Objective: Patients with first-episode psychosis have a high prevalence of tobacco use. We aimed to examine the prevalence and course of tobacco use during early psychosis using meta-analysis.
Data Sources: Systematic search of MEDLINE (1948-2011), Embase (1947-2011), CINAHL (1984-2011), PsycINFO (1967-2011), and ISI Web of Science (1900-2011) using the search terms [psychosis OR schizophrenia] AND [tobacco OR smoking OR nicotine].
Study Selection: We located 10 studies reporting the age at initiation of daily tobacco use and the age at onset of psychosis, 31 studies reporting prevalence of tobacco use in patients with first-episode psychosis, 10 studies comparing smoking to age-/gender-matched controls, and 7 studies reporting prevalence of tobacco use at intervals after treatment.
Data Extraction: The following data were extracted: age at initiation of daily tobacco use and at onset of psychosis, the proportion of patients with first-episode psychosis who used tobacco, the proportion of the general population who used tobacco, and the proportion of patients with psychosis who used tobacco at various intervals after initiation of antipsychotic treatment.
Results: The pooled estimate for the interval between initiation of tobacco use and the onset of psychosis was 5.3 years (standardized mean difference = 0.85). The estimated prevalence of tobacco users in first episode of psychosis is 58.9% (95% CI, 54.3%-63.4%). There is a strong association between first-episode psychosis and tobacco use (OR = 6.04; 95% CI, 3.03-12.02) compared with healthy controls. The prevalence of tobacco use at intervals between 6 and 120 months after treatment remained unchanged (OR = 0.996; 95% CI, 0.907-1.094).
Conclusions: Patients with first-episode psychosis tend to have smoked for some years prior to the onset of psychosis, have high prevalence of tobacco use at the time of presenting for treatment, and are much more likely to smoke than aged-matched controls. Their apparent difficulty in quitting has implications for tobacco cessation programs and efforts to reduce cardiovascular disease among people with mental illness.
J Clin Psychiatry 2012;73(4):468-475
© Copyright 2012 Physicians Postgraduate Press, Inc.
Submitted: June 18, 2011; accepted September 15, 2011. (doi:10.4088/JCP.11r07222).
Corresponding author: Hannah Newall, MBBS, Coffs Harbour Health Campus, Pacific Hwy, Coffs Harbour, 2450 Australia ([email protected]).
See related blog by Newall.
Find more articles on this and other psychiatry and CNS topics:
The Journal of Clinical Psychiatry
The Primary Care Companion for CNS Disorders
ABSTRACT
Objective: Patients with first-episode psychosis have a high prevalence of tobacco use. We aimed to examine the prevalence and course of tobacco use during early psychosis using meta-analysis.
Data Sources: Systematic search of MEDLINE (1948-2011), Embase (1947-2011), CINAHL (1984-2011), PsycINFO (1967-2011), and ISI Web of Science (1900-2011) using the search terms [psychosis OR schizophrenia] AND [tobacco OR smoking OR nicotine].
Study Selection: We located 10 studies reporting the age at initiation of daily tobacco use and the age at onset of psychosis, 31 studies reporting prevalence of tobacco use in patients with first-episode psychosis, 10 studies comparing smoking to age-/gender-matched controls, and 7 studies reporting prevalence of tobacco use at intervals after treatment.
Data Extraction: The following data were extracted: age at initiation of daily tobacco use and at onset of psychosis, the proportion of patients with first-episode psychosis who used tobacco, the proportion of the general population who used tobacco, and the proportion of patients with psychosis who used tobacco at various intervals after initiation of antipsychotic treatment.
Results: The pooled estimate for the interval between initiation of tobacco use and the onset of psychosis was 5.3 years (standardized mean difference = 0.85). The estimated prevalence of tobacco users in first episode of psychosis is 58.9% (95% CI, 54.3%-63.4%). There is a strong association between first-episode psychosis and tobacco use (OR = 6.04; 95% CI, 3.03-12.02) compared with healthy controls. The prevalence of tobacco use at intervals between 6 and 120 months after treatment remained unchanged (OR = 0.996; 95% CI, 0.907-1.094).
Conclusions: Patients with first-episode psychosis tend to have smoked for some years prior to the onset of psychosis, have high prevalence of tobacco use at the time of presenting for treatment, and are much more likely to smoke than aged-matched controls. Their apparent difficulty in quitting has implications for tobacco cessation programs and efforts to reduce cardiovascular disease among people with mental illness.
J Clin Psychiatry 2012;73(4):468-475
© Copyright 2012 Physicians Postgraduate Press, Inc.
Submitted: June 18, 2011; accepted September 15, 2011. (doi:10.4088/JCP.11r07222).
Corresponding author: Hannah Newall, MBBS, Coffs Harbour Health Campus, Pacific Hwy, Coffs Harbour, 2450 Australia ([email protected]).
Patients with chronic psychotic illness have higher rates of cardiovascular disease and premature death than the general community. The standardized mortality ratio in those with psychotic illness compared to the general population has increased over time, and this rise is primarily due to increasing rates of cardiovascular disease.1 This increase in cardiovascular disease might be partly due to metabolic side effects of the weight gain associated with atypical antipsychotic medication.1 However, tobacco use is the greatest predictor of cardiovascular risk in psychiatric populations.2 The financial burden of tobacco dependence also contributes to the poverty and social disadvantage experienced by many patients.3
The association between schizophrenia and tobacco use is well established. A systematic review4 of 42 studies from 20 nations showed that a much higher proportion of patients with schizophrenia use tobacco than the general population (OR = 5.9), they are more likely to have a history of lifetime tobacco use (8 studies, OR = 3.1), and they have lower cessation rates than patients with other disorders and than members of the general community (6 studies, OR = 0.19). However, this review did not employ meta-analytic methods and did not specifically examine the temporal associations between tobacco use and the onset of psychosis. In addition, many of the analyzed studies examined the tobacco use histories of patients with established psychotic illness,5-9 whose account of earlier tobacco use might be confounded by recall bias. A meta-analysis of the interval between the initiation of tobacco use and the onset of psychosis, the prevalence of tobacco users at the time of presentation for treatment, and the course of tobacco use after initial treatment would more clearly define the epidemiology of tobacco use in early psychosis. Examining these temporal associations would inform theories as to why tobacco use is initiated at high rates in such populations, which could lead to interventions to reduce tobacco use in first-episode psychosis patients.
