The objective of this article is to help clinicians make an accurate diagnosis by considering hypercalcemia as a potential cause of psychosis. A patient case is presented, along with a review of the literature dissecting the association between calcium and psychiatric symptoms. Clinical implications and suggestions for management of hypercalcemia and psychosis in the setting of primary hyperparathyroidism are provided.
Case Report, Review of the Literature, and Management Considerations
ABSTRACT
The objective of this article is to help clinicians make an accurate diagnosis by considering hypercalcemia as a potential cause of psychosis. A patient case is presented, along with a review of the literature dissecting the association between calcium and psychiatric symptoms. Clinical implications and suggestions for management of hypercalcemia and psychosis in the setting of primary hyperparathyroidism are provided.
Prim Care Companion CNS Disord 2018;20(6):18nr02356
To cite: Bojdani E, Zhang T, Shetty S, et al. Hypercalcemia and psychosis: case report, review of the literature, and management considerations. Prim Care Companion CNS Disord. 2018;20(6):18nr02356.
To share: https://doi.org/10.4088/PCC.18nr02356
© Copyright 2018 Physicians Postgraduate Press, Inc.
aHarvard South Shore Psychiatry Residency Training Program, Brockton, Massachusetts
bVA Boston Healthcare System, Brockton, Massachusetts
cDepartment of Psychiatry, Harvard Medical School, Boston, Massachusetts
dBoston University School of Medicine, Boston, Massachusetts
*Corresponding author: Ermal Bojdani, MD, Harvard South Shore/Boston VA Medical Center–Brockton, Psychiatry Residency Training Program, 940 Belmont St (116A7), Brockton, MA 02301 ([email protected]).
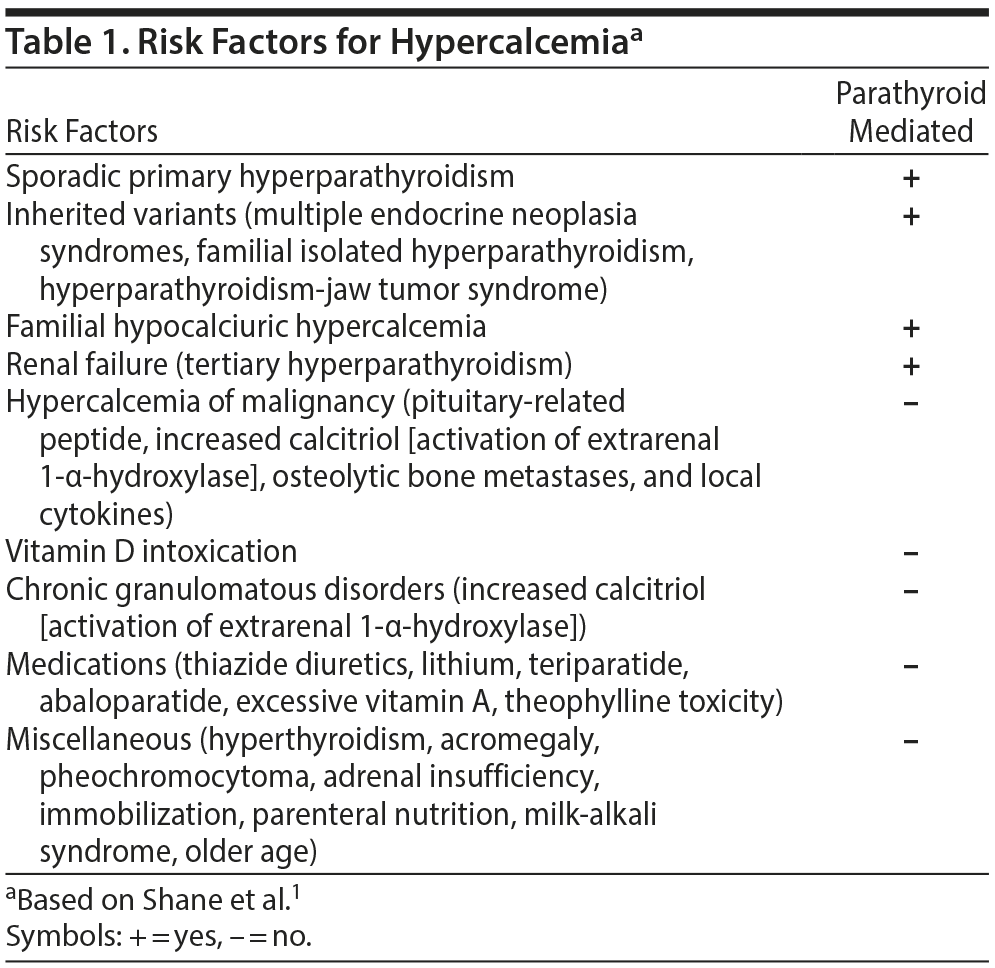
Hypercalcemia is a relatively common clinical entity, and risk factors for its development include sporadic and inherited conditions, renal failure, and various medications (Table 1).1 Clinical manifestations involve, but are not limited to, the renal, gastrointestinal, musculoskeletal, cardiovascular, and neurologic systems. Clinical evaluation and laboratory studies help to diagnose the cause of hypercalcemia and to rule out worrisome, untreated comorbidity. In addition to measuring serum calcium (with correction for albumin if applicable), measurement of intact parathyroid hormone (PTH) helps to distinguish PTH-mediated from non–PTH-mediated causes of hypercalcemia. When PTH concentrations are < 20 pg/mL, other tests such as for PTH-related protein, vitamin A, vitamin D metabolites, and thyroid-stimulating hormone (TSH) and serum and urinary protein electrophoresis may be helpful in making the diagnosis.
