J Clin Psychiatry 2021;82(2):20l13702
To cite: Porras-Segovia A, Baca-García E, Courtet P, et al. If suicide were COVID-19: a neglected cause of premature death. J Clin Psychiatry. 2021;82(2):20l13702.
To share: https://doi.org/10.4088/JCP.20l13702
© Copyright 2021 Physicians Postgraduate Press, Inc.
aInstituto de Investigación Sanitaria Fundación Jiménez Díaz, Madrid, Spain
bDepartment of Emergency Psychiatry and Acute Care, CHU Montpellier, University of Montpellier, Montpellier, France
cNew York State Psychiatric Institute, Columbia University, New York, New York
dPerelman School of Medicine, University of Pennsylvania, Philadelphia, Pennsylvania
eDepartment of Psychiatry, Hospital Universitario Fundación Jiménez Díaz, Madrid, Spain
fDepartment of Psychiatry, University Hospital Rey Juan Carlos, Mostoles, Spain
gDepartment of Psychiatry, General Hospital of Villalba, Madrid, Spain
hDepartment of Psychiatry, University Hospital Infanta Elena, Valdemoro, Spain
iDepartment of Psychiatry, Madrid Autonomous University, Madrid, Spain
jCIBERSAM (Centro de Investigacion Biomédica en Red Salud Mental), Carlos III Institute of Health, Madrid, Spain
kUniversidad Catolica del Maule, Talca, Chile
lDepartment of Psychiatry, Centre Hospitalier Universitaire de Nîmes, Nîmes, France
To the Editor:
A sad soul can kill you quicker, far quicker, than a germ.
—John Steinbeck
In the year since the start of the pandemic (as of January 19, 2021), coronavirus disease 2019 (COVID-19) has claimed 2,057,095 lives worldwide, while the number of cases exceeds 95 million.1 According to data from the World Health Organization, suicide accounts for about 800,000 deaths worldwide every year, while the number of suicide attempts may be more than 20 times higher, or more than 16 million suicide attempts every year.2
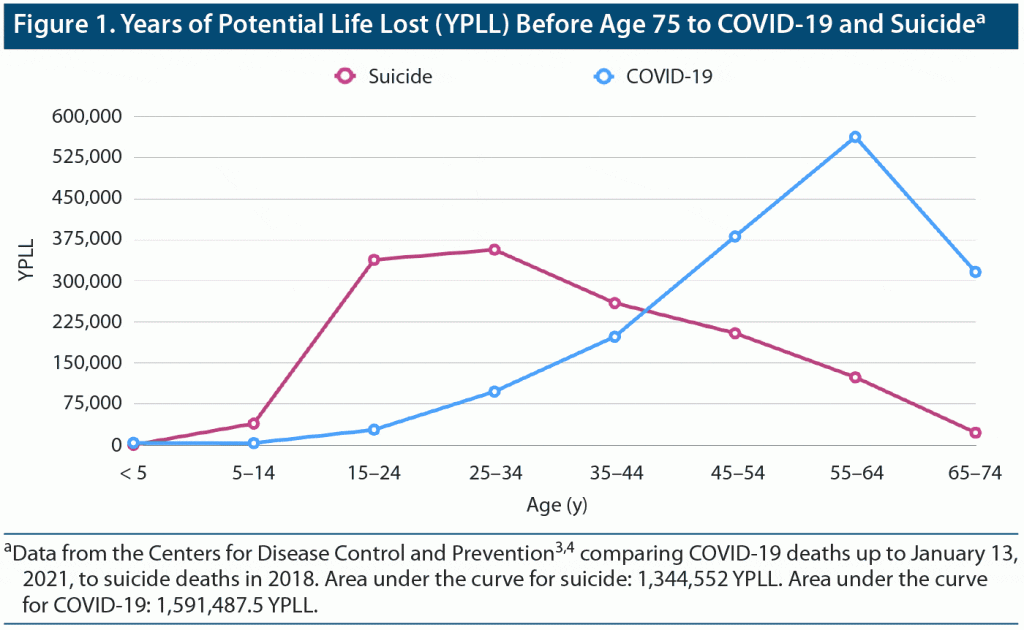
Focusing on the US, as of January 13, 2021, 329,593 COVID-19 deaths have been reported,3 compared with the 47,096 deaths by suicide that occurred in the whole of 2018.4 However, an estimation using data from the Centers for Disease Control and Prevention reveals that COVID-19 has resulted in 1,591,487.5 years of potential life lost (YPLL) before age 75 in the US,3 while suicide resulted in 1,344,552 YPLL in 20184 (Figure 1).