This meta-analysis has 4 aims, which are to determine (1) the length of time between initiation of daily tobacco use and onset of psychosis (meta-analysis of initiation of tobacco use), (2) the proportion of patients with first-episode psychosis who smoke tobacco at the time of initial treatment for psychosis (meta-analysis of the prevalence of tobacco use), (3) the odds of tobacco use in first-episode psychosis when compared with appropriately matched controls (meta-analysis of odds of tobacco use), and (4) the longitudinal rates of tobacco use in cohorts of patients with first-episode psychosis (meta-analysis of the course of tobacco use).
DATA SOURCES
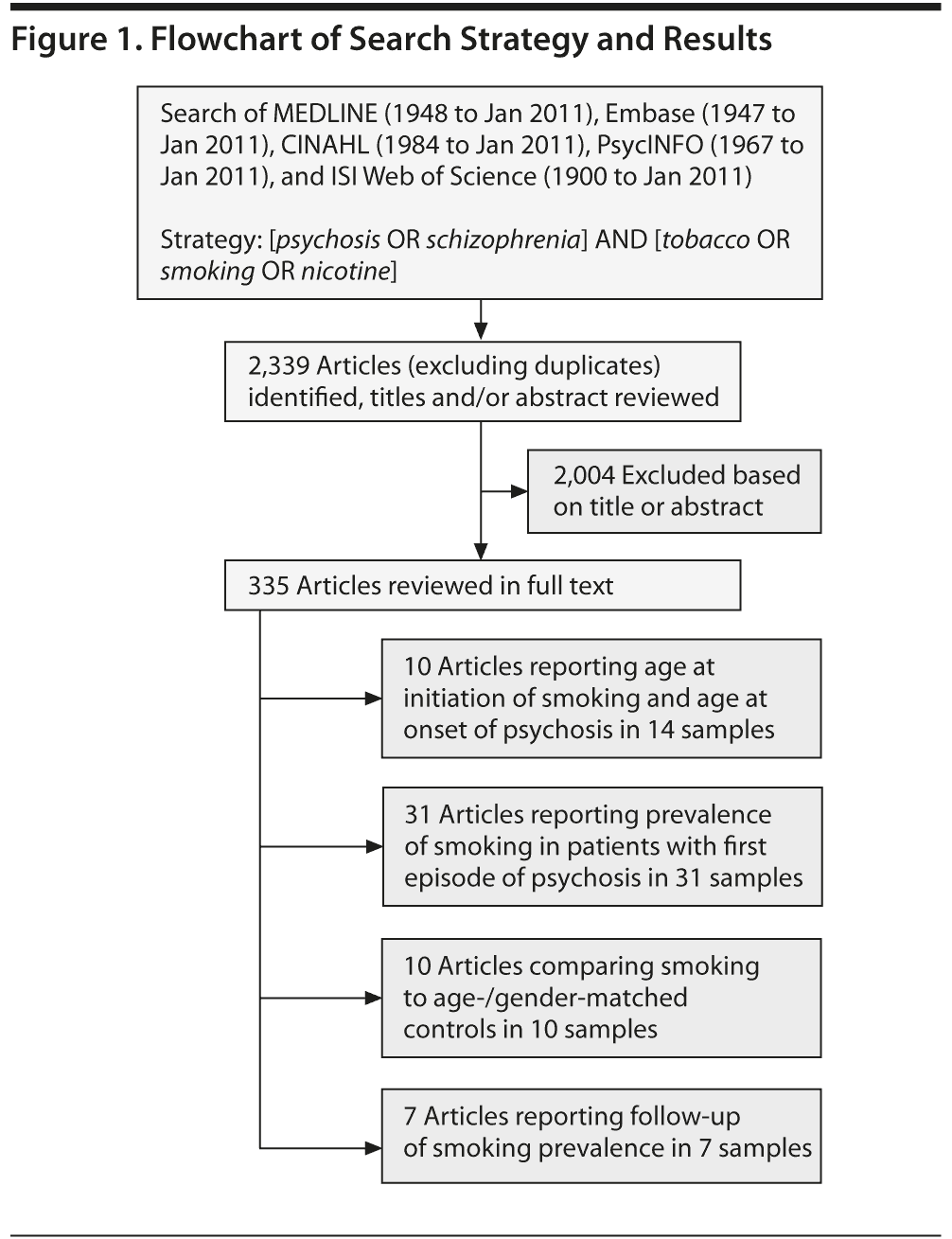
The systematic search of English-language publications indexed in 5 electronic databases (CINAHL, Embase, PsycINFO, MEDLINE, and ISI Web of Science) is shown in Figure 1. A broad search strategy was employed because tobacco use data were not mentioned in either the title or abstract of many articles, and hence all articles that appeared to report on tobacco, cannabis, or substance use by cohorts of patients with first-episode psychosis were examined in full text by N.M. and H.D.N. The reference lists of relevant articles were hand searched to locate articles not detected by electronic searches. Authors of articles describing studies that might have recorded, but not published, data on tobacco use were contacted with a request for unpublished data.
- Tobacco smoking is a risk factor for developing cardiovascular disease in patients with psychotic illness.
- The prevalence of tobacco use before, at, and after the first episode of psychosis is around 60% and remains constant after the illness is established.
- The initiation of tobacco use precedes the onset of psychosis by a mean of 5.3 years.
- Ultrahigh-risk and first-episode psychosis patients are an ideal target for smoking cessation programs, which should be routinely offered in first-episode psychosis services.
STUDY SELECTION
The articles yielded for each of the individual meta-analyses are outlined in Figure 1, and details of the articles included in each meta-analysis are outlined in Supplementary eTable 1 (available at PSYCHIATRIST.COM). Studies were included in the 3 meta-analyses if they reported the mean and standard deviation of age at onset of psychosis and age at initiation of daily tobacco use in patients with psychosis. Studies of chronic patients, in which tobacco use was assessed after first episode of psychosis, were included in the meta-analysis of initiation of tobacco use because the estimated date of initiating daily tobacco use is retrospective regardless of whether the measure is made at diagnosis of psychosis or at some time thereafter.
Studies were included in any of the meta-analyses if they reported (1) cohorts of patients with first-episode psychosis, including first-episode schizophrenia, schizoaffective disorder, other schizophrenia-spectrum disorder, or affective psychosis; and (2) the proportion of patients with first-episode psychosis using tobacco at the time of presentation to services.
Studies were excluded if they reported on patients with drug-induced or organic psychoses and if they reported on patients who had already been described in other studies.
Definition of Tobacco Use
Daily tobacco use was the threshold definition in each study, although there was some variation in how this was quantified. In all of the studies, the level of tobacco use was considered to be clinically significant, usually because the patient used tobacco regularly when it was available. We were unable to examine between-study heterogeneity of heavy or more continuous tobacco use and less heavy, intermittent, or discontinued tobacco use because few studies stratified patients according to their tobacco intake. The random effects model used in the meta-analyses only requires that thresholds are consistently applied within studies and allows for differences in the studied populations such as the threshold for inclusion in the tobacco using group.