Hypercalcemia has been associated with psychiatric symptoms, and the psychopathology usually emerges after a prolonged period of subclinical hypercalcemia.2 A direct mechanism between hypercalcemia and psychosis has not yet been characterized. However, calcium is known to play a role in the metabolism of monoamines in the central nervous system by modulating dopaminergic and cholinergic metabolism and neurotransmission along synaptic junctions, causing changes in mood and cognition.2,3 Calcium abnormalities have been reported in the setting of catatonic episodes in patients with schizophrenia3 and in endocrine disorders.
The patient depicted in this case report presented to the emergency department with a history of hypercalcemia, elevated PTH > 20 pg/mL, and psychotic symptoms. His primary hyperparathyroidism was believed to be a potential leading cause of his neuropsychiatric symptoms. We describe the patient’s history, review the relationship between calcium and psychosis, and make recommendations for clinical management.
METHODS
A PubMed search was conducted using the search terms calcium and psychosis. The search resulted in over 40 articles, which were reviewed for relevance. Articles in languages other than English and those that lacked an abstract or were published before 1984 were excluded from the review. Sixteen articles were fully examined and incorporated in the review.1–16
CASE REPORT
Mr A is a 43-year-old married black man who presented for evaluation of paranoia. He grew up in Nigeria and after completing college immigrated to the United States, where he struggled to adjust as an immigrant. He met his wife while in the Army. Due to emerging emotional distress, he was placed under close supervision during his Army tenure. Upon return from combat service, he experienced significant symptoms of anxiety, anger, hypervigilance, paranoia that people including coworkers were following him when he traveled, and delusions. Occasional olfactory and visual hallucinations of seeing shapes or shadows were also reported. These symptoms continued, occurring intermittently over 2 years, worsening in the recent 3 months, and affecting his work performance, which led to suspension. The symptoms also caused interpersonal conflict with his wife and physical aggression toward nonliving objects. He once threatened with a suicidal ideation in the heat of an argument, but did not attempt suicide. He suffered from insomnia, and paranoia caused him to place locks on the windows and cameras in his home. These symptoms led to involuntary psychiatric hospitalization, and he was started on olanzapine for psychosis and agitation, trazodone as needed for insomnia, and hydroxyzine as needed for anxiety. He did not wish to continue these medications at discharge, believing he did not need them.
