CME Background Information
Financial Disclosure
The faculty for this CME activity and the CME Institute staff were asked to complete a statement regarding all relevant personal and financial relationships between themselves or their spouse/partner and any commercial interest. The Accreditation Council for Continuing Medical Education (ACCME) defines a commercial interest as any entity producing, marketing, re-selling, or distributing health care goods or services consumed by, or used on, patients. The ACCME defines relevant financial relationships as financial relationships in any amount occurring within the past 12 months that create a conflict of interest. The CME Institute has resolved any conflicts of interest that were identified. No member of the CME Institute staff reported any relevant personal financial relationships. Faculty financial disclosure is as follows:
Dr Harvey is a consultant for Acadia, Alkermes, BioXcel, Boehringer Ingelheim, Intra Cellular Therapies, Minerva, Regeneron, and Sunovion; has received grant/research support from Stanley Medical Research Institute and Takeda; and has received other financial or material support for the Brief Assessment of Cognition in Schizophrenia. Dr Kane is a consultant for and has received honoraria from Acadia, Alkermes, Allergan, Dainippon Sumitomo, Lundbeck, Intra-Cellular Therapies, Janssen, Johnson & Johnson, LB Pharmaceuticals, Merck, Minerva, Neurocrine, Otsuka, Reviva, Roche, Saladex, Sunovion, Takeda, and Teva; has received grant/research support from Otsuka, Lundbeck, Sunovion, and Janssen; and is a stock shareholder of Vanguard Research Group and LB Pharmaceuticals.
The opinions expressed herein are those of the faculty and do not necessarily reflect the opinions of the CME provider and publisher or the commercial supporter.
Support Statement
Supported by an educational grant from Intra-Cellular Therapies, Inc.
Learning Objective
After completing this educational activity, you should be able to:
- Addressing adverse events that affect adherence in patients with schizophrenia
- Adopt a patient-centered approach to treatment for patients with schizophrenia
Accreditation Statement
The CME Institute of Physicians Postgraduate Press, Inc., is accredited by the Accreditation Council for Continuing Medical Education to provide continuing medical education for physicians.
Credit Designation
The CME Institute of Physicians Postgraduate Press, Inc., designates this journal-based CME activity for a maximum of 1.00 AMA PRA Category 1 Credit™. Physicians should claim only the credit commensurate with the extent of their participation in the activity.
Note: The American Nurses Credentialing Center (ANCC) and the American Academy of Physician Assistants (AAPA) accept certificates of participation for educational activities certified for AMA PRA Category 1 Credit™ from organizations accredited by the ACCME.
To obtain credit for this activity, study the material and complete the CME Posttest and Evaluation.
Release, Review, and Expiration Dates
This brief report activity was published in April 2021 and is eligible for AMA PRA Category 1 Credit™ through June 30, 2023. The latest review of this material was March 2021.
Statement of Need and Purpose
The goals of schizophrenia treatment are to control symptoms, prevent relapse, and improve functioning and quality of life. For many patients, these goals are not being met. Unfortunately, clinicians often make decisions that are not concordant with clinical evidence or guidelines. Psychiatrists cite personal experience as the factor that most influences their decision-making about treatment for patients with schizophrenia. Clinicians are often not taking a patient-centered approach to schizophrenia treatment selection; thus, patients feel uninvolved in the choice of their treatment and report less satisfaction with care. Guidelines recommend taking into account not only comorbid illness, concurrent medications, previous medication experiences, and side effect profiles but also patient preferences when selecting antipsychotics. Clinicians would benefit from a review of effective, evidence-based care to help patients improve adherence. They also need to know about new agents that may treat a broader range of symptoms and limit side effects that decrease patients’ adherence and must recognize the importance of adopting a patient-centered approach to schizophrenia treatment.
Disclosure of Off-Label Usage
Dr Harvey has determined that, to the best of his knowledge, no investigational information about pharmaceutical agents or device therapies that is outside US Food and Drug Administration–approved labeling has been presented in this activity.
Review Process
The faculty members agreed to provide a balanced and evidence-based presentation and discussed the topics and CME objectives during the planning sessions. The faculty’s submitted content was validated by CME Institute staff, and the activity was evaluated for accuracy, use of evidence, and fair balance by the Chair and a peer reviewer who is without conflict of interest.
Acknowledgment
This activity is derived from the teleconference series “Overcoming Adherence Issues and Providing Patient-Centered Care for People Living With Schizophrenia,” which was held in October and November 2020 and supported by an educational grant from Intra-Cellular Therapies, Inc. The opinions expressed herein are those of the faculty and do not necessarily reflect the opinions of the CME provider and publisher or the commercial supporter.
Clinical Points
- Use a patient-centric approach that focuses on alleviating problems that inhibit treatment adherence, such as adverse effects (AEs).
- A lower dose of antipsychotic agents may minimize AEs without impairing efficacy, thereby increasing the likelihood of treatment adherence.
- Evaluating patients’ concerns about particular AEs can help in matching treatment regimens to patients’ preferences as much as possible.
- Simplify dosing frequency and eliminate unnecessary medications to encourage adherence.
- Long-acting injectables are preferred over oral medications for many patients who have problems with adherence but who are responsive to treatment.
- Psychosocial interventions may improve patients’ medication adherence and thereby aid recovery.
Introduction
Schizophrenia is a severe, lifelong disorder that affects cognitive, behavioral, and emotional functioning.1 It is ranked among the top 25 leading causes of disability worldwide.2 Many individuals with schizophrenia experience numerous relapses and ongoing impairment, and less than 15% of individuals achieve functional recovery.3 Over the last 70 years, recovery rates and associated disability following a first psychotic episode in patients with schizophrenia have not improved despite regular clinical care.4
In this Academic Highlights, Drs Harvey and Kane will address best practices for improving adherence and outcomes for people living with schizophrenia, including lessening the side effect burden and providing comprehensive, patient-centric care.
