See letter by Modesto-Lowe et al, and replies by Peccoralo et al and Sim and Chew
In the spring of 2020, New York City (NYC) was the epicenter of the coronavirus disease 2019 (COVID-19) pandemic in the United States. To date, NYC has experienced the highest number of COVID-19-related fatalities, with more than 19,000 confirmed deaths.1 The initial surge of the COVID-19 pandemic was especially stressful for frontline health care workers (FHCWs), who endured unprecedented levels of exposure to illness and death, worked in conditions placing themselves at considerable risk, and balanced the care of their families while fulfilling their professional duties.2
Although a growing number of studies have documented the adverse psychological consequences of the COVID-19 pandemic in FHCWs,2 no known study has examined the potential influence of factors associated with psychological resilience—defined as the process of adapting well in the face of adversity—in this population.
Given that acute stress may predict risk for chronic psychological difficulties,3 characterization of potential resilience-promoting factors during the acute phase of highly stressful events may help identify targets for prevention and early intervention efforts designed to promote the long-term mental health of FHCWs. We explored this question using data from more than 2,500 FHCWs during the spring 2020 acute pandemic surge in NYC.
Methods
Data were collected between April 14 and May 11, 2020, during the peak and initial decline of the acute patient surge. An anonymous, incentivized ($25 gift card) survey was emailed to a purposively selected sample of 6,026 FHCWs at Mount Sinai Hospital, an urban tertiary care hospital in NYC. The eligible study population included health care workers most likely to be directly involved in the care of patients infected with COVID-19, as a result of either their standard practice or anticipated redeployment within the study period. The research team worked with hospital and administrative leaders to identify those most likely to be involved in frontline care prior to procuring contact information for study invitation. Of those invited, 3,360 (55.8%) completed the survey, of whom 2,579 (76.8%) reported directly providing care for patients with COVID-19 and had complete data. Supplementary Table 1 describes sample characteristics. The Institutional Review Board at the Icahn School of Medicine at Mount Sinai approved the study.
A broad range of both occupational and personal COVID-19-related stressors (Supplementary Table 1) as well as resilience-promoting factors (Supplementary Table 2) were assessed.
