Click to enlarge page
Awareness that concussions are more serious than previously believed has been increasing. Also known as mild traumatic brain injury (mTBI), concussions often occur, and often multiple times, in both military and sports settings. Brain injuries can seriously and negatively impact patients, leading to changes in personality, sleep problems, and cognitive impairments and can increase the risk for suicide, posttraumatic stress disorder, depression, and anxiety. In some people, repetitive mTBI can lead to chronic traumatic encephalopathy (CTE), a neurodegenerative disorder. Evidence-based treatments are needed for both mTBI and CTE. Currently, symptom management and education are the best strategies to help those who have received multiple concussions. Prevention education about concussions and the use of return-to-play guidelines are especially important for young athletes.
From the Veterans Affairs (VA) Northwest Network Mental Illness Research, Education, and Clinical Center (MIRECC); Department of Psychiatry and Behavioral Sciences, University of Washington School of Medicine; and the University of Washington Alzheimer’s Disease Research Center, Seattle (Dr Peskind); Department of Neurology, Washington University School of Medicine, St. Louis, Missouri (Dr Brody); Military and Veterans’ Clinical Rehabilitation Research, Faculty of Rehabilitation Medicine, University of Alberta, Edmonton, Alberta, Canada (Dr Cernak); Departments of Neurology and Pathology, VA Boston, and the Center for the Study of Traumatic Encephalopathy and the Alzheimer’s Disease Center, Boston University, Boston, Massachusetts (Dr McKee); and Neurology Service, Cleveland VA Medical Center, Cleveland, Ohio (Dr Ruff).’ ‹
Find more articles on this and other psychiatry and CNS topics:
The Journal of Clinical Psychiatry
The Primary Care Companion for CNS Disorders
This Commentary section of The Journal of Clinical Psychiatry presents the highlights of the planning teleconference series “Military- and Sports-Related Mild Traumatic Brain Injury: Clinical Presentation, Management, and Long-Term Consequences,” which was held on August 27, 2012. This report was prepared and independently developed by the CME Institute of Physicians Postgraduate Press, Inc.
The teleconference was chaired by Elaine R. Peskind, MD, Veterans Affairs (VA) Northwest Network Mental Illness Research, Education, and Clinical Center (MIRECC); Department of Psychiatry and Behavioral Sciences, University of Washington School of Medicine; and the University of Washington Alzheimer’s Disease Research Center, Seattle. The faculty were David Brody, MD, PhD, Department of Neurology, Washington University School of Medicine, St. Louis, Missouri; Ibolja Cernak, MD, ME, MHS, PhD, Military and Veterans’ Clinical Rehabilitation Research, Faculty of Rehabilitation Medicine, University of Alberta, Edmonton, Alberta, Canada; Ann McKee, MD, Departments of Neurology and Pathology, VA Boston, and the Center for the Study of Traumatic Encephalopathy and the Alzheimer’s Disease Center, Boston University, Boston, Massachusetts; and Robert L. Ruff, MD, PhD, Neurology Service, Cleveland VA Medical Center, Cleveland, Ohio.
Financial disclosure: Dr Peskind is a consultant for Avanir and Eli Lilly, has received grant/research support from Eli Lilly, is a member of the speakers/advisory boards for Novartis and Forest, and is a stock shareholder of Elan and Bristol-Myers Squibb. Drs Brody, Cernak, McKee, and Ruff have no personal affiliations or financial relationships with any commercial interest to disclose relative to the activity.
The opinions expressed herein are those of the faculty and do not necessarily reflect the views of the CME provider and publisher.
J Clin Psychiatry 2013;74(2):180-188 (doi:10.4088/JCP.12011co1c)
© Copyright 2013 Physicians Postgraduate Press, Inc.
Awareness of the potential long-term effects of mild traumatic brain injury (mTBI) has increased in recent years. Certain populations, such as military service members and athletes who play contact sports, are susceptible to repetitive mTBI.
With the United States operations in Iraq and Afghanistan, where explosive devices have been commonly used, blast-related brain injuries have come under scrutiny.1 Each year, about 28,000 service members experience a traumatic brain injury, most of which are considered mild but are frequently repetitive.2 In the sports world, a consequence of repeated mild brain trauma that was first identified in boxing as “punch drunk” syndrome has been recognized in other contact sports as well.3
The US Army and the National Football League have recently partnered to share research and to encourage current and former personnel to recognize their own or others’ brain injuries and seek help. Elaine R. Peskind, MD, gathered nationally renowned experts and chaired a discussion on the effects of military-related and sports-related mTBI, long-term consequences, management, and prevention.
DEFINING CONSEQUENCES OF BRAIN TRAUMA
Dr Peskind: I would like to begin by defining the following terms: mTBI, concussion, persistent postconcussive symptoms, and chronic traumatic encephalopathy (CTE).
Dr Brody: Traumatic brain injury is damage to the brain’s structure and function caused by an acute external physical force. What is considered “mild” has varied quite a bit, but a widely used definition of mTBI is loss of consciousness for up to 30 minutes, a change in mental status for up to 24 hours, or posttraumatic amnesia for up to 24 hours (Table 1).4 If any of these problems lasts longer than the specified time, or if intracranial pathology appears on structural imaging of the brain, then the injury is considered moderate or severe. Acute symptoms may appear immediately or a few minutes after the injury (Table 2).5
A concussion is an mTBI. No distinction between concussion and mTBI exists, except that concussion is commonly used in the sports world and mTBI is commonly used in the trauma literature. These are closed-head rather than penetrating injuries.
Most people recover from a concussion/mTBI within 7 days.6 Symptoms persisting for more than 3 months that are directly related to the injury are considered persistent postconcussive symptoms.7
Dr McKee: A possible consequence of repetitive mild brain trauma is CTE. This progressive neurodegenerative disorder is characterized by the accumulation of hyperphosphorylated tau protein that begins focally and then spreads to involve most of the central nervous system.8 In its early stages, CTE symptoms include difficulty concentrating, depression, and behavioral and personality changes.9 As the disease progresses, patients may have short-term memory loss and cognitive changes, and then, in its late stage, dementia. Parkinsonism and signs of motor neuron disease can also occur, as well as difficulties with gait and speech.
Dr Peskind: What is the life expectancy once symptoms of CTE start?
Dr McKee: Compared with well-known neurodegenerative diseases like Alzheimer’s disease and frontotemporal dementia, CTE progresses much more slowly. It is still a matter of debate as to when symptoms attributable to CTE begin to materialize. When I first reviewed the literature, I noticed a latent period of about 8 years between the head injury event and when symptoms became noticeable. However, in a recent series of verified instances of CTE in my practice, some individuals have been symptomatic within a few years of the injury.
