Objective: To examine the prevalence and correlates of attempting suicide in the past 12 months among adults with past-year suicidal ideation in the United States.
Method: Data were from 229,600 persons aged 18 years or older who participated in the 2008-2012 National Survey on Drug Use and Health. Among them, 12,300 reported having past-year suicidal ideation, and over 2,000 of those reported attempting suicide within the past 12 months prior to survey interview. Descriptive analyses and pooled and stratified (by suicide plan and major depressive episode [MDE]) multivariate logistic regression models were applied. Major depressive episode was based on assessments of individual diagnostic criteria from the Diagnostic and Statistical Manual of Mental Disorders, Fourth Edition (DSM-IV).
Results: Among persons aged 18 years or older in the United States, 3.8% reported having suicidal ideation in the past 12 months. Among past-year suicidal ideators, 13.2% attempted suicide in the past 12 months. The prevalence of past 12-month suicide attempt among past-year ideators with MDE was higher than among those without MDE (14.1% vs 12.0%). Past 12-month suicide attempt was more common among ideators with a suicide plan than among ideators without a plan (37.0% vs 3.7%). However, the prevalence of suicide attempt was higher among ideators with a plan but without MDE than among ideators with a plan and MDE (42.1% vs 32.9%). Compared with ideators without a plan, ideators with a plan had a higher (adjusted odds ratio [AOR] = 2.2; 95% confidence interval [CI], 1.47-3.45) suicide attempt risk among those without MDE (AOR = 22.4; 95% CI,16.55-30.27) than among those with MDE (AOR = 10.7; 95% CI, 7.91-14.49).
Conclusions: Among adult suicidal ideators, factors associated with their progression from ideation to suicide attempt may vary by their suicide plan and major depression status. Focusing attention on high-risk subgroups may be warranted.
This CME activity is expired. For more CME activities, visit CMEInstitute.com.
Find more articles on this and other psychiatry and CNS topics:
The Journal of Clinical Psychiatry
The Primary Care Companion for CNS Disorders

ABSTRACT
Objective: To examine the prevalence and correlates of attempting suicide in the past 12 months among adults with past-year suicidal ideation in the United States.
Method: Data were from 229,600 persons aged 18 years or older who participated in the 2008-2012 National Survey on Drug Use and Health. Among them, 12,300 reported having past-year suicidal ideation, and over 2,000 of those reported attempting suicide within the past 12 months prior to survey interview. Descriptive analyses and pooled and stratified (by suicide plan and major depressive episode [MDE]) multivariate logistic regression models were applied. Major depressive episode was based on assessments of individual diagnostic criteria from the Diagnostic and Statistical Manual of Mental Disorders, Fourth Edition (DSM-IV).
Results: Among persons aged 18 years or older in the United States, 3.8% reported having suicidal ideation in the past 12 months. Among past-year suicidal ideators, 13.2% attempted suicide in the past 12 months. The prevalence of past 12-month suicide attempt among past-year ideators with MDE was higher than among those without MDE (14.1% vs 12.0%). Past 12-month suicide attempt was more common among ideators with a suicide plan than among ideators without a plan (37.0% vs 3.7%). However, the prevalence of suicide attempt was higher among ideators with a plan but without MDE than among ideators with a plan and MDE (42.1% vs 32.9%). Compared with ideators without a plan, ideators with a plan had a higher (adjusted odds ratio [AOR] = 2.2; 95% confidence interval [CI], 1.47-3.45) suicide attempt risk among those without MDE (AOR = 22.4; 95% CI,16.55-30.27) than among those with MDE (AOR = 10.7; 95% CI, 7.91-14.49).
Conclusions: Among adult suicidal ideators, factors associated with their progression from ideation to suicide attempt may vary by their suicide plan and major depression status. Focusing attention on high-risk subgroups may be warranted.
J Clin Psychiatry 2015;76(3):295-302
© Copyright 2015 Physicians Postgraduate Press, Inc.
Submitted: June 4, 2014; accepted September 25, 2014 (doi:10.4088/JCP.14m09287).
Corresponding author: Beth Han, MD, PhD, MPH, 1 Choke Cherry Rd, Room 7-1010, Rockville, MD 20857 ([email protected]).
In 2012, about 9.0 million adults (3.9%) reported that they had serious thoughts of suicide (suicidal ideation), and over 1.3 million (0.6%) reported that they attempted suicide in the past year.1 About 13% of suicidal ideators in a given year made a suicide attempt during that year.1 Suicide attempt is the strongest known clinical predictor for death by suicide.1-5 Because targeted suicide prevention and treatment strategies focus on populations at risk for suicide, suicide risk assessments often start after having evidence of suicidal ideation.2,6,7
Factors that predict the short-term transition from suicidal ideation to suicide attempt are not well understood.8,9 Although a few studies10-13 examined lifetime mental disorders and first suicide attempt among adults with lifetime suicidal ideation, assessment of more proximal risk may be more relevant for clinicians’ decision-making.8,9 One study investigated factors associated with suicide plan among past-year ideators and assessed factors associated with suicide attempt among past-year ideators.7 None of the existing studies systematically investigated the role that suicide plan plays in the progressions to past 12-month suicide attempt among past-year suicidal ideators in the United States.
Having a suicide plan is considered a psychiatric emergency as it is associated with an imminent medically lethal attempt and high suicide risk.14-17 However, many adults attempt suicide with no apparent suicide plan. The theoretical continuum of risk for attempting suicide, starting from passive suicidal ideation (desire for death) to suicidal ideation, then to suicide plan, and eventually to suicide attempt, is not always supported by empirical data.18 In 2012, although 1.0 million adults reported planning and attempting suicide, 0.3 million reported attempting suicide without a suicide plan.1 To reduce suicide risk, it is critical to understand how factors triggering the progression from suicide plan to suicide attempt differ from factors triggering the transition from suicidal ideation directly to suicide attempt. Also, targeted suicide prevention strategies need to identify specific sociodemographic subgroups. Thus, understanding whether and how associations between sociodemographic characteristics, mental disorders, and suicide attempt in the past 12 months vary by past-year suicide plan status among past-year ideators may help guide prevention programs and clinical intervention efforts.
