ABSTRACT
During the past decade, nearly a dozen small and large, prospective and retrospective observational studies examined cognitive neurodevelopmental outcomes in childhood after gestational exposure to antidepressant drugs. Many of the studies found that exposure was associated with poorer outcomes on measures of language, cognition, intellectual skills, and academic performance, but, in most instances, the association appeared to be more related to maternal depression during pregnancy and other confounds than to antidepressant use during pregnancy. A large new population-based observational study specifically examined language and mathematics performance in serial, nationally standardized tests. The study found that, in fully adjusted analyses, in children and adolescents aged 9–15 years, a history of gestational exposure to antidepressant drugs was associated with a small (by about 2 out of 100 points) but statistically significantly poorer performance in mathematics but not in language. The findings were consistent though attenuated in a large number of important and appropriate sensitivity analyses, some of which adjusted for confounding in additional ways. The body of literature reviewed suggests that prenatal antidepressant exposure is indeed associated with cognitive neurodevelopmental deficits and that the deficits are attenuated or eliminated by adjustment for maternal depression and other confounds. It is suggested that the deficits that remain despite adjustment may be due to residual confounding from unmeasured behavioral and internal environment variables associated with untreated maternal depression. Thus, prenatal antidepressant exposure may merely be a marker rather than the cause of cognitive neurodevelopmental deficits. Whereas the literature in the field does not drive a case for withholding antidepressants from depressed pregnant women, decision-making must remain a shared process.
J Clin Psychiatry 2022;83(1):22f14388
To cite: Andrade C. Gestational exposure to antidepressant drugs and neurodevelopment: an examination of language, mathematics, intelligence, and other cognitive outcomes. J Clin Psychiatry. 2022;83(1):22f14388.
To share: https://doi.org/10.4088/JCP.22f14388
© Copyright 2022 Physicians Postgraduate Press, Inc
Gestational exposure to antidepressant drugs, especially the selective serotonin reuptake inhibitors (SSRIs), has been studied with regard to a large number of adverse outcomes. These include adverse antenatal outcomes such as impaired fertility, spontaneous or elective abortion, and intrauterine growth retardation; adverse perinatal outcomes such as preterm birth, assisted or complicated delivery, and postpartum hemorrhage; adverse fetal outcomes such as small for gestational age, small head circumference, and major congenital malformations; adverse postnatal outcomes such as neonatal seizures, poor neonatal adaptation syndrome, and persistent pulmonary hypertension of the newborn; and adverse neurodevelopmental outcomes such as general or specific intellectual disabilities, autism spectrum disorder, and attention-deficit/hyperactivity disorder. Whereas plausible mechanisms suggest a small but statistically significant risk for very few adverse outcomes, such as postpartum hemorrhage, for the most part the adverse outcomes are attenuated or extinguished after adjustment for confounding, implying that antidepressant use during pregnancy is a marker for the adverse outcomes rather than the cause.
Gestational exposure to anticonvulsant drugs, especially valproate, has been associated with impaired neurocognitive development.1,2 Antidepressant drugs have also been investigated in this regard.3 These studies are briefly reviewed, in chronological sequence, with specific reference to studies that examined language, mathematics, intelligence, and cognitive test performances.
Studies in the Last Decade: 2011 to 2020
In a small prospective study, Nulman et al4 found that children gestationally exposed to venlafaxine (n = 62) or SSRIs (n = 62) had verbal, performance, and full scale IQ scores that were significantly lower than these scores in unexposed children (n = 62); however, scores in antidepressant-exposed children were similar to those in children exposed to maternal depression but not to antidepressants (n = 54). This suggests that maternal depression explains the association between prenatal antidepressant exposure and lower IQ scores. In a small sibling pair analysis (n = 45 pairs), Nulman et al5 found that sibs gestationally exposed vs unexposed to SSRIs did not differ in verbal, performance, or full scale IQ scores.
In a very small study of children gestationally exposed (n = 20) vs unexposed (n = 21) to antidepressants, full scale IQ scores were not associated with antidepressant exposure.6 In another small study (n = 103), gestational exposure to SSRIs was not associated with performance on a range of IQ subtests.7 In a small (n = 178) prospective cohort, Johnson et al8 found that expressive language scores were lower in children prenatally exposed to serotonin reuptake inhibitors (SRIs); cognitive functioning, otherwise, was not associated with SRI exposure.