Effects of the Frequency and Nature of mTBI
Dr Peskind: How do patients with repetitive mTBI, whether from sports-related impacts or combat-related blasts, differ clinically from those with a single mTBI?
Dr Ruff: My colleagues and I10 studied a group of veterans who had at least 1 mTBI with loss of consciousness. The rate of neurologic deficits increased proportionally with the number of mTBI episodes: more than 90% who had more than 5 episodes had a neurologic deficit, while less than 20% with 1 mTBI had a neurologic deficit. Others have found that service members with multiple mTBIs have a significantly higher frequency of depression, anxiety, and posttraumatic stress disorder (PTSD) than those with a single mTBI.11
What we do not know yet is whether time factors into the effects of multiple injuries. That is, do 2 blasts that are separated by 2 years have the same effects as 2 blasts that are separated by weeks?
Dr Cernak: Although blast mTBI and impact mTBI are similar episodes, differences do exist. One of the essential differences between civilian and sport-type impact mTBI and blast mTBI lies in the fact that in the vicinity of an explosion the soldier’s entire body—not only his or her head—is exposed to the blast and interacts with blast effects. Consequently, blast TBI is caused by multiple, interwoven mechanisms of systemic, local, and cerebral responses to blast exposure, often occurring simultaneously. Indeed, accumulating clinical and experimental evidence shows that systemic and local alterations initiated by a blast significantly influence the brain’s response and, thus, contribute to the pathobiology of acute and/or chronic deficits due to the blast.12-14 The frequent complaints that veterans often report about impaired olfaction, gastrointestinal complications, chronic pain, and unstable blood pressure support the importance of these multiorgan changes due to blasts.
Dr Ruff: Yes. In our study,10 the rate of neurologic deficits was significantly greater among veterans who experienced combat mTBI (52%) than civilian mTBI (10%; P < .001).
One difference between sports-related mTBI and blast-related mTBI is that, with blast mTBI, the person frequently has 2 episodes of head trauma very close in time, often within seconds. After the blast itself, which may cause minimal injury, secondary and tertiary consequences may cause injury, such as impact from being blown out of a military personnel vehicle.
Dr Peskind: And different combinations of that scenario exist. For example, I have heard of instances where soldiers have been pinned down, under fire, and mortared several times 20 to 40 minutes apart.

- When evaluating current and former military personnel or athletes, question them and a collateral source (eg, family members, friends) about concussions or mild traumatic brain injury (mTBI).
- Screen for posttraumatic stress disorder, suicidal ideation, impulsivity, and sleep problems in patients who have experienced concussions.
- If a patient who has had repetitive mTBI is exhibiting symptoms of dementia, consider chronic traumatic encephalopathy (CTE) in the differential diagnosis.
- Manage acute and persistent symptoms of mTBI, and watch for the emergence of new evidence-based treatments as research in this field expands.
- Promote prevention of mTBI by providing education about brain safety to children who are entering contact sports, and educate patients who have had concussions and their families about how to avoid further brain injuries.
Dr McKee, do you think there is an essential difference between blast injury and impact injury?
Dr McKee: In the postmortem blast-injured veterans that I have been able to examine, the nature of the injuries and extent of CTE neuropathology appear indistinguishable from sports concussion injuries I have seen. The blast wind produces force that creates an acceleration and deceleration of the head similar to a sports concussion (although the magnitude of acceleration in a blast is much stronger than that in a sports-related concussion). The mechanism of the brain injury is similar, according to our blast neurotrauma mouse model.15 Of course, this phenomenon needs to be studied further to absolutely establish that.
Dr Cernak: We have to be careful when talking about experimental models because the varying animals and study designs make comparison difficult. As Dr Ruff mentioned, blast injuries might be caused by differing blast effects.12,14,16 Indeed, explosions may cause 4 major patterns of injury: (1) primary blast injury caused by the blast wave itself; (2) secondary injury caused by the fragments of debris propelled by the explosion; (3) tertiary injury because of the acceleration of the body or part of the body by the blast wind; and (4) flash burns (ie, quaternary blast effect) because of the transient but intense heat of the explosion.16,17
People may receive varying injuries from the blast wave, depending on factors such as how close to the explosion they were and what type and amount of explosives were used. Many times, service members initially have mild, low-intensity blast exposure, to which they give little importance. While the primary blast effects are unique to the environment where the explosion occurred, the secondary and tertiary blast effects might be compared with the injury scenarios involving direct impact to the head or acceleration and deceleration of the head and body, which Dr McKee was talking about. With a low-intensity blast, acceleration-deceleration is unlikely to occur, but neurologic deficits may still develop,18 especially after repeated low-intensity blasts.
Substantial numbers of mild blast TBIs are caused by primary blasts. While the importance of multisystem, multiorgan response to blast exposure is more obvious in moderate-to-severe brain injuries, it is often neglected in the case of mild blast TBI.
Although there is an ongoing debate about the most vital mechanisms underlying primary blast-induced mTBI, the existing literature points to the following potential mechanisms: (1) direct interaction with the head through direct passage of the blast wave through the skull and/or acceleration and/or rotation of the head and (2) transfer of kinetic energy from the blast wave through large blood vessels in the abdomen and chest to the central nervous system. That is, as the front of the blast overpressure interacts with the body surface and compresses the abdomen and chest, it transfers its kinetic energy to the body’s fluid phase. The resulting hydraulic interaction initiates oscillating waves that traverse the body at about the speed of sound in water and deliver the kinetic energy of the blast wave to the brain. Once delivered, that kinetic energy causes both morphological and functional damage to distinct brain structures. The two potential ways of interaction do not exclude each other. Most recent experimental data suggest both the importance of the blast’s direct interaction with the head15 and the role of shockwave-induced vascular load19 in the pathogenesis of blast TBI.13,20-22
Patients’ Daily Challenges Following Repetitive mTBI
Dr Peskind: Dr Brody, what are the biggest challenges that patients with repetitive mTBI face on a day-to-day basis?
Dr Brody: The problems are highly variable.23 Often, families and friends notice changes in patients’ personalities and will complain about this more than patients do themselves.
