A growing body of literature suggests that ketamine, administered in subanesthetic doses, has early-onset antidepressant action in patients with severe and even treatment-refractory depression. Many case reports, open-label studies, and randomized controlled trials (RCTs) suggest that ketamine may have dramatic antisuicidal effects, as well. This article examines the benefits of ketamine in patients with suicidal ideation with particular focus on the findings of recent RCTs and meta-analyses. Important findings are that a single dose of ketamine is associated with antisuicidal benefits that emerge within an hour of administration and persist for up to a week. The benefits are seen in patients with mild as well as clinically significant suicidal ideation. The benefits are observed in midazolam- as well as saline-controlled trials. Effect sizes are medium to large. The improvement in suicidal ideation is only partly explained by improvement in depression severity. It is concluded that there is consistent evidence that a single dose of ketamine has dramatic antisuicidal action that emerges almost immediately after dosing and persists for at least a week. The short- and intermediate-term safety and efficacy of ketamine as a crisis intervention treatment for suicidal patients merit study. Areas that need research are outlined.


ABSTRACT
A growing body of literature suggests that ketamine, administered in subanesthetic doses, has early-onset antidepressant action in patients with severe and even treatment-refractory depression. Many case reports, open-label studies, and randomized controlled trials (RCTs) suggest that ketamine may have dramatic antisuicidal effects, as well. This article examines the benefits of ketamine in patients with suicidal ideation with particular focus on the findings of recent RCTs and meta-analyses. Important findings are that a single dose of ketamine is associated with antisuicidal benefits that emerge within an hour of administration and persist for up to a week. The benefits are seen in patients with mild as well as clinically significant suicidal ideation. The benefits are observed in midazolam- as well as saline-controlled trials. Effect sizes are medium to large. The improvement in suicidal ideation is only partly explained by improvement in depression severity. It is concluded that there is consistent evidence that a single dose of ketamine has dramatic antisuicidal action that emerges almost immediately after dosing and persists for at least a week. The short- and intermediate-term safety and efficacy of ketamine as a crisis intervention treatment for suicidal patients merit study. Areas that need research are outlined.
J Clin Psychiatry 2018;79(2):18f12242
To cite: Andrade C. Ketamine for depression, 6: effects on suicidal ideation and possible use as crisis intervention in patients at suicide risk. J Clin Psychiatry. 2018;79(2):18f12242.
To share: https://doi.org/10.4088/JCP.18f12242
© Copyright 2018 Physicians Postgraduate Press, Inc.
Previous articles in this column discussed the efficacy, adverse effects, and possible mechanism(s) of action of subanesthetic doses of ketamine in the treatment of depression1; the indications and contexts for the use of ketamine as an off-label antidepressant2; the antidepressant benefits and adverse effects of ketamine and its enantiomers3; issues related to dosing, rate of administration, route of administration, duration of treatment, and frequency of sessions when ketamine is used to treat depression4; and potential pharmacokinetic and pharmacodynamic interactions when ketamine is used as an off-label treatment for depression.5 The present article examines the effects of ketamine on suicidal ideation and its possible use as a pharmacologic crisis intervention in patients at suicide risk.
The first randomized, double-blind, placebo-controlled (crossover) trial of subanesthetic dosing with ketamine in patients with major depressive illness found that, among other results, ketamine reduced the severity of suicidal ideation.6 Subsequently, many case reports,7-12 uncontrolled and open-label trials, and randomized controlled trials (RCTs) confirmed this finding. Data from uncontrolled and controlled trials have been examined in meta-analyses.
Ketamine Reduces Suicidality Within 1-4 Hours in At-Risk Patients: Results of Meta-Analysis
In a systematic review and meta-analysis of uncontrolled and controlled (ketamine arms only) clinical trials of the immediate antisuicidal action of ketamine, Bartoli et al13 identified 5 studies (pooled N = 99) that assessed outcomes at or within 4 hours of a single dose of intravenous (IV) ketamine in inpatients or outpatients (3 studies) or emergency room patients (2 studies) with active suicidal ideation. Two studies administered ketamine as an IV bolus (0.2 mg/kg; pooled N = 63); the other 3 administered ketamine as an IV infusion (0.5 mg/kg; pooled N = 36).
