See original letter by Wakefield and Schmitz.
Dr Gilman and Colleagues Reply
To the Editor: We appreciate the interest of Drs Wakefield and Schmitz in our study of the bereavement exclusion in major depressive disorder (MDD).1 In fact it was Wakefield and colleagues’ prior work on this issue2,3 that motivated our study.
The crux of their letter is that our ability to identify cases of complicated bereavement was compromised by methodological decisions and by the structure of the National Epidemiologic Survey on Alcohol and Related Conditions (NESARC) interview, both of which distort our findings and invalidate our conclusions. Most importantly, they criticized our inclusion of multiepisode depression cases; they also suggested that we should have used the NESARC’s "feeling worthless" item to determine the presence of "morbid preoccupation with worthlessness." To be sure, the NESARC is not the perfect dataset for validating the diagnostic criteria for MDD, and we addressed many of its shortcomings in the Limitations section of our article.
Briefly, the NESARC assessed the detailed symptoms of depression that were present during participants’ worst episode of mood disturbance. As a result, only for the single-episode cases could it be established whether or not a bereavement-related depression was or was not accompanied by DSM-IV "complicated" symptoms (eg, psychomotor retardation). With respect to worthlessness, the DSM-IV complicated symptom of "morbid preoccupation with worthlessness" signifies a much greater degree of severity than is indicated by the Criterion A symptom of "feelings of worthlessness"; we thought it dubious to use the "worthlessness" item to infer the presence of morbid preoccupation.
Drs Wakefield and Schmitz raise concerns that warrant further evaluation. Therefore, we reanalyzed the NESARC data, retaining only single-episode cases of depression. Of the 8,626 cases meeting symptom criteria for a depressive episode analyzed in our original report, 4,141 (weighted percent = 47.8) experienced a single lifetime episode. Of these single-episode cases, 131 were excluded from a DSM-IV diagnosis due to bereavement and 350 were included as DSM-IV cases despite concurrent bereavement due to symptom severity (ie, complicated bereavement). Following Drs Wakefield and Schmitz, we reclassified 24 of the 131 bereavement-excluded cases that reported "feelings of worthlessness" into the complicated bereavement group. Thus, of all single-episode cases, 88.8% were categorized as major depressive episode (MDE), 2.5% were categorized as bereavement-excluded depression, and 8.7% were categorized as complicated bereavement (bereavement-related depression that qualified for MDE because of severity or duration).
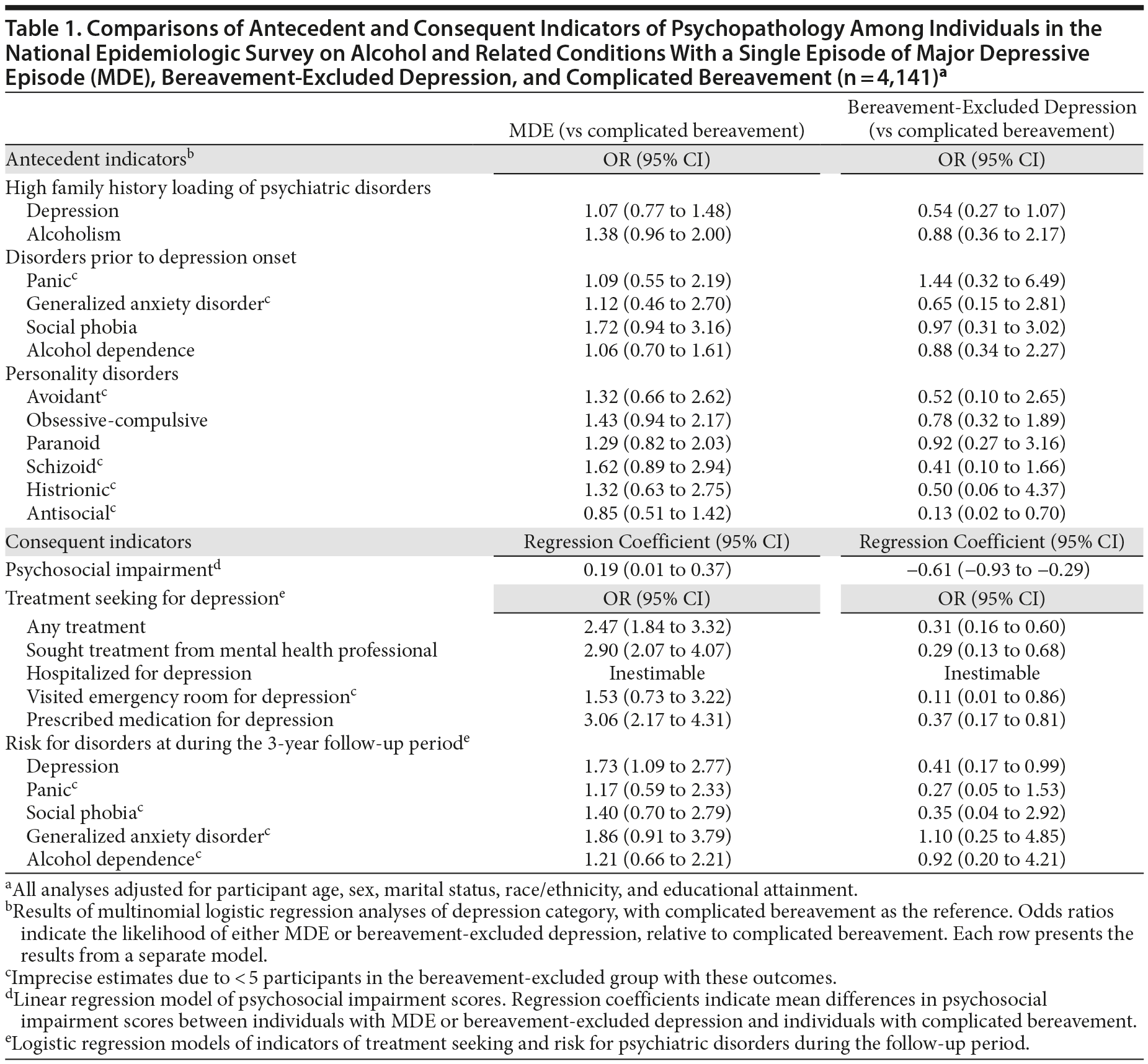
We used the same analytic methods as in our original report, but to address Drs Wakefield and Schmitz, we used complicated bereavement as the reference group (Table 1). In the comparisons of bereavement-excluded depression with complicated bereavement (what Drs Wakefield and Schmitz refer to as "complicated"/"uncomplicated" comparisons, presented in column 2), bereavement-excluded depression did not differ from complicated bereavement on any of the antecedent indicators except that the bereavement-excluded group had a lower odds of prior antisocial personality disorder. In terms of the consequent indicators, the bereavement-excluded group reported a lower level of psychosocial impairment, was less likely to seek depression treatment, and had a lower risk for major depression during the follow-up interview 3 years later.
