Cultural Background and Barriers to Mental Health Care for African American Adults

CME Background
Articles are selected for credit designation based on an assessment of the educational needs of CME participants, with the purpose of providing readers with a curriculum of CME articles on a variety of topics throughout each volume. Activities are planned using a process that links identified needs with desired results.
To obtain credit, read the article, correctly answer the Posttest question and complete the Evaluation.
CME Objective
After studying this article, you should be able to:
‘ ¢ Assess patient and provider cultural biases toward ADHD symptoms and treatment
Accreditation Statement
The CME Institute of Physicians Postgraduate Press, Inc., is accredited by the Accreditation Council for Continuing Medical Education to provide continuing medical education for physicians.
Credit Designation
The CME Institute of Physicians Postgraduate Press, Inc., designates this journal-based CME activity for a maximum of 0.5 AMA PRA Category 1 Creditâ„¢. Physicians should claim only the credit commensurate with the extent of their participation in the activity.
Note: The American Academy of Physician Assistants (AAPA) accepts certificates of participation for educational activities certified for AMA PRA Category 1 Creditâ„¢ from organizations accredited by ACCME or a recognized state medical society. Physician assistants may receive a maximum of 0.5 hour of Category I credit for completing this program.
Date of Original Release/Review
This educational activity is eligible for AMA PRA Category 1 Creditâ„¢ through March 31, 2017. The latest review of this material was January 2015.
Financial Disclosure
All individuals in a position to influence the content of this activity were asked to complete a statement regarding all relevant personal financial relationships between themselves or their spouse/partner and any commercial interest. The CME Institute has resolved any conflicts of interest that were identified. In the past year, Alan J. Gelenberg, MD, Editor in Chief, has been a consultant for Zynx Health and Bloom Burton, has received grant/research support from Pfizer, and has been a stock shareholder of Healthcare Technology Systems. No member of the CME Institute staff reported any relevant personal financial relationships. Faculty financial disclosure appears with the article.
J Clin Psychiatry 2015;76(3):279-283 (doi:10.4088/JCP.13008co5c)
© Copyright 2015 Physicians Postgraduate Press, Inc.
This Commentary section of The Journal of Clinical Psychiatry presents the highlights of the planning teleconference series “Challenges in the Recognition and Management of ADHD in African American Adults in the United States,” which was held in April and May 2014. This report was prepared and independently developed by the CME Institute of Physicians Postgraduate Press, Inc., and was supported by an educational grant from Shire.
The teleconference was chaired by Anthony L. Rostain, MD, Department of Psychiatry and Pediatrics and the Adult Developmental Disorders Section, University of Pennsylvania Perelman School of Medicine, Philadelphia. The faculty were J. Russell Ramsay, PhD, Department of Psychiatry and the Adult ADHD Treatment and Research Program, University of Pennsylvania Perelman School of Medicine, Philadelphia; and Roberta Waite, EdD, PMHCNS-BC, FAAN, Department of Nursing, Assistant Dean of Academic Integration and Evaluation of Community Programs, Drexel University College of Nursing and Health Professions, Philadelphia, Pennsylvania.
Financial disclosure: Dr Rostain is a consultant for Biobehavioral Diagnostics, Pearson, Alcobra, and Shire; has received grant/research support from AHRQ and SUNY Upstate; is a member of the speakers/advisory board for Biobehavioral Diagnostics and Pearson; and has received royalties from Routledge/Taylor & Francis. Dr Ramsay is a consultant for Shire; has received honoraria from the Pennsylvania Psychological Association; and has received royalties from Routledge/Taylor & Francis and the American Psychological Association. Dr Waite has no personal affiliations or financial relationship with any commercial interest to disclose relative to the activity.
The opinions expressed herein are those of the faculty and do not necessarily reflect the opinions of the CME provider and publisher or the commercial supporter.
Historical, economic, and cultural issues all contribute to barriers to African Americans’ mental health care in the United States. African Americans compose about 12% of the US population, with over 50% living in the South.1 Significant health disparities exist between the white majority and African Americans (a culturally diverse group including immigrants from Africa, the Caribbean, Central America, and other areas).2
Health disparities encompass differences in domains of health, such as illness incidence, access to care, and outcomes of care.1 Mental health conditions, such as depression and attention-deficit/hyperactivity disorder (ADHD), can impede patients’ social and occupational functioning if they remain undiagnosed and untreated.3
Clinicians must learn the historical background of African Americans and psychiatry in the United States, recognize barriers to care, and incorporate strategies to overcome barriers that hinder African Americans from receiving mental health care services.