In a large population-based study, Brown et al9 found no significant increase in the risk of speech/language disorder, scholastic disorder, or motor disorder in children gestationally exposed to maternal depression and SSRIs (n = 15,596) relative to children gestationally exposed to maternal depression but not SSRIs (n = 9,537). When these 2 groups of children were each compared with children gestationally unexposed to both maternal depression and SSRIs (n = 31,207), all associations were significant in crude analyses but attenuated for speech/language disorders and became nonsignificant for scholastic and motor disorders in analyses that adjusted for confounders. These findings suggest that maternal depression explains much or possibly all of the association between prenatal antidepressant exposure and poorer cognitive and motor development during childhood. Interestingly, children of women who had purchased SSRIs on 2 or more occasions during pregnancy were at significantly higher risk of speech/language disorder (but not of scholastic or motor disorder) relative to children gestationally exposed to only maternal depression. Readers may note that this last analysis may have controlled for maternal depression but could not adjust for severity of the depression.
In a small prospective study of children gestationally exposed to SSRIs (n = 71), maternal depression (n = 385), or neither (n = 5,427), El Marroun et al10 found that SSRI exposure was not associated with executive functions at age 4 years, non-verbal intelligence at age 5 years, or neuropsychological test performance at age 7 years. However, SSRI-exposed children showed poorer language performance than children who had been exposed to maternal depression but not to SSRIs.
In a large population-based cohort study, Viktorin et al11 found that, relative to no exposure (n = 172,646), gestational exposure to antidepressant drugs (n = 3,982) was associated with an almost doubled risk of intellectual disability; however, the risk was no longer statistically significant after adjusting for confounding variables. Finally, in another large population-based cohort study,12 children gestationally exposed to SSRIs (n = 3,314) were compared with children of mothers who had used SSRIs previously but not during the index pregnancy (n = 3,536). In adjusted analyses, only SSRI exposure in all trimesters of pregnancy was associated with only delayed start of elementary schooling and not special education needs.
In summary, some but not all of these 9 observational studies found that prenatal exposure to antidepressant drugs was associated with impaired performance on measures of language, cognition, intellectual skills, and academic performance in pediatric samples; however, in most instances, the association appeared to be related more to maternal depression during pregnancy than to the use of antidepressant drugs during pregnancy.
2021: The Study by Christensen et al13
A large new population-based retrospective cohort study has now been published.13 The authors drew data from linked population registers in Denmark. The sample comprised 575,369 primary and secondary schoolchildren, born during 1997–2009, who had completed at least 1 standardized language test (total, 1,392,370 tests) or 1 standardized mathematics test (total, 786,553 tests) as part of the Danish National Test Program during 2010–2018. The language tests covered language comprehension, decoding, and reading comprehension. The mathematics tests addressed numbers, algebra, geometry, statistics, and probability. The tests were adaptive and computer-based and were administered several times as the child progressed through schooling. The results were mapped into a single score between 1 and 100 with higher values indicating better performance.
The age of the sample at the different times of testing ranged from about 9 to 15 years. The sample was 51% male. Nearly 1.8% (n = 10,198) of the sample had been gestationally exposed to antidepressants; gestational exposure was defined as the mother having filled at least 1 prescription for antidepressants during the month before pregnancy or any time during pregnancy. A history of psychiatric disorder was more common in mothers (44.4% vs 4.5%) as well as fathers (8.2% vs 3.0%) in antidepressant exposed vs antidepressant unexposed pregnancies.