DATA EXTRACTION
The methods were based on guidelines for Meta-Analysis of Observational Studies in Epidemiology (MOOSE).10 The data were extracted independently by N.M. and H.D.N. There were 5 disagreements regarding effect size data in the meta-analysis of the prevalence of tobacco use, 2 in the meta-analysis of odds ratios, and none in the meta-analyses of course and initiation of tobacco use. Disagreements were resolved by a joint examination of the articles. The following data were extracted: the mean age and standard deviation at initiation of daily tobacco use and age at onset of psychosis and the sample size of the group (meta-analysis of initiation of tobacco use); the proportion of patients with first-episode psychosis who used tobacco and the sample size of the group (meta-analysis of the prevalence of tobacco use); the proportion of the general population, or of age- and gender-matched controls, who used tobacco and the sample sizes of the groups (meta-analysis of odds of tobacco use); and the proportion of patients with psychosis who used tobacco at various intervals after initiation of antipsychotic treatment and the sample size of the group at follow-up (meta-analysis of course of tobacco use).
The following methodological characteristics and quality measures were recorded: the proportion of patients with affective psychosis in each sample, the proportion of male subjects in each sample, the year in which the sample was collected, the mean age of each sample, the geographic region in which the study was undertaken, information on whether subjects were recruited consecutively, use of objective diagnostic measures of psychosis, and use of objective measures to assess tobacco use status.
Meta-Analysis
Meta-analytically estimated standardized mean difference, logit event rates, and odds ratios were computed using Comprehensive Meta-Analysis Version 2 (Biostat, Eaglewood, New Jersey). Between-study heterogeneity was assessed using the I2 statistic, and between-group heterogeneity was assessed using Q value statistics. A random-effects meta-analysis was chosen on an a priori basis for all analyses because of the differences between studies in patient groups and methods.
Between-study heterogeneity might be associated with socioeconomic status of the sample, because tobacco use is associated with lower socioeconomic status in high-income countries,11 and by other methodological or study quality considerations. Hence, we assessed whether between-study heterogeneity in effect size was associated with (1) the proportion of patients in each study who were male, because men in most countries are generally more likely to use tobacco than women; (2) the geographical region of the study, because the prevalence of tobacco use and the onset of tobacco use varies between regions; (3) the year the study was published, because prevalence of tobacco use has declined in most advanced countries; (4) the proportion of patients with affective psychosis, to examine whether tobacco use might have been commenced in response to unrelated affective symptoms; (5) examination of consecutive presentations (quality measure); (6) use of a systematic measure of tobacco use (quality measure); or (7) use of systematic methods to diagnose psychosis (quality measure).
Publication Bias
Two methods were used to investigate publication bias. First, a funnel (Egger’s ) plot of the effect size versus the variance12 was inspected for the presence of smaller samples that might have been published because they reported high prevalence of tobacco use. Second, Duval and Tweedie’s “trim and fill” method was used to examine the possible effect of hypothetically missing samples on the pooled estimate of the standardized mean difference, logit event rate, or odds ratio.13
RESULTS
Meta-Analysis of Initiation of Tobacco Use
Fourteen data samples with a combined sample size of 1,618 subjects (per sample, mean [SD] = 115.6 [167.7]) were included in the meta-analysis of initiation. One sample14 was excluded because it examined a pediatric population.
Meta-Analysis of the Prevalence of Tobacco Use
Thirty-one data samples with a combined sample size of 4,082 subjects (per sample, mean [SD] = 132 [125]) were included in the meta-analysis of prevalence. This dataset incorporated 1 sample from an unpublished source (M. T. Compton, MD, 2011) and 3 samples15-17 that were included after the primary researchers provided additional data suitable for meta-analysis (M. Di Forti, MD, 2009; G. Berger, MD, 2008; and B. Kirkpatrick, MD, 2009). Four samples were excluded because the authors were unable to provide additional information needed for meta-analysis. Six articles18-23 were excluded because they reported on samples described in other articles.
Meta-Analysis of Odds of Tobacco Use
Ten data samples were included in the meta-analysis of odds ratios. The dataset reported a combined sample size of 745 patients (per sample, mean [SD] = 75 [81]) with first-episode psychosis and 544 controls (per sample, mean [SD] = 54 [46]). These samples were derived from a subset of the articles (Supplementary eTable 1) and included 1 sample16 after researchers provided additional data and 1 study22 that could not be included in the meta-analysis of prevalence. Two other samples were excluded because the authors were unable to provide additional information needed for meta-analysis.
Meta-Analysis of Course of Tobacco Use
Seven articles reported the proportion of tobacco users in groups of patients with first-episode psychosis and at periods of follow-up between 6 and 120 months (mean [SD] follow-up = 29 [41]) after first admission for treatment was included in the meta-analysis of course. The combined sample size was 1,653 subjects (per sample, mean [SD] = 118 [111]). The inclusion criteria required that samples provided the proportion of tobacco users in a cohort at hospital admission for first episode of psychosis and then at another time point from which an odds ratio at the end time point was determined. Two published studies were excluded because the authors were unable to provide additional information needed for meta-analysis.
Meta-Analytic Results
Meta-analysis of tobacco initiation. Meta-analysis indicated that regular tobacco use begins a mean of 5.3 years before onset of psychosis (standardized mean difference = 0.85; 95% CI, −0.97 to −0.72) (Supplementary eFigure 1). Between-study heterogeneity was low (Q13 = 24.8, P = .025, I2 = 47.5).
There was little evidence of publication bias. There were too few studies for a meaningful examination of a funnel plot; the trim and fill analysis did not identify samples that were to the left or right of the pooled mean.
