Objective: We examined health care utilization, clinical profiles (such as sociodemographic features, clinical severity), and outcomes (inpatient admission, revisit within 24 hours of discharge) of patients who were admitted to a 23-hour observation unit within the emergency service of a tertiary psychiatric hospital and hypothesized that a specific clinical profile (greater clinical severity, lower psychosocial functioning) predicted subsequent inpatient hospitalization.
Method: The medical records of all patients admitted to the observation unit from February 5, 2007, to February 4, 2012 (N = 2,158) were assessed for relevant data. Clinical severity and level of psychosocial functioning were assessed using Clinical Global Impressions-Severity (CGI-S) and Global Assessment of Functioning (GAF) scales, respectively.
Results: Overall, the patients seen were predominantly Chinese males > 36 years old who had diagnoses including stress-related, anxiety, affective spectrum, and psychotic disorders. The clinical severity score (CGI-S) improved significantly following discharge from the observation unit (t1,1848 = 23.316; P < .001). Logistic regression analyses revealed that self-referred (P = .001), older patients (P = .007) with past psychiatric history (P = .019), lower GAF scores (P = .025), and less improvement of CGI-S scores (P = .001) were associated with inpatient admission after a 23-hour stay in the observation unit.
Conclusions: Our study findings affirmed our hypothesis and supported the utility of the observation unit in monitoring the overall clinical status of patients, which was linked with subsequent inpatient admissions. Better management of these patients at the outpatient level can potentially decrease unnecessary hospitalization and reduce health care cost as well as illness burden on patients and caregivers.
The 23-Hour Observation Unit Admissions Within the
Emergency Service at a National Tertiary Psychiatric Hospital:
Clarifying Clinical Profiles, Outcomes, and
Predictors of Subsequent Hospitalization
ABSTRACT
Objective: We examined health care utilization, clinical profiles (such as sociodemographic features, clinical severity), and outcomes (inpatient admission, revisit within 24 hours of discharge) of patients who were admitted to a 23-hour observation unit within the emergency service of a tertiary psychiatric hospital and hypothesized that a specific clinical profile (greater clinical severity, lower psychosocial functioning) predicted subsequent inpatient hospitalization.
Method: The medical records of all patients admitted to the observation unit from February 5, 2007, to February 4, 2012 (N = 2,158) were assessed for relevant data. Clinical severity and level of psychosocial functioning were assessed using Clinical Global Impressions–Severity (CGI-S) and Global Assessment of Functioning (GAF) scales, respectively.
Results: Overall, the patients seen were predominantly Chinese males > 36 years old who had diagnoses including stress-related, anxiety, affective spectrum, and psychotic disorders. The clinical severity score (CGI-S) improved significantly following discharge from the observation unit (t1,1848 = 23.316; P < .001). Logistic regression analyses revealed that self-referred (P = .001), older patients (P = .007) with past psychiatric history (P = .019), lower GAF scores (P = .025), and less improvement of CGI-S scores (P = .001) were associated with inpatient admission after a 23-hour stay in the observation unit.
Conclusions: Our study findings affirmed our hypothesis and supported the utility of the observation unit in monitoring the overall clinical status of patients, which was linked with subsequent inpatient admissions. Better management of these patients at the outpatient level can potentially decrease unnecessary hospitalization and reduce health care cost as well as illness burden on patients and caregivers.
Prim Care Companion CNS Disord 2015;17(4):doi:10.4088/PCC.15m01789
© Copyright 2015 Physicians Postgraduate Press, Inc.
Submitted: January 22, 2015; accepted March 24, 2015.
Published online: July 16, 2015.
Corresponding author: Kang Sim, MBBS, MMed, MScHPE, FAMS, Department of General Psychiatry, Institute of Mental Health/Woodbridge Hospital, 10, Buangkok View, Singapore 539747 ([email protected]).