Psychological resilience was operationalized as low psychological distress (ie, composite measure of COVID-19-related posttraumatic stress, major depressive, and generalized anxiety disorder symptoms assessed using validated self-report measures) in the presence of high exposure to COVID-19-related stressors (details provided in Supplementary Table 1). Multiple regression and relative importance analyses were conducted to identify independent variables associated with psychological resilience scores and the variance in these scores that was attributable to each of these variables.
Results
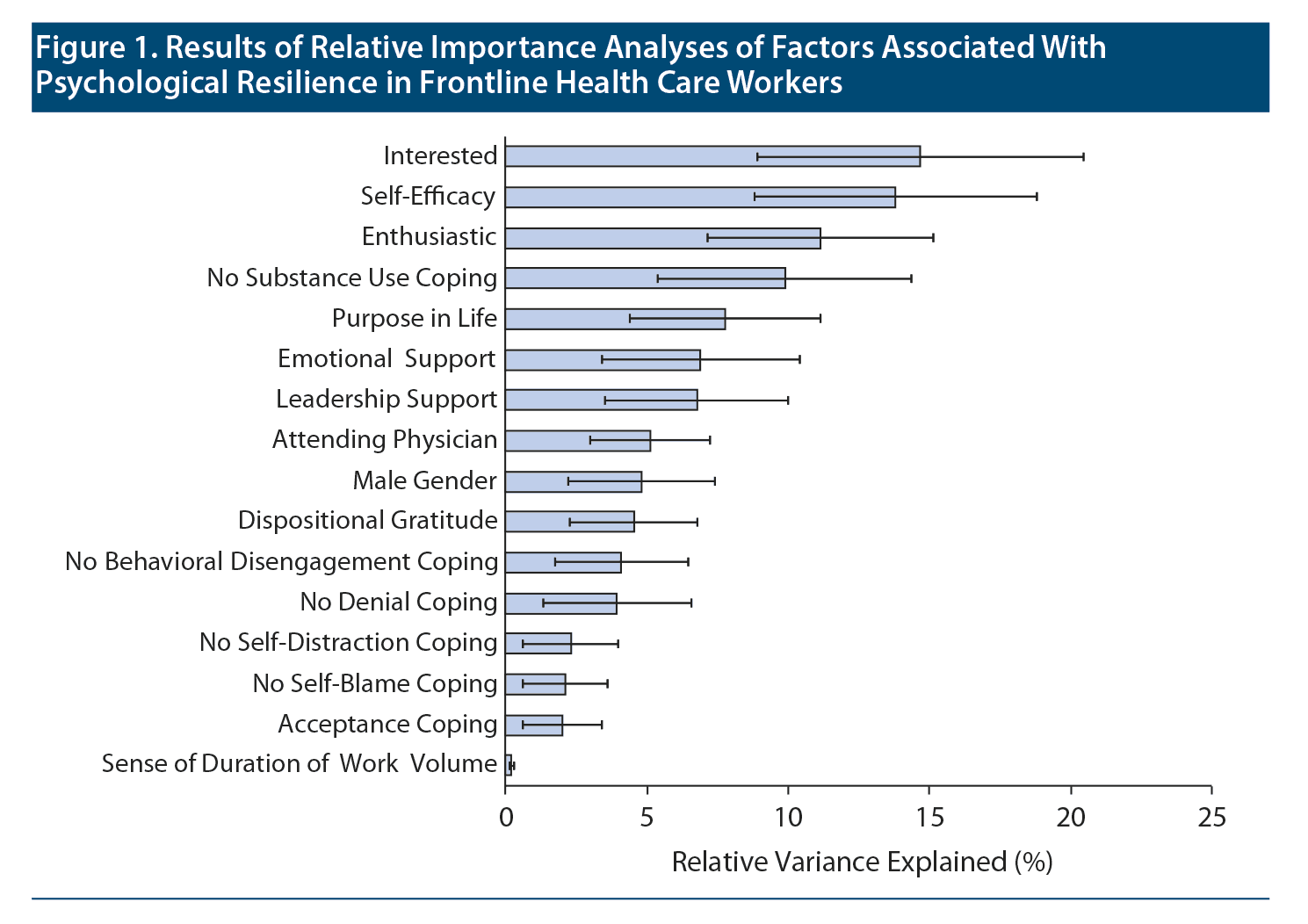
As shown in Figure 1, relative importance analyses revealed that positive emotions (interested [relative variance explained [RVE] = 14.7%], enthusiastic [RVE = 11.2%]), self-efficacy (RVE = 13.8%), nonengagement in substance use coping (RVE = 9.9%), higher purpose in life (RVE = 7.8%), and emotional support (RVE = 6.9%) and leadership support (RVE = 6.8%) were most strongly associated with psychological resilience, collectively explaining > 70% of the variance in these scores. Supplementary Table 3 shows results of analyses examining factors associated with psychological resilience.
Discussion
To our knowledge, this is the first study to examine factors associated with psychological resilience in FHCWs during the acute phase of the COVID-19 pandemic.
Multiple factors—including positive emotions, self-efficacy, purpose in life, and social support, as well as nonengagement in maladaptive coping strategies (eg, substance use)—emerged as strong correlates of resilience. These findings, which are consistent with prior research in other populations of trauma survivors, suggest that emotional, behavioral, and socio-contextual factors may contribute to resilience in FHCWs during the acute phase of the COVID-19 pandemic.
Collectively, these results underscore the importance of assessing how individual-level interventions to bolster positive emotions and self-efficacy,4,5 as well as broader organizational strategies aimed at enhancing social support, work-related meaning and purpose, and engagement,6 may help bolster psychological resilience in FHCWs. Further research is needed to examine longitudinal trajectories of psychological distress and related issues such as substance misuse in FHCWs, biopsychosocial mechanisms underlying resilience, and the efficacy of prevention and early intervention strategies to enhance and sustain resilience in this population.
Published online: December 29, 2020.
Author contributions: Dr Pietrzak had full access to all of the data in the study and takes responsibility for the integrity of the data and accuracy of the data analysis. Concept and design: All authors. Acquisition, analysis, or interpretation of data: All authors. Drafting of the manuscript: Pietrzak, Feder, Southwick, Ripp. Critical revision of the manuscript for important intellectual content: All authors. Statistical analysis: Pietrzak. Administrative, technical, or material support: Feingold, Ripp, Peccoralo, Charney Supervision: Southwick, Ripp.
