Because this piece does not have an abstract, we have provided for your benefit the first 3 sentences of the full text.
To the Editor: Ketamine’s ability to bring about rapid and dramatic improvement in patients with refractory depression has biotech companies and clinicians scrambling for ketamine alternatives. d-cycloserine (DCS) showed efficacy in depression as early as 1959 but lay dormant until recently.
As published in the June 2015 issue of the Journal, Kantrowitz and colleagues used ketamine priming followed by a high dose of DCS (1,000 mg/d) with impressive results (also refer to the study by Heresco-Levy et al).
See reply by Kantrowitz et al and letter by Kantrowitz et al
This work may not be copied, distributed, displayed, published, reproduced, transmitted, modified, posted, sold, licensed, or used for commercial purposes. By downloading this file, you are agreeing to the publisher’s Terms & Conditions.
Low-Dose d-Cycloserine for Depression?
To the Editor: Ketamine’s ability to bring about rapid and dramatic improvement in patients with refractory depression has biotech companies and clinicians scrambling for ketamine alternatives. d-cycloserine (DCS) showed efficacy in depression as early as 19591 but lay dormant until recently.
As published in the June 2015 issue of the Journal, Kantrowitz and colleagues used ketamine priming followed by a high dose of DCS (1,000 mg/d) with impressive results2 (also refer to the study by Heresco-Levy et al3).
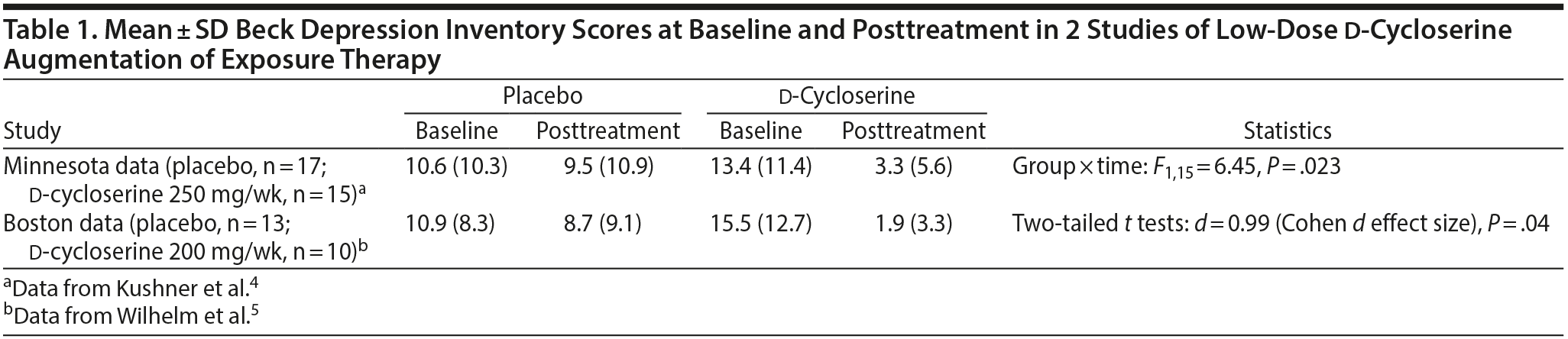
We4 and a group led by Wilhelm in Boston5 independently used a low-dose DCS (Table 1) strategy to facilitate cognitive-behavioral therapy-related memory consolidation. In a dose-finding study for negative symptoms in schizophrenia, Goff and coworkers6 reported an optimal DCS dose of 50 mg/d. This glycine (associated with N-methyl-d-aspartate [NMDA] receptor) agonism concept of DCS, akin to rapastinel (formerly GLYX-13; under clinical trial), deserves a closer look.
Although the primary goal of these studies4,5 was to enhance extinction learning in exposure treatment for OCD cases, both studies documented improvement in depressive symptoms (see Table 1). Although depressive symptoms were mild in both studies, lack of posttreatment group differences in OCD symptoms preclude a possibility that improved OCD symptoms contributed to the reduction in depression.
This report is not to claim an efficacy of DCS in depression but rather to suggest further studies on intermittent application of this old agent that works through NMDA mechanisms and would possibly help clinicians manage some of their depression cases.
References
1. Crane GE. Cyloserine as an antidepressant agent. Am J Psychiatry. 1959;115(11):1025-1026. PubMed doi:10.1176/ajp.115.11.1025
2. Kantrowitz JT, Halberstam B, Gangwisch J. Single-dose ketamine followed by daily d-cycloserine in treatment-resistant bipolar depression [letter]. J Clin Psychiatry. 2015;76(6):737-738. PubMed doi:10.4088/JCP.14l09527
3. Heresco-Levy U, Gelfin G, Bloch B, et al. A randomized add-on trial of high-dose d-cycloserine for treatment-resistant depression. Int J Neuropsychopharmacol. 2013;16(3):501-506. PubMed doi:10.1017/S1461145712000910
4. Kushner MG, Kim SW, Donahue C, et al. d-cycloserine augmented exposure therapy for obsessive-compulsive disorder. Biol Psychiatry. 2007;62(8):835-838. PubMed doi:10.1016/j.biopsych.2006.12.020
5. Wilhelm S, Buhlmann U, Tolin DF, et al. Augmentation of behavior therapy with d-cycloserine for obsessive-compulsive disorder. Am J Psychiatry. 2008;165(3):335-341, quiz 409. PubMed doi:10.1176/appi.ajp.2007.07050776
6. Goff DC, Tsai G, Manoach DS, et al. Dose-finding trial of d-cycloserine added to neuroleptics for negative symptoms in schizophrenia. Am J Psychiatry. 1995;152(8):1213-1215. PubMed doi:10.1176/ajp.152.8.1213
aDepartment of Psychiatry, University of Minnesota, Minneapolis
bYale University School of Medicine, VA Connecticut Healthcare System, West Haven, Connecticut
Potential conflicts of interest: None.
Funding/support: None.
J Clin Psychiatry 2016;77(8):e1007
dx.doi.org/10.4088/JCP.15lr10272
© Copyright 2016 Physicians Postgraduate Press, Inc.
This PDF is free for all visitors!