Vitamin D Deficiency Among Psychiatric Inpatients

ABSTRACT
Objective: Previous studies in northern Europe and Australia have indicated that vitamin D deficiency is common in psychiatric patients. This study aimed to determine the prevalence of vitamin D deficiency among psychiatric inpatients in a large North American city. The association of vitamin D status with clinical characteristics was also explored, and subgroups of patients that are more vulnerable to vitamin D deficiency were identified.
Method: This descriptive study looked at 107 unselected consecutive admissions to a psychiatric inpatient service in New York City between September and early December 2010. All patients were aged 18 years and older. Psychiatric diagnoses were established by attending psychiatrists as part of the routine assessment using criteria from the DSM-IV. Serum levels of 25-hydroxyvitamin D were measured by high-performance liquid chromatography, tandem mass spectrometry. A vitamin D-deficient state was defined as serum 25-hydroxyvitamin D level ≤ 20 ng/mL.
Results: Fifty-six (52.3%) patients were classified as deficient in vitamin D. Age and 25-hydroxyvitamin D level were significantly correlated (P = .001). Seventy-one percent of patients from age 18 to 34 years were deficient in vitamin D; this rate was significantly higher than the rate of deficiency in older patients (P = .017). No significant relationships were found between 25-hydroxyvitamin D level and gender, race/ethnicity, glycosylated hemoglobin, body mass index, and major psychiatric diagnostic categories.
Conclusions: A high percentage of psychiatric inpatients are deficient in vitamin D. Younger patients were more at risk for deficiency. Screening for vitamin D deficiency should be part of the health assessment of patients with major psychiatric illnesses.
Prim Care Companion CNS Disord 2012;14(2):doi:10.4088/PCC.11m01230
© Copyright 2012 Physicians Postgraduate Press, Inc.
Submitted: June 10, 2011; accepted September 9, 2011.
Published online: April 19, 2012.
Corresponding author: Robert E. McCue, MD, Department of Psychiatry, Woodhull Medical & Mental Health Center, New York University School of Medicine, 760 Broadway, Brooklyn, NY 11206 ([email protected]).
Vitamin D deficiency has been reported to be a prevalent contemporary health problem with consequences beyond abnormalities in bone, calcium, and phosphorus metabolism. A deficiency in vitamin D has been associated with certain cancers (breast, colon, prostate), autoimmune disorders, and cardiovascular disease.1 In addition, the mental health consequences of vitamin D deficiency are also becoming clearer. Insufficient vitamin D has been linked to depressive symptoms,2-7 cognitive impairment,8-10 and the development of schizophrenia.11 There is evidence that vitamin D deficiency is also related to medical problems1 such as obesity, diabetes mellitus, and hypertension, to which patients with psychiatric illnesses are particularly vulnerable.
While screening patients with psychiatric disorders for medical problems has been recognized as valuable, vitamin D sufficiency is not routinely included as part of the screening. However, there is evidence that such screening should be included. The prevalence of vitamin D deficiency among Scandinavian outpatients with psychiatric disorders has been reported to be 56%12 and 67%.13 Among 53 inpatients at a private clinic in Australia, 58% were vitamin D deficient.14 More alarming, Tiangga et al15 found that 100% of 17 hospitalized male psychiatric inpatients in London, England, were vitamin D deficient, while Cardinal and Gregory16 found deficiency in 83% of 12 hospitalized elderly psychiatric inpatients in Cambridge, United Kingdom. In all of these studies, deficiency was defined in the generally accepted manner17 as a serum 25-hydroxyvitamin D (25-[OH]D) level ≤ 20 ng/mL (50 nmol/L). All studies concluded with the recommendation that psychiatric patients, particularly hospitalized patients, should be screened for vitamin D deficiency.
This descriptive study looked at a large number of newly admitted psychiatric inpatients in an impoverished urban area in New York City to examine whether a high rate of vitamin D deficiency in psychiatric patients is also present in North America. The main objective was to quantify the prevalence of vitamin D deficiency in this group in order to guide the modification of health risk screening procedures. A secondary objective was to identify subgroups of patients in this population that are more vulnerable to vitamin D deficiency.
