Objective: To examine the association between individual s’ ‹ymptoms of posttraumatic stress disorder (PTSD) and measures of functioning, quality of life, and suicidal ideation given that previous research has focused on PTSD diagnosis and symptom clusters.
Methods: Data from a large, contemporary, nationally representative sample of 1,484 US military veterans who participated in the National Health and Resilience in Veterans Study from September-October 2013 were analyzed to examine the association between individual DSM-5 PTSD symptoms and measures of mental, physical, and cognitive functioning; quality of life; and suicidal ideation.
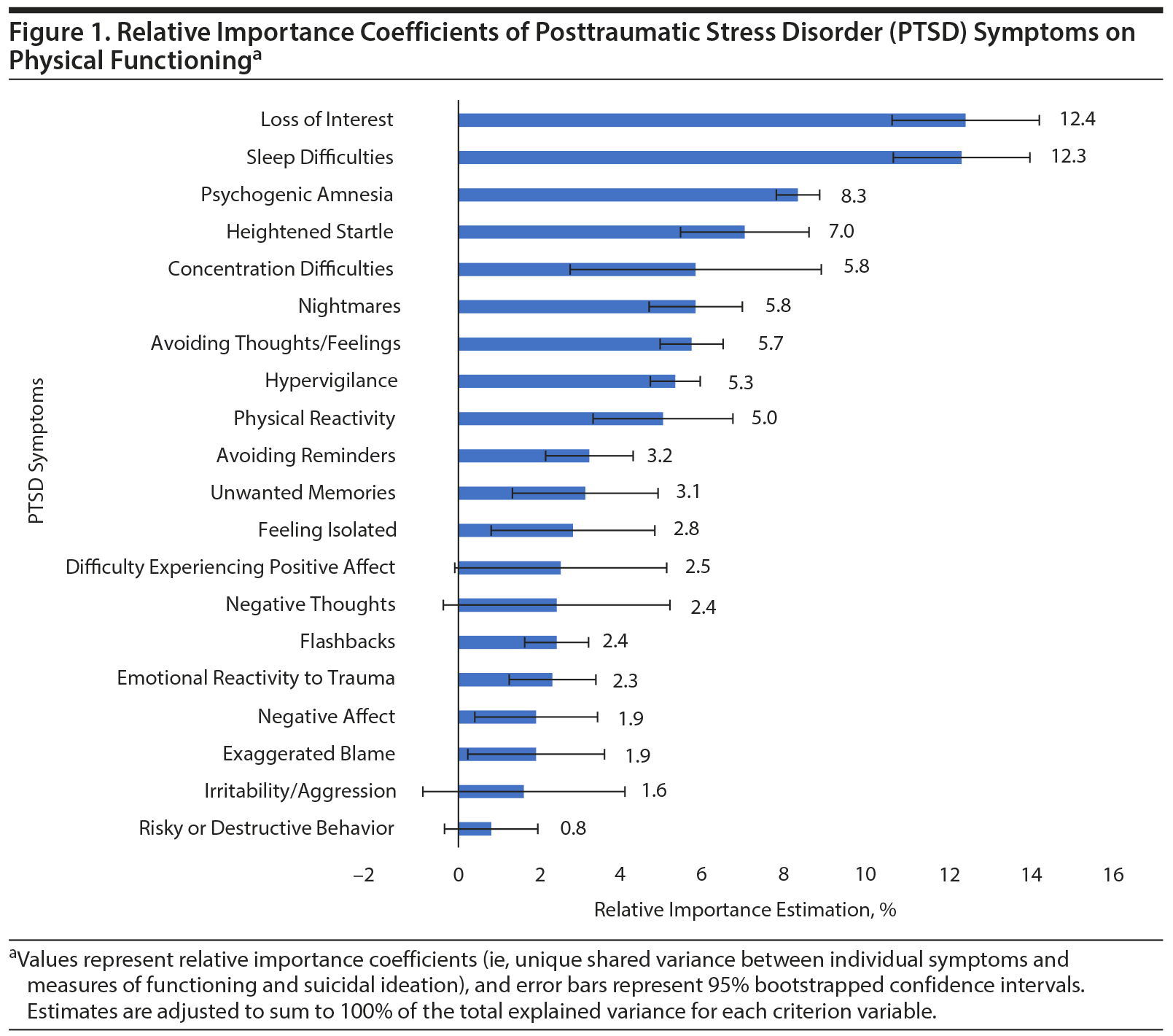
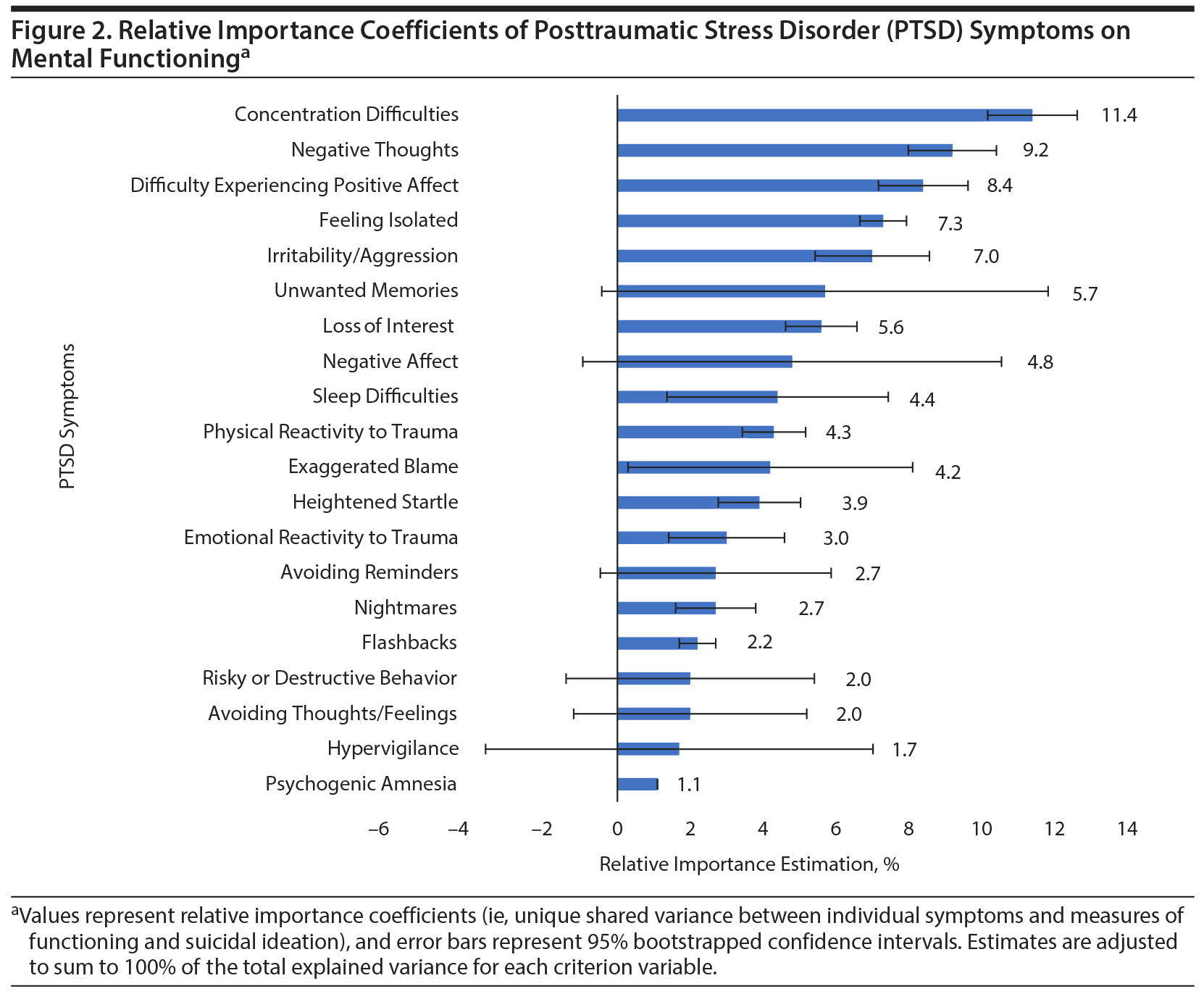
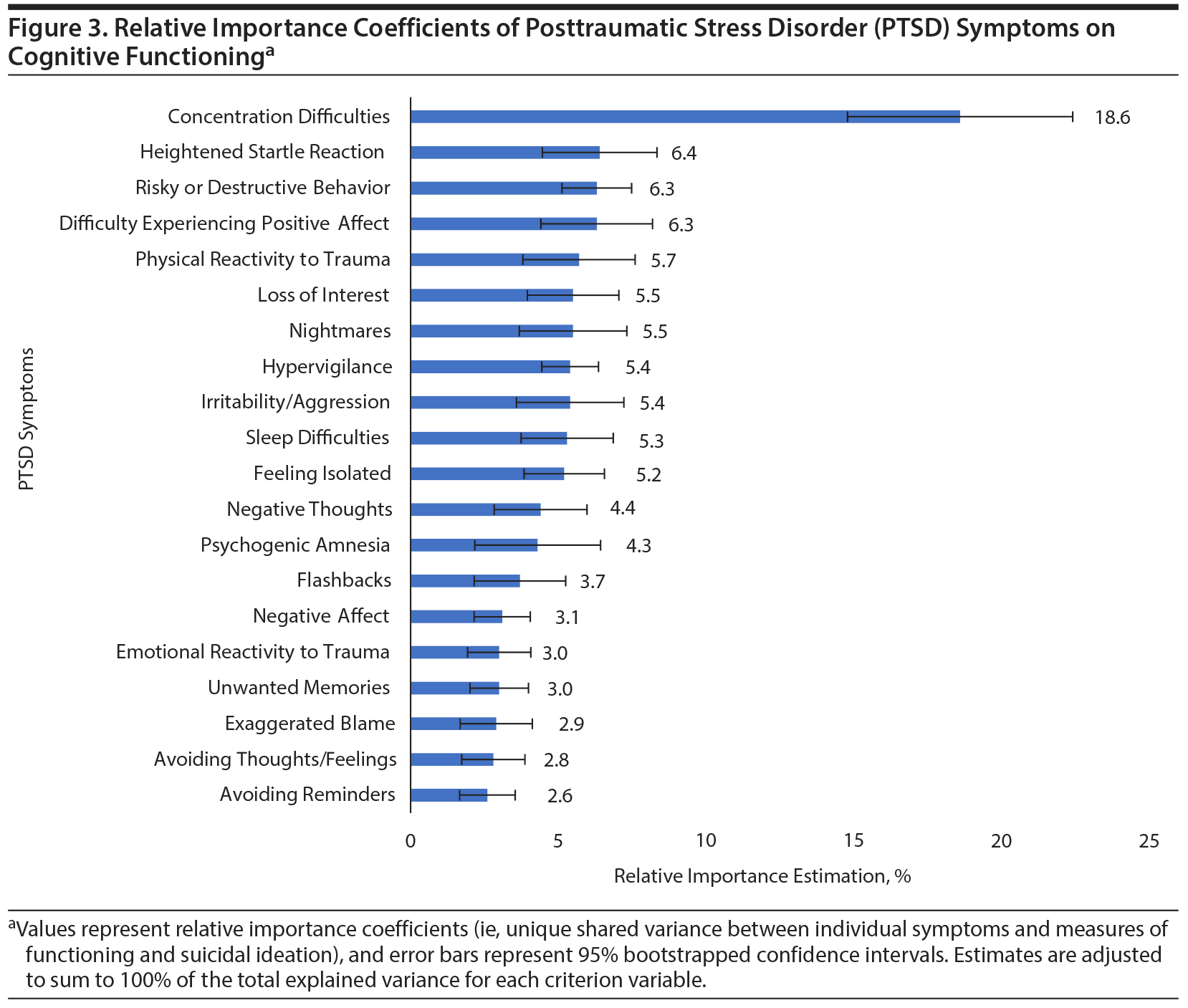
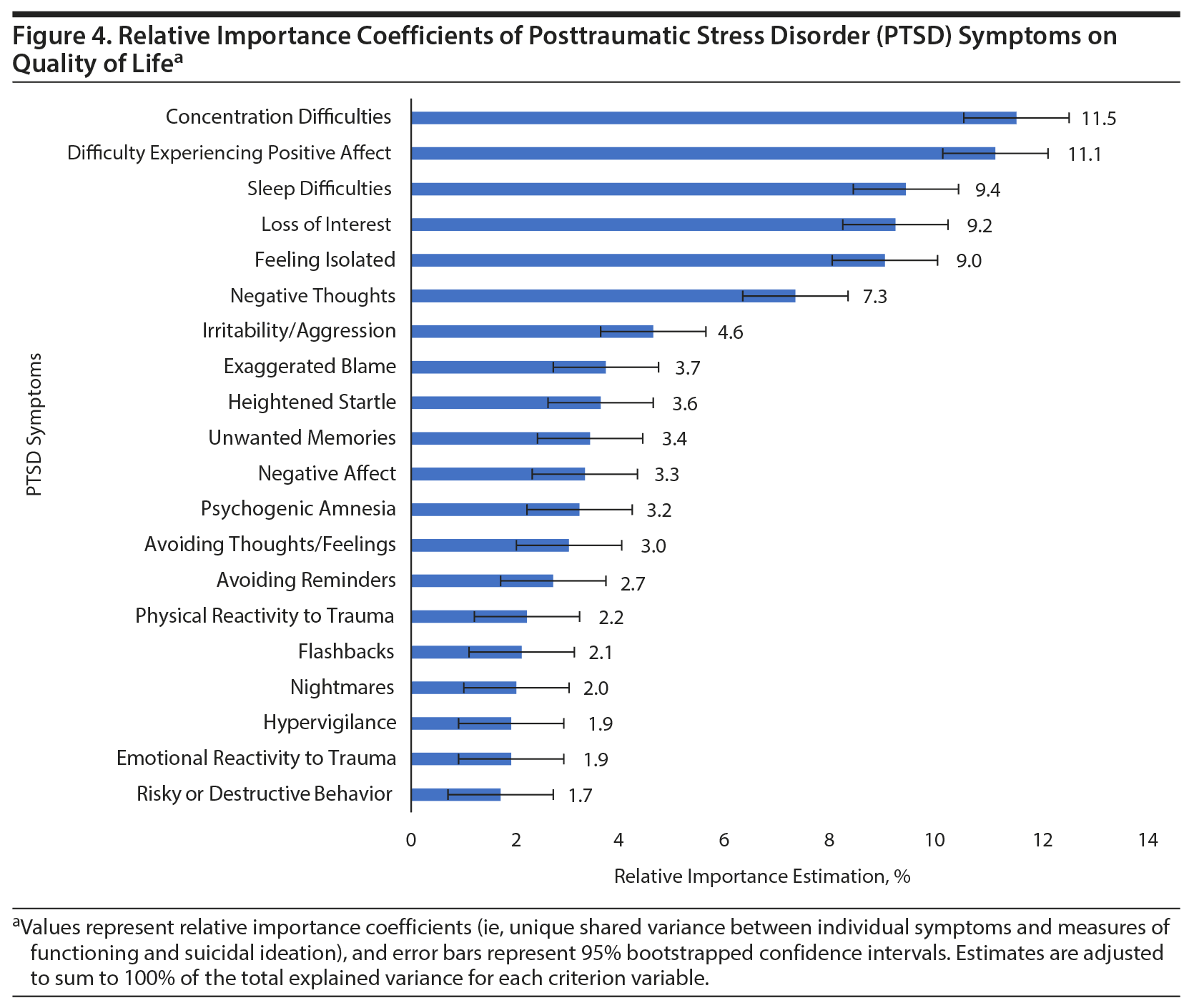
Results: Nonspecific anhedonic and hyperarousal symptoms of PTSD were significantly associated with the various measures of functioning and explained a significant portion of variance across the different measures (P values < .05). Specifically, the following symptoms explained the most variance in physical functioning: loss of interest (12.4%), sleep difficulties (12.3%), and psychogenic amnesia (8.3%); mental functioning: concentration difficulties (11.4%), negative thoughts (9.2%), and difficulties experiencing positive affect (8.4%); cognitive functioning: concentration difficulties (18.6%), heightened startle (6.4%), and difficulty experiencing positive affect and risky/destructive behavior (both 6.3%); quality of life: concentration difficulties (11.5%), difficulty experiencing positive affect (11.1%), and sleep difficulties (9.4%); and suicidal ideation: difficulty experiencing positive affect (12.3%), negative thoughts (11.3%), and irritability/aggression (9.5%). These findings persisted after adjustment for lifetime trauma burden and severity of PTSD and depressive symptoms.
Conclusions: Nonspecific PTSD symptoms are most strongly related to measures of functioning, quality of life, and suicidal ideation in US veterans. These results underscore the potential clinical utility of a symptom-based approach to the assessment, monitoring, and treatment of PTSD.’ ‹
CME Background
Articles are selected for credit designation based on an assessment of the educational needs of CME participants, with the purpose of providing readers with a curriculum of CME articles on a variety of topics throughout each volume. Activities are planned using a process that links identified needs with desired results.
