Because this piece does not have an abstract, we have provided for your benefit the first 3 sentences of the full text.
To the Editor: We recently demonstrated differences in objective recordings of motor activity between inpatients with unipolar depression with and without motor retardation. Findings of lower mean levels and increased intraindividual variability in activity in the motor-retarded group and more disorganized activity in the non-motor-retarded group suggest that variations in activity may be used to distinguish phenotypically different depressive subgroups.
Analytic methods of actigraphy data, which to date have focused mainly on mean levels and parametric variability measures, need to be enhanced to advance research in this area of major clinical interest.
This work may not be copied, distributed, displayed, published, reproduced, transmitted, modified, posted, sold, licensed, or used for commercial purposes. By downloading this file, you are agreeing to the publisher’s Terms & Conditions.
Distribution and Characteristics of Active and Inactive Periods Distinguish Unipolar Depression With and Without Motor Retardation
To the Editor: We recently demonstrated differences in objective recordings of motor activity between inpatients with unipolar depression with and without motor retardation.1 Findings of lower mean levels and increased intraindividual variability in activity in the motor-retarded group and more disorganized activity in the non-motor-retarded group suggest that variations in activity may be used to distinguish phenotypically different depressive subgroups.
Analytic methods of actigraphy data, which to date have focused mainly on mean levels and parametric variability measures, need to be enhanced to advance research in this area of major clinical interest. We sought to find complementary ways of describing variability in activity and of distinguishing motor retardation from non-motor retardation. According to Barabási,2 timing of human behavioral events can be characterized by bursts of activity followed by inactive periods. The features and