Background: Previous research suggests that various types of childhood maltreatment frequently co-occur and confer risk for attempting suicide. However, it is unknown whether the effect of childhood maltreatment on this risk occurs through diverse, specific mechanisms or through a generalized liability, independently of psychopathology. Although these competing explanations have different implications for intervention, they have never been evaluated empirically.
Method: Structural equation modeling was used to examine the effect of different types of childhood maltreatment (ie, sexual abuse, physical and emotional abuse and neglect) on suicide attempt risk, and on age at first suicide attempt and repeated suicide attempts among attempters. Analyses controlled for demographic characteristics and DSM-IV Axis I and Axis II disorders. Data were drawn from a nationally representative survey of US adults, the 2004-2005 National Epidemiologic Survey on Alcohol and Related Conditions (N = 34,653).
Results: Childhood maltreatment was associated with an increased risk for attempting suicide and an earlier age at first suicide attempt among attempters, independently of psychopathology (P < .005). These associations operated mainly through the latent variable representing effects shared by the different types of childhood maltreatment, although sexual abuse had an additional, direct effect on the risk of suicide attempt. Childhood maltreatment types were not significantly associated with a history of multiple suicide attempts (all P values > .05).
Conclusions: The association between childhood maltreatment and suicide attempt operates mainly through a single broad liability, suggesting that the mechanisms underlying this dimension should be considered as an important therapeutic target for suicide prevention.
Find more articles on this and other psychiatry and CNS topics:
The Journal of Clinical Psychiatry
The Primary Care Companion for CNS Disorders
ABSTRACT
Background: Previous research suggests that various types of childhood maltreatment frequently co-occur and confer risk for attempting suicide. However, it is unknown whether the effect of childhood maltreatment on this risk occurs through diverse, specific mechanisms or through a generalized liability, independently of psychopathology. Although these competing explanations have different implications for intervention, they have never been evaluated empirically.
Method: Structural equation modeling was used to examine the effect of different types of childhood maltreatment (ie, sexual abuse, physical and emotional abuse and neglect) on suicide attempt risk, and on age at first suicide attempt and repeated suicide attempts among attempters. Analyses controlled for demographic characteristics and DSM-IV Axis I and Axis II disorders. Data were drawn from a nationally representative survey of US adults, the 2004-2005 National Epidemiologic Survey on Alcohol and Related Conditions (N = 34,653).
Results: Childhood maltreatment was associated with an increased risk for attempting suicide and an earlier age at first suicide attempt among attempters, independently of psychopathology (P < .005). These associations operated mainly through the latent variable representing effects shared by the different types of childhood maltreatment, although sexual abuse had an additional, direct effect on the risk of suicide attempt. Childhood maltreatment types were not significantly associated with a history of multiple suicide attempts (all P values > .05).
Conclusions: The association between childhood maltreatment and suicide attempt operates mainly through a single broad liability, suggesting that the mechanisms underlying this dimension should be considered as an important therapeutic target for suicide prevention.
J Clin Psychiatry 2015;76(7):916-923
10.4088/JCP.14m09420
© Copyright 2015 Physicians Postgraduate Press, Inc.
aDepartment of Psychiatry, New York State Psychiatric Institute/Columbia University, New York
bDepartment of Biostatistics, Mailman School of Public Health, Columbia University, New York, New York
cAssistance Publique-H×´pitaux de Paris (APHP), Corentin Celton Hospital, Department of Psychiatry, Paris Descartes University, PRES Sorbonne Paris Cité, Paris, France
dINSERM UMR 894, Psychiatry and Neurosciences Center, Paris Descartes University, PRES Sorbonne Paris Cité, Paris, France
*Corresponding author: Nicolas Hoertel, MD, MPH, Department of Psychiatry, Corentin Celton Hospital, Paris Descartes University, 4 parvis Corentin Celton; 92130 Issy-les-Moulineaux, France ([email protected]).
Despite considerable advances in our understanding of its neurobiology, suicide continues to be a major public health concern.1 Exposure to childhood maltreatment (ie, abuse and/or neglect) is highly prevalent in the general population2 and considered one of the main environmental risk factors for suicide.3,4
Although there is a well-established relationship between childhood maltreatment and later suicide attempts,5-9 it is unknown whether the effects of childhood maltreatment on this risk occur through diverse, specific mechanisms or through a generalized liability. Although these competing explanations have different implications for intervention, they have never been evaluated empirically. In addition, most published research focused on the effects of childhood maltreatment on suicide risk has relied on samples of convenience and examined a single type of maltreatment (eg, sexual abuse or physical abuse),3,10-13 despite ample evidence that these exposures frequently co-occur.2,14,15 Lastly, most previous studies have not controlled for the presence of psychopathology, which may at least partially mediate the link between childhood maltreatment and suicide attempt.2,12,15-23 To date, it remains unclear whether childhood maltreatment in general or particular types of childhood maltreatment impact on the risk for attempting suicide or on the age at first suicide attempt or the risk of repeated suicide attempts beyond the risk of attempting suicide. In addition to advancing the understanding of the mechanisms through which childhood maltreatment leads to suicide attempts, this knowledge has also important implications for suicide prevention if it allows to better identify, among individuals with a history of childhood maltreatment, those at greater risk for suicide attempt and for repeated suicide attempts beyond the risk of attempting suicide.
We used data from Wave 2 of National Epidemiologic Survey on Alcohol and Related Conditions (NESARC), a nationally representative sample of the US adult population, to examine the effects of 5 types of childhood maltreatment (ie, emotional neglect, physical neglect, emotional abuse, physical abuse, and sexual abuse) on the risk of suicide attempts in the general population, the age of first suicide attempt, and the risk of repeated suicide attempts among suicide attempters, while controlling for demographic characteristics (ie, age, sex, race/ethnicity, and family poverty) and psychopathology. We used a latent variable approach to examine the associations between childhood maltreatment and suicide attempts to disentangle the effects shared among all types of childhood maltreatment versus those that could be specific to some types of maltreatment.
METHOD
Sample
Data were drawn from the 2004-2005 NESARC, the second wave of the NESARC. The Wave 1 NESARC was a nationally representative face-to-face survey of 43,093 civilian noninstitutionalized US residents aged 18 years and older, conducted in 2001-2002 by the US Census Bureau under the direction of the National Institute on Alcoholism and Alcohol Abuse (NIAAA) and described in detail elsewhere.24,25 The overall survey response rate was 70.2%, resulting in 34,653 completed interviews.24 Wave 2 NESARC data were weighted to reflect design characteristics of the NESARC survey and be representative of the US civilian population based on the 2000 census. The research protocol, including written informed consent procedures, received full human subjects review and approval from the US Census Bureau and the Office of Management and Budget.24 The present study analyses are based on the 34,653 participants in Wave 2, which included measures of childhood maltreatment.
Measures
Participants were interviewed face to face with the Alcohol Use Disorder and Associated Disabilities Interview Schedule, DSM-IV version (AUDADIS-IV), a fully structured diagnostic instrument designed for experienced lay interviewers.24

- In a large nationally representative sample, all types of childhood maltreatment are associated with greater risk of suicide attempt and with earlier age at first suicide attempt among attempters, independently of psychopathology and sociodemographic characteristics.