To obtain credit, read the article, correctly answer the questions in thcmee Posttest, and complete the Evaluation. A $10 processing fee will apply.
CME Objective
After studying this article, you should be able to:
● Use a symptom-focused approach for the assessment, monitoring, and treatment of PTSD
Accreditation Statement
The CME Institute of Physicians Postgraduate Press, Inc., is accredited by the Accreditation Council for Continuing Medical Education to provide continuing medical education for physicians.
Credit Designation
The CME Institute of Physicians Postgraduate Press, Inc., designates this journal-based CME activity for a maximum of 1.0 AMA PRA Category 1 Credit™. Physicians should claim only the credit commensurate with the extent of their participation in the activity.
Note: The American Academy of Physician Assistants (AAPA) accepts certificates of participation for educational activities certified for AMA PRA Category 1 Credit™ from organizations accredited by ACCME or a recognized state medical society. Physician assistants may receive a maximum of 1.0 hour of Category I credit for completing this program.
Release, Expiration, and Review Dates
This educational activity was published in April 2019 and is eligible for AMA PRA Category 1 Credit™ through April 30, 2021. The latest review of this material was April 2019.
Financial Disclosure
All individuals in a position to influence the content of this activity were asked to complete a statement regarding all relevant personal financial relationships between themselves or their spouse/partner and any commercial interest. The CME Institute has resolved any conflicts of interest that were identified. In the past year, Larry Culpepper, MD, MPH, Editor in Chief, has been a consultant for Alkermes, Harmony Biosciences, Merck, Shire, Supernus, and Sunovion. No member of the CME Institute staff reported any relevant personal financial relationships. Faculty financial disclosure appears at the end of the article.
ABSTRACT
Objective: To examine the association between individual symptoms of posttraumatic stress disorder (PTSD) and measures of functioning, quality of life, and suicidal ideation given that previous research has focused on PTSD diagnosis and symptom clusters.
Methods: Data from a large, contemporary, nationally representative sample of 1,484 US military veterans who participated in the National Health and Resilience in Veterans Study from September-October 2013 were analyzed to examine the association between individual DSM-5 PTSD symptoms and measures of mental, physical, and cognitive functioning; quality of life; and suicidal ideation.