Psychotherapy with a psychologist was of unclear benefit, partially due to his variable record of attendance. He continued to leave various jobs, quitting due to concern that others were out to get him or being fired for poor performance and emotional disturbance. He eventually again became paranoid about people following him and presented to the emergency department after a 14-day episode of mania and psychosis. The episode started with an argument with his wife, and he subsequently went missing for 2 days. He reported being in Amsterdam on his way to Nigeria, but the flight would not accept him for travel. On day 6, he returned to his wife in the United States and paranoia continued. When in the waiting room at a dentist’s appointment for one of his children, he was paranoid that people were looking at him weirdly, so much so that he took their young son and went on an undisclosed journey, eventually making their way to Philadelphia, taking rests and sleeping a few hours at a time. After a car accident with no injury, he rented another car and made his way to New York, at which time he asked his wife to pick them up. His wife filed a missing persons report. From New York he drove to Georgia and from there texted family, reporting being scared that people were following him and seeking help. By this point, children’s services became involved. He eventually had a second car accident with no injury, and he was picked up by Georgia police. He returned on day 14 to the airport, where he was picked up by family and brought to the emergency department.
At the hospital, Mr A’s family reported no family history of psychiatric disorders and confirmed that he taking no psychiatric medications. During the interview, he was guarded. He denied illicit substance use, head trauma, or loss of consciousness. Psychiatric review of systems was positive for hypervigilance, triggers of seeing people in uniform, insomnia, anger, and irritability.
On physical and mental status examination, Mr A’s vital signs were significant for a blood pressure of 142/102 mm Hg and a body mass index of 37.9 kg/m2. He appeared obese, with otherwise unremarkable physical findings, wearing a facial mask due to concern for allergies. He was sleepy but cooperative when awake. He had a slowed rate, rhythm, volume, and prosody with spontaneous speech, which at times was hard to understand due to his accent. He endorsed a linear and goal-directed thought process. He denied psychotic symptoms, although family reported he was afraid people were out to get him. His mood was sleepy, and his affect was tired. He was oriented to person and place, only missing the day of the week. He was able to tell about some of his travels but left parts out. His insight and judgment were deemed severely limited.
Review of Mr A’s laboratory history included a plasma calcium level of 11.3 mg/dL (reference range, 8.5–10.5 mg/dL), PTH of 80.1 pg/mL (reference range, 10–65 pg/mL), and a negative urine toxicology screen. His TSH level (0.46 μIU/mL [reference range, 0.35–5.00]) was within normal limits and hemoglobin A1c was 6.9% (4.0%–5.6%). His lipid profile, kidney function, white blood cell counts, platelets, and electrolytes were within normal limits; hemoglobin was 13.2 g/dL (14–17 g/dL), and liver function test results were slightly abnormal (alanine aminotransferase: 73 units/L [reference range, 7–52 U/L], aspartate aminotransferase: 56 units/L [reference range, 5–34 U/L]). A broad differential was considered, including whether his history of elevated calcium could be contributing to his psychosis.
CASE SUMMARY
Diagnostic Considerations and Outcome
Mr A presented with psychotic and manic symptoms; initially it was unclear which DSM-5 criteria he met. The differential diagnoses included a brief psychotic disorder, schizophreniform disorder, schizophrenia, bipolar II disorder, bipolar I disorder with psychotic features, schizoaffective disorder, and posttraumatic stress disorder (PTSD). We also wanted to rule out a medical condition contributing to his symptoms. Given that primary psychotic disorders generally begin in the teen years, we found it unusual for Mr A to present with psychosis later in life. PTSD was high on the list of differential diagnoses given his combat history and that he was irritable, guarded, and paranoid. However, the manic episode did not quite fit the criteria for PTSD, thus bipolar I disorder with psychotic features was considered. The remaining question was whether a medical condition was contributing to Mr A’s symptoms. His history of mildly elevated PTH (80.1 pg/mL [reference range, 10–65 pg/mL]) with mild hypercalcemia of 11.3 mg/dL (reference range, 8.5–10.5 mg/dL) led to a review of the literature for the association of hypercalcemia and psychosis. The review suggested that hypercalcemia of any level can lead to psychosis, which would most likely respond to treatment aimed at lowering calcium levels as well as antipsychotic treatment. An endocrinology consult revealed strong suspicion for primary hyperparathyroidism given Mr A’s history of elevated calcium and PTH for over a year. However, further evaluation and treatment were not possible due to lack of follow-up in the endocrinology clinic. Psychosis due to elevated serum calcium and bipolar I disorder with psychotic features remained at the top of the differential diagnosis list. The patient was treated with haloperidol and valproic acid with good results.