- The associations of childhood maltreatment with these risks operate mainly through a single broad liability representing the shared effects of maltreatment, although sexual abuse has an additional, direct effect on the risk of suicide attempt.
- Mechanisms underlying this broad liability could be considered as an important therapeutic target for progress in suicide prevention.
Childhood Maltreatment
Five types of childhood maltreatment were examined: emotional neglect, physical neglect, emotional abuse, physical abuse, and sexual abuse.2 Respondents completed 19 questions regarding exposure to the types of maltreatment occurring before age 17 years adapted from the Conflict Tactics Scale and the Childhood Trauma Questionnaire.2 All response options ranged from never (1) to very often (5), with the exception of emotional neglect, which ranged from “never” to “always” and was reverse coded for the purposes of analysis. A test-retest study of these items indicated excellent intraclass test-retest reliability coefficients ranging from 0.79 for physical abuse to 0.88 for emotional abuse.26 Keyes et al2 found that a 5-factor confirmatory factor analysis model fit the 19 childhood maltreatment items very well.
Suicide Attempt Outcomes
All participants were asked whether they ever attempted suicide. Those who answered positively were further asked about their age at the time of the first/single suicide attempt and whether it happened once or at least 2 times. Among the 1,265 suicide attempters, respectively 25 and 22 participants did not report age at the time of first attempt and whether they made at least 2 suicide attempts. Missing data were imputed using Markov chain Monte Carlo methods.27 Results were unchanged in sensitivity analyses excluding respondents with missing data.
Covariates
All models controlled for age at the time of Wave 2 interview, sex, race/ethnicity (white vs nonwhite), family poverty (considered present if participants reported that their family received money from any government assistance program before they were aged 18 years old), and psychopathology. Psychopathology was assessed with the following variables: any mood disorder (including major depressive disorder, bipolar disorder, and dysthymia), any anxiety disorder (including generalized anxiety disorder, posttraumatic stress disorder [as per DSM-IV used in this study], panic disorder, social anxiety disorder, and specific phobia), any personality disorder (including paranoid, schizoid, schizotypal, antisocial, borderline, histrionic, narcissistic, avoidant, obsessive-compulsive, and dependent personality disorders), alcohol use disorders, drug use disorders, nicotine dependence, pathological gambling, and attention-deficit/hyperactivity disorder (ADHD). In individuals with a history of suicide attempt, Axis I disorders were assessed at the time of the first suicide attempt. In individuals without a history of attempts, Axis I disorders were assessed on a lifetime basis. Axis II disorders were assessed on a lifetime basis for all respondents. The AUDADIS-IV substance dependence, mood and anxiety disorders, and personality disorders diagnoses demonstrated good to excellent test-retest reliability in clinical and general population samples.25
Statistical Analyses
We performed logistic regressions to determine whether each type of childhood maltreatment was associated with suicide attempt in the general population and/or repeated suicide attempts among suicide attempters, while controlling for sociodemographic characteristics and psychopathology. Among suicide attempters, a Cox proportional hazards regression model28 was used to compare age at first suicide attempt distributions between participants with and without each childhood maltreatment type, while controlling for psychopathology at the time of the first/single suicide attempt and sociodemographic characteristics. This model provides an estimate of the effect of each maltreatment type on age at first suicide attempt. Consistent with prior work,3,29 a participant was considered to have suffered childhood maltreatment if the respondent reported frequent exposure (sometimes, often or very often), except for sexual abuse, which was considered present if the respondent indicated at least 1 episode.
Next, we built upon the same 5-factor confirmatory factor analysis (CFA) model previously fit by Keyes et al2 and performed a second-order CFA model to determine whether a shared maltreatment factor fit the underlying structure of childhood maltreatment. We examined measures of goodness-of-fit, including the comparative fit index (CFI), the Tucker-Lewis index (TLI), and the root mean squared error of approximation (RMSEA).30 Comparative fit index and TLI values greater than 0.95 and values of RMSEA less than 0.06 are commonly used to indicate good model fit and were used as cutoffs.
Finally, we used a structural equation model to assess shared and specific effects of the different types of childhood maltreatment on each suicide attempt outcome. Specifically, while controlling for sociodemographic characteristics and psychopathology, we successively examined (1) the effect of the shared maltreatment factor (representing the shared effects of the 5 latent dimensions underlying the structure of childhood maltreatment) on each suicide attempt outcome and (2) the effects of the 5 types of childhood maltreatment on each suicide attempt outcome above and beyond their shared effects through the childhood maltreatment factor. Response options (scores from 1 to 5) for each of the 19 maltreatment items were modeled as ordered categorical indicators of the maltreatment factors, which were analyzed as latent variables.
Since the 5 childhood maltreatment factors frequently co-occur, an advantage of modeling a second-order latent abuse factor is that their shared and specific effects are disambiguated in an easier way than if they were to be included as multiple separate predictors mutually adjusted for one another.31 The relationships examined between the specific maltreatment factors and each suicide attempt outcome are interpreted as the direct effects because they indicate effect of the specific maltreatment type that is not mediated through the shared maltreatment factor. To avoid including effects that could be significant due to multiple testing and because of the large sample size,27,32,33 we decided a priori to evaluate statistical significance using a 2-sided design with α set at .005.