Results: Nonspecific anhedonic and hyperarousal symptoms of PTSD were significantly associated with the various measures of functioning and explained a significant portion of variance across the different measures (P values < .05). Specifically, the following symptoms explained the most variance in physical functioning: loss of interest (12.4%), sleep difficulties (12.3%), and psychogenic amnesia (8.3%); mental functioning: concentration difficulties (11.4%), negative thoughts (9.2%), and difficulties experiencing positive affect (8.4%); cognitive functioning: concentration difficulties (18.6%), heightened startle (6.4%), and difficulty experiencing positive affect and risky/destructive behavior (both 6.3%); quality of life: concentration difficulties (11.5%), difficulty experiencing positive affect (11.1%), and sleep difficulties (9.4%); and suicidal ideation: difficulty experiencing positive affect (12.3%), negative thoughts (11.3%), and irritability/aggression (9.5%). These findings persisted after adjustment for lifetime trauma burden and severity of PTSD and depressive symptoms.
Conclusions: Nonspecific PTSD symptoms are most strongly related to measures of functioning, quality of life, and suicidal ideation in US veterans. These results underscore the potential clinical utility of a symptom-based approach to the assessment, monitoring, and treatment of PTSD.
Prim Care Companion CNS Disord 2019;21(2):18m02402
To cite: Kachadourian LK, Harpaz-Rotem I, Tsai J, et al. Posttraumatic stress disorder symptoms, functioning, and suicidal ideation in US military veterans: a symptomics approach. Prim Care Companion CNS Disord. 2019;21(2):18m02402.
To share: https://doi.org/10.4088/PCC.18m02402
© Copyright 2019 Physicians Postgraduate Press, Inc.
aUS Department of Veterans Affairs National Center for PTSD, VA Connecticut Healthcare System, West Haven, Connecticut
bDepartment of Psychiatry, Yale University School of Medicine, New Haven, Connecticut
cUS Department of Veterans Affairs New England, Mental Illness Research, Education, and Clinical Center, West Haven, Connecticut
*Corresponding author: Lorig K. Kachadourian, PhD, US Department of Veterans Affairs National Center for PTSD, VA Connecticut Healthcare System, 950 Campbell Ave 116A-4, West Haven, CT 06516 ([email protected]).