Potential conflicts of interest: Dr Feder is named co-inventor on an issued patent in the US, and several issued patents outside the US, filed by the Icahn School of Medicine at Mount Sinai (ISMMS) for the use of ketamine as a therapy for PTSD. This intellectual property has not been licensed. Dr Charney is named as co-inventor on patents filed by the Icahn School of Medicine at Mount Sinai (ISMMS) relating to the treatment for treatment-resistant depression, suicidal ideation, and other disorders. ISMMS has entered into a licensing agreement with Janssen Pharmaceuticals, Inc. and it has and will receive payments from Janssen under the license agreement related to these patents for the treatment of treatment- resistant depression and suicidal ideation. Consistent with the ISMMS Faculty Handbook (the medical school policy), Dr Charney is entitled to a portion of the payments received by the ISMMS. Since SPRAVATO has received regulatory approval for treatment-resistant depression, ISMMS and thus, through the ISMMS, Dr Charney, will be entitled to additional payments, beyond those already received, under the license agreement. Dr Charney is a named co-inventor on several patents filed by ISMMS for a cognitive training intervention to treat depression and related psychiatric disorders. The ISMMS has entered into a licensing agreement with Click Therapeutics, Inc. and has and will receive payments related to the use of this cognitive training intervention for the treatment of psychiatric disorders. In accordance with the ISMMS Faculty Handbook, Dr Charney has received a portion of these payments and is entitled to a portion of any additional payments that the medical school might receive from this license with Click Therapeutics. Dr Charney is a named co-inventor on a patent application filed by the ISMMS for the use of intranasally administered neuropeptide Y (NPY) for the treatment of mood and anxiety disorders. This intellectual property has not been licensed. Dr Charney is a named co-inventor on a patent application in the US and several issued patents outside the US filed by the ISMMS related to the use of ketamine for the treatment of posttraumatic stress disorder. This intellectual property has not been licensed. The other authors have no disclosures to report.
Funding/support: This study was supported by internal funding devoted to COVID-19-related projects from the Icahn School of Medicine at Mount Sinai. Preparation of this report was supported in part by the US Department of Veterans Affairs National Center for Posttraumatic Stress Disorder (Dr Pietrzak).
Role of the sponsor: The funders had no role in the design and conduct of the study; collection, management, analysis, and interpretation of the data; preparation, review, or approval of the manuscript; and decision to submit the manuscript for publication.
Acknowledgments: The authors thank all of the participants at the Mount Sinai Hospital who participated in this study. They also acknowledge the COVID-19 Psychological Impact Study Team for their contributions to this project: Chi C. Chan, PhD; Carly A. Kaplan, BS; Halley Kaye-Kauderer, BA; Jaclyn Verity, MPH; Larissa Burka, RN; Alicia Hurtado, MD; and James W. Murrough, MD, PhD.
Supplementary material: See accompanying pages.
REFERENCES
1. City of New York, Department of Health. Main data page: cases, hospitalizations, and deaths. Accessed October 19, 2020. https://www1.nyc.gov/site/doh/covid/covid-19-data.page
2. Sheraton M, Deo N, Dutt T, et al. Psychological effects of the COVID 19 pandemic on healthcare workers globally: a systematic review. Psychiatry Res. 2020;292:113360. PubMed CrossRef
3. Bryant RA. The current evidence for acute stress disorder. Curr Psychiatry Rep. 2018;20(12):111. PubMed CrossRef
4. Joyce S, Shand F, Tighe J, et al. Road to resilience: a systematic review and meta-analysis of resilience training programmes and interventions. BMJ Open. 2018;8(6):e017858. PubMed CrossRef
5. Maunder RG, Lancee WJ, Mae R, et al. Computer-assisted resilience training to prepare healthcare workers for pandemic influenza: a randomized trial of the optimal dose of training. BMC Health Serv Res. 2010;10(1):72. PubMed CrossRef
6. West CP, Dyrbye LN, Erwin PJ, et al. Interventions to prevent and reduce physician burnout: a systematic review and meta-analysis. Lancet. 2016;388(10057):2272-2281. PubMed CrossRef
aUS Department of Veterans Affairs National Center for Posttraumatic Stress Disorder, VA Connecticut Healthcare System, West Haven, Connecticut
bDepartment of Psychiatry, Yale School of Medicine, New Haven, Connecticut
cDepartment of Medical Education, Icahn School of Medicine at Mount Sinai, New York, New York
dDepartment of Psychiatry, Icahn School of Medicine at Mount Sinai, New York, New York
eOffice of Well-Being and Resilience, Icahn School of Medicine at Mount Sinai, New York, New York
*Corresponding author: Robert H. Pietrzak, PhD, MPH, US Department of Veterans Affairs National Center for Posttraumatic Stress Disorder, VA Connecticut Healthcare System, 950 Campbell Ave 151E, West Haven, CT 06516 ([email protected]).
J Clin Psychiatry 2021;82(1):20l13749
To cite: Pietrzak RH, Feingold JH, Feder A, et al. Psychological resilience in frontline health care workers during the acute phase of the COVID-19 pandemic in New York City. J Clin Psychiatry. 2021;82(1):20l13749.
To share: https://doi.org/10.4088/JCP.20l13749
© Copyright 2020 Physicians Postgraduate Press, Inc.
This PDF is free for all visitors!