Psychosis is one of the most serious among the adverse effects associated with cannabis use. The association between cannabis use and psychosis has been variously explored in a series of recent meta-analyses. The results of these meta-analyses show that persons who develop psychosis experience onset of psychosis about 2-3 years earlier if they are cannabis users; this effect is not observed with alcohol or other substance use. Higher levels of cannabis use are associated with greater risk of psychosis. Current cannabis abuse or dependence (but not past use or lower levels of current use) increases the risk of transition into psychosis in persons at ultrahigh risk of psychosis. About a third of patients with first-episode psychosis are cannabis users, and, at follow-up, about half of these users are found to continue their cannabis use. Continued cannabis use (in those who are treated after developing psychosis) is associated with higher risk of relapse into psychosis, and discontinuation of cannabis use reduces the risk of relapse to that in cannabis nonusers. Finally, persons with psychosis who continue to use cannabis have more severe positive symptoms and poorer levels of functioning. Because experimental studies in humans show that cannabinoids and cannabis can induce psychotic symptoms, it is reasonable to assume that the epidemiologic data indicate a causal effect of cannabis in anticipating, triggering, or exacerbating psychosis in vulnerable individuals and in worsening the course and outcome of the illness in those who continue to use the substance. Given the public health implications of these findings, the trend to legalize medical marijuana must be viewed with concern, and efforts are necessary to educate patients and the public about the serious mental and physical health risks associated with cannabis use and abuse.
- Persons who develop psychosis experience earlier onset of illness (by 2-3 years) if they are cannabis users.
- Higher levels of cannabis use are associated with a higher risk of development of psychosis.
- Current cannabis abuse or dependence is associated with an increased risk of transition into psychosis in persons at ultrahigh risk of psychosis. Studies in first-episode psychosis suggest that about a third of patients are cannabis users.
- Cannabis use continues in a significant proportion of patients even after the onset of psychosis. Discontinuation of cannabis use after onset of psychosis brings down the risk of relapse (after antipsychotic treatment) to the level of that in cannabis nonusers.

ABSTRACT
Psychosis is one of the most serious among the adverse effects associated with cannabis use. The association between cannabis use and psychosis has been variously explored in a series of recent meta-analyses. The results of these meta-analyses show that persons who develop psychosis experience onset of psychosis about 2-3 years earlier if they are cannabis users; this effect is not observed with alcohol or other substance use. Higher levels of cannabis use are associated with greater risk of psychosis. Current cannabis abuse or dependence (but not past use or lower levels of current use) increases the risk of transition into psychosis in persons at ultrahigh risk of psychosis. About a third of patients with first-episode psychosis are cannabis users, and, at follow-up, about half of these users are found to continue their cannabis use. Continued cannabis use (in those who are treated after developing psychosis) is associated with higher risk of relapse into psychosis, and discontinuation of cannabis use reduces the risk of relapse to that in cannabis nonusers. Finally, persons with psychosis who continue to use cannabis have more severe positive symptoms and poorer levels of functioning. Because experimental studies in humans show that cannabinoids and cannabis can induce psychotic symptoms, it is reasonable to assume that the epidemiologic data indicate a causal effect of cannabis in anticipating, triggering, or exacerbating psychosis in vulnerable individuals and in worsening the course and outcome of the illness in those who continue to use the substance. Given the public health implications of these findings, the trend to legalize medical marijuana must be viewed with concern, and efforts are necessary to educate patients and the public about the serious mental and physical health risks associated with cannabis use and abuse.
J Clin Psychiatry 2016;77(6):e739-e742
dx.doi.org/10.4088/JCP.16f10918
© Copyright 2016 Physicians Postgraduate Press, Inc.
Introduction
A previous article in this column1 examined the benefits and risks of cannabinoids and cannabis and summarized that, in randomized controlled trials, cannabinoids increase the risk of total adverse events, serious adverse events, and dropout due to adverse events. Cannabis acutely impairs psychomotor performance and increases the risk of fatal and nonfatal traffic accidents. Chronic cannabis use is associated with long-term impairments in cognitive performance, with respiratory disorders, and with the development of dependence. Other adverse outcomes are also reported.1 The present article focuses on one adverse outcome that had deliberately received only brief mention in the previous article, that is, the risk of psychosis, a state that has long been associated with cannabis use.2 Of note, interventional research on cannabis use in psychosis is out of the scope of this review, and the reader is referred to other resources.3,4
Cannabis Use Is Associated With an Earlier Onset of Psychosis
In a systematic review and meta-analysis, Large et al5 identified 83 studies with 131 samples that reported age at onset of psychotic illness in substance users (pooled N = 8,167) and nonusers (pooled N = 14,352). In all studies, the degree of substance use was considered clinically significant.