In this meta-analysis,13 ketamine was associated with substantial pre- vs posttreatment decrease in suicidal ideation at the last posttreatment assessment point. The effect size was large (SMD = 0.92; 95% CI, 0.44-1.40) and heterogeneity was low. Large, statistically significant benefit was observed from as early as 40 minutes posttreatment.
Limitations of this meta-analysis13 were many: the authors included uncontrolled as well as controlled studies; the number of studies was small; the pooled sample size was small; only within-groups analysis was performed (these are sensitive to placebo effects and yield larger effect sizes than between-groups analysis); and one of the studies14 was recently retracted. Therefore, the findings of this meta-analysis are, at best, a pointer to the potential of ketamine to quickly reduce suicidal ideation.
Ketamine Reduces Suicidality in At-Risk Patients: 1 Day to 1 Week Results of Individual Patient Data Meta-Analysis
In a larger and more informative systematic review and meta-analysis, Wilkinson et al15 obtained individual patient data from single ketamine session, saline- or midazolam-controlled RCTs (k = 10) of patients with active suicidal ideation (pooled N = 167). One RCT recruited patients with posttraumatic stress disorder and another recruited patients with mixed diagnoses; the remainder included only patients with major depression. The patients with suicidal ideation who were included in the meta-analysis were more severely depressed than those who did not have suicidal ideation and who were excluded. Included patients did not differ significantly in ketamine (pooled N = 93) vs control (pooled N = 74) groups on sociodemographic and important clinical parameters such as baseline severity of depression.
The findings of this meta-analysis15 are summarized in Table 1. In short, on almost all outcomes at almost all time points between posttreatment days 1 and 7, ketamine was superior to control intervention. However, the advantage for ketamine was smaller in midazolam-controlled trials relative to saline-controlled trials; effect sizes were 0.34 to 0.69 for the former vs 0.69 to 0.90 for the latter. This suggests that unmasking of the treatment blind may have boosted the placebo effect.
A limitation of this meta-analysis15 is that although there were 10 studies that contributed data, the pooled sample size was still small. The analyses examined single item scores in depression rating scales that assessed depression severity; there were no data based on specific suicide rating scales that assessed the frequency and severity of suicidal ideation, intent and planning, hopelessness, and other elements. No primary outcome was stated in the plan of analysis, and no correction for multiple hypothesis testing was applied. More importantly, patients in the RCTs were generally treatment-resistant and thereby enriched for a lesser likelihood of response to placebo; however, in clinical practice, patients who are acutely suicidal are not typically antidepressant-refractory and so may more readily respond to nonspecific aspects of whatever intervention is applied.16 Importantly, even patients with mild suicidal ideation were included in the analysis; worse still, many of the source studies specifically excluded patients at serious suicidal risk. In this context, what clinicians really want to know is the efficacy of ketamine as a crisis intervention in these very patients, that is, patients with the highest levels of suicidal ideation and intent. Many of these concerns were expressed in an editorial17 that discussed the meta-analysis.
Recent Randomized Controlled Trials of Ketamine in Patients With Clinically Significant Suicidal Ideation
At least 2 RCTs,18,19 not included in the meta-analyses discussed,13,15 have recently been published. Both RCTs recruited patients with clinically significant suicidal ideation, operationalized as a Scale for Suicidal Ideation (SSI) score of at least 4.
In the first RCT,18 16 patients with bipolar depression and clinically significant suicidal ideation were randomized to receive IV ketamine (0.5 mg/kg) or midazolam (0.02 mg/kg); ongoing psychotropics, barring benzodiazepines, were continued unchanged during the study. One day after treatment, SSI scores attenuated substantially and near-significantly more with ketamine than with midazolam. The lack of statistical significance was not disappointing because the study was a pilot investigation and was underpowered.
In perhaps the largest and most important RCT to date, Grunebaum et al19 randomized 80 inpatients with moderately severe major depressive disorder and clinically significant suicidal ideation (mean SSI score of approximately 15) to receive a single infusion of either ketamine (0.5 mg/kg) or midazolam (0.02 mg/kg); ongoing antidepressant medications, if any, were continued unchanged, but benzodiazepine use was barred. Nearly half of the patients had a prior history of suicide attempt.