In the military context, the problems that I see overwhelmingly are anxiety disorders, including PTSD, sleep disorders, headaches, and subjective cognitive impairment, such as concentration and memory problems. Service members’ cognitive dysfunctions are often not well reflected by objective cognitive testing, but are nonetheless of great concern to the patients.24
In the civilian context, people with repetitive injuries often have a great deal of depression. Sleep disorders and headaches are also common in this group, as are subjective cognitive complaints and changes in personality.
In the sports context, I have seen a high degree of variability. Many former professional football players who have had multiple concussive injuries are remarkably free of symptoms. If they do have symptoms, changes in personality, impulsiveness, and behavioral disturbances, such as aggression and mood instability, can be major problems. Chronic headaches may also occur. Some athletes experience chronic pain due to multiple injuries, and a negative synergy seems to occur in which a head injury and other injuries make each other worse.
Dr Ruff: In the military context, the presentation is similar to that in the civilian arena, with a great deal of depression combined with a persistent anxiety disorder or PTSD.11 Sleep disturbance is a major complaint,25 and lack of sleep can compound attention difficulties and short tempers. In regard to cognitive testing, people not only often feel that they are more impaired than they likely are but also believe themselves to have been much more highly functioning than they probably were. If predeployment test results are on file, they can be used for comparison.4
Dr Peskind: My colleagues and I have had to increase the difficulty of neuropsychological assessments to show any difference between veterans with and without mTBI. The usual assessments do not demonstrate significant differences, but now we are using some real-life multitasking assessment tools that do show a difference. Service members’ complaints are grounded in real problems, but during testing, their cognitive abilities have to be pushed to demonstrate the impairment. Their perception of cognitive impairment may be also influenced by the presence of depression, anxiety, or PTSD.24
Effect of mTBI on the Risk For Suicide and PTSD
Dr Peskind: Studies26,27 in both veteran and civilian populations have found rates of suicide that are 2 to 3 times greater among those with a history of mTBI than among those without mTBI. One way that mTBI plays a role in increased risk of suicide is via its frequent co-occurrence with disorders that increase suicide risk, such as PTSD and depression.28,29 Another way is via increased impulsivity—ie, changes in frontal white matter resulting from an mTBI may alter the likelihood of acting impulsively on suicidal feelings.30
Dr McKee: Damage from an mTBI affects regions of the brain that govern impulsivity and disinhibition; patients might not think about future consequences and just live in the moment. With many individuals who have mTBI, I have been struck by the histories of extreme impulsivity; for example, one moment they were talking to a girlfriend or parent and the next moment, very unexpectedly, they have hanged themselves. The impulsive behavior that characterizes these suicides seems much greater than what you see in patients with depression alone.
Dr Peskind: Those brain changes may create a situation in which thoughts are more likely to be impulsively acted on should they occur.
Dr Brody: That is an important area for future investigation.
Dr Peskind: Does mTBI increase the risk for PTSD independently of the severity of combat operations exposure that would lead to the mTBI?
Dr Brody: I think that mTBI does increase the risk of PTSD. I have seen a substantially higher burden of PTSD in US military personnel with blast-related mTBI than in those with nonblast-related mTBI. I have also noticed that combat exposure severity does not seem to be correlated with severity of PTSD in this population. A study31 of military personnel with mTBI from blunt trauma, blast trauma, or both reported that any mTBI was associated with a greater incidence of PTSD than was no mTBI.
Distinguishing PTSD From mTBI
Dr Peskind: In veterans and active duty service members with mTBI, what symptoms distinguish PTSD from mTBI?
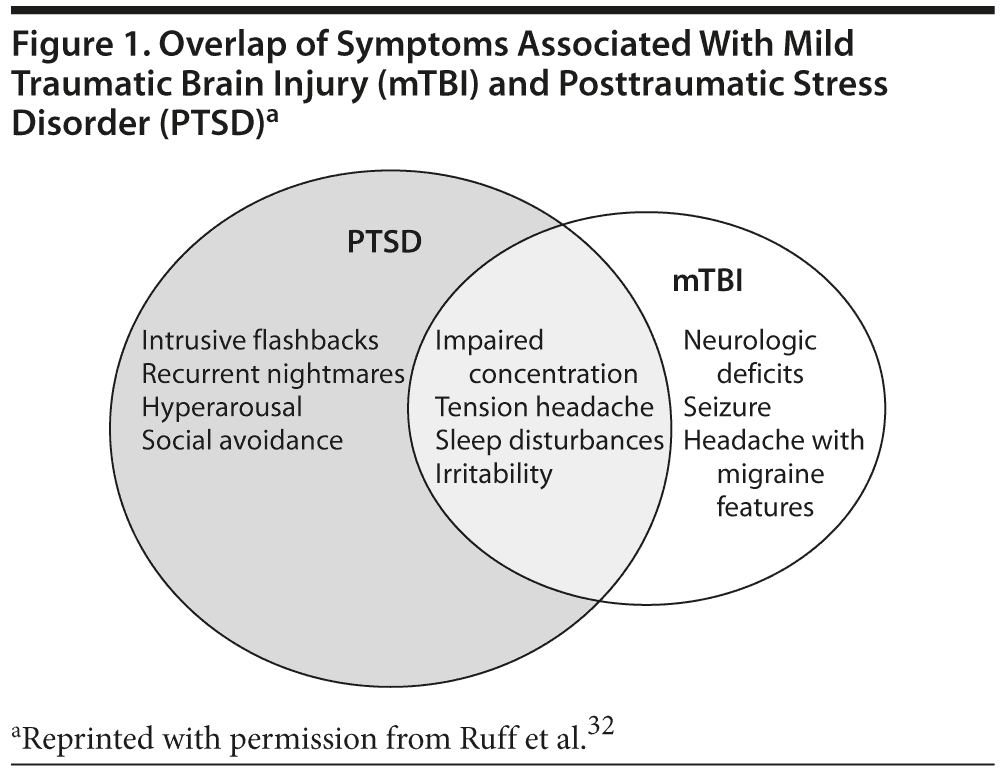
Dr Ruff: A number of postconcussive symptoms certainly can be equally attributable to PTSD, such as having difficulty falling or staying asleep, being irritable, and having poor concentration (Figure 1).32 Headaches are nonspecific symptoms, but the migraine features that can appear in both civilian and combat-related mTBI headaches are not characteristic manifestations of PTSD, nor are some of the subtle impairments in neurologic examinations that occur in people with combat-related mTBI.