At present, the option of brief psychiatric hospitalization can be provided through the twin roles of the hospital emergency room (ER) services.1–3 For example, the ER may include psychiatric holding beds, with the capacity to observe a patient in the ER for up to 23 hours,2 or crisis beds, which allow brief stays that seek to reduce unnecessary admissions to the inpatient psychiatric unit.2–6 There is evidence that brief hospitalizations are associated with tangible benefits for both the service users and providers.1–5,7–11 For example, the patients gain earlier functional independence following rapid stabilization and reduction of psychiatric symptoms, including self-harm behavior.4,8 Patients discharged from brief hospitalization can more immediately utilize community resources, which can decrease the chances of subsequent rehospitalization. In addition, brief hospitalization has been associated with a higher level of patient satisfaction with treatment as well as a reduction in waste of hospital resources.4,5,8,12 A Cochrane review13 of extant studies on brief hospitalization concluded that it was associated with better outcomes in discouraging revolving readmissions, promoting better coordinated care for patients with severe mental illnesses. Breslow et al4 reported that most patients admitted for brief hospitalization were diagnosed with schizophrenia or personality disorder. Previous studies found that clinical factors such as suicidality, danger to others, severity of psychiatric symptoms, and a diagnosis of psychotic disorder were associated with increased rates of psychiatric inpatient admissions.14–19 However, data are scant regarding clinical outcomes of patients who require brief psychiatric hospitalization including changes in clinical severity or subsequent hospitalization.
Based on extant data, in our study, we sought to examine clinical profiles (sociodemographic features, clinical severity, psychosocial functioning) and outcomes (inpatient admission, revisit to ER within 24 hours following discharge from brief hospitalization) of patients admitted under brief hospitalization termed as the observation unit within the ER at a national tertiary psychiatric hospital in Singapore. We hypothesized that a specific clinical profile (greater clinical severity, lower psychosocial functioning) predicted subsequent inpatient hospitalization.
METHOD
This retrospective study examined the clinical profiles and outcomes of patients admitted to our observation unit in the ER and aimed to determine specific factors that may predict subsequent hospitalization. The Institute of Mental Health is the only tertiary psychiatric hospital in Singapore with 2,000 inpatient beds, which serves a local population of 5.2 million people. The hospital started a 6-bed 23-hour observation unit within its emergency services in 2007.
The observation unit services provide acute and crisis intervention for emotionally and mentally disturbed patients, whose conditions are not clinically assessed to be of sufficient severity or risk to require inpatient admission. Patients who present to the ER are offered observation unit admission if they fulfill the inclusion criteria (Table 1). Following intake assessment by a medical officer, the patients are subsequently reviewed by a specialist for further management decisions such as discharge with review appointments at the outpatient clinic or transfer to an inpatient ward. Additional interventions by a medical social worker or a counselor are also offered if deemed necessary. At the time of discharge from the observation unit, the patients are also provided information about available community support services and are advised about the need to return for review.

Study Sample and Data Collection
The study sample comprised 2,158 patients admitted to the observation unit among 71,420 ER admissions during the same time period (from February 5, 2007, to February 4, 2012). The data were extracted from the available hospital records and included sociodemographic information (age, gender), clinical features (mode of referral, past psychiatric history, diagnosis), clinical assessment scores (Clinical Global Impressions–Severity scale [CGI-S] at admission,20 Global Assessment of Functioning scale [GAF]21), and outcome factors (CGI-S scores at discharge, revisit to ER within 24 hours after discharge from the observation unit). The interviewer-rated CGI-S assesses the clinical severity of the patient at admission and discharge from the observation unit and has a score range from 0 to 6, with a higher score indicating greater illness severity. The clinician-rated GAF assesses the severity of psychopathology and level of psychosocial and occupational functioning of each patient and has a score range from 0 to 100, with a higher score indicating a better level of psychosocial functioning. This study was reviewed by the institutional review board of our hospital (project was deemed to be a clinical audit study) and approved by the chairman of the medical board, Institute of Mental Health, Singapore.
Data Analysis
All statistical analyses were performed using the Statistical Package for the Social Sciences, version 16 (SPSS Inc, Chicago, Illinois). Frequency analysis was done to determine the percentage of categorical variables such as gender, diagnosis, mode of referral, past psychiatric history, CGI-S score, age group and GAF group, outcome from the observation unit, and revisits to the ER within 24 hours. Paired t tests were performed for statistical comparisons of noncategorical factors such as CGI-S scores at admission and discharge from the observation unit. For comparisons of more than 2 groups of patients, 1-way analysis of variance was used. The χ2 test was performed for comparisons of categorical data. Logistic regression analysis was done to determine the predictors of subsequent inpatient admission from the outpatient unit.