All analyses were conducted in Mplus Version 7.127 to take into account the complex sample design of the NESARC survey. The default estimator for the analysis was the variance-adjusted weighted least squares, a robust estimator appropriate for ordered categorical and dichotomous observed variables such as the ones used in the present study.27
RESULTS
Comparing Rates of Childhood Maltreatment Among Individuals With and Without a Lifetime History of Suicide Attempt
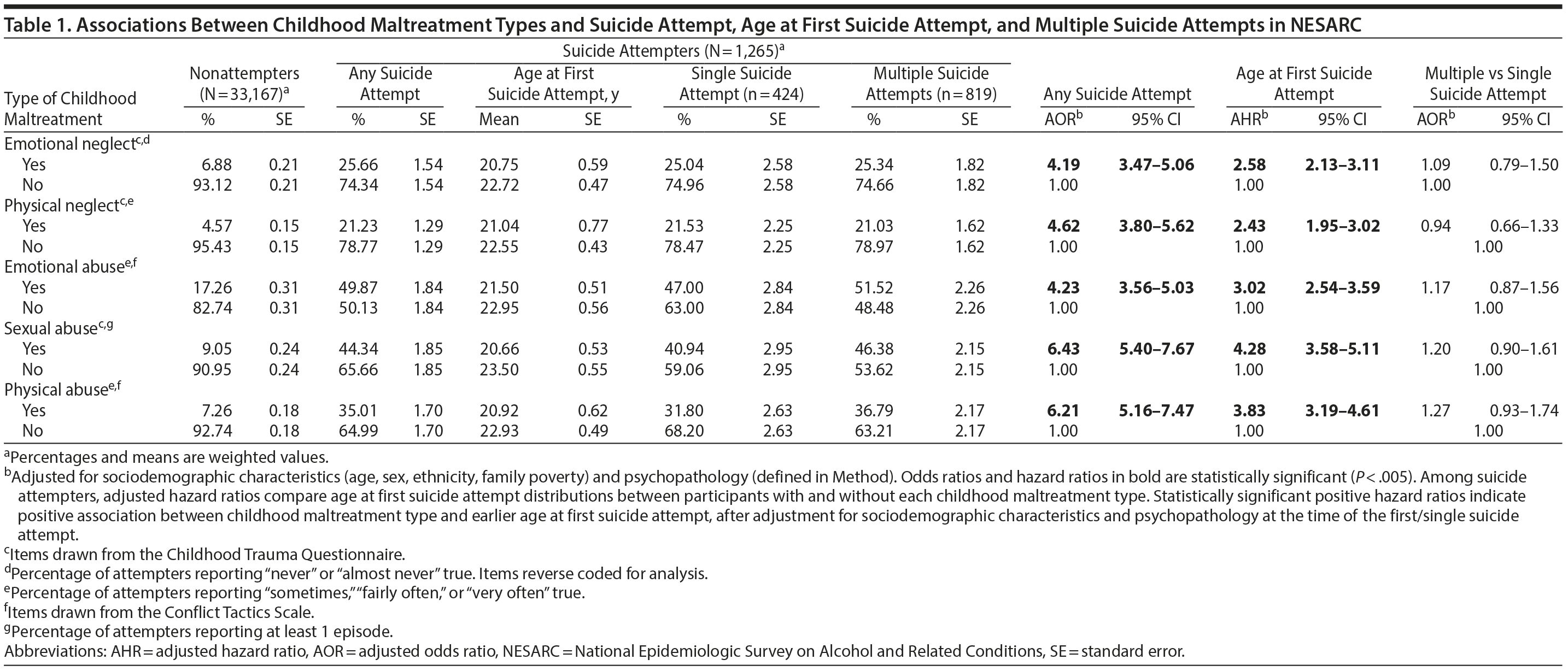
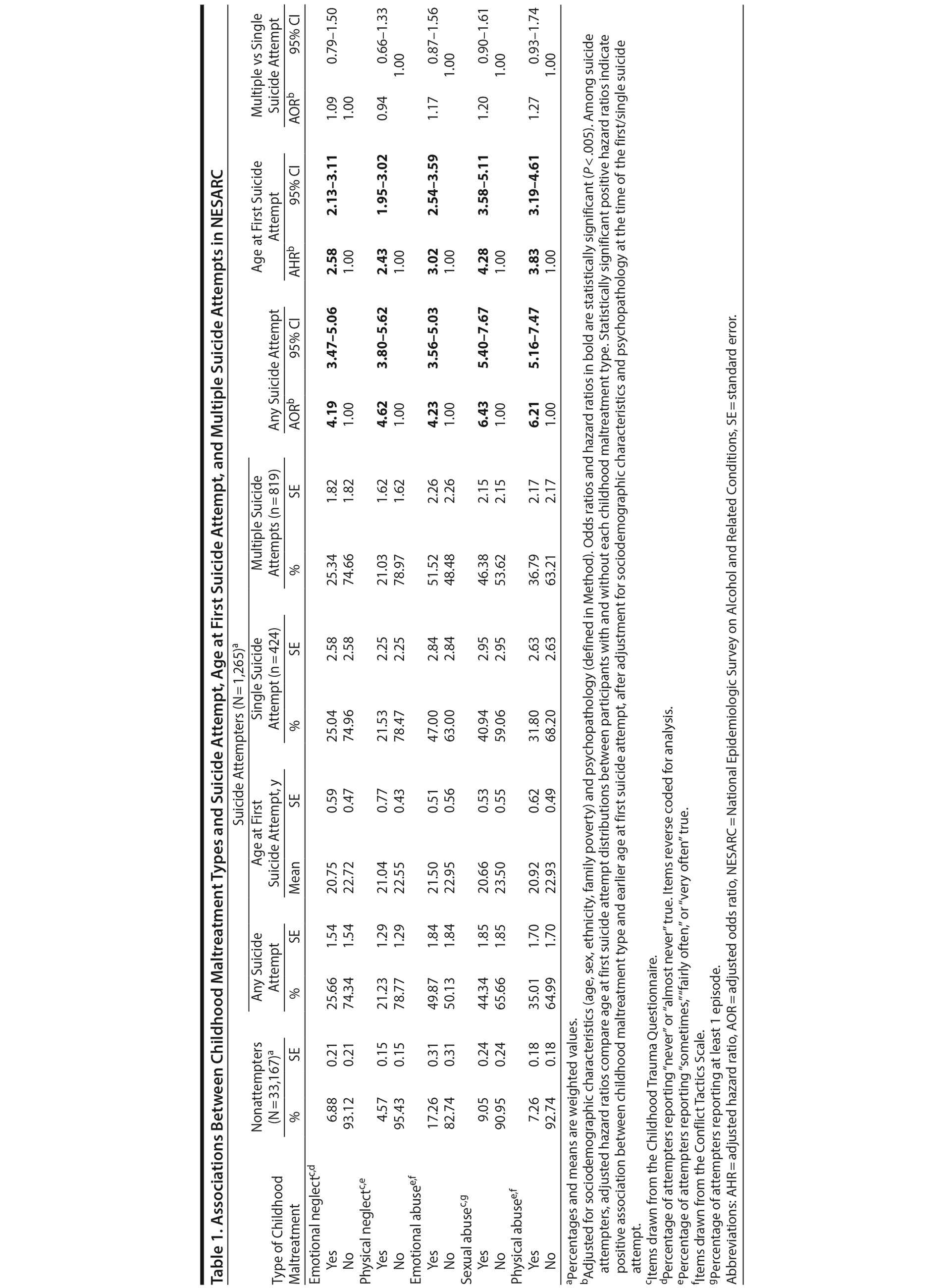
After adjusting for sociodemographic characteristics and psychopathology, all types of childhood maltreatment were significantly associated with a lifetime history of suicide attempt in the general population and with a younger age at first suicide attempt among attempters (Table 1). Sexual abuse showed the strongest association with suicide attempt and age at first suicide attempt following these adjustments. By contrast, there were no significant differences in the rates of any type of childhood maltreatment between individuals with single versus multiple suicide attempts. Therefore, we did not examine this outcome using structural equation models framework.
Structure of Childhood Maltreatment
The second-order CFA of the 5 childhood maltreatment factors measured by a single common maltreatment factor provided an excellent fit to the data (CFI = 0.983, TLI = 0.980, and RMSEA = 0.038).