Furthermore, major depression is the most common individual disorder among people with suicidal behaviors.4,19 The general public and even clinicians often assume that major depression is essential for suicide.20 However, 1 study suggests that lifetime major depression increased subsequent suicidal ideation risk, but was not related to first suicide attempt among ideators.11 No existing studies have examined whether and how associations between sociodemographic characteristics, mental disorders, suicide plan, and suicide attempt in the past 12 months vary by past-year major depression among past-year ideators.
Using recent large nationally representative data, this study examines factors associated with past 12-month suicide attempt among past-year ideators, particularly focusing on ideators with/without suicide plan and major depression. Our results may help clinicians identify adults with high risk of suicide and help improve targeted suicide prevention efforts.

- Having a suicide plan is considered a psychiatric emergency. The role that formulating a suicide plan plays in the short-term transition from suicidal ideation to suicide attempt is unknown.
- The absence of major depression should not be mistaken for the absence of suicide risk. Suicide prevention efforts need to target nondepressed ideators with a suicide plan.
METHOD
Data Source
This study examined data from 229,600 persons aged 18 or older who participated in the 2008-2012 National Survey on Drug Use and Health (NSDUH; http://www.samhsa.gov/data/
population-data-nsduh). Among them, 12,300 reported having past-year suicidal ideation, and over 2,000 of those reported attempting suicide within the past 12 months prior to survey interview.
The NSDUH is the primary source of information on substance use and mental health among the civilian, noninstitutionalized population aged 12 years or older in the United States and is conducted by the Substance Abuse and Mental Health Services Administration (SAMHSA).21 Since 2008, the NSDUH has been collecting nationally representative data on suicidal ideation and suicide attempts among the civilian, noninstitutionalized population aged 18 years or older in the United States.
NSDUH data were collected by interviewers during in-person visits to households and noninstitutional group quarters. Audio computer-assisted self-administered interviewing was used, providing respondents with a private, confidential way to record answers.
Measures
Suicidal ideation, suicide plan, and suicide attempts. The 2008-2012 NSDUH questionnaires asked all adult respondents: “At any time during the past 12 months, did you seriously think about trying to kill yourself?” Those who said yes to this question were then asked: “Did you make any plans to kill yourself during the past 12 months?” and “Did you try to kill yourself during the past 12 months?”
Self-rated health and mental health status. Since poor self-rated health was associated with death by suicide,22,23 we assessed self-rated health. Past 12-month major depressive episode (MDE) and substance use disorders (dependence on or abuse of alcohol or illicit drugs, including marijuana, cocaine, hallucinogens, heroin, and inhalants or nonmedical use of prescription pain relievers, sedatives, stimulants, or tranquilizers) were based on assessments of individual diagnostic criteria from the Diagnostic and Statistical Manual of Mental Disorders, Fourth Edition (DSM-IV).24 The presence of anxiety disorders was determined if the respondent was told by a doctor or other health professional in the past 12 months that he/she had an anxiety disorder. These measures had good validity and reliability.25-27
Sociodemographics and recent involvement with the criminal justice system. This study examined age, gender, race/ethnicity, education, marital status, employment status, health insurance, family income, metropolitan statistical area, and region. Since suicide attempt was common among adults with recent involvement with the criminal justice system,28 we investigated the number of times respondents were arrested/booked in the past year.
Statistical Analyses
Descriptive analyses were conducted to estimate the prevalence of attempting suicide in the past 12 months among past-year ideators by the above factors. Bivariate logistic regression modeling was applied to investigate factors associated with attempting suicide among ideators. Significant (at the .05 level) factors at the bivariate level were selected for the multivariate logistic regression modeling. We examined potential interactions between sociodemographic factors, mental disorders, and suicide plan status. Also, we assessed potential interactions between sociodemographics, mental disorders, suicide plan, and MDE status. A backward stepwise procedure was applied to remove insignificant interactions. Using the variance inflation factors, multicollinearity was assessed during multivariate modeling. Multicollinearity was not found in the final parsimonious multivariate model.
The final multivariate logistic regression pooled model identified 3 significant interactions (education and suicide plan [P = .0105], suicide plan and MDE [P = .0002], and race/ethnicity and MDE [P = .0006]). To better understand how these factors were associated with attempting suicide, stratified multivariate models by suicide plan and MDE were conducted. All analyses used SUDAAN software29 to account for the NSDUH’s complex sample design and sampling weights.