The findings of the meta-analysis are presented in Table 1. In summary, there was no statistical evidence that suggested publication bias. Using a random effects model, the authors5 found that onset of psychosis was 2.0 years earlier in broadly defined substance users and 2.7 years earlier in those who used cannabis, but not significantly earlier in those who used alcohol. Heterogeneity in the age-at-onset effect size principally arose from differences in the proportion of cannabis users between samples; when the proportion of cannabis users in a sample was larger, mean age at onset of psychosis was earlier. This meta-analysis could not examine the temporal relationship between onset of substance use and onset of psychosis. Nevertheless, the findings suggest that there is something specific about cannabis use that results in its association with an earlier onset of psychotic illness.
Helle et al6 also found that cannabis but no other substance use significantly predicted (earlier) age at onset of schizophrenia spectrum disorder. Other studies, published after the meta-analysis of Large et al,5 have also identified an earlier age at onset of psychosis in cannabis users.7-10 Some data suggest that an earlier age of initiation of cannabis use may predict earlier age at onset of psychosis.11,12
Cannabis Use Is Associated With a Dose-Dependent Increase in the Risk of Psychosis
Cannabis has long been associated with an increased risk of psychosis.2 Is the risk dose-dependent? Many cross-sectional and longitudinal (observational) studies have suggested so. Marconi et al13 therefore examined the subject in a systematic review and meta-analysis.
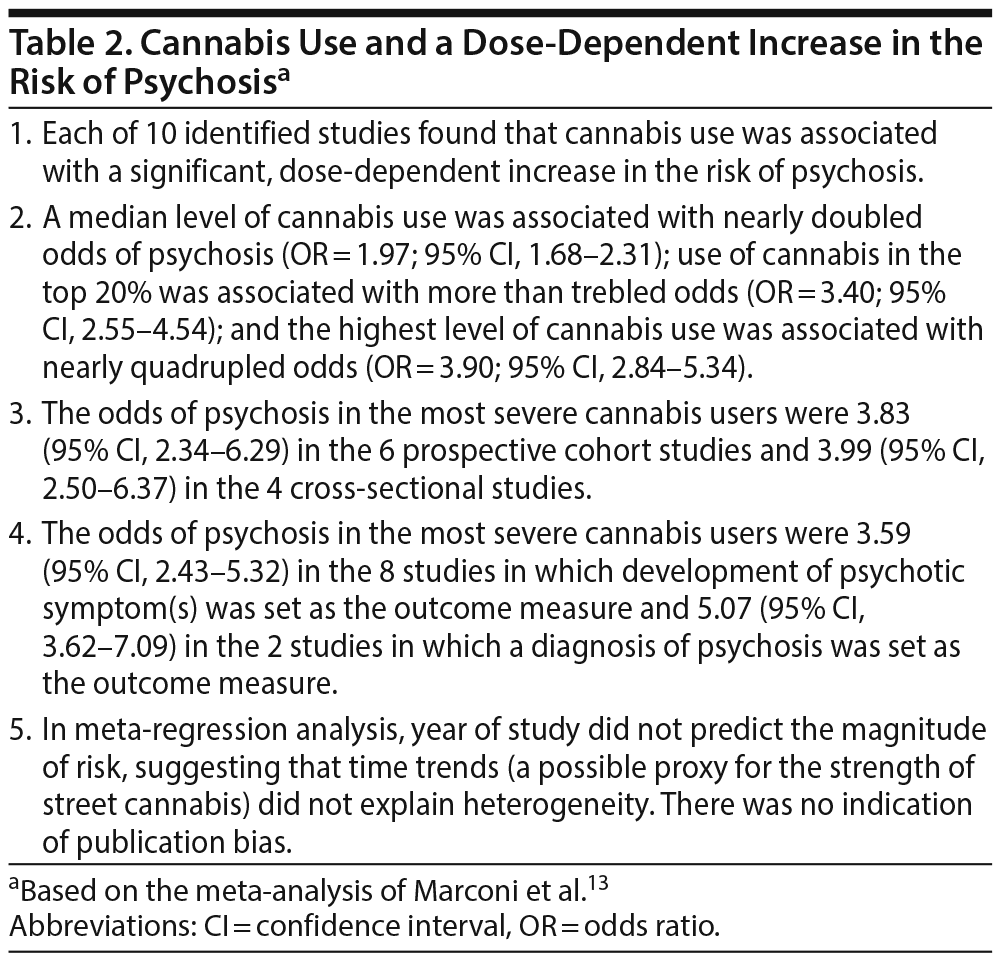
These authors13 identified 10 studies (pooled N = 66,816) that quantified cannabis intake before the onset of psychotic symptomatology that was defined using validated clinical measures. There were 6 prospective studies, 3 cross-sectional studies, and 1 case-control study conducted in 7 developed countries in 3 continents. Most of the studies quantified cannabis use in terms of lifetime frequency of use or use at baseline. Psychosis was mostly commonly defined in terms of development of specified symptoms or clinical diagnosis. The risk of psychosis was examined in random effects models (heterogeneity was high) with level of exposure to cannabis estimated as a continuous variable; cannabis never-users comprised the reference category.