METHOD
Setting
The survey took place in a 135-bed psychiatric inpatient service that treats acutely ill adult patients and is part of a 363-bed general hospital. The hospital serves an impoverished urban population in New York City. Data were collected between September 2010 and the first 2 weeks of December 2010.
Patients
The patients were unselected consecutive cases, who were admitted to 3 of the 6 units of the psychiatric inpatient service. All patients were aged 18 years or older. Psychiatric diagnoses were established by attending psychiatrists as part of the routine assessment using criteria from the DSM-IV. All patients received a complete medical assessment at admission.
Laboratory Analyses
Serum 25-(OH)D was analyzed by high-performance liquid chromatography, tandem mass spectrometry (Quest Diagnostics, Teterboro, New Jersey). Both 25-(OH)D2 (from ergocalciferol) and 25-(OH)D3 (from cholecalciferol) were measured.
Statistical Analyses
Patients with a serum 25-(OH)D level ≤ 20 ng/mL were classified as deficient. Statistical analysis was performed using SOFA Statistics version 1.1.0 (Paton-Simpson and Associates Ltd, Auckland, New Zealand, 2011). The significance level was .05, 2-sided. Group differences were analyzed using either the Student t test or analysis of variance. These tests are robust for deviations from normality. Correlations between continuous variables were analyzed using the Pearson test of linear correlation.

- Vitamin D deficiency has metabolic and mental health consequences beyond abnormalities in bone metabolism.
- Current evidence suggests that vitamin D deficiency is prevalent among patients with psychiatric disorders.
- Screening for vitamin D deficiency should be part of the health assessment of patients with major psychiatric illnesses.
Ethics
After previous random sampling suggested that vitamin D deficiency might be prevalent among our patients, a decision was made to assess vitamin D status on all admissions. This decision was made on clinical grounds and was independent of this study. This study is an examination of the results of that decision. As the review of the data did not interfere with patient care and personal health information was safeguarded, this study was deemed exempt from institutional review board approval. As is standard practice, all patients were orally informed about the testing for vitamin D status, presented with their results, and treated with vitamin D when appropriate.
RESULTS
Patient Characteristics
The study included 107 patients. Of these, 70 (65.4%) were men and 37 (34.6%) were women. The mean ± SD age was 43.3 ± 15.8 years, with a range of 18 to 78 years. Fifty-eight (54.2%) were black, 32 (29.9%) were Latino, and 17 (15.9%) were white. Sixty patients were diagnosed as having a psychotic disorder: 30 (28.0%) with schizophrenia, 24 (22.4%) with schizoaffective disorder, 4 (3.7%) with psychotic disorder not otherwise specified, and 2 (1.9%) with substance-induced psychotic disorder. Forty-three patients were diagnosed with a mood disorder: 24 (22.4%) with bipolar disorder, 16 (15.0%) with major depressive disorder, 2 (1.9%) with substance-induced mood disorder, and 1 (0.9%) with dysthymic disorder. Other diagnoses were dementia (n=2, 1.9%) and impulse control disorder not otherwise specified (n=2, 1.9%). Six (5.6%) patients were taking oral vitamin D at the time of admission; they were included in the analysis.
Medical Issues
Twenty-seven (25.2%) patients had Type 2 diabetes mellitus and 33 (30.8%) had hypertension. The mean ± SD body mass index (BMI) was 29.2 ± 7.3 kg/m2; 38 (35.5%) patients were classified as obese, with a BMI ≥ 30 kg/m2. The mean ± SD glycosylated hemoglobin (hemoglobin A1c) level was 5.9% ± 1.2%.