HISTORY OF PSYCHIATRY AND AFRICAN AMERICANS
Exploring the historical experiences that contribute to mistrust and underutilization of mental health care services among African Americans is key if effective change is to occur. One reason that some African Americans mistrust the mental health care system is a troubling history of racism rooted in medical research and diagnosis.4
Before the Civil War, pseudoscience was instrumental in initiating racial myths to defend slavery in the United States by describing African Americans as intellectually weak and innately submissive.4 Because of the belief that slavery was a natural condition for African Americans, the desire to escape it was pathologized. A slave-specific disorder, drapetomania, was invented to describe behaviors by slaves such as running away to seek freedom, destroying property on a plantation, being disobedient, talking back, fighting with their masters, or refusing to work. After the Civil War, unethical experimentation on African Americans continued to take place, such as in the Tuskegee syphilis study, as well as sterilization without consent.4
While these are only a few of the factors associated with a fear of medicine in general among some African Americans, acknowledging this history can help clinicians understand why some African Americans believe that the diagnosis and treatment of the behaviors characteristic of ADHD are an attempt at social control.5 African Americans may also fear misdiagnosis, labeling, or being misunderstood due to inadequate knowledge about African American culture among mental health providers.
BARRIERS TO MENTAL HEALTH CARE
Many barriers affect health care utilization among African Americans. Factors such as income, health insurance, and attitudes may hinder patients from seeking or obtaining care, while other barriers stem from access problems or bias among health care providers.
Patient Factors
Low income. The median income of African American households is less than two-thirds that of non-Hispanic white households, with 27% of African Americans living below the poverty level compared with about 10% of non-Hispanic white people.6 The rate of poverty for rural African American households is triple the rate for rural non-Hispanic white households (40.6% and 13.5%, respectively).7 In 2012, the unemployment rate for African Americans was 14% compared with 7% in the white population.8
These disparities in income and employment are due to a variety of factors, such as family composition and educational attainment. Family composition influences poverty levels because families with 2 adults will most likely have more sources of income than single-adult families.7 Because income and employment are linked to educational attainment, high school and college graduation rates can affect the earning potential of African Americans. The high school graduation rate for African American students in 2011 and 2012 was 69%, which was much lower than the 88% rate for Asian and Pacific Islander students, 86% for non-Hispanic white students, and 73% for Hispanic students.9
Lack of health insurance. Lack of health insurance also plays a large role in the inadequate health care of African Americans.2 The rate of uninsured African Americans in 2012 was 19% compared with 11% of non-Hispanic white people.6 These percentages reveal startling disparities for African Americans, which affect their mental health care utilization. For example, only 6% of African American children had used mental health care services compared with 14% of white children, according to parents’ reports in a study of 5,147 US fifth graders.10 This study also showed that fewer African American and Hispanic children with recent symptoms of ADHD, oppositional defiant disorder, or conduct disorder had used mental health care services compared with white children.10
While income and insurance are 2 major factors contributing to mental health care utilization, other barriers, such as negative attitudes toward mental health disorders or treatments, may also exist.
Attitudes. Some African Americans may be concerned about the medicalization of social problems, believing that the problem of hyperactive children results from insufficient school resources and from culturally insensitive teachers. Others lack an understanding about the nature of mental health disorders and about the benefits of evidence-based treatment. A sizable percentage of African Americans fear that stimulant medications can lead to misuse, abuse, and addiction. Some believe that behavior problems related to ADHD are due to negative personality traits.3 African Americans may mistrust health care providers or have concerns about provider competence with their racial group, especially if they have experienced mistreatment by a mental health professional.11

- The history of psychiatry may contribute to African Americans’ feelings of mistrust and fear regarding mental health care.
- Patient-related barriers to care include low income, lack of health insurance coverage, and negative attitudes, while health care system barriers include limited numbers of specialists and culturally competent providers.