Dr Peskind: My colleagues and I performed the Neurobehavioral Symptom Inventory in veterans with blast-induced mTBI.33 At least two-thirds of veterans endorsed several symptoms of moderate or severe intensity that are equally attributable to PTSD, such as anxiety, difficulty sleeping, irritability, and poor concentration. However, some symptoms they endorsed cannot be attributed to PTSD, such as migraine-type headache, ringing in the ears and hearing difficulty, and forgetfulness.
While areas of brain abnormality in people with PTSD overlap with those in people with mTBI,32 our neuroimaging data suggest that certain brain changes are specific to mTBI and appear regardless of the presence of PTSD.33
Repetitive TBI: Differences Between CTE and Other Neurodegenerative Disorders
Dr Peskind: Following multiple concussions, the development of CTE is a possibility. I recently diagnosed my first 2 cases of probable CTE in living persons. One is a 63-year-old retired professional football player who had a long prodrome with minor memory problems but more prominent behavior problems. Now, he is having more pronounced cognitive difficulties and meets criteria for dementia. Also, I have seen a 39-year-old war veteran who had an undiagnosed perinatal hypoxic injury that was found by imaging; he had asymmetric lateral ventricles. He had done very well in life—graduated from college, had a successful career—and then was deployed in the National Guard. He experienced 6 impact and blast concussions in Iraq and now has cognitive difficulties that meet criteria for dementia.
What are the neuropathological similarities and differences between CTE and other neurodegenerative disorders?
Dr McKee: The neuropathology of CTE, in most cases, is a pure tauopathy. In more than half of the individuals with CTE, you will not see the accumulation of β-amyloid, which develops in all instances of Alzheimer’s disease.8 Also, in the early stages, CTE has a prominent perivascular distribution of lesions. No other known tauopathy has a perivascular origin. This is hopefully a clue to its pathogenesis.
CTE also has a patchy and irregular neurodegeneration. That means that CTE does not affect the brain in a diffuse pattern like Alzheimer’s disease but instead tends to have focal hot spots. These focal hot spots are believed to be the result of the physical forces produced by the trauma; the damage is most severe where there are stress points in the brain, such as the depths of the cerebral sulcus, where the greatest degree of axonal injury is located.
Another distinction is that, in the late stages, CTE tends to affect widespread brain stem regions, specifically affecting the locus ceruleus and substantia nigra. That may be a clue as to why depression is so common, especially with the involvement of the locus ceruleus. We also see involvement of deep nuclei, like the thalamus and hypothalamus, which may contribute to sleep disorders and some of the cognitive issues that are seen in individuals with CTE.
Dr Peskind: And potentially pain. It strikes me that CTE looks nothing like Alzheimer’s disease. The long behavioral prodrome seems more like behavioral-variant frontotemporal dementia (FTD) followed by cognitive dysfunction, but CTE progresses much more slowly. In patients with probable CTE, I find the typical FTD presentation of loss of facial expression, flat affect, personality changes, and monotone speech, as well as the first cognitive changes that include neglecting personal hygiene and problems with executive function. However, patients’ memory is relatively intact.
Dr Cernak: How do you explain the localization of those changes in the deeper brain structures—the brain stem, locus ceruleus, thalamus, and hypothalamus—compared with the usual acceleration-deceleration concussion injuries, which are more on the surface of the cortical region?
Dr McKee: A number of long brain stem tracts are affected in acceleration-deceleration injuries, so I think some of the brain stem and thalamic involvement is from the acute injury. In people with progressive neurologic deterioration, tau is spread throughout the nervous system, but we do not know exactly how it spreads. Theories have suggested that a tauopathy is a prion or protein templating disorder,34 but other possibilities include glial to glial cell transmission or maybe secretion from different cells and reuptake through the extracellular fluid.35 The acute injury triggers the neurodegeneration in some people, but how the neurodegeneration progresses and, in its final stages, encompasses most of the CNS is still being studied.
Service Members and CTE
Dr Peskind: Dr McKee, you and your colleagues15 recently described postmortem cases of CTE in Iraq and Afghanistan veterans who had experienced blasts, and a similar case was published by Omalu and colleagues.36 What are the implications of these cases for our Iraq and Afghanistan veterans and service members?
Dr McKee: On the most basic level, these cases emphasize the need for the identification of acute blast or concussive injuries and proper management after the injury. The person needs to undergo a sophisticated set of examinations by medical professionals. The injured person needs to rest until he or she is asymptomatic and should not be allowed to go back to the battlefield until fully recovered.
We need to keep in mind that CTE is a possibility following concussions. Service members who have received blast or concussive injuries are at risk, although we do not know how great the risk is or how many individuals will be affected. The research gives the imperative to be able to diagnose this condition in living military personnel, as well as athletes, so that we can hopefully come up with ways of treating it and monitoring their progression.
Athletes and CTE
Dr Peskind: Recently, we have been hearing a lot in the news about professional football players with CTE. Why is this happening now?
Dr McKee: America’s favorite sport is football, and any time a disorder appears among popular players, it gets national attention. A number of high-profile athletes who have died, some by suicide, had requested that their brains be donated for scientific study, and their brains did show CTE.3,37 People have started to wonder how often this serious damage is happening in a sport that is so popular.
Dr Peskind: The average professional defensive lineman today weighs more than 300 pounds. To some degree, the risk of injury is purely physics. These huge players are also fast, and force equals mass times acceleration.
Dr McKee: The game has been ratcheted up in terms of the size, speed, and athleticism of the players. I think that the belief was that hits received while playing were inconsequential, but now we see that the damage can cause permanent deterioration. I think the game will be reassessed and eventually get safer.
Dr Cernak: In football players, hockey players, boxers, and those who play any contact or collision sport with high-velocity impact, the impact is not just to the head but to the whole body.31 Because of greater applied force on the brain, the sports in which the whole body can be exposed to a high-velocity impact may have a higher frequency of CTE compared with contact sports that do not have the potential for high-velocity, whole-body impact.3
Managing mTBI
Dr Peskind: What are the state-of-the-art procedures for clinical assessment and treatment or management of patients with repetitive mTBI?
Dr Brody: The state-of-the-art method for clinical assessment really is gathering a detailed history from the patient and, most importantly, gathering collateral history from a reliable source who has known the patient well both before and after the various injuries were sustained. Patients themselves are often not completely accurate. Medical records are typically unreliable or incomplete as well. Neurologic examinations and imaging are currently only partially helpful in assessment.