distribution of active and inactive periods characterize activity behavior in patients with depression and with schizophrenia and differ from those of healthy controls.3-5 These results add to previous findings using analyses of variability and complexity.1,6-9 The aim of the present study was to reanalyze previously published1 actigraphy data using these new advanced methods to quantify the regulation of motor behavior and distinguish the groups with and without motor retardation.
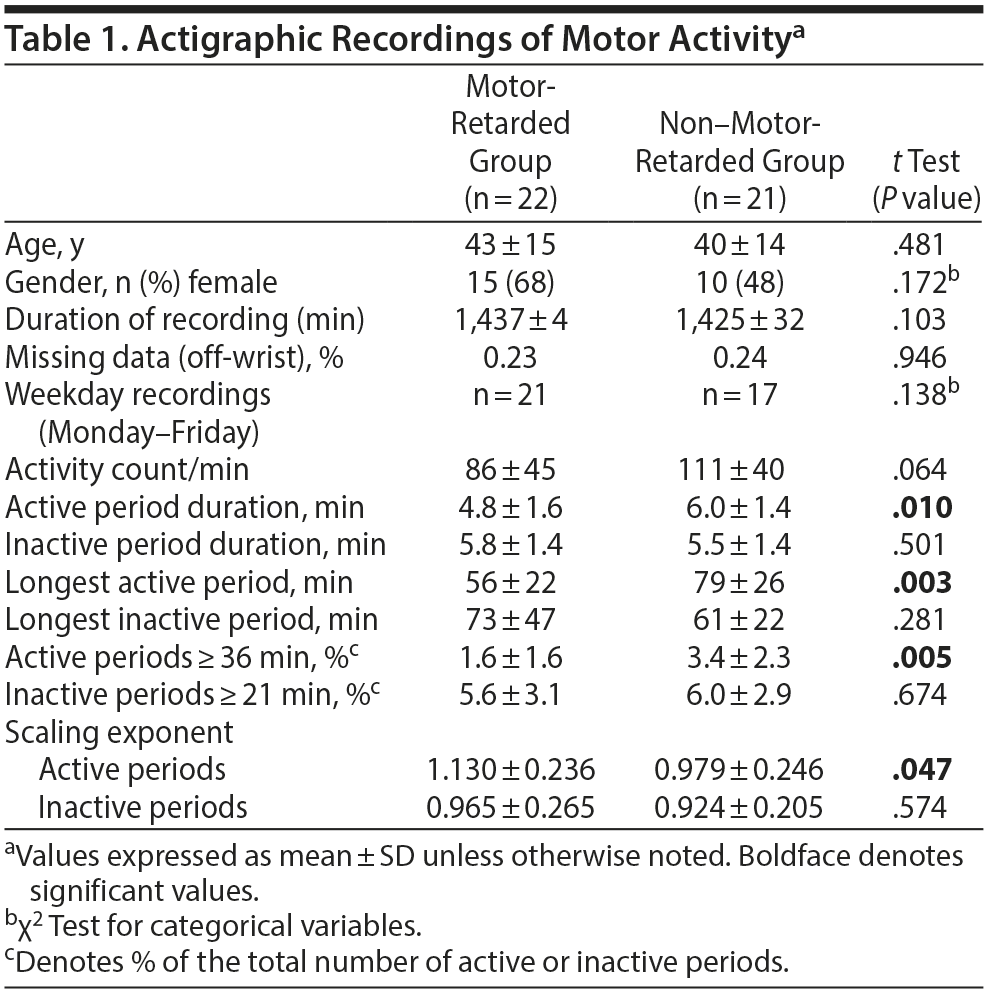
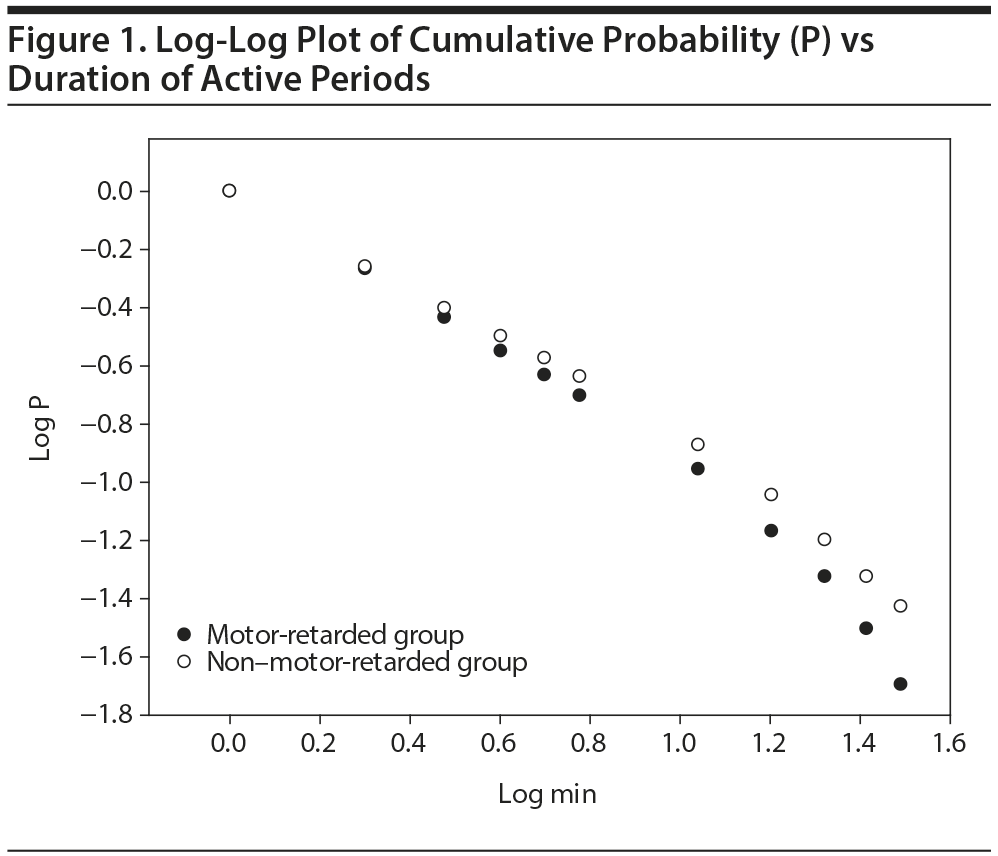
Methods. Consecutively, acutely admitted inpatients with unipolar depression (ICD-10 F32 and F33) with adequate recordings from the previous sample were separated into 2 groups on the basis of a clinical assessment of motor activity level: 22 with motor retardation and 21 without motor retardation. More detailed information about subjects and equipment is provided elsewhere.1 We analyzed 24-hour actigraphy recordings using the following methods: each minute was defined as active or inactive, according to whether the activity count was above or below 10% of the mean for the whole 24-hour period. An active or inactive period was then defined as a continuous sequence of active or inactive intervals with a length (A) of 1 minute or longer, and the cumulative probability (P) that an active or inactive period had a length of ≥ A minutes was determined. In accordance with a previous study,5 we plotted P versus A on a log-log graph using lengths from 1 to 35 minutes for active periods and 1 to 20 minutes for inactive periods, and we calculated the slope of the line (scaling exponent, absolute value) that best fitted the data, using the least squares method. For each patient, we also calculated the mean duration of active and inactive periods, the longest active and inactive periods, the number of active periods with a length of ≥ 36 minutes, and the number of inactive periods with a length of ≥ 21 minutes. Independent-samples t tests for continuous variables and χ2 tests for categorical variables were used to compare groups.
