Objective: To explore in Arab communities the prevalence, dynamics, and resources available to address the physical and psychological consequences that may arise from psychiatric disorders.
Methods: An online survey of psychiatrists and primary care physicians from 17 Arab countries was conducted between September 2011 and June 2012. The survey serves as a needs assessment in a scientifically valid and culturally sensitive manner. Additionally, it focuses attention on the clinical strengths and weaknesses of Middle Eastern primary health care and mental health centers in identifying and treating trauma-related health and mental health issues.
Results: The 90 survey respondents comprised psychiatrists (n = 53) and primary care physicians (n = 37). They practiced in 3 clinical settings: primary mental health (27%), inpatient mental health (43%), and primary health care (29%). Traumas frequently reported by their patients were attributed to recent death of a close relative or friend (62.3%), domestic violence (41.4%), divorce/separation (72.1%), serious traffic accident (45.6%), sexual assault/rape (20.3%), child abuse (20.3%), psychological effects of war (30.9%), victims of crime (15.9%), refugees/internally displaced persons (20.6%), physical effects of war (19.1%), torture (13.2%), elderly abuse (11.6%), psychological effects of a natural disaster (7.4%), physical effect of a natural disaster (7.2%), and child soldiers (4.3%). Psychiatrists had significantly more patients with the following traumatic experiences: divorce/separation (81.4% vs 57.1%, P = .039), recent death of a close relative or friend (72.7% vs 47.6%, P = .048), and domestic violence (51.1% vs 19.0%, P = .014). Clinical teams comprised substantial numbers of students but small numbers of community volunteers and school counselors.
Conclusions: This study highlights the need to develop awareness and training programs in Arab communities to identify and properly treat traumatized individuals in psychiatric and primary care settings.
Trauma-Informed Care Survey of Psychiatrists
and Primary Care Physicians in the Middle East
ABSTRACT
Objective: To explore in Arab communities the prevalence, dynamics, and resources available to address the physical and psychological consequences that may arise from psychiatric disorders.
Methods: An online survey of psychiatrists and primary care physicians from 17 Arab countries was conducted between September 2011 and June 2012. The survey serves as a needs assessment in a scientifically valid and culturally sensitive manner. Additionally, it focuses attention on the clinical strengths and weaknesses of Middle Eastern primary health care and mental health centers in identifying and treating trauma-related health and mental health issues.
Results: The 90 survey respondents comprised psychiatrists (n = 53) and primary care physicians (n = 37). They practiced in 3 clinical settings: primary mental health (27%), inpatient mental health (43%), and primary health care (29%). Traumas frequently reported by their patients were attributed to recent death of a close relative or friend (62.3%), domestic violence (41.4%), divorce/separation (72.1%), serious traffic accident (45.6%), sexual assault/rape (20.3%), child abuse (20.3%), psychological effects of war (30.9%), victims of crime (15.9%), refugees/internally displaced persons (20.6%), physical effects of war (19.1%), torture (13.2%), elderly abuse (11.6%), psychological effects of a natural disaster (7.4%), physical effect of a natural disaster (7.2%), and child soldiers (4.3%). Psychiatrists had significantly more patients with the following traumatic experiences: divorce/separation (81.4% vs 57.1%, P = .039), recent death of a close relative or friend (72.7% vs 47.6%, P = .048), and domestic violence (51.1% vs 19.0%, P = .014). Clinical teams comprised substantial numbers of students but small numbers of community volunteers and school counselors.
Conclusions: This study highlights the need to develop awareness and training programs in Arab communities to identify and properly treat traumatized individuals in psychiatric and primary care settings.
Prim Care Companion CNS Disord 2017;19(5):17m02157
https://doi.org/10.4088/PCC.17m02157
© Copyright 2017 Physicians Postgraduate Press, Inc.
aCollege of Medicine and Health Sciences, United Arab Emirates University, Al Ain, United Arab Emirates
bCreighton University School of Medicine, Omaha, Nebraska
cHarvard Program in Refugee Trauma, Boston, Massachusetts
dCollege of Business, United Arab Emirates University, Al Ain, United Arab Emirates
*Corresponding author: Ossama T. Osman, MD, College of Medicine and Health Sciences, United Arab Emirates University, Al Ain, United Arab Emirates ([email protected]).
Psychological trauma is increasingly recognized as being at the core of many psychiatric disorders. In recent years, there has been an increase in awareness of the role of psychological sequelae of trauma as a predisposing and comorbid condition. It is estimated that as many as 100–140 million people in the Arab world suffer from 1 or more psychiatric disorders.1 Violence, war, political and social instability, and change have all played a role in increasing the regional prevalence of trauma. The physical and psychological consequences of trauma are disabling to individuals, families, and communities. Furthermore, the negative effects of these conditions have spread through social networks and across generations. Maternal mental health issues, for example, are associated with negative physical, developmental, and psychological outcomes in their offspring, who in turn may develop an increased risk of mental health disorders that then persist and worsen in adulthood. Additionally, mental health and substance misuse conditions are risk factors for the development of chronic noncommunicable diseases, such as atherosclerotic vascular disease, diabetes, and chronic lung disease. Both mental health conditions and noncommunicable diseases have a significant impact on health and economic productivity and are major causes of morbidity and mortality in low- and middle-income countries. Recently, the United Nations and the World Health Organization (WHO) reasserted the importance of mental health in the Millennium Development Goals.2
Limited data concerning mental health resources in the primary care setting are available from local scientific literature in the Middle East. Assessment of the structure and function of psychiatric resources in the region, however, is beginning to receive increased attention. In 2008, WHO launched the Mental Health Gap Action Program3 aimed at reducing the disparity between existing mental health resources and those available to address neurologic, mental health, and substance use problems. Several countries in the Middle Eastern region were identified as requiring special attention under this program. In 2010, WHO carried out an extensive descriptive study4 of the mental health resources and systems available in 14 of the 22 countries in the region (WHO-AIMS). This study confirmed the scarcity of mental health resources in the region. Additionally, it highlighted an uneven distribution of facilities and resources together with the poor integration of mental health services into other parts of the health care system and the community. Of the countries studied, about half lacked any formal mental health legislation. Only 3 of the 14 countries surveyed reported having an emergency or disaster preparedness plan for mental health.4 Other studies5,6 have revealed that cultural factors that include stigma, social dynamics, and characteristics of the medical system in the primary care setting often result in a small number of patients being identified or ever receiving psychiatric care.