RESULTS
Clinical Profile of the Patients
The sociodemographic and clinical characteristics of 2,158 patients admitted to the observation unit over the 5-year period are shown in Table 2. We found that 12.2% and 14.4% of the CGI-S scores at admission to and discharge from the observation unit, respectively, were not recorded in the forms. Overall, the subjects were predominately male (64%) and relatively young, with a mean ± age of 36.38 ± 14.65 years. Among the 3 diagnostic categories, about half of the subjects had mood, anxiety, and stress disorders, while those with psychotic disorders constituted 20.7% of the sample. More than half of the patients (57.7%) had past known psychiatric history and contacts with the hospital. A substantial proportion of the patients were self-referred (44.5%), but the majority (55.2%) were referred from other hospitals and agencies such as the police (519 subjects, 24.1%), accident and emergency departments of other hospitals (269 subjects, 12.5%), step-down facilities (159 subjects, 7.4%), the Singapore Armed Forces (154 subjects, 7.1%), and other sources of referral (90 subjects, 4.2%).
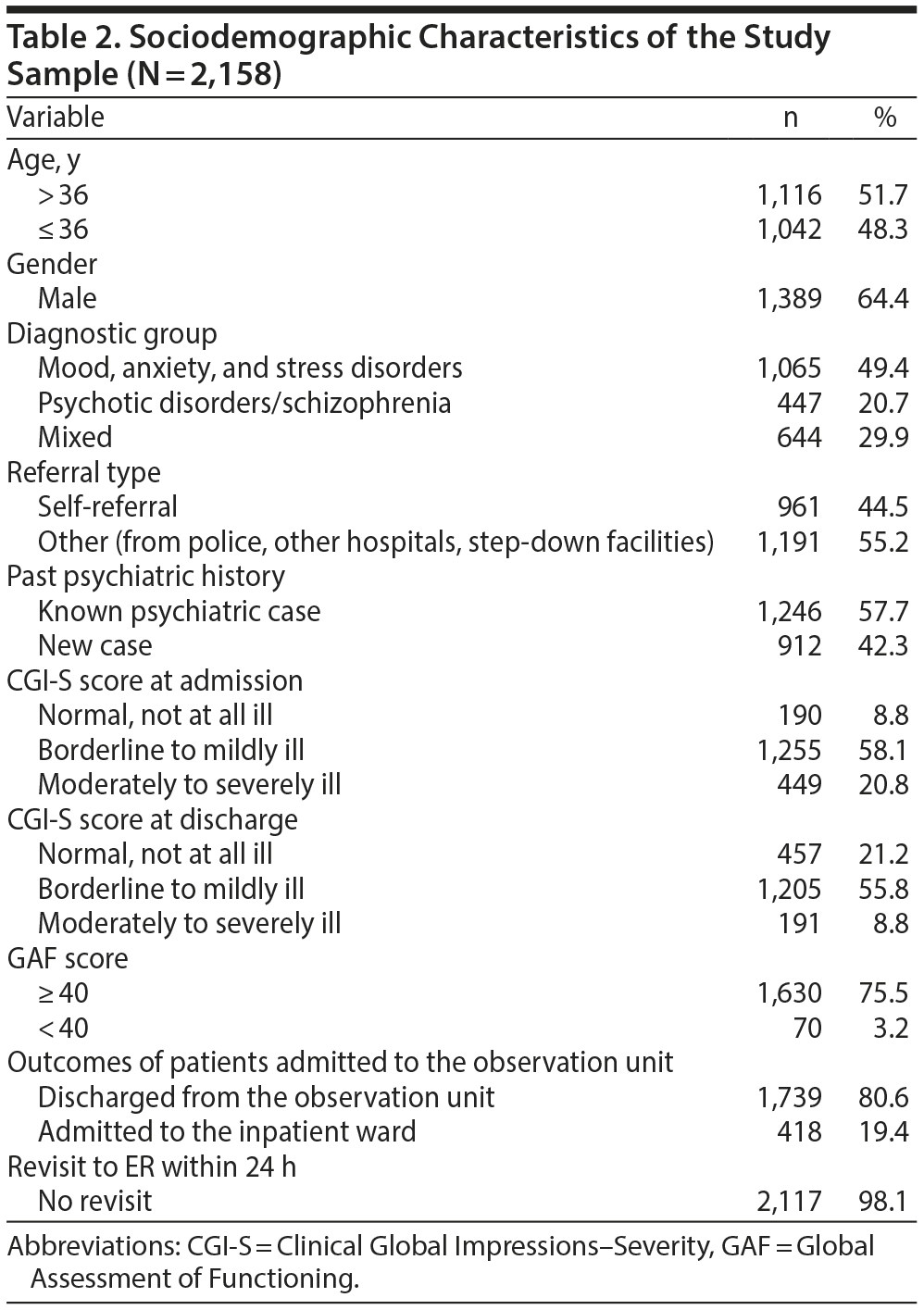
More than half of the patients had CGI-S scores in the range of borderline (34.4%) or mildly (23.7%) mentally ill, while one-fifth were within the range of moderately-severely mentally ill at admission.