The patient’s history should be taken by someone who is well versed in the common complaints and difficulties following repetitive concussive TBIs. It is not enough to ask open-ended questions—instead, a hypothesis-testing approach should be used. Questions should be specific to symptoms that frequently occur, such as whether this person is having certain types of sleep difficulties, impulsivity, changes in personality, difficulty with controlling violent temper impulses, or difficulty with restraint in using drugs and alcohol or in spending money.
After assessment, we turn to the question of treatment or management. This condition has no cure or definitive treatment, but we can provide symptom management and we can comfort and educate the patient.4 I try to identify and address the primary problems that are causing the most distress to the patient, the collateral source, and the family.
I also provide information about prevention of further injuries to reduce the likelihood that this condition will progress or worsen. I spend a lot of time educating the patient and the collateral source on safety and prevention of risky behaviors. Sometimes the main form of care that clinicians can provide is education (see below).
Educational Resources About Mild Traumatic Brain Injury (mTBI)
Defense and Veterans Brain Injury Center
Free educational materials for service members, veterans, families, and clinicians
www.dvbic.org/resources
Centers for Disease Control
Free training and fact sheets for coaches, parents, athletes, and clinicians (Heads Up)
www.cdc.gov/concussion/sports
Brain Injury Association of America
Network of state affiliates, local chapters, and support groups to advance brain injury prevention, research, treatment, and education and to improve the quality of life for people affected by brain injury
www.biausa.org
PACE: Protecting Athletes Through Concussion Education
Program to encourage a preseason “baseline” evaluation of athletes for subsequent postinjury comparison
www.dsgpace.org
Dr Peskind: When my colleagues and I conduct studies of people with mTBI, we give the participants high-quality bicycle helmets. We also educate them about using seat belts in vehicles and taking safety precautions in skiing, skateboarding, mixed martial arts, and other sports that have a high risk of participants sustaining a brain injury.
Dr Brody: Management is more complex for a high-level athlete, like a collegiate athlete who has had multiple concussions and is now entering professional sports. For this type of person, a lot of his or her life, livelihood, and self-identity have been centered on that sport, and to stop playing it would be difficult.
Dr Ruff: While we are discussing symptom management and education, I want to comment about sleep disturbance, which is often reported by patients with mTBI.38 An α-1 blocker, prazosin, has been useful to improve sleep in people with PTSD.39-44 We also need to educate patients about behaviors that compromise their ability to sleep, such as engaging in shooter video games before going to bed or using power drinks during the day to increase their level of alertness and concentration.
Dr Peskind: Yes, young service members often overuse caffeine. I saw one soldier who drank two 2L bottles of high-caffeine soda per day to stay awake for his job. That sets up a vicious circle of sleep disturbance at night and daytime sleepiness.
Dr Brody, what should we tell patients about the prognosis of mTBI?
Dr Brody: Typically, I tell patients that the prognosis is highly variable. Unfortunately, I cannot give anyone a really accurate prognosis because not enough information is available to assess the severity of the damage done by repetitive mTBI; however, CTE is a possible outcome. This is a major area in which research needs to be done. For patients with a history of multiple concussions and probable CTE or some sort of dementia, I like to introduce them to a support group.