Lessening the Side Effect Burden to Improve Adherence Among Individuals With Schizophrenia
According to Dr Kane, clinicians tend to put great emphasis on symptom resolution and functioning as treatment goals, whereas patients put greater value on well-being and quality of life.5 Many patients may experience more difficulty with adverse effects (AEs) than clinicians realize, he explained. AEs are a frequent reason for nonadherence to antipsychotic treatment among patients with schizophrenia.6 Dr Kane stated that poor adherence is associated with an increased risk of relapse, which may be associated with treatment resistance when medication is resumed (Figure 1).7
Figure 1. Risks Associated With Intolerable Adverse Effects in Patients Living With Schizophrenia
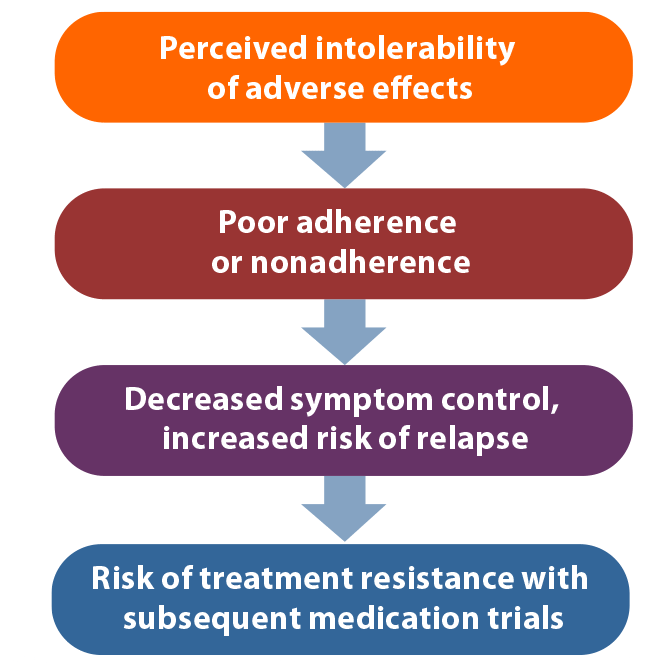
Based on Kane and Correll.7
Patient Perspectives
Here, patients living with schizophrenia describe adverse effects with their prescribed antipsychotics, and some consider whether they are balanced by efficacy:
“All antipsychotics cause me an anxiety which isn’t there if I am not on meds. It’s the kind of anxiety that makes me scared of driving/other people’s driving and law and parents’ death. I have this fear that something bad will happen that will get me in trouble.”8
“I can function better I suppose, meaning that what I experience daily with hallucinations are [sic] more easy to ignore (still there though). Delusions and paranoia are almost not there. Sometimes they will come flowing out but it doesn’t last long while on the meds. As far as side effects go with the meds, I have almost zero energy every day. I have insomnia and hardly sleep and almost no appetite at all. Due to hardly ever getting hungry, I at times just forget to even eat. The meds has [sic] helped but they are no miracle cure. They cause many other new problems that you have to deal with, and at times the ‘cure’ is worse then [sic] the illness.”9
“I struggle with insomnia or sometimes sleep too much to the point it’s super hard to get up—no in-between. This is gonna cause a lot of trouble when I do get a job.”9
“I have gained massive weight … and become diabetic. My delusions are improved however.”8
“All of these medications unfortunately have the potential for negative side effects. I notice a couple side effects like grogginess and more hunger, but the benefits outweigh the negatives for me.”9
Adverse Effects and Nonadherence
Dr Kane explained that meta-analyses of acute antipsychotic treatment10 and maintenance antipsychotic treatment11,12 indicate that, although some agents have symptom efficacy advantages over others, greater differences are found in their clinically relevant side effect profiles. When atypical antipsychotics were first introduced, it was hoped that because they had fewer neurologic side effects than older antipsychotics, they would significantly increase the adherence rate. Yet, Dr Kane stated, nonadherence continues to be an enormous problem.13,14
According to data from the CATIE study,15 which examined the comparative effectiveness of second-generation antipsychotics for 1,493 individuals with schizophrenia, hypersomnia/sleepiness was the most commonly reported AE among patients receiving olanzapine, quetiapine, risperidone, and perphenazine. The rates of treatment discontinuation due to intolerable side effects before the study was completed were 18% with olanzapine, 10% with risperidone, and 15% each with quetiapine, perphenazine, and ziprasidone.
Certain antipsychotic-related AEs are especially problematic for patients. Dr Kane noted that the AE that patients describe as having the most negative impact on their quality of life is weight gain,16 which is often associated with some antipsychotics, particularly olanzapine. One recent patient survey17 (N = 200) reported that, while 92% of patients said that their oral antipsychotic treatment improved symptoms and 67% indicated that they needed medication, only half of the patients thought that the antipsychotic did more good than harm. The 3 most commonly reported side effects were anxiety (88%), feeling drowsy or tired (86%), and trouble concentrating (85%).17 More respondents rated weight gain and sexual dysfunction as extremely or very bothersome than they did other AEs.17 Dr Kane mentioned that another patient survey,18 in which only 43% of respondents reported complete adherence, found reduced adherence with the following types of AEs: agitation, extrapyramidal symptoms (EPS), sedation and cognition problems, prolactin and endocrine effects, and metabolic effects.
Adverse Effects and Health Risks
Dr Kane explained that patients with schizophrenia may have health risks related to genetics and lifestyle, meaning that AEs not only can be bothersome to patients but also can exacerbate existing morbidity and mortality risks.19 Many patients are overweight and smoke, he noted.20 The Recovery After an Initial Schizophrenia Episode (RAISE) study,20 which assessed first-episode patients (aged 15 to 40 years) who were treated with antipsychotic drugs for less than 6 months, showed that the patients had a myriad of health concerns. Of the 404 patients, 57% had dyslipidemia, 10% experienced high blood pressure, and 13% had metabolic syndrome. Based on hemoglobin A1c results, 15% were prediabetic, and 3% had diabetes.20 Because of the short duration of antipsychotic use, these data illustrate that exposure to antipsychotics is not the only factor increasing the risk of health problems.
Techniques for Reducing Adverse Effects
Dr Kane shared that, in his clinical experience, he has found that prescribing the lowest effective dose of antipsychotics may minimize AEs. Both efficacy and AEs may increase as dosage increases.21 The increase in efficacy diminishes considerably above twice the minimum effective dose.21,22 In maintenance treatment, he explained that it is important to try using the lowest effective dosage to reduce the risk of AEs and increase the likelihood that patients will adhere to treatment. Dr Kane stated that often in his clinical practice he has seen patients who are receiving higher than necessary doses, which are not associated with greater efficacy but are associated with greater AEs. Additionally, once-daily administration of antipsychotic treatment is not inferior in efficacy to divided doses, and some AEs, such as anxiety and sleepiness, are reduced by using once-daily dosing.23 Dr Kane also noted that because the newer antipsychotic agents have lower rates of motor, metabolic, cardiovascular, and endocrinal AEs than the older agents,24,25 patients may find them more tolerable.
Guidelines26–28 recommend that, in making treatment decisions, clinicians consider medication side effect profiles and patient preferences. With a patient-centered approach, noted Dr Kane, clinicians assess not only patients’ degree of adherence but also their reasons for nonadherence. By evaluating patients’ concerns about particular AEs, clinicians can make an effort to match treatment regimens to patients’ preferences as much as possible so that adherence problems related to AEs might be resolved.
Patient-Centered Treatment Strategies to Improve Outcomes in Schizophrenia
In his presentation, Dr Harvey discussed factors that are associated with successful clinical and functional outcomes in patients with schizophrenia. These factors include a short duration of untreated psychosis,29 an early response to antipsychotic treatment,30 a collaborative therapeutic alliance,31 a supportive family or caregiver,32 and opportunities to engage in functional activities and specialized interventions.33
Defining Remission and Recovery
The Remission in Schizophrenia Working Group (RSWG) developed the first consensus-based criteria34 for symptom remission as applied to schizophrenia. The RSWG employed the Positive and Negative Syndrome Scale (PANSS),35 which defines remission as symptom ratings of mild or lower severity (PANSS score ≤ 3) for at least 6 months.34
Criteria for functional recovery36 typically require patients to experience symptom remission, vocational function, independent living, and peer relationships for more than 2 years. According to Dr Harvey, however, in his clinical experience, he finds it critical to view recovery more as a process than an outcome.37,38 Dr Harvey and his colleague Alan S. Bellack, PhD, created a model for functional remission37 that delineates domains of functioning as well as levels and breadth of accomplishment across the functional domains (Figure 2). The 3 domains of functioning are independent living, productive activities, and social life. In these domains, patients may make no attempt at progress or may attempt achievements without success, but they may also reach various levels of accomplishment, including making progress with little success, achieving partial success, and achieving full success. Their breadth of accomplishment describes how many domains in which they are achieving progress or success. When patients are striving to make accomplishments, whether in 1 domain or more, clinicians should view their efforts as important steps in the process toward recovery.
Figure 2. Functional Remission Model for Patients With Schizophrenia
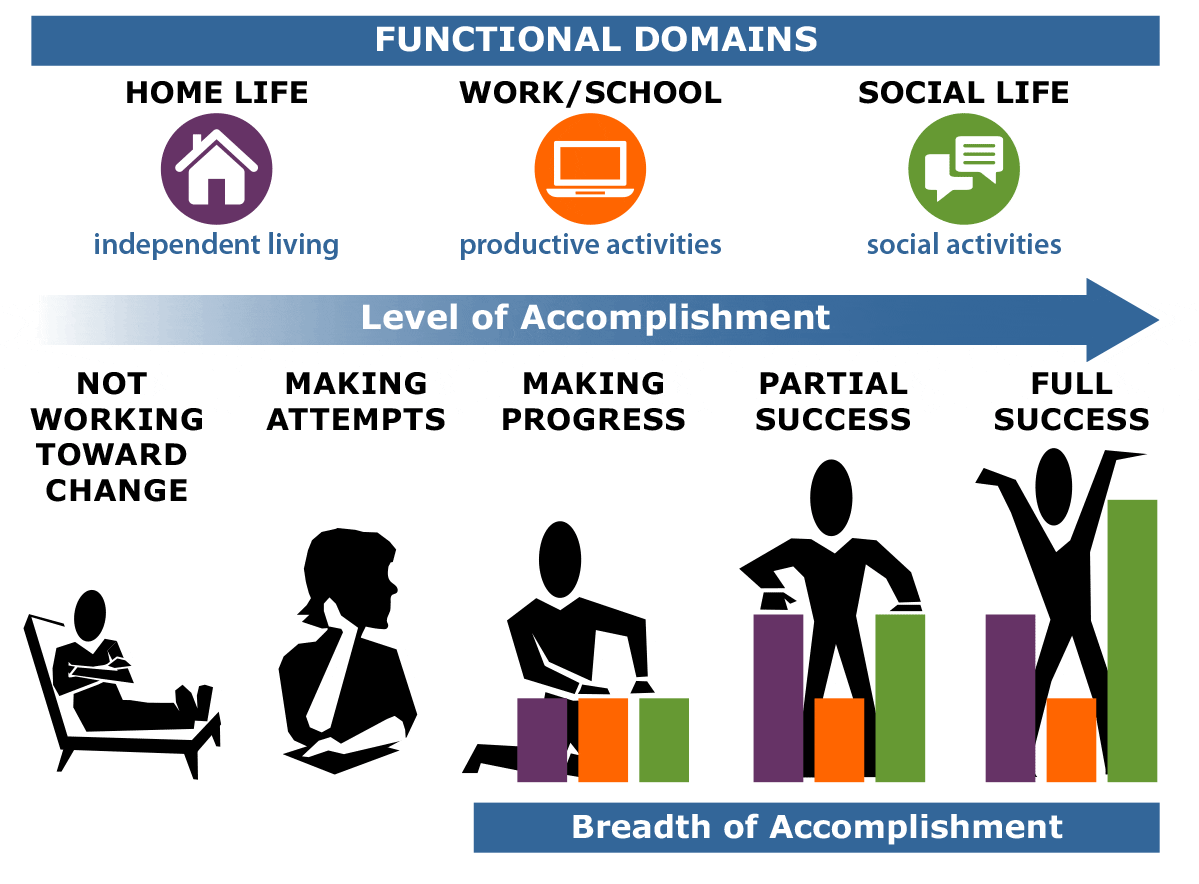
Based on Harvey and Bellack.37
Patient Perspectives
Patients shared their experiences taking steps toward recovery:
“I’ve seen a steady improvement in my life since starting antipsychotics about a year ago. I started [a medication] last February or so. It worked really well for me overall but around the end of October I had a major episode that lasted for about 2–3 weeks. I didn’t think I was ever going to get out of it. My psychiatrist then switched [to another antipsychotic]. I’ve snapped out of that episode and now I feel like I’m starting to get my life on track. I’ve been able to hold down a part time job because of it, which has in return been a positive thing for me instead of sitting at home in my head all day.”9
“I have been working for a year at my job and am doing well. I still have symptoms but weather the storm and am doing fairly well. I don’t work full-time though but am able to pay my bills and for my food. I am doing ok and am grateful for the medication. … Without medication, I was homeless and severely symptomatic. I learned from my experience of homelessness that I need to be on medication at all costs. I also realized I would rather work than do nothing. So, since I want to work, I need to take my medication. … I know that being compliant is key for my survival and independence.”9
Nonadherence and Relapse
Relapses of psychotic symptoms impede recovery.39 With each successive relapse, Dr Harvey explained, the next remission becomes harder to achieve.40 The single biggest risk factor for relapse is medication nonadherence.41 A 2020 analysis of studies that reported medication nonadherence found that, among 2,643 patients with schizophrenia, the rate of nonadherence was 56%.42 In a naturalistic study43 that followed 876 patients with schizophrenia for 1 year after hospital discharge, the relapse rates were 21% among adherent patients and 55% among nonadherent patients.
Patient Perspectives