Between 4 and 24 hours after intervention, the fall in SSI scores was 4-5 points greater with ketamine than with midazolam; the effect size at 24 hours was 0.75, which is medium to large. Reduction in mean SSI scores by > 50% was observed in 55% vs 30% of ketamine vs midazolam patients, respectively (number needed to treat = 4). Improvement in the Profile of Mood States depression subscale mediated only 34% of the effect on ketamine on the SSI score. The mean SSI score in the ketamine group, which fell to about 5 a day after the infusion, remained in the 5-6 point range during a 6-week follow-up period in which treatments were optimized to individual needs.
This study19 is important because of the large sample size, the use of midazolam as a biologically active control, and the assessment of suicidal ideation using the SSI. Another strength is that patients were not limited to those who were antidepressant-refractory; this makes the sample more representative of depressed and suicidal patients in clinical practice. The study is limited by the absence of the assessment of the effects of ketamine in a double-blind, controlled fashion beyond 1 day.
Other Relevant Studies
In a small pilot study conducted in a military emergency department setting, Burger et al20 randomized depressed and suicidal patients who met criteria for inpatient care to receive IV ketamine (0.2 mg/kg) or saline placebo. Two of 3 ketamine patients had dramatic reductions in suicidality and hopelessness within 40 minutes; no such improvements were observed in any of 7 saline controls. In a small, 3-week, open-label study,21 repeated ketamine administration (0.50-0.75 mg/kg, IV) was shown to attenuate mild but chronic suicidal ideation in 14 patients with major depressive disorder.
In a poorly described study,22 a single dose of ketamine (0.5 mg/kg IV) was associated with greater reduction in suicidal ideation than control treatment (midazolam) in patients (N = 42) with newly diagnosed cancer who were acutely depressed and suicidal. The benefits, however, were significant only at days 1 and 3 and not at day 7 posttreatment. This study provides preliminary support for the early antisuicidal action of ketamine in acutely depressed and suicidal patients who do not have major depression.
Comments
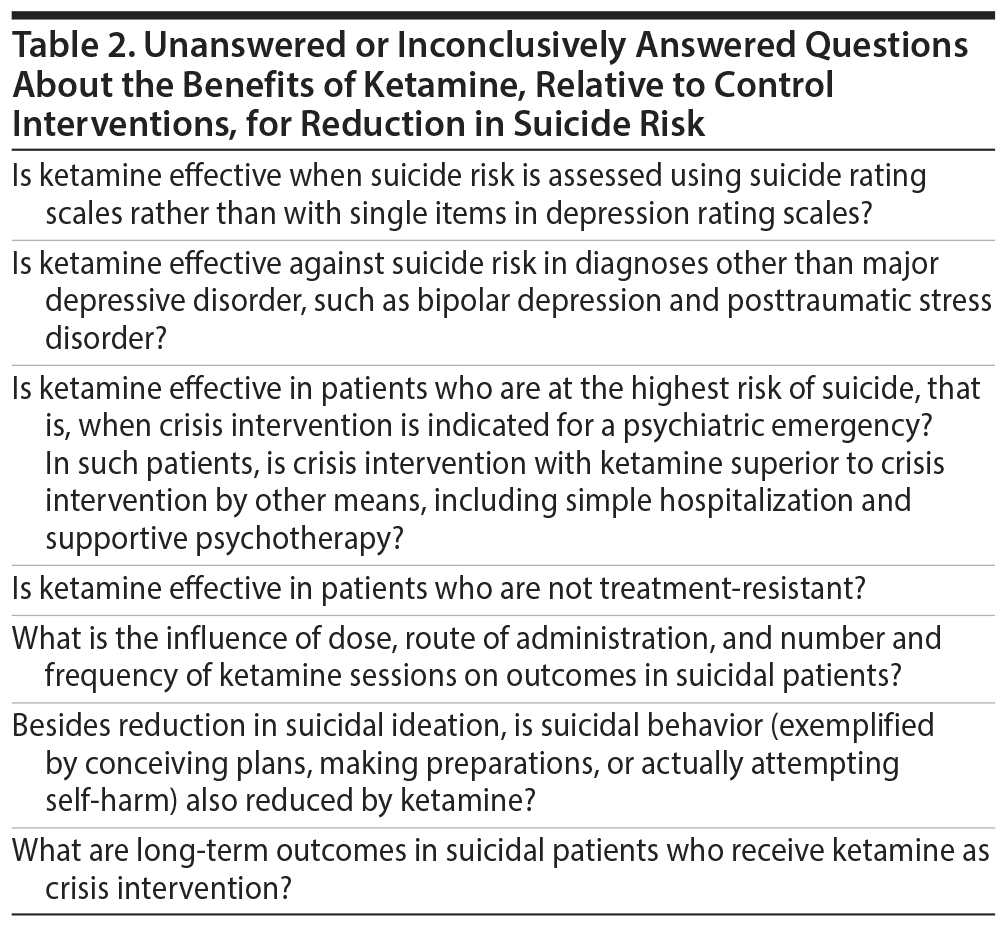