Comparisons of Patients Discharged From the Observation Unit Versus Admitted to the Hospital
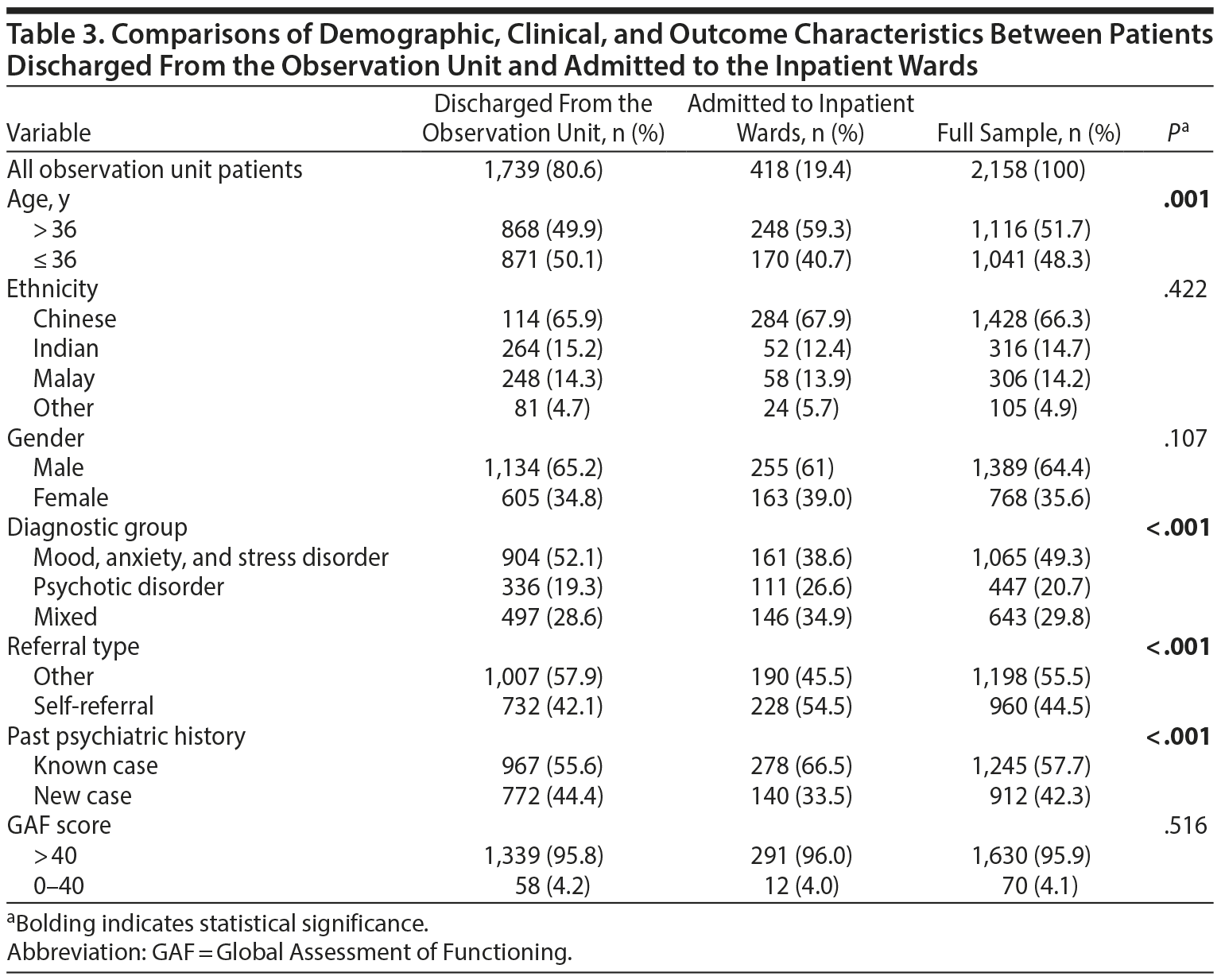
Overall, the CGI-S score improved significantly following discharge from the observation unit (t1,1848 = 23.316, P < .001). Table 3 shows the demographic, clinical, and outcome characteristics of patients discharged from the observation unit versus those who were admitted to inpatient wards. Older (P = .001), self-referred (P < .001) patients with past psychiatric history (P < .001) and with specific diagnoses such as psychotic disorders (P < .001) were more likely to be hospitalized from the observation unit. Logistic regression analysis found that older age (> 36 years old; P = .007; Exp[B] = 1.57; 95% CI, 1.13–2.17), self-referred patients (P = .001; Exp[B] = 1.84; 95% CI, 1.34–2.53) with past psychiatric history (P = .019; Exp[B] = 1.52; 95% CI, 1.07–2.15), lower level of psychosocial functioning (P = .025; Exp[B] = 2.45; 95% CI, 1.18–5.38), and less improvement on CGI-S score while in the observation unit (P = .001; Exp[B] = 5.35; 95% CI, 4.20–6.80) predicted subsequent hospitalization.