Here, a patient describes maintaining his adherence, despite friends telling him not to, because he does not want to relapse:
“I’ve got this longstanding women [sic] friend …, she keeps on pushing me to come off meds. Usually with friends I explain, [and] then if they don’t drop it, I question their motives and whether they really are friends. We have a lot of arguments as she watches these questionable you tube videos. Today she watched one about mental health; when I said I don’t want to hear more, we had an argument.
“I’m the first to say in an ideal world I wouldn’t need meds but this isn’t an ideal world. In what I consider the real world, I’ve seen schitzoprenics [sic] get into some terrible situations by coming off meds… What goes with it [is] alienating what few people I know, losing what I’ve gained over the years.
I“I asked my GP what would happen, she said we don’t know but without any guarentees [sic], [it’s] playing with fire.”44
Reasons for Nonadherence
Patients may fail to fill medication prescriptions or may fail to take medication they have. Dr Harvey discussed 3 factors that are empirically associated with adherence failure: cognitive challenges, unawareness of illness, and problems with organization.41,45
Cognitive challenges. Impairments in memory, executive function, and cognitive performance are associated with nonadherence.46 These impairments correlate directly with performance-based assessments of the ability to manage medication: patients are not able to remember to fill their medication, are unable to remember how to take their medication, or are not organized enough to manage to properly take their medication.
Unawareness of illness. Functional insight is often impaired due to a patient’s deficit of awareness of their illness.47 This lack of insight may leave patients with schizophrenia unable to index how likely they are to succeed in certain tasks, what training they might need, and what tasks they are capable of performing. Dr Harvey shared that, in his clinical experience, if a patient is not aware that they have an illness, and they do not appreciate the fact that their medication has a specific purpose, they may not adhere simply because they cannot piece together the reasons for taking the medication.
Organizational challenges. According to Dr Harvey, organizational challenges, which lie on the boundary between cognitive challenges and lack of illness insight, affect patients in various ways. For example, he mentioned that some patients typically fill their prescriptions but do not store the medication adequately, and other patients generally fill their prescriptions only when they are reminded by someone else.
Dr Harvey pointed out that many patients lack the functional capacity necessary to navigate the refill system.48 In our current health care system, prescriptions are sent to the pharmacy electronically, and if the patient has the right device, they receive a message that their medication is ready to be picked up. If the refill system is not automated via text messages, refills have to be ordered using the telephone or internet, and internet access is still inaccessible for many populations, such as US veterans.49,50
Other organizational challenges identified by Dr Harvey include the following: some antipsychotics (eg, ziprasidone51) have food requirements; patients may have to meet laboratory requirements to get their medication refill52; and lack of attendance at mental health clinic appointments may result in a patient being terminated from the clinic.53–55
Improving Outcomes With Patient-Centered Treatment Strategies
Shared decision-making. Samalin and colleagues56 found that psychiatrists cited personal experience as the factor that most influenced their decision-making about treatment for patients with schizophrenia. Too often, clinicians do not recognize that patients want to be involved in clinical decisions. One study57 found that antipsychotic treatment decisions were made without input from patients or caregivers 67% of the time. The use of shared decision-making strategies could reduce perceived coercion by patients with schizophrenia in regard to prescribed treatments.58 Active involvement in treatment decisions may alleviate the patient’s fears and disperse negative thoughts about previous experiences. Patients who have been allowed to take a more active role in clinical decisions have been found to report greater satisfaction with treatment.59
Simplification of treatment. Simplification of treatment regimens60 can increase medication adherence, reduce relapses, and aid recovery. For example, research indicates that certain medications, particularly anticonvulsants and antidepressants, show little efficacy in schizophrenia.61–64 Dr Harvey noted that data are particularly poor for antidepressants prescribed to treat negative symptoms.65 If the clinician adds an anticonvulsant or an antidepressant to a patient’s treatment regimen for schizophrenia, that regimen may have little efficacy and yet may be very challenging for the patient to keep up with.66,67
People with schizophrenia are also commonly treated with more than 1 antipsychotic, but data suggest that treating a patient with 2 antipsychotics does not have benefit compared to monotherapy.68,69 Additionally, Dr Harvey shared that in his clinical experience, once-per-day dosing is an effective way to prescribe medication. Dosing frequency is diminished further with the use of long-acting injectable (LAI) antipsychotics, which can be given once per month or less often. A 12-month study70 comparing the use of oral medication versus LAIs reported that patients receiving LAIs had lower discontinuation rates and fewer inpatient admissions and hospital days.