Posttraumatic stress disorder (PTSD) is one of the most prevalent psychiatric disorders in military and veteran populations.1,2 PTSD is associated with lower levels of general health, lower overall ratings of general health, more sick call visits, more missed workdays, more physical symptoms, and somatic symptoms.3 PTSD is also highly comorbid with other mental disorders, including substance use4 and mood (eg, major depressive disorder) and anxiety disorders,5 and is associated with an increased risk of suicidal behavior6 and decreased quality of life.7
Research examining the association between PTSD symptom clusters and different aspects of functioning, as opposed to the presence or absence of PTSD, have found the hyperarousal symptom cluster to be strongly associated with physical health problems,8-12 and both the hyperarousal and emotional numbing symptom clusters have been associated with decreased overall quality of life and relationship dysfunction.13,14 The hyperarousal and avoidance/numbing clusters have consistently been shown to be associated with alcohol misuse; the avoidance/numbing cluster also has been associated with heavy smoking.15 Finally, the avoidance and reexperiencing symptom clusters have been associated with an increased risk of suicidal ideation.16,17
To date, the role of individual PTSD symptoms in relation to functional measures relevant to trauma survivors has been largely neglected in previous research studies. Examination of the association between individual PTSD symptoms and such measures is important, as there is great variability in symptom presentation among trauma survivors, and some symptoms may contribute more strongly to different aspects of functioning than others.18 Studies examining individual symptoms in other disorders have been conducted, and findings have provided important information as to which symptoms are more relevant for particular measures of functioning compared to others. For example, Fried and Nesse18 examined the associations between individual depressive symptoms and psychosocial impairment and whether symptoms differed in their associations with different domains including work, home management, social activities, private activities, and close relationships. They found that symptoms varied substantially in their associations depending on the domain, thus underscoring the importance of a symptom-focused approach to identifying correlates of functional difficulties.18
To date, little is known about how individual symptoms of PTSD relate to different measures of functioning relevant to trauma survivors, such as mental, cognitive, and physical functioning, as well as suicidality.13,19-21 For example, Davis et al20 examined the association between individual symptoms of PTSD and suicidal ideation in a sample of trauma-exposed female undergraduates. Results showed that detachment/estrangement was the only PTSD symptom positively associated with suicidal ideation after controlling for negative response bias, depression, type of trauma, and all other PTSD symptoms.20 Another study by Forbes et al13 examined individual symptoms of PTSD—in addition to the different symptom clusters—and quality of life using a sample of injury patients recruited from hospitals in Australia. Findings revealed that the individual PTSD symptoms of anger, hypervigilance, and detachment were most strongly associated with quality of life.13 While these studies provide important insight into how different PTSD symptoms are associated with different measures of functioning in trauma survivors, additional research in population-based samples is needed to evaluate the generalizability of these findings.
In the current study, we sought to build on this emerging body of work to examine the relation between individual DSM-5 PTSD symptoms and different aspects of functioning, quality of life, and suicidal ideation in a large, contemporary, nationally representative sample of US military veterans. To quantify the relative contribution of individual symptoms in relation to these measures, we conducted relative importance (RI) analyses,22,23 which decompose total variance explained in regression models into proportional contributions, thus quantifying the RI of individual symptoms in relation to measures of physical, mental, and cognitive functioning; quality of life; and suicidal ideation.
METHODS
Participants
The sample consisted of 1,484 US military veterans who participated in the National Health and Resilience in Veterans Study (NHRVS), a nationally representative survey that was conducted in 2013. Participants completed a 60-minute anonymous web-based survey. The NHRVS sample was drawn from a research panel of more than 50,000 households and maintained by GfK Knowledge Networks, Inc, a survey research firm in Palo Alto, California. A total of 1,602 adults responded to an initial screening question that confirmed veterans’ status, and 1,484 completed the survey, resulting in a response rate of 92.6%. To permit generalizability of study results to the entire population of US veterans, poststratification weights were computed by GfK statisticians and applied on the basis of demographic distributions (ie, age, sex, race/ethnicity, education, census region, and metropolitan area) from the most recent Current Population Survey (US Census Bureau).24 All participants provided informed consent, and the study was approved by the Human Subjects Subcommittee of the VA Connecticut Healthcare System.
Clinical Points
- Individual posttraumatic stress disorder (PTSD) symptoms are differentially associated with physical, mental, and cognitive functioning; quality of life; and suicidal ideation in US military veterans.
- A symptom-focused approach provides a more nuanced method for the assessment, monitoring, and treatment of PTSD symptoms.
- Treatment approaches for PTSD could be tailored for individual patients depending on their symptom presentation and functional difficulties.
Assessments
Trauma history. History of trauma was assessed using the Trauma History Screen,25 a self-report measure that assesses the occurrence of 13 potentially traumatic life events. Potential traumas across the lifespan including physical or sexual assault during childhood or adulthood, traumatic events during military service, accidents, and unexpected loss of loved ones were assessed. The occurrence of life-threatening illness or injury also was assessed.
PTSD symptoms. Individual symptoms of PTSD were assessed using the Posttraumatic Stress Disorder Checklist for DSM-5 (PCL-5).26 The PCL-5 is a 20-item self-report questionnaire that assesses DSM-5 PTSD symptoms. Respondents are asked to report the extent to which they are bothered by PTSD symptoms in response to their “worst” traumatic event assessed by the Trauma History Screen in the past month from 0 (not at all) to 4 (extremely). The Cronbach α in the current sample was 0.95.
Functioning. Mental and physical health functioning was assessed using the 8-item Short-Form Health Survey (SF-8),27 a validated, abbreviated version of the SF-12,28 one of the most widely used measures of physical and mental health-related functioning. Item responses are used to generate standardized physical component (Cronbach α = 0.85) and mental component (α = 0.85) summary scores. Component summary scores range from 0 to 100, with a score of 50 representing the mean level of functioning in the general population and each 10-point interval representing 1 standard deviation. Higher scores reflect better functioning.
Cognitive functioning was assessed using the Medical Outcomes Study Cognitive Functioning Scale-Revised.29 This 6-item scale assesses past-month difficulties in 6 cognitive domains, including reasoning, concentration and thinking, confusion, memory, attention, and psychomotor speed. Higher scores indicate better functioning (α = 0.93).
Suicidal ideation. Suicidal ideation within the past 2 weeks was assessed using the suicidal ideation item on the Patient Health Questionnaire-9.30 This item was divided into 2 separate questions to assess passive and active suicidal ideation.31 Specifically, participants were asked how often over the past 2 weeks they had been (1) bothered by thoughts that they were better off dead (passive suicidal ideation) and (2) had thoughts of hurting themselves in some way (active suicidal ideation).2 Response options ranged from 0 (not at all) to 3 (nearly every day). These items were combined and recoded (ie, 0 = 0 [absence of passive or active suicidal ideation in the past 2 weeks]; 1-3 = 1 [presence of passive or active suicidal ideation in past 2 weeks]).