In this study, we conducted a needs assessment among psychiatrists and primary care physicians practicing in clinical settings in regional mental health facilities and primary care centers in the Middle East. This study is part of a global mental health partnership between the Zayed Institute for Public Health, United Arab Emirates University (Al Ain, United Arab Emirates) and the Harvard Program in Refugee Trauma (Boston, Massachusetts).
METHODS
Participants and Design
A confidential online survey was sent via e-mail to 103 psychiatrists and primary care physicians in 17 Arab countries. The primary investigator (O.T.O.) made phone calls to many of the responders explaining the purpose of the survey and the online completion process. We used a snowball sampling technique. The primary author provided contact information from an extensive list of colleagues from throughout the Arab region. The other authors supplemented the information with contacts of their own. Several secondary contacts were developed via the primary contacts. All respondents were either psychiatrists or primary care physicians.
The anonymous survey was completed between September 2011 and June 2012. The survey included an informed consent statement and definitions for the terminology used throughout the survey. The main survey dimensions included demographic information about respondent and facility, composition of health and mental health practitioners, mental health problems, social issues, therapeutic drugs, mental health training, research, monitoring, and program evaluation. In addition, there were questions assessing practitioner confidence in addressing trauma-related mental health problems.
Arab league countries were categorized into lower and higher groups depending on the number of psychiatrists per 100,000 population on the basis of previously published data.7 Those countries with approximately 1 psychiatrist per 100,000 population or greater were classified as high, and those with smaller numbers were classified as low.
Statistical Analysis
We exported the survey responses from the online survey website into SPSS statistical software release 20 (IBM Inc, Chicago, Illinois) and reviewed the data carefully for missing values and duplicate entries. We obtained descriptive statistics including percentages, means, and standard errors, and responses on the 6-point scale were treated as continuous variables for analysis. Analytic statistical testing, where appropriate, was conducted using 1-way analysis of variance and χ2 tests. We applied 2-tailed testing using a significance level of .05.