Important findings from the study are presented in Table 2. In summary, cannabis use was associated with a dose-dependent increase in the risk of psychosis; the risk was doubled in the average user and quadrupled in the heaviest users. The finding was consistent, showing little variation across of type of study design (cross-sectional or longitudinal) and method of identification of psychosis (broad or narrow).
Cannabis Use Increases Transition to Psychosis in High-Risk Patients
What is the effect of cannabis use in persons at high risk of psychosis? This question was examined by Kraan et al14 in a systematic review and meta-analysis of prospective studies. These authors14 identified 7 relevant studies (pooled N = 1,171) with a follow-up duration of 1-4 years. Random effects meta-analysis was performed.
Important findings from the meta-analysis are presented in Table 3. In summary, current cannabis abuse or dependence, but not other levels of current use or past use, were associated with increased risk of transition into psychosis in subjects at ultrahigh risk of psychosis. Of note, this meta-analysis could not control for the influence of other risk factors for transition into psychosis.
Cannabis Use Is Highly Prevalent in First-Episode Psychosis
If cannabis use is an important variable in patients with psychosis, it would be useful to know how common it is in first-episode psychosis (FEP) and thereafter. This subject was examined by Myles et al15 in a systematic review and meta-analysis of observational studies. These authors15 identified 37 relevant samples. Random effects meta-analysis was performed because heterogeneity was expected. Geographic variations and time trends were also examined.
Important findings from the meta-analysis are presented in Table 4. In summary, cannabis use was found to be prevalent in about a third of patients with FEP. At follow-up, the odds of continued cannabis use were halved. The findings suggest that, given the established toxic effect of continued cannabis use on the course of schizophrenia,16 more effective intervention strategies are required to decrease cannabis use in patients with FEP.
Cannabis Use Continues to Compromise Outcomes After Onset of Psychosis
How is the course of existing psychosis affected in cannabis users, specifically with regard to continuation vs discontinuation of cannabis use? This question was examined by Schoeler et al16 in a systematic review and meta-analysis. These authors identified 24 relevant studies of patients with existing psychosis (pooled N = 16,565) who were followed for at least 6 months. Outcomes were expressed using Cohen d.
Important findings from this meta-analysis are presented in Table 5. In summary, in patients with psychosis, continued use of cannabis was associated with longer hospitalization and higher risk of relapse; discontinuation of cannabis brought the risk of relapse down to that in nonusers. Cannabis use was also associated with more severe positive (but not negative) symptoms and poorer levels of functioning.
These findings emphasize the importance of targeting cannabis use (with abstinence as the goal) in patients with psychosis. It may be noted, however, that effect sizes in this meta-analysis were small.
Explaining the Association Between Cannabis Use and the Risk of Psychosis
Cannabis use may be associated with psychosis as a causal factor, as a trigger, as an exacerbating variable, as a consequence of psychotic illness, or as combinations of these explanations. The data from the meta-analyses and other studies described in previous sections are epidemiologic in nature and therefore cannot establish a preference for any explanation. However, there is strong randomized, double-blind, placebo-controlled evidence from laboratory studies that shows that natural and synthetic cannabinoid agonists reliably produce psychosis-like positive, negative, cognitive, and psychophysiologic symptoms in healthy humans and exacerbate psychotic symptoms in patients with schizophrenia.17 It is therefore reasonable to conclude that cannabis plays some etiologic role in at least some persons who use the substance and who subsequently develop psychosis. Interestingly, possible neurotransmitter mechanisms, neural mechanisms, and genetic vulnerabilities have all been described for cannabis-related psychosis,17,18 as have possible distinctive psychopathologic characteristics19 and possible different manifestations of psychosis20 resulting from cannabis exposure.