Considerations for Treating Hypercalcemia
Hypercalcemia due to primary hyperparathyroidism is a relatively common clinical problem.1 In symptomatic cases, including presentations with acute neuropsychiatric symptoms, the severity of symptoms, degree of hypercalcemia, and rate of rise of serum calcium concentration often guide the urgency of therapy.4 In the case of Mr A, given an acute exacerbation of symptoms in the setting of chronic primary hyperparathyroidism, one could have considered providing both immediate and long-term treatment in consultation with primary care and endocrinology. The neuropsychiatric symptoms, most likely due to an increase in serum calcium, an increase in PTH, or both, might improve with immediate therapy consisting of isotonic saline and administration of calcitonin, the combination of which would substantially reduce serum calcium concentrations within 12 to 48 hours.4 Paranoia could persist and lead Mr A to not attend endocrinology follow-up where definitive therapy with parathyroidectomy would most likely be recommended to cure his primary hyperparathyroidism with severe neuropsychiatric symptoms.5
In this case, given Mr A’s lack of follow-up and current state of hypercalcemia and psychosis, it is appropriate to recommend supportive preventive measures and treatment with a calcimimetic. Preventive measures include avoiding factors known to aggravate hypercalcemia such as lithium carbonate therapy, thiazide diuretics, prolonged inactivity, volume depletion, and a calcium diet > 1,000 mg/d; encouraging 6–8 glasses of water per day; physical activity as tolerated; and maintenance of moderate calcium (1,000 mg/d) and vitamin D (400–800 IU/d) intake. In symptomatic patients in whom bone density is not in the osteoporotic range, the calcimimetic agent cinacalcet, rather than a bisphosphonate, is recommended.5 Cinacalcet is believed to increase the sensitivity of the calcium-sensing receptor on the parathyroid gland, thus it concomitantly lowers PTH, serum calcium, and serum phosphorus levels, leading to prevention of progressive bone disease and other adverse events associated with dysregulation in mineral metabolism. Common side effects include nausea, diarrhea, arthralgia, paresthesia, and myalgia. While treatment with cinacalcet is not permanent and PTH concentrations do not normalize (but do decrease), it would be reasonable to administer a trial of cinacalcet and monitor for improvement in paranoia. If the paranoia improves, Mr A might be better able to more appropriately evaluate whether he is comfortable with the continuing risk associated with untreated primary hyperparathyroidism. If the paranoia does not improve, this may suggest that another etiology is more likely and other untreated comorbidities should be investigated.
DISCUSSION
Neuropsychiatric disturbances have been reported in cases of mild hypercalcemia due to otherwise asymptomatic primary hyperparathyroidism, with symptoms including anxiety, depression, suicidality, anger, irritability, hallucinations, delusions, and impaired cognition with stupor and delirium.2,6,7 The relationship between hypercalcemia and psychiatric symptoms, including psychosis, is most likely causal in nature. Paranoid psychosis and delusions in the setting of hypercalcemia8–11 often remit upon normalization of serum calcium or treatment of parathyroid adenoma.8,11 In a retrospective investigation12 of patients with primary hyperparathyroidism who underwent surgical intervention, psychiatric symptoms were found in 23% (102/441), spanning the severity of hypercalcemia. Hallucinations and paranoid thinking were found in 4 patients.12 Abnormality of serum calcium in the other direction, hypocalcemia, has also been implicated in psychosis; however, the data to support this relationship are limited.9
Severe psychopathology, including delusions, has been seen in patients with mild hypercalcemia.8 Paranoia and delusions have been reported in primary hyperparathyroidism with a serum calcium level of 2.94 mmol/L (normal level: 2.2–2.6 mmol/L) and an elevated parathyroid hormone level of 9.6 mmol/L (normal level: 1.1–6.9 mmol/L).13 Irritability and hallucinations (auditory, visual) have been reported in patients with higher serum calcium levels (17.8 mg/dL).14 While it has been hypothesized that there may be a modest correlation between the degree of hypercalcemia and severity of psychiatric manifestations,15 Alarcón and Franceschini11 and others2,6,16 suggest that no such correlation exists. Instead, even mild or moderate increases in serum calcium can precipitate psychiatric symptomatology including psychosis.11 Alarcón and Franceschini11 and Joborn et al12 agree, through their retrospective study and literature review, respectively, that depressive mood symptoms and confusional states seem to be the more common manifestations of hypercalcemia-induced psychiatric symptoms.
