexperiencing (cluster B), avoidance (cluster C), alterations in cognitions and mood (cluster D), and arousal and reactivity (cluster E). Rather than being defined as an anxiety or mood disorder, trauma-related disorders are defined as their own entity. Existing studies12,13 on PP-PTSD symptom clusters are scarce and have focused almost exclusively on assessing the prevalence of predefined clusters, with the highest rates found for hyperarousal and lowest rates for avoidance. A single factor analysis study14 documented 2 factors pertaining to reexperiencing and avoidance and numbing and arousal in PP-PTSD, although the analysis was based on DSM-IV symptoms.
Here, we studied a large sample of postpartum women, some of whom reported clinically relevant childbirth-related PP-PTSD symptoms. We examined the clustering of PP-PTSD symptoms and the extent to which it accords with DSM-5 clusters.
METHODS
Participants
This study is part of a project on psychological outcomes of childbirth.15 Via announcements on postpartum websites, we recruited participants who were at least 18 years of age and gave birth within the past 6 months. Women were asked to complete an anonymous survey and were informed that by agreeing to participate, they were implying their consent. Partners Human Research Committee (Massachusetts General Hospital, Boston, Massachusetts) granted exemption.
The sample included 685 women who were, on average, 3 months postpartum (SD=1.5) and 31 years old (SD=4.80), with 79% giving birth to a healthy baby at term and 64% delivering vaginally. The majority was married (93%), had at least a college education (71%), lived in North America (66%), and was middle class (median household income: $50,000–$99,000).
Measures
Childbirth-related PTSD symptoms were assessed via the commonly used PTSD Checklist for DSM-5 (PCL-5).16 Participants rated PTSD symptom severity over the past month from 0 (not at all) to 4 (extremely) on 20 items with the index event anchored to “most recent childbirth.” The PCL-5 has good psychometric properties,17 and reliability in this study was high (α = 0.95). Conforming to DSM-5,1 we defined PP-PTSD as moderate symptom severity (scores ≥ 2), including at least 1 reexperiencing item (cluster B), 1 avoidance item (cluster C), 2 alterations in cognitions and mood items (cluster D), and 2 arousal and reactivity items (cluster E).
Childbirth-related peritraumatic stress reactions during or immediately following childbirth were assessed in regard to distress and dissociation. We used the well-validated Peritraumatic Distress Inventory (PDI)18 that lists 13 items, each rated from 0 (not at all) to 4 (extremely) (eg, feeling guilty, helpless). The PDI has good psychometric properties,18 and reliability in this study was high (α = 0.89). Dissociation was measured via the commonly used Peritraumatic Dissociative Experiences Questionnaire (PDEQ) that lists 10 items, each rated from 0 (not at all) to 4 (extremely true) (eg, “What was happening seemed unreal to me.”). The PDEQ has good psychometric properties,19,20 and reliability in this study was high (α = 0.91). Additionally, perceived danger during or immediately after delivery (DSM-5 PTSD criterion A)1 was assessed with a single item rated from 0 to 4 (“Did you feel you were or your baby was in danger during or immediately after the delivery?”).
RESULTS
Overall, 8.6% of the data were missing, with Little’s Missing Completely At Random (MCAR) test21 indicating missing completely at random (χ22,654 = 1642.80, P = 1.00). We subsequently handled missing data via multiple imputation.
Descriptive Statistics
Twenty percent of the sample (n = 136) was classified as having PP-PTSD. Of the women delivering healthy babies at term, 17% endorsed PP-PTSD (n = 92). Overall, negative cognitions and mood was the most frequently endorsed symptom cluster (49%), followed by hyperarousal and reactivity (45%), reexperiencing (36%), and avoidance (27%).
A series of Pearson correlations between PP-PTSD symptom severity and level of childbirth-related peritraumatic stress reactions revealed strong positive associations. PP-PTSD symptoms were correlated with PDI, PDEQ, and sense of danger, with an r of 0.71, 0.67, and 0.48, respectively. The more peritraumatic stress women endorsed, the higher their PTSD symptoms.
PP-PTSD Symptom Clustering
We utilized hierarchical cluster analysis to detect grouping of PP-PTSD symptoms. Furthest neighbors clustering with squared Euclidean distances to estimate commonalities produced the most distinct clusters. The results of this analysis are depicted in Figure 1.