- Clinicians can address barriers to care by providing education to patients and communities, promoting policies to improve insurance and access to services for minority patients, and focusing on prevention and early intervention.
Mental illness is associated with considerable stigma among African Americans, which contributes to avoidance of diagnosis and treatment. Social stigma associated with seeking professional help is a significant barrier to treatment, and African Americans may rely mainly on family or friends when they have a problem.12
Fear of treatment or of hospitalization can also keep African Americans from visiting a mental health provider.13 African Americans tend to have a strong sense of pride, self-reliance, and family privacy, which are resilient qualities but which may also discourage people from seeking help. For example, “toughing it out” is advocated in African American culture during difficult times.12
Health Care System Factors
African Americans often receive poorer quality care and lack access to culturally competent care.2 Several problems in the health care system could be improved to reach more African Americans with mental health disorders and increase the quality of their care.
Limited access. The number and location of mental health care providers greatly influence the availability of treatment for African Americans.13 Generally, a shortage of mental health care providers exists,14 and fewer mental health care providers are located in rural areas.13 Additionally, few mental health providers are African American—fewer than 5% of psychologists, psychiatrists, and social workers.13 In addition, as in any specialty, mental health providers can lack cultural competence.
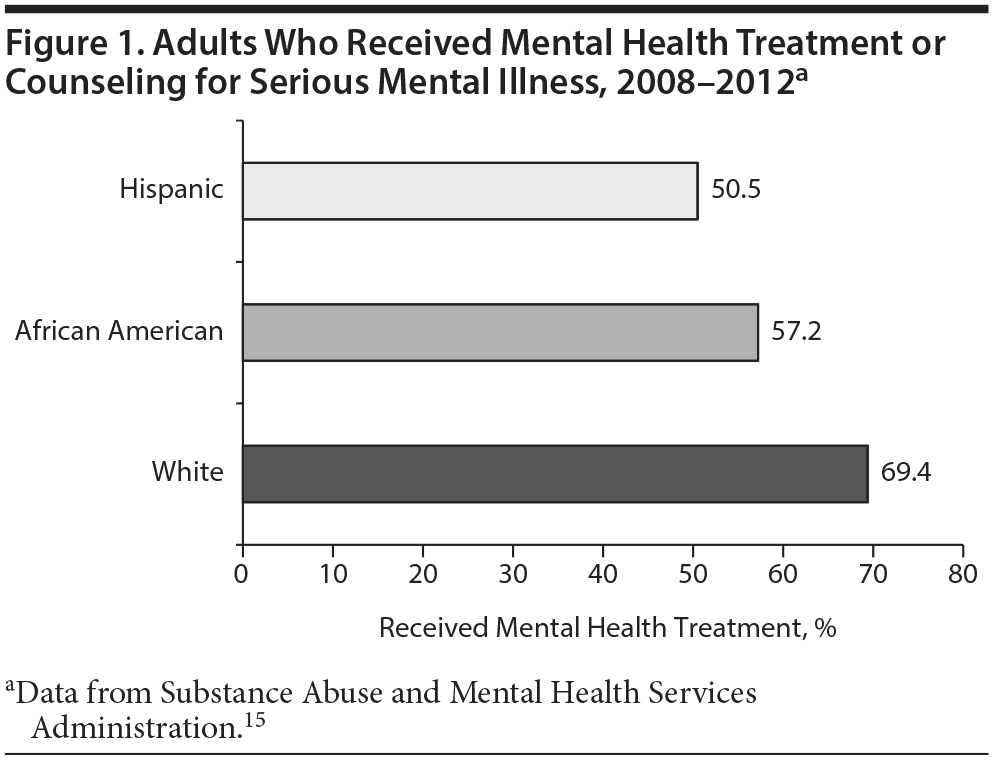
From 2008 to 2012, the rate of adults who received treatment for serious mental illnesses was 57% for African Americans but almost 70% for white adults (Figure 1).15 Regarding access to depression treatment, 41% of African Americans received any treatment versus 60% of white patients, and rates of adequate treatment were 12% for African Americans versus 33% for white patients.11 This difference is significant because it speaks to disparities that exist in the actual delivery of care to those seeking help. Although the prevalence of ADHD among African American children is similar to that among white children (9.5% and 10.6% in 2009, respectively),16 white children are nearly twice as likely to receive ADHD medications.17 These rates indicate a need for improved access to care and more effective treatment and follow-up in African American patients. Additionally, African Americans are more likely to seek health care from hospital emergency departments rather than outpatient offices that can provide better preventive treatment and follow-up.13
Specific subpopulations within the African American community are at higher risk for mental illness, including people who are homeless, incarcerated, or supported by welfare. These subpopulations often have limited access to mental health care due to their poor socioeconomic status.13 Furthermore, if care is available, African American patients with poor socioeconomic status may be unable to manage the logistics of getting to and following through on a comprehensive evaluation and follow-up treatment. Ideal treatment for many individuals may be a combination of psychosocial and pharmacologic treatment,18 which means coordinating several appointments with different providers.