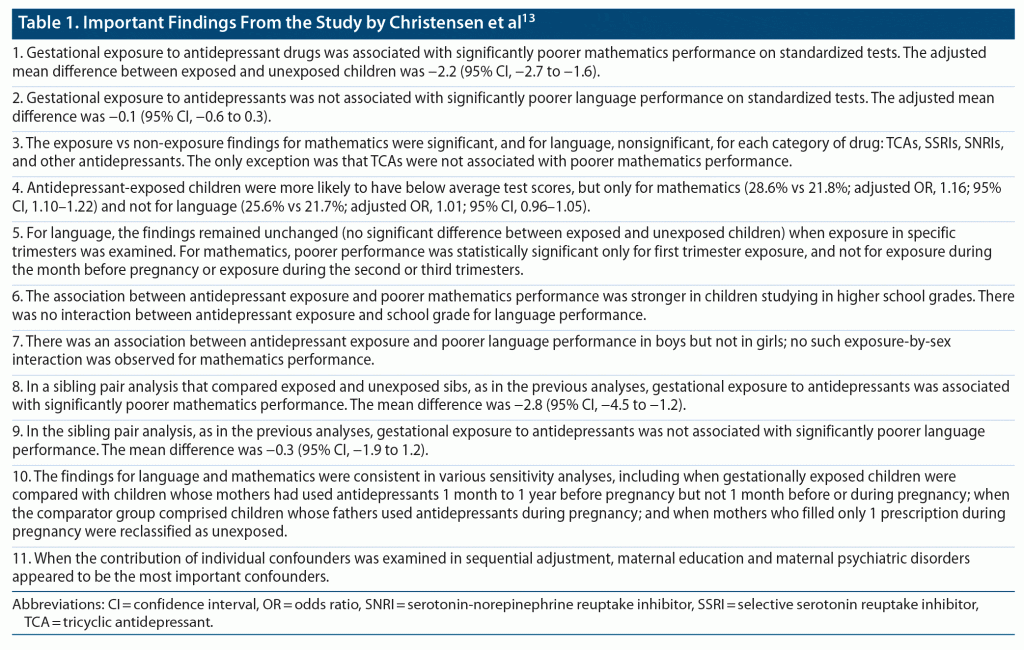
Analyses were adjusted for important confounders, including maternal age and education, paternal income, maternal and paternal psychiatric history, and maternal prescriptions filled for antianxiety, antiseizure, and antipsychotic medications during pregnancy. The main findings of this study are presented in Table 1.
In summary, in minimally adjusted analyses, in children and adolescents aged 9–15 years, a history of gestational exposure to antidepressant drugs was associated with significantly poorer performances in the standardized language and mathematics tests. In fully adjusted analyses, exposure was associated with a small (by about 2 out of 100 points) but statistically significantly poorer performance in mathematics but not in language. This finding was common to almost all categories of antidepressant drugs and was consistent (but mostly attenuated) in a large number of sensitivity analyses, including an exposed vs unexposed sibling pair analysis and an analysis that compared antidepressant use during pregnancy vs only pre-pregnancy use.
Antidepressant Drugs as a Marker of Disadvantage
In the Christensen et al13 study, the mean test scores for language were 53.4 vs 56.6 out of 100 points in exposed vs unexposed children; the raw (unadjusted) difference was 3.2 out of 100 points. The mean test scores for mathematics were 52.1 vs 57.4 out of 100 points in exposed vs unexposed children; the raw difference was 5.3 out of 100 points. These differences are numerically noticeable in magnitude; whereas they may not be clinically significant at the individual level, they are of potential concern at the population level, especially for mathematics, because of the large number of children exposed.
The difference between exposed and unexposed children was statistically significant for both language and mathematics in all analyses (main analysis as well as sensitivity analyses) that minimally adjusted for confounding variables. However, in all of the fully adjusted analyses (main analysis as well as sensitivity analyses), the differences were no longer statistically significant for language, and, in almost all of the fully adjusted analyses, the differences remained statistically significant for mathematics. Importantly, in the fully adjusted main analyses, the numerical difference between exposed and unexposed children was almost completely extinguished for language and was more than halved for mathematics; and, in many of the sensitivity analyses, the numerical difference for mathematics attenuated even further. These findings mean that children who are gestationally exposed to antidepressant drugs are disadvantaged in both language and mathematics, but the disadvantage is entirely explained by confounding with regard to language, and substantially explained by confounding with regard to mathematics. In other words, antidepressant use in pregnancy is a marker of neurodevelopmental disadvantage and is unlikely to be a cause of the disadvantage.
