Objective: The first-onset affective episode requiring inpatient treatment in the postpartum period can be a marker of bipolar disorder, but it is unknown whether milder postpartum affective episodes are also indicators of underlying bipolarity. Therefore, we aimed to study whether women with a nonpsychotic postpartum affective episode treated with antidepressants have an increased risk of bipolar disorder.
Methods: A register-based cohort study was conducted in Denmark of 122,622 parous women without psychiatric history who received a first-time antidepressant prescription during 1997-2012. We compared women with a first-time antidepressant prescription, which was our indicator of a first-onset affective disorder, within 1 year postpartum to women with a first-time antidepressant prescription outside the postpartum period. Our outcome was psychiatric contact for bipolar disorder (ICD-10 criteria) during follow-up, and we estimated hazard ratios using Cox regressions.
Results: The risk of bipolar disorder among women with a postpartum affective episode was higher than that in women with an affective episode outside the postpartum period. The risk of bipolar disorder was 1.66 (95% CI, 1.12-2.48) for postpartum antidepressant monotherapy and 10.15 (95% CI, 7.13-14.46) for postpartum antidepressant therapy plus a subsequent prescription for anxiolytics when these therapies were compared to antidepressant monotherapy outside the postpartum period.
Conclusions: First-onset nonpsychotic postpartum affective disorder can be a marker of underlying bipolarity. Women who fill an antidepressant prescription following childbirth should be asked about hypomanic or manic symptoms and monitored long term. Clinically, when antidepressant monotherapy is ineffective or the individual woman experiences persistent and concerning symptoms, health professionals should consider a possible bipolar spectrum disorder.

Depression and Anxiety in the Postpartum Period and Risk of Bipolar Disorder:
A Danish Nationwide Register-Based Cohort Study
ABSTRACT
Objective: The first-onset affective episode requiring inpatient treatment in the postpartum period can be a marker of bipolar disorder, but it is unknown whether milder postpartum affective episodes are also indicators of underlying bipolarity. Therefore, we aimed to study whether women with a nonpsychotic postpartum affective episode treated with antidepressants have an increased risk of bipolar disorder.
Methods: A register-based cohort study was conducted in Denmark of 122,622 parous women without psychiatric history who received a first-time antidepressant prescription during 1997-2012. We compared women with a first-time antidepressant prescription, which was our indicator of a first-onset affective disorder, within 1 year postpartum to women with a first-time antidepressant prescription outside the postpartum period. Our outcome was psychiatric contact for bipolar disorder (ICD-10 criteria) during follow-up, and we estimated hazard ratios using Cox regressions.
Results: The risk of bipolar disorder among women with a postpartum affective episode was higher than that in women with an affective episode outside the postpartum period. The risk of bipolar disorder was 1.66 (95% CI, 1.12-2.48) for postpartum antidepressant monotherapy and 10.15 (95% CI, 7.13-14.46) for postpartum antidepressant therapy plus a subsequent prescription for anxiolytics when these therapies were compared to antidepressant monotherapy outside the postpartum period.
Conclusions: First-onset nonpsychotic postpartum affective disorder can be a marker of underlying bipolarity. Women who fill an antidepressant prescription following childbirth should be asked about hypomanic or manic symptoms and monitored long term. Clinically, when antidepressant monotherapy is ineffective or the individual woman experiences persistent and concerning symptoms, health professionals should consider a possible bipolar spectrum disorder.
J Clin Psychiatry 2017;78(5):e469-e476
https://doi.org/10.4088/JCP.16m10970
© Copyright 2017 Physicians Postgraduate Press, Inc.
aThe National Center for Register-based Research, Aarhus University, Aarhus, Denmark
bCIRRAU-Centre for Integrated Register-based Research, Aarhus University, Aarhus, Denmark
cLundbeck Foundation Initiative for Integrative Psychiatric Research, iPSYCH, Aarhus, Denmark
dDepartment of Clinical Epidemiology, Aarhus University Hospital, Aarhus, Denmark
eDepartment of Psychiatry, University of North Carolina at Chapel Hill School of Medicine, Chapel Hill
fThe Department of Psychiatry, Erasmus Medical Centre, Rotterdam, The Netherlands
‘ ¡Drs Bergink and Munk-Olsen are shared last authors.
*Corresponding author: Xiaoqin Liu, PhD, The National Center for Register-based Research, Aarhus University, Fuglesangs Allé 4, 8210 Aarhus V, Denmark ([email protected]).
Childbirth may trigger a severe psychiatric episode,1-3 often labeled as postpartum psychosis,4 which affects around 1/1,000 new mothers1 and usually requires acute psychiatric hospitalization. Consistent evidence3,5 has correlated postpartum psychosis with later conversion to bipolar disorder, and bipolar history in family members is an important risk factor for postpartum psychosis.6 Moreover, various psychiatric episodes treated at inpatient psychiatric facilities during the postpartum period have a higher conversion rate to bipolar disorder compared to psychiatric episodes not related to childbirth.7
Nonpsychotic affective disorders are among the most common morbidities during the postpartum period, with depressive disorders affecting around 5%-13% of new mothers and anxiety disorders, approximately 13%.8 Up to now, a single study9 has reported that 54% of women referred for postpartum depression were rediagnosed with bipolar disorder later in life. On the basis of this and empirical evidence from clinical observations, we hypothesized that childbirth can trigger a bipolar disease course, and nonpsychotic postpartum affective episodes may also be associated with later development of bipolar disorder similar to what has been documented in postpartum episodes requiring inpatient treatment.7
Most women with symptoms of anxiety, depression, or both who seek health care both during and outside the postpartum period are treated in primary care by general practitioners in Denmark.10 Frequently used treatment options are antidepressant medications (selective serotonin reuptake inhibitors [SSRIs], serotonin-norepinephrine reuptake inhibitors [SNRIs], and tricyclic antidepressants [TCAs]).11 Consequently, we conducted a population-based cohort study using information on the first-time prescription by general practitioners for an antidepressant following childbirth as the indicator of the first-onset affective status in the postpartum period and studied subsequent risk of bipolar disorder. The aim of the present study was to investigate whether women with a postpartum affective episode treated with antidepressants had an increased risk of bipolar disorder at later stages.