Patients who are suicidal are usually managed as inpatients because suicide completion is less likely in an inpatient setting than in the community; psychotherapy, pharmacotherapy, and/or electroconvulsive therapy (ECT) are then initiated, as appropriate. However, none of these interventions is associated with dramatic antidepressant and antisuicidal benefits, as appears possible with ketamine. Therefore, if unanswered questions (Table 2) can be resolved in favor of ketamine, subanesthetic dosing with ketamine may become an important crisis intervention strategy to buy time while other treatments are instituted and take effect.23
As discussed in earlier articles in this series,1,2,4 respiratory risks with ketamine are low, even in anesthetic doses, and the drug is relatively safe, even in untrained hands, such as when used in military medical emergencies. An important possibility, then, is that ketamine may be a potential pharmacologic crisis intervention for the suicidal patient even in low-resource, primary care settings in developing countries, where facilities for psychiatric admission, psychotherapy, and ECT are unavailable. In this context, there is need to explore whether oral or subcutaneous ketamine is also effective with appropriate dose adjustments to compensate for poor bioavailability and other pharmacokinetics matters.4 Given that elaborate monitoring facilities are unlikely to be available in low-resource settings, the risk-benefit profile of ketamine in such settings requires study, and minimum standards of care require to be set. There are already reports in the literature of the safe and effective domiciliary self-administration of sublingual ketamine, as required, in patients with suicidal ideation.11
Subanesthetic dosing with ketamine has the potential to enter emergency medicine and mainstream psychiatry as a crisis intervention treatment for suicidal patients.23
Published online: March 27, 2018.
 Each month in his online column, Dr Andrade considers theoretical and practical ideas in clinical psychopharmacology with a view to update the knowledge and skills of medical practitioners who treat patients with psychiatric conditions.
Each month in his online column, Dr Andrade considers theoretical and practical ideas in clinical psychopharmacology with a view to update the knowledge and skills of medical practitioners who treat patients with psychiatric conditions.
Department of Clinical Psychopharmacology and Neurotoxicology, National Institute of Mental Health and Neurosciences, Bangalore, India ([email protected]).
Financial disclosure and more about Dr Andrade.