Serum 25-Hydroxyvitamin D Level
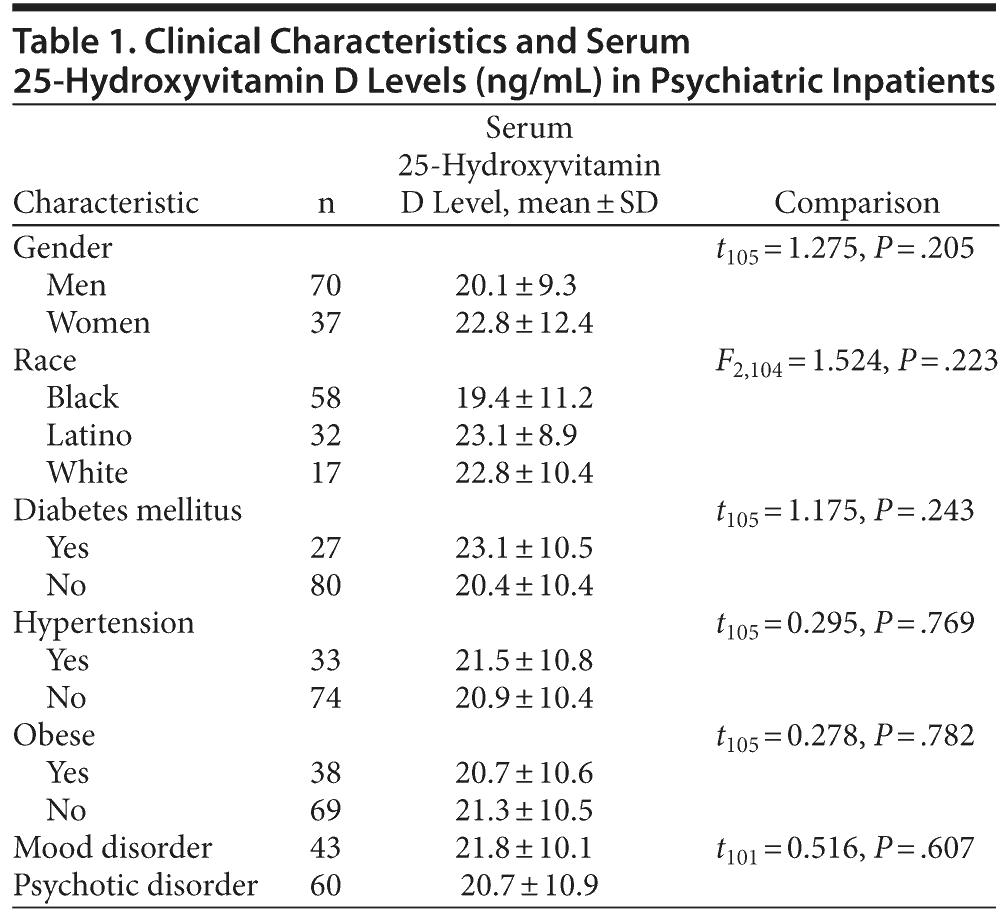
The mean ± SD serum 25-(OH)D level was 21.1 ± 10.4 ng/mL; the median was 19.0 ng/mL, with a range of 5.0 to 63.0. Fifty-six (52.3%) patients were classified as deficient. There was a statistically significant correlation between serum 25-(OH)D level and age (Pearson r = 0.31, df = 105, P = .001) but not between 25-(OH)D and BMI (Pearson r = −0.10, df = 105, P = .30) or hemoglobin A1c (Pearson r = −0.01, df = 90, P = .91). Table 1 shows that there were no statistically significant differences in 25-(OH)D levels when examining gender, race/ethnicity, major psychiatric diagnoses, and the presence or absence of Type 2 diabetes mellitus, hypertension, and obesity.
Twenty-nine patients (27.1%) had a detectable level of 25-(OH)D2 that is assumed to be from nutritional supplements rather than from sun exposure; the mean ± SD serum level was 2.82 ± 6.13 ng/mL. For 25-(OH)D3, the mean ± SD serum level was 18.25 ± 9.14 ng/mL. Patients who had detectable 25-(OH)D2 levels were significantly less likely to be deficient in vitamin D (χ21 = 19.64, P < .0001) than those with nondetectable levels. Fifty-one (65.4%) patients without detectable 25-(OH)D2 levels were deficient compared to 5 (17.2%) patients who had detectable levels.