RESULTS
Prevalence of Attempting Suicide in the Past Year Among Adults With Suicidal Ideation
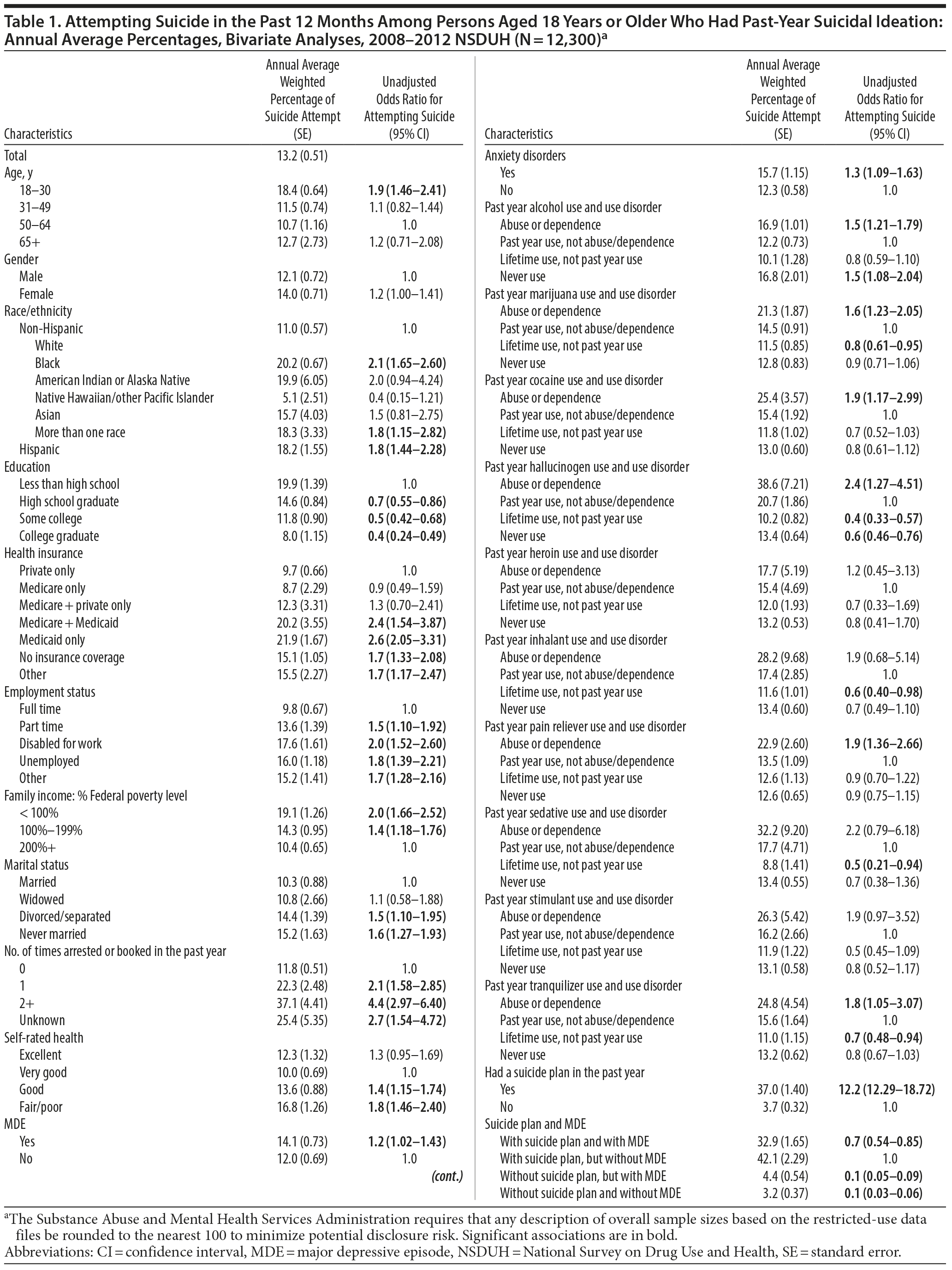
Among persons aged 18 years or older in the United States, 3.8% reported having suicidal ideation in the past 12 months prior to survey interview. Table 1 shows that among adults with past-year suicidal ideation, 13.2% attempted suicide in the past 12 months. The prevalence of past 12-month suicide attempt was higher among ideators aged 18-30 than among ideators aged 50-64 (18.4% vs 10.7%). The prevalence of suicide attempt was lower among white ideators than among black ideators, ideators with over 1 race, and among Hispanic ideators (11.0% vs 20.2%, 18.3%, and 18.2%, respectively). The prevalence of suicide attempt was higher among ideators with less than high school education than among ideators with college or more education (19.9% vs 8.0%).
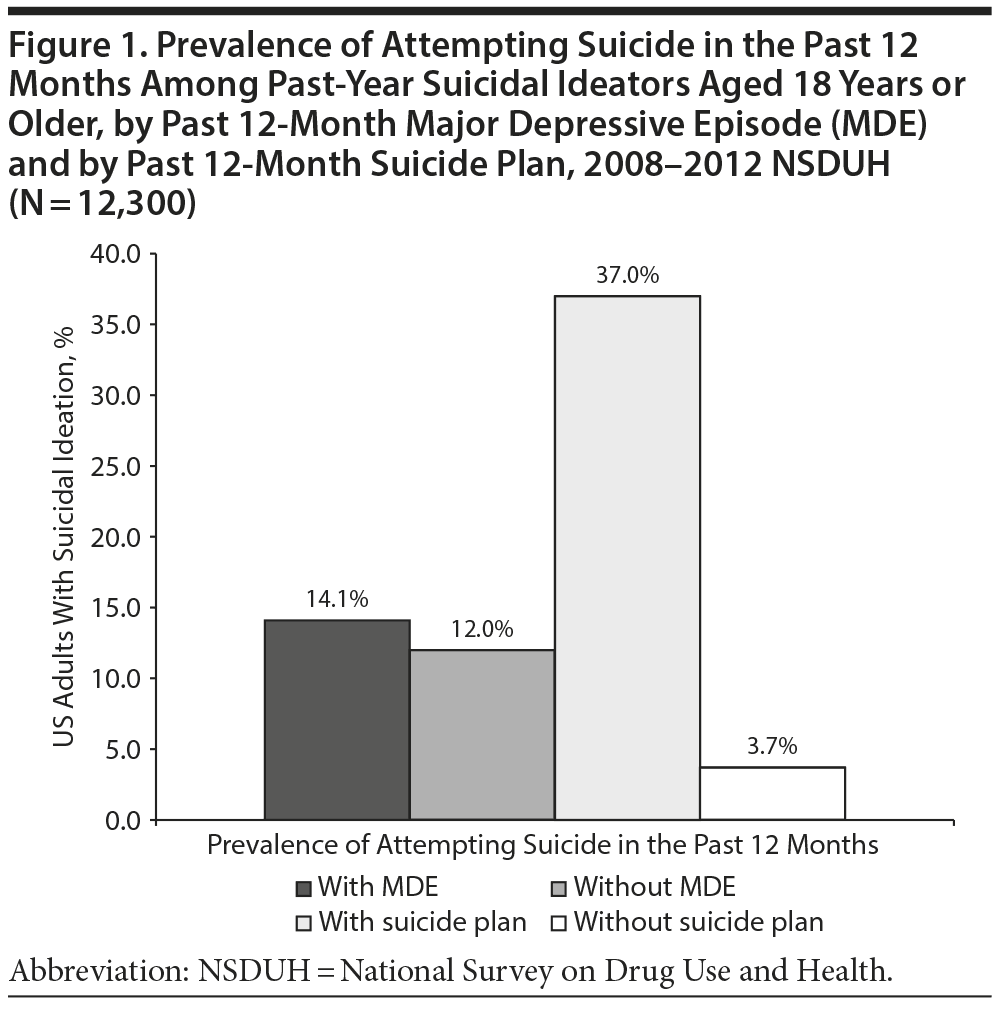
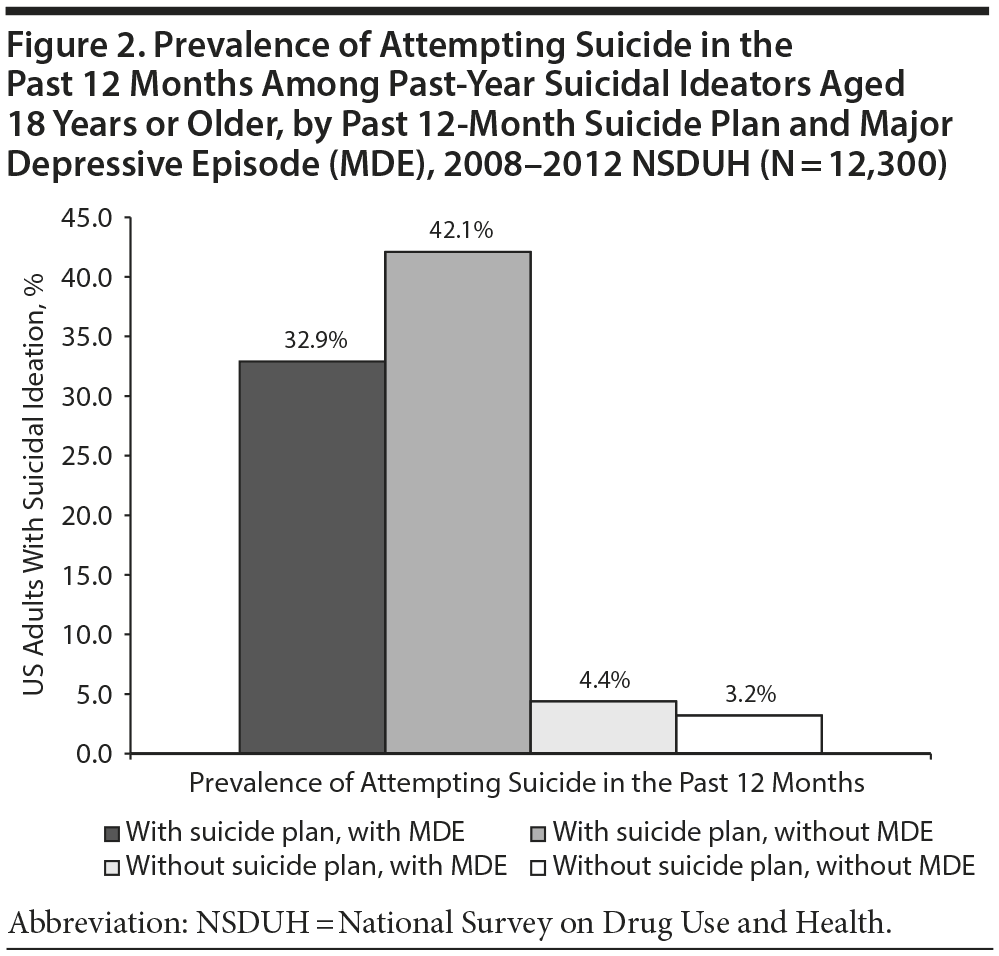
Figure 1 and Table 1 show that the prevalence of suicide attempt was higher among ideators with MDE than among ideators without MDE (14.1% vs 12.0%). The prevalence of suicide attempt was much higher among ideators with a suicide plan than among ideators without a plan (37.0% vs 3.7%). Figure 2 and Table 1 reveal that the prevalence of suicide attempt was significantly lower among ideators with a suicide plan and MDE than among ideators with a plan, but without MDE (32.9% vs 42.1%).
Ideators with alcohol use disorder were more likely to attempt suicide than ideators who drank alcohol, but had no alcohol use disorder in the past year (16.9% vs 12.2%). The prevalence of suicide attempt was higher among ideators with marijuana, cocaine, hallucinogen, pain reliever, or tranquilizer use disorder than among ideators who used the corresponding drug, but did not have the corresponding drug use disorder (21.3% vs 14.5%; 25.4% vs 15.4%; 38.6% vs 20.7%; 22.9% vs 13.5%; and 24.8% vs 15.6%, respectively).