Results. Patients with unipolar depression with and without motor retardation differ in characterization and distribution of active periods (Table 1). Patients with motor retardation demonstrated significantly shorter mean active period durations, and their longest active sequence was shorter compared to non-motor-retarded patients. Furthermore, the percentage of active sequences with duration of more than 36 minutes was significantly lower for the motor-retarded patients and the scaling exponent for the active periods higher (Figure 1). None of the variables pertaining to inactive periods differentiated the groups.
These findings indicate that motor retardation implies being active in shorter bursts with fewer long bursts compared to non-motor retardation. Studying active and inactive periods constitutes a complementary way of differentiating depressive subgroups and has additional value in analysis of motor activity patterns in psychiatric disorders. This study also shows that it is feasible to characterize group differences with 24-hour observational periods, compared to 5-12 days in previous studies.
References
1. Krane-Gartiser K, Henriksen TE, Vaaler AE, et al. Actigraphically assessed activity in unipolar depression: a comparison of inpatients with and without motor retardation. J Clin Psychiatry. 2015;76(9):1181-1187. PubMed doi:10.4088/JCP.14m09106
2. Barabási AL. The origin of bursts and heavy tails in human dynamics. Nature. 2005;435(7039):207-211. PubMed doi:10.1038/nature03459
3. Nakamura T, Kiyono K, Yoshiuchi K, et al. Universal scaling law in human behavioral organization. Phys Rev Lett. 2007;99(13):138103. PubMed doi:10.1103/PhysRevLett.99.138103
4. Sano W, Nakamura T, Yoshiuchi K, et al. Enhanced persistency of resting and active periods of locomotor activity in schizophrenia. PLoS ONE. 2012;7(8):e43539. PubMed doi:10.1371/journal.pone.0043539
5. Fasmer OB, Hauge E, Berle JØ, et al. Distribution of active and resting periods in the motor activity of patients with depression and schizophrenia. Psychiatry Investig. 2016;13(1):112-120. PubMed doi:10.4306/pi.2016.13.1.112
6. Hauge ER, Berle JO, Oedegaard KJ, et al. Nonlinear analysis of motor activity shows differences between schizophrenia and depression: a study using Fourier analysis and sample entropy. PLoS ONE. 2011;6(1):e16291. PubMed doi:10.1371/journal.pone.0016291
7. Berle JO, Hauge ER, Oedegaard KJ, et al. Actigraphic registration of motor activity reveals a more structured behavioural pattern in schizophrenia than in major depression. BMC Res Notes. 2010;3(1):149. PubMed doi:10.1186/1756-0500-3-149
8. Johnsen E, Fasmer OB, van Wageningen H, et al. The influence of glutamatergic antagonism on motor variability, and comparison to findings in schizophrenia patients. Acta Neuropsychiatr. 2013;25(2):105-112. PubMed doi:10.1111/j.1601-5215.2012.00674.x
9. Krane-Gartiser K, Henriksen TEG, Morken G, et al. Actigraphic assessment of motor activity in acutely admitted inpatients with bipolar disorder. PLoS ONE. 2014;9(2):e89574. PubMed doi:10.1371/journal.pone.0089574
aDepartment of Neuroscience, Norwegian University of Science and Technology, and Department of Psychiatry, St Olav’s University Hospital, Trondheim, Norway
bDepartment of Clinical Medicine, Section for Psychiatry, Faculty of Medicine and Dentistry, University of Bergen, and Division of Psychiatry, Haukeland University Hospital, Bergen, Norway
Potential conflicts of interest: The authors declare no competing interests.
Funding/support: The study was financially supported by the Department of Neuroscience, Norwegian University of Science and Technology (NTNU), and St Olav’s University Hospital, Trondheim, Norway.
Role of the sponsor: The funding organizations had no role in the design or conduct of the study.
Acknowledgments: The authors are grateful to Kjetil Sørensen, Master in Mental Health, St Olav’s University Hospital, for managing the data collection and to Erlend Fasmer, BEng, for making programs to automatically extract the active and inactive sequences from the actigraphy recordings. These individuals have no relevant financial disclosures.
J Clin Psychiatry 2016;77(6):841-842
dx.doi.org/10.4088/JCP.15l10408
© Copyright 2016 Physicians Postgraduate Press, Inc.
This PDF is free for all visitors!