Comparisons of Patients Revisiting the ER Versus
Nonrevisits 24 Hours After Observation Unit Discharge
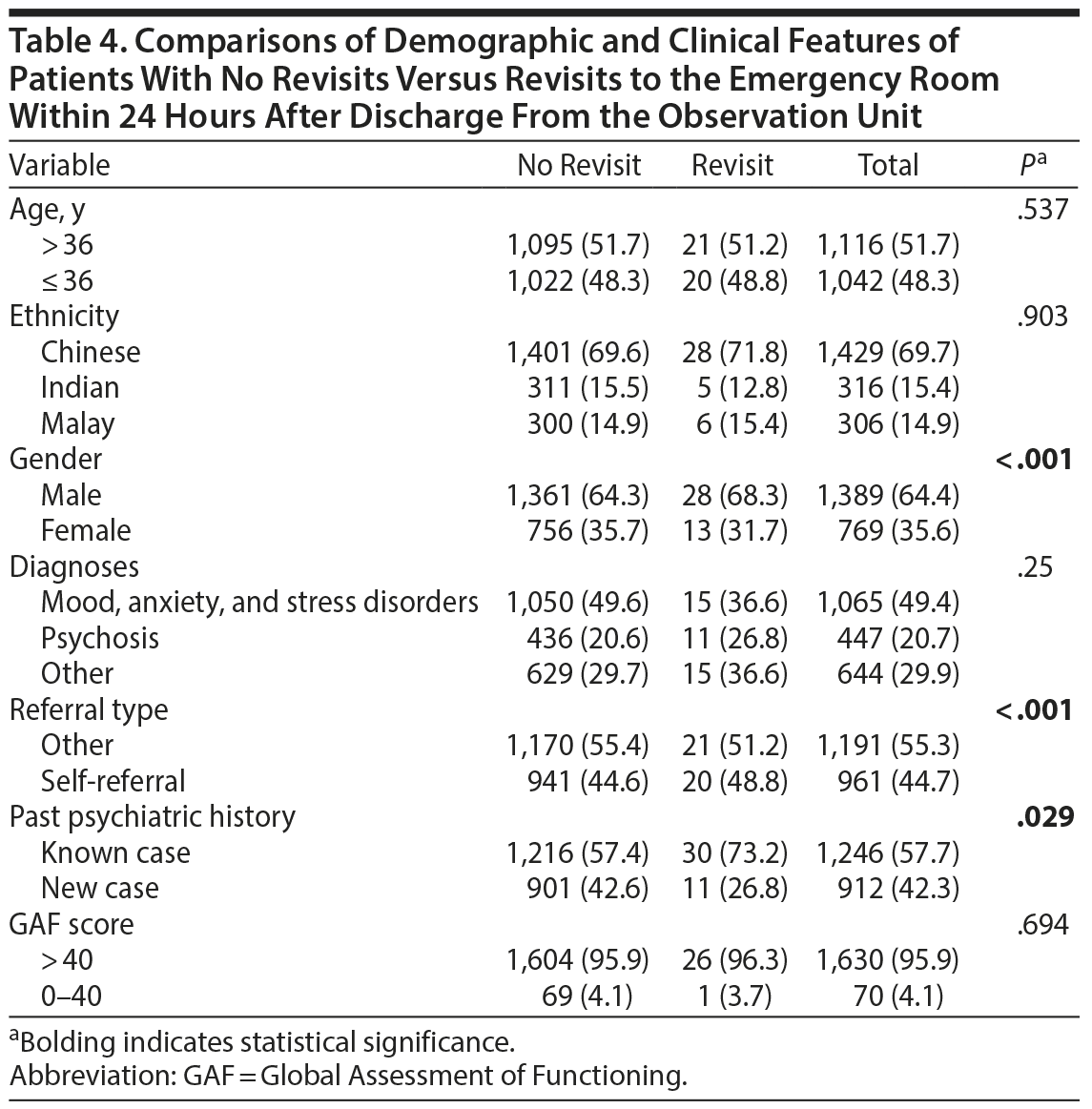
Table 4 shows comparisons of the demographic and clinical data of patients revisiting the ER within 24 hours after discharge from the observation unit versus nonrevisits. Only 1.9% revisited the ER within 24 hours after discharge (Table 2). Male patients (P < .001) who were self-referred (P < .001) and with a past psychiatric history (P < .029) were more likely to revisit the ER within 24 hours after discharge from the observation unit.