Providers’ biases. Different biases may influence how a health care provider views different disorders, such as schizophrenia or ADHD, in African American patients. One such bias is a belief that ADHD symptoms are the fault of the individual or of his or her environment. Physicians may believe that behavior that results from underlying ADHD is instead the result of individual shortcomings, particularly in adults, because it is associated with violation of social norms (eg, interrupting others, being reckless).19 A tendency also exists to overestimate environmental factors (such as poor parenting or poor education) that may contribute to the manifestation of ADHD behaviors and to underestimate actual illness.19 For example, a health care professional may think, “The school district is bad, so that is why I’ m seeing these problems in this patient.” While environment should be a consideration in making the diagnosis, it can also be part of a bias that might lead to underdiagnosis.
ADHD symptoms in some patients may also be viewed as a behavioral issue, not a clinical issue, requiring only nonclinical support such as seeking help from a pastor or school counselor. Getting help from those resources can be beneficial in adults with ADHD, and is possibly even indicated, but it may not be all that is required. Additionally, the symptoms may be viewed as stemming from another behavioral or clinical issue requiring nonspecialty support or counseling. The patient may be advised to see a therapist, but if the ADHD diagnosis is lacking, specialty care may not be sought.
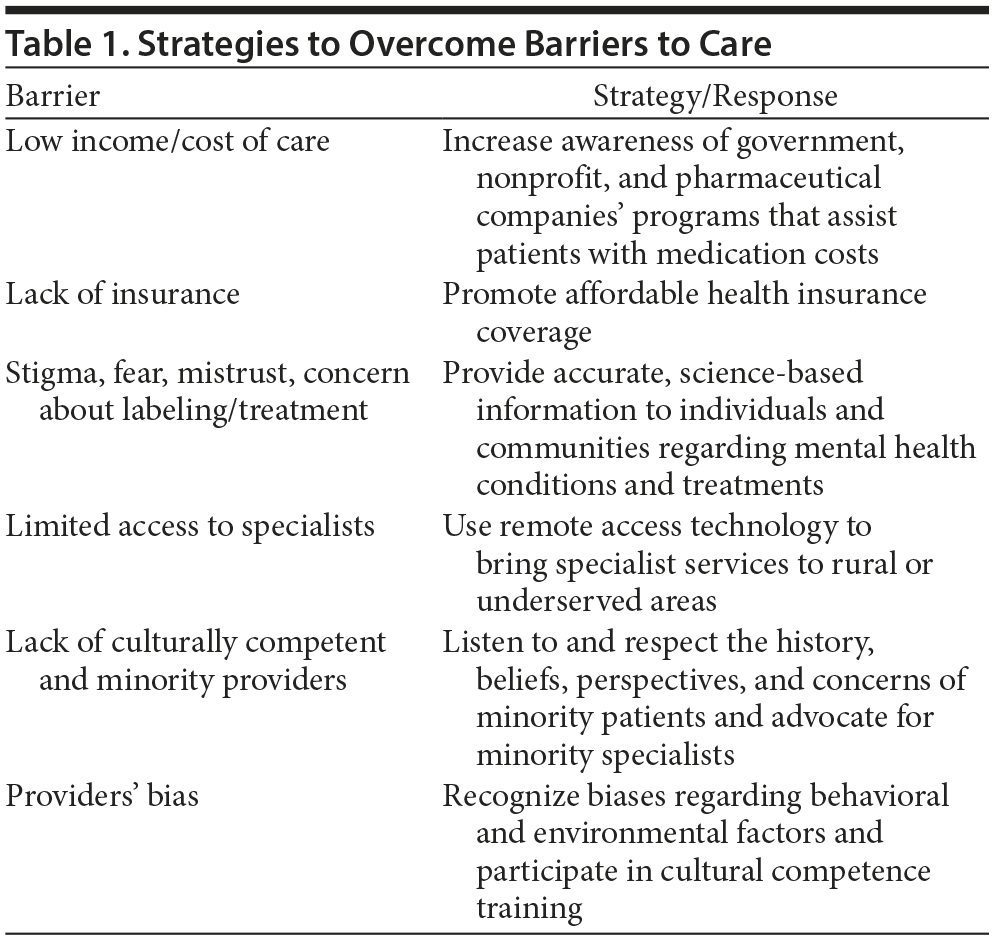
STRATEGIES TO ADDRESS BARRIERS TO CARE
The first step toward improving mental health care among African Americans is to conduct stigma awareness training in every facet of society, including religious leaders, health care providers, schools, and community groups and organizations (Table 1).2 Everyone needs to understand how stigma surrounds mental illness and how it creates barriers to care. It is also important to talk openly about mental disorders, substance abuse, and the burdens these impose on individuals, families, and society so misconceptions can be addressed and corrected. Individuals living with a mental disorder in minority communities need the support of family and friends to help them overcome the isolation that social stigma imposes. In addition, clinicians can provide accurate, science-based information to family and friends of African American patients to help dispel the most common myths regarding mental illness.3