In the comparisons of MDE with complicated bereavement (in column 1), there were no significant differences on any of the antecedent indicators. In the analyses of consequent indicators, the MDE group reported slightly more impairment, was more likely to seek treatment, and had a higher odds of major depression during the follow-up interview.
Thus, when limited to single-episode cases, bereavement-excluded depression could be viewed as "less pathological" than complicated bereavement in terms of its prospective course, but not in terms of its preexisting vulnerability. In contrast, MDE could be viewed as "more pathological" than complicated bereavement in terms of its prospective course, but also not in terms of preexisting vulnerability. One could argue whether the antecedent or consequent validator comparisons should be given equal weight; perhaps the consequent outcomes might be viewed as more important clinically. However, in terms of diagnostic validation, this issue remains uncertain. We therefore interpret these results as providing at best equivocal support for the validity of the DSM-IV criteria for complicated bereavement.4 This is because the DSM-IV framework does not anticipate substantial differences between complicated bereavement and MDE, which we observed, but does anticipate differences between complicated bereavement and bereavement-excluded depression, which we observed in part. These findings suggest that the DSM-IV criteria do not function entirely as intended, specifically with respect to weaknesses in the definition of "complicated bereavement."4 The approach we used remains an indirect one, however, and diagnostic validator comparisons alone cannot provide definitive evidence regarding the boundaries between disorder and non-disorder.
Our study provided an additional result that bears on the bereavement debate—the societal impact of eliminating it. The DSM-IV bereavement exclusion removed only 2.3% of all individuals meeting symptomatic criteria for MDE from a diagnosis. If we were to exempt individuals with a past history of depression from the bereavement exclusion, as Wakefield and First recently proposed,5 the bereavement exclusion would remove only 1.2% of all depressive episodes that would otherwise meet diagnostic criteria for MDE based on symptoms, 2-week duration, and clinical significance. Therefore, the fears that have been expressed,3 particularly on the Internet and in the popular press, regarding a dramatic expansion of psychiatric diagnosis and treatment that would occur following the elimination of the bereavement exclusion seem profoundly overstated. (cf, "Anyone with depressive symptoms for just two weeks after suffering a significant loss would be diagnosed with major depressive disorder, massively pathologizing normal intense grief."6 ‘ ¦ "We can look forward ‘ ¦ to a time when medication will be given more routinely to people who are grieving; even when they have a relatively mild depressive feeling during that grief."7).