DISCUSSION
There were several main findings that affirmed our a priori hypothesis. First, the CGI-S score improved significantly following discharge from the observation unit. Second, self-referred, older patients with a past psychiatric history, lower GAF score, and less clinical improvement were associated with inpatient admission after a 23-hour stay in the observation unit. Third, male, self-referred patients with a past known psychiatric history were more likely to revisit the ER within 24 hours after discharge from the observation unit.
Patients initially admitted to the observation unit were predominately adult males. Overt aggression and impulsive behavior are generally more common in male patients, especially those presenting with psychotic spectrum disorders and psychiatric comorbidities including alcohol or substance abuse/dependence and personality disorders.22 The community has a lower tolerance for even mildly aggressive behavior among males compared with females, resulting in relatively higher admissions for men.23 In addition, male patients who tend to have higher rates of alcohol and substance use disorders are more likely to come to the attention of the police and may be referred for psychiatric evaluation with subsequent admission to the hospital including the observation unit.24 Mood, anxiety, and stress disorders were the most common diagnoses in patients admitted to the observation unit. An earlier national mental health study in Singapore showed that the most common mental disorders in the community were major depressive disorder at 6.3%, alcohol abuse at 3.5%, and obsessive-compulsive disorder at 3.0%.25 Patients presenting with stress disorders can improve relatively quickly following treatment and a brief respite in the observation unit.4 Patients with such disorders and their families also are more likely to agree to admission to the observation unit rather than acute inpatient wards, wherein more disturbed and unwell patients are placed.26 Patients with psychotic disorders can benefit from observation unit admission for a variety of reasons including extrapyramidal side effects and poor adjustment to external stressors.4 In cases in which patients have a relapse of psychosis, there is increased likelihood of admission directly to inpatient wards,19 as these patients often have a concomitant lower level of psychosocial functioning and more severe clinical illness, as was found in our study even after a brief stay in the observation unit.
In our study, the clinical severity of patients at admission to the observation unit was predominantly borderline to mildly ill (rated on the CGI-S), and they were observed to have a higher level of psychosocial functioning (rated on the GAF). The significant improvement of CGI-S scores following discharge and the observation that most of the patients (80.6%) were discharged from the observation unit within 23 hours of admission suggest that observation unit admission may be beneficial in patients with less severe clinical manifestations of their psychiatric conditions.
Our findings are in agreement with that of the study by Breslow et al,4 who examined outcomes of crisis hospitalization of patients with schizophrenia and personality disorder and found significant improvement in psychiatric symptoms following crisis hospitalization. Furthermore, Wallsten et al27 reported that 58% of 233 patients treated in psychiatric emergency units showed an improvement of clinical condition and psychosocial functioning.
Regarding factors associated with hospital admission, we found that older age was associated with greater likelihood of subsequent hospitalization, which is consistent with earlier findings by Unick et al.18 We also found that self-referred patients with a past psychiatric history were more likely to be admitted to the hospital subsequently. Self-referred patients may denote a lack of social support,18 which can also predispose to more frequent ER revisits following a brief period of stabilization in the hospital as we found in this study. The more severely mentally ill patients were more likely to be brought to the hospital by other agencies such as the police or transferred from the ER of other local general hospitals and are often admitted directly to the inpatient wards. We found that more patients with past psychiatric history were admitted to our observation unit, and these patients may then also be subsequently hospitalized or associated with revisits within a day after discharge from the observation unit. Clinically, these known patients can present with adverse effects of their prescribed medications or relapse of their illness, which can often be managed in the observation unit, unless the lack of clinical improvement with lower psychosocial functioning warrants formal hospitalization.18,19 Revisits to the ER for psychiatric consultations are not uncommon, especially for certain conditions such as anxiety and addictive disorders and even medical comorbidity.28 In contrast, we found association of revisits after discharge from the observation unit with past psychiatric history but not specific diagnoses in our study. We also found a relationship between revisits and male gender, which is consistent with that of earlier studies.28,29
There were several limitations in this study. First, the data were obtained from the records of the admissions to the observation unit at the ER of a national tertiary psychiatric hospital; hence, the findings may not be generalizable to the observation unit in a general hospital setting with a psychiatry department or in private hospitals. Second, we did not use other formal rating scales for documenting the differing nature of psychopathology and level of psychosocial functioning for the various psychiatric conditions apart from the CGI-S and GAF. Third, we did not track longer-term outcomes of those individuals who were discharged from the observation unit beyond 24 hours or following admission to the inpatient wards.
Further research is needed to examine a large sample size over a longer period of time to study the benefits of the observation unit service such as whether use would decrease the rates of very short-term inpatient acute ward admissions lasting a few days as well as reduce the impact on community functioning seen with a more prolonged period of hospitalization.
In conclusion, we found a specific clinical profile of patients admitted to our observation unit who then needed further hospitalization (patients who were older, self-referred, with past psychiatric history, and with lower level of psychosocial functioning or experiencing less clinical improvement while in the observation unit) or were found to revisit the ER shortly after discharge from the observation unit (patients who were males, self-referred, and with past psychiatric history). Of note, patients admitted to the observation unit who were discharged showed significant clinical improvement as evident by reductions in clinical severity scores. These findings behoove us as psychiatric care providers to focus on these vulnerable individuals to further optimize outpatient management even in the psychiatric emergency room setting. Better management of these patients at the outpatient level can potentially decrease unnecessary hospitalization and reduce health care cost as well as illness burden on patients and caregivers.
Author affiliations: Department of General Psychiatry, Institute of Mental Health, Singapore (Drs San San Thinn, Chai, Su, Sengupta, Jacob, and Sim and Mss Koh and Xu); and Research Division, Institute of Mental Health, Singapore (Mss Kuswanto and Sum).
Potential conflicts of interest: None reported.
Funding/support: None reported.
Acknowledgments: The authors would like to thank all participants, their families, and our hospital staff for their support of this study.
REFERENCES
1. Walker WR, Parsons LB, Skelton WD. Brief hospitalization on a crisis service: a study of patient and treatment variables. Am J Psychiatry. 1973;130(8):896–900. doi:10.1176/ajp.130.8.896 PubMed
2. Gillig PM, Hillard JR, Bell J, et al. The psychiatric emergency service holding area: effect on utilization of inpatient resources. Am J Psychiatry. 1989;146(3):369–372. doi:10.1176/ajp.146.3.369 PubMed
3. Rhine MW, Mayerson P. Crisis hospitalization within a psychiatric emergency service. Am J Psychiatry. 1971;127(10):1386–1391. doi:10.1176/ajp.127.10.1386 PubMed
4. Breslow RE, Klinger BI, Erickson BJ. Crisis hospitalization on a psychiatric emergency service. Gen Hosp Psychiatry. 1993;15(5):307–315. doi:10.1016/0163-8343(93)90023-H PubMed
5. Francis E, Marchand W, Hart M, et al. Utilization and outcome in an overnight psychiatric observation program at a Veterans Affairs Medical Center. Psychiatr Serv. 2000;51(1):92–95. doi:10.1176/ps.51.1.92 PubMed
6. Ross MA, Hockenberry JM, Mutter R, et al. Protocol-driven emergency department observation units offer savings, shorter stays, and reduced admissions. Health Aff (Millwood). 2013;32(12):2149–2156. doi:10.1377/hlthaff.2013.0662 PubMed
7. Svindseth MF, Nøttestad JA, Dahl AA. A study of outcome in patients treated at a psychiatric emergency unit. Nord J Psychiatry. 2010;64(6):363–371. doi:10.3109/08039481003690273 PubMed
8. Jayaram G, Tien AY, Sullivan P, et al. Elements of a successful short-stay inpatient psychiatric service. Psychiatr Serv. 1996;47(4):407–412. doi:10.1176/ps.47.4.407 PubMed
9. Schneider SE, Ross IM. Ultra-short hospitalization for severely mentally ill patients. Psychiatr Serv. 1996;47(2):137–138. doi:10.1176/ps.47.2.137 PubMed
10. Herz MI, Endicott J, Gibbon M. Brief hospitalization: two-year follow-up. Arch Gen Psychiatry. 1979;36(6):701–705. doi:10.1001/archpsyc.1979.01780060091011 PubMed
11. Herz MI, Endicott J, Spitzer RL. Brief hospitalization: a two-year follow-up. Am J Psychiatry. 1977;134(5):502–507. doi:10.1176/ajp.134.5.502 PubMed