Children, Contact Sports, and mTBI
Dr Peskind: Athletes tend to start playing sports as children. Dr McKee, you have reported that symptoms of CTE have been seen in athletes as young as 25 years old.8
Dr McKee: Yes. That is a reason for us to reevaluate what we encourage our children to do. We want our children to have the healthiest future that they can possibly have, so we should be careful when allowing them to participate in contact sports. Parents need to know that their child’s coaching staff is well aware of what a concussion is, how to look for a concussion, and how to manage a concussion properly. Sports organizations for children should also limit the use of the head and hits to the head.
Dr Peskind: If you were a parent of a school-aged child today, would you allow him or her to play football or even soccer?
Dr McKee: I do not see any reason for playing football before high school. I would be concerned because so much remains unknown about children and concussions. Besides the games, players have to participate in so many practices. I would want to know about the quality of the medical surveillance and the knowledge of the coach as well as the other players, because often the individual does not know that he or she has been hit in a dangerous way.45 Safety depends on a collective awareness of the importance of these injuries and how they need to be treated.
Dr Brody: I would educate my children about the risks and benefits of sports. Sports, including football, definitely have benefits. Football is not a completely harmful activity. My advice is that if they play and they have one concussion, then they should probably stop. If they decide to go forward, they should understand the risks of doing so.
Dr Ruff: I would not try to prevent my grandchildren from engaging in sports because I think doing so would somewhat socially isolate them. If a single concussion occurs, the individual should be pulled out.
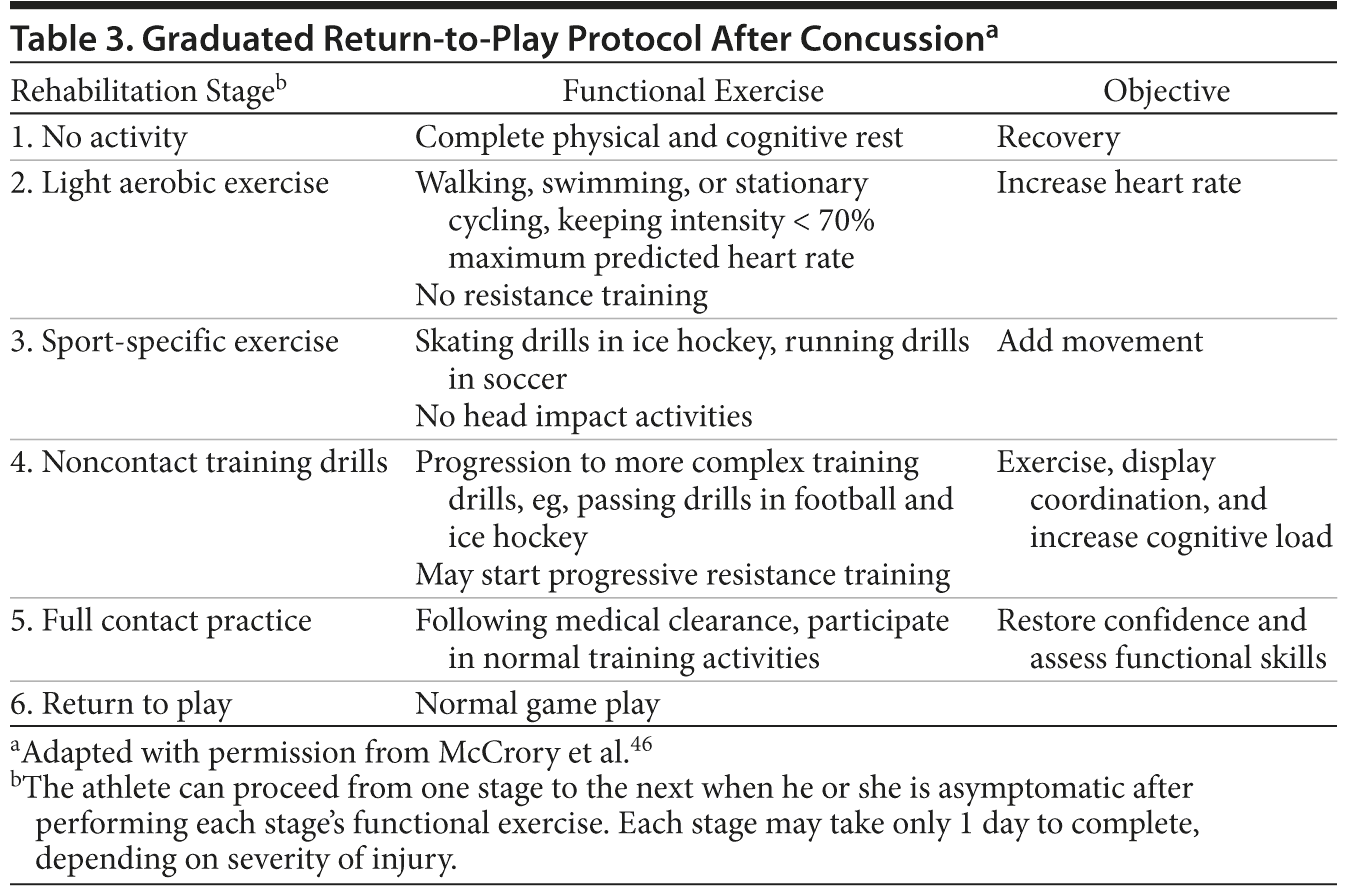
Dr Cernak: I agree that there are many benefits of sports, including football and soccer, and we cannot isolate our children in a bubble. We should teach them about recognizing the problem so that they are not afraid to say, “Oh, I hit my head and now I feel dizzy.” They should follow the return-to-play guidelines after impacts (Table 3).46
Dr Peskind: I have a granddaughter, and I suggest noncontact sports to her parents, like swimming or track.
Dr Cernak: Some sports promote teamwork better than others. In team sports, you have social development and group interactions that are precious later.
Dr Brody: Concussions are not a universal consequence of playing contact sports.
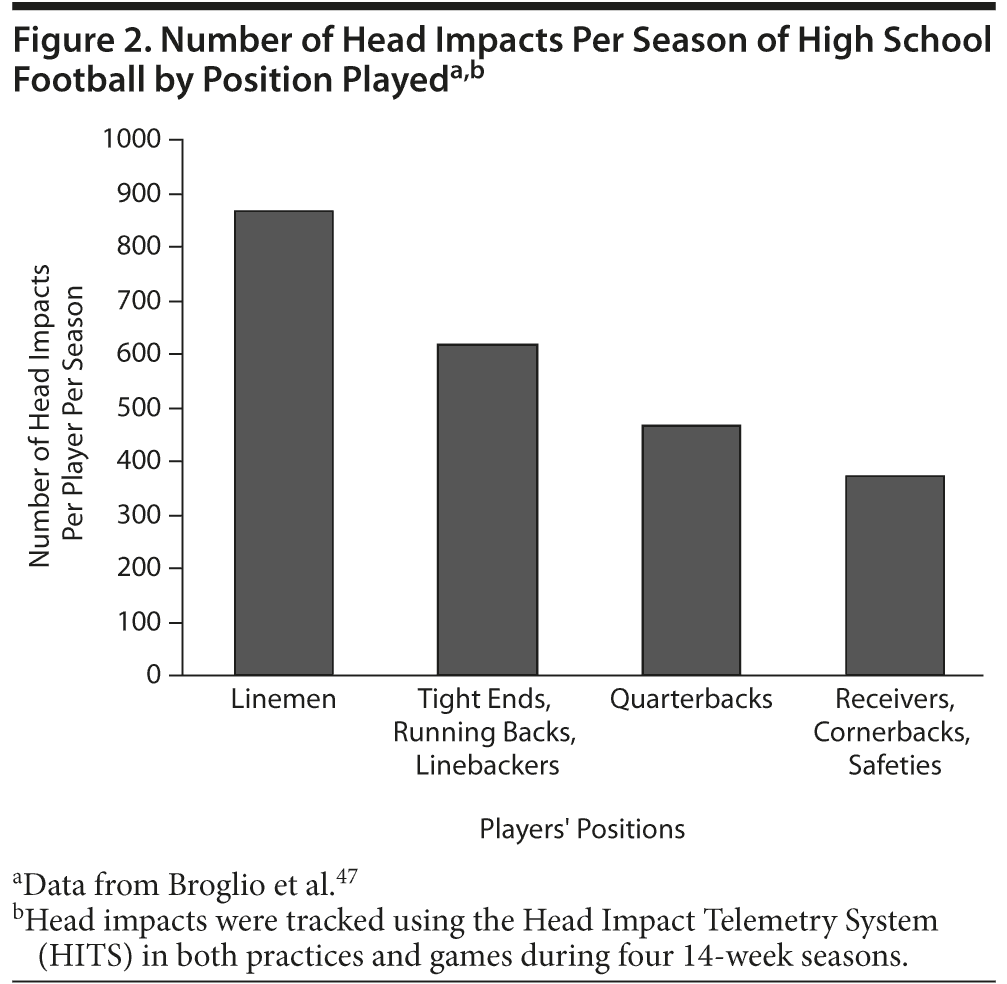
Dr McKee: I agree, but a subconcussive impact happens almost in every play of the game. Helmet-installed technology has shown that, in one season, a single player can experience nearly 900 head impacts in high school football and nearly 1500 head impacts in college football, depending on the position played, and many are subconcussive hits (Figure 2).47,48 So, we cannot use concussions as the only measurement of safety. Multiple subconcussive injuries may lead to brain health risks as well.49
Dr Brody: Subconcussive injuries may be substantial. However, I have asked collateral sources detailed questions about the functioning of players who have had multiple subconcussive injuries, and they do not seem to be having problems. This is clearly an area requiring further research.
Dr McKee: No, not everybody who plays football gets a neurodegenerative disorder, but subconcussive injury has the potential to lead to this problem.
Dr Brody: That is possible. A good topic for future investigation is how to assess for a subconcussive injury.