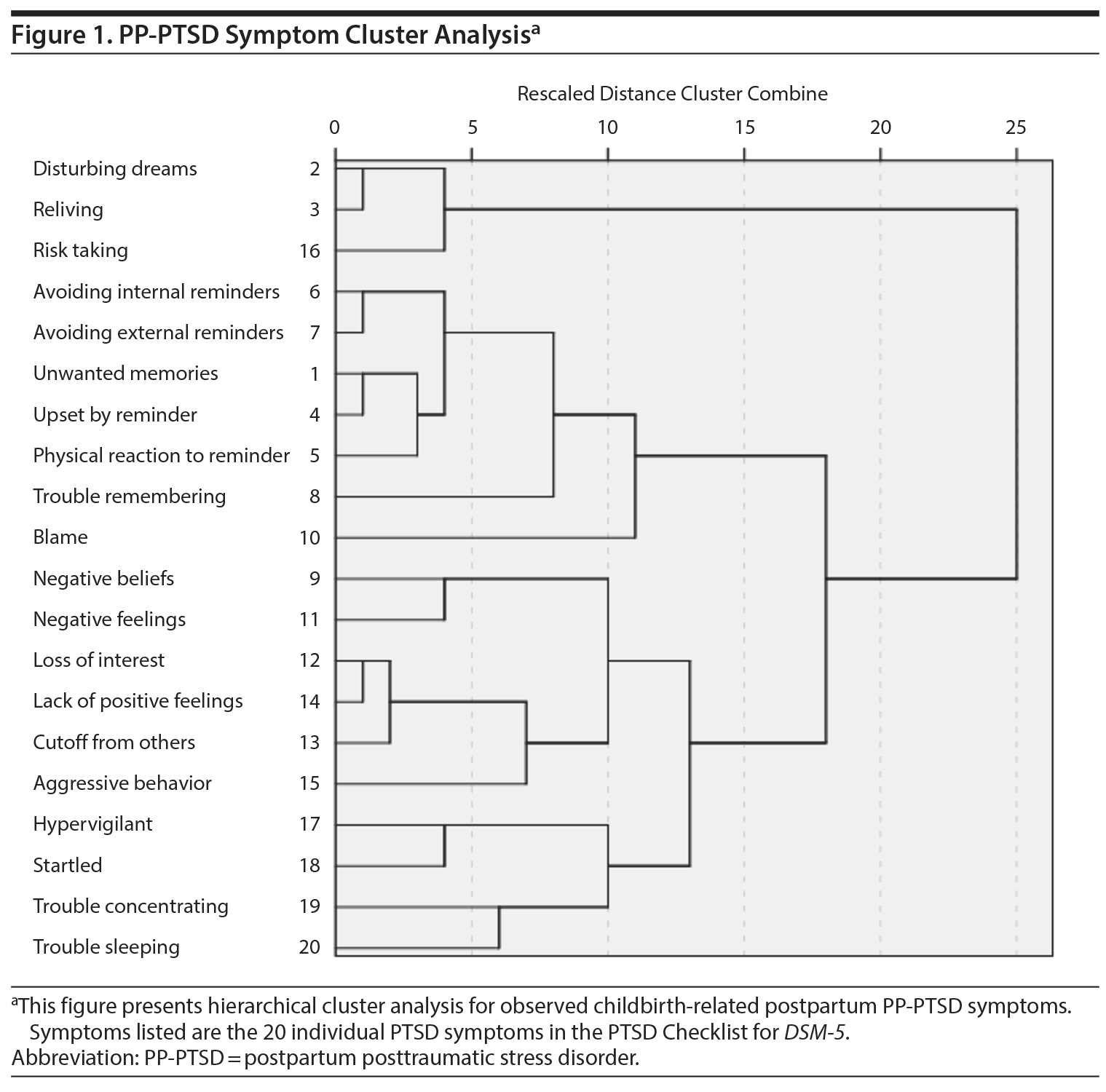
The analysis detected 4 clusters: reexperiencing pertaining to nightmares and flashbacks (items 2, 3, 16), other reexperiencing symptoms (ie, unwanted memories) grouped with avoidance symptoms (items 1, 4, 5, 6, 7, 8, 10), negative cognitions and mood (items 9, 11, 12, 13, 14, 15), and symptoms of hyperarousal and reactivity (items 17, 18, 19, 20). As can be seen, in comparison with DSM-5, the original reexperiencing cluster is narrowed, now pertaining to reliving symptoms. Other reexperiencing symptoms of unwanted memories are grouped in the avoidance cluster. The other 2 clusters accord with DSM classification.
DISCUSSION
The notion that childbirth could be associated with a traumatic experience is not commonly discussed, nor is the occurrence of PP-PTSD symptoms following birth. As we expected that a significant minority of women would report elevated PTSD symptoms associated with a stressful childbirth experience, we tested the question of whether the presentation of PP-PTSD symptoms resembles the symptom clusters of DSM-5.
The main analysis revealed that PP-PTSD symptoms group into 4 distinguished clusters including reliving, namely flashbacks and nightmares; avoidance coupled with unwanted memories (ie, other re-experiencing symptoms); negative cognitions and mood; and arousal and reactivity. Altogether, the presentation of PTSD symptoms in relation to childbirth generally resembles the formal symptom clusters of PTSD.