With regard to workup and management, one should consider calcium elevation as a potential contributor in all patients with psychiatric symptoms, and serum calcium levels should be obtained in those with atypical presentations or risk factors for hypercalcemia (see Table 1).1 Hypercalcemia should be assessed first by obtaining a serum PTH level. Isotonic saline and calcitonin are for symptomatic hypercalcemia acutely, and use of cinacalcet in the setting of chronic primary hyperparathyroidism in patients with neuropsychiatric symptoms who do not undergo surgery is recommended. Antipsychotic medications like haloperidol serve an adjunctive role.
Some patients with primary hyperparathyroidism may initially present with psychiatric symptoms only. Thus, one should consider calcium elevation as a potential contributor in all patients with psychiatric symptoms, and serum calcium level should be obtained in those with atypical presentations or risk factors for hypercalcemia.1 Calcium levels > 10.5 mg/dL should raise suspicion for underlying pathology. In addition to measuring serum calcium (with repeated testing of total calcium and correction for albumin as needed), measurement of intact PTH helps to distinguish PTH-mediated from non–PTH-mediated causes of hypercalcemia. When PTH concentrations are < 20 pg/mL, other tests may be helpful in making the diagnosis. Nonsurgical hypercalcemia treatments have often been used prior to surgical intervention (saline, calcitonin, calcium channel blockers), leading to improvement in psychiatric symptoms.11,14 For patients with psychosis in the setting of elevated serum calcium > 10.5 mg/dL, one may consider immediate therapy with isotonic saline and administration of calcitonin, the combination of which would substantially reduce serum calcium concentrations within 12 to 48 hours.4 If the symptomatic hypercalcemia is believed to be due to primary hyperparathyroidism, parathyroid surgery is recommended. If such patients do not engage in a surgical intervention, aside from advising use of preventive measures as previously discussed, the calcimimetic agent cinacalcet, rather than a bisphosphonate, is recommended,5 especially if the patient’s bone density is not in the osteoporotic range. Cinacalcet is initially dosed at 30 mg twice daily, and the dose may be increased incrementally every 2–4 weeks as necessary to normalize serum calcium levels. Cinacalcet should be administered with food to increase bioavailability, and serum calcium should be measured within 1 week after initiation of therapy or any dose adjustment. Monitoring for progression of disease includes checking serum calcium, creatinine, and estimated glomerular filtration rate annually and bone density (hip, spine, and forearm) every 1 to 2 years. Antipsychotic medications like haloperidol serve an adjunctive role for acute management; however, treatment of the underlying cause of hypercalcemia may lead to resolution of symptoms and eventual discontinuation of antipsychotics.
Submitted: July 23, 2018; accepted September 21, 2018.
Published online: November 29, 2018.
Potential conflicts of interest: The authors have no conflicts of interest.
Funding/support: None.
Acknowledgments: The authors thank Lynn E. Delisi, MD, Harvard Medical School, Boston, Massachusetts, for her help in discussing, reviewing, and editing this manuscript. Dr Delisi has no conflict of interest to disclose.