RESULTS
We received 90 completed responses from 103 psychiatrists and primary care physicians invited to participate in the survey. We first present the demographic characteristics of the respondents by specialty, practice setting, and country. We then present the overall frequency of the common types of traumas reportedly seen. Subsequently, we compare responses of psychiatrists and primary care physicians about their perception of confidence in the ability of primary care practitioners in their country to provide trauma-related mental health services. Finally, we divide the countries into 2 groups: low number of psychiatrists (< 1 psychiatrist per 100,000 population) and high number of psychiatrists (≥ 1 psychiatrists per 100,000 population).
Demographics
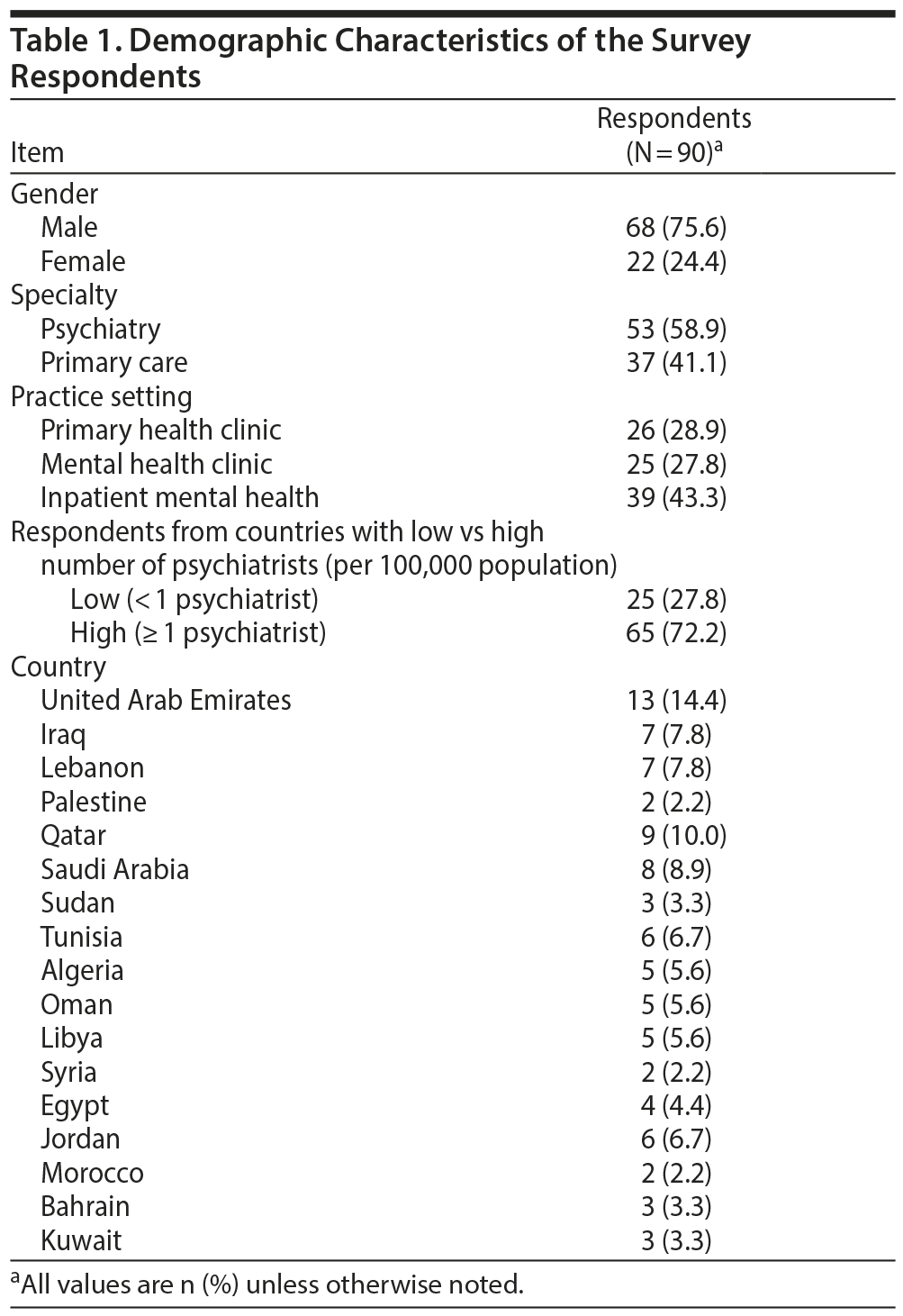
Table 1 describes the demographic information for the 90 respondent psychiatrists (n = 53) and primary care physicians (n = 37) of both genders (F = 22, mean = 68) from 17 Arab countries. These respondents practiced in 3 different clinical settings: mental health (28%), inpatient mental health (43%), and primary health care (29%). Of the 90 respondents, 25 (27.8%) were from 7 Arab countries with low numbers of psychiatrists.
Composition of Clinical Teams
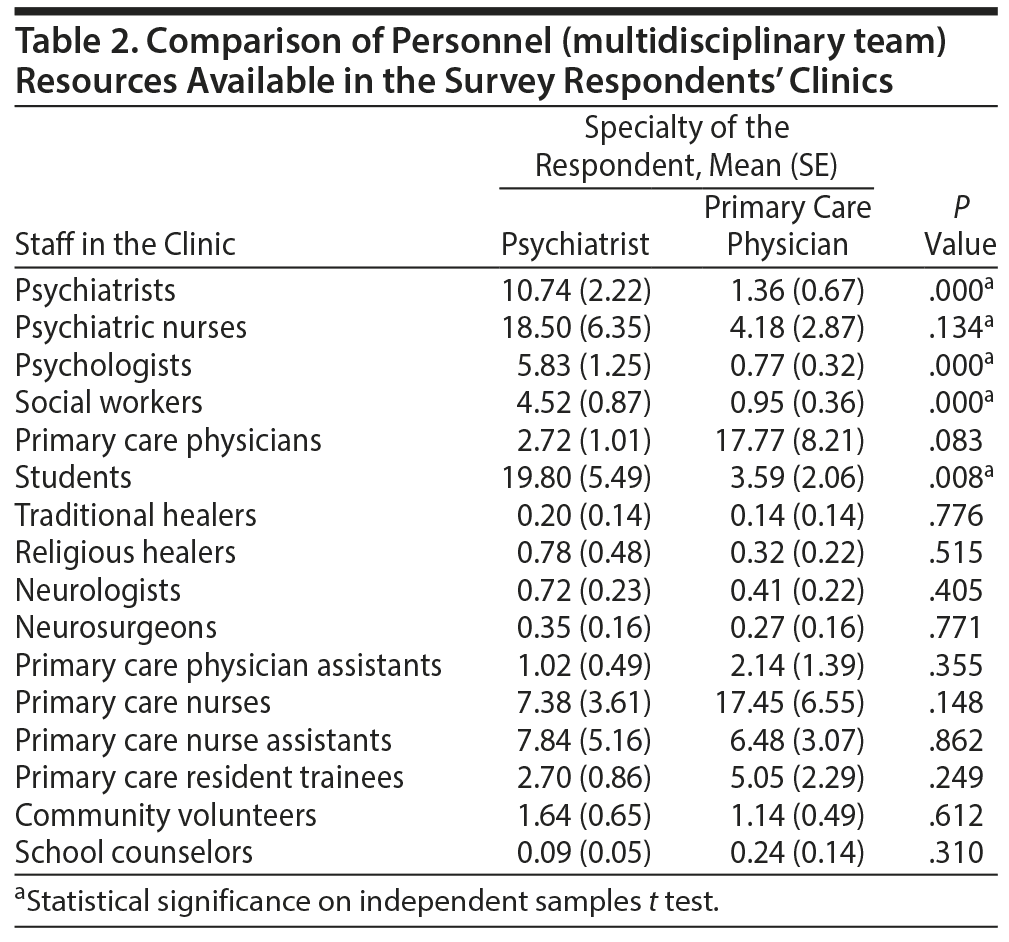
Table 2 compares the number of personnel resources in the clinics of the respondent psychiatrists and primary care physicians. More specialized mental health and social workers were available in the psychiatry settings compared to primary care. In both settings, respondents reported few traditional or religious healers, community volunteers, or school counselors to be part of the clinical team. Of interest is the relatively large number of students reported to be present in both psychiatric and primary care centers. This finding necessitates focused attention to developing programs for their education and training and dedicating qualified staff for their mentoring and clinical supervision to help them acquire necessary basic competencies in trauma-informed care.