Reliving symptoms is argued to be a distinguished core feature of PTSD.22 Reliving the trauma as if it was happening in the present is a strong predictor of the course of the disorder.23 Flashbacks have been found in individuals with PTSD compared with trauma-exposed individuals who may experience involuntary memories but do not develop the disorder.24,25 Trauma nightmares have also been shown to be central in PTSD.26,27 The reliving cluster in PP-PTSD suggests that the condition may be triggered by a traumatic birth experience rather than merely an abnormal anxiety response.
The evidence of a cluster of avoidance symptoms coupled with undesired memories of the childbirth, such as feeling upset and having a physical reaction to the birth reminder, is not entirely unexpected. Ayers and colleagues14 report similar results. Avoidance may have a strategic escape function to manage unwanted trauma reminders.28 Avoidance strategies for women with PP-PTSD might be unsuccessful due to recurrent inevitable reminders of childbirth-related stimuli (eg, the baby), resulting in avoidance coupled with childbirth reminders.
The distinguished negative cognitions and mood cluster found in this study accords with the recent DSM classification. Avoidance and numbing symptoms have been shown not to belong in the same cluster in nonpostpartum samples.29 Evidence of a separate numbing symptom cluster in PP-PTSD may, in part, contribute to the high comorbidity rates with symptoms of postpartum depression.15,30 Our finding of 49% of the current sample endorsing symptoms of the negative cognitions and mood cluster is in line with comorbidity rates of PTSD and depression in nonpostpartum samples.31
Several limitations of the study should be noted. PP-PTSD symptoms were measured at a single time point, although assessment was around 3 months’ postpartum—a time period in which symptoms become stable. A related issue is that the retrospective report of peritraumatic stress might have been influenced by a woman’s PTSD symptom status. Although we assessed PP-PTSD with a well-validated measure, we did not assess whether a participant had clinically diagnosed PTSD. Given the current sample, although large in size, was derived from a web survey, the possibility of sample selection bias, severity-related reporting bias, and the potential of the same person completing the survey more than once and providing false information regarding inclusion criteria should be noted. Future research examining the nature of PP-PTSD symptoms across the postpartum period is thus warranted.
In summary, we document that among women who experience childbirth-related PTSD symptoms in the first postpartum months, symptom clusters, for the most part, appear to resemble the clusters of PTSD symptoms precipitated by other potentially traumatic events. On a broader level, our work offers empirical support for a PP-PTSD syndrome following at-term delivery with a healthy baby. Characterizing PP-PTSD symptoms by integrating descriptive and biological measures may further advance our knowledge of this neglected postpartum condition.
Submitted: April 27, 2018; accepted July 12, 2018.
Published online: September 27, 2018.
Potential conflicts of interest: None.
Funding/support: None.
REFERENCES
1. American Psychiatric Association. Diagnostic and Statistical Manual for Mental Disorders. Fifth Edition. Washington, DC: American Psychiatric Association; 2013.
2. Dekel S, Ein-Dor T, Gordon KM, et al. Cortisol and PTSD symptoms among male and female high-exposure 9/11 survivors. J Trauma Stress. 2013;26(5):621–625. PubMed CrossRef
3. Dekel S, Ein-Dor T, Rosen JB, et al. Differences in cortisol response to trauma activation in individuals with and without comorbid PTSD and depression. Front Psychol. 2017;8:797. PubMed CrossRef
4. Sherin JE, Nemeroff CB. Post-traumatic stress disorder: the neurobiological impact of psychological trauma. Dialogues Clin Neurosci. 2011;13(3):263–278. PubMed
5. Ayers S, Bond R, Bertullies S, et al. The aetiology of post-traumatic stress following childbirth: a meta-analysis and theoretical framework. Psychol Med. 2016;46(6):1121–1134. PubMed CrossRef
6. Grekin R, O’Hara MW. Prevalence and risk factors of postpartum posttraumatic stress disorder: a meta-analysis. Clin Psychol Rev. 2014;34(5):389–401. PubMed CrossRef
7. Olde E, van der Hart O, Kleber R, et al. Posttraumatic stress following childbirth: a review. Clin Psychol Rev. 2006;26(1):1–16. PubMed CrossRef
8. Czarnocka J, Slade P. Prevalence and predictors of post-traumatic stress symptoms following childbirth. Br J Clin Psychol. 2000;39(pt 1):35–51. PubMed CrossRef
9. Dekel S, Stuebe C, Dishy G. Childbirth induced posttraumatic stress syndrome: a systematic review of prevalence and risk factors. Front Psychol. 2017;8:560. PubMed CrossRef
10. Berkhin P. A Survey of Clustering Data Mining Techniques, Grouping Multidimensional Data. Heidelberg, Germany: Springer; 2006:25–71.