Patient consent: Consent was received from the patient to publish this case, and information has been de-identified to protect anonymity.
REFERENCES
1. Shane E, Rosen CJ, Mulder JE. Diagnostic approach to hypercalcemia. UpToDate website. https://www.uptodate.com/contents/diagnostic-approach-to-hypercalcemia?search=diagnostic%20approach%20to%20hypercalcemia&source=search_result&selectedTitle=1~150&usage_type=default&display_rank=1. Accessed September 9, 2018.
2. Parks KA, Parks CG, Onwuameze OE, et al. Psychiatric complications of primary hyperparathyroidism and mild hypercalcemia. Am J Psychiatry. 2017;174(7):620–622. PubMed CrossRef
3. Singh P, Bauernfreund Y, Arya P, et al. Primary hyperparathyroidism presenting as acute psychosis secondary to hypercalcaemia requiring curative parathyroidectomy. J Surg Case Rep. 2018;2018(2):rjy023. PubMed CrossRef
4. Shane E, Berenson JR, Rosen CJ, et al. Treatment of hypercalcemia. UpToDate website. https://www.uptodate.com/contents/treatment-of-hypercalcemia?search=
treatment%20of%20hypercalcemia&source
=search_result&selectedTitle=1~150&usage_type=default&display_rank=1. Accessed September 8, 2018.
5. Silverberg SJ, Fuleihan GE, Rosen CJ, et al. Primary hyperparathyroidism: management. UpToDate website. https://www.uptodate.com/contents/primary-hyperparathyroidism-management?search=primary%20hyperparathyroidism%20management&source=search_result&selectedTitle=1~113&usage_type=default&display_rank=1. Accessed September 7, 2018.
6. Casella C, Pata G, Di Betta E, et al. Neurological and psychiatric disorders in primary hyperparathyroidism: the role of parathyroidectomy. Ann Ital Chir. 2008;79(3):157–161, discussion 161–163. PubMed
7. Watson LC, Marx CE. New onset of neuropsychiatric symptoms in the elderly: possible primary hyperparathyroidism. Psychosomatics. 2002;43(5):413–417. PubMed CrossRef
8. Rosenthal M, Gil I, Habot B. Primary hyperparathyroidism: neuropsychiatric manifestations and case report. Isr J Psychiatry Relat Sci. 1997;34(2):122–125. PubMed
9. Ang AW, Ko SM, Tan CH. Calcium, magnesium, and psychotic symptoms in a girl with idiopathic hypoparathyroidism. Psychosom Med. 1995;57(3):299–302. PubMed CrossRef
10. Ebel H, Schlegel U, Klosterkötter J. Chronic schizophreniform psychosis in primary hyperparathyroidism. Nervenarzt. 1992;63(3):180–183. PubMed
11. Alarcón RD, Franceschini JA. Hyperparathyroidism and paranoid psychosis: case report and review of the literature. Br J Psychiatry. 1984;145(5):477–486. PubMed CrossRef
12. Joborn C, Hetta J, Palmér M, et al. Psychiatric symptomatology in patients with primary hyperparathyroidism. Ups J Med Sci. 1986;91(1):77–87. PubMed CrossRef
13. Irvine E, Yap YW, Purewal T, et al. A case of acute confusion: Cushing’s syndrome presenting with primary hyperparathyroidism. BMJ Case Rep. 2017;2017:bcr-2016-218694. PubMed CrossRef
14. Papa A, Bononi F, Sciubba S, et al. Primary hyperparathyroidism: acute paranoid psychosis. Am J Emerg Med. 2003;21(3):250–251. PubMed CrossRef
15. Riley DM, Watt DC. Hypercalcemia in the etiology of puerperal psychosis. Biol Psychiatry. 1985;20(5):479–488. PubMed CrossRef
16. Goyal A, Chumber S, Tandon N, et al. Neuropsychiatric manifestations in patients of primary hyperparathyroidism and outcome following surgery. Indian J Med Sci. 2001;55(12):677–686. PubMed
Enjoy this premium PDF as part of your membership benefits!