Correlates of Attempting Suicide in the Past Year Among Adults With Suicidal Ideation
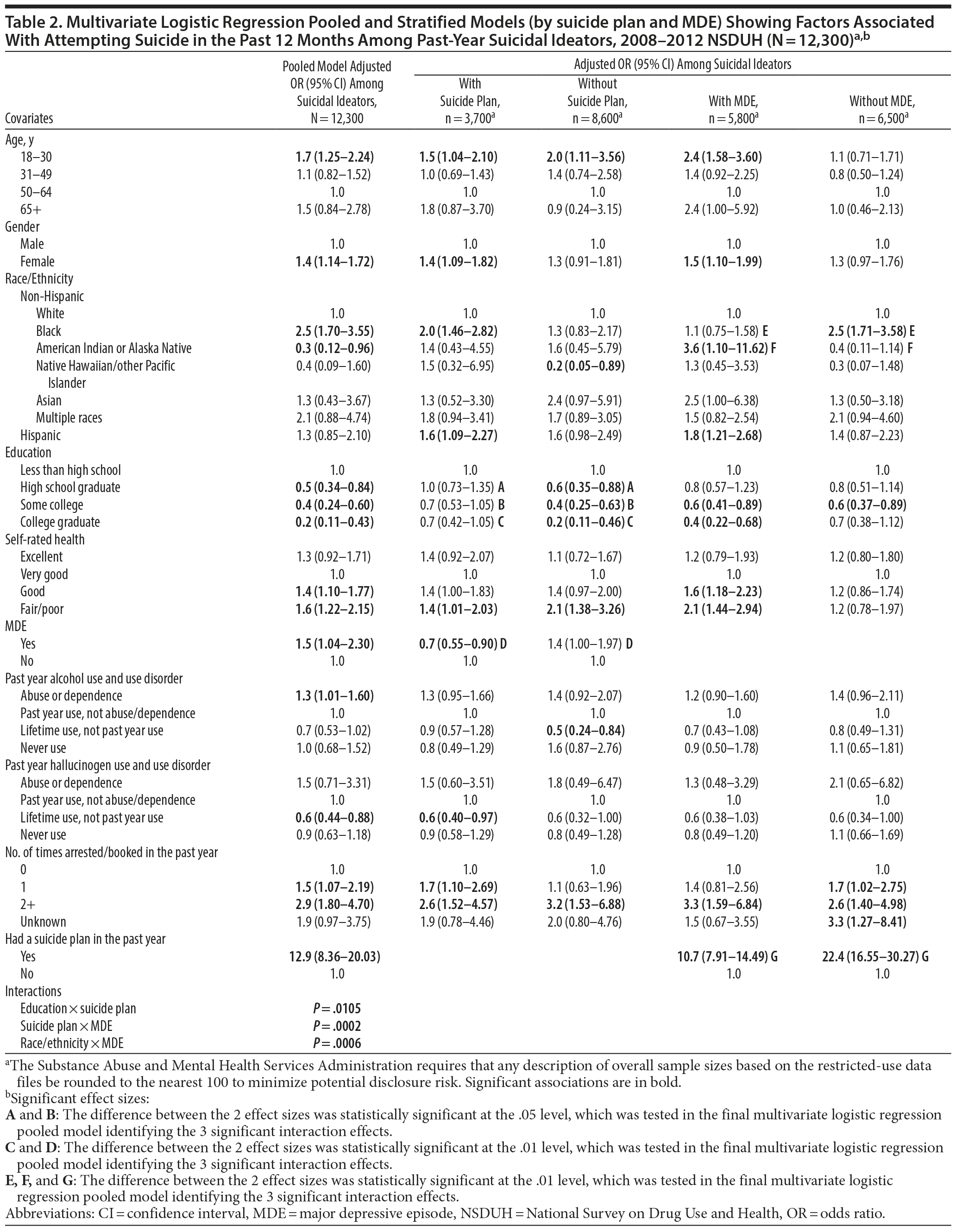
Table 2 shows the results of the multivariate logistic regression pooled model and stratified multivariate models by suicide plan and MDE. Table 2 also highlights significant differences in the effect sizes of factors associated with suicide attempt. Key significant results are summarized below.
Age and gender. Ideators aged 18-30 years were more likely to attempt suicide than ideators aged 50-64 years (adjusted odds ratios [AORs] = 1.5-2.4), except that younger age was not at higher risk for suicide attempt among ideators with MDE. Among ideators with a plan or among ideators with MDE, women were more likely to attempt suicide than men (AORs = 1.4-1.5).
Race/ethnicity. Among ideators with a suicide plan, Hispanics and blacks had a higher suicide attempt risk than whites (AORs = 1.6-2.0). Among ideators without a suicide plan, Native Hawaiians or Pacific Islanders had a lower suicide attempt risk than whites (AOR = 0.2; 95% confidence interval [CI], 0.05-0.89). Among ideators with MDE, Hispanics had a higher suicide attempt risk than whites (AOR = 1.8; 95% CI, 1.21-2.68).
The significant interaction effect between race/ethnicity and MDE indicates that compared with whites, blacks had a higher (AOR = 2.2; 95% CI, 1.28-3.70) suicide attempt risk among ideators without MDE (AOR = 2.5; 95% CI, 1.71-3.58) than among ideators with MDE (AOR = 1.1; 95% CI, 0.75-1.58). Compared with whites, American Indians or Alaska Natives had a much higher (AOR = 10.8; 95% CI, 2.30-51.09) suicide attempt risk among ideators with MDE (AOR = 3.6; 95% CI, 1.10-11.62) than among ideators without MDE (AOR = 0.4; 95% CI, 0.11-1.14).