Psychosocial interventions. Dr Harvey said that offering psychosocial intervention programs is another way to support individuals with schizophrenia.71 Nonpharmacologic therapies not only complement medication, they may also ensure that patients remain adherent to their medications.72 Psychotherapies, such as cognitive-behavioral therapy (CBT), supportive therapy, and compliance therapy, educate patients about the importance of taking their medications. One recent study73 found a 57% recovery rate in patients with schizophrenia who received psychosocial interventions.
Rehabilitative programs targeting social cognition may further facilitate the recovery progress and re-engagement with work, school, and life. Studies74–77 indicate that cognitive remediation, social cognition training, and functional skills training lead to improvements in employment, cognition, and negative symptoms. Functional skills can be assessed using computer-based simulations of everyday activities, such as banking, refilling prescriptions, and completing forms.48 Studies have found reductions in both clinical symptom severity and rehospitalization when patients work for pay.78 Participation in paid work is also associated with increased quality of life.79
Patient Perspectives
An individual living with schizophrenia discusses her recovery with the support of her mother and health care provider:
“I had my first psychosis when I was 19. … A year later I stopped my meds and had another psychosis and month long hospital stay. Both my hospitalizations were involuntary….
“Thankfully I found a medication I could tolerate. I fought with hallucinations for years. At my first job I didn’t talk to anyone for 6 months. I had to relearn how to commutate [communicate]. People didn’t react well when I told them I had schizophrenia so I learned to hide it. …
“The last time I had a relapse I was told by the doctor, every time I have one, the harder it is to come back. My mom forced me to take my medication. She would watch me take it. Over the years I gained enough insight to know I need meds. Psychosis is my biggest fear. I never want to end up in that state of mind again. I just want to give hope to those out there suffering from this illness that with the right meds and dedication you can overcome this illness enough to where you can find peace in life.”80
Case Practice Question
DeShawn is 23 years old and has had schizophrenia for 2 years. When he began treatment, he had trouble concentrating and started gaining weight, so he was reluctant to keep taking medication. After a period of nonadherence, DeShawn relapsed and was rehospitalized. After his discharge on a different antipsychotic that is less associated with weight gain, his mother decided DeShawn needed different outpatient care, so she brought him to your office. As you discuss the road to recovery with them, which of the following statements would you avoid, based on evidence? |
|
a. You will monitor his antipsychotic adherence, response, and side effects to find the minimum effective dose so that DeShawn’s adverse effects might be reduced. |
|
b. If antipsychotic monotherapy does not adequately manage symptoms, you can prescribe DeShawn 2 different medications. |
|
c. If DeShawn is interested in not taking daily medication, he could try a long-acting injectable antipsychotic. |
|
d. Finding paid work, which DeShawn says he wants to do, is a suitable goal. |
Discussion of the Case Practice Question
Preferred response: The preferred response is b. If antipsychotic monotherapy does not adequately manage symptoms, you can prescribe DeShawn 2 different medications.
Explanation: Both efficacy and AEs may increase as antipsychotic dosage increases.21 Guidelines28 recommend monitoring adherence, response, and AEs. Data suggest that treating a patient with 2 antipsychotics does not have benefit compared to monotherapy.68,69 Less frequent dosing can improve patients’ adherence,70,81 and some patients prefer LAI antipsychotics.82 Person-centered care involves understanding patients’ goals,28 such as obtaining paid work, which is associated with improved quality of life79 and greater clinical stability.78
Conclusion
Schizophrenia is a severe, lifelong disorder that affects cognitive, behavioral, and emotional functioning. Many individuals living with schizophrenia experience numerous relapses and ongoing impairment. Adverse effects are a frequent reason for medication nonadherence among patients with schizophrenia, and nonadherence is a major risk factor for relapse. Strategies that may contribute to better outcomes include addressing patients’ side effect burden, simplifying the medication regimen, using shared decision-making, and offering psychosocial interventions. Clinicians should view recovery as a process and applaud patients’ steps toward progress in various functional domains even when patients do not fully succeed in all domains.
From the Series: Overcoming Adherence Issues and Providing Patient-Centered Care for People Living With Schizophrenia
To cite: Harvey PD, Kane JM. Addressing patients’ unmet needs to improve outcomes in schizophrenia. J Clin Psychiatry. 2021;82(3):IC20018AH3C.
To share: https://doi.org/10.4088/JCP.IC20018AH3C
© Copyright 2021 Physicians Postgraduate Press, Inc.
References
1. American Psychiatric Association. Diagnostic and Statistical Manual for Mental Disorders. Fifth Edition. Washington, DC: American Psychiatric Association; 2013.