REFERENCES
1. Andrade C. Ketamine for depression, 1: clinical summary of issues related to efficacy, adverse effects, and mechanism of action. J Clin Psychiatry. 2017;78(4):e415-e419. PubMed CrossRef
2. Andrade C. Ketamine for depression, 2: diagnostic and contextual indications. J Clin Psychiatry. 2017;78(5):e555-e558. PubMed CrossRef
3. Andrade C. Ketamine for depression, 3: does chirality matter? J Clin Psychiatry. 2017;78(6):e674-e677. PubMed CrossRef
4. Andrade C. Ketamine for depression, 4: in what dose, at what rate, by what route, for how long, and at what frequency? J Clin Psychiatry. 2017;78(7):e852-e857. PubMed CrossRef
5. Andrade C. Ketamine for depression, 5: potential pharmacokinetic and pharmacodynamic drug interactions. J Clin Psychiatry. 2017;78(7):e858-e861. PubMed CrossRef
6. Berman RM, Cappiello A, Anand A, et al. Antidepressant effects of ketamine in depressed patients. Biol Psychiatry. 2000;47(4):351-354. PubMed CrossRef
7. Sampath H, Sharma I, Dutta S. Treatment of suicidal depression with ketamine in rapid cycling bipolar disorder. Asia-Pac Psychiatry. 2016;8(1):98-101. PubMed CrossRef
8. Gurnani T, Khurshid KA. Role of ketamine in severe depression with suicidal ideation: insights from a case study. Asian J Psychiatr. 2017;29:112-113. PubMed CrossRef
9. Bigman D, Kunaparaju S, Bobrin B. Use of ketamine for acute suicidal ideation in a patient with chronic pain on prescribed cannabinoids. BMJ Case Rep. 2017;bcr-2017-222059. PubMed CrossRef
10. López-D×az A, Fernandez-Gonzalez JL, Lujan-Jiminez JE, et al. Use of repeated intravenous ketamine therapy in treatment-resistant bipolar depression with suicidal behaviour: a case report from Spain. Ther Adv Psychopharmacol. 2017;7(4):137-140. PubMed CrossRef
11. Grande LA. Sublingual ketamine for rapid relief of suicidal ideation. Prim Care Companion CNS Disord. 2017;19(2):16l02012. PubMed CrossRef
12. Vulser H, Vulser C, Rieutord M, et al. Ketamine use for suicidal ideation in the general hospital: case report and short review. J Psychiatr Pract. 2018;24(1):56-59. PubMed
13. Bartoli F, Riboldi I, Crocamo C, et al. Ketamine as a rapid-acting agent for suicidal ideation: a meta-analysis. Neurosci Biobehav Rev. 2017;77:232-236. PubMed CrossRef
14. Larkin GL, Beautrais AL. A preliminary naturalistic study of low-dose ketamine for depression and suicide ideation in the emergency department. Int J Neuropsychopharmacol. 2017;20(7):611. PubMed CrossRef
15. Wilkinson ST, Ballard ED, Bloch MH, et al. The effect of a single dose of intravenous ketamine on suicidal ideation: a systematic review and individual participant data meta-analysis. Am J Psychiatry. 2018;175(2):150-158. PubMed CrossRef
16. Andrade C. There’s more to placebo-related improvement than the placebo effect alone. J Clin Psychiatry. 2012;73(10):1322-1325. PubMed CrossRef
17. Trivedi MH. Antisuicidal effects of ketamine: a promising first step. Am J Psychiatry. 2018;175(2):97-98. PubMed CrossRef
18. Grunebaum MF, Ellis SP, Keilp JG, et al. Ketamine versus midazolam in bipolar depression with suicidal thoughts: a pilot midazolam-controlled randomized clinical trial. Bipolar Disord. 2017;19(3):176-183. PubMed CrossRef
19. Grunebaum MF, Galfalvy HC, Choo TH, et al. Ketamine for rapid reduction of suicidal thoughts in major depression: a midazolam-controlled randomized clinical trial [published online ahead of print December 5, 2017]. Am J Psychiatry. PubMed CrossRef
20. Burger J, Capobianco M, Lovern R, et al. A double-blinded, randomized, placebo-controlled sub-dissociative dose ketamine pilot study in the treatment of acute depression and suicidality in a military emergency department setting. Mil Med. 2016;181(10):1195-1199. PubMed CrossRef
21. Ionescu DF, Swee MB, Pavone KJ, et al. Rapid and sustained reductions in current suicidal ideation following repeated doses of intravenous ketamine: secondary analysis of an open-label study. J Clin Psychiatry. 2016;77(6):e719-e725. PubMed CrossRef
22. Fan W, Yang H, Sun Y, et al. Ketamine rapidly relieves acute suicidal ideation in cancer patients: a randomized controlled clinical trial. Oncotarget. 2017;8(2):2356-2360. PubMed CrossRef
23. Sathyanarayana Rao TS, Andrade C. A possible role for ketamine in suicide prevention in emergency and mainstream psychiatry. Indian J Psychiatry. 2017;59(3):259-261. PubMed CrossRef
This PDF is free for all visitors!