Education. Among ideators without a suicide plan, those with high school or more education were at lower risk for attempting suicide than those with less than high school education. The significant interaction effect between education and suicide plan suggested that compared with ideators with less than high school education, ideators with high school or more education had a lower (AORs = 0.3-0.5) suicide attempt risk among those without a plan (AORs = 0.2-0.6) than among those with a plan (AORs = 0.7-1.0).
MDE and suicide plan. Similar to results in Figure 2, our multivariate results showed that compared with ideators without a suicide plan, ideators with a suicide plan had a higher (AOR = 2.2; 95% CI, 1.47-3.45) suicide attempt risk among those without MDE (AOR = 22.4; 95% CI, 16.55-30.27) than among those with MDE (AOR = 10.7; 95% CI, 7.91-14.49).
Alcohol use and use disorder. Alcohol use and use disorder was not associated with suicide attempt among ideators with a suicide plan. However, alcohol use and use disorder was strongly associated with suicide attempt among ideators without a suicide plan (P = .0034). Among ideators without a plan, those using alcohol but having no past 12-month alcohol use disorder had similar high suicide attempt risk to those having alcohol use disorder, but lifetime alcohol users without past 12-month use had lower suicide attempt risk than past 12-month alcohol users without use disorder (AOR = 0.5, 95% CI, 0.24-0.84).
Illicit drug use and use disorder. After adjusting for covariates, only past 12-month hallucinogen use and use disorder were associated with suicide attempt at the multivariate level (P = .0060). Among ideators with a plan, those using hallucinogens but having no past 12-month hallucinogen use disorder had similar high suicide attempt risk to those having hallucinogen use disorder, but lifetime hallucinogen users without past 12-month use had lower suicide attempt risk compared with past 12-month hallucinogen users without use disorder (AOR = 0.6, 95% CI, 0.40-0.97).
DISCUSSION
Suicide attempt is a leading risk factor for future attempts and death by suicide.2,3,30,31 To our knowledge, this is the first study examining how past-year sociodemographic characteristics and mental disorders are associated with past 12-month suicide attempt based on nationally representative data and how the associations vary by past 12-month suicide plan and major depression status. Our results may be useful for guiding suicide prevention programs and clinical intervention efforts.
First, this study reveals that employment and marital status are not related to past 12-month suicide attempt among past-year ideators. Some studies reported that unemployment and being unmarried were associated with suicide attempt.19,32 A recent study found that unemployment elevated suicidal ideation risk among adults aged 18-25 years, and being married reduced suicidal ideation risk among adults aged 26 years or older.33 However, once adults have developed suicidal ideation, our study indicates that employment status and marital status are no longer associated with suicide attempt. Employment and marital status may impact an adult’s thoughts of suicide, but they may not directly trigger his/her likelihood of attempting suicide.
Second, this study shows that among past-year ideators, younger age, female gender, racial/ethnic minorities, and lower education were associated with increased risks of past 12-month suicide attempt, depending on suicide plan or major depression status. Our results suggest that clinicians should especially assess suicide risk among depressed American Indian or Alaska Native adults with suicidal ideation, Hispanic ideators with depression or a suicide plan, and black ideators with a suicide plan or without depression. Also, clinicians should be aware that among ideators without a plan, those with low education tend to attempt suicide and should be a target group for suicide prevention efforts.
Third, this study helps clinicians better understand the complex relationships between suicide plan, major depression, and suicide attempt among ideators. Although major depression elevated suicidal ideation risk,33 our results not only confirm a previous finding that major depression, per se, may not trigger further progression from ideation to plan and attempt or from ideation to attempt11 but also highlight the important role that suicide plan plays during the progressions among ideators. We find that among ideators without a plan, major depression was not especially related to suicide attempt. Importantly, ideators with a suicide plan, but without major depression have a higher suicide attempt risk than the 3 groups: ideators with a plan and major depression; ideators without a plan, but with major depression; and ideators with neither a plan nor major depression. Once nondepressed ideators have a suicide plan, their probability to attempt suicide is 22 times higher than nondepressed ideators without a plan. Since lack of major depression does not necessarily prevent ideators from attempting suicide, this study helps clinicians understand the importance of not limiting suicide risk assessments to screening for major depression. Our results support the notion of the suicidality spectrum (suicidal ideation, suicide plan, and suicide attempt) as a separate entity, not just a symptom of MDE or borderline personality disorder.20,34 It is critical that the absence of major depression should not be mistaken for the absence of suicide risk and that suicide prevention efforts target nondepressed ideators with a suicide plan.
Fourth, this study indicates that clinicians need to assess suicide risk among ideators with alcohol use but without a suicide plan. A previous study shows that ideators with lifetime alcohol use disorder but without a plan had an elevated risk for the first suicide attempt.11 Our results reveal that among ideators without a plan, those with past 12-month alcohol use but without use disorder have similar high suicide attempt risk to those with past 12-month alcohol use disorder, but lifetime drinkers with past-year suicidal ideation who abstained from alcohol in the past year have a much lower suicide attempt risk than past 12-month alcohol users. These important findings indicate that suicide prevention programs must pay attention to drinking habits of ideators without a suicide plan and encourage them to abstain from alcohol.
Fifth, to our knowledge, this is the first study that has systematically examined associations between past 12-month specific illicit drug use and use disorders and suicide attempt in the past 12 months among past-year ideators, as the NSDUH provides nationally representative data on substance use and use disorders and suicidal ideation and behavior. Our study reveals that among ideators with a suicide plan, those using hallucinogens but having no past 12-month hallucinogen use disorder have a similar high suicide attempt risk to those having hallucinogen use disorder, but lifetime hallucinogen users without past 12-month use have a much lower suicide attempt risk than past 12-month hallucinogen users. Suicide prevention programs should target ideators with both a suicide plan and hallucinogen use, regardless of their hallucinogen use disorder status, and encourage them to abstain from hallucinogens.