Effects of Childhood Maltreatment Types on the Risk of Suicide Attempt
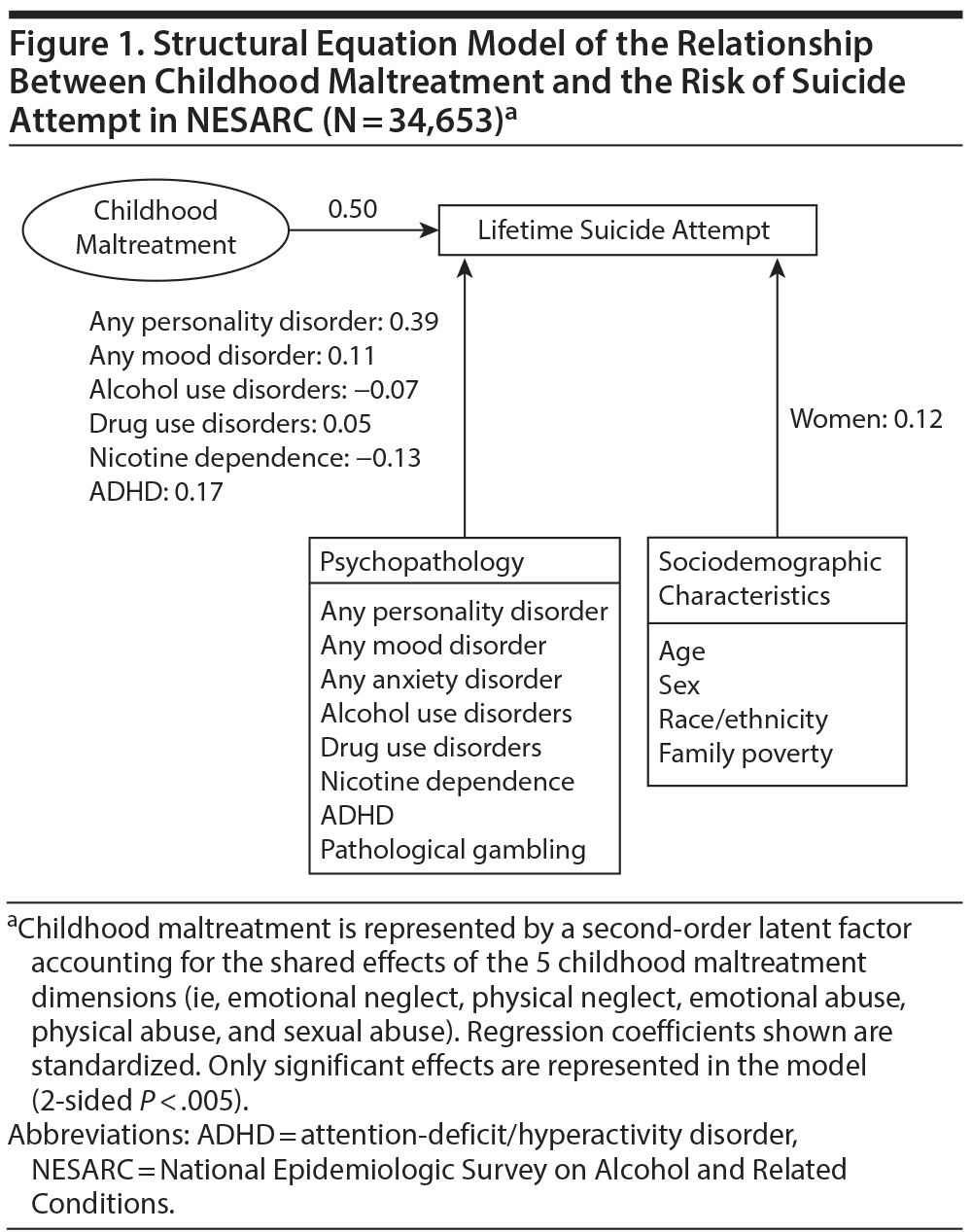
After adjusting for sociodemographic characteristics and mental disorders, the latent variable representing the shared effect of all childhood maltreatment types increased the risk of suicide attempt (Figure 1). Furthermore, beyond the effect due to the latent shared maltreatment factor, the sexual abuse factor had a significant (P < .005) direct positive effect on the risk of suicide attempt (see Supplementary eFigure 1 at PSYCHIATRIST.COM). By contrast, after adjusting for the shared maltreatment factor, physical neglect and emotional abuse had negative coefficients in the model, suggesting that these types of maltreatment increased the risk of suicide attempt to a lesser extent than sexual abuse.
Effects of Childhood Maltreatment Types on Age at First Suicide Attempt
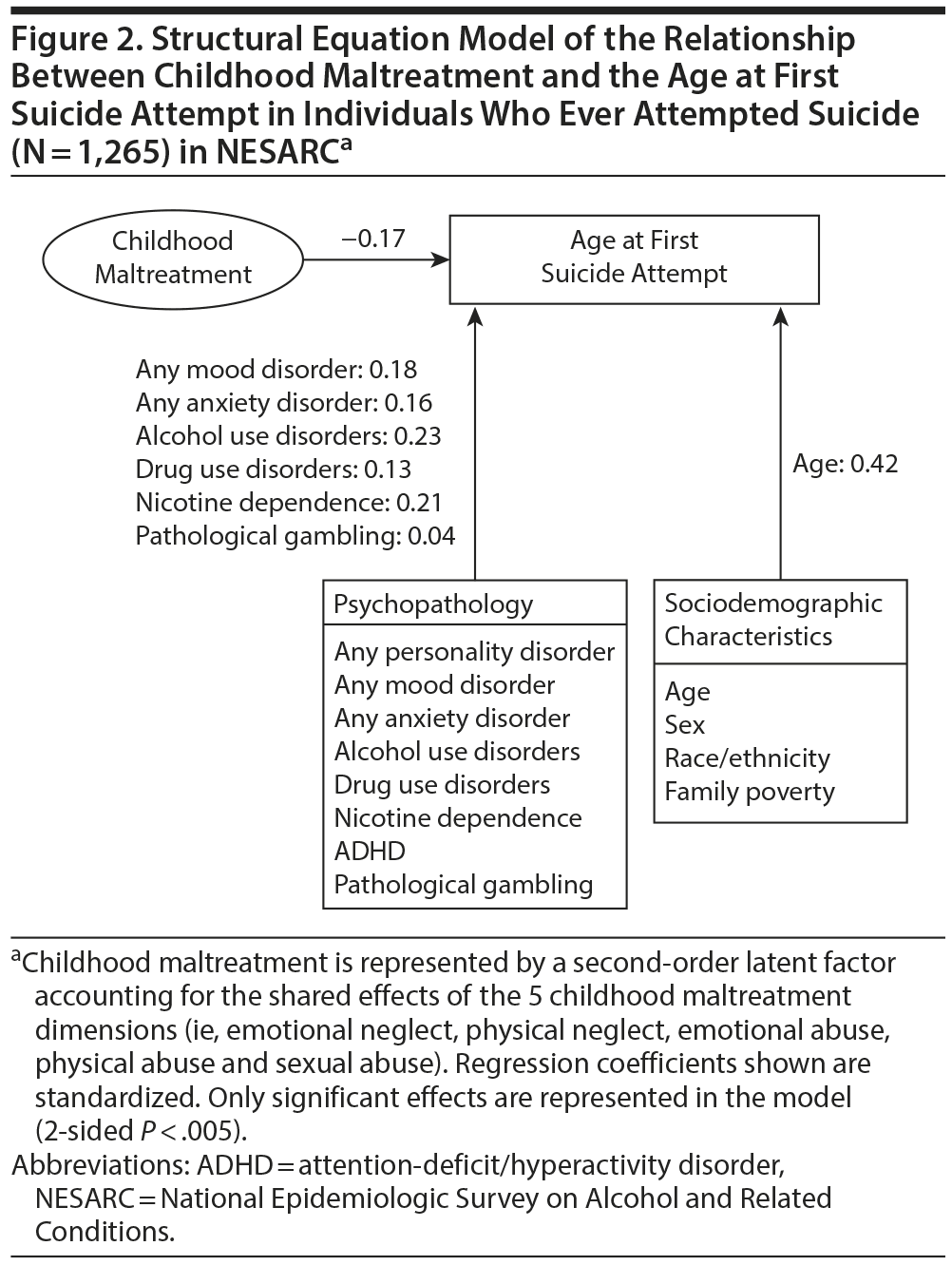
After adjusting for sociodemographic characteristics and mental disorders, the latent shared maltreatment factor significantly decreased the age at first suicide attempt among suicide attempters (Figure 2 and Supplementary eFigure 2). There were no direct effects from any type of childhood maltreatment beyond the effect due to the latent shared maltreatment factor.