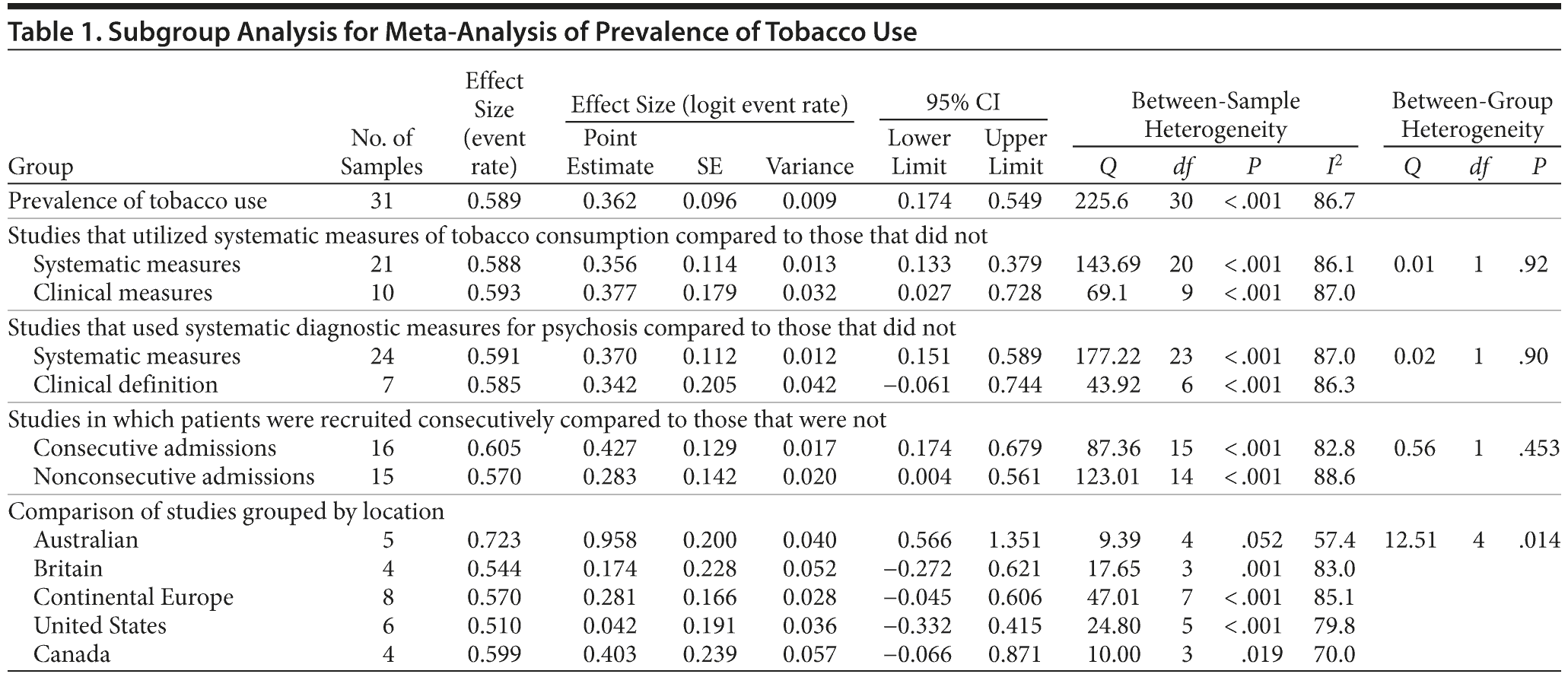
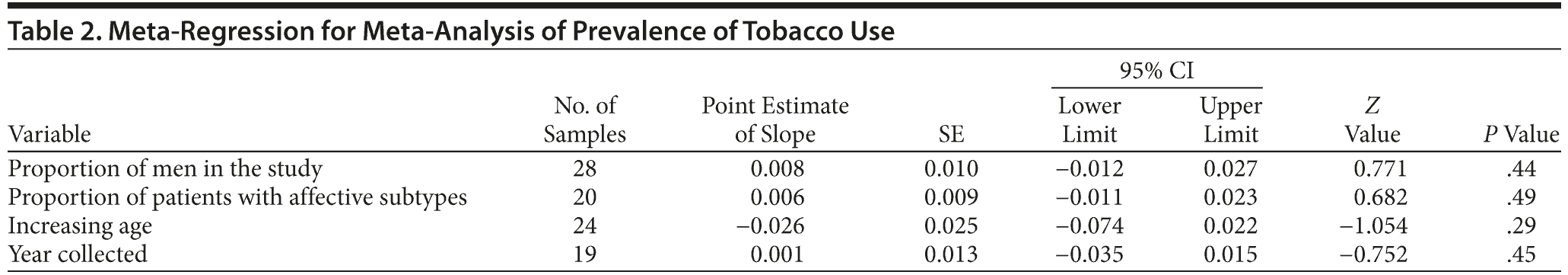
Meta-analysis of the prevalence of tobacco users. We found that 58.9% (95% CI, 54.3%-63.4%) of patients with psychosis smoked tobacco at the time they first presented for treatment (Supplementary eFigure 2). There was a high degree of between-sample heterogeneity (I2 = 86.7%) (Table 1), which was not explained by the proportion of patients with affective psychosis, the proportion of male subjects in a study, or the year of data collection on meta-regression (Table 2). However, there were differences in the prevalence of tobacco users according to geographic region, with the highest prevalence of tobacco use recorded in Australia (z = 4.75, P < .01), followed by Canada (z = 1.68, P = .09), Europe (z = 1.68, P = .09), Britain (z = 0.76, P = .45), and the United States (z = 0.22, P = .83).
The measures of study quality we examined did not make a significant contribution to between-group heterogeneity (see Table 1). This was the case for samples using systematic measures of tobacco use (z = 3.12, P < .01) compared with those that did not (z = 2.11, P = .04), samples using systematic measures to diagnose psychosis (z = 3.31, P < .01) compared with those that did not (z = 1.66, P = .10), and samples recruiting patients consecutively (z = 3.31, P < .01) compared with those that used other methods of sampling (z = 1.99, P = .05).
The funnel plot indicated slight asymmetry as a result of small samples, with an effect size greater than the mean of larger samples; and trim and fill analysis identified 4 samples that might have biased the results toward a higher rate of tobacco use. The exclusion of these studies reduced the point estimate from 58.9% to 56.4%, with wider confidence intervals (95% CI, 51.7%-60.9%). This suggests that bias toward publication of smaller studies showing a higher prevalence of tobacco use had a small impact on the pooled estimate.