11. Scott AJ, Knott M. A cluster analysis method for grouping means in the analysis of variance. Biometrics. 1974;30(3):507–512. CrossRef
12. Cigoli V, Gilli G, Saita E. Relational factors in psychopathological responses to childbirth. J Psychosom Obstet Gynaecol. 2006;27(2):91–97. PubMed CrossRef
13. Maggioni C, Margola D, Filippi F. PTSD, risk factors, and expectations among women having a baby: a two-wave longitudinal study. J Psychosom Obstet Gynaecol. 2006;27(2):81–90. PubMed CrossRef
14. Susan A, Harris R, Sawyer A, et al. Posttraumatic stress disorder after childbirth: analysis of symptom presentation and sampling. J Affect Disord. 2009;119(1–3):200–204. PubMed CrossRef
15. Dekel S, Thiel F, Dishy G, et al. Is childbirth-induced PTSD associated with low maternal attachment [epub ahead of print]? Arch Womens Ment Health. May 21, 2018. PubMed CrossRe
16. Weathers FW, Litz BT, Keane TM, et al. The PTSD Checklist for DSM-5 (PCL-5). 2013. National Center for PTSD website. https://www.ptsd.va.gov/.
17. Blevins CA, Weathers FW, Davis MT, et al. The Posttraumatic Stress Disorder Checklist for DSM-5 (PCL-5): development and initial psychometric evaluation. J Trauma Stress. 2015;28(6):489–498. PubMed CrossRef
18. Brunet A, Weiss DS, Metzler TJ, et al. The Peritraumatic Distress Inventory: a proposed measure of PTSD criterion A2. Am J Psychiatry. 2001;158(9):1480–1485. PubMed CrossRef
19. Birmes P, Brunet A, Benoit M, et al. Validation of the Peritraumatic Dissociative Experiences Questionnaire self-report version in two samples of French-speaking individuals exposed to trauma. Eur Psychiatry. 2005;20(2):145–151. PubMed CrossRef
20. Bui E, Brunet A, Olliac B, et al. Validation of the Peritraumatic Dissociative Experiences Questionnaire and Peritraumatic Distress Inventory in school-aged victims of road traffic accidents. Eur Psychiatry. 2011;26(2):108–111. PubMed CrossRef
21. Rubin DB. Multiple Imputation for Nonresponse in Surveys. Indianapolis, IN: John Wiley & Sons; 2009.
22. Brewin CR. Episodic memory, perceptual memory, and their interaction: foundations for a theory of posttraumatic stress disorder. Psychol Bull. 2014;140(1):69–97. PubMed CrossRef
23. Kleim B, Ehlers A, Glucksman E. Early predictors of chronic posttraumatic stress disorder in assault survivors. Psychol Med. 2007;37(10):1457–1467. PubMed CrossRef
24. Birrer E, Michael T, Munsch S. Intrusive images in PTSD and in traumatized and non-traumatized depressed patients: a cross-sectional clinical study. Behav Res Ther. 2007;45(9):2053–2065. PubMed CrossRef
25. Brewin CR. Intrusive autobiographical memories in depression and posttraumatic stress disorder. Appl Cogn Psychol. 1998;12(4):359–370. CrossRef
26. Spoormaker VI, Montgomery P. Disturbed sleep in posttraumatic stress disorder: secondary symptom or core feature? Sleep Med Rev. 2008;12(3):169–184. PubMed CrossRef
27. Pillar G, Malhotra A, Lavie P. Posttraumatic stress disorder and sleep: what a nightmare! Sleep Med Rev. 2000;4(2):183–200. PubMed CrossRef
28. Foa EB, Riggs DS, Gershuny BS. Arousal, numbing, and intrusion: symptom structure of PTSD following assault. Am J Psychiatry. 1995;152(1):116–120. PubMed CrossRef
29. Zoellner LA, Bedard-Gilligan MA, Jun JJ, et al. The evolving construct of posttraumatic stress disorder (PTSD): DSM-5 criteria changes and legal implications. Psychol Inj Law. 2013;6(4):277–289. PubMed CrossRef
30. Söderquist J, Wijma B, Thorbert G, et al. Risk factors in pregnancy for posttraumatic stress and depression after childbirth. BJOG. 2009;116(5):672–680. PubMed CrossRef
31. O’Donnell ML, Creamer M, Pattison P. Posttraumatic stress disorder and depression following trauma: understanding comorbidity. Am J Psychiatry. 2004;161(8):1390–1396. PubMed CrossRef
Enjoy this premium PDF as part of your membership benefits!