2. Chong HY, Teoh SL, Wu DB-C, et al. Global economic burden of schizophrenia: a systematic review. Neuropsychiatr Dis Treat. 2016;12:357–373. PubMed CrossRef
3. Remington G, Foussias G, Fervaha G, et al. Treating negative symptoms in schizophrenia: an update. Curr Treat Options Psychiatry. 2016;3(2):133–150. PubMed CrossRef
4. Fusar-Poli P, McGorry PD, Kane JM. Improving outcomes of first-episode psychosis: an overview. World Psychiatry. 2017;16(3):251–265. PubMed CrossRef
5. Gründer G, Bauknecht P, Klingberg S, et al. Treatment goals for patients with schizophrenia—a narrative review of physician and patient perspectives. Pharmacopsychiatry. 2021;54(2):53–59. PubMed CrossRef
6. Dufort A, Zipursky RB. Understanding and managing treatment adherence in schizophrenia [published online January 3, 2019]. Clin Schizophr Relat Psychoses. PubMed CrossRef
7. Kane JM, Correll CU. Optimizing treatment choices to improve adherence and outcomes in schizophrenia. J Clin Psychiatry. 2019;80(5):IN18031AH1C. PubMed CrossRef
8. Aripiprazole. Mental Health Forum. Accessed February 18, 2021. https://www.mentalhealthforum.net/forum/threads/aripiprazole.307217
9. How much has your life been improved since you’ve went on an antipsychotic? Mental Health Forum. Published February 10, 2021. Accessed March 2, 2021. https://www.mentalhealthforum.net/forum/threads/how-much-has-your-life-been-improved-since-youve-went-on-an-antipsychotic.354382/
10. Huhn M, Nikolakopoulou A, Schneider-Thoma J, et al. Comparative efficacy and tolerability of 32 oral antipsychotics for the acute treatment of adults with multi-episode schizophrenia: a systematic review and network meta-analysis. Lancet. 2019;394(10202):939–951. PubMed CrossRef
11. Kishimoto T, Hagi K, Nitta M, et al. Long-term effectiveness of oral second-generation antipsychotics in patients with schizophrenia and related disorders: a systematic review and meta-analysis of direct head-to-head comparisons. World Psychiatry. 2019;18(2):208–224. PubMed CrossRef
12. Ceraso A, Lin JJ, Schneider-Thoma J, et al. Maintenance treatment with antipsychotic drugs for schizophrenia. Cochrane Database Syst Rev. 2020;8:CD008016. PubMed CrossRef
13. Dolder CR, Lacro JP, Jeste DV. Adherence to antipsychotic and nonpsychiatric medications in middle-aged and older patients with psychotic disorders. Psychosom Med. 2003;65(1):156–162. PubMed CrossRef
14. MacEwan JP, Forma FM, Shafrin J, et al. Patterns of adherence to oral atypical antipsychotics among patients diagnosed with schizophrenia. J Manag Care Spec Pharm. 2016;22(11):1349–1361. PubMed CrossRef
15. Lieberman JA, Stroup TS, McEvoy JP, et al; Clinical Antipsychotic Trials of Intervention Effectiveness (CATIE) Investigators. Effectiveness of antipsychotic drugs in patients with chronic schizophrenia. N Engl J Med. 2005;353(12):1209–1223. PubMed CrossRef
16. McIntyre RS. Understanding needs, interactions, treatment, and expectations among individuals affected by bipolar disorder or schizophrenia: the UNITE global survey. J Clin Psychiatry. 2009;70(suppl 3):5–11. PubMed CrossRef
17. Doane MJ, Sajatovic M, Weiden PJ, et al. Antipsychotic treatment experiences of people with schizophrenia: patient perspectives from an online survey. Patient Prefer Adherence. 2020;14:2043–2054. PubMed CrossRef
18. Dibonaventura M, Gabriel S, Dupclay L, et al. A patient perspective of the impact of medication side effects on adherence: results of a cross-sectional nationwide survey of patients with schizophrenia. BMC Psychiatry. 2012;12(1):20. PubMed CrossRef
19. Stahl SM, Mignon L, Meyer JM. Which comes first: atypical antipsychotic treatment or cardiometabolic risk? Acta Psychiatr Scand. 2009;119(3):171–179. PubMed CrossRef
20. Correll CU, Robinson DG, Schooler NR, et al. Cardiometabolic risk in patients with first-episode schizophrenia spectrum disorders: baseline results from the RAISE-ETP study. JAMA Psychiatry. 2014;71(12):1350–1363. PubMed CrossRef
21. Takeuchi H, MacKenzie NE, Samaroo D, et al. Antipsychotic dose in acute schizophrenia: a meta-analysis. Schizophr Bull. 2020;46(6):1439–1458. PubMed CrossRef
22. Leucht S, Crippa A, Siafis S, et al. Dose-response meta-analysis of antipsychotic drugs for acute schizophrenia. Am J Psychiatry. 2020;177(4):342–353. PubMed CrossRef
23. Kikuchi YS, Ataka K, Yagisawa K, et al. Clozapine administration and the risk of drug-related pure red cell aplasia: a novel case report. J Clin Psychopharmacol. 2014;34(6):763–764. PubMed CrossRef
24. Solmi M, Murru A, Pacchiarotti I, et al. Safety, tolerability, and risks associated with first- and second-generation antipsychotics: a state-of-the-art clinical review. Ther Clin Risk Manag. 2017;13:757–777. PubMed CrossRef
25. Corponi F, Fabbri C, Bitter I, et al. Novel antipsychotics specificity profile: A clinically oriented review of lurasidone, brexpiprazole, cariprazine and lumateperone. Eur Neuropsychopharmacol. 2019;29(9):971–985. PubMed CrossRef
26. Keating D, McWilliams S, Schneider I, et al. Pharmacological guidelines for schizophrenia: a systematic review and comparison of recommendations for the first episode. BMJ Open. 2017;7(1):e013881. PubMed CrossRef
27. Remington G, Addington D, Honer W, et al. Guidelines for the pharmacotherapy of schizophrenia in adults. Can J Psychiatry. 2017;62(9):604–616. PubMed CrossRef
28. Keepers GA, Fochtmann LJ, Anzia JM, et al. The American Psychiatric Association Practice Guideline for the Treatment of Patients With Schizophrenia. 3rd ed. Arlington, VA: American Psychiatric Association Publishing; 2021.