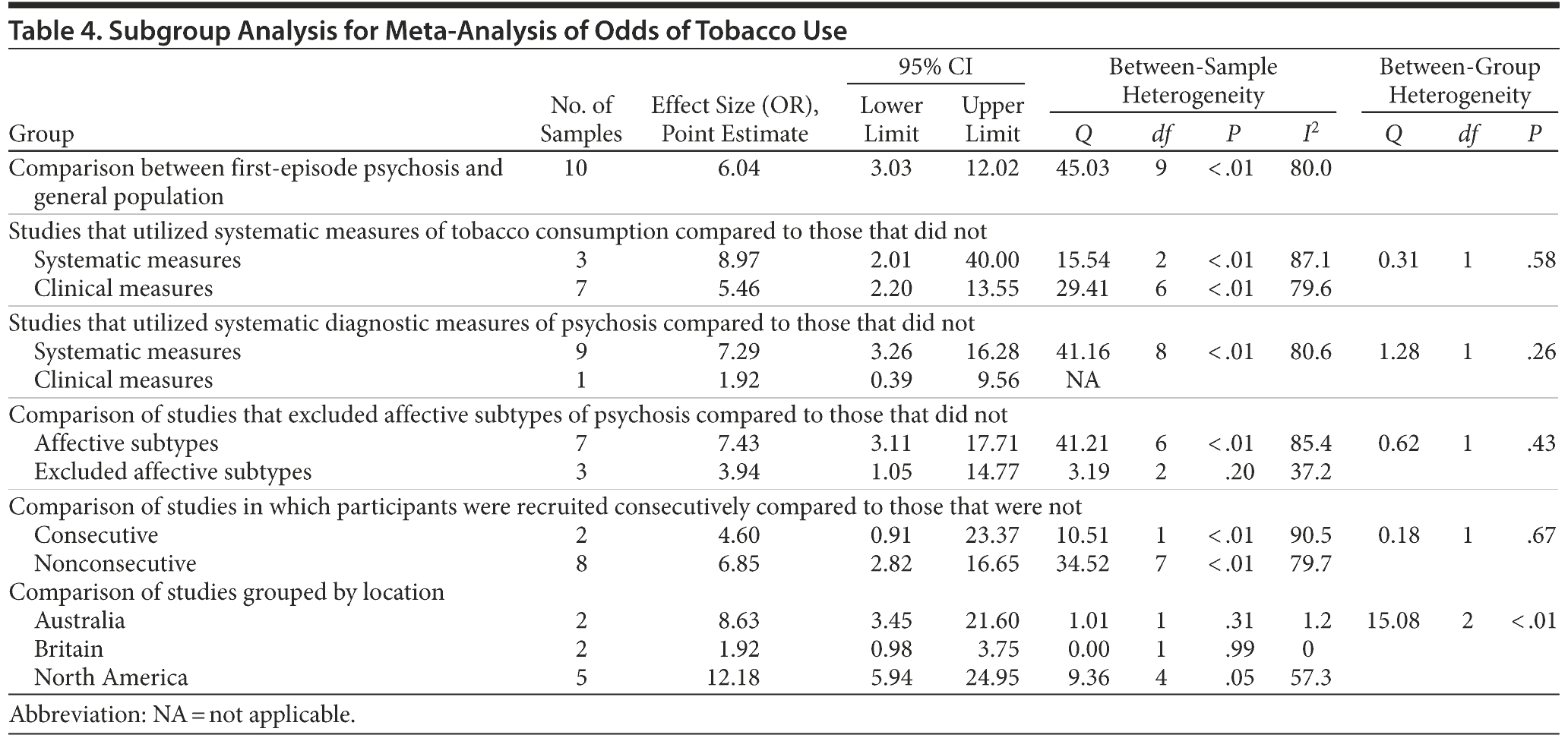
Meta-analysis of odds of tobacco use. The pooled estimate for the odds of patients presenting with tobacco use in first-episode psychosis was 6.04 (95% CI, 3.03-12.02) compared with age- and gender-matched controls (Supplementary eFigure 3). Between-study heterogeneity for odd ratios was also high (I2 = 80.0). Meta-regression suggested that studies with a greater proportion of male subjects had no significant impact on odds of tobacco use (Table 3). Similarly, subgroup analysis of studies that excluded affective subtypes (z = 2.03, P < .04) compared with those that included affective subtypes (z = 4.52, P < .01) did not explain between-study heterogeneity. There was evidence that geographic region contributed to between-study heterogeneity (Table 4), with the North American studies (z = 6.83, P < .01) recording the highest odds, followed by the Australian studies (z = 4.60, P < .01), and the studies from Britain recorded the lowest prevalence (z = 1.90, P < .06). There were not enough samples to examine between-study heterogeneity associated with studies conducted in Asia or the Middle East.
An examination of quality measures did not explain the heterogeneity in odds ratios (see Table 4). This was true for studies using systematic measures of tobacco use (z = 2.88, P < .01) compared with those that did not (z = 3.66, P < .01), studies using systematic diagnostic measures of psychosis (z = 4.84, P < .01) compared with those that did not (z = 0.59, P = .55), and studies recruiting patients consecutively (z = 1.84, P = .07) compared with those that did not (z = 4.24, P < .01).
There was little evidence of publication bias. There were too few studies for a meaningful examination of a funnel plot, and the trim and fill analysis did not identify any samples either to the left or right of the pooled mean.
Meta-analysis of course of tobacco use. At follow-up between 6 months and 120 months, we found the odds ratio of initiating tobacco use was 0.996 (95% CI, 0.907-1.094) (Supplementary eFigure 4). Moreover, there was no between-study heterogeneity (I2 = 0).
There were too few studies for meaningful examination of the funnel plot. The trim and fill method identified and removed 1 study, suggesting an adjusted mean of 0.992 (95% CI, 0.905-1.089).
DISCUSSION
The aim of this meta-analysis was to explore the complex relationship between tobacco use and the early phase of psychotic illness. Defining when tobacco use begins in relation to the onset of psychosis, and the course of tobacco use after the development of psychotic illness, may help to explain why tobacco use is so prevalent in this population and to improve our understanding of the illness itself. Moreover, the availability of an accurate estimate of the prevalence of tobacco use at first-episode psychosis may prevent inaccurate reporting of the prevalence of tobacco use in both the lay and scientific literature.
The pooled estimate, from available data, for the proportion of patients with tobacco use at the time of presenting for treatment of first-episode psychosis is 59%, and the odds of tobacco use among patients with first-episode psychosis compared to age- and gender-matched controls is about 6. Regular tobacco use precedes onset of psychosis by about 5 years, and the proportion of tobacco users changes little over time. The high prevalence and persistence of tobacco use in patients with psychosis confirmed by this study suggest that more attention needs to be paid to the reasons for commencing tobacco use prior to diagnosis as well as to exploring new ways of assisting patients to stop smoking tobacco.
The reasons for the association between tobacco use and psychotic illness could include the existence of a shared diathesis between addiction and mental illness because tobacco helps patients cope with prodromal or subclinical symptoms such as inattention and depression, because it alleviates symptoms of psychosis, or because nicotine reduces medication side effects.4 The prevalence of tobacco use among people with schizophrenia might also be elevated because of lower rates of cessation. Our finding that tobacco use begins, on average, 5 years before onset of psychosis suggests that tobacco use is not initiated as a way of controlling the positive symptoms that emerge at the onset of psychosis because this interval is much longer than estimates of the typical duration of untreated psychosis24 and most patients have taken up tobacco use long before they experience positive symptoms. Moreover, the high prevalence of tobacco use prior to treatment with antipsychotic medication and the stability of tobacco use after treatment suggest that patients do not start using tobacco in order to mitigate the side effects of psychotropic medication, although some patients may fail to stop using tobacco for this reason.