This study has several limitations. NSDUH questionnaires did not measure desire for death among adult respondents and did not ask about suicide attempt among respondents who reported having no past-year suicidal ideation. Also, the endorsement of suicidal ideation and plan was based on single questions that could be interpreted differently by respondents. Moreover, we could not examine the onset time, or the number, severity, and methods of suicide attempts, as the NSDUH did not collect them. NSDUH questionnaires did not measure family history of suicide and suicide attempts and experience with stressful life events, so we could not examine these factors, which may be related to past-year suicide attempt. Importantly, we did not examine the impact of mental health treatment on suicide attempt among ideators because NSDUH questionnaires did not collect the temporal order between receipt of mental health treatment and suicide attempt so that the results related to mental health treatment would be difficult to interpret. Furthermore, NSDUH questionnaires did not collect death by suicide and mental disorders characterized by agitation, impulsiveness, and aggression. In addition, we did not find an association between anxiety disorders and suicide attempt among ideators with a plan, which may be due to potential misclassification of anxiety disorders coded in this study. A respondent may have an anxiety disorder even if they were not told about this diagnosis by a doctor or health professional in the past year. Finally, the NSDUH is a self-reported survey and is subject to recall bias.
Despite these limitations, this study addressed Aspirational Goal 3 of the National Action Alliance for Suicide Prevention’s Research8,9 and examined the complex progressions to past 12-month suicide attempt among US adults with past-year suicidal ideation. Our results may inform suicide-related public awareness programs and help clinicians identify suicidal ideators with especially high risk of attempting suicide. To ultimately improve suicide prevention efforts, further research needs to examine differences in factors predicting suicide attempt and death by suicide among adults with suicidal ideation.
Disclosure of off-label usage: The authors have determined that, to the best of their knowledge, no investigational information about pharmaceutical agents that is outside US Food and Drug Administration-approved labeling has been presented in this article.
Author affiliations: Substance Abuse and Mental Health Services Administration, Rockville, Maryland (Drs Han and McKeon and Mr Gfroerer) and National Institute on Drug Abuse, National Institutes of Health, Bethesda, Maryland (Dr Compton).
Financial disclosure: Dr Compton is a stock shareholder of Pfizer. Drs Han and McKeon and Mr Gfroerer have no personal affiliations or financial relationships with any commercial interest to disclose relative to the article.
Funding/support: None reported.
Disclaimers: The findings and conclusions of this study are those of the authors and do not necessarily reflect the views of the Substance Abuse and Mental Health Services Administration and the National Institute on Drug Abuse of the National Institutes of Health, US Department of Health and Human Services.
Acknowledgments: The authors thank Lisa Colpe, PhD, MPH, of the National Institute of Mental Health, Rockville, Maryland, for her comments on a very earlier draft. Dr Colpe had no conflict of interest to report.
Additional information: The data collection protocol of the National Survey on Drug Use and Health was approved by the Institutional Review Board at the RTI International.
REFERENCES
1. Substance Abuse and Mental Health Services Administration. Results from the 2012 National Survey on Drug Use and Health: Mental Health Findings. NSDUH Series H-47; HHS Publication No. SMA 13-4805. Rockville, MD: Substance Abuse and Mental Health Services Administration; 2013.
2. US Department of Health and Human Services (HHS). Office of the Surgeon General and National Action Alliance for Suicide Prevention. The 2012 national strategy for suicide prevention: goals and objectives for action. http://www.surgeongeneral.gov/library/reports/national-strategy-suicide-prevention/full-report.pdf. Updated September 2012. Accessed on October 15, 2013.
3. Suominen K, Isometsפ E, Suokas J, et al. Completed suicide after a suicide attempt: a 37-year follow-up study. Am J Psychiatry. 2004;161(3):562-563. PubMed doi:10.1176/appi.ajp.161.3.562
4. Kessler RC, Berglund P, Borges G, et al. Trends in suicide ideation, plans, gestures, and attempts in the United States, 1990-1992 to 2001-2003. JAMA. 2005;293(20):2487-2495. PubMed doi:10.1001/jama.293.20.2487
5. While D, Bickley H, Roscoe A, et al. Implementation of mental health service recommendations in England and Wales and suicide rates, 1997-2006: a cross-sectional and before-and-after observational study. Lancet. 2012;379(9820):1005-1012. PubMed doi:10.1016/S0140-6736(11)61712-1
6. Mann JJ, Apter A, Bertolote J, et al. Suicide prevention strategies: a systematic review. JAMA. 2005;294(16):2064-2074. PubMed doi:10.1001/jama.294.16.2064
7. Borges G, Angst J, Nock MK, et al. A risk index for 12-month suicide attempts in the National Comorbidity Survey Replication (NCS-R). Psychol Med. 2006;36(12):1747-1757. PubMed doi:10.1017/S0033291706008786
8. Glenn CR, Nock MK. Improving the short-term prediction of suicidal behavior. Am J Prev Med. 2014;47(suppl 2):S176-S180. PubMed doi:10.1016/j.amepre.2014.06.004
9. Action Alliance for Suicide Prevention. A prioritized research agenda for suicide prevention: an action plan to save lives. http://actionallianceforsuicideprevention.org/sites/
actionallianceforsuicideprevention.org/files/Agenda.pdf. Accessed on August 27, 2014.