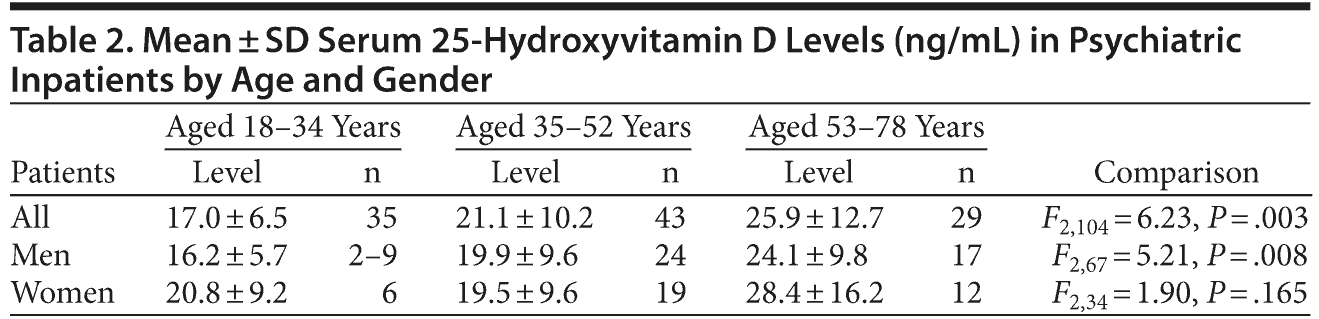
Table 2 shows serum 25-(OH)D levels among the age categories, which were also used in the study by Humble et al.12 There was a statistically significant difference among the 3 age groups, with the youngest group having the lowest level. When the age groups were divided by gender, only the male patients had significantly different serum 25-(OH)D levels among them, with the youngest having the lowest levels. Pairwise comparisons of the age groups for male patients showed that the youngest group had significantly lower serum 25-(OH)D levels compared to both the middle (t = 2.53, df = 51, P = .014) and oldest (t = 3.44, df = 44, P = .001) age groups. The difference in levels between the middle and oldest age group in male patients was not significant (t = −0.60, df = 39, P = .55). There was also a statistically significant relationship between a patient’s age group and being classified as deficient in vitamin D (χ22 = 8.11, P = .017), with 71.4% (25/35) of the youngest age group being deficient, while the middle and oldest age groups had deficiency rates of 46.5% (20/43) and 37.9% (11/29), respectively. Again, this comparison was significant for male patients (χ22 = 8.59, P = .014) but not female patients (χ22 = 0.14, P = .93).
DISCUSSION
This is the first study looking at the prevalence of vitamin D deficiency among psychiatric patients in North America. The majority (52.3%) of our unselected sample of psychiatric inpatients was deficient in vitamin D. These results are similar to studies that have looked at psychiatric patients in northern Europe and Australia. Recently, the National Center for Health Statistics reported18 that the mean prevalence of 25-(OH)D levels ≤ 20 ng/mL in the US general population, aged 19 years and older, was 37.5%. The results from our study suggest that the level of deficiency, already high among North Americans, is even higher among patients with major psychiatric illness. Some experts in the field propose that the 25-(OH)D level must be greater than 30 ng/mL to be sufficient19; with those criteria, 91 (85.0%) patients in our sample would be classified as deficient.
The majority of our patients had dark skin, which is considered a risk factor for vitamin D deficiency, as more sun exposure is needed to maintain adequate blood levels. Dealberto20 has hypothesized a connection between having dark skin, being an immigrant, and having a greater risk of schizophrenia. Vitamin D deficiency is thought to be an important part of this connection. Black patients did have the lowest levels of 25-(OH)D in our sample, but this difference was not statistically significant.
The amount of 25-(OH)D is related to sun exposure. Levels fluctuate during the year with the highest from the sunlight of summer. As there is a 1-month to 2-month lag between changes in sun exposure and 25-(OH)D level,6 the samples in our patients, which were collected in autumn, most likely represent 25-(OH)D levels near their annual peak.