Mental Health Problems Encountered by Respondents
Figure 1 shows responses regarding the frequency of trauma-related health and mental health issues presenting in clinical settings. The most commonly reported traumas were recent death of a close relative or friend (62.3%), domestic violence (41.4%), divorce/separation (72.1%), serious traffic accident, (45.6%), sexual assault/rape (20.3%), child abuse (45.6%), psychological effects of war (30.9%), victim of crime (15.9%), refugees/internally displaced persons (20.6%), physical effects of war (19.1%), torture (13.2%), elderly abuse (11.6%), psychological effects of a natural disaster (7.4%), physical effects of a natural disaster (7.2%), and child soldiers (4.3%).
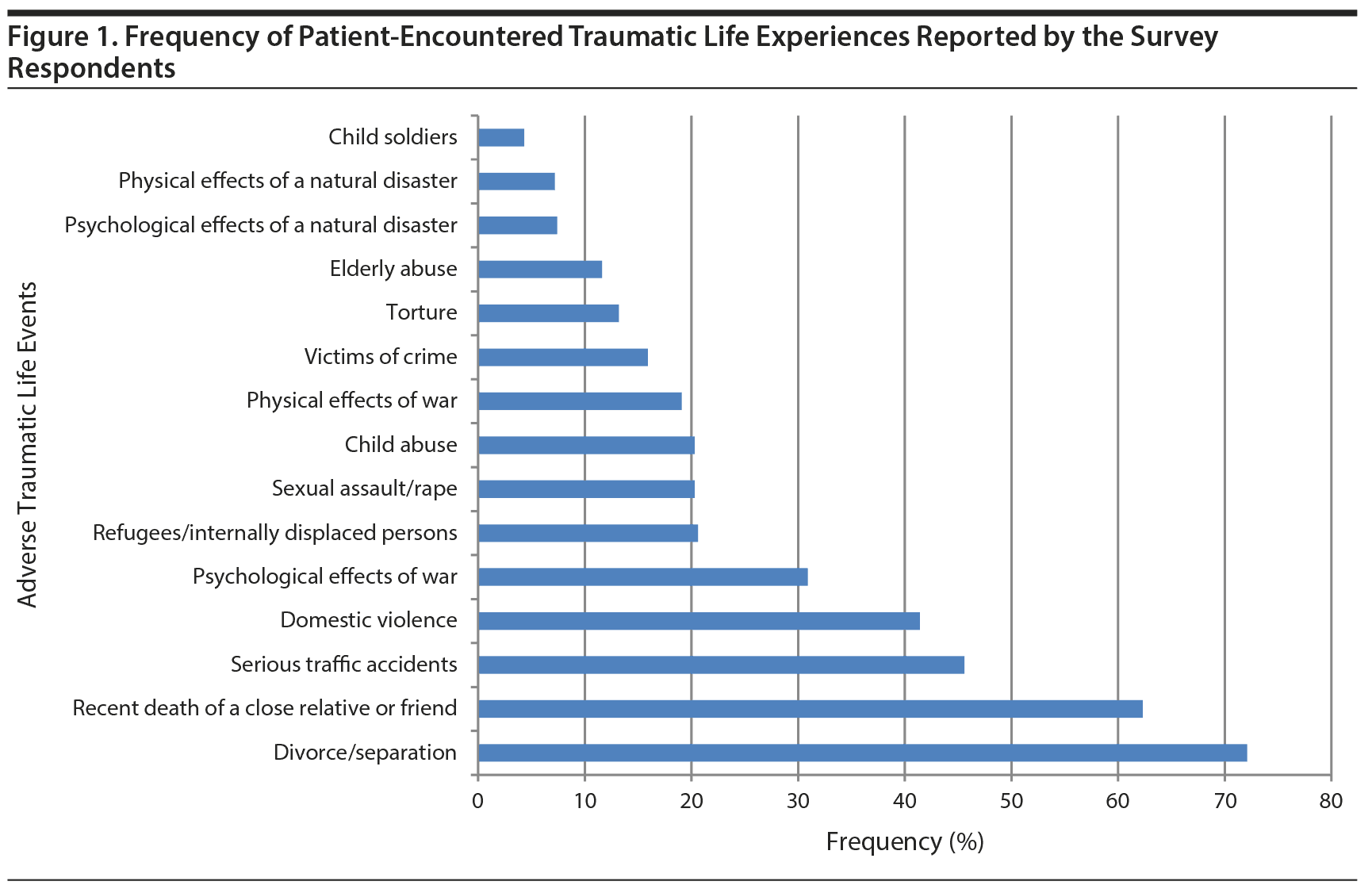
Table 3 compares responses of psychiatrists and primary care physicians. Psychiatrists reported a significant number of patients with the following traumatic experiences compared to primary care physicians: divorce/separation (81.4% vs 57.1%, P = .039), the recent death of a close relative or friend (72.7% vs 47.6%, P = .048), and domestic violence (51.1% vs 19.0%, P = .014). On the other hand, there were other types of traumas with no statistically significant differences in frequency between the 2 groups of respondents: psychological effects of war, torture, victims of crime, serious traffic accidents, sexual assault/rape, and child and elderly abuse.
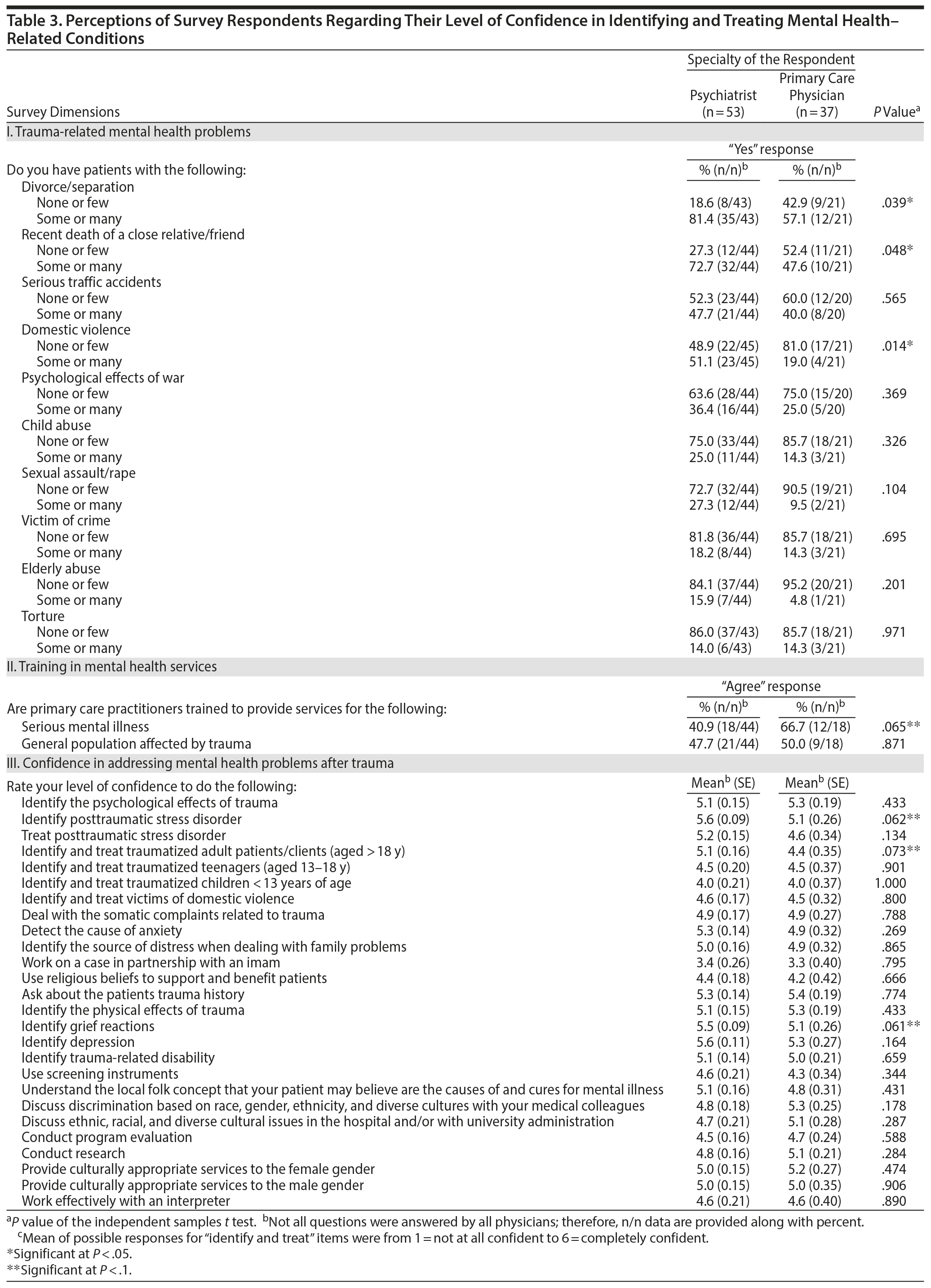
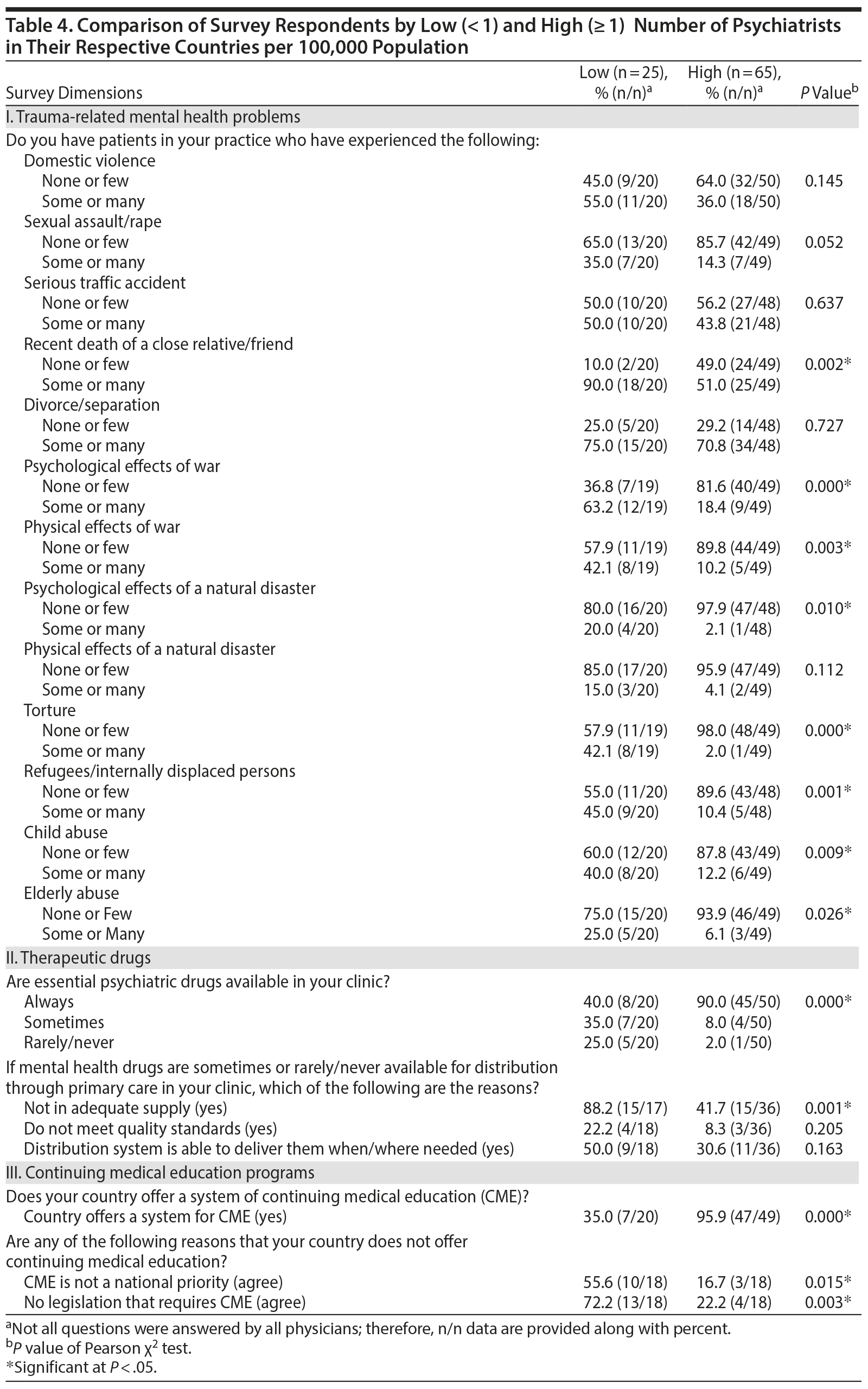
Table 4 compares responses of psychiatrists and primary care physicians practicing in countries with low versus high numbers of psychiatrists. Significant differences were identified in the frequency of the following traumas: psychological effects of war (low: 63.2% vs high: 18.4%, P = .000), victims of crime (low: 40% vs high: 6.1%, P = .000), refugees/internally displaced persons (low: 45.0 vs high: 10.4%, P = .001), torture (low: 42.1 vs high: 2.0%, P = .000), child abuse (low: 40.0% vs high: 12.2%, P = .009), sexual assault/rape (low: 35.0% vs high: 14.3%, P = .052), elderly abuse (low: 25.0% vs high: 6.1%, P = .026), physical effects of war (low: 42.1% vs high: 10.2%, P = .003), and psychological effects of natural disaster (low: 20.0% vs high: 2.1%, P = .010).
Training for Primary Care Physicians
and Therapeutic Drugs
Table 3 shows that half of the respondent psychiatrists (48%) and primary care physicians (50%) believe primary care practitioners in their countries are trained to provide trauma-related mental health services with no statistically significant difference (P = .871). However, with respect to providing services for the general population with serious mental illness, there was a trend for more primary care physicians than psychiatrists to respond that primary care practitioners in their countries are trained in this regard (P value = .065).
Access to psychiatric drugs was reported to be problematic in many cases. Respondents reported a lack of an adequate supply of medications in their clinical settings (65.7%), misdistribution of medications (50.0%), and the limitation of availability of these drugs to psychiatric facilities and psychiatrists (32.4%).
Confidence in Addressing
Patients’ Mental Health Problems After Trauma
Both groups of respondents felt equally comfortable in identifying and treating mental health problems in their patients after trauma. A trend was evident for psychiatrists to feel more confident being able to identify posttraumatic stress disorder, identify and treat adult (> 18 years) traumatized patients, and identify grief reactions (P = .062, P = .073, and P = .061, respectively).
Continuing Medical Education Programs
The majority (65%) of respondents from countries with lower number of psychiatrists reported having no system for continuing medical education. About 72% reported that their countries have no legislation to require continuing medication education, and nearly half (44.4%) acknowledged it is not a national priority.
DISCUSSION
The findings of this study suggest a widespread perception among front-line practitioners that there is a need for increased focus on psychological and psychiatric morbidity in the region, particularly as it relates to trauma. This finding is consistent with a large body of literature5,7 indicating that while psychiatric problems are common in the region, insufficient resources exist to address them. Overall, most Arab countries direct less than 2% of their national health care budget toward mental health. Some countries reported budgeting little or nothing at all for mental health issues.4
We also found that many patients experience social problems putting them at risk for mental illness or representing barriers to care. These social problems include divorce or separation and refugee status. Among women in Arab countries, separation or divorce often results in social marginalization, and support is often unavailable.8,9 Depressive and other psychiatric symptoms in patients presenting to primary care are often related to marital problems.10,11 Interestingly, psychiatrists reported seeing divorced patients more frequently than did primary care physicians, which may be a manifestation of a low recognition of psychosocial problems at the primary care level.