METHODS
Definition of Study Population
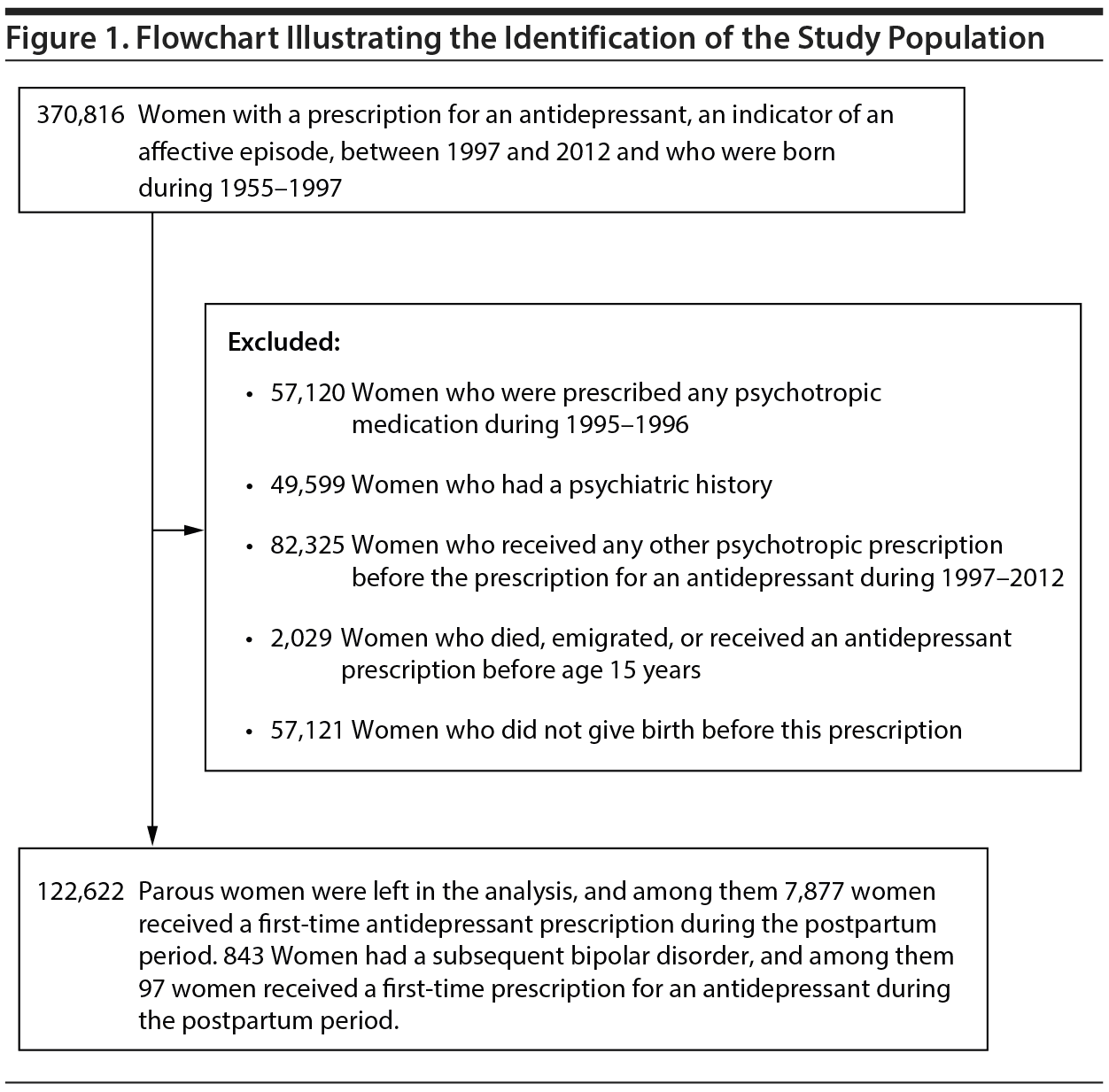
The population-based cohort study was based on data from Danish national registers. We first identified women with a prescription for an antidepressant between 1997 and 2012 and who were born during 1955-1997 from the Danish Civil Registration System (CRS) (N = 370,816).12 The CRS contains information on all live-born children and new residents in Denmark. It includes a unique 10-digit individual personal identification number that can be used for linkage within and between all national registers. Information on the prescription for an antidepressant was extracted from the Danish National Prescription Registry (DNPR).13 The Registry covers all dispensed prescriptions in Denmark since 1995, and information on prescriptions prior to 1995 is not available. To ensure that the dispensation of an antidepressant was an indicator of the first-onset affective episode, we excluded women who were dispensed any psychotropic medication during 1995-1996 (n = 57,120), which is known as a washout period in pharmacoepidemiology. Further, we excluded women who had a psychiatric history or received any other psychotropic prescription prior to the prescription for an antidepressant during 1997-2012 (n = 131,924). Psychiatric history was defined as any previous inpatient or outpatient visit for psychiatric disorders registered in the Danish Psychiatric Central Research Register,14 which contains information on the date of psychiatric contact along with all diagnoses. The register holds information on all treatments at psychiatric hospitals and psychiatric wards in general hospitals from 1969 onward and includes outpatient treatments since 1995. The International Classification of Diseases, Eighth Revision (ICD-8) was used until 1993 and Tenth Revision (ICD-10), from 1994 onward. The ICD-8 codes for psychiatric disorders were 290-351 and ICD-10 codes were F**. We also excluded women who died, emigrated, or received an antidepressant prescription before their 15th birthday (n = 2,029) and women who did not give birth before this prescription (n = 57,121). After applying these exclusion criteria, we included 122,622 parous women in the analysis, of whom 843 women had a psychiatric contact for bipolar disorder at later stages (Figure 1). Each woman was followed up from the day of a first-time prescription for an antidepressant during 1997-2012 until emigration, death, the first-time psychiatric contact for bipolar disorder, or the end of 2012, whichever came first.
Definition of Exposure Variables: First-Onset Postpartum Affective Episode
We used the first prescription ever redeemed for an antidepressant recorded in the DNPR as the indicator of the first-onset affective episode. We used date of the first-time prescription for an antidepressant and date of the first-onset affective episode interchangeably in this study. We use the term antidepressants throughout this article but acknowledge that SSRIs, SNRIs, and TCAs are used to treat a wide spectrum of affective symptomatology including depressive disorders and anxiety disorders as well as mixed symptomatology. We identified the first-time prescription for an antidepressant within 1 year after any delivery as our indicator of the first-onset affective episode during the postpartum period and took into account if antidepressants were administered as monotherapy or whether subsequent prescriptions for anxiolytics, mood stabilizers, or antipsychotics were added.

- Nonpsychotic affective disorders are the most common morbidities during the postpartum period. It is unknown whether mild to moderate postpartum affective episodes are indicators of underlying bipolarity.