Increased age has been linked to vitamin D deficiency. However, in our study, younger patients, particularly younger males, had significantly lower 25-(OH)D levels and a higher prevalence of being vitamin D deficient. Humble et al12 found similar results. Our sample had a small number of younger female patients, so no valid comparison can be made between genders in the younger age group. We can only speculate as to why younger psychiatric patients are more likely to be deficient in vitamin D. Perhaps younger patients have a lifestyle that exposes them to less sunlight and a diet with less vitamin D content than older patients. Another possible explanation is that more younger patients may have been taking medications such as anticonvulsants, steroids, or highly active antiretroviral therapy that enhance the destruction of 25-(OH)D. However, since many of our patients reported that they had not taken medication consistently before being admitted to the hospital, we do not have adequate data to test this hypothesis.
The connections between vitamin D deficiency and obesity, hypertension, and type 2 diabetes mellitus are demonstrated in our patient population who had a high prevalence of these medical illnesses. Obesity is a risk factor for lower 25-(OH)D levels1 as well as for type 2 diabetes mellitus and hypertension; lower 25-(OH)D levels result in less insulin production and increased renin synthesis,1 which increases vulnerability to developing type 2 diabetes mellitus and hypertension. Renal damage from diabetes mellitus or hypertension can decrease synthesis of 1,25-dihydroxyvitamin D, the active metabolite of vitamin D. These relationships highlight the value of assessing vitamin D status when managing chronic health problems such as obesity, hypertension, and type 2 diabetes mellitus.
The single site of this study is a limitation to generalizing the results. Another limitation is that an adequate level of 25-(OH)D and the best means of assaying it have not been definitively established. While some experts recommend using a higher cutoff value to determine deficiency, others believe it should be lower. As a result, our rates of deficiency may be higher or lower depending on how deficiency is defined.
In conclusion, vitamin D deficiency was highly prevalent in our sample of psychiatric inpatients. These results are in agreement with other studies and support our decision to screen for vitamin D deficiency as a part of the health assessment of patients with major psychiatric illnesses. Since most patients are deficient in vitamin D, a cost-efficient alternative to screening may be to treat all patients with pharmacologic doses of vitamin D (50,000 IU of ergocalciferol). Pietras et al21 looked at patients treated with ergocalciferol for up to 6 years and found it helpful in maintaining sufficient levels of 25-(OH)D without toxic effects. Identifying and treating vitamin D deficiency may provide many benefits to our patients, including having a positive effect on the psychiatric illness itself. However, further studies are needed to validate the latter point.
Author affiliations: Department of Psychiatry, Woodhull Medical and Mental Health Center, New York University School of Medicine, Brooklyn, New York.
Potential conflicts of interest: None reported.
Funding/support: None reported.
REFERENCES
1. Holick MF. Vitamin D deficiency. N Engl J Med. 2007;357(3):266-281. PubMed doi:10.1056/NEJMra070553
2. Stewart R, Hirani V. Relationship between vitamin D levels and depressive symptoms in older residents from a national survey population. Psychosom Med. 2010;72(7):608-612. PubMed doi:10.1097/PSY.0b013e3181e9bf15
3. Ganji V, Milone C, Cody MM, et al. Serum vitamin D concentrations are related to depression in young adult US population: the Third National Health and Nutrition Examination Survey. Int Arch Med. 2010;3(1):29. PubMed doi:10.1186/1755-7682-3-29