Survey respondents also indicated that they were not highly confident in managing patients with various types of psychosocial problems. This finding most likely reflects the lack of exposure to these issues in most medical training programs in the region, which have failed to effectively incorporate psychosocial issues into curricula. This problem is particularly serious because of the lack of culturally relevant research on these topics.12 Also, there is a lack of social consensus on many issues that may be common among some sectors of society but have been reported to be associated with significant psychological morbidity, such as polygamous marriage.13–16 Additionally, physicians may feel pressure to adhere to strong social conventions that discourage bringing up topics that may result in embarrassment.17
An interesting finding was the differences in types of problems reported in countries with lower or higher numbers of practicing psychiatrists per capita. Several possibilities exist to explain this finding. Countries with higher numbers of psychiatrists tend to be wealthier than countries with lower numbers. Poverty is a known risk factor for mental illness. Consequently, it would be more likely that medical systems in less wealthy countries were less organized and their acute needs greater than those in wealthier countries. In addition, psychiatrists from poorer Arab countries often migrate to the richer countries for better job opportunities. Two countries, Iraq and Palestine, were involved in complex emergency situations at the time of the survey. Finally, the possibility exists that countries with fewer psychiatrists per capita have larger populations of patients with mental illness. This might result in increased disruption of families and communities through social network effects, thereby exacerbating existing problems. Interestingly, practitioners working in countries with a low number of psychiatrists per capita seemed to be more satisfied with the availability and quality of essential medications, although distribution was reported to be more problematic.
Regional literature5,7,18 indicates a high and unmet need with regard to the treatment of mental illness. Karam et al19 reported that only 10.9% of a nationally representative sample in Lebanon with a 12-month duration of a DSM disorder sought medical treatment, and almost all of it came from the general medical sector. Another study20 in Israel indicated that Jews sought treatment for mental health problems at a much higher rate than Arab Muslims or Christians living in the same regions. A number of studies5,11,21,22 have also suggested that many patients and families sought traditional or religious-based treatment instead of medical treatment, particularly in the case of mental illness or substance use disorders.
This study also shows that substantial numbers of people suffering from the psychological and physical sequelae of trauma are presenting to primary care settings. Respondents reported that victims of domestic violence and patients involved in serious traffic accidents or suffering from the psychological effects of war commonly present for care. Additionally, in Arab countries patients with posttraumatic stress disorder commonly present with somatic symptoms. Therefore, it is very likely that the majority of people with posttraumatic stress disorder are seen only in a primary care setting and are less likely to be identified compared to those seen by psychiatrists.23,24
We also found that several types of violence appear to occur more frequently than commonly believed. These violence types included the abuse of children and the elderly and sexual assault. Because of the culturally sensitive nature of these issues, little regional literature exists that explores these problems in depth. Given the implications for individuals and society, it will be important for the medical systems to engage with their communities to develop interdisciplinary collaborations in legal, religious, and cultural realms to generate consensus on the prevention, evaluation, and solutions for these problems. The adoption of best practices from other world regions may or may not be effective, as they may have unintended consequences if holistic and culturally congruent approaches are not pursued.25
In most Arab countries, traditional and religious healers, community volunteers, and other lay groups have not been integrated into mainstream medical care, and this is confirmed by our survey results. The absence of family and consumer/user community-based organizations and the lack of integration into school systems were also noted in the WHO-AIMS study.4 Mainstream medical practice in the Arab region tends to be more influenced by Western practices and discoveries than by local practices, data, or research. Research to develop a more sophisticated, multidisciplinary understanding of these healing traditions and how best to integrate them into modern medical systems, especially mental health, is required.
In recent years, health authorities in several Arab countries have made changes to improve the quality of the medical services they provide; however, mental health care is often neglected. This survey, for example, highlighted that in many areas, medications to treat psychiatric illness were unavailable in the primary care setting. Reported problems included supply shortages for essential drugs, distribution difficulties, poor quality medications, and high cost. These issues affect care delivery and influence physicians’ sense of self-efficacy and morale.26 Given the widespread reluctance of patients and families to access dedicated psychiatric services, the lack of psychiatric medications in primary care represents an additional barrier to the treatment of mental health conditions.26–29
Many clinicians in the survey also reported that continuing medical education is not required in their practice settings. This may be due to a lack of resources and requires serious attention to ensure that these practitioners continuously update their knowledge.
This study has several limitations. The survey respondent methodology, which while providing important information, may not be generalizable in the larger context. Cultural factors, stigma, or professional bias may affect these psychiatrist and primary care physician respondents. Few women were survey respondents. While this may be because there are fewer women in leadership positions within the health systems of many Arab countries, it also may have biased the responses. Some respondents did not fill out the form completely, leading to missing data. We did not survey all countries in the Arab league. However, it is often difficult to obtain adequate response rates in studies from the region. The WHO-AIMS study,4 for example, received responses from only 14 of the 20 countries surveyed.
The findings in this study indicate a need to continue efforts toward developing global mental health alliances. Clearly, improvements in awareness, education, planning, and resource allocation are necessary. In addition, the development and implementation of culturally appropriate models of understanding and addressing psychiatric issues related to trauma will be important to maximize the cost-effectiveness and sustainability of these interventions. Through these efforts and other partnerships, we hope to develop regional centers of excellence in research and training for trauma-informed mental health services.
Submitted: May 6, 2017; accepted July 26, 2017.
Published online: September 28, 2017.
Potential conflicts of interest: None.
Funding/support: The study was supported by a grant from United Arab Emirates University (grant no. “31M033”2010).
Role of the sponsor: United Arab Emirates University had no role in the design, analysis, interpretation, review, or approval of the manuscript for publication.
REFERENCES
1. World Health Organization. Maternal, child and adolescent mental health: challenges and strategic directions 2010–2015. http://applications.emro.who.int/dsaf/dsa1214.pdf. Accessed August 31, 2017.
2. World Health Organization. Mental health and development: integrating mental health into all development efforts including MDGs. http://www.who.int/mental_health/policy/mhtargeting/mh_policyanalysis_who_undesa.pdf. Accessed August 31, 2017.