- Postpartum affective episodes are associated with increased risks of bipolar disorder. Women who fill an antidepressant prescription following childbirth should be asked about current and previous symptoms of hypomania or mania and monitored long term.
Information on antidepressant monotherapy prescribed by a general practitioner and subsequent prescriptions for anxiolytics, mood stabilizers, or antipsychotics was obtained from the DNPR. Anatomic therapeutical chemical (ATC) classification codes were used for antidepressants (N06A), anxiolytics (benzodiazepine derivatives [N03AE01 and N05BA], buspirone [N05BE01], and zolpidem and zopiclone [N05CF]), mood stabilizers (N03AF01, N03AF02, N03AG01, N03AX09, N03AX11, N03AX12, N05AN01), and typical and atypical antipsychotics (N05A excluding N05AN01). See a detailed list of ATC codes and generic drug names in Supplementary eTable 1.
Definition of Outcome Variable: Bipolar Disorder
Our outcome was the first-time psychiatric contact for bipolar disorder (main diagnosis only) during the maximum 16-year follow-up after the first-time prescription for an antidepressant, and this information was extracted from the Danish Psychiatric Central Research Register. The ICD-10 codes for bipolar disorder were F30 and F31.
Statistical Analysis
All data were analyzed in Stata 13.1 (Statacorp, College Station, Texas) using Cox proportional hazards regression model. We estimated hazard ratios (HRs) of bipolar disorder in women with a first-onset affective episode during the postpartum period in comparison to women with a first-onset affective episode outside the postpartum period (reference group). We employed a running-line least-squares smoothing technique to smooth the Kaplan-Meier curves to illustrate the cumulative incidence rates of bipolar disorder.
To examine whether the risk of bipolar disorder depended on the timing of initial postpartum affective episode, we categorized the timing of the first-onset postpartum affective episode into 2 groups: within 0-180 days and 181-365 days after delivery. To determine whether the risk of bipolar disorder changed over time, we divided the elapsed time since the first-onset affective episode into 3 periods: 0-5 years, 6-10 years, and 11-16 years.
To explore the risk of bipolar disorder in different types of antidepressant treatment, we treated antidepressant treatment as a time-dependent variable. All women were in the antidepressant monotherapy group at the initial treatment. If a subsequent prescription for an anxiolytic, mood stabilizer, or antipsychotic prescription was dispensed prior to the diagnosis of bipolar disorder, women would then change treatment group and be included in the group receiving an anxiolytic or antipsychotic/mood stabilizer subsequent to antidepressant therapy, ie, antidepressant + subsequent anxiolytic therapy group or antidepressant + subsequent mood stabilizer or antipsychotic therapy group. Women were placed in these groups even if they later discontinued their antidepressant.
In the multivariate analyses, we adjusted for calendar year of birth (1955-1969, 1970-1984, or 1985-1997), age (< 25 years, 25-34 years, or ≥ 35 years), civil status (married; or single, divorced, or widowed), and parity (first or ≥ 2) at baseline (ie, time of the first-time prescription for an antidepressant).12,14,15 We adjusted for parental psychiatric history (bipolar disorder in either parent, other psychiatric disorder in either parent, or no psychiatric history) as a time-dependent variable.
To investigate whether observed associations were influenced by age difference in women with a first-onset postpartum affective episode and women with a first-onset affective episode outside the postpartum period, we analyzed the data by stratifying on age groups. Sensitivity analyses included further adjustments for education (elementary school, or above elementary school) and income (lowest quartile, second quartile, third quartile, or highest quartile) at baseline16 and excluded women who were pregnant again at the time of receiving the index antidepressant prescription. Further, we expanded our defined washout period to 5 years and included 109,108 parous women born during 1955-1997 who filled antidepressant prescriptions from 2000 to 2012 with no previous psychotropic prescription dispensed either before the index prescription or during 1995-1999.
Ethical Considerations
The study was approved by the Danish Data Protection Agency. No informed consent is needed for a register-based study with public health interest based on anonymized data according to the legislation in Denmark.
RESULTS
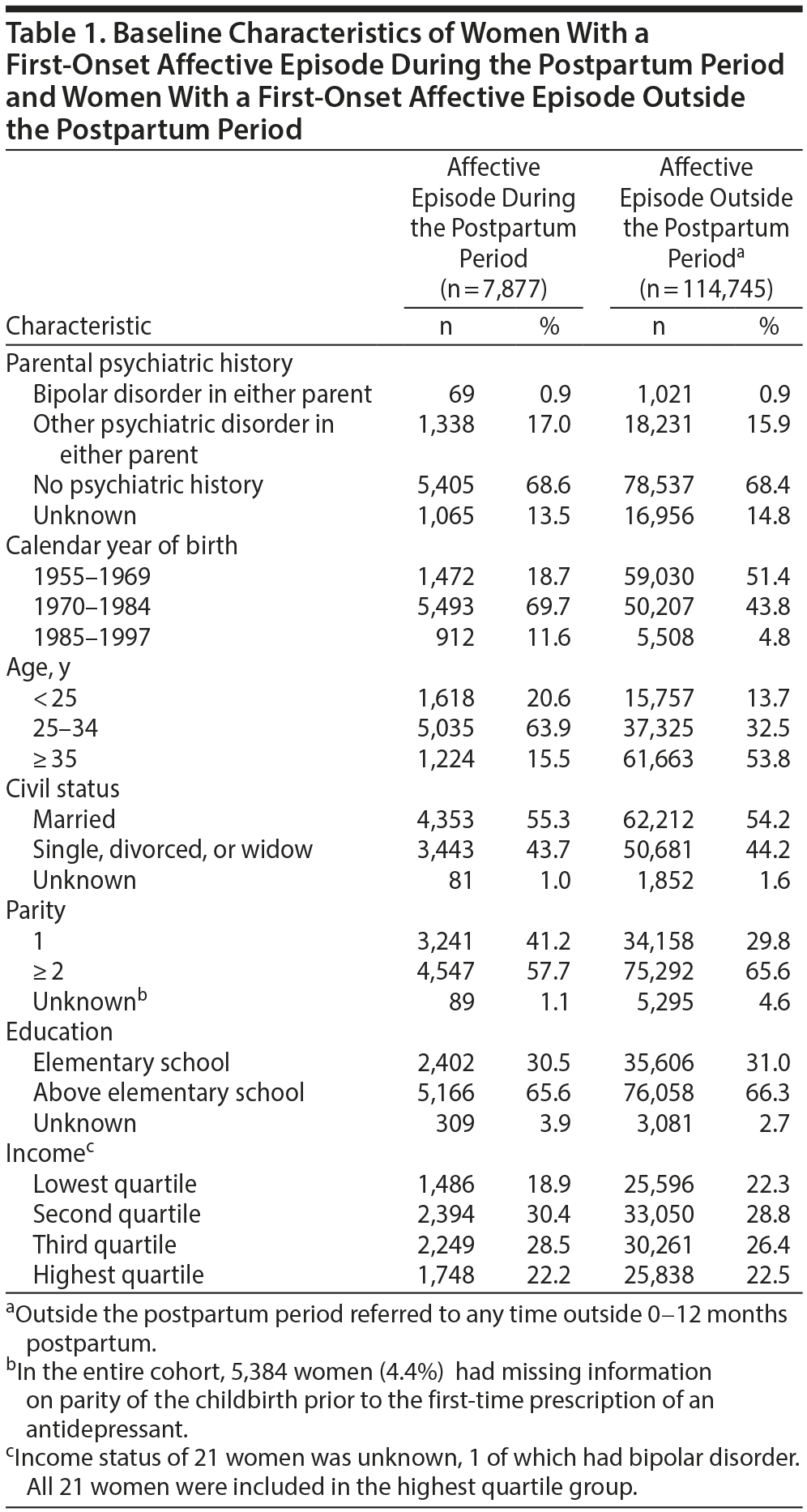
During our study period 1997-2012, a total of 122,622 parous women had a first-onset affective episode. The mean ± SD age at the time of the affective episode was 35.2 ± 8.7 years (range, 15.0-57.9). Altogether, 7,877 women had a first-onset affective episode during the postpartum period. Table 1 presents the baseline characteristics of the study population. Women with a first-onset postpartum affective episode differed from women with a first-onset affective episode outside the postpartum period regarding age distribution and parity, but both groups were comparable in terms of parental psychiatric history, civil status, education, and income.
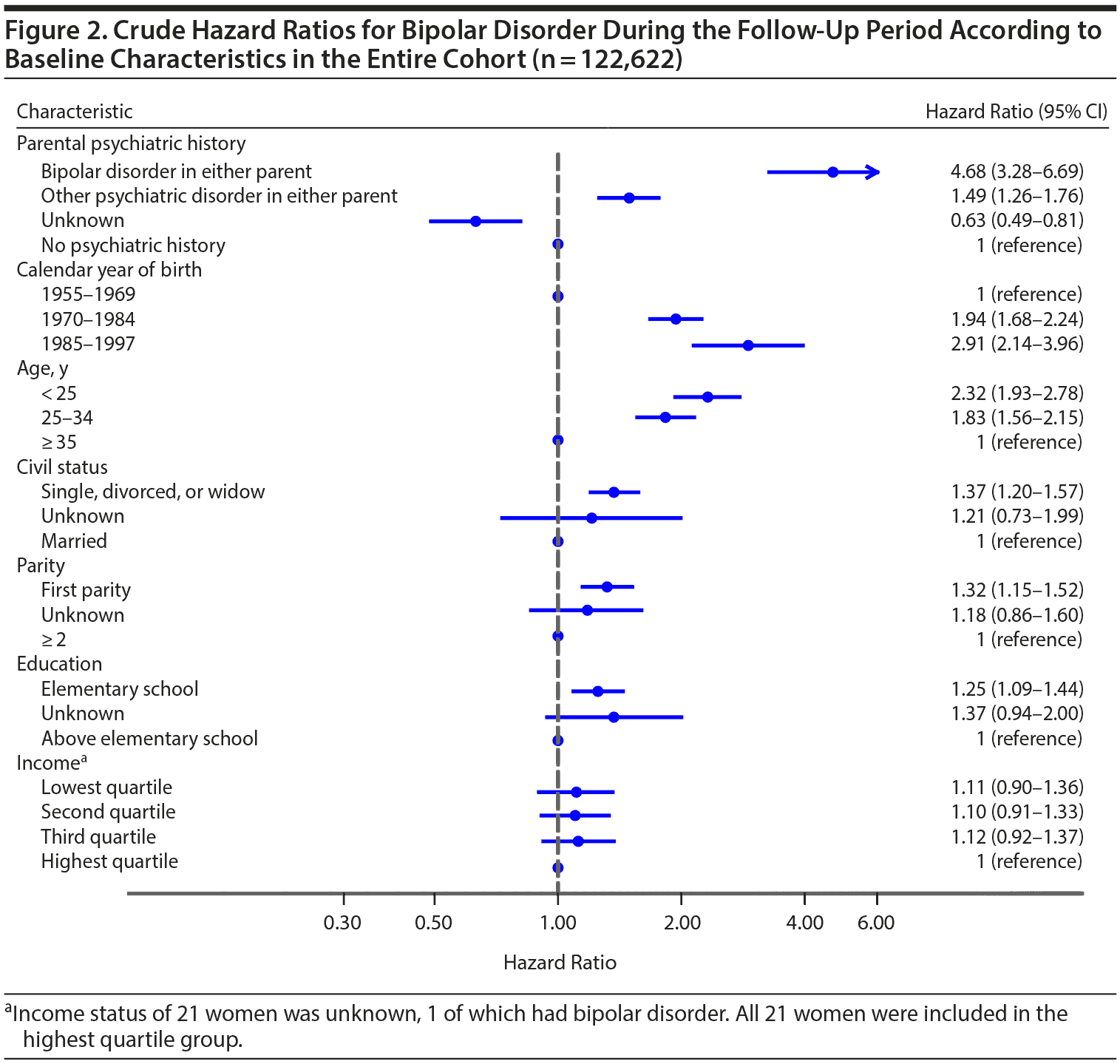
Figure 2 shows the possible risk factors for bipolar disorder in the entire cohort. Identified risk factors for bipolar disorder included records of parental psychiatric history, with HRs of 4.68 (95% CI, 3.28-6.69) for parental history of bipolar disorder and 1.49 (95% CI, 1.26-1.76) for parental history of other psychiatric disorder. Other risk factors included being younger, single, divorced or widowed, and nulliparous and having lower education level at the time of the first-onset affective episode.
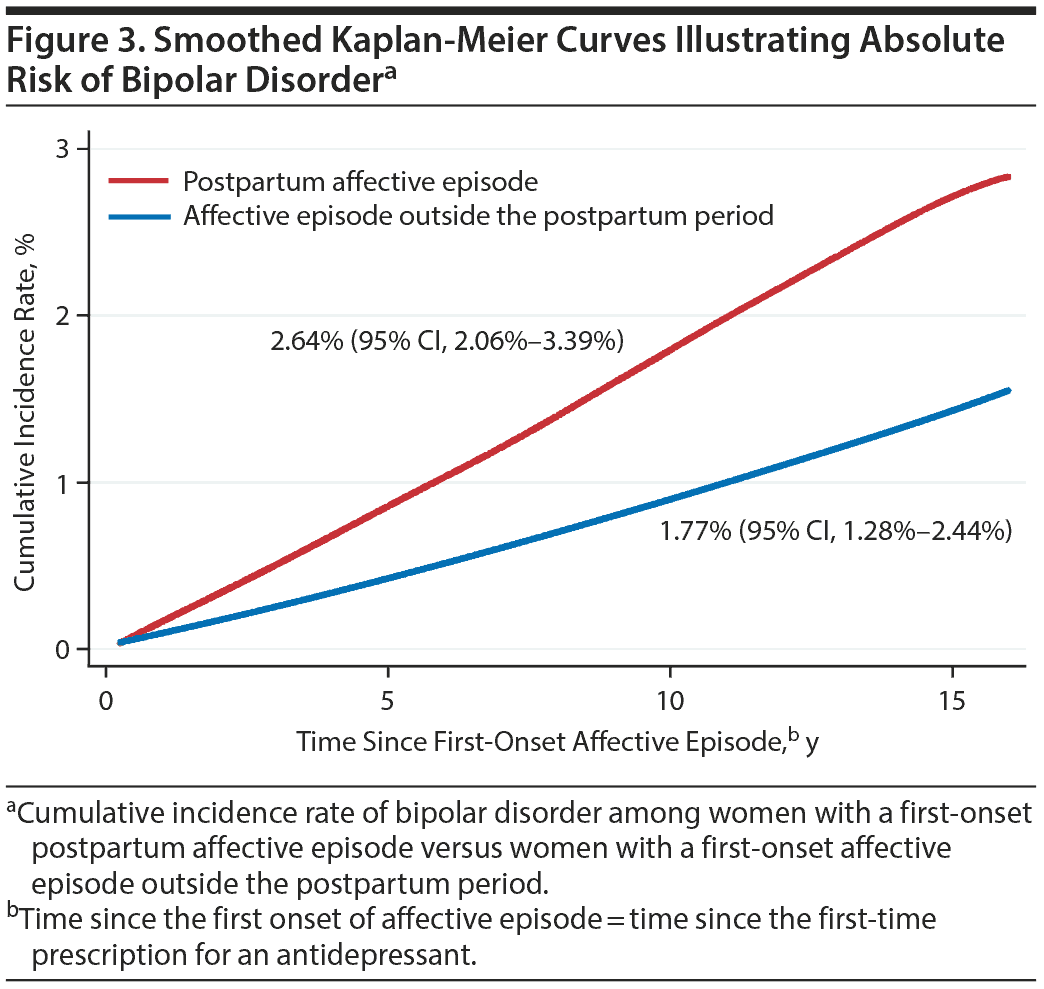
The median time from date of the first-onset postpartum affective episode to date of the first-time psychiatric contact for bipolar disorder was 4.5 years (interquartile range, 1.8-7.7). Figure 3 displays the cumulative incidence rate of bipolar disorder by using Kaplan-Meier curves. Sixteen years after initial treatment with antidepressants, 2.64% (95% CI, 2.06%-3.39%) of women with a postpartum affective episode developed bipolar disorder in comparison to 1.77% (95% CI, 1.28%-2.44%) of women with an affective episode outside the postpartum period. The risk of bipolar disorder among women with a postpartum affective episode was higher as compared to women with an affective episode outside the postpartum period (HR = 1.67; 95% CI, 1.35-2.08). Note, this did not take into account any effects of subsequent prescription for anxiolytics, mood stabilizers, or antipsychotics.
Similar associations were observed among women who had a first-onset affective episode 0-180 days and 181-365 days after delivery. Additionally, the risk of bipolar disorder remained increased during the entire follow-up period (Supplementary eTable 2).
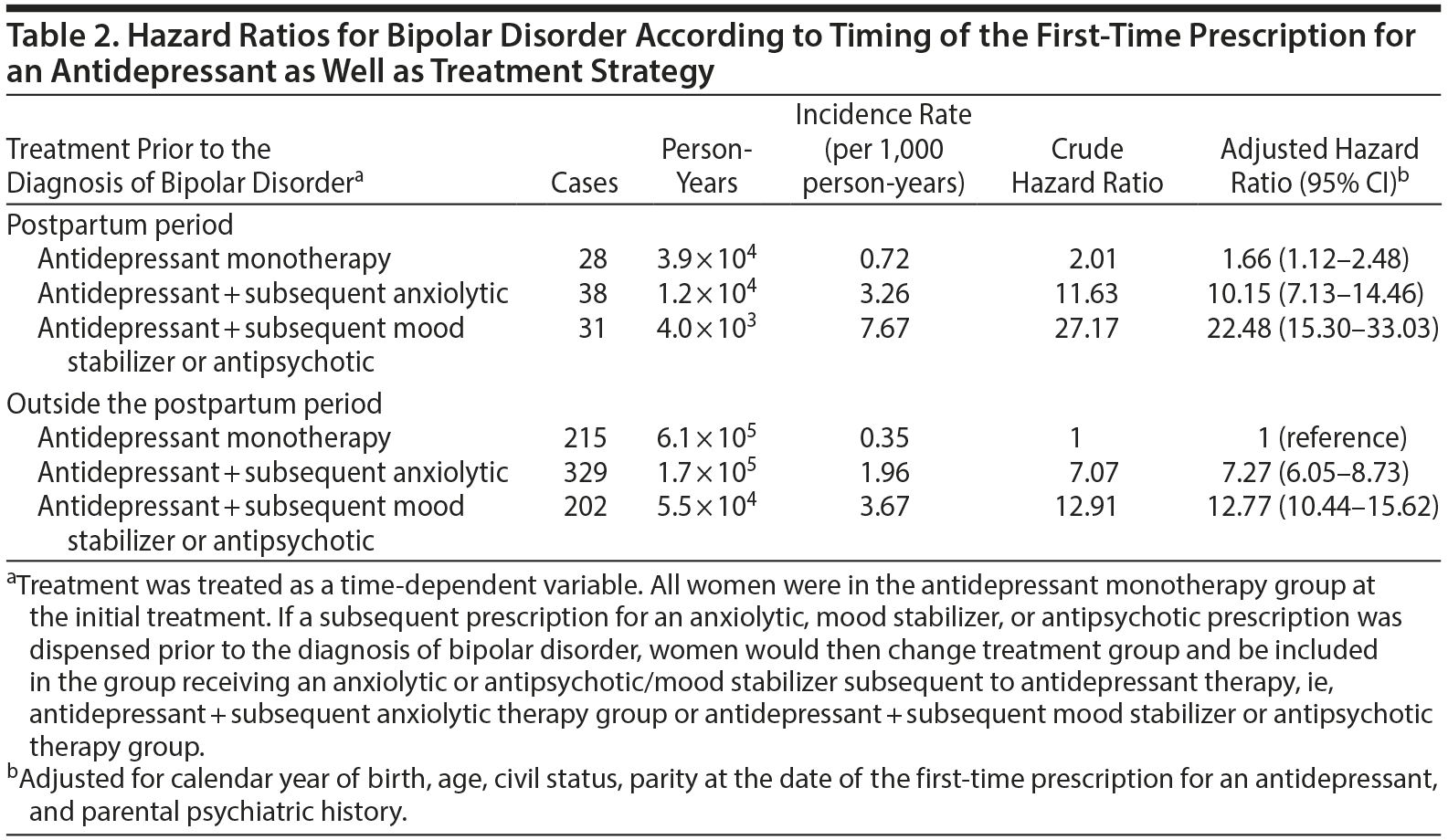
The median duration was 2.1 years (interquartile range, 0.5-4.9) from date of the first-time prescription for an antidepressant to date of addition of subsequent anxiolytic and 1.9 years (interquartile range, 0.5-4.8) to date of addition of mood stabilizer or antipsychotic, which was not affected by the type of first-time antidepressant (SSRIs vs non-SSRIs). Compared to antidepressant monotherapy outside the postpartum period, the HR for antidepressant monotherapy postpartum was 1.66 (95% CI, 1.12-2.48). Antidepressant use postpartum with a subsequent prescription for an anxiolytic was associated with a higher risk of bipolar disorder (HR = 10.15; 95% CI, 7.13-14.46). The highest risk was observed in postpartum women with the subsequent addition of a mood stabilizer or antipsychotic (HR = 22.48; 95% CI, 15.30-33.03) (Table 2).
Sensitivity Analyses
To account for the influence by age difference between women with a first-onset postpartum affective episode and women with a first-onset affective episode outside the postpartum period, we analyzed the data by stratifying on age groups: the HR for age < 25 years was 1.79 (95% CI, 1.17-2.73); for age 25-34 years, 1.57 (95% CI, 1.19-2.07); and for age ≥ 35 years, 1.99 (95% CI, 1.05-3.76). The associations of a first-onset postpartum affective episode and subsequent bipolar disorder did not change substantially after further adjustment for income and education at baseline (HR = 1.68; 95% CI, 1.35-2.08). After excluding 1,131 women who were pregnant at the time of the first-onset affective episode, similar associations were observed. In the sensitivity analyses, when we extended our washout period to 5 years, the results did not change significantly.
DISCUSSION
In our cohort study, we found that women with a first-onset postpartum affective episode had an increased risk of bipolar disorder in comparison to women with a first-onset affective episode outside the postpartum period during a maximum 16-year follow-up. The risk for subsequent bipolar disorder was more pronounced among postpartum women who received subsequent treatment with an anxiolytic.
Postpartum Affective Episode and Subsequent Bipolar Disorder
Previous work17,18 has suggested an association between antidepressant therapy and a subsequent occurrence of hypomanic or manic symptoms or bipolar disorder diagnosis. In the present study, we showed that women with a first-time prescription for an antidepressant within 1 year after childbirth are at a higher risk of subsequently being diagnosed with bipolar disorder compared to women with a first-time antidepressant therapy outside the postpartum period (HR = 1.67; 95% CI, 1.35-2.08).
Diagnosing bipolar symptomatology is complex,19 especially in the postpartum period. Misdiagnosis of bipolar symptoms during the postpartum period is therefore a possible explanation for the observed results, as episodes of mood elevation can be misconstrued as the normal joy of motherhood.20 An underestimation of bipolar vulnerability and possible underdiagnosis of bipolar disorder might have severe consequences, including ineffective treatment strategies, delayed referral to specialized psychiatric care, and underestimation of relapse risks after subsequent pregnancies. This will undoubtedly result in an unfavorable disease course for these women.
In contrast to concerns of underdiagnosing bipolar disorder, concerns regarding overdiagnosing the disorders are equally present in clinical practice. We do not expect that overdiagnosis of bipolar disorder during the postpartum period is a major concern, because in absolute numbers, only 2.64% of women were diagnosed with bipolar disorder during follow-up. However, overdiagnosing bipolar disorder in this group of women will also have severe consequences. A formal diagnosis of “bipolar disorder” after a single postpartum episode might lead to significant maternal distress with unnecessary exposure to long-term mood stabilizers or antipsychotics.21
Another explanation for the observed results is that hypomanic or manic symptoms are not present during the acute postpartum period but emerge at a later stage. This is supported by our finding of a median of 4.5 years from the date of the first-onset postpartum affective episode to the date of bipolar disorder diagnosis. Many episodes of bipolar disorder present initially with depressive symptoms, and it is difficult to distinguish a major depressive episode from a bipolar depressive episode in the absence of current or prior hypomanic or manic symptoms.17 In this scenario, the increased risk of bipolar disorder could reflect a change in symptoms over time toward a bipolar disease course.
The Link Between Childbirth and Bipolar Disorder
Childbirth and bipolar disorder have been linked across various studies. Previous studies22,23 have reported high rates of recurrence following childbirth in women with bipolar disorder. Moreover, among postpartum psychiatric episodes treated at inpatient psychiatric facilities, approximately 15% of the women converted to bipolar disorder during the 15-year follow-up period.7 Results from the present study add to the existing knowledge base, as we now demonstrate that less severe, nonpsychotic affective episodes following childbirth also can be markers of underlying bipolar disorder. Jointly, these results reconfirm that childbirth in particular can trigger a bipolar disease course also in women with an initial milder disease episode.
