Alzheimer’s Disease:
Implications of the Updated
Diagnostic and Research Criteria
Alzheimer’s disease (AD) is the most common form of disabling cognitive impairment in older people. AD dementia has been estimated to affect an estimated 5.4 million Americans, and by 2050, it is projected to affect about 13.5 million older US adults.1,2 According to the World
Alzheimer’s Report,3 the number of afflicted people and the associated costs of AD are projected to skyrocket around the world due to the growing number of people living to older ages.
In 1984, Work Groups for the National Institute of Neurological and Communicative Disorders and Stroke (NINCDS) and the Alzheimer’s
Disease and Related Disorders Association (ADRDA, more commonly known as the Alzheimer’s Association) developed the original clinical diagnostic
criteria for AD.4 At that time, AD was considered a discrete clinicopathological entity, requiring evidence of dementia and likely or confirmed evidence of moderate-to-severe AD neuropathology.5
Progress in research during the past 27 years has led investigators to
reconceptualize AD as a progressive sequence of biological changes, some of which can be measured using brain imaging and other biomarkers, which roughly correspond to preclinical and increasingly severe clinical stages of the disorder. Among several findings, researchers have shown that many patients with mild cognitive impairment (MCI) have biological evidence of AD and are at increased risk for progression to AD dementia6; identified pathophysiologic evidence of AD years before the onset of symptoms in cognitively normal people at increased risk for MCI and dementia due to AD; suggested that AD-modifying treatments might have the most profound
effect if started before the onset of symptoms, when extensive neuropathology may already be evident; and characterized other disease processes that may contribute to disabling cognitive impairment (eg, Lewy bodies and vascular disease) in patients with or without pathophysiologic evidence of AD.
To begin the process of revising the diagnostic criteria, the National Institute on Aging (NIA) and the Alzheimer’s Association held advisory meetings in 2009, during which attendees agreed that 3 separate work groups be formed in relationship to the dementia, MCI, and preclinical stages of AD.7 The work groups were asked to review scientific progress, propose diagnostic criteria for dementia due to AD and dementia due to MCI, and begin to establish research criteria for preclinical stages of AD. Five of the work group members participated in this Commentary discussion: Guy M. McKhann, MD, chaired the work group on AD dementia, as well as the work group that proposed the original NINCDS/ADRDA diagnostic criteria in 1984. Marilyn S. Albert, PhD, chaired the work group on MCI due to AD. Ronald C. Petersen, MD, PhD (a pioneer in MCI research), served as a member of the MCI due to AD work group. Reisa A. Sperling, MD, chaired the work group on preclinical AD, and Eric M. Reiman, MD, served as a member; both of these investigators have been actively involved in the use of brain imaging techniques in the preclinical stages of AD.
The recommendations established by each work group were presented at the 2010 International Conference on Alzheimer’s Disease and were posted on the Alzheimer’s Association’s Web site for public review. After submitted comments were incorporated by the work groups as appropriate, a subcommittee reviewed the semi-final publications and made additional revisions, and then the publications were submitted for peer review. The criteria were published online ahead of print (Table 1)7 just before this Commentary discussion occurred.8,9

In addition to the NIA and the Alzheimer’s Association, other organizations have been actively involved in the development of revised diagnostic criteria for AD. The American Psychiatric Association (APA) began the process for revising the Diagnostic and Statistical Manual of Mental Disorders (DSM), including the diagnostic criteria for AD dementia, over a decade ago. After several rounds of planning conferences and white paper submissions, a task force was formed and work group members were vetted and selected by 2008.
For AD, the DSM-5 Neurocognitive Disorders Work Group, of which Deborah Blacker, MD, ScD, and Dr
Petersen are members, developed a proposal10 based on literature reviews, data analyses, and questions, comments,
and concerns submitted to the APA via a DSM-5 preview Web site. In the proposed criteria, the work group recommended that the chapter be renamed “Neurocognitive Disorders” rather than the former “Delirium, Dementia, Amnestic, and Other Cognitive Disorders.” This would include delirium and major and mild neurocognitive disorders, of which AD would be an etiologic subtype. Currently, field testing is being conducted with the proposed criteria, and, after revising the criteria
according to the field test results, the DSM-5 is slated to be published in 2013.
In addition, Bruno Dubois and colleagues in the International Working Group for New Research Criteria for the Diagnosis of AD11 have proposed research criteria to capitalize on the development of promising brain imaging and cerebrospinal fluid (CSF) AD biomarkers in patients with dementia and MCI. Dr Petersen also served as a member of this working group.
Despite some differences in the terminology and intended use of the NIA/Alzheimer’s Association diagnostic and
research criteria, DSM-5 diagnostic criteria (in development), and International Working Group Research Criteria, each has a number of common elements, and all are intended to reflect a work in progress, subject to modification with new research developments. The following discussion is
intended to put the new and proposed criteria into context and to give clinicians practical advