See more Academic Highlights in this series: Part 2 | Part 3
This Academic Highlights section of The Journal of Clinical Psychiatry presents the highlights of the virtual roundtable “Patient Functioning and Life Engagement: Unmet Needs in MDD and Schizophrenia,” which was held May 10, 2022.
The roundtable was chaired by Christoph U. Correll, MD, Zucker School of Medicine at Hofstra/Northwell, Hempstead, New York, and Charité Universitätsmedizin, Berlin, Germany. The faculty were Zahinoor Ismail, MD, Department of Psychiatry, Hotchkiss Brain Institute, Cumming School of Medicine, University of Calgary, Calgary, Alberta, Canada; Roger S. McIntyre, MD, Mood Disorder Psychopharmacology Unit, University Health Network, Department of Psychiatry, University of Toronto; Institute of Medical Science, University of Toronto; and Departments of Psychiatry and Pharmacology, University of Toronto, Toronto, Ontario, Canada; Roueen Rafeyan, MD, Department of Psychiatry, Feinberg School of Medicine, Northwestern University, Chicago, Illinois; and Michael E. Thase, MD, Department of Psychiatry, Perelman School of Medicine of the University of Pennsylvania, and the Corporal Michael J. Crescenz Veterans Affairs Medical Center, Philadelphia, Pennsylvania.
Financial disclosures: Dr Correll has stock options in Cardio Diagnostics, Mindpax, and LB Pharma; has received consulting fees from AbbVie, Acadia, Alkermes, Allergan, Angelini, Axsome, Cardio Diagnostics, Cerevel, Compass Pathways, Gedeon Richter, Holmusk, IntraCellular Therapies, Janssen/J&J, Karuna, LB Pharma, Lundbeck, MedAvante-ProPhase, MedInCell, Medscape, Merck, Mindpax, Mylan, Neurocrine, Noven, Otsuka, Pfizer, Pharmabrain, PPD Biotech, Recordati, Relmada, Rovi, Seqirus, Servier, SK Life Science, Sumitomo Dainippon, Sunovion, Supernus, Takeda, Teva, and Viatris; has received grant/research support from Janssen and Takeda; has received honoraria for speaking/teaching from AbbVie, Acadia, Alkermes, Allergan, Angelini, Axsome, Compass, Gedeon Richter, IntraCellular Therapies, Janssen/J&J, Karuna, LB Pharma, Lundbeck, MedAvante-ProPhase, MedInCell, Merck, Mylan, Neurocrine, Noven, Otsuka, Recordati, Rovi, Seqirus, Servier, SK Life Science, Sumitomo Dainippon, Sunovion, Supernus, Takeda, Teva, and Viatris; has received advisory board fees from AbbVie, Acadia, Alkermes, Allergan, Angelini, Axsome, Compass, Gedeon Richter, IntraCellular Therapies, Janssen/J&J, Karuna, LB Pharma, Lundbeck, MedAvante-ProPhase, MedInCell, Merck, Mylan, Neurocrine, Noven, Otsuka, Recordati, Rovi, Seqirus, Servier, SK Life Science, Sumitomo Dainippon, Sunovion, Supernus, Takeda, Teva, and Viatris; and has received other financial/material support from UpToDate. Dr Ismail has received consulting fees from Otsuka/Lundbeck. Dr McIntyre is a CEO of Braxia Scientific Corp.; has received speaking/consulting fees from Lundbeck, Janssen, Alkermes, Mitsubishi Tanabe, Purdue, Pfizer, Otsuka, Takeda, Neurocrine, Sunovion, Bausch Health, Novo Nordisk, Kris, Sanofi, Eisai, Intra-Cellular, NewBridge Pharmaceuticals, Abbvie, and Atai Life Sciences; and has received research grant support from CIHR/GACD/National Natural Science Foundation of China (NSFC). Dr Rafeyan has received honoraria for speaking/teaching from Otsuka, Sunovion, Takeda, Allergan, AbbVie, Intracellular, Neurocrine, Teva, and Alkermes. Dr Thase is an employee of the Perelman School of Medicine at the University of Pennsylvania; has received consulting fees from Acadia, Akili, Alkermes, Allergan, Axsome Therapeutics, BioHaven, Bocemtium Consulting, Boehringer Ingelheim International, CatalYm GmbH, Clexio Biosciences, Gerson Lehrman Group, H. Lundbeck A/S, Jazz Pharmaceuticals, Janssen, Johnson & Johnson, Luye Pharma Group, Merck & Company, Otsuka Pharmaceutical Company, Ltd, Pfizer, Sage, Seelos, Sunovion, and Takeda; has received grant/research support from Acadia, Allergan, AssureRx Health, Axsome Therapeutics, BioHaven, Intracellular, Johnson & Johnson, Otsuka Pharmaceutical Company, Ltd, Patient-Centered Outcomes Research Institute (PCORI), and Takeda; and has received royalties from American Psychiatric Foundation, Guilford Publications, Herald House, Wolters-Kluwer, and W.W. Norton & Company. His spouse is employed by Peloton Advantage.