The high prevalence of tobacco use among patients, the long interval between the commencement of tobacco use and the emergence of psychosis, and the stability of tobacco use in patients who develop psychosis suggest the presence of a common underlying susceptibility to psychosis and tobacco addiction. It is possible that the subjective experiences of people prone to develop psychosis are alleviated by tobacco use. For example, tobacco use has been shown to result in improvement in subjective experiences25,26 and objective measures empirically reported by some patients.27,28 Nicotine might be used to mitigate negative symptoms associated with emerging as well as chronic psychosis19,29-31; however, it is unlikely that frank positive symptoms encourage tobacco use because there is no increase in use following diagnosis.
At least 1 study, which was carefully controlled for shared socioeconomic risk factors, suggested that tobacco use constitutes a risk factor for future psychotic illness.32 There may also be a common neurobiological basis for both tobacco addiction and psychosis, such as the P50 gating deficit found in most patients with schizophrenia and in up to 50% of their first-degree relatives,33 that has been proposed as a possible example of molecular causation for schizophrenia.34 This deficit, linked to the 15q14 locus of the α7 nicotinic receptor,35 is thought to be related to impaired attention and might represent a biological mediator of negative symptoms and cognitive deficits. Our results should encourage research into a common neurobiological basis for both psychotic illness and tobacco addiction.36,37 However, concurrent cannabis use among tobacco smokers is a confounding factor that should be examined in future research.38
These findings confirm the need for mental health services to do more to address tobacco use by patients with psychosis. There has been a nihilistic attitude toward tobacco cessation, perhaps because many psychiatrists are unwilling to broach the subject of tobacco cessation with patients because of their lack of confidence that intervention is effective.39 There is some doubt about the usefulness of psychosocial intervention alone in combating tobacco addiction in the severely mentally ill,40 and low rates of cessation suggest that a combined clinical and pharmacologic approach might be needed. If there is a neurobiological basis for tobacco dependence in many patients, adequate nicotine replacement therapy would appear to be an ethical requirement of mental health facilities that prohibit tobacco use. Of note, we found no evidence for a decline in tobacco use among patients with psychosis according to the year at which data were collected, despite the decline in tobacco use in the nonpsychiatric population observed throughout the developed world.41 This might indicate that people susceptible to developing psychosis are less receptive to public health campaigns or to other measures to reduce tobacco use.42 There were also significant differences in the prevalence of tobacco use according to geographic region, with the highest rate of tobacco use by patients recorded in Australia, followed by Canada, Europe, Britain, and the United States (see Table 1). The proportion of tobacco use among patients does not correspond to tobacco use in the wider community, and further examination of the social and biological factors for taking up tobacco use in specific populations could improve our understanding of the nature of the association and improve cessation programs.
The high prevalence of tobacco use represents a substantial disease burden on this population.43 There is increased recognition of the metabolic side effects of antipsychotic medications44 and the need for early intervention to reduce cardiovascular risk in first-episode psychosis.45 There is an interaction between cardiovascular risk factors, but tobacco use remains the greatest single risk factor for future cardiovascular morbidity, and modifying tobacco use among patients with psychosis could reduce 10-year cardiovascular mortality for these patients by as much as a quarter.46 Our finding that 59% of patients with first-episode psychosis already use tobacco regularly indicates that more effort is required to reduce tobacco use in first-episode patients. Moreover, the burgeoning clinical interest in the detection of those considered ultrahigh risk for developing psychosis provides a further opportunity for research into tobacco use and treatment innovation.
Reducing the time that patients use tobacco is likely to improve the success of tobacco cessation interventions. The development of specialist first-episode services in many countries means that first-episode psychosis patients may be more likely to have intensive specialist intervention and follow-up than patients with more established illness. Hence, antitobacco interventions could be more effective and should be an integral part of first-episode treatments. The evidence pointing toward an underlying neurobiological basis for the high prevalence of tobacco use might help to explain why people with psychotic illness attempt to stop using tobacco at the same rate as the general population but are less likely to consolidate these attempts.47 Research into the molecular biology of nicotine addiction, which is clinically appropriate to tobacco cessation programs, perhaps deserves a higher priority.
An important limitation of this study is that we were unable to examine the rates of tobacco use uptake and cessation within the individual studies. It might be that the rate of cessation was similar to the rate of initiation of tobacco use, leaving the proportion of tobacco users stable. Similarly, because the included samples typically provided the prevalence of tobacco use in study populations rather than examining between-group differences in smokers and nonsmokers, we were unable to examine the effect of a range of confounding variables on heterogeneity or effect size. In theory, we could have added to the relatively small number of studies reporting tobacco use in control groups by using public health data in some of the regions where the studies were conducted. However, we decided that the methodological and sampling differences between data for the general population and the population from which the samples were drawn were probably too great for valid statistical comparison.
CONCLUSIONS
This meta-analysis found that 59% of patients with first-episode psychosis use tobacco at the time of presenting for treatment. The odds of tobacco use in first-episode psychosis was 6 when compared to nonpsychiatric populations. We also found that the initiation of tobacco use precedes the onset of psychosis by 5 years, and once the illness is established, the prevalence of tobacco use varies little over time. These findings provide further support for the hypothesis that patients with psychosis have an underlying neurobiological susceptibility to using tobacco that is unrelated to positive symptoms of psychosis or the effect of treatment with antipsychotic medication. These findings have important implications for the prevention of cardiovascular disease in these populations and for the development of tobacco cessation programs for those with severe mental illnesses.
Disclosure of off-label usage: The authors have determined that, to the best of their knowledge, no investigational information about pharmaceutical agents that is outside US Food and Drug Administration-approved labeling has been presented in this article.
Author affiliations: Coffs Harbour Health Campus, Coffs Harbour (Drs Myles and Newall); School of Psychiatry, University of New South Wales (Drs Myles, Newall, Curtis, Nielssen, and Large); Department of Psychiatry, Prince of Wales Hospital (Drs Curtis and Large), Randwick; Department of Psychiatry, St Vincent’s Hospital, Darlinghurst (Dr Nielssen), Australia; general practitioner (retired), North Staffordshire, United Kingdom (Dr Shiers).