CONCLUSION
Concussions are more serious than previously believed. Brain injuries, especially multiple ones, can have serious negative impacts on patients, leading to changes in personality, sleep problems, and cognitive impairment and can increase the risk for suicide, PTSD, depression, and anxiety. In some people, repetitive mTBI can lead to CTE, a neurodegenerative disorder. As awareness and reporting of mTBI in both military and sports settings increase, evidence-based treatments and targeted suicide prevention strategies will hopefully emerge. Meanwhile, symptom management and education can help those who have already received concussions, and education and the use of return-to-play guidelines can contribute to prevention among youths.
Drug name: prazosin (Minipress and others).
Disclosure of off-label usage: The chair has determined that, to the best of her knowledge, prazosin is not approved by the US Food and Drug Administration for the treatment of headache and sleep disturbance in mTBI with PTSD.
REFERENCES
1. Elder GA, Cristian A. Blast-related mild traumatic brain injury: mechanisms of injury and impact on clinical care. Mt Sinai J Med. 2009;76(2):111-118. PubMed doi:10.1002/msj.20098
2. Marion DW, Curley KC, Schwab K, et al for the mTBI Diagnostics Workgroup. Proceedings of the military mTBI Diagnostics Workshop, St. Pete Beach, August 2010. J Neurotrauma. 2011;28(4):517-526. PubMed doi:10.1089/neu.2010.1638
3. Gavett BE, Stern RA, McKee AC. Chronic traumatic encephalopathy: a potential late effect of sport-related concussive and subconcussive head trauma. Clin Sports Med. 2011;30(1):179-188, xi. PubMed doi:10.1016/j.csm.2010.09.007
4. US Department of Veterans Affairs and Department of Defense. Clinical Practice Guideline for Management of Concussion/Mild Traumatic Brain Injury. Washington, DC: US Department of Veterans Affairs; 2009 http://www.healthquality.va.gov/mtbi/concussion_mtbi_full_1_0.pdf. Accessed January 8, 2013.
5. American Academy of Neurology and National Institute of Neurological Disorders and Stroke. Traumatic brain injury. Published 2013. http://www.aan.com/apps/disorders/index.cfm?event=database:disorder.view&disorder_id=1092. Accessed January 8, 2013.
6. McCrea M, Guskiewicz KM, Marshall SW, et al. Acute effects and recovery time following concussion in collegiate football players: the NCAA Concussion Study. JAMA. 2003;290(19):2556-2563. PubMed doi:10.1001/jama.290.19.2556
7. Saulle M, Greenwald BD. Chronic traumatic encephalopathy: a review. Rehabil Res Pract. 2012;2012:816069. PubMed
8. McKee AC, Cantu RC, Nowinski CJ, et al. Chronic traumatic encephalopathy in athletes: progressive tauopathy after repetitive head injury. J Neuropathol Exp Neurol. 2009;68(7):709-735. PubMed doi:10.1097/NEN.0b013e3181a9d503
9. McKee AC, Stein TD, Nowinski CJ, et al. The spectrum of disease in chronic traumatic encephalopathy. [published online ahead of print December 2, 2012]. Brain. doi:10.1093/brain/aws307. PubMed
10. Ruff RL, Riechers RGI 2nd, Wang X-F, et al. A case-control study examining whether neurological deficits and PTSD in combat veterans are related to episodes of mild TBI. BMJ Open. 2012;2(2):e000312. PubMed doi:10.1136/bmjopen-2011-000312
11. Vanderploeg RD, Belanger HG, Horner RD, et al. Health outcomes associated with military deployment: mild traumatic brain injury, blast, trauma, and combat associations in the Florida national guard. Arch Phys Med Rehabil. 2012;93(11):1887-1895. PubMed doi:10.1016/j.apmr.2012.05.024
12. Cernak I, Savic J, Ignjatovic D, et al. Blast injury from explosive munitions. J Trauma. 1999;47(1):96-103, discussion 103-104. PubMed doi:10.1097/00005373-199907000-00021
13. Cernak I. The importance of systemic response in the pathobiology of blast-induced neurotrauma. Front Neurol. 2010;1:151. PubMed
14. Cernak I, Ahmed FA. A comparative analysis of blast-induced neurotrauma and blunt-traumatic brain injury reveals significant differences in injury mechanisms. Med Data Rev. 2010;2(4):297-304.
15. Goldstein LE, Fisher AM, Tagge CA, et al. Chronic traumatic encephalopathy in blast-exposed military veterans and a blast neurotrauma mouse model. Sci Transl Med. 2012;4(134):134ra60. PubMed doi:10.1126/scitranslmed.3003716
16. Cernak I, Noble-Haeusslein LJ. Traumatic brain injury: an overview of pathobiology with emphasis on military populations. J Cereb Blood Flow Metab. 2010;30(2):255-266. PubMed doi:10.1038/jcbfm.2009.203
17. Mellor SG. The pathogenesis of blast injury and its management. Br J Hosp Med. 1988;39(6):536-539. PubMed
18. Koliatsos VE, Cernak I, Xu L, et al. A mouse model of blast injury to brain: initial pathological, neuropathological, and behavioral characterization. J Neuropathol Exp Neurol. 2011;70(5):399-416. PubMed doi:10.1097/NEN.0b013e3182189f06
19. Long JB, Bentley TL, Wessner KA, et al. Blast overpressure in rats: recreating a battlefield injury in the laboratory. J Neurotrauma. 2009;26(6):827-840. PubMed doi:10.1089/neu.2008.0748
20. Cernak I, Ignjatović D, Andelić G, et al. Metabolic changes as part of the general response of the body to the effect of blast waves [article in Serbian]. Vojnosanit Pregl. 1991;48(6):515-522. PubMed
21. Cernak I, Savic J, Malicevic Z, et al. Involvement of the central nervous system in the general response to pulmonary blast injury. J Trauma. 1996;40(suppl):S100-S104. PubMed doi:10.1097/00005373-199603001-00023
22. Cernak I, Savic VJ, Lazarov A, et al. Neuroendocrine responses following graded traumatic brain injury in male adults. Brain Inj. 1999;13(12):1005-1015. PubMed doi:10.1080/026990599121016