Quality of life. Quality of life was assessed with the Quality of Life Enjoyment and Satisfaction Questionnaire-Short Form,32 a 16-item measure that asks respondents about their satisfaction in the past week with various aspects of their lives (eg, work, family). Respondents are asked to rate their satisfaction from 1 (very poor) to 5 (very good), and scores are summed for a total score (α = 0.94).
Data Analysis
Data analyses proceeded in 3 steps. First, to determine whether PTSD symptoms were differentially associated with measures of functioning and suicidal ideation, we conducted 2 sets of regression analyses following Fried and Nesse.18 In the first set, regression weights were free to vary (“heterogeneity model” in which symptoms may be differentially associated with functioning and suicidal ideation). In the second set, regression weights were constrained to be equal (“homogeneity model” in which each symptom contributes equally in predicting functioning and suicidal ideation). A χ2 test was used to compare the 2 models, and collinearity diagnostics were conducted to assess for the presence of multicollinearity. The α was set to 0.001 for these analyses to reduce the likelihood of type I error. Consistent with previous research,18 age and sex were included as covariates. Mplus version 833 was used for these analyses.
Second, to assess the unique proportion of variance in functioning and suicidal ideation measures associated with each PTSD symptom, we conducted RI analyses using the R package relaimpo.34 In these analyses, the LMG metric was used to estimate the RI of each PTSD symptom by dividing the total R2 into individual values of explained variance for each PTSD symptom, which sums to the total explained R2.35 Confidence intervals and P values of the RI coefficients were also computed to determine which PTSD symptoms were significantly associated with each of the dependent variables and to evaluate whether RI differed across PTSD symptoms.
Third, to evaluate whether associations between PTSD symptoms and measures of functioning and suicidal ideation were driven by overall severity of trauma exposure and PTSD symptoms, we conducted a second set of RI analyses, with cumulative lifetime trauma burden and overall PCL-5 scores entered as additional independent variables.
RESULTS
A total of 1,268 veterans in the sample reported having been exposed to trauma. The sample was a mean of 60.6 years of age (SD = 15.2; range, 20-94), predominantly male (89.8%), white (75.0%), and married/cohabitating (68.9%). The mean number of traumas was 4.1 (SD = 2.9; range, 1-15) and mean number of years since index trauma was 24.0 (SD = 19.1; range, 0-92). The most prevalent index traumas were sudden death of close family member or friend (31.3%), life-threatening illness or injury (14.4%), and military-related trauma (8.3%). The mean PCL-5 score was 11.1 (SD = 13.5; range, 0-80), with 142 (13.7%) and 94 (10.1%) veterans scoring ≥ 31, which is indicative of probable PTSD36 on the lifetime and past-month versions of the PCL-5, respectively.
Collinearity diagnostics for regressions comparing homogeneity and heterogeneity models indicated that variance inflation factors did not exceed 5 for any PTSD symptom, indicating no multicollinearity.37 Comparison of these models revealed that the heterogeneity model, which allowed variable contributions of PTSD symptoms to measures of functioning and suicidal ideation, fit the data significantly better than the homogeneity model in which PTSD symptoms were constrained to contribute equally to these variables (P < .001).
As shown in Supplementary Table 1, the heterogeneity model explained 19%-63% of the variance in measures of physical functioning, mental functioning, cognitive functioning, quality of life, and suicidal ideation. With regard to specific symptoms, loss of interest, sleep difficulties, psychogenic amnesia, heightened startle reaction, and avoiding thoughts and feelings were independently associated with physical functioning; physical reactivity to trauma, negative thoughts, difficulty experiencing positive affect, irritability/aggression, unwanted memories, and concentration and sleep difficulties were associated with mental functioning; nightmares, physical reactivity to trauma, psychogenic amnesia, negative thoughts and affect, difficulty experiencing positive affect, irritability/aggression, heightened startle reaction, and concentration and sleep difficulties were associated with cognitive functioning; psychogenic amnesia, negative thoughts, loss of interest, feeling isolated, difficulty experiencing positive affect, and concentration and sleep difficulties were associated with quality of life; and negative thoughts, difficulty experiencing positive affect, and risky or destructive behavior were associated with suicidal ideation.
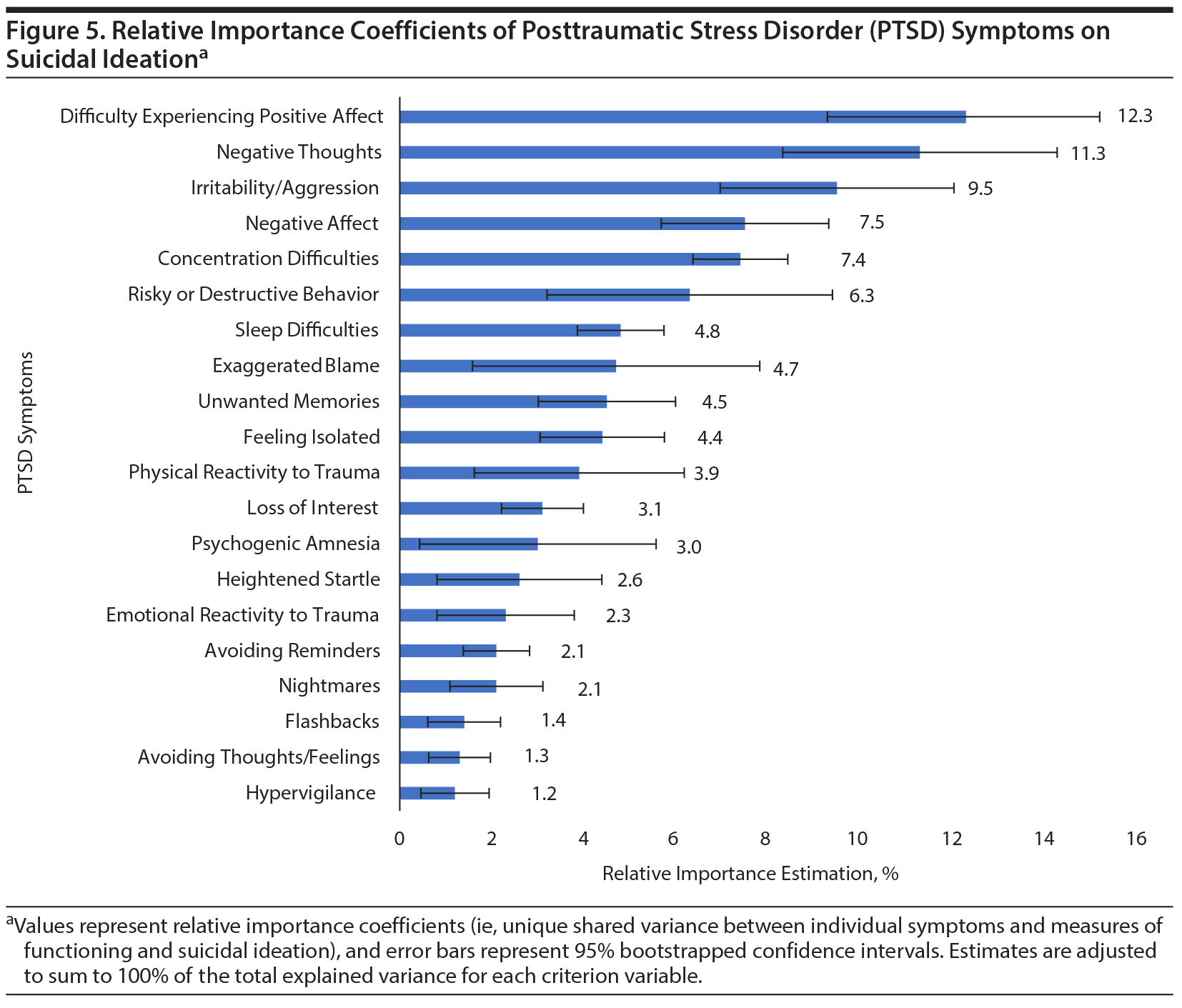
Figures 1, 2, 3, 4, and 5 show the RI estimates of each of the PTSD symptoms in relation to measures of functioning, quality of life, and suicidal ideation. Specifically, for physical functioning, symptoms with the greatest RI coefficients included loss of interest (12.4%), sleep difficulties (12.3%), and psychogenic amnesia (8.3%). For mental functioning, symptoms with the greatest RI coefficients included concentration difficulties (11.4%), negative thoughts (9.2%), and difficulties experiencing positive affect (8.4%). For cognitive functioning, symptoms with the greatest RI coefficients included concentration difficulties (18.6%), heightened startle (6.4%), and difficulty experiencing positive affect and risky/destructive behavior (both 6.3%). For quality of life, symptoms with the greatest RI coefficients included concentration difficulties (11.5%), difficulty experiencing positive affect (11.1%), and sleep difficulties (9.4%). For suicidal ideation, symptoms with the greatest RI coefficients included difficulty experiencing positive affect (12.3%), negative thoughts (11.3%), and irritability/aggression (9.5%).