DISCUSSION
In a large nationally representative sample, all types of childhood maltreatment were strongly associated with the risk of suicide attempt and with earlier age at first suicide attempt among attempters, and their effect occurred mostly through a latent dimension representing the shared effects of maltreatment, independently of sociodemographic characteristics and Axis I and Axis II disorders. Furthermore, sexual abuse had direct effects on the risk of suicide attempt above and beyond the shared effects of all types of childhood maltreatment. We also found that childhood maltreatment did not significantly increase the risk of repeated suicide attempts among suicide attempters. Several novel findings emerged in the present study.
We found that the associations of each type of childhood maltreatment with increased risk for suicide attempt and earlier age of first suicide attempt among attempters were mostly mediated through a latent variable accounting for the shared effects of the different types of maltreatment, rather than directly through each type of maltreatment. Although the mechanisms linking childhood maltreatment and suicidal behavior remain unknown, several explanations may contribute to this association. First, childhood maltreatment can disrupt developmental processes related to strengthening of emotional regulation and associated interpersonal skills, including insecure attachment styles, impairments in emotional perception and reward processing,10,34 and increased impulsivity and neuroticism.10,35-41 These disruptions may decrease the threshold for suicidal behavior in individuals experiencing stressful events.10,34 Second, the higher rates of suicide attempt in individuals with childhood maltreatment may result from epigenetic modifications.42 For example, McGowan et al43 found that childhood maltreatment may increase the risk of suicide by altering hypothalamic-pituitary-adrenal (HPA) stress responses through the epigenetic hypermethylation of the Nr3C1 gene. Third, the long-term decreased social support associated with childhood maltreatment44 could also contribute to increased risk of attempting suicide.
Although much of the association between childhood maltreatment and risk of suicide attempt was mediated through the shared maltreatment factor, sexual abuse increased the risk of suicide attempt, above and beyond the effect of that factor. The stronger effect of childhood sexual abuse on the risk of suicide attempt is consistent with epidemiologic evidence indicating that sexual abuse (1) constitutes one of the main risk factors for suicide attempt45,46 and is more strongly associated with suicidal behavior than other forms of childhood maltreatment3,10,46-49 and (2) has longer-term impact on psychosocial functioning.50,51 Childhood sexual abuse may differ from other types of childhood adversity in its greater capacity to disrupt the underlying neurobiological structures involved in stress response52 and to increase the sensitivity to depressogenic life experiences53 and the susceptibility to environmental influences.54 It is also likely that the dysregulation of the HPA axis, which is more strongly associated to childhood sexual abuse than to other types of childhood maltreatment,54 may be moderated by the genetic background of the individual such as 5-HTTLPR, FKBP5, and Val66Met polymorphisms.54-57 Finally, family environmental correlates of suicide attempts, including increased family discord and low social support, are more prevalent among sexually abused children58 and may also contribute to this association.
We also found that no type of childhood maltreatment predicted repeated suicide attempts among individuals who ever attempted suicide. This finding is in contrast with some studies conducted in clinical samples45,59-61 but consistent with data derived from 2 nationally representative samples of the US general population.62 Individuals with history of multiple suicide attempts could be considered as a unique subgroup of suicide attempters.62-66 Using Beck’s theory of modes,41 a previous study63 suggested that the suicidal mode in individuals with a history of multiple suicide attempts becomes highly accessible in memory and requires minimal triggering stimuli to be activated.63 Building upon this model, our results suggest that underlying mechanisms of childhood maltreatment leading to increased risk of suicide are different from the mechanisms associated with repeated suicide attempts.
Our findings have important implications. From the etiologic point of view, they indicate that effects of childhood maltreatment on the risk of attempting suicide and on the age of suicide attempt among attempters occur mostly through a broad latent factor, representing the shared vulnerabilities triggered by the experience of childhood maltreatment. These results underscore the importance of adopting dimensional approaches in the study of childhood maltreatment and suicidal behavior, which may help disentangle biological and psychological mechanisms underlying the shared and specific associations of childhood maltreatment types with suicide attempt. In addition, our findings suggest that the mechanisms that link childhood maltreatment to increased risk of suicide are independent of risk factors leading to multiple suicide attempts. From a clinical point of view, our results extend prior work67,68 and underscore the key role of all types of maltreatment in suicide attempts. Because these childhood experiences increase the risk of suicide attempt mainly through a broad liability, our findings also suggest that preventing actual child maltreatment thanks to universal and selective interventions that have been successfully applied67 and the use of indicated interventions targeting this dimension in victims of childhood maltreatment could lead to substantial progress in suicide prevention.
This study should be interpreted in light of some limitations. First, retrospective reporting of childhood maltreatment may be subject to recall bias.2,15,69 However, longitudinal studies testing the validity of retrospective child maltreatment self-report, including childhood sexual abuse, generally find more false-negatives than false-positives.70-72 Second, for participants who attempted suicide before age 17, our analysis of suicide lifetime attempts did not allow us to establish the temporal precedence between the exposure to childhood maltreatment and suicide outcomes.73,74 Nonetheless, suicide attempts and mental disorders are rare in prepubescence,3,4 and additional analyses excluding participants who attempted suicide at age 12 or under did not modify the statistical significance of effects of childhood maltreatment on suicide attempt and age at first suicide attempt among attempters (eFigures 3 and 4). In addition, although it remains possible that there could be a third variable related to both, suicide attempts are unlikely to lead in most cases to childhood maltreatment. Last, information on approximate age at onset of each childhood maltreatment type, parental history of having been themselves victims of childhood maltreatment, and family environmental context (such as family discord), which have been found to be linked with higher suicidal intent,10,49,58 was not available in NESARC.