23. McAllister TW. Neurobiological consequences of traumatic brain injury. Dialogues Clin Neurosci. 2011;13(3):287-300. PubMed
24. Spencer RJ, Drag LL, Walker SJ, et al. Self-reported cognitive symptoms following mild traumatic brain injury are poorly associated with neuropsychological performance in OIF/OEF veterans. J Rehabil Res Dev. 2010;47(6):521-530. PubMed doi:10.1682/JRRD.2009.11.0181
25. Collen J, Orr N, Lettieri CJ, et al. Sleep disturbances among soldiers with combat-related traumatic brain injury. Chest. 2012;142(3):622-630. PubMed doi:10.1378/chest.11-1603
26. Teasdale TW, Engberg AW. Suicide after traumatic brain injury: a population study. J Neurol Neurosurg Psychiatry. 2001;71(4):436-440. PubMed doi:10.1136/jnnp.71.4.436
27. Brenner LA, Ignacio RV, Blow FC. Suicide and traumatic brain injury among individuals seeking Veterans Health Administration services. J Head Trauma Rehabil. 2011;26(4):257-264. PubMed doi:10.1097/HTR.0b013e31821fdb6e
28. Barnes SM, Walter KH, Chard KM. Does a history of mild traumatic brain injury increase suicide risk in veterans with PTSD? Rehabil Psychol. 2012;57(1):18-26. PubMed doi:10.1037/a0027007
29. Greenberg J, Tesfazion AA, Robinson CS. Screening, diagnosis, and treatment of depression. Mil Med. 2012;177(suppl):60-66. PubMed
30. Yurgelun-Todd DA, Bueler CE, McGlade EC, et al. Neuroimaging correlates of traumatic brain injury and suicidal behavior. J Head Trauma Rehabil. 2011;26(4):276-289. PubMed doi:10.1097/HTR.0b013e31822251dc
31. Kontos AP, Kotwal RS, Elbin R, et al. Residual effects of combat-related mild traumatic brain injury [published online ahead of print October 2, 2012]. J Neurotrauma. doi:10.1089/neu.2012.2506. PubMed
32. Ruff RL, Riechers RGI, Ruff SS. Relationships between mild traumatic brain injury sustained in combat and post-traumatic stress disorder. F1000 Med Rep. 2010;2:64. PubMed
33. Peskind ER, Petrie EC, Cross DJ, et al. Cerebrocerebellar hypometabolism associated with repetitive blast exposure mild traumatic brain injury in 12 Iraq war Veterans with persistent post-concussive symptoms. Neuroimage. 2011;54(suppl 1):S76-S82. PubMed doi:10.1016/j.neuroimage.2010.04.008
34. Guest WC, Silverman JM, Pokrishevsky E, et al. Generalization of the prion hypothesis to other neurodegenerative diseases: an imperfect fit. J Toxicol Environ Health A. 2011;74(22-24):1433-1459. PubMed doi:10.1080/15287394.2011.618967
35. Clavaguera F, Bolmont T, Crowther RA, et al. Transmission and spreading of tauopathy in transgenic mouse brain. Nat Cell Biol. 2009;11(7):909-913. PubMed doi:10.1038/ncb1901
36. Omalu B, Hammers JL, Bailes J, et al. Chronic traumatic encephalopathy in an Iraqi war veteran with posttraumatic stress disorder who committed suicide. Neurosurg Focus. 2011;31(5):E3. PubMed doi:10.3171/2011.9.FOCUS11178
37. Omalu B, Bailes J, Hamilton RL, et al. Emerging histomorphologic phenotypes of chronic traumatic encephalopathy in American athletes. Neurosurgery. 2011;69(1):173-183, discussion 183. PubMed doi:10.1227/NEU.0b013e318212bc7b
38. Hoge CW, McGurk D, Thomas JL, et al. Mild traumatic brain injury in US Soldiers returning from Iraq. N Engl J Med. 2008;358(5):453-463. PubMed doi:10.1056/NEJMoa072972
39. Germain A, Richardson R, Moul DE, et al. Placebo-controlled comparison of prazosin and cognitive-behavioral treatments for sleep disturbances in US Military Veterans. J Psychosom Res. 2012;72(2):89-96. PubMed doi:10.1016/j.jpsychores.2011.11.010
40. Calohan J, Peterson K, Peskind ER, et al. Prazosin treatment of trauma nightmares and sleep disturbance in soldiers deployed in Iraq. J Trauma Stress. 2010;23(5):645-648. PubMed doi:10.1002/jts.20570
41. Raskind MA, Peterson K, Williams T, et al. A trial of prazosin for combat trauma PTSD with nightmares in active duty soldiers returned from Iraq and Afghanistan. Am J Psychiatry. In press.
42. Raskind MA, Thompson C, Petrie EC, et al. Prazosin reduces nightmares in combat veterans with posttraumatic stress disorder. J Clin Psychiatry. 2002;63(7):565-568. PubMed doi:10.4088/JCP.v63n0705
43. Raskind MA, Peskind ER, Kanter ED, et al. Reduction of nightmares and other PTSD symptoms in combat veterans by prazosin: a placebo-controlled study. Am J Psychiatry. 2003;160(2):371-373. PubMed doi:10.1176/appi.ajp.160.2.371
44. Ruff RL, Ruff SS, Wang XF. Improving sleep: initial headache treatment in OIF/OEF veterans with blast-induced mild traumatic brain injury. J Rehabil Res Dev. 2009;46(9):1071-1084. PubMed doi:10.1682/JRRD.2009.05.0062
45. McCrea M, Hammeke T, Olsen G, et al. Unreported concussion in high school football players: implications for prevention. Clin J Sport Med. 2004;14(1):13-17. PubMed doi:10.1097/00042752-200401000-00003
46. McCrory P, Meeuwisse W, Johnston K, et al. Consensus statement on concussion in sport: the 3rd International Conference on Concussion in Sport held in Zurich, November 2008. Br J Sports Med. 2009;43(suppl 1):i76-i90. PubMed doi:10.1136/bjsm.2009.058248
47. Broglio SP, Eckner JT, Martini D, et al. Cumulative head impact burden in high school football. J Neurotrauma. 2011;28(10):2069-2078. PubMed doi:10.1089/neu.2011.1825
48. Crisco JJ, Fiore R, Beckwith JG, et al. Frequency and location of head impact exposures in individual collegiate football players. J Athl Train. 2010;45(6):549-559. PubMed doi:10.4085/1062-6050-45.6.549
49. Stern RA, Riley DO, Daneshvar DH, et al. Long-term consequences of repetitive brain trauma: chronic traumatic encephalopathy. PM R. 2011;3(suppl 2):S460-S467. PubMed doi:10.1016/j.pmrj.2011.08.008
This PDF is free for all visitors!