Clinical Relevance: Detailed Assessment for Bipolar Disorder in Women With Postpartum Affective Episodes
Our findings of a higher risk of bipolar disorder in women with a range of antidepressant-treated postpartum affective episodes have potential implications for clinical practice. It is recommended that all postpartum women seeking help for depressive episodes or anxiety are asked questions about current and prior hypomanic or manic symptoms,24 and administration of the Mood Disorders Questionnaire could be a useful assessment instrument.25 Last, clinical questions regarding parental history of psychiatric disorders, in particular bipolar disorder,6 will further help to assess an adequate bipolar risk profile.
In our study, a higher risk of bipolar disorder was observed among women who required a subsequent addition of an anxiolytic, mood stabilizer, or antipsychotic. Importantly, we do not interpret this finding as indicating that additional pharmacologic treatments increase the risk of bipolar disorder, given that evidence shows that mood-stabilizing medications are effective in preventing a relapse of bipolar disorder.26 A more likely explanation is that additional pharmacologic treatment is prescribed due to the severity of symptoms, treatment refractoriness, or emergence of comorbid psychiatric conditions.27 Overall, a poor response or failure to maintain response to antidepressants may provide a clue about an underlying bipolarity,27,28 and when antidepressant monotherapy is ineffective or the individual woman experiences changes in symptoms, health professionals should consider a possible bipolar spectrum disorder.
Monitoring of Antidepressant Use During the Postpartum Period
Antidepressants are a first-line treatment option for the majority of women with depressive and anxiety disorders postpartum,11 but antidepressants have shown little efficacy in the treatment of bipolar disorder.29 To treat patients with bipolar spectrum disorder with antidepressants, especially antidepressant monotherapy, may not be effective and might lead to an exacerbation of current episodes26,30 and increase the risk of suicide.31 It is crucial to carefully monitor symptom response to treatment and the disease course.32
Methodological Considerations
The Danish registers cover the entire Danish population with almost complete follow-up, which minimizes the impact of selection bias. Our study has a large sample size and long observation periods. The use of the prescription for an antidepressant as the indicator of affective status includes a wide range of severity of affective disorders. Linkage of several national registers enables us to adjust for several important confounders.
Our study has several limitations. First, we used first prescription for an antidepressant as a proxy for first-onset affective episode. Women with an affective disorder not treated by antidepressants are not included. Moreover, first antidepressant prescription may not necessarily indicate first onset. Also, antidepressants are prescribed to treat not only affective disorders but also other symptoms such as chronic insomnia,33 and we may have misclassified some women without affective disorders as cases. These misclassifications will, however, be nondifferential and bias our findings toward null.34 We did not have information on the indication for antidepressant treatment (ie, the underlying diagnosis), and we were therefore not able to examine the different effects on bipolar disorder from a primary depressive episode versus primary anxiety disorders. Second, to ensure the inclusion of women with an initial prescription for an antidepressant, we introduced a 2-year washout period. It is possible that we included women who had a prescription for an antidepressant before the establishment of the prescription register. Nonetheless, the results remained similar when we extended our washout period to 5 years, which verified our findings. Third, to include a homogeneous study population, we excluded women who had any psychiatric history before the first-time prescription for an antidepressant. Our findings thereby may not be generalizable to women with a preexisting psychiatric disorder.
CONCLUSION
Women with postpartum affective episodes have increased risks of bipolar disorder later in life, and women who fill an antidepressant prescription following childbirth should be asked about current and previous symptoms of hypomania or mania and monitored for these symptoms long term. Overall, our results lend further support to the link between childbirth and bipolar disorder.
Submitted: May 24, 2016; accepted September 8, 2016.
Disclosure of off-label usage: The authors have determined that, to the best of their knowledge, no investigational information about pharmaceutical agents that is outside US Food and Drug Administration-approved labeling has been presented in this article.
Financial disclosure: Drs Liu, Agerbo, Li, Bergink, and Munk-Olsen and Ms Meltzer-Brody have no personal affiliations or financial relationships with any commercial interest to disclose relative to the article.
Funding/support: Drs Liu and Munk-Olsen and Ms Meltzer-Brody are supported by the National Institute of Mental Health (R01MH104468). Drs Munk-Olsen and Agerbo are supported by iPSYCH, the Lundbeck Foundation Initiative for Integrative Psychiatric Research. Dr Li is supported by the European Research Council (ERC-2010-StG-260242-PROGEURO) and the Nordic Cancer Union (2013-129830). Dr Bergink has received funding from The Netherlands Organization for Scientific Research (clinical fellow and VENI incentive).
Role of the sponsor: The supporters had no role in the study design, data collection, analysis, interpretation, or publication of this study.
Supplementary material: See accompanying pages.
Find more articles on this and other psychiatry and CNS topics:
The Journal of Clinical Psychiatry
The Primary Care Companion for CNS Disorders
REFERENCES
1. Munk-Olsen T, Laursen TM, Pedersen CB, et al. New parents and mental disorders: a population-based register study. JAMA. 2006;296(21):2582-2589. PubMed doi:10.1001/jama.296.21.2582
2. Munk-Olsen T, Laursen TM, Mendelson T, et al. Risks and predictors of readmission for a mental disorder during the postpartum period. Arch Gen Psychiatry. 2009;66(2):189-195. PubMed doi:10.1001/archgenpsychiatry.2008.528
3. Jones I, Chandra PS, Dazzan P, et al. Bipolar disorder, affective psychosis, and schizophrenia in pregnancy and the post-partum period. Lancet. 2014;384(9956):1789-1799. PubMed doi:10.1016/S0140-6736(14)61278-2
4. Bergink V, Boyce P, Munk-Olsen T. Postpartum psychosis: a valuable misnomer. Aust N Z J Psychiatry. 2015;49(2):102-103. PubMed doi:10.1177/0004867414564698
5. Sit D, Rothschild AJ, Wisner KL. A review of postpartum psychosis. J Womens Health (Larchmt). 2006;15(4):352-368. PubMed doi:10.1089/jwh.2006.15.352
6. Munk-Olsen T, Laursen TM, Pedersen CB, et al. Family and partner psychopathology and the risk of postpartum mental disorders. J Clin Psychiatry. 2007;68(12):1947-1953. PubMed doi:10.4088/JCP.v68n1217
7. Munk-Olsen T, Laursen TM, Meltzer-Brody S, et al. Psychiatric disorders with postpartum onset: possible early manifestations of bipolar affective disorders. Arch Gen Psychiatry. 2012;69(4):428-434. PubMed doi:10.1001/archgenpsychiatry.2011.157
8. Howard LM, Molyneaux E, Dennis CL, et al. Non-psychotic mental disorders in the perinatal period. Lancet. 2014;384(9956):1775-1788. PubMed doi:10.1016/S0140-6736(14)61276-9
9. Sharma V, Khan M, Corpse C, et al. Missed bipolarity and psychiatric comorbidity in women with postpartum depression. Bipolar Disord. 2008;10(6):742-747. PubMed doi:10.1111/j.1399-5618.2008.00606.x
10. Munk-Olsen T, Gasse C, Laursen TM. Prevalence of antidepressant use and contacts with psychiatrists and psychologists in pregnant and postpartum women. Acta Psychiatr Scand. 2012;125(4):318-324. PubMed doi:10.1111/j.1600-0447.2011.01784.x
11. Bandelow B, Sher L, Bunevicius R, et al; WFSBP Task Force on Mental Disorders in Primary Care; WFSBP Task Force on Anxiety Disorders, OCD and PTSD. Guidelines for the pharmacological treatment of anxiety disorders, obsessive-compulsive disorder and posttraumatic stress disorder in primary care. Int J Psychiatry Clin Pract. 2012;16(2):77-84. PubMed doi:10.3109/13651501.2012.667114
12. Pedersen CB. The Danish Civil Registration System. Scand J Public Health. 2011;39(suppl 7):22-25. PubMed doi:10.1177/1403494810387965
13. Kildemoes HW, S׸rensen HT, Hallas J. The Danish National Prescription Registry. Scand J Public Health. 2011;39(suppl 7):38-41. PubMed doi:10.1177/1403494810394717
14. Mors O, Perto GP, Mortensen PB. The Danish Psychiatric Central Research Register. Scand J Public Health. 2011;39(suppl 7):54-57. PubMed doi:10.1177/1403494810395825
15. Knudsen LB, Olsen J. The Danish Medical Birth Registry. Dan Med Bull. 1998;45(3):320-323. PubMed
16. Petersson F, Baadsgaard M, Thygesen LC. Danish registers on personal labour market affiliation. Scand J Public Health. 2011;39(suppl):95-98. PubMed doi:10.1177/1403494811408483
17. Patel R, Reiss P, Shetty H, et al. Do antidepressants increase the risk of mania and bipolar disorder in people with depression? a retrospective electronic case register cohort study. BMJ Open. 2015;5(12):e008341. PubMed doi:10.1136/bmjopen-2015-008341
18. Tondo L, Vázquez G, Baldessarini RJ. Mania associated with antidepressant treatment: comprehensive meta-analytic review. Acta Psychiatr Scand. 2010;121(6):404-414. PubMed doi:10.1111/j.1600-0447.2009.01514.x
19. Angst J. Do many patients with depression suffer from bipolar disorder? Can J Psychiatry. 2006;51(1):3-5. PubMed doi:10.1177/070674370605100102
20. Heron J, Craddock N, Jones I. Postnatal euphoria: are ‘ the highs’ an indicator of bipolarity? Bipolar Disord. 2005;7(2):103-110. PubMed doi:10.1111/j.1399-5618.2005.00185.x
21. Singh T, Rajput M. Misdiagnosis of bipolar disorder. Psychiatry (Edgmont). 2006;3(10):57-63. PubMed
22. Maina G, Rosso G, Aguglia A, et al. Recurrence rates of bipolar disorder during the postpartum period: a study on 276 medication-free Italian women. Arch Women Ment Health. 2014;17(5):367-372. PubMed doi:10.1007/s00737-013-0405-4
23. Di Florio A, Forty L, Gordon-Smith K, et al. Perinatal episodes across the mood disorder spectrum. JAMA Psychiatry. 2013;70(2):168-175. PubMed doi:10.1001/jamapsychiatry.2013.279
24. Sharma V, Burt VK, Ritchie HL. Bipolar II postpartum depression: detection, diagnosis, and treatment. Am J Psychiatry. 2009;166(11):1217-1221. PubMed doi:10.1176/appi.ajp.2009.08121902
25. Clark CT, Sit DK, Driscoll K, et al. Does screening with the MDQ and EPDS improve identification of bipolar disorder in an obstetrical sample? Depress Anxiety. 2015;32(7):518-526. PubMed doi:10.1002/da.22373
26. Viktorin A, Lichtenstein P, Thase ME, et al. The risk of switch to mania in patients with bipolar disorder during treatment with an antidepressant alone and in combination with a mood stabilizer. Am J Psychiatry. 2014;171(10):1067-1073. PubMed doi:10.1176/appi.ajp.2014.13111501
27. Sharma V. Loss of response to antidepressants and subsequent refractoriness: diagnostic issues in a retrospective case series. J Affect Disord. 2001;64(1):99-106. PubMed doi:10.1016/S0165-0327(00)00212-3
28. Ghaemi SN, Ko JY, Goodwin FK. “Cade’s disease” and beyond: misdiagnosis, antidepressant use, and a proposed definition for bipolar spectrum disorder. Can J Psychiatry. 2002;47(2):125-134. PubMed
29. El-Mallakh RS, Vöhringer PA, Ostacher MM, et al. Antidepressants worsen rapid-cycling course in bipolar depression: A STEP-BD randomized clinical trial. J Affect Disord. 2015;184:318-321. PubMed doi:10.1016/j.jad.2015.04.054
30. Yildiz A, Sachs GS. Do antidepressants induce rapid cycling? a gender-specific association. J Clin Psychiatry. 2003;64(7):814-818. PubMed doi:10.4088/JCP.v64n0712
31. ×–zerdem A, Rasgon N. Women with bipolar disorder: a lifetime challenge from diagnosis to treatment. Bipolar Disord. 2014;16(1):1-4. PubMed doi:10.1111/bdi.12161
32. Molyneaux E, Trevillion K, Howard LM. Antidepressant treatment for postnatal depression. JAMA. 2015;313(19):1965-1966. PubMed doi:10.1001/jama.2015.2276
33. Wong J, Motulsky A, Eguale T, et al. Treatment indications for antidepressants prescribed in primary care in Quebec, Canada, 2006-2015. JAMA. 2016;315(20):2230-2232. PubMed doi:10.1001/jama.2016.3445
34. Rothman KJ, Greenland S, Lash TL. Validity in epidemiologic studies. In: Rothman KJ, Greenland S, Lash TL, eds. Modern Epidemiology. Philadelphia, PA: Lippincott Williams & Wilkins; 2008:162-185.
Editor’s Note: We encourage authors to submit papers for consideration as a part of our Focus on Women’s Mental Health section. Please contact Marlene P. Freeman, MD, at [email protected].
This PDF is free for all visitors!