Second, clinicians need education on the disparities in health care between African Americans and other groups so they can advocate policies that promote care equity.2 For example, clinicians can support and advance policies that increase diversity in the mental health care workforce.20 Having more minority providers could improve access to care and build trust between African American patients and providers.20 Policies that ensure access to comprehensive, affordable health coverage (such as the Affordable Care Act) should help reduce the number of uninsured people. Clinicians also need to be aware of the link between mental health disorders and chronic disease because patients with both face more challenges staying healthy and adhering to treatment.2 Clinicians can also benefit from cultural competence training to better understand the circumstances and symptom reports of African American patients.20
Third, clinicians should help increase community awareness of mental health services to improve utilization and follow-up, including among high-risk populations such as those who are homeless, incarcerated, and unemployed.2 Access to specialists may be improved with increased availability of remote access to expert case consultation services.
Finally, a focus on prevention and early intervention will help patients deal with mental health conditions before they become chronic problems.2 While no single solution can reduce the barriers to care, clinicians can help by improving access to quality health care; by providing education to African American patients, families, and communities; and by incorporating culturally competent strategies for managing patients of different races.
CONCLUSION
The history of psychiatry and African Americans plays a role in some current barriers to care, such as attitudes of mistrust and fear of treatment. Additionally, income or insurance problems may be hindering patients from obtaining mental health care. Health care providers must be alert for signs of mental health disorders, such as depression and ADHD, in their adult patients and refer patients to specialists, if indicated and available. Providers must guard against biases that could affect their diagnosis or attitudes toward African American patients. Finally, clinicians should educate patients and communities on mental health disorders and services, advocate policies to improve insurance coverage and access to specialists, and take time to understand the unique beliefs, perspectives, and concerns of African American patients.
Disclosure of off-label usage: Dr Rostain has determined that, to the best of his knowledge, no investigational information about pharmaceutical agents that is outside US Food and Drug Administration-approved labeling has been presented in this activity.
References
1. Trujillo M. Multicultural aspects of mental health. Prim Psychiatry. 2008;15(4).
2. American Psychiatric Association. APA Fact Sheet: Mental Health Disparities: African Americans. http://www.psychiatry.org/File%20Library/Practice/Diversity/Diversity%20Resources/Fact-Sheet—African-American.pdf. Published 2014. Accessed October 16, 2014.
3. National Alliance on Mental Illness. ADHD and adults: a look at cultural differences. http://www.nami.org/Template.cfm?Section=ADHD&Template=/ContentManagement/ContentDisplay.cfm&ContentID=106391. Accessed October 16, 2014.