Despite these limitations, our findings underscore the pernicious long-term effects of childhood maltreatment on the risk of suicidal behavior. Preventing childhood maltreatment may have broad benefits to reduce not only the suffering of these children and adolescents but also the burden of suicide.
Submitted: July 29, 2014; accepted October 23, 2014.
Disclosure of off-label usage: The authors have determined that, to the best of their knowledge, no investigational information about pharmaceutical agents that is outside US Food and Drug Administration-approved labeling has been presented in this activity.
Financial disclosures: Dr Oquendo receives royalties for use of the Columbia Suicide Severity Rating Scale; has received financial compensation from Pfizer for the safety evaluation of a clinical facility in 2006, unrelated to this study; has received unrestricted educational grants and/or lecture fees from AstraZeneca, Bristol-Myers Squibb, Eli Lilly, Janssen, Otsuka, Pfizer, Sanofi-Aventis, and Shire; and her family owns stock in Bristol-Myers Squibb. Dr Limosin is a member of the speakers/advisory boards for Janssen, Euthérapie, Lundbeck, and Roche. Drs Hoertel, Franco, Wall, Wang, and Blanco have no personal affiliations or financial relationships with any commercial interest to disclose relative to the article.
Funding/support: Supported by National Institutes of Health grants DA019606, DA023200, MH076051, and MH082773 (Dr Blanco); the New York State Psychiatric Institute (Drs Blanco, Oquendo, and Wall); and a fellowship grant from Public Health Expertise (Dr Hoertel).
Role of the sponsors: The sponsors had no additional role in the design and conduct of the study; collection, management, analysis, and interpretation of the data; and preparation, review, or approval of the manuscript.
Additional information: The original data set for the National Epidemiologic Survey on Alcohol and Related Conditions (NESARC) is available from the National Institute on Alcohol Abuse and Alcoholism (http://www.niaaa.nih.gov).
Supplementary material: Available at PSYCHIATRIST.COM.
Find more articles on this and other psychiatry and CNS topics:
The Journal of Clinical Psychiatry
The Primary Care Companion for CNS Disorders
REFERENCES
1. Rockett IRH, Regier MD, Kapusta ND, et al. Leading causes of unintentional and intentional injury mortality: United States, 2000-2009. Am J Public Health. 2012;102(11):e84-e92. PubMed doi:10.2105/AJPH.2012.300960
2. Keyes KM, Eaton NR, Krueger RF, et al. Childhood maltreatment and the structure of common psychiatric disorders. Br J Psychiatry. 2012;200(2):107-115. PubMed doi:10.1192/bjp.bp.111.093062
3. Dube SR, Anda RF, Felitti VJ, et al. Childhood abuse, household dysfunction, and the risk of attempted suicide throughout the life span: findings from the Adverse Childhood Experiences Study. JAMA. 2001;286(24):3089-3096. PubMed doi:10.1001/jama.286.24.3089
4. Ezzati M, Lopez AD, Rodgers A, et al; Comparative Risk Assessment Collaborating Group. Selected major risk factors and global and regional burden of disease. Lancet. 2002;360(9343):1347-1360. PubMed doi:10.1016/S0140-6736(02)11403-6
5. Brezo J, Paris J, Vitaro F, et al. Predicting suicide attempts in young adults with histories of childhood abuse. Br J Psychiatry. 2008;193(2):134-139. PubMed doi:10.1192/bjp.bp.107.037994
6. Wanner B, Vitaro F, Tremblay RE, et al. Childhood trajectories of anxiousness and disruptiveness explain the association between early-life adversity and attempted suicide. Psychol Med. 2012;42(11):2373-2382. PubMed doi:10.1017/S0033291712000438
7. Fergusson DM, Horwood LJ, Ridder EM, et al. Suicidal behaviour in adolescence and subsequent mental health outcomes in young adulthood. Psychol Med. 2005;35(7):983-993. PubMed doi:10.1017/S0033291704004167
8. Bruffaerts R, Demyttenaere K, Borges G, et al. Childhood adversities as risk factors for onset and persistence of suicidal behaviour. Br J Psychiatry. 2010;197(1):20-27. PubMed doi:10.1192/bjp.bp.109.074716
9. Borges G, Nock MK, Haro Abad JM, et al. Twelve-month prevalence of and risk factors for suicide attempts in the World Health Organization World Mental Health Surveys. J Clin Psychiatry. 2010;71(12):1617-1628. PubMed doi:10.4088/JCP.08m04967blu
10. Lopez-Castroman J, Melhem N, Birmaher B, et al. Early childhood sexual abuse increases suicidal intent. World Psychiatry. 2013;12(2):149-154. PubMed doi:10.1002/wps.20039
11. Briere J, Evans D, Runtz M, et al. Symptomatology in men who were molested as children: a comparison study. Am J Orthopsychiatry. 1988;58(3):457-461. PubMed doi:10.1111/j.1939-0025.1988.tb01606.x
12. Fergusson DM, Boden JM, Horwood LJ. Exposure to childhood sexual and physical abuse and adjustment in early adulthood. Child Abuse Negl. 2008;32(6):607-619. PubMed doi:10.1016/j.chiabu.2006.12.018
13. Joiner TE Jr, Sachs-Ericsson NJ, Wingate LRR, et al. Childhood physical and sexual abuse and lifetime number of suicide attempts: a persistent and theoretically important relationship. Behav Res Ther. 2007;45(3):539-547. PubMed doi:10.1016/j.brat.2006.04.007
14. Dong M, Anda RF, Felitti VJ, et al. The interrelatedness of multiple forms of childhood abuse, neglect, and household dysfunction. Child Abuse Negl. 2004;28(7):771-784. PubMed doi:10.1016/j.chiabu.2004.01.008
15. Green JG, McLaughlin KA, Berglund PA, et al. Childhood adversities and adult psychiatric disorders in the national comorbidity survey replication, 1: associations with first onset of DSM-IV disorders. Arch Gen Psychiatry. 2010;67(2):113-123. PubMed doi:10.1001/archgenpsychiatry.2009.186