In light of our study’s equivocal support for the DSM-IV‘s bereavement-exclusion/complicated-bereavement exception, we commented that removing the bereavement exclusion would eliminate a diagnostic criterion that is largely inconsistent with DSM‘s "descriptive approach that attempted to be neutral with respect to theories of etiology."8(pxxvi) That is because the bereavement exclusion assumes a causal relationship between the loss of a loved one and a depressive episode, an assumption predominantly guided by theories of stress and mental illness.9 Basing the diagnostic criteria on specific causal models was common in early versions of the DSM (eg, depressive neurosis in DSM-II was defined as "an excessive reaction of depression due to an internal conflict or to an identifiable event such as the loss of a love object or cherished possession"10[p40]), but was essentially abandoned by DSM-III. We agree with Wakefield and his colleagues that social context is an important consideration in defining the pathological significance of depressive symptoms and that aspects of social context, including the loss of a loved one, are important determinants of the onset and clinical course of major depression.11-13 We believe that psychiatry should strive to move beyond a purely descriptive nosology to one based on etiology. Unfortunately, our results suggest that the validity of the current distinction between uncomplicated and complicated bereavement remains unclear.
References
1. Gilman SE, Breslau J, Trinh NH, et al. Bereavement and the diagnosis of major depressive episode in the National Epidemiologic Survey on Alcohol and Related Conditions. J Clin Psychiatry. 2012;73(2):208-215. PubMed doi:10.4088/JCP.10m06080
2. Wakefield JC, Schmitz MF, First MB, et al. Extending the bereavement exclusion for major depression to other losses: evidence from the National Comorbidity Survey. Arch Gen Psychiatry. 2007;64(4):433-440. PubMed doi:10.1001/archpsyc.64.4.433
3. Horwitz AV, Wakefield JC. The Loss of Sadness: How Psychiatry Transformed Normal Sorrow into Depressive Disorder. New York, NY: Oxford University Press; 2007.
4. Gilman SE, Breslau J, Trinh NH, et al. Epidemiologic evidence concerning the bereavement exclusion in major depression. Arch Gen Psychiatry. 2012;69(11):1179-1180, author reply 1180-1181. PubMed doi:10.1001/archgenpsychiatry.2012.383
5. Wakefield JC, First MB. Validity of the bereavement exclusion to major depression: does the empirical evidence support the proposal to eliminate the exclusion in DSM-5? World Psychiatry. 2012;11(1):3-10. PubMed doi:10.1016/j.wpsyc.2012.01.002
6. Wakefield JC. Psychiatry’s conceptual malpractice. http://www.project-syndicate.org/commentary/psychiatry-s-conceptual-malpractice. Updated June 24, 2010. Accessed January 22, 2013.
7. Cornish A, Block M. Psychiatrists to take new approach in bereavement [Jerome Wakefield interview]. All Things Considered. http://www.npr.org/2012/12/06/166682774/psychiatrists-to-take-new-approach-in-bereavement Updated December 6, 2012. Accessed January 22, 2013.
8. American Psychiatric Association. Diagnostic and Statistical Manual of Mental Disorders. Fourth Edition, Text Revision. Washington, DC: American Psychiatric Association; 2000.
9. Dohrenwend BP. The role of adversity and stress in psychopathology: some evidence and its implications for theory and research. J Health Soc Behav. 2000;41(1):1-19. PubMed doi:10.2307/2676357
10. American Psychiatric Association. Diagnostic and Statistical Manual of Mental Disorders, Second Edition. Washington, DC: American Psychiatric Association; 1968.
11. Boelen PA. A prospective examination of the association between the centrality of a loss and post-loss psychopathology. J Affect Disord. 2012;137(1-3):117-124. PubMed doi:10.1016/j.jad.2011.12.004
12. Gilman SE, Trinh NH, Smoller JW, et al. Psychosocial stressors and the prognosis of major depression: a test of Axis IV. Psychol Med. 2013;43(2):303-316. PubMed
13. Gilman SE, Dupuy JM, Perlis RH. Risks for the transition from major depressive disorder to bipolar disorder in the National Epidemiologic Survey on Alcohol and Related Conditions. J Clin Psychiatry. 2012;73(6):829-836. PubMed doi:10.4088/JCP.11m06912
Author affiliations: Department of Society, Human Development, and Health (Dr Gilman) and Department of Epidemiology (Drs Gilman, Murphy, and Smoller), Harvard School of Public Health; Department of Psychiatry, Massachusetts General Hospital and Harvard Medical School (Drs Trinh, Fava, Murphy, and Smoller), Boston; and RAND Corporation, Pittsburgh, Pennsylvania (Dr Breslau).
Potential conflicts of interest:Dr Fava reports several potential conflicts of interest, all of which are listed in the original article referred to in this letter. Drs Gilman, Breslau, Trinh, Murphy, and Smoller have no conflicts of interest to report.
Funding/support: The work reported in the original article referred to in this letter was supported in part by National Institutes of Health grants MH087544, DA080887, and MH66057 .
J Clin Psychiatry 2013;74(7):741-743 (doi:10.4088/JCP.12lr08310a).
© Copyright 2013 Physicians Postgraduate Press, Inc.