Financial disclosure: Dr Nielssen has received speaker fees from AstraZenecca. Dr Shiers serves on the board of Rethink Charity as an unpaid trustee; is a consultant to National Audit of Schizophrenia UK, a program led by the Royal College of Psychiatrists UK; is an unpaid consultant to National Institute for Health and Clinical Excellence (NICE) UK; has been employed by National Mental Health Development Unit UK; has served on speakers bureaus of Janssen and Norwegian Medical Association; and is currently a member of the Guideline Development Group for new NICE guidence for children and young people affected by psychosis and schizophrenia. Drs Myles, Newall, Curtis, and Large have no personal affiliations or financial relationships with any commercial interest to disclose relative to the article.
Funding/support: None reported.
Disclaimer: The views expressed in this article are not those of the Guideline Development Group, National Collaborating Centre for Mental Health, or NICE.
Acknowledgments: The authors would like to acknowledge the following authors and their associates for providing unpublished data from their studies: B. Kirkpatrick, MD; M. Di Forti, MD; M. T. Compton, MD; and G. Berger, MD. The authors also thank Peter Arnold, MBBS, a retired professional editor, for his assistance in the preparation of this article. Dr Arnold has no personal affiliations or financial relationships with any commercial interest to disclose relative to the article.
Supplementary material: Available at PSYCHIATRIST.COM.
REFERENCES
1. Saha S, Chant D, McGrath J. A systematic review of mortality in schizophrenia: is the differential mortality gap worsening over time? Arch Gen Psychiatry. 2007;64(10):1123-1131. PubMed doi:10.1001/archpsyc.64.10.1123
2. Brown S, Kim M, Mitchell C, et al. Twenty-five year mortality of a community cohort with schizophrenia. Br J Psychiatry. 2010;196(2):116-121. PubMed doi:10.1192/bjp.bp.109.067512
3. Steinberg ML, Williams JM, Ziedonis DM. Financial implications of cigarette smoking among individuals with schizophrenia. Tob Control. 2004;13(2):206. PubMed
4. de Leon J, Diaz FJ. A meta-analysis of worldwide studies demonstrates an association between schizophrenia and tobacco smoking behaviors. Schizophr Res. 2005;76(2-3):135-157. PubMed doi:10.1016/j.schres.2005.02.010
5. Kelly C, McCreadie RG. Smoking habits, current symptoms, and premorbid characteristics of schizophrenic patients in Nithsdale, Scotland. Am J Psychiatry. 1999;156(11):1751-1757. PubMed
6. Beratis S, Katrivanou A, Gourzis P. Factors affecting smoking in schizophrenia. Compr Psychiatry. 2001;42(5):393-402. PubMed doi:10.1053/comp.2001.26273
7. Liao DL, Yang JY, Lee SM, et al. Smoking in chronic schizophrenic inpatients in Taiwan. Neuropsychobiology. 2002;45(4):172-175. PubMed doi:10.1159/000063666
8. Uzun O, Cansever A, BasoÄŸlu C, et al. Smoking and substance abuse in outpatients with schizophrenia: a 2-year follow-up study in Turkey. Drug Alcohol Depend. 2003;70(2):187-192. PubMed doi:10.1016/S0376-8716(02)00362-9
9. Gurpegui M, Mart×nez-Ortega JM, Aguilar MC, et al. Smoking initiation and schizophrenia: a replication study in a Spanish sample. Schizophr Res. 2005;76(1):113-118. PubMed doi:10.1016/j.schres.2004.12.007
10. Stroup DF, Berlin JA, Morton SC, et al. Meta-analysis of observational studies in epidemiology: a proposal for reporting. Meta-analysis of Observational Studies in Epidemiology (MOOSE) group. JAMA. 2000;283(15):2008-2012. PubMed doi:10.1001/jama.283.15.2008
11. Schaap MM, Kunst AE. Monitoring of socio-economic inequalities in smoking: learning from the experiences of recent scientific studies. Public Health. 2009;123(2):103-109. PubMed doi:10.1016/j.puhe.2008.10.015
12. Cooper H, Hedges L. Handbook of Research Synthesis. New York, NY: Russell Sage Foundation; 1994.
13. Duval S, Tweedie R. Trim and fill: a simple funnel-plot-based method of testing and adjusting for publication bias in meta-analysis. Biometrics. 2000;56(2):455-463. PubMed doi:10.1111/j.0006-341X.2000.00455.x
14. Ilomפki R, Riala K, Hakko H, et al; Study 70 Workgroup. Temporal association of onset of daily smoking with adolescent substance use and psychiatric morbidity. Eur Psychiatry. 2008;23(2):85-91. PubMed doi:10.1016/j.eurpsy.2007.10.009
15. Fernandez-Egea E, Bernardo M, Heaphy CM, et al. Telomere length and pulse pressure in newly diagnosed, antipsychotic-naive patients with nonaffective psychosis. Schizophr Bull. 2009;35(2):437-442. PubMed doi:10.1093/schbul/sbn169
16. Di Forti M, Morgan C, Dazzan P, et al. High-potency cannabis and the risk of psychosis. Br J Psychiatry. 2009;195(6):488-491. PubMed doi:10.1192/bjp.bp.109.064220
17. Berger GE, Proffitt T-M, McConchie M, et al. Dosing quetiapine in drug-naive first-episode psychosis: a controlled, double-blind, randomized, single-center study investigating efficacy, tolerability, and safety of 200 mg/day vs 400 mg/day of quetiapine fumarate in 141 patients aged 15 to 25 years. J Clin Psychiatry. 2008;69(11):1702-1714. PubMed doi:10.4088/JCP.v69n1105
18. Barnes TRE, Mutsatsa SH, Hutton SB, et al. Comorbid substance use and age at onset of schizophrenia. Br J Psychiatry. 2006;188(3):237-242. PubMed doi:10.1192/bjp.bp.104.007237
19. Rabinowitz J, Bromet EJ, Lavelle J, et al. Prevalence and severity of substance use disorders and onset of psychosis in first-admission psychotic patients. Psychol Med. 1998;28(6):1411-1419. PubMed doi:10.1017/S0033291798007399
20. Ramsay CE, Abedi GR, Marson JD, et al. Overview and initial validation of two detailed, multidimensional, retrospective measures of substance use: the Lifetime Substance Use Recall (LSUR) and Longitudinal Substance Use Recall for 12 Weeks (LSUR-12) Instruments. J Psychiatr Res. 2011;45(1):83-91. PubMed doi:10.1016/j.jpsychires.2010.04.018