4. Milaneschi Y, Shardell M, Corsi AM, et al. Serum 25-hydroxyvitamin D and depressive symptoms in older women and men. J Clin Endocrinol Metab. 2010;95(7):3225-3233. PubMed doi:10.1210/jc.2010-0347
5. May HT, Bair TL, Lappé DL, et al. Association of vitamin D levels with incident depression among a general cardiovascular population. Am Heart J. 2010;159(6):1037-1043. PubMed doi:10.1016/j.ahj.2010.03.017
6. Humble MB. Vitamin D, light and mental health. J Photochem Photobiol B. 2010;101(2):142-149. PubMed doi:10.1016/j.jphotobiol.2010.08.003
7. Parker G, Brotchie H. ‘ D’ for depression: any role for vitamin D? ‘ Food for Thought’ II. Acta Psychiatr Scand. 2011;124(4):243-249. doi:10.1111/j.1600-0447.2011.01705.x
8. Annweiler C, Schott AM, Allali G, et al. Association of vitamin D deficiency with cognitive impairment in older women: cross-sectional study. Neurology. 2010;74(1):27-32. PubMed doi:10.1212/WNL.0b013e3181beecd3
9. Buell JS, Dawson-Hughes B, Scott TM, et al. 25-Hydroxyvitamin D, dementia, and cerebrovascular pathology in elders receiving home services. Neurology. 2010;74(1):18-26. PubMed doi:10.1212/WNL.0b013e3181beecb7
10. Llewellyn DJ, Lang IA, Langa KM, et al. Vitamin D and risk of cognitive decline in elderly persons. Arch Intern Med. 2010;170(13):1135-1141. PubMed doi:10.1001/archinternmed.2010.173
11. McGrath JJ, Eyles DW, Pedersen CB, et al. Neonatal vitamin D status and risk of schizophrenia: a population-based case-control study. Arch Gen Psychiatry. 2010;67(9):889-894. PubMed doi:10.1001/archgenpsychiatry.2010.110
12. Humble MB, Gustafsson S, Bejerot S. Low serum levels of 25-hydroxyvitamin D (25-OHD) among psychiatric out-patients in Sweden: relations with season, age, ethnic origin and psychiatric diagnosis. J Steroid Biochem Mol Biol. 2010;121(1-2):467-470. PubMed doi:10.1016/j.jsbmb.2010.03.013
13. Berg AO, Melle I, Torjesen PA, et al. A cross-sectional study of vitamin D deficiency among immigrants and Norwegians with psychosis compared to the general population. J Clin Psychiatry. 2010;71(12):1598-1604. PubMed doi:10.4088/JCP.09m05299yel
14. Berk M, Jacka FN, Williams LJ, et al. Is this D vitamin to worry about? vitamin D insufficiency in an inpatient sample. Aust N Z J Psychiatry. 2008;42(10):874-878. PubMed doi:10.1080/00048670802345516
15. Tiangga E, Gowda A, Dent JA. Vitamin D deficiency in psychiatric in-patients and treatment with daily supplements of calcium and ergocalciferol. Psychiatr Bull. 2008;32(10):390-393. doi:10.1192/pb.bp.107.019109
16. Cardinal RN, Gregory CA. Osteomalacia and vitamin D deficiency in a psychiatric rehabilitation unit: case report and survey. BMC Res Notes. 2009;2(1):82. PubMed doi:10.1186/1756-0500-2-82
17. Holick MF, Binkley NC, Bischoff-Ferrari HA, et al; Endocrine Society. Evaluation, treatment, and prevention of vitamin D deficiency: an Endocrine Society clinical practice guideline. J Clin Endocrinol Metab. 2011;96(7):1911-1930. PubMed doi:10.1210/jc.2011-0385
18. Looker AC, Johnson CL, Lacher DA, et al. Vitamin D Status: United States 2001-2008. NCHS data brief, no 59. Hyattsville, MD: National Center for Health Statistics; 2011.
19. Henry HL, Bouillon R, Norman AW, et al. 14th Vitamin D Workshop consensus on vitamin D nutritional guidelines. J Steroid Biochem Mol Biol. 2010;121(1-2):4-6. PubMed doi:10.1016/j.jsbmb.2010.05.008
20. Dealberto MJ. Ethnic origin and increased risk for schizophrenia in immigrants to countries of recent and longstanding immigration. Acta Psychiatr Scand. 2010;121(5):325-339. PubMed doi:10.1111/j.1600-0447.2009.01535.x
21. Pietras SM, Obayan BK, Cai MH, et al. Vitamin D2 treatment for vitamin D deficiency and insufficiency for up to 6 years. Arch Intern Med. 2009;169(19):1806-1808. PubMed doi:10.1001/archinternmed.2009.361