16. Johnson JG, Cohen P, Brown J, et al. Childhood maltreatment increases risk for personality disorders during early adulthood. Arch Gen Psychiatry. 1999;56(7):600-606. PubMed doi:10.1001/archpsyc.56.7.600
17. Arseneault L, Cannon M, Fisher HL, et al. Childhood trauma and children’s emerging psychotic symptoms: a genetically sensitive longitudinal cohort study. Am J Psychiatry. 2011;168(1):65-72. PubMed doi:10.1176/appi.ajp.2010.10040567
18. Read J, van Os J, Morrison AP, et al. Childhood trauma, psychosis and schizophrenia: a literature review with theoretical and clinical implications. Acta Psychiatr Scand. 2005;112(5):330-350. PubMed doi:10.1111/j.1600-0447.2005.00634.x
19. Kendler KS, Bulik CM, Silberg J, et al. Childhood sexual abuse and adult psychiatric and substance use disorders in women: an epidemiological and cotwin control analysis. Arch Gen Psychiatry. 2000;57(10):953-959. PubMed doi:10.1001/archpsyc.57.10.953
20. Clark DB, Lesnick L, Hegedus AM. Traumas and other adverse life events in adolescents with alcohol abuse and dependence. J Am Acad Child Adolesc Psychiatry. 1997;36(12):1744-1751. PubMed doi:10.1097/00004583-199712000-00023
21. Widom CS, Marmorstein NR, White HR. Childhood victimization and illicit drug use in middle adulthood. Psychol Addict Behav. 2006;20(4):394-403. PubMed doi:10.1037/0893-164X.20.4.394
22. Phillips NK, Hammen CL, Brennan PA, et al. Early adversity and the prospective prediction of depressive and anxiety disorders in adolescents. J Abnorm Child Psychol. 2005;33(1):13-24. PubMed doi:10.1007/s10802-005-0930-3
23. Widom CS, DuMont K, Czaja SJ. A prospective investigation of major depressive disorder and comorbidity in abused and neglected children grown up. Arch Gen Psychiatry. 2007;64(1):49-56. PubMed doi:10.1001/archpsyc.64.1.49
24. Grant BF, Goldstein RB, Chou SP, et al. Sociodemographic and psychopathologic predictors of first incidence of DSM-IV substance use, mood and anxiety disorders: results from the Wave 2 National Epidemiologic Survey on Alcohol and Related Conditions. Mol Psychiatry. 2009;14(11):1051-1066. PubMed doi:10.1038/mp.2008.41
25. Grant BF, Dawson DA, Stinson FS, et al. The Alcohol Use Disorder and Associated Disabilities Interview Schedule-IV (AUDADIS-IV): reliability of alcohol consumption, tobacco use, family history of depression and psychiatric diagnostic modules in a general population sample. Drug Alcohol Depend. 2003;71(1):7-16. PubMed doi:10.1016/S0376-8716(03)00070-X
26. Ruan WJ, Goldstein RB, Chou SP, et al. The Alcohol Use Disorder and Associated Disabilities Interview Schedule-IV (AUDADIS-IV): reliability of new psychiatric diagnostic modules and risk factors in a general population sample. Drug Alcohol Depend. 2008;92(1-3):27-36. PubMed doi:10.1016/j.drugalcdep.2007.06.001
27. Muthen LK, Muthen BO. Mplus User’s Guide. Los Angeles, CA: Muthen and Muthen; 1998-2006.
28. Machin D, Cheung YB, Parmar M. Survival Analysis: A Practical Approach. 2nd ed. Chichester, UK: Wiley; 2006. doi:10.1002/0470034572
29. Dube SR, Felitti VJ, Dong M, et al. Childhood abuse, neglect, and household dysfunction and the risk of illicit drug use: the adverse childhood experiences study. Pediatrics. 2003;111(3):564-572. PubMed doi:10.1542/peds.111.3.564
30. Hu L, Bentler PM. Cutoff criteria for fit indexes in covariance structure analysis: conventional criteria versus new alternatives. Struct Equ Model A Multidiscip J. 1999;6(1):1-55. doi:10.1080/10705519909540118
31. Wall MM, Li R. Comparison of multiple regression to two latent variable techniques for estimation and prediction. Stat Med. 2003;22(23):3671-3685. PubMed doi:10.1002/sim.1588
32. Godfrey K. Statistics in practice: comparing the means of several groups. N Engl J Med. 1985;313(23):1450-1456. PubMed doi:10.1056/NEJM198512053132305
33. Hoertel N, Le Strat Y, Angst J, et al. Subthreshold bipolar disorder in a US national representative sample: prevalence, correlates and perspectives for psychiatric nosography. J Affect Disord. 2013;146(3):338-347. PubMed doi:10.1016/j.jad.2012.09.016
34. Pechtel P, Pizzagalli DA. Effects of early life stress on cognitive and affective function: an integrated review of human literature. Psychopharmacology (Berl). 2011;214(1):55-70. PubMed doi:10.1007/s00213-010-2009-2
35. Glaser JP, van Os J, Portegijs PJM, et al. Childhood trauma and emotional reactivity to daily life stress in adult frequent attenders of general practitioners. J Psychosom Res. 2006;61(2):229-236. PubMed doi:10.1016/j.jpsychores.2006.04.014
36. Heim C, Nemeroff CB. The role of childhood trauma in the neurobiology of mood and anxiety disorders: preclinical and clinical studies. Biol Psychiatry. 2001;49(12):1023-1039. PubMed doi:10.1016/S0006-3223(01)01157-X
37. McLaughlin KA, Conron KJ, Koenen KC, et al. Childhood adversity, adult stressful life events, and risk of past-year psychiatric disorder: a test of the stress sensitization hypothesis in a population-based sample of adults. Psychol Med. 2010;40(10):1647-1658. PubMed doi:10.1017/S0033291709992121
38. Etkin A, Schatzberg AF. Common abnormalities and disorder-specific compensation during implicit regulation of emotional processing in generalized anxiety and major depressive disorders. Am J Psychiatry. 2011;168(9):968-978. PubMed doi:10.1176/appi.ajp.2011.10091290
39. Goldstein RZ, Volkow ND. Dysfunction of the prefrontal cortex in addiction: neuroimaging findings and clinical implications. Nat Rev Neurosci. 2011;12(11):652-669. PubMed doi:10.1038/nrn3119
40. Mann JJ. Neurobiology of suicidal behaviour. Nat Rev Neurosci. 2003;4(10):819-828. PubMed doi:10.1038/nrn1220
41. Beck AT. Beyond belief: a theory of modes, personality and psychopathology. In: Salkovskis PM, ed. Frontiers in Cognitive Therapy. New York, NY: Guilford Press; 1996:1-25.