21. Stewart T, Goulding SM, Pringle M, et al. A descriptive study of nicotine, alcohol, and cannabis use in urban, socially disadvantaged, predominantly African-American patients with first-episode nonaffective psychosis. Clin Schizophr Related Psychoses. 2010;3(4):217-225. doi:10.3371/CSRP.3.4.4
22. Luty J, Kelly C, McCreadie RG. Smoking habits, body mass index and risk of heart disease: prospective 2 1/2-year follow-up of first episode schizophrenic patients. J Subst Use. 2002;7(1):15-18. doi:10.1080/14659890110110374
23. Wade D, Harrigan S, Edwards J, et al. Course of substance misuse and daily tobacco use in first-episode psychosis. Schizophr Res. 2006;81(2-3):145-150. PubMed doi:10.1016/j.schres.2005.09.010
24. Large M, Nielssen O, Slade T, et al. Measurement and reporting of the duration of untreated psychosis. Early Interv Psychiatry. 2008;2(4):201-211. PubMed doi:10.1111/j.1751-7893.2008.00080.x
25. Hughes JR, Hatsukami DK, Mitchell JE, et al. Prevalence of smoking among psychiatric outpatients. Am J Psychiatry. 1986;143(8):993-997. PubMed
26. Forchuk C, Norman R, Malla A, et al. Schizophrenia and the motivation for smoking. Perspect Psychiatr Care. 2002;38(2):41-49. PubMed doi:10.1111/j.1744-6163.2002.tb00656.x
27. Adler LE, Hoffer LD, Wiser A, et al. Normalization of auditory physiology by cigarette smoking in schizophrenic patients. Am J Psychiatry. 1993;150(12):1856-1861. PubMed
28. Olincy A, Ross RG, Young DA, et al. Improvement in smooth pursuit eye movements after cigarette smoking in schizophrenic patients. Neuropsychopharmacology. 1998;18(3):175-185. PubMed doi:10.1016/S0893-133X(97)00095-X
29. Berman I, Viegner B, Merson A, et al. Differential relationships between positive and negative symptoms and neuropsychological deficits in schizophrenia. Schizophr Res. 1997;25(1):1-10. PubMed doi:10.1016/S0920-9964(96)00098-9
30. Bilder RM, Goldman RS, Volavka J, et al. Neurocognitive effects of clozapine, olanzapine, risperidone, and haloperidol in patients with chronic schizophrenia or schizoaffective disorder. Am J Psychiatry. 2002;159(6):1018-1028. PubMed doi:10.1176/appi.ajp.159.6.1018
31. Gur RE, Calkins ME, Gur RC, et al. The Consortium on the Genetics of Schizophrenia: neurocognitive endophenotypes. Schizophr Bull. 2007;33(1):49-68. PubMed doi:10.1093/schbul/sbl055
32. Weiser M, Reichenberg A, Grotto I, et al. Higher rates of cigarette smoking in male adolescents before the onset of schizophrenia: a historical-prospective cohort study. Am J Psychiatry. 2004;161(7):1219-1223. PubMed doi:10.1176/appi.ajp.161.7.1219
33. Adler LE, Hoffer LJ, Griffith J, et al. Normalization by nicotine of deficient auditory sensory gating in the relatives of schizophrenics. Biol Psychiatry. 1992;32(7):607-616. PubMed doi:10.1016/0006-3223(92)90073-9
34. Adler LE, Olincy A, Waldo M, et al. Schizophrenia, sensory gating, and nicotinic receptors. Schizophr Bull. 1998;24(2):189-202. PubMed
35. Freedman R, Coon H, Myles-Worsley M, et al. Linkage of a neurophysiological deficit in schizophrenia to a chromosome 15 locus. Proc Natl Acad Sci U S A. 1997;94(2):587-592. PubMed doi:10.1073/pnas.94.2.587
36. Wiles NJ, Zammit S, Bebbington P, et al. Self-reported psychotic symptoms in the general population: results from the longitudinal study of the British National Psychiatric Morbidity Survey. Br J Psychiatry. 2006;188(6):519-526. PubMed doi:10.1192/bjp.bp.105.012179
37. Esterberg ML, Jones EM, Compton MT, et al. Nicotine consumption and schizotypy in first-degree relatives of individuals with schizophrenia and non-psychiatric controls. Schizophr Res. 2007;97(1-3):6-13. PubMed doi:10.1016/j.schres.2007.08.024
38. O’ Cathail SM, O’ Connell OJ, Long N, et al. Association of cigarette smoking with drug use and risk taking behaviour in Irish teenagers. Addict Behav. 2011;36(5):547-550. PubMed doi:10.1016/j.addbeh.2011.01.012
39. Price JH, Ambrosetti LM, Sidani JE, et al. Psychiatrists’ smoking cessation activities with Ohio community mental health center patients. Community Ment Health J. 2007;43(3):251-266. PubMed doi:10.1007/s10597-006-9074-3
40. Tsoi DT, Porwal M, Webster AC. Interventions for smoking cessation and reduction in individuals with schizophrenia. Cochrane Database Syst Rev. 2010;(6):CD007253. PubMed
41. Giskes K, Kunst AE, Benach J, et al. Trends in smoking behaviour between 1985 and 2000 in nine European countries by education. J Epidemiol Community Health. 2005;59(5):395-401. PubMed doi:10.1136/jech.2004.025684
42. West S, Shipman S. Fast Facts: Smoking Cessation. London, UK: Health Press Ltd; 2007.
43. Wildgust HJ, Beary M. Are there modifiable risk factors which will reduce the excess mortality in schizophrenia? J Psychopharmacol. 2010;24(suppl):37-50. PubMed doi:10.1177/1359786810384639
44. Rummel-Kluge C, Komossa K, Schwarz S, et al. Head-to-head comparisons of metabolic side effects of second generation antipsychotics in the treatment of schizophrenia: a systematic review and meta-analysis. Schizophr Res. 2010;123(2-3):225-233. PubMed doi:10.1016/j.schres.2010.07.012
45. Hetrick S, Alvarez-Jiménez M, Parker A, et al. Promoting physical health in youth mental health services: ensuring routine monitoring of weight and metabolic indices in a first episode psychosis clinic. Australas Psychiatry. 2010;18(5):451-455. PubMed doi:10.3109/10398561003731189
46. Bobes J, Arango C, Garcia-Garcia M, et al. Healthy lifestyle habits and 10-year cardiovascular risk in schizophrenia spectrum disorders: an analysis of the impact of smoking tobacco in the CLAMORS schizophrenia cohort. Schizophr Res. 2010;119(1-3):101-109. PubMed doi:10.1016/j.schres.2010.02.1030
47. McClave AK, McKnight-Eily LR, Davis SP, et al. Smoking characteristics of adults with selected lifetime mental illnesses: results from the 2007 National Health Interview Survey. Am J Public Health. 2010;100(12):2464-2472. PubMed doi:10.2105/AJPH.2009.188136