Public Health Implications
A reasonable implication of the findings presented in previous sections is that if cannabis use is curtailed in the population, the onset of nonaffective psychoses such as schizophrenia might be delayed in some persons, and the course and outcome of the illness could become more favorable. Even if psychosis is inevitable, a later onset of illness would allow extra years for neurodevelopment in youth, higher education, and more time for social and vocational adjustment. These are worthwhile gains. Thus, cannabis use is a modifiable risk factor in the primary and secondary prevention of psychosis; however, the population attributable risk associated with cannabis exposure is presently uncertain.
General Notes About the Studies Described in This Article
The potency of cannabis preparations could not be examined in any of the meta-analyses described in this article. This is an important consideration because many studies have associated high potency cannabis use with greater risk or earlier occurrence of psychosis.21-23 However, in some of the meta-analyses, year of study did not predict outcomes; here, year of study may be a proxy for potency because the potency of street cannabis has been suggested to have increased over time.
Many potentially important confounds could not be examined in the various meta-analyses; these include, for example, the effects of socioeconomic status and the use of tobacco. Finally, none of the studies discussed in this article could establish whether there is a safe level of cannabis use. This remains an unknown in the medical literature.
Parting Note
Advocates of medical marijuana who argue that association with adverse outcomes does not prove cause might do well to consider that, if cannabis were to be suggested as a prescription drug by the pharmaceutical industry, the wealth of evidence of adverse outcomes associated with it would send social activists, human rights advocates, lawyers, and the mass media into a frenzy of outrage. Legislating marijuana into legitimacy does not make it safe.
 Each month in his online column, Dr Andrade considers theoretical and practical ideas in clinical psychopharmacology with a view to update the knowledge and skills of medical practitioners who treat patients with psychiatric conditions.
Each month in his online column, Dr Andrade considers theoretical and practical ideas in clinical psychopharmacology with a view to update the knowledge and skills of medical practitioners who treat patients with psychiatric conditions.
Department of Clinical Psychopharmacology and Neurotoxicology, National Institute of Mental Health and Neurosciences, Bangalore, India ([email protected]).
Financial disclosure and more about Dr Andrade.
REFERENCES
1. Andrade C. Cannabis and neuropsychiatry, 1: benefits and risks. J Clin Psychiatry. 2016;77(5):e551-e554.
2. Moore TH, Zammit S, Lingford-Hughes A, et al. Cannabis use and risk of psychotic or affective mental health outcomes: a systematic review. Lancet. 2007;370(9584):319-328. PubMed doi:10.1016/S0140-6736(07)61162-3
3. Hjorthoj CR, Baker A, Fohlmann A, et al. Intervention efficacy in trials targeting cannabis use disorders in patients with comorbid psychosis systematic review and meta-analysis. Curr Pharm Des. 2014;20(13):2205-2211. PubMed doi:10.2174/13816128113199990431
4. McLoughlin BC, Pushpa-Rajah JA, Gillies D, et al. Cannabis and schizophrenia. Cochrane Database Syst Rev. 2014;10:CD004837. PubMed
5. Large M, Sharma S, Compton MT, et al. Cannabis use and earlier onset of psychosis: a systematic meta-analysis. Arch Gen Psychiatry. 2011;68(6):555-561. PubMed doi:10.1001/archgenpsychiatry.2011.5
6. Helle S, Ringen PA, Melle I, et al. Cannabis use is associated with 3 years earlier onset of schizophrenia spectrum disorder in a naturalistic, multi-site sample (N=1119). Schizophr Res. 2016;170(1):217-221. PubMed doi:10.1016/j.schres.2015.11.027