This evidence-based peer-reviewed Academic Highlights was prepared by Healthcare Global Village, Inc. Financial support for preparation and dissemination of this Academic Highlights was provided by H. Lundbeck A/S and Otsuka Product Development and Commercialization. The faculty acknowledges Sarah Brownd, MA, ELS, for editorial assistance in developing the manuscript. The opinions expressed herein are those of the faculty and do not necessarily reflect the views of Healthcare Global Village, Inc., the publisher, or the commercial supporters. This article is distributed by H. Lundbeck A/S and Otsuka Product Development and Commercialization for educational purposes only.
J Clin Psychiatry 2022;83(4):LU21112AH1
To cite: Correll CU, Ismail Z, McIntyre RS, et al. Patient functioning and life engagement: unmet needs in major depressive disorder and schizophrenia. J Clin Psychiatry. 2022;83(4):LU21112AH1
To share: https://doi.org/10.4088/JCP.LU21112AH1
© 2022 Physicians Postgraduate Press, Inc.
Definitions of treatment success used in clinical trials of medications for serious mental illness have generally focused on reduction in symptoms assessed via observer-rated instruments such as the Montgomery-Asberg Depression Rating Scale and the Hamilton Depression Rating Scale in MDD and the Positive and Negative Syndrome Scale (PANSS) and Brief Psychiatric Rating Scale in schizophrenia. In recent years, there has been a shift toward incorporating outcomes into clinical research that are patient-reported and reflect outcomes and goals that are meaningful to the patient.1,2 These outcomes include aspects of functioning (eg, activities of daily living and role fulfillment),3 as well as life engagement, which interacts with symptomatic and functional outcomes and encompasses aspects such as motivation and vitality.
In a recent roundtable meeting, a panel of 5 experts discussed life engagement and its relationship to symptoms and functioning in patients with major depressive disorder (MDD) and schizophrenia. This Academic Highlights summarizes their discussion.
LIFE ENGAGEMENT
In the context of mental health, patient life engagement consists of positive health aspects relating to cognition (including “hot” cognition, ie, cognition colored by emotion), vitality, motivation, and reward, and the ability to feel pleasure.4 Research has demonstrated associations between life engagement and increased well-being and decreased psychological distress.5 Functional outcomes associated with life engagement include a sense of perceived significance and fulfillment of one’s life and participation in valued and meaningful activities.6 Dr Correll characterized life engagement as involving the entire person and having behavioral, emotional, and cognitive aspects, as well as a higher level of meaning and purpose. He explained that the essence of engagement is to connect with the world and others and to regain a sense of self that often becomes eroded by mental illness and its symptoms.
Life Engagement in MDD Patients
Life engagement as a treatment goal addresses MDD symptomatology: among patients with inadequate response to antidepressants, lack of motivation, a key aspect of life engagement, is the most common non-core symptom,7 and anhedonia scores are especially elevated in patients with unremitted MDD compared with other illnesses.8 Further, as demonstrated in a survey by the Depression and Bipolar Support Alliance, patients indicate that aspects of life engagement reflect outcomes that are important to them.9 Another survey comparing the outcomes that physicians and patients consider important in remission from depression showed that the items ranked most important by physicians mostly reflected absence of depressive symptoms, while those highly ranked by patients tended to reflect positive affect.10
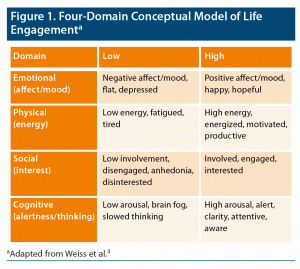
To capture the essential elements of life engagement, exit interview data were pooled from 3 open-label studies11–13 of adjunctive brexpiprazole in MDD patients with inadequate response to antidepressants. The interviews assessed patients’ experiences with MDD prior to the trials and their perception of treatment benefits after finishing the trials. Vocabulary used in the 105 transcripts was reviewed, and, in consultation with a panel of expert psychiatrists, a model of life engagement was developed.4 The model consists of 4 domains: emotional (affect/mood), physical (energy), social (interest), and cognitive (alertness/thinking). Figure 1 shows this conceptual framework for life engagement. Based on the roundtable discussion, Dr Correll proposed expanding the model to include a fifth domain, Identity (meaning/purpose/belonging), with low levels characterized by a sense of isolation, fragmentation, lack of purpose, and disconnectedness and high levels characterized by a sense of belonging, meaning, self-efficacy, and connectedness.
Clinical picture. Regarding the clinical profile of a patient who is disengaged, Dr McIntyre acknowledged that there is not a singular phenotype for disengagement in depression. However, in his experience, lassitude, or apathy, is a defining feature of the commonly encountered patient who presents with disengagement at his clinic. He explained that, in these patients, maladaptive behaviors such as substance use may be a proxy for disengagement:
As to the profile of an MDD patient who is engaged with life, positive valence was cited by Dr Thase as an important component: “Positive affect; the sense that one can feel something that is joyful to experience, close to a peak experience; and the ability to engage in a warm and well-related fashion. The feelings go beyond being functionally back to one’s better self. In describing life engagement, I think of terms like ‘lit up,’ meaning alive and full of life.”
Life Engagement in Patients With Schizophrenia
Life engagement encompasses outcomes that are important to patients with schizophrenia as well.14 A study of 105 schizophrenia outpatients revealed that their most valued goals for treatment included improved cognition, satisfaction, and independence.4,15
To investigate whether the 4-domain model of life engagement developed from MDD exit interview data would also resonate with patients with schizophrenia, qualitative interviews were conducted with adults with schizophrenia who were receiving maintenance treatment with an antipsychotic.16 Patients spontaneously described their understanding of life engagement and then evaluated the relevance of the 4-domain conceptual model of life engagement. A majority of the patients, 64%, provided a definition of life engagement that aligned with the study definition. When presented with the 4-domain model of life engagement previously identified from exit interviews with MDD patients, 96% of the patients felt that all 4 domains were important to life engagement.16
Clinical picture. In describing the clinical picture of a patient engaged with life, Dr Rafeyan mentioned a patient of his with schizophrenia for whom the journey to find appropriate medications has been difficult. Although the patient’s symptoms are stabilized, he still experiences residual symptoms including auditory hallucinations. However, he regularly attends a day program, and when he comes for office visits, he has a bright, neat outfit on, his eyes are “smiling,” and he has excitement about his life and what he is doing. Dr Rafeyan stated that, as a clinician, this is a major turning point for him in terms of the patient’s treatment journey. As a point of contrast, he said that he often sees patients for whom symptoms are fairly well controlled, but their interaction with their surroundings, their family, and their peers and colleagues is minimal, and there is no excitement; those patients are disengaged with life.
SYMPTOMATIC IMPROVEMENT AND LIFE ENGAGEMENT
Symptom control plays a critical role in determining patients’ quality of life, and recent longitudinal data demonstrated the influence of symptoms on subjective satisfaction and interest in life.17 However, symptom control has been shown to be only one factor affecting quality of life. Data based on patient-reported outcomes from the Sequenced Treatment Alternatives to Relieve Depression (STAR*D) study indicated that after treatment, > 50% of MDD patients continued to experience severely impaired quality of life, and, even among patients in remission, 32% continued to experience reduced quality of life.18 A systematic review19 identifying domains important to people with serious mental illness found that although symptoms, or “ill-being,” were an intrinsic aspect of quality of life, others included feeling in control and having autonomy, a positive self-image, a sense of belonging, engagement in meaningful and enjoyable activities, and hope and optimism.
The roundtable participants agreed that, in terms of chronology, symptom improvement must happen first or at least concurrently with the improvement of functioning and life engagement. For both MDD20 and schizophrenia,21 “time is brain,” and the longer symptoms go untreated, the harder it is to improve to a point where one can engage. Dr Ismail explained that although focusing on symptoms is important in the acute phase, other factors emerge later in the treatment journey as important to the patient’s sense of wellness:
Although the relationship between symptomatic outcomes and life engagement outcomes is fluid, Dr Correll stated,
Clinical picture. Dr Ismail provided a profile of a patient with schizophrenia who, despite symptom reduction, has incomplete functional improvement and a lack of life engagement:
FUNCTIONING AND LIFE ENGAGEMENT
Functional Improvement
For both schizophrenia and MDD, life engagement is intertwined with patient functioning, since it reflects the functional outcomes of life fulfillment, well-being, and participation in activities that are meaningful to the individual.4,6 Although related, functioning and life engagement differ; functioning is a broader term centered on role fulfillment and performance of activities in a social context,22 while life engagement is more closely related to quality of life and grounded in a subjective sense of connection with others, as well as the ability to experience pleasure.
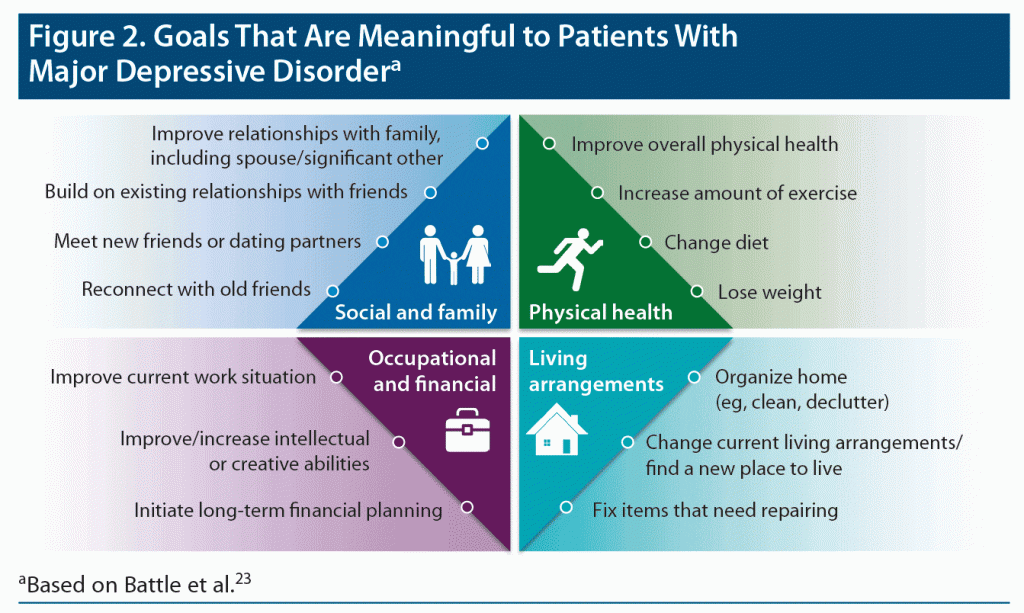
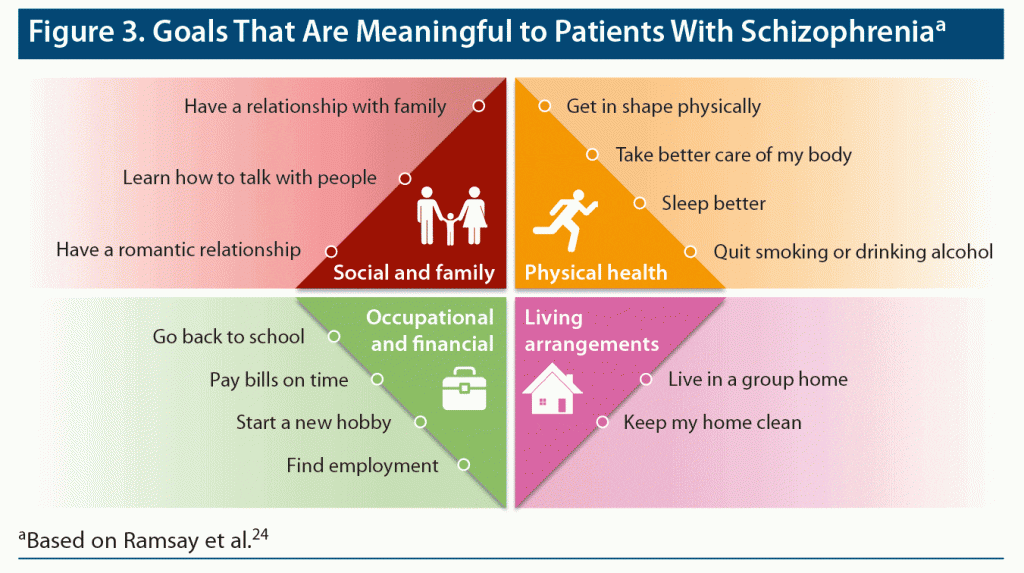
Goals for functional improvement differ for patients with MDD vs schizophrenia (Figure 2 and Figure 3),23,24 but for both disorders, it is intuitively clear that achievement of these functional goals would be affected by aspects of life engagement such as motivation and energy. As shown in a network analysis, motivation and pleasure have pivotal roles in determining social functioning and are intervention targets for improving functional outcomes.25 The roundtable participants also cited cognition as an area of overlap affecting both life engagement and functional (eg, psychosocial, occupational) outcomes.26
The relationship between life engagement and functional improvement was summarized as being bidirectional in nature: the more a patient engages—is alert, has energy, has interest in social activities—the more functional they become, and the more functional the patient becomes, the more opportunities they have to engage. Dr Rafeyan explained further:
Functional Recovery
Functional recovery can be thought of in the simplest terms as a return to the patient’s highest pre-disease level of functioning in domains such as those listed in Figures 2 and 3 (eg, work and domestic responsibilities, self-care, independent living, family and social relationships, participation in community activities). Alternately, for some patients, recovery may mean achievement of functioning in these areas for the first time.
Both functioning and aspects of life engagement play important roles in patients’ definitions of recovery. According to a study by Zimmerman et al,27 the 3 items most often judged by MDD patients to be important in determining remission were, first, the presence of positive mental health features such as optimism and self-confidence; second, feeling like one’s usual, normal self; and third, a return to usual level of functioning. Along these lines, Dr McIntyre commented that the elements important for full recovery are resolution of symptoms and return of function, but also a regain of the full repertoire of well-being that patients recall prior to their illness onset.
Recovery is also a personal journey that is unique to the patient,28 and an area of commonality between functional recovery and life engagement is that both are influenced by the patient’s own life context. This personalization was highlighted by Dr Rafeyan: “I usually approach the goal of recovery as trying to help my patients have meaningful lives—whatever that means to the patient. That might mean taking pride in helping around the house, or working part-time, or feeling happy and looking forward to attending their day program, or being able to socialize with their colleagues.”
Dr Ismail again pointed to a bidirectional relationship between functioning and life engagement, this time in the context of recovery. Without life engagement, he stated, there may be some functional improvement, but it is modest, or skin deep. A throughline between life engagement and functional recovery is the patient’s sense of agency, or “CEO status” over their own life and relationships. As one recovers fully and regains functioning, one also gains the ability to manage their interface with the world and control their engagement with the world in a way that is suitable for them.
Clinical picture. Dr Thase described what a patient might look like if they were functionally recovered but not engaged with life. A patient of his was the managing partner of a large firm. She worked 60 hours a week and earned a high salary, and she made decisions that influenced the lives and well-being of many people. But she wasn’t happy; life had no joy or “spark.” She also did not desire sex and mentioned that she and her partner had not been sexually active for months. This patient’s functional recovery, in the professional domain, would be at perhaps the 95th or 99th percentile. On a multidimensional functional recovery scale that includes intimate relationships and friendships, she might have been at the 75th percentile across domains. She was not truly well, though, and what was missing for her was the capacity to engage with life. Therefore, despite having a clear response to treatment for a long period of time, without relapses, she lacked the dimension that would make her truly well even though she was functionally recovered.
COLLABORATING WITH PATIENTS TO INCORPORATE LIFE ENGAGEMENT AS A GOAL
Treatment guidelines for both MDD29–31 and schizophrenia32–34 state that patients’ preferences and goals should be discussed with the patient in the context of adequate background information, and the patient’s personal goals should then be part of treatment planning. In fact, discordance between patient and clinician treatment goals that goes unaddressed can lead to reduced adherence and influence treatment outcomes.15 Patients value the reestablishment of a sense of engagement as a high-priority therapeutic objective,10,16 relayed Dr McIntyre, and that alone serves as the clarion call for action with respect to discussing life engagement with patients and assessing it.
Dr Ismail observed that collaborating with patients on life engagement as an outcome is also significant because it reflects a paradigm shift from the traditional treatment goals. Previously, the motivation for schizophrenia treatment was to bring a patient’s symptoms to a level at which the patient is not bothering anyone, whereas in the current and future approach, the goal is for the patient to have a productive life that is meaningful to them and those who are close to them. He explained that in the past, the bar had been set low in “industrial psychiatry”: sedate the patient, reduce their positive symptom burden, and move on. This approach takes away the patient’s agency, their individual wishes and desires, and their voice. Every person with schizophrenia is an individual who wants to live a meaningful and enjoyable life, so looking ahead to improvement beyond simple symptom control is essential.
The panelists acknowledged that physicians might be reluctant to initiate a potentially long conversation about life engagement, since visit time is short. However, Dr McIntyre argued, using a framework to set objectives, such as SMART (Specific, Measurable, Attainable, Relevant, and Time-bound), “actually saves you time. And in addition to producing concrete objectives, for me it has also provided fertile ground to understand what engagement would mean for that patient.”
Benefits for Patients
In considering the question of what assessment of life engagement would mean for patients, it was agreed that the importance of shared goal-setting lies partly in the patient’s being able to see what is possible. Dr Correll emphasized, “It’s important for patients to focus on goals that are formulated, and having higher aims for patients can actually lead them down that path.” Dr Rafeyan observed that if clinicians do not assess life engagement and make sure patients are engaged with life, many patients will do the minimum: they will stay by themselves and isolate, which can exacerbate symptoms; he added that, post-pandemic, we are all familiar with the effects of isolation.
Dr Rafeyan further explained that, importantly, discussions about life engagement can even help put patients at ease about psychiatric treatment in general. “Many patients are very appreciative of the discussions about life engagement and find them helpful, especially initially. Often, patients come to our offices for the first time and have never seen a psychiatrist or mental health provider before, and they’re very uneasy about our interventions and medications; they’re concerned about the effects medication will have on them. Especially in schizophrenia, we often hear patients express, ‘I don’t want to be a zombie’: that’s the mental image they have about psychiatric treatment. So when they hear from us that our goal for them is in fact the opposite—for them to be functioning to their best ability and go back to doing things that they did before, or maybe weren’t able to do because of the disease—it helps them understand that our goal is different. Discussing functional goals and life engagement early helps dispel the myth many hold about psychiatric treatment, which is very important.” The importance of functional goals and life engagement invites the need for measurement of these outcomes in clinical and research settings.35
Goal-Setting for Patients With MDD vs Schizophrenia
Dr Correll posited that patients with MDD might be more engaged than those with schizophrenia to begin with. Clinicians could draw on previous engagement and essentially reconnect the patient to existing goals rather than having to create new goals, because people with mood disorders tend to be more connected to life in general than people with schizophrenia. Dr Thase agreed that more collaboration in the development of a patient-centric plan could be expected in a subset of the population with mood disorders. However, he also made the point that the effects of early onset, chronic depression that begins in adolescence can be as defining and debilitating as those seen in schizophrenia in terms of impairment and one’s perception of what is possible:
Timing
Dr Ismail emphasized that the road to life engagement starts with the initial clinical interaction and never stops. He advises his trainees to keep both relapse prevention and full recovery of functioning and engagement in mind from the patient’s first visit, in the clinic, or even in first-episode patients in the emergency department (ED). The idea is to treat with longer-term outcomes in mind: simply sedating patients and having them become less psychotic and less agitated in the ED is insufficient. He also pointed to the role of early treatment of schizophrenia in preserving the patient’s ability to engage.
 A “Quadruple Aim” for Clinicians
A “Quadruple Aim” for Clinicians
Dr Correll issued the following challenge to clinicians:
- Be engaged with the goal of helping patients achieve life engagement by discussing it with them and implementing a concrete treatment plan (eg, using the SMART framework).
- Be engaged with the patient and use interpersonal skills to create an effective treatment alliance, because without it, there could be difficulty with adherence or with pursuing goals. For that, interpersonal skills are needed.
- Be engaged with the treatment team and the patient’s significant others: Connect with the multiprofessional treatment team and nonprofessional care partners in the patient’s life to make achievement of life engagement more likely and sustainable.
- Be engaged with their own lives: If clinicians just “function” and are not engaged in things that give them resources so they can pass on the “spark” of engagement, they will fall short of helping patients achieve it.
Published online: August 3, 2022.
References (35)

- Weldring T, Smith SMS. Patient-Reported Outcomes (PROs) and Patient-Reported Outcome Measures (PROMs). Health Serv Insights. 2013;6:61–68. PubMed CrossRef
- Mercieca-Bebber R, King MT, Calvert MJ, et al. The importance of patient-reported outcomes in clinical trials and strategies for future optimization. Patient Relat Outcome Meas. 2018;9:353–367. PubMed CrossRef
- Graf C. The Lawton Instrumental Activities of Daily Living Scale. Am J Nurs. 2008;108(4):52–62, quiz 62–63. PubMed CrossRef
- Weiss C, Meehan SR, Brown TM, et al. Effects of adjunctive brexpiprazole on calmness and life engagement in major depressive disorder: post hoc analysis of patient-reported outcomes from clinical trial exit interviews. J Patient Rep Outcomes. 2021;5(1):128. PubMed CrossRef
- Ho MY, Cheung FM, Cheung SF. The role of meaning in life and optimism in promoting well-being. Pers Individ Dif. 2010;48(5):658–663. CrossRef
- Bartrés-Faz D, Cattaneo G, Solana J, et al. Meaning in life: resilience beyond reserve. Alzheimers Res Ther. 2018;10(1):47. PubMed CrossRef
- Mago R, Fagiolini A, Weiller E, et al. Understanding the emotions of patients with inadequate response to antidepressant treatments: results of an international online survey in patients with major depressive disorder. BMC Psychiatry. 2018;18(1):33. PubMed CrossRef
- Trøstheim M, Eikemo M, Meir R, et al. Assessment of anhedonia in adults with and without mental illness: a systematic review and meta-analysis. JAMA Netw Open. 2020;3(8):e2013233. PubMed CrossRef
- Rosenblat JD, Simon GE, Sachs GS, et al. Treatment effectiveness and tolerability outcomes that are most important to individuals with bipolar and unipolar depression. J Affect Disord. 2019;243:116–120. PubMed CrossRef
- Demyttenaere K, Donneau AF, Albert A, et al. What is important in being cured from depression? discordance between physicians and patients (1). J Affect Disord. 2015;174:390–396. PubMed CrossRef
- Fava M, Okame T, Matsushima Y, et al. Switching from inadequate adjunctive or combination treatment options to brexpiprazole adjunctive to antidepressant: an open-label study on the effects on depressive symptoms and cognitive and physical functioning. Int J Neuropsychopharmacol. 2017;20(1):22–30. PubMed CrossRef
- Davis LL, Ota A, Perry P, et al. Adjunctive brexpiprazole in patients with major depressive disorder and anxiety symptoms: an exploratory study. Brain Behav. 2016;6(10):e00520. PubMed CrossRef
- Weisler RH, Ota A, Tsuneyoshi K, et al. Brexpiprazole as an adjunctive treatment in young adults with major depressive disorder who are in a school or work environment. J Affect Disord. 2016;204:40–47. PubMed CrossRef
- Meehan SR, He Y, de Jong Laird A, et al. Path analyses to explore the direct and indirect effects of brexpiprazole on life engagement: post hoc analysis of six clinical studies in depression and schizophrenia. Poster presented at the American Society of Clinical Psychopharmacology Annual Meeting; June 1, 2021.
- Bridges JFP, Slawik L, Schmeding A, et al. A test of concordance between patient and psychiatrist valuations of multiple treatment goals for schizophrenia. Health Expect. 2013;16(2):164–176. PubMed CrossRef
- Meehan SR, Weiss C, Adair M. Exploring the concept of life engagement from the perspective of patients with schizophrenia: a study using patient interviews. Presented at the American Society of Clinical Psychopharmacology (ASCP) Annual Meeting; June 1, 2021.
- Carrà G, Crocamo C, Bartoli F, et al. Influence of positive and negative symptoms on hedonic and eudaemonic well-being in people with schizophrenia: A longitudinal analysis from the EuroSc study. Schizophr Res. 2022;244:21–28. PubMed CrossRef
- IsHak WW, Mirocha J, James D, et al. Quality of life in major depressive disorder before/after multiple steps of treatment and one-year follow-up. Acta Psychiatr Scand. 2015;131(1):51–60. PubMed CrossRef
- Connell J, Brazier J, O’Cathain A, et al. Quality of life of people with mental health problems: a synthesis of qualitative research. Health Qual Life Outcomes. 2012;10(1):138. PubMed CrossRef
- Moylan S, Maes M, Wray NR, et al. The neuroprogressive nature of major depressive disorder: pathways to disease evolution and resistance, and therapeutic implications. Mol Psychiatry. 2013;18(5):595–606. PubMed CrossRef
- Penttilä M, Jääskeläinen E, Hirvonen N, et al. Duration of untreated psychosis as predictor of long-term outcome in schizophrenia: systematic review and meta-analysis. Br J Psychiatry. 2014;205(2):88–94. PubMed CrossRef
- WHO. International Classification of Functioning, Disability and Health. ICF; 2001.
- Battle CL, Uebelacker L, Friedman MA, et al. Treatment goals of depressed outpatients: a qualitative investigation of goals identified by participants in a depression treatment trial. J Psychiatr Pract. 2010;16(6):425–430. PubMed CrossRef
- Ramsay CE, Broussard B, Goulding SM, et al. Life and treatment goals of individuals hospitalized for first-episode nonaffective psychosis. Psychiatry Res. 2011;189(3):344–348. PubMed CrossRef
- Hu HX, Lau WYS, Ma EPY, et al. The important role of motivation and pleasure deficits on social functioning in patients with schizophrenia: a network analysis. Schizophr Bull. 2022;sbac017. PubMed CrossRef
- McIntyre RS, Cha DS, Soczynska JK, et al. Cognitive deficits and functional outcomes in major depressive disorder: determinants, substrates, and treatment interventions. Depress Anxiety. 2013;30(6):515–527. PubMed CrossRef
- Zimmerman M, McGlinchey JB, Posternak MA, et al. How should remission from depression be defined? the depressed patient’s perspective. Am J Psychiatry. 2006;163(1):148–150. PubMed CrossRef
- Windell D, Norman R, Malla AK. The personal meaning of recovery among individuals treated for a first episode of psychosis. Psychiatr Serv. 2012;63(6):548–553. PubMed CrossRef
- Gelenberg AJ, Freeman MP, Markowitz JC, et al. Work Group on Major Depressive Disorder. Practice Guideline for the Treatment of Patients With Major Depression Disorder. American Psychiatric Publishing; 2010.
- Bauer M, Pfennig A, Severus E, et al; World Federation of Societies of Biological Psychiatry. Task Force on Unipolar Depressive Disorders. World Federation of Societies of Biological Psychiatry (WFSBP) guidelines for biological treatment of unipolar depressive disorders, part 1: update 2013 on the acute and continuation treatment of unipolar depressive disorders. World J Biol Psychiatry. 2013;14(5):334–385. PubMed CrossRef
- Kennedy SH, Lam RW, McIntyre RS, et al. CANMAT Depression Work Group. Canadian Network for Mood and Anxiety Treatments (CANMAT) 2016 clinical guidelines for the management of adults with major depressive disorder: section 3. Pharmacological treatments. Can J Psychiatry. 2016;61(9):540–560. PubMed CrossRef
- Hasan A, Falkai P, Wobrock T, et al; WFSBP Task force on Treatment Guidelines for Schizophrenia. World Federation of Societies of Biological Psychiatry (WFSBP) guidelines for biological treatment of schizophrenia, part 2: update 2012 on the long-term treatment of schizophrenia and management of antipsychotic-induced side effects. World J Biol Psychiatry. 2013;14(1):2–44. PubMed CrossRef
- Keepers GA, Fochtmann LJ, Anzia JM, et al; (Systematic Review). The American Psychiatric Association Practice Guideline for the treatment of patients with schizophrenia. Am J Psychiatry. 2020;177(9):868–872. PubMed CrossRef
- Remington G, Addington D, Honer W, et al. Guidelines for the pharmacotherapy of schizophrenia in adults. Can J Psychiatry. 2017;62(9):604–616. PubMed CrossRef
- McIntyre RS, Ismail Z, Watling CP, et al. Patient-reported outcome measures for life engagement in mental health: a systematic review. J Patient Rep Outcomes. 2022;6(1):62. PubMed CrossRef
This PDF is free for all visitors!