Residual Confounding
The disadvantage for mathematics was substantially reduced but not eliminated in the fully adjusted main analysis that compared exposed and unexposed children. Might residual confounding explain the uneliminated disadvantage? Genetic and environmental variables are usually suggested as explanations for residual confounding. However, the finding of disadvantage in mathematics in the fully adjusted main analysis was confirmed in a fully adjusted exposed vs unexposed sibling pair analysis. This sibling pair analysis would have attenuated residual confounding by controlling for some shared maternal (eg, maternal genes, maternal behavior) and environmental (eg, opportunities for health, opportunities to learn) confounds. However, the sibling pair analysis would not have been able to control for depression-related confounds (eg, poor nutrition, altered internal hormonal and other environment) in the antidepressant-exposed pregnancies. In fact, when comparing antidepressant exposed vs unexposed pregnancies, other than randomization, nothing can control for depression-related confounds.
As a side note, here, a sibling pair analysis incompletely adjusts for shared genetic and environmental confounds. This is because sibs don’t inherit an identical set of genes and because sibs don’t grow in identical family, social, and school environments.
As a second side note, Christensen et al13 also observed poorer performance in mathematics but not in language in a fully adjusted analysis that compared antidepressant use during pregnancy with only pre-pregnancy antidepressant use. Such an analysis could have controlled for depressive illness as a trait in the mother but may not have controlled for depressive illness as a state during pregnancy. In any case, even if both groups of mothers were depressed during pregnancy, it is likely that the group that used antidepressants was more severely depressed, which could explain why the antidepressants were used. So, here, severity of maternal depression, and the behaviors and the internal environment associated therewith, is the unmeasured and unadjusted residual confound.
As a final side note, what if the women who used antidepressants became well while the women with antidepressant use before but not during pregnancy experienced untreated depression during pregnancy? In such a situation, confounding by maternal depression could actually suppress rather than reveal a relationship between antidepressant exposure and poor outcomes.
The bottom line is that cause vs association is best determined in randomized controlled trials, failing which, in observational studies that actually rate the presence and severity of depression (and behaviors and health indices associated therewith) across the course of pregnancy.
Other Notes
Christensen et al13 found that poorer performance in mathematics was specifically associated with first trimester exposure to antidepressants. The fetal brain is poorly differentiated in the first trimester, and so it is likely that if an adversity has an impact on the first trimester brain, the impact will have more general consequences than an effect that is restricted to mathematics. In any case, regardless of the trimester during which the adversity acted, why should mathematics functions be specifically affected?
There are 2 overlapping considerations here. One is that a wider range of cognitive abilities was affected but, because only language and mathematics were studied, other impairments were not detected. The other is that language and mathematics (and perhaps other abilities) were affected, but the language deficits were compensated for by overtraining because language is widely used in everyday life and is the medium in which scholastic instruction is conveyed. This may also explain the study finding of wider mathematics deficits in higher grades; the greater challenge in higher grades may have exposed an impaired ability in mathematics that was not compensated for by overtraining, as in the case of language.
If a wider range of cognitive abilities was affected, IQ should be lower in children gestationally exposed to antidepressant drugs. However, this does not appear to be the case, as suggested by the limited literature available on the subject, reviewed in an earlier section. This may support the consideration that the poorer mathematics performance was an artifact of residual confounding, and a reason why greater statistical adjustment for mathematics is required is that mathematics is not an overlearned ability as is language.
Take-Home Messages
- In children and adolescents aged 9–15 years, a history of gestational exposure to antidepressant drugs may be associated with slightly poorer performance in language and mathematics tests (especially the latter). The poorer performances may not be clinically significant at the individual level but are of potential concern at the population level because of the large number of children exposed.
- After adjusting for confounding, the poorer performance associated with antidepressant exposure is extinguished for language and is much attenuated for mathematics. This implies that antidepressant use in pregnancy is a marker for neurodevelopmental disadvantage in language and mathematics and is unlikely to be a cause of the disadvantage.
- Maternal depression, behaviors associated with maternal depression, the internal environment in maternal depression, and the magnitude and severity of all of these are inadequately measured and unmeasured variables that may be responsible for residual confounding in analyses that continue to find a disadvantage associated with gestational exposure to antidepressants despite adjustment for (other) confounders.
- In the light of the above, and in the light of the considerable clinical and other benefits that result from treated as compared with untreated depression, the studies reviewed in this article do not make a case for withholding antidepressants from depressed pregnant women. Decision-making must nevertheless remain a process that is shared between pregnant women, their significant others, and the treating team.