4. Suite DH, La Bril R, Primm A, et al. Beyond misdiagnosis, misunderstanding and mistrust: relevance of the historical perspective in the medical and mental health treatment of people of color. J Natl Med Assoc. 2007;99(8):879-885. PubMed
5. Olaniyan O, dosReis S, Garriett V, et al. Community perspectives of childhood behavioral problems and ADHD among African American parents. Ambul Pediatr. 2007;7(3):226-231. PubMed doi:10.1016/j.ambp.2007.02.002
6. DeNavas-Walt C, Proctor BD, Smith JC. Income, Poverty, and Health Insurance Coverage in the United States: 2012. Washington, DC: US Government Printing Office; 2013. http://www.census.gov/prod/2013pubs/p60-245.pdf.
7. US Department of Agriculture. Rural Poverty and Well-being: Poverty Demographics. www.ers.usda.gov/topics/rural-economy-population/rural-poverty-well-being/poverty-demographics.aspx. Updated September 30, 2013. Accessed October 16, 2014.
8. US Bureau of Labor Statistics. Labor Force Characteristics by Race and Ethnicity, 2012. Washington, DC: US Dept of Labor; October 2013. Report 1044. http://www.bls.gov/cps/cpsrace2012.pdf.
9. Stetser MC, Stillwell R. Public High School Four-Year On-Time Graduation Rates and Event Dropout Rates: School Years 2010-11 and 2011-12. Washington, DC: US Dept of Education; April 2014. NCES 2014-391. http://www.nces.ed.gov/pubs2014/2014391.pdf.
10. Coker TR, Elliott MN, Kataoka S, et al. Racial/ethnic disparities in the mental health care utilization of fifth grade children. Acad Pediatr. 2009;9(2):89-96. PubMed doi:10.1016/j.acap.2008.11.007
11. Alegr×a M, Chatterji P, Wells K, et al. Disparity in depression treatment among racial and ethnic minority populations in the United States. Psychiatr Serv. 2008;59(11):1264-1272. PubMed doi:10.1176/ps.2008.59.11.1264
12. Vogel DL, Wester SR, Larson LM. Avoidance of counseling: psychological factors that inhibit seeking help. J Couns Dev. 2007;85(4):410-422. doi:10.1002/j.1556-6678.2007.tb00609.x
13. US Department of Health and Human Services. Mental health care for African Americans. In: Mental Health: Culture, Race, and Ethnicity: a Supplement to Mental Health: a Report of the Surgeon General. Rockville, MD: US Dept of Health and Human Services, Substance Abuse and Mental Health Services Administration, Center for Mental Health Services; 2001.
14. Kaiser Family Foundation. Mental Health Care Health Professional Shortage Areas (HPSAs). http://kff.org/other/state-indicator/mental-health-care-health-professional-shortage-areas-hpsas/. Updated April 28, 2014. Accessed October 16, 2014.
15. Substance Abuse and Mental Health Services Administration. Behavioral Health Barometer: United States, 2013. Rockville, MD: Substance Abuse and Mental Health Services Administration, 2013. http://www.samhsa.gov/data/sites/default/files/National_BHBarometer/
National_BHBarometer.pdf.
16. Akinbami LJ, Liu X, Pastor PN, et al. Attention deficit hyperactivity disorder among children aged 5-17 years in the United States, 1998-2009. NCHS Data Brief. 2011;70:1-8. PubMed
17. Jonas BS, Gu Q, Albertorio-Diaz JR. Psychotropic medication use among adolescents: United States, 2005-2010. NCHS Data Brief. 2013;135:1-8. PubMed
18. Rostain AL, Ramsay JR. A combined treatment approach for adults with ADHD: results of an open study of 43 patients. J Atten Disord. 2006;10(2):150-159. PubMed doi:10.1177/1087054706288110
19. Mueller AK, Fuermaier AB, Koerts J, et al. Stigma in attention deficit hyperactivity disorder. Atten Defic Hyperact Disord. 2012;4(3):101-114. PubMed doi:10.1007/s12402-012-0085-3
20. McGuire TG, Miranda J. New evidence regarding racial and ethnic disparities in mental health: policy implications. Health Aff (Millwood). 2008;27(2):393-403. PubMed doi:10.1377/hlthaff.27.2.393