29. Murru A, Carpiniello B. Duration of untreated illness as a key to early intervention in schizophrenia: a review. Neurosci Lett. 2018;669:59–67. PubMed CrossRef
30. Carbon M, Correll CU. Clinical predictors of therapeutic response to antipsychotics in schizophrenia. Dialogues Clin Neurosci. 2014;16(4):505–524. PubMed CrossRef
31. Chang JG, Roh D, Kim C-H. Association between therapeutic alliance and adherence in outpatient schizophrenia patients. Clin Psychopharmacol Neurosci. 2019;17(2):273–278. PubMed CrossRef
32. Verma PK, Walia TS, Chaudhury S, et al. Family psychoeducation with caregivers of schizophrenia patients: impact on perceived quality of life. Ind Psychiatry J. 2019;28(1):19–23. PubMed CrossRef
33. Owen MJ, Sawa A, Mortensen PB. Schizophrenia. Lancet. 2016;388(10039):86–97. PubMed CrossRef
34. Andreasen NC, Carpenter WT Jr, Kane JM, et al. Remission in schizophrenia: proposed criteria and rationale for consensus. Am J Psychiatry. 2005;162(3):441–449. PubMed CrossRef
35. Kay SR, Fiszbein A, Opler LA. The positive and negative syndrome scale (PANSS) for schizophrenia. Schizophr Bull. 1987;13(2):261–276. PubMed CrossRef
36. Liberman RP, Kopelowicz A, Ventura J, et al. Operational criteria and factors related to recovery from schizophrenia. Int Rev Psychiatry. 2002;14(4):256–272. CrossRef
37. Harvey PD, Bellack AS. Toward a terminology for functional recovery in schizophrenia: is functional remission a viable concept? Schizophr Bull. 2009;35(2):300–306. PubMed CrossRef
38. Yildiz M. Recovery as a process in severe mental illnesses. Noro Psikiyatri Arsivi. 2015;52(1):1–3. PubMed CrossRef
39. Olivares JM, Sermon J, Hemels M, et al. Definitions and drivers of relapse in patients with schizophrenia: a systematic literature review. Ann Gen Psychiatry. 2013;12(1):32. PubMed CrossRef
40. Haddad PM, Brain C, Scott J. Nonadherence with antipsychotic medication in schizophrenia: challenges and management strategies. Patient Relat Outcome Meas. 2014;5:43–62. PubMed CrossRef
41. Higashi K, Medic G, Littlewood KJ, et al. Medication adherence in schizophrenia: factors influencing adherence and consequences of nonadherence, a systematic literature review. Ther Adv Psychopharmacol. 2013;3(4):200–218. PubMed CrossRef
42. Semahegn A, Torpey K, Manu A, et al. Psychotropic medication non-adherence and its associated factors among patients with major psychiatric disorders: a systematic review and meta-analysis. Syst Rev. 2020;9(1):17. PubMed CrossRef
43. Xiao J, Mi W, Li L, et al. High relapse rate and poor medication adherence in the Chinese population with schizophrenia: results from an observational survey in the People’s Republic of China. Neuropsychiatr Dis Treat. 2015;11(11):1161–1167. PubMed CrossRef
44. A close friend pushes me to come off meds. Mental Health Forum. Published March 1, 2021. Accessed March 2, 2021. https://www.mentalhealthforum.net/forum/threads/a-close-friend-pushes-me-to-come-off-meds.359339/
45. Acosta FJ, Bosch E, Sarmiento G, et al. Evaluation of noncompliance in schizophrenia patients using electronic monitoring (MEMS) and its relationship to sociodemographic, clinical and psychopathological variables. Schizophr Res. 2009;107(2-3):213–217. PubMed CrossRef
46. Bowie CR, Harvey PD. Cognitive deficits and functional outcome in schizophrenia. Neuropsychiatr Dis Treat. 2006;2(4):531–536. PubMed CrossRef
47. Choudhury S, Khess CRJ, Bhattacharyya R, et al. Insight in schizophrenia and its association with executive functions. Indian J Psychol Med. 2009;31(2):71–76. PubMed CrossRef
48. Czaja SJ, Loewenstein DA, Lee CC, et al. Assessing functional performance using computer-based simulations of everyday activities. Schizophr Res. 2017;183:130–136. PubMed CrossRef
49. McInnes DK, Gifford AL, Kazis LE, et al. Disparities in health-related internet use by US veterans: results from a national survey. Inform Prim Care. 2010;18(1):59–68. PubMed CrossRef
50. Wireline Competition Bureau. Report on Promoting Broadband Internet Access Service for Veterans, Pursuant to the Repack Airwaves Yielding Better Access for Users of Modern Services Act of 2018. US Federal Communications Commission. Published May 2019. https://docs.fcc.gov/public/attachments/DOC-357270A1.pdf
51. Citrome L. Using oral ziprasidone effectively: the food effect and dose-response. Adv Ther. 2009;26(8):739–748. PubMed CrossRef
52. Kelly DL, Ben-Yoav H, Payne GF, et al. Blood draw barriers for treatment with clozapine and development of a point-of-care monitoring device. Clin Schizophr Relat Psychoses. 2018;12(1):23–30. PubMed CrossRef
53. Miller MJ, Ambrose DM. The problem of missed mental healthcare appointments. Clin Schizophr Relat Psychoses. 2019;12(4):177–184. PubMed CrossRef
54. Ibironke Thomas F, Osasu Olotu S, Ohiole Omoaregba J. Prevalence, factors and reasons associated with missed first appointments among out-patients with schizophrenia at the Federal Neuro-Psychiatric Hospital, Benin City. BJPsych Open. 2018;4(2):49–54. PubMed CrossRef
55. Peterson K, McCleery E, Anderson J, et al. Evidence brief: comparative effectiveness of appointment recall reminder procedures for follow-up appointments. VA Evidence Synthesis Program Evidence Briefs. VA Evidence Synthesis Program Reports. US Department of Veterans Affairs; 2011. Accessed December 9, 2020. http://www.ncbi.nlm.nih.gov/books/NBK384609/
56. Samalin L, Garnier M, Auclair C, et al. Clinical decision-making in the treatment of schizophrenia: focus on long-acting injectable antipsychotics. Int J Mol Sci. 2016;17(11):1935. PubMed CrossRef