7. Dragt S, Nieman DH, Schultze-Lutter F, et al; EPOS group. Cannabis use and age at onset of symptoms in subjects at clinical high risk for psychosis. Acta Psychiatr Scand. 2012;125(1):45-53. PubMed doi:10.1111/j.1600-0447.2011.01763.x
8. Allegri F, Belvederi Murri M, Paparelli A, et al. Current cannabis use and age of psychosis onset: a gender-mediated relationship? results from an 8-year FEP incidence study in Bologna. Psychiatry Res. 2013;210(1):368-370. PubMed doi:10.1016/j.psychres.2013.06.010
9. Tosato S, Lasalvia A, Bonetto C, et al. The impact of cannabis use on age of onset and clinical characteristics in first-episode psychotic patients: data from the Psychosis Incident Cohort Outcome Study (PICOS). J Psychiatr Res. 2013;47(4):438-444. PubMed doi:10.1016/j.jpsychires.2012.11.009
10. Donoghue K, Doody GA, Murray RM, et al. Cannabis use, gender and age of onset of schizophrenia: data from the ׆SOP study. Psychiatry Res. 2014;215(3):528-532. PubMed doi:10.1016/j.psychres.2013.12.038
11. Galvez-Buccollini JA, Proal AC, Tomaselli V, et al. Association between age at onset of psychosis and age at onset of cannabis use in non-affective psychosis. Schizophr Res. 2012;139(1-3):157-160. PubMed doi:10.1016/j.schres.2012.06.007
12. Stefanis NC, Dragovic M, Power BD, et al. Age at initiation of cannabis use predicts age at onset of psychosis: the 7- to 8-year trend. Schizophr Bull. 2013;39(2):251-254. PubMed doi:10.1093/schbul/sbs188
13. Marconi A, Di Forti M, Lewis CM, et al. Meta-analysis of the association between the level of cannabis use and risk of psychosis [published online ahead of print February 15, 2016]. Schizophr Bull. PubMed doi:10.1093/schbul/sbw003
14. Kraan T, Velthorst E, Koenders L, et al. Cannabis use and transition to psychosis in individuals at ultra-high risk: review and meta-analysis. Psychol Med. 2016;46(4):673-681. PubMed doi:10.1017/S0033291715002329
15. Myles H, Myles N, Large M. Cannabis use in first episode psychosis: meta-analysis of prevalence, and the time course of initiation and continued use. Aust N Z J Psychiatry. 2016;50(3):208-219. PubMed doi:10.1177/0004867415599846
16. Schoeler T, Monk A, Sami MB, et al. Continued versus discontinued cannabis use in patients with psychosis: a systematic review and meta-analysis. Lancet Psychiatry. 2016;3(3):215-225. PubMed doi:10.1016/S2215-0366(15)00363-6
17. Sherif M, Radhakrishnan R, D’ Souza DC, et al. Human laboratory studies on cannabinoids and psychosis. Biol Psychiatry. 2016;79(7):526-538. PubMed doi:10.1016/j.biopsych.2016.01.011
18. Volkow ND, Swanson JM, Evins AE, et al. Effects of cannabis use on human behavior, including cognition, motivation, and psychosis: a review. JAMA Psychiatry. 2016;73(3):292-297. PubMed doi:10.1001/jamapsychiatry.2015.3278
19. Baldacchino A, Hughes Z, Kehoe M, et al. Cannabis psychosis: examining the evidence for a distinctive psychopathology in a systematic and narrative review. Am J Addict. 2012;21(suppl 1):S88-S98. PubMed doi:10.1111/j.1521-0391.2012.00295.x
20. Wilkinson ST, Radhakrishnan R, D’ Souza DC. Impact of cannabis use on the development of psychotic disorders. Curr Addict Rep. 2014;1(2):115-128. PubMed doi:10.1007/s40429-014-0018-7
21. Di Forti M, Morgan C, Dazzan P, et al. High-potency cannabis and the risk of psychosis. Br J Psychiatry. 2009;195(6):488-491. PubMed doi:10.1192/bjp.bp.109.064220
22. Di Forti M, Sallis H, Allegri F, et al. Daily use, especially of high-potency cannabis, drives the earlier onset of psychosis in cannabis users. Schizophr Bull. 2014;40(6):1509-1517. PubMed doi:10.1093/schbul/sbt181
23. Di Forti M, Marconi A, Carra E, et al. Proportion of patients in south London with first-episode psychosis attributable to use of high potency cannabis: a case-control study. Lancet Psychiatry. 2015;2(3):233-238. PubMed doi:10.1016/S2215-0366(14)00117-5
This PDF is free for all visitors!