12. Clarke P, Hafner RJ, Holme G. The brief admission unit in emergency psychiatry. J Clin Psychol. 1997;53(8):817–823. doi:10.1002/(SICI)1097-4679(199712)53:8<817::AID-JCLP5>3.0.CO;2-C PubMed
13. Alwan NA, Johnnstone P, Zolese G. Length of hospitalization for people with severe mental illness. Cochrane Database Syst Rev 2008;(1):CD000384. doi:10.1002/14651858.cd000384.pub2 PubMed
14. Goldberg JF, Ernst CL, Bird S. Predicting hospitalization versus discharge of suicidal patients presenting to a psychiatric emergency service. Psychiatr Serv. 2007;58(4):561–565. doi:10.1176/ps.2007.58.4.561 PubMed
15. Kunen S, Prejean C, Gladney B, et al. Disposition of emergency department patients with psychiatric comorbidity: results from the 2004 National Hospital Ambulatory Medical Care Survey. Emerg Med J. 2006;23(4):274–275. doi:10.1136/emj.2005.027367 PubMed
16. Lyons JS, Stutesman J, Neme J, et al. Predicting psychiatric emergency admissions and hospital outcome. Med Care. 1997;35(8):792–800. doi:10.1097/00005650-199708000-00005 PubMed
17. Rabinowitz J, Massad A, Fennig S. Factors influencing disposition decisions for patients seen in a psychiatric emergency service. Psychiatr Serv. 1995;46(7):712–718. doi:10.1176/ps.46.7.712 PubMed
18. Unick GJ, Kessell E, Woodard EK, et al. Factors affecting psychiatric inpatient hospitalization from a psychiatric emergency service. Gen Hosp Psychiatry. 2011;33(6):618–625. doi:10.1016/j.genhosppsych.2011.06.004 PubMed
19. Way BB, Banks S. Clinical factors related to admission and release decisions in psychiatric emergency services. Psychiatr Serv. 2001;52(2):214–218. doi:10.1176/appi.ps.52.2.214 PubMed
20. Guy W. ECDEU Assessment Manual for Psychopharmacology. Rockville, MD: US Department of Health, Education, and Welfare Public Health Service Alcohol, Drug Abuse, and Mental Health Administration; 1976.
21. Jones SH, Thornicroft G, Coffey M, et al. A brief mental health outcome scale: reliability and validity of the Global Assessment of Functioning (GAF). Br J Psychiatry. 1995;166(5):654–659. doi:10.1192/bjp.166.5.654 PubMed
22. Colasanti A, Natoli A, Moliterno D, et al. Psychiatric diagnosis and aggression before acute hospitalisation. Eur Psychiatry. 2008;23(6):441–448. doi:10.1016/j.eurpsy.2007.09.005 PubMed
23. Catalano RA, Kessell E, Christy A, et al. Involuntary psychiatric examinations for danger to others in Florida after the attacks of September 11, 2001. Psychiatr Serv. 2005;56(7):858–862. doi:10.1176/appi.ps.56.7.858 PubMed
24. US Department of Health and Human Services. Tenth Special Report to Congress on Alcohol and Health. Bethesda, MD: US Dept of Health and Human Services; 2000. http://pubs.niaaa.nih.gov/publications/10report/intro.pdf. Accessed April 24, 2015.
25. Chong SA, Abdin E, Vaingankar JA, et al. A population-based survey of mental disorders in Singapore. Ann Acad Med Singapore. 2012;41(2):49–66. PubMed
26. Odenheimer JF. Day hospital as an alternative to the psychiatric ward: attitudes and responses of relatives. Arch Gen Psychiatry. 1965;13(1):46–53. doi:10.1001/archpsyc.1965.01730010048006 PubMed
27. Wallsten T, Kjellin L, Lindström L. Short-term outcome of inpatient psychiatric care: impact of coercion and treatment characteristics. Soc Psychiatry Psychiatr Epidemiol. 2006;41(12):975–980. doi:10.1007/s00127-006-0131-6 PubMed
28. Brennan JJ, Chan TC, Hsia RY, et al. Emergency department utilization among frequent users with psychiatric visits. Acad Emerg Med. 2014;21(9):1015–1022. doi:10.1111/acem.12453 PubMed
29. Weisman G, Feirstein A, Thomas C. Three-day hospitalization: a model for intensive intervention. Arch Gen Psychiatry. 1969;21(5):620–629. doi:10.1001/archpsyc.1969.01740230108015 PubMed
Enjoy this premium PDF as part of your membership benefits!