3. Programme MHGA. (mhGAP): Scaling Up Care for Mental, Neurological and Substance Use Disorders. Geneva, Switzerland: World Health Organization; 2008.
4. World Health Organization. Mental health systems in the eastern Mediterranean region. http://applications.emro.who.int/dsaf/dsa1219.pdf. Accessed August 31, 2017.
5. Nasser SC, Salamoun MM. Treatment of mental disorders and pathways to care in Arab countries. Int J Psychiatry Clin Pract. 2011;15(1):12–18. PubMed CrossRef
6. Patel V. Mental health in low- and middle-income countries. Br Med Bull. 2007;81-82(1):81–96. PubMed CrossRef
7. Okasha A, Karam E, Okasha T. Mental health services in the Arab world. World Psychiatry. 2012;11(1):52–54. PubMed CrossRef
8. Cohen O, Savaya R. Adjustment to divorce: a preliminary study among Muslim Arab citizens of Israel. Fam Process. 2003;42(2):269–290. PubMed CrossRef
9. Savaya R, Cohen O. Divorce among Moslem Arabs living in Israel comparison of reasons before and after the actualization of the marriage. J Fam Issues. 2003;24(3):338–351. CrossRef
10. Hamid H, Abu-Hijleh NS, Sharif SL, et al. A primary care study of the correlates of depressive symptoms among Jordanian women. Transcult Psychiatry. 2004;41(4):487–496. PubMed CrossRef
11. Daradkeh TK, Alawan A, Al Ma’aitah R, et al. Psychiatric morbidity and its sociodemographic correlates among women in Irbid, Jordan. East Mediterr Health J. 2006;12(suppl 2):S107–S117. PubMed
12. Osman OT, Afifi M. Mental health research in the United Arab Emirates from 1989 to 2008. Asia Pac J Public Health. 2010;22S(3 suppl):48–53. PubMed CrossRef
13. Al-Krenawi A. A study of psychological symptoms, family function, marital and life satisfactions of polygamous and monogamous women: the Palestinian case. Int J Soc Psychiatry. 2012;58(1):79–86. PubMed CrossRef
14. Al-Krenawi A, Graham JR. A comparison of family functioning, life and marital satisfaction, and mental health of women in polygamous and monogamous marriages. Int J Soc Psychiatry. 2006;52(1):5–17. PubMed CrossRef
15. Al-Krenawi A, Graham JR, Al Gharaibeh F. A comparison study of psychological, family function marital and life satisfactions of polygamous and monogamous women in Jordan. Community Ment Health J. 2011;47(5):594–602. PubMed CrossRef
16. Slonim-Nevo V, Al-Krenawi A. Success and failure among polygamous families: the experience of wives, husbands, and children. Fam Process. 2006;45(3):311–330. PubMed CrossRef
17. Nasir LS, Al-Qutob R. Barriers to the diagnosis and treatment of depression in Jordan: a nationwide qualitative study. J Am Board Fam Pract. 2005;18(2):125–131. PubMed CrossRef
18. Amawi N, Mollica RF, Lavelle R, et al. An Annotated bibliography on trauma, mental health, and primary health care in the Middle East. http://hprt-cambridge.org/wp-content/uploads/2014/08/Amawi-et-al-Annoted-Bibliography-Trauma-Middle-East-2014.pdf. Accessed September 5, 2017.
19. Karam EG, Mneimneh ZN, Karam AN, et al. Prevalence and treatment of mental disorders in Lebanon: a national epidemiologic survey. Lancet. 2006;367(9515):1000–1006. PubMed doi:10.1016/S0140-6736(06)68427-4
20. Al-Krenawi A. Mental health service utilization among the Arabs in Israel. Soc Work Health Care. 2002;35(1–2):577–589. PubMed CrossRef
21. Al-Krenawi A, Graham JR, Ophir M, et al. Ethnic and gender differences in mental health utilization: the case of Muslim Jordanian and Moroccan Jewish Israeli out-patient psychiatric patients. Int J Soc Psychiatry. 2001;47(3):42–54. PubMed CrossRef
22. al-Lamki Z, Ohlin C. A community-based study of childhood handicap in Oman. J Trop Pediatr. 1992;38(6):314–316. PubMed CrossRef
23. Farhood LF, Noureddine SN. PTSD, depression, and health status in Lebanese civilians exposed to a church explosion. Int J Psychiatry Med. 2003;33(1):39–53. PubMed CrossRef
24. Ben Thabet J, Sallemi R, Hasïri I, et al. Psycho-emotional impact of a child’s disability on parents [French]. Arch Pediatr. 2013;20(1):9–16. PubMed CrossRef
25. Al-Qutob R, Mawajdeh S, Allosh R, et al. The effect of prenatal knowledge of fetal sex on birth weight: a study from Jordan. Health Care Women Int. 2004;25(3):281–291. PubMed CrossRef
26. Al-Qutob R, Nasir LS. Provider perceptions of reproductive health service quality in Jordanian public community health centers. Health Care Women Int. 2008;29(5):539–550. PubMed CrossRef
27. AbuMadini MS, Rahim SI. Psychiatric admission in a general hospital: patients profile and patterns of service utilization over a decade. Saudi Med J. 2002;23(1):44–50. PubMed
28. Al-Adawi S, Dorvlo ASS, Al-Ismaily SS, et al. Perception of and attitude towards mental illness in Oman. Int J Soc Psychiatry. 2002;48(4):305–317. PubMed CrossRef
29. Eapen V, Ghubash R. Help-seeking for mental health problems of children: preferences and attitudes in the United Arab Emirates. Psychol Rep. 2004;94(2):663–667. PubMed CrossRef
This PDF is free for all visitors!