Incorporation of severity of trauma exposure and PTSD symptoms into the RI analyses revealed that severity of trauma exposure and PTSD symptoms explained a mean of 3.6% (range, 0.8%-10.0%) and 6.2% (range, 4.8%-6.9%) of the total variance in measures of functioning, quality of life, and suicidal ideation, respectively, with the same PTSD symptoms showing significant associations with these measures. These results suggest that the nature of PTSD symptoms shows unique associations with these measures, above and beyond overall severity of trauma exposure and PTSD symptoms.
Given that depressive symptoms may additionally contribute to reductions in functioning and quality of life and suicide risk,38-41 we also conducted analyses that included current depressive symptoms, which were assessed using the Patient Health Questionnaire-2.42 Results of these analyses revealed increases in R2 values: 0.23 for physical functioning, 0.67 for mental functioning, 0.66 for cognitive functioning, 0.49 for quality of life, and 0.45 for suicidal ideation. Depressive symptoms explained 6.6%, 21.5%, 9.1%, 19.9%, and 26.6% of the total variance in measures of physical, mental, and cognitive functioning; quality of life; and suicidal ideation, respectively. The same individual PTSD symptoms that explained the most variance in these measures remained significant, albeit reduced in magnitude, in these analyses.
DISCUSSION
The relatively new approach of examining individual symptoms associated with measures of functioning, quality of life, and suicidality provides more nuanced information as to which specific symptoms are most strongly and uniquely related to such measures. This approach could help inform more personalized prevention and treatment approaches in veterans and other trauma-affected populations at risk for or currently suffering from PTSD symptoms.
In the current study, although certain trauma-specific PTSD symptoms explained a significant portion of variance in certain measures of functioning (eg, heightened startle and cognitive functioning), the nonspecific symptoms of this disorder (eg, concentration difficulties, sleep difficulties, loss of interest) were the strongest correlates across various measures in terms of the proportion of relative variance explained. For example, sleep difficulties explained a significant proportion of variance in physical functioning and quality of life, and concentration difficulties explained a significant proportion of variance in mental functioning, cognitive functioning, and quality of life. Difficulty experiencing positive affect also was a robust correlate of mental functioning, quality of life, and suicidal ideation. Of note, when depressive symptoms were incorporated into the RI analyses, they explained a considerable proportion of variance in measures of mental functioning, quality of life, and suicidal ideation (19.9%-26.6% relative variance explained). This finding, which is consistent with prior work, underscores the importance of nonspecific PTSD and depressive symptoms in contributing to functional difficulties, reduced quality of life, and suicide risk in trauma survivors.
Interestingly, some of the nonspecific PTSD symptoms typically considered to be more anhedonic in nature (eg, loss of interest, negative thoughts, difficulty experiencing positive affect) appeared to have a significant deleterious effect on functioning, quality of life, and suicidal ideation. This finding is consistent with recent research documenting a 7-factor model of DSM-5 symptoms of PTSD that showed an anhedonic symptom cluster to be strongly associated with mental functioning and quality of life,43 as well as with other research documenting strong associations between emotional numbing and generalized distress.31
Some of the current findings differed from previous research. For example, Forbes et al13 found symptoms of anger/irritability, hypervigilance, and detachment (ie, feelings of isolation) to be most strongly associated with quality of life, whereas in the current study, concentration difficulties, difficulty experiencing positive affect, and sleep difficulties were the strongest correlates. Previous research20 also found feelings of detachment/estrangement to be most strongly associated with suicidal ideation; however, in the current study, difficulty experiencing positive affect, negative thoughts, and irritability/aggression were found to be the strongest correlates. Differences between these studies and the current study could be due to the samples used. The Forbes et al13 study analyzed data from a community sample who primarily experienced motor vehicle accidents as their traumas, and the Davis et al20 study analyzed data from female undergraduate students. Both samples differ from the current sample of older, predominantly male, non-combat-exposed veterans, whose index traumas occurred an average of 24 years earlier. That said, our research findings are consistent with other previous research44 documenting associations between both internalizing (eg, difficulty experiencing positive affect) and externalizing (eg, irritability/aggression) symptoms and suicidal ideation. Our findings are also consistent with other research45,46 that found emotional numbing is strongly linked to reduced psychosocial functioning in military samples.
The current findings suggest that it may be useful to target more general, nonspecific PTSD symptoms, in addition to more trauma-specific symptoms (eg, intrusive memories and nightmares, avoiding thoughts and feelings related to the trauma), in PTSD prevention and treatment efforts in veterans. At the same time, the strongest correlates differed across domains, underscoring the importance of taking a more symptom-focused approach not only to the assessment and monitoring of PTSD, but also in treatment efforts designed to enhance specific functional outcomes and to mitigate suicide risk. For example, although measures designed to assess the severity of PTSD symptoms (eg, PCL-5) typically involve summing the responses of each symptom to create a total severity score, individual elevated symptoms could be more closely examined to guide treatment. Such treatment approaches could be tailored for individuals depending on their symptom presentation and functional difficulties. Although evidence-based treatments that target PTSD symptoms more generally (eg, prolonged exposure,47 cognitive-processing therapy48) are routinely implemented with veterans, interventions that target specific symptoms could also be implemented as either stand-alone or adjunctive treatments. For example, targeting anhedonic/internalizing symptoms in combination with externalizing symptoms of irritability and aggression with psychological treatments that focus on anger management49 or depression (eg, behavioral activation50) may be useful in mitigating suicide risk in veterans. Further, targeting sleep difficulties using treatments such as cognitive-behavioral therapy for insomnia51 may help mitigate physical difficulties and preserve overall quality of life in this population. Further research is needed to evaluate the efficacy of such approaches in promoting functional outcomes and quality of life and in mitigating suicide risk in veterans and other trauma-affected populations.