42. Teicher MH, Samson JA. Childhood maltreatment and psychopathology: a case for ecophenotypic variants as clinically and neurobiologically distinct subtypes. Am J Psychiatry. 2013;170(10):1114-1133. PubMed doi:10.1176/appi.ajp.2013.12070957
43. McGowan PO, Sasaki A, D’ Alessio AC, et al. Epigenetic regulation of the glucocorticoid receptor in human brain associates with childhood abuse. Nat Neurosci. 2009;12(3):342-348. PubMed doi:10.1038/nn.2270
44. Vranceanu AM, Hobfoll SE, Johnson RJ. Child multi-type maltreatment and associated depression and PTSD symptoms: the role of social support and stress. Child Abuse Negl. 2007;31(1):71-84. PubMed doi:10.1016/j.chiabu.2006.04.010
45. Brown J, Cohen P, Johnson JG, et al. Childhood abuse and neglect: specificity of effects on adolescent and young adult depression and suicidality. J Am Acad Child Adolesc Psychiatry. 1999;38(12):1490-1496. PubMed doi:10.1097/00004583-199912000-00009
46. Fergusson DM, Horwood LJ, Lynskey MT. Parental separation, adolescent psychopathology, and problem behaviors. J Am Acad Child Adolesc Psychiatry. 1994;33(8):1122-1131, discussion 1131-1133. PubMed doi:10.1097/00004583-199410000-00008
47. Afifi TO, Brownridge DA, Cox BJ, et al. Physical punishment, childhood abuse and psychiatric disorders. Child Abuse Negl. 2006;30(10):1093-1103. PubMed doi:10.1016/j.chiabu.2006.04.006
48. Brent DA, Baugher M, Bridge J, et al. Age- and sex-related risk factors for adolescent suicide. J Am Acad Child Adolesc Psychiatry. 1999;38(12):1497-1505. PubMed doi:10.1097/00004583-199912000-00010
49. Brent DA, Oquendo M, Birmaher B, et al. Familial pathways to early-onset suicide attempt: risk for suicidal behavior in offspring of mood-disordered suicide attempters. Arch Gen Psychiatry. 2002;59(9):801-807. PubMed doi:10.1001/archpsyc.59.9.801
50. Spataro J, Mullen PE, Burgess PM, et al. Impact of child sexual abuse on mental health: prospective study in males and females. Br J Psychiatry. 2004;184(5):416-421. PubMed doi:10.1192/bjp.184.5.416
51. Pérez-Fuentes G, Olfson M, Villegas L, et al. Prevalence and correlates of child sexual abuse: a national study. Compr Psychiatry. 2013;54(1):16-27. PubMed doi:10.1016/j.comppsych.2012.05.010
52. Aguilera M, Arias B, Wichers M, et al. Early adversity and 5-HTT/BDNF genes: new evidence of gene-environment interactions on depressive symptoms in a general population. Psychol Med. 2009;39(9):1425-1432. PubMed doi:10.1017/S0033291709005248
53. Kendler KS, Kuhn JW, Prescott CA. Childhood sexual abuse, stressful life events and risk for major depression in women. Psychol Med. 2004;34(8):1475-1482. PubMed doi:10.1017/S003329170400265X
54. Tottenham N, Sheridan MA. A review of adversity, the amygdala and the hippocampus: a consideration of developmental timing. Front Hum Neurosci. 2009;3:68. PubMed
55. Brown GW, Harris TO. Depression and the serotonin transporter 5-HTTLPR polymorphism: a review and a hypothesis concerning gene-environment interaction. J Affect Disord. 2008;111(1):1-12. PubMed doi:10.1016/j.jad.2008.04.009
56. Nestler EJ, Barrot M, DiLeone RJ, et al. Neurobiology of depression. Neuron. 2002;34(1):13-25. PubMed doi:10.1016/S0896-6273(02)00653-0
57. Roy A, Hodgkinson CA, Deluca V, et al. Two HPA axis genes, CRHBP and FKBP5, interact with childhood trauma to increase the risk for suicidal behavior. J Psychiatr Res. 2012;46(1):72-79. PubMed doi:10.1016/j.jpsychires.2011.09.009
58. Fergusson DM, Woodward LJ, Horwood LJ. Risk factors and life processes associated with the onset of suicidal behaviour during adolescence and early adulthood. Psychol Med. 2000;30(1):23-39. PubMed doi:10.1017/S003329179900135X
59. Talbot NL, Duberstein PR, Cox C, et al. Preliminary report on childhood sexual abuse, suicidal ideation, and suicide attempts among middle-aged and older depressed women. Am J Geriatr Psychiatry. 2004;12(5):536-538. PubMed doi:10.1097/00019442-200409000-00014
60. Vajda J, Steinbeck K. Factors associated with repeat suicide attempts among adolescents. Aust N Z J Psychiatry. 2000;34(3):437-445. PubMed doi:10.1080/j.1440-1614.2000.00712.x
61. Ystgaard M, Hestetun I, Loeb M, et al. Is there a specific relationship between childhood sexual and physical abuse and repeated suicidal behavior? Child Abuse Negl. 2004;28(8):863-875. PubMed doi:10.1016/j.chiabu.2004.01.009
62. Pagura J, Cox BJ, Sareen J, et al. Factors associated with multiple versus single episode suicide attempts in the 1990-1992 and 2001-2003 United States national comorbidity surveys. J Nerv Ment Dis. 2008;196(11):806-813. PubMed doi:10.1097/NMD.0b013e31818b6a77
63. Forman EM, Berk MS, Henriques GR, et al. History of multiple suicide attempts as a behavioral marker of severe psychopathology. Am J Psychiatry. 2004;161(3):437-443. PubMed doi:10.1176/appi.ajp.161.3.437
64. Andover MS, Zlotnick C, Miller IW. Childhood physical and sexual abuse in depressed patients with single and multiple suicide attempts. Suicide Life Threat Behav. 2007;37(4):467-474. PubMed doi:10.1521/suli.2007.37.4.467
65. Br×¥dvik L, Berglund M. Repetition and severity of suicide attempts across the life cycle: a comparison by age group between suicide victims and controls with severe depression. BMC Psychiatry. 2009;9(1):62. PubMed doi:10.1186/1471-244X-9-62
66. Scoliers G, Portzky G, van Heeringen K, et al. Sociodemographic and psychopathological risk factors for repetition of attempted suicide: a 5-year follow-up study. Arch Suicide Res. 2009;13(3):201-213. PubMed doi:10.1080/13811110902835130
67. Mikton C, Butchart A. Child maltreatment prevention: a systematic review of reviews. Bull World Health Organ. 2009;87(5):353-361. PubMed doi:10.2471/BLT.08.057075
68. Anda RF, Felitti VJ, Bremner JD, et al. The enduring effects of abuse and related adverse experiences in childhood: a convergence of evidence from neurobiology and epidemiology. Eur Arch Psychiatry Clin Neurosci. 2006;256(3):174-186. PubMed doi:10.1007/s00406-005-0624-4
69. Hardt J, Rutter M. Validity of adult retrospective reports of adverse childhood experiences: review of the evidence. J Child Psychol Psychiatry. 2004;45(2):260-273. PubMed doi:10.1111/j.1469-7610.2004.00218.x
70. Fergusson DM, Horwood LJ, Woodward LJ. The stability of child abuse reports: a longitudinal study of the reporting behaviour of young adults. Psychol Med. 2000;30(3):529-544. PubMed doi:10.1017/S0033291799002111
71. Widom C, Morris S. Accuracy of adult recollections of childhood victimization, part 2: childhood sexual abuse. Psychol Assess. 1997;9(1):34-46. doi:10.1037/1040-3590.9.1.34
72. Widom CS, Shepard RL. Accuracy of adult recollections of childhood victimization, part 1: childhood physical abuse. Psychol Assess. 1996;8(4):412-421. doi:10.1037/1040-3590.8.4.412
73. Le Strat Y, Hoertel N. Correlation is no causation: gymnasium proliferation and the risk of obesity. Addiction. 2011;106(10):1871-1872. PubMed doi:10.1111/j.1360-0443.2011.03547.x
74. Wagner BM. Family risk factors for child and adolescent suicidal behavior. Psychol Bull. 1997;121(2):246-298. PubMed doi:10.1037/0033-2909.121.2.246