10. Kessler RC, Borges G, Walters EE. Prevalence of and risk factors for lifetime suicide attempts in the National Comorbidity Survey. Arch Gen Psychiatry. 1999;56(7):617-626. PubMed doi:10.1001/archpsyc.56.7.617
11. Nock MK, Hwang I, Sampson NA, et al. Mental disorders, comorbidity and suicidal behavior: results from the National Comorbidity Survey Replication. Mol Psychiatry. 2010;15(8):868-876. PubMed doi:10.1038/mp.2009.29
12. Joe S, Baser RE, Breeden G, et al. Prevalence of and risk factors for lifetime suicide attempts among blacks in the United States. JAMA. 2006;296(17):2112-2123. PubMed doi:10.1001/jama.296.17.2112
13. Conner KR, Hesselbrock VM, Meldrum SC, et al. Transitions to, and correlates of, suicidal ideation, plans, and unplanned and planned suicide attempts among 3,729 men and women with alcohol dependence. J Stud Alcohol Drugs. 2007;68(5):654-662. PubMed
14. Centers for Diseases Control and Prevention. Suicide facts at a glance 2012. http://www.cdc.gov/violenceprevention/pdf/Suicide_DataSheet-a.pdf. Accessed on May 1, 2014.
15. Nakagawa A, Grunebaum MF, Oquendo MA, et al. Clinical correlates of planned, more lethal suicide attempts in major depressive disorder. J Affect Disord. 2009;112(1-3):237-242. PubMed doi:10.1016/j.jad.2008.03.021
16. Coryell W, Young EA. Clinical predictors of suicide in primary major depressive disorder. J Clin Psychiatry. 2005;66(4):412-417. PubMed doi:10.4088/JCP.v66n0401
17. Brown GK, Henriques GR, Sosdjan D, et al. Suicide intent and accurate expectations of lethality: predictors of medical lethality of suicide attempts. J Consult Clin Psychol. 2004;72(6):1170-1174. PubMed doi:10.1037/0022-006X.72.6.1170
18. Baca-Garcia E, Perez-Rodriguez MM, Oquendo MA, et al. Estimating risk for suicide attempt: are we asking the right questions? Passive suicidal ideation as a marker for suicidal behavior. J Affect Disord. 2011;134(1-3):327-332. PubMed doi:10.1016/j.jad.2011.06.026
19. Nock MK, Borges G, Bromet EJ, et al. Suicide and suicidal behavior. Epidemiol Rev. 2008;30(1):133-154. PubMed doi:10.1093/epirev/mxn002
20. Oquendo MA, Baca-Garc×a E, Mann JJ, et al. Issues for DSM-V: suicidal behavior as a separate diagnosis on a separate axis. Am J Psychiatry. 2008;165(11):1383-1384. PubMed doi:10.1176/appi.ajp.2008.08020281
21. Substance Abuse and Mental Health Services Administration. National Survey on Drug Use and Health. http://www.oas.samhsa.gov/nsduh.htm. Updated April 14, 2009. Accessed on May 1, 2014.
22. Rockett IR, Wang S, Lian Y, et al. Suicide-associated comorbidity among US males and females: a multiple cause-of-death analysis. Inj Prev. 2007;13(5):311-315. PubMed doi:10.1136/ip.2007.015230
23. Fujino Y, Mizoue T, Tokui N, et al. Prospective cohort study of stress, life satisfaction, self-rated health, insomnia, and suicide death in Japan. Suicide Life Threat Behav. 2005;35(2):227-237. PubMed doi:10.1521/suli.35.2.227.62876
24. American Psychiatric Association. Diagnostic and Statistical Manual of Mental Disorders, Fourth Edition. Washington, DC: American Psychiatric Association; 1994.
25. Grucza RA, Abbacchi AM, Przybeck TR, et al. Discrepancies in estimates of prevalence and correlates of substance use and disorders between two national surveys. Addiction. 2007;102(4):623-629. PubMed doi:10.1111/j.1360-0443.2007.01745.x
26. Jordan BK, Karg RS, Batts KR, et al. A clinical validation of the National Survey on Drug Use and Health assessment of substance use disorders. Addict Behav. 2008;33(6):782-798. PubMed doi:10.1016/j.addbeh.2007.12.007
27. Substance Abuse and Mental Health Services Administration. Reliability of Key Measures in the National Survey on Drug Use and Health. Office of Applied Studies, Methodology Series M-8, HHS Publication No. SMA 09-4425. Rockville, MD: National Institute of Mental Health; 2010.
28. Cook TB. Recent criminal offending and suicide attempts: a national sample. Soc Psychiatry Psychiatr Epidemiol. 2013;48(5):767-774. PubMed
29. Shah B, Barnwell B, Bieler G. SUDAAN User’s Manual. Version 9.1. Research Triangle Park, NC: Research Triangle Institute; 2005.
30. Baca-Garcia E, Perez-Rodriguez MM, Keyes KM, et al. Suicidal ideation and suicide attempts in the United States: 1991-1992 and 2001-2002. Mol Psychiatry. 2010;15(3):250-259. PubMed doi:10.1038/mp.2008.98
31. Baca-Garcia E, Perez-Rodriguez MM, Keyes KM, et al. Suicidal ideation and suicide attempts among Hispanic subgroups in the United States: 1991-1992 and 2001-2002. J Psychiatr Res. 2011;45(4):512-518. PubMed doi:10.1016/j.jpsychires.2010.09.004
32. Burrows S, Auger N, Roy M, et al. Socio-economic inequalities in suicide attempts and suicide mortality in Québec, Canada, 1990-2005. Public Health. 2010;124(2):78-85. PubMed doi:10.1016/j.puhe.2010.01.008
33. Han B, McKeon R, Gfroerer J. Suicidal ideation among community-dwelling adults in the United States. Am J Public Health. 2014;104(3):488-497. PubMed doi:10.2105/AJPH.2013.301600
34. American Psychiatric Association. Diagnostic and Statistical Manual of Mental Disorders, Fifth Edition. Washington, DC: American Psychiatric Association; 2013.
This PDF is free for all visitors!