57. Potkin S, Bera R, Zubek D, et al. Patient and prescriber perspectives on long-acting injectable (LAI) antipsychotics and analysis of in-office discussion regarding LAI treatment for schizophrenia. BMC Psychiatry. 2013;13(1):261. PubMed CrossRef
58. Fiorillo A, Barlati S, Bellomo A, et al. The role of shared decision-making in improving adherence to pharmacological treatments in patients with schizophrenia: a clinical review. Ann Gen Psychiatry. 2020;19(1):43. PubMed CrossRef
59. Clarke E, Puschner B, Jordan H, et al. Empowerment and satisfaction in a multinational study of routine clinical practice. Acta Psychiatr Scand. 2015;131(5):369–378. PubMed CrossRef
60. Burton SC. Strategies for improving adherence to second-generation antipsychotics in patients with schizophrenia by increasing ease of use. J Psychiatr Pract. 2005;11(6):369–378. PubMed CrossRef
61. Terevnikov V, Joffe G, Stenberg J-H. Randomized controlled trials of add-on antidepressants in schizophrenia. Int J Neuropsychopharmacol. 2015;18(9):pyv049. PubMed CrossRef
62. Galling B, Vernon JA, Pagsberg AK, et al. Efficacy and safety of antidepressant augmentation of continued antipsychotic treatment in patients with schizophrenia. Acta Psychiatr Scand. 2018;137(3):187–205. PubMed CrossRef
63. Wang Y, Xia J, Helfer B, et al. Valproate for schizophrenia. Cochrane Database Syst Rev. 2016;11(11):CD004028. PubMed CrossRef
64. Citrome L. Adding lithium or anticonvulsants to antipsychotics for the treatment of schizophrenia: useful strategy or exercise in futility? J Clin Psychiatry. 2009;70(6):932–933. PubMed CrossRef
65. Hinkelmann K, Yassouridis A, Kellner M, et al. No effects of antidepressants on negative symptoms in schizophrenia. J Clin Psychopharmacol. 2013;33(5):686–690. PubMed CrossRef
66. Zink M, Englisch S, Meyer-Lindenberg A. Polypharmacy in schizophrenia. Curr Opin Psychiatry. 2010;23(2):103–111. PubMed CrossRef
67. Toto S, Grohmann R, Bleich S, et al. Psychopharmacological treatment of schizophrenia over time in 30,908 inpatients: data from the AMSP study. Int J Neuropsychopharmacol. 2019;22(9):560–573. PubMed CrossRef
68. Civan Kahve A, Kaya H, Gül Çakıl A, et al. Multiple antipsychotics use in patients with schizophrenia: why do we use it, what are the results from patient follow-ups? Asian J Psychiatr. 2020;52:102063. PubMed CrossRef
69. Farrell C, Brink J. The prevalence and factors associated with antipsychotic polypharmacy in a forensic psychiatric sample. Front Psychiatry. 2020;11:263. PubMed CrossRef
70. Shah A, Xie L, Kariburyo F, et al. Treatment patterns, healthcare resource utilization and costs among schizophrenia patients treated with long-acting injectable versus oral antipsychotics. Adv Ther. 2018;35(11):1994–2014. PubMed CrossRef
71. Mueser KT, Deavers F, Penn DL, et al. Psychosocial treatments for schizophrenia. Annu Rev Clin Psychol. 2013;9(1):465–497. PubMed CrossRef
72. Patel KR, Cherian J, Gohil K, et al. Schizophrenia: overview and treatment options. P T. 2014;39(9):638–645. PubMed
73. Buonocore M, Bosia M, Baraldi MA, et al. Achieving recovery in patients with schizophrenia through psychosocial interventions: a retrospective study. Psychiatry Clin Neurosci. 2018;72(1):28–34. PubMed CrossRef
74. Ventura J, Subotnik KL, Gretchen-Doorly D, et al. Cognitive remediation can improve negative symptoms and social functioning in first-episode schizophrenia: A randomized controlled trial. Schizophr Res. 2019;203:24–31. PubMed CrossRef
75. Lindenmayer J-P, Khan A, McGurk SR, et al. Does social cognition training augment response to computer-assisted cognitive remediation for schizophrenia? Schizophr Res. 2018;201:180–186. PubMed CrossRef
76. McGurk SR, Mueser KT, Xie H, et al. Cognitive enhancement treatment for people with mental illness who do not respond to supported employment: a randomized controlled trial. Am J Psychiatry. 2015;172(9):852–861. PubMed CrossRef
77. Nuechterlein KH, Ventura J, Subotnik KL, et al. A randomized controlled trial of cognitive remediation and long-acting injectable risperidone after a first episode of schizophrenia: improving cognition and work/school functioning. Psychol Med. 2020;1–10. PubMed CrossRef
78. Bell MD, Lysaker PH. Clinical benefits of paid work activity in schizophrenia: 1-year followup. Schizophr Bull. 1997;23(2):317–328. PubMed CrossRef
79. Bryson G, Lysaker P, Bell M. Quality of life benefits of paid work activity in schizophrenia. Schizophr Bull. 2002;28(2):249–257. PubMed CrossRef
80. I keep getting asked “how are you so normal?” Schizophrenia.com. Published March 2, 2021. Accessed March 2, 2021. https://forum.schizophrenia.com/t/i-keep-getting-asked-how-are-you-so-normal/228839
81. Medic G, Higashi K, Littlewood KJ, et al. Dosing frequency and adherence in chronic psychiatric disease: systematic review and meta-analysis. Neuropsychiatr Dis Treat. 2013;9:119–131. PubMed CrossRef
82. Blackwood C, Sanga P, Nuamah I, et al. Patients’ preference for long-acting injectable versus oral antipsychotics in schizophrenia: results from the patient-reported medication preference questionnaire. Patient Prefer Adherence. 2020;14:1093–1102. PubMed CrossRef
To cite: Harvey PD, Kane JM. Addressing patients’ unmet needs to improve outcomes in schizophrenia. J Clin Psychiatry. 2021;82(3):IC20018AH3C
To share: https://doi.org/10.4088/JCP.IC20018AH3C
© Copyright 2021 Physicians Postgraduate Press, Inc.
aUniversity of Miami Miller School of Medicine, Florida
bZucker School of Medicine at Hofstra/Northwell, Hempstead, New York