Parting Note
Christensen et al13 found that, in fully adjusted analyses, tricyclic antidepressants (TCAs) were not associated with poorer performance in either language or mathematics. So, should TCAs be preferred for use in pregnancy if cognitive neurodevelopment is the outcome of interest? No, because the analysis for TCAs may have been underpowered. In any case, an isolated finding should not drive clinical recommendations. And, finally, the antidepressant that should be advised is the one that works for and is well tolerated by the patient; else, what is the point in prescribing the antidepressant?
 Each month in his online column, Dr Andrade considers theoretical and practical ideas in clinical psychopharmacology with a view to update the knowledge and skills of medical practitioners who treat patients with psychiatric conditions.
Each month in his online column, Dr Andrade considers theoretical and practical ideas in clinical psychopharmacology with a view to update the knowledge and skills of medical practitioners who treat patients with psychiatric conditions.
Department of Clinical Psychopharmacology and Neurotoxicology, National Institute of Mental Health and Neurosciences, Bangalore, India ([email protected]).
Financial disclosure and more about Dr Andrade.
References (13)

- Inoyama K, Meador KJ. Cognitive outcomes of prenatal antiepileptic drug exposure. Epilepsy Res. 2015;114:89–97. PubMed CrossRef
- Andrade C. Valproate in pregnancy: recent research and regulatory responses. J Clin Psychiatry. 2018;79(3):18f12351. PubMed CrossRef
- Rommel A-S, Bergink V, Liu X, et al. Long-term effects of intrauterine exposure to antidepressants on physical, neurodevelopmental, and psychiatric outcomes: a systematic review. J Clin Psychiatry. 2020;81(3):19r12965. PubMed CrossRef
- Nulman I, Koren G, Rovet J, et al. Neurodevelopment of children following prenatal exposure to venlafaxine, selective serotonin reuptake inhibitors, or untreated maternal depression. Am J Psychiatry. 2012;169(11):1165–1174. PubMed CrossRef
- Nulman I, Koren G, Rovet J, et al. Neurodevelopment of children prenatally exposed to selective reuptake inhibitor antidepressants: Toronto Sibling Study. J Clin Psychiatry. 2015;76(7):e842–e847. PubMed CrossRef
- Galbally M, Lewis AJ, Buist A. Child developmental outcomes in preschool children following antidepressant exposure in pregnancy. Aust N Z J Psychiatry. 2015;49(7):642–650. PubMed CrossRef
- Hermansen TK, Røysamb E, Augusti EM, et al. Behavior and inhibitory control in children with prenatal exposure to antidepressants and medically untreated depression. Psychopharmacology (Berl). 2016;233(8):1523–1535. PubMed CrossRef
- Johnson KC, Smith AK, Stowe ZN, et al. Preschool outcomes following prenatal serotonin reuptake inhibitor exposure: differences in language and behavior, but not cognitive function. J Clin Psychiatry. 2016;77(2):e176–e182. PubMed CrossRef
- Brown AS, Gyllenberg D, Malm H, et al. Association of selective serotonin reuptake inhibitor exposure during pregnancy with speech, scholastic, and motor disorders in offspring. JAMA Psychiatry. 2016;73(11):1163–1170. PubMed CrossRef
- El Marroun H, White TJ, Fernandez G, et al. Prenatal exposure to selective serotonin reuptake inhibitors and non-verbal cognitive functioning in childhood. J Psychopharmacol. 2017;31(3):346–355. PubMed CrossRef
- Viktorin A, Uher R, Kolevzon A, et al. Association of antidepressant medication use during pregnancy with intellectual disability in offspring. JAMA Psychiatry. 2017;74(10):1031–1038. PubMed CrossRef
- Kragholm K, Andersen MP, Mortensen RN, et al. Exposure to selective serotonin reuptake inhibitors in utero and early elementary school outcomes. Acta Psychiatr Scand. 2018;137(6):481–490. PubMed CrossRef
- Christensen J, Trabjerg BB, Sun Y, et al. Association of maternal antidepressant prescription during pregnancy with standardized test scores of Danish school-aged children. JAMA. 2021;326(17):1725–1735. PubMed CrossRef
This PDF is free for all visitors!