To understand the social impact of these two conditions, we must consider the age at which death occurs.5 Most of the COVID-19 victims were 85 years or older,3 and they often had a history of chronic physical conditions, especially respiratory diseases.3 By comparison, suicide is the second leading cause of death among 15- to 29-year-olds,2 and up to 90% of victims had a history of mental illness, most frequently depressive disorders.6 Both the COVID-19 pandemic and suicidal behavior are major public health issues, and COVID-19 has appropriately received unprecedented attention in public health, biomedical research, and the media, while suicidal behavior continues to be neglected. There is no doubt that COVID-19 is one of the greatest health challenges we have ever faced, but suicide also requires a sustained and effortful attention that continues to be denied. Suicidal behavior has been so neglected that rates of suicide in the US have dramatically increased by 35% between 1999 and 2018.4
This comparative grievance is not exclusive to COVID-19. It is normative for physical health to absorb more clinical and research resources than mental health. A 2014 Nature article highlighted this disparity using cancer and depression as examples, stating: “If the extent of human suffering were used to decide which diseases deserve the most medical attention, then depression would be near the top of the list.”7
This disparity in resource deployment is especially notable in the case of COVID-19 because prevention measures aimed at combating the pandemic may increase suicidal behavior.8,9 In addition to the increased social isolation and economic consequences of the pandemic, face-to-face mental health care has been hampered or disrupted, further exacerbating the situation of psychiatric patients.10 COVID-19 prevention measures are fully justified by the severity of the situation and the risk of massive contagion, but we must do our best to minimize their impact on other areas. Moreover, while we are hopeful that the recent development of vaccines will soon rid us of the COVID-19 pandemic, suicide has remained a leading cause of death for decades, and we have not yet been able to provide effective prevention measures. The sustained mortality rates and the direct and indirect economic costs of suicide generate an overwhelming cumulative impact over time.
Both COVID-19 and suicide are preventable. Studies show that a large number of deaths from COVID-19 could be avoided by the use of a face mask.11 Suicide prevention measures undertaken in Denmark in recent decades—a combination of restriction of access to lethal means and specific clinical programs—have resulted in a substantial decrease in suicide attempts: from 38 attempts per 100,000 people in 1980 to 11.4 per 100,000 in 2007.12
The disparity in resources for addressing suicide and COVID-19 is evidence of an unexplained gap that still exists between concern for physical illness and concern for mental illness. In the late 20th century, HIV infection was one of the leading causes of YPLL in the US.13 Thanks to the development of antiretroviral therapies, life expectancy of those infected with HIV now resembles that of the general population.14 This increase is proof that when public and private health systems devote themselves to solving a health problem, mortality rates drop dramatically. We are still waiting for society to show the same degree of concern for suicide.
Published online: February 23, 2021.
Potential conflicts of interest: The authors declare they have no conflicts of interest.
Funding/support: This work received grant support from Instituto de Salud Carlos III (cofunded by European Regional Development Fund/European Social Fund) (CM19/00026), Ministerio de Ciencia, Innovación y Universidades (RTI2018-099655-B-I00), and Comunidad de Madrid (Y2018/TCS-4705).
Role of the sponsor: The supporters had no role in the writing or publication of this letter.
Disclaimer: Dr Courtet, JCP’s “Focus on Suicide” Section Editor, was not involved in the editorial review or decision to publish this letter.
References (14)

- Coronavirus cases and deaths. Worldometer. Accessed January 19, 2021. https://www.worldometers.info/coronavirus/
- Suicide: key facts. World Health Organization. Accessed January 19, 2021. https://www.who.int/news-room/fact-sheets/detail/suicide/
- Weekly updates by select demographic and geographic characteristics: provisional death counts for coronavirus disease 2019 (COVID-19). Centers for Disease Control and Prevention. Accessed January 19, 2021. https://www.cdc.gov/nchs/nvss/vsrr/covid_weekly/index.htm
- WISQARS Leading Causes of Death Reports, 1981–2018. Centers for Disease Control and Prevention. Accessed January 19, 2021. https://webappa.cdc.gov/sasweb/ncipc/leadcause.html
- Gardner JW, Sanborn JS. Years of potential life lost (YPLL): what does it measure? Epidemiology. 1990;1(4):322–329. PubMed CrossRef NLM
- Oquendo MA, Baca-Garcia E. Suicidal behavior disorder as a diagnostic entity in the DSM-5 classification system: advantages outweigh limitations. World Psychiatry. 2014;13(2):128–130. PubMed CrossRef NLM
- Ledford H. Medical research: if depression were cancer. Nature. 2014;515(7526):182–184. PubMed CrossRef NLM
- Kawohl W, Nordt C. COVID-19, unemployment, and suicide. Lancet Psychiatry. 2020;7(5):389–390. PubMed CrossRef NLM
- Reger MA, Stanley IH, Joiner TE. Suicide mortality and coronavirus disease 2019: a perfect storm? JAMA Psychiatry. 2020;77(11):1093–1094. PubMed CrossRef NLM
- Moreno C, Wykes T, Galderisi S, et al. How mental health care should change as a consequence of the COVID-19 pandemic. Lancet Psychiatry. 2020;7(9):813–824. PubMed CrossRef NLM
- Brooks JT, Butler JC, Redfield RR. Universal masking to prevent SARS-CoV-2 transmission: the time is now. Published online July 14, 2020. JAMA. PubMed CrossRef NLM
- Nordentoft M, Erlangsen A. Suicide: turning the tide. Science. 2019;365(6455):725. PubMed CrossRef NLM
- Selik RM, Chu SY. Years of potential life lost due to HIV infection in the United States. AIDS. 1997;11(13):1635–1639. PubMed CrossRef NLM
- How far have we come on AIDS? World Health Organization. November 27, 2018. Accessed January 19, 2021. https://www.who.int/westernpacific/news/commentaries/detail-hq/how-far-have-we-come-on-aids
This PDF is free for all visitors!