Limitations of the current study include the cross-sectional nature of the investigation, which temper conclusions regarding causality. Furthermore, all variables were assessed via self-report, and the assessment of suicidal ideation was limited in that it only consisted of 2 items. Future research that includes a more comprehensive assessment of suicidality would be important in further elucidating symptom-level associations with different aspects of suicidality. Finally, the current findings also may be generalizable to a certain subset of military veterans, as this sample consisted of older, primarily male, noncombat veterans who experienced their “worst” traumatic events many years earlier. These individuals may be more likely to experience the specific kinds of PTSD symptoms endorsed and thus more likely to have functional problems as a consequence of them.
These limitations notwithstanding, the current study adds to the burgeoning “symptomics” literature by examining how individual symptoms of particular psychiatric disorders may be linked to outcomes of interest in these populations.18 This is a novel approach that provides insight into how the more nuanced clinical manifestation of these disorders may affect functioning, quality of life, and other clinical measures relevant in these populations, such as suicidality. Further research is needed to evaluate the generalizability of these results in other samples of trauma survivors; identify longitudinal associations between individual PTSD symptoms and measures of functioning, quality of life, and suicidality; and determine the clinical utility of symptom-based approaches in assessment, monitoring, and treatment of PTSD and other psychiatric disorders.
Submitted: October 25, 2018; accepted January 26, 2019.
Published online: April 25, 2019.
Disclosure of off-label usage: The authors have determined that, to the best of their knowledge, no investigational information about pharmaceutical agents that is outside US Food and Drug Administration-approved labeling has been presented in this article.
Financial disclosure: Dr Pietrzak is a scientific consultant to Cogstate, Ltd, for work that bears no relationship to the current project. Drs Kachadourian, Harpaz-Rotem, Tsai, and Southwick have no personal affiliations or financial relationships with any commercial interest to disclose relative to this article.
Funding/support: This work was supported in part by Career Development Award no. IK2 CX-001259-01 from the US Department of Veterans Affairs Clinical Sciences R&D Service (Dr Kachadourian). The National Health and Resilience in Veterans Study is supported by the US Department of Veterans Affairs National Center for Posttraumatic Stress Disorder.
Role of the sponsor: The sponsor had no role in the design and conduct of the study; collection, management, analysis, and interpretation of data; or preparation, review, or approval of the manuscript.
Disclaimer: The views and opinions expressed in this report are those of the authors and should not be construed to represent the US government.
Supplementary material: See accompanying pages.
Find more articles on this and other psychiatry and CNS topics:
The Journal of Clinical Psychiatry
The Primary Care Companion for CNS Disorders
REFERENCES
1. Hoge CW, Auchterlonie JL, Milliken CS. Mental health problems, use of mental health services, and attrition from military service after returning from deployment to Iraq or Afghanistan. JAMA. 2006;295(9):1023-1032. PubMed CrossRef
2. Dohrenwend BP, Turner JB, Turse NA, et al. The psychological risks of Vietnam for US veterans: a revisit with new data and methods. Science. 2006;313(5789):979-982. PubMed CrossRef
3. Hoge CW, Terhakopian A, Castro CA, et al. Association of posttraumatic stress disorder with somatic symptoms, health care visits, and absenteeism among Iraq war veterans. Am J Psychiatry. 2007;164(1):150-153. PubMed CrossRef
4. Jakupcak M, Tull MT, McDermott MJ, et al. PTSD symptom clusters in relationship to alcohol misuse among Iraq and Afghanistan war veterans seeking post-deployment VA health care. Addict Behav. 2010;35(9):840-843. PubMed CrossRef
5. Pietrzak RH, Goldstein RB, Southwick SM, et al. Prevalence and Axis I comorbidity of full and partial posttraumatic stress disorder in the United States: results from wave 2 of the National Epidemiologic Survey on Alcohol and Related Conditions. J Anxiety Disord. 2011;25(3):456-465. PubMed CrossRef
6. Pietrzak RH, Goldstein MB, Malley JC, et al. Risk and protective factors associated with suicidal ideation in veterans of Operations Enduring Freedom and Iraqi Freedom. J Affect Disord. 2010;123(1-3):102-107. PubMed CrossRef
7. Schnurr PP, Lunney CA, Bovin MJ, et al. Posttraumatic stress disorder and quality of life: extension of findings to veterans of the wars in Iraq and Afghanistan. Clin Psychol Rev. 2009;29(8):727-735. PubMed CrossRef
8. Clum GA, Nishith P, Resick PA. Trauma-related sleep disturbance and self-reported physical health symptoms in treatment-seeking female rape victims. J Nerv Ment Dis. 2001;189(9):618-622. PubMed CrossRef
9. Kimerling R, Clum GA, Wolfe J. Relationships among trauma exposure, chronic posttraumatic stress disorder symptoms, and self-reported health in women: replication and extension. J Trauma Stress. 2000;13(1):115-128. PubMed CrossRef
10. Norris RL, Maguen S, Litz BT, et al. Physical health symptoms in peacekeepers: has the role of deployment stress been overrated? Stress Trauma Crisis Int J. 2005;8(4):251-265. CrossRef
11. Tsai J, Harpaz-Rotem I, Armour C, et al. Dimensional structure of DSM-5 posttraumatic stress disorder symptoms: results from the National Health and Resilience in Veterans Study. J Clin Psychiatry. 2015;76(5):546-553. PubMed CrossRef
12. Woods SJ, Wineman NM. Trauma, posttraumatic stress disorder symptom clusters, and physical health symptoms in post abused women. Arch Psychiatr Nurs. 2004;18(1):26-34. PubMed
13. Forbes D, Nickerson A, Bryant RA, et al. The impact of post-traumatic stress disorder symptomatology on quality of life: the sentinel experience of anger, hypervigilance and restricted affect [published online ahead of print May 1, 2018]. Aust N Z J Psychiatry. PubMed CrossRef
14. Taft CT, Watkins LE, Stafford J, et al. Posttraumatic stress disorder and intimate relationship problems: a meta-analysis. J Consult Clin Psychol. 2011;79(1):22-33. PubMed CrossRef
15. Cook J, Jakupcak M, Rosenheck R, et al. Influence of PTSD symptom clusters on smoking status among help-seeking Iraq and Afghanistan veterans. Nicotine Tob Res. 2009;11(10):1189-1195. PubMed CrossRef
16. Bell JB, Nye EC. Specific symptoms predict suicidal ideation in Vietnam combat veterans with chronic post-traumatic stress disorder. Mil Med. 2007;172(11):1144-1147. PubMed CrossRef
17. Lemaire CM, Graham DP. Factors associated with suicidal ideation in OEF/OIF veterans. J Affect Disord. 2011;130(1-2):231-238. PubMed CrossRef
18. Fried EI, Nesse RM. The impact of individual depressive symptoms on impairment of psychosocial functioning. PLoS One. 2014;9(2):e90311. PubMed CrossRef
19. Bensley KM, Seelig AD, Armenta RF, et al. Posttraumatic stress disorder symptom association with subsequent risky and problem drinking initiation. J Addict Med. 2018;12(5):353-362. PubMed CrossRef
20. Davis MT, Witte TK, Weathers FW. Posttraumatic stress disorder and suicidal ideation: the role of specific symptoms within the framework of the interpersonal-psychological theory of suicide. Psychol Trauma. 2014;6(6):610-618. CrossRef
21. Seelig AD, Bensley KM, Williams EC, et al; Millennium Cohort Study Team. Longitudinal examination of the influence of individual posttraumatic stress disorder symptoms and clusters of symptoms on the initiation of cigarette smoking. J Addict Med. 2018;12(5):363-372. PubMed CrossRef
22. Tonidandel S, LeBreton JM. Determining the relative importance of predictors in logistic regression: an extension of relative weights analysis. Organ Res Methods. 2010;13(4):767-781. CrossRef
23. Tonidandel S, LeBreton JM. Relative importance analysis: a useful supplement to regression analysis. J Bus Psychol. 2011;26(1):1-9. CrossRef
24. United States Census Bureau. Current Population Survey (CPS). https://www.census.gov/programs-surveys/cps.html. Accessed March 14, 2019.
25. Carlson EB, Smith SR, Palmieri PA, et al. Development and validation of a brief self-report measure of trauma exposure: the Trauma History Screen. Psychol Assess. 2011;23(2):463-477. PubMed CrossRef
26. Weathers FW, Litz BT, Keane TM, et al. The PTSD Checklist for DSM-5 (PCL-5). Washington, DC: US Department of Veterans Affairs, National Center for Posttraumatic Stress Disorder; 2013.
27. Ware JE, Kosinski M, Dewey JE, et al. How to Score and Interpret Single Item Health Status Measures: A Manual for Users of the SF-8 Health Survey. Lincoln, RI: Quality Metric Incorporated; 2001.
28. Ware JE, Kosinski M, Tuner-Bowker DM, et al. Version 2 of the SF-12 Health Survey. Boston, MA: Quality Metric; 2002.
29. Stewart AL, Ware JE, Sherbourne CD, et al. Psychological distress/well-being and cognitive functioning measures. In: Stewart AL, Ware JE, eds. Measuring Functioning and Well-Being: The Medical Outcomes Study Approach. Durham, NC: Duke University; 1992:102-142.
30. Kroenke K, Spitzer RL. The PHQ-9: a new depression diagnostic and severity measure. Psychiatr Ann. 2002;32(9):509-521. CrossRef
31. Thompson KE, Vasterling JJ, Benotsch EG, et al. Early symptom predictors of chronic distress in Gulf War veterans. J Nerv Ment Dis. 2004;192(2):146-152. PubMed CrossRef
32. Endicott J, Nee J, Harrison W, et al. Quality of Life Enjoyment and Satisfaction Questionnaire: A new measure. Psychopharmacol Bull. 1993;29(2):321-326. PubMed
33. Muthén, LK, Muthén, BO. Mplus User’s Guide, 8th ed. Los Angeles, CA: Muthén & Muthén; 1998-2017.
34. Grömping U. Relative importance for linear regression in R: the package relaimpo. J Stat Softw. 2006;17(1):1-27. CrossRef
35. Grömping U. Estimators of relative importance in linear regression based on variance decomposition. Am Stat. 2007;61(2):139-147. CrossRef
36. Bovin MJ, Marx BP, Weathers FW, et al. Psychometric properties of the PTSD Checklist for Diagnostic and Statistical Manual of Mental Disorders-Fifth Edition (PCL-5) in veterans. Psychol Assess. 2016;28(11):1379-1391. PubMed CrossRef
37. Heiberger RM, Holland B. Statistical Analysis and Data Display: An Intermediate Course with Examples in S-plus, R, and SAS. New York, NY: Springer Texts in Statistics; 2004.
38. Hirschfeld RM, Montgomery SA, Keller MB, et al. Social functioning in depression: a review. J Clin Psychiatry. 2000;61(4):268-275. PubMed CrossRef
39. Wang S, Blazer DG. Depression and cognition in the elderly. Annu Rev Clin Psychol. 2015;11(1):331-360. PubMed CrossRef
40. Sivertsen H, Bj׸rkl׸f GH, Engedal K, et al. Depression and quality of life in older persons: a review. Dement Geriatr Cogn Disord. 2015;40(5-6):311-339. PubMed CrossRef
41. Bachmann S. Epidemiology of suicide and the psychiatric perspective. Int J Environ Res Public Health. 2018;15(7):1425. PubMed CrossRef
42. Kroenke K, Spitzer RL, Williams JB. The Patient Health Questionnaire-2: validity of a two-item depression screener. Med Care. 2003;41(11):1284-1292. PubMed CrossRef
43. Pietrzak RH, Tsai J, Armour C, et al. Functional significance of a novel 7-factor model of DSM-5 PTSD symptoms: results from the National Health and Resilience in Veterans study. J Affect Disord. 2015;174(174):522-526. PubMed CrossRef
44. Brezo J, Paris J, Turecki G. Personality traits as correlates of suicidal ideation, suicide attempts, and suicide completions: a systematic review. Acta Psychiatr Scand. 2006;113(3):180-206. PubMed CrossRef
45. Rona RJ, Jones M, Iversen A, et al. The impact of posttraumatic stress disorder on impairment in the UK military at the time of the Iraq war. J Psychiatr Res. 2009;43(6):649-655. PubMed CrossRef
46. Sayers SL, Farrow VA, Ross J, et al. Family problems among recently returned military veterans referred for a mental health evaluation. J Clin Psychiatry. 2009;70(2):163-170. PubMed CrossRef
47. Foa EB, Hembree EA, Cahill SP, et al. Randomized trial of prolonged exposure for posttraumatic stress disorder with and without cognitive restructuring: outcome at academic and community clinics. J Consult Clin Psychol. 2005;73(5):953-964. PubMed CrossRef
48. Resick PA, Nishith P, Weaver TL, et al. A comparison of cognitive-processing therapy with prolonged exposure and a waiting condition for the treatment of chronic posttraumatic stress disorder in female rape victims. J Consult Clin Psychol. 2002;70(4):867-879. PubMed CrossRef
49. Shea MT, Lambert J, Reddy MK. A randomized pilot study of anger treatment for Iraq and Afghanistan veterans. Behav Res Ther. 2013;51(10):607-613. PubMed CrossRef
50. Addis ME, Martell CM. Overcoming Depression One Step at a Time. Oakland, CA: Harbinger Publications; 2004.
51. Perlis ML, Jungquist C, Smith MT, et al. Cognitive Behavioral Treatment of Insomnia. New York, NY: Springer; 2005.
Enjoy this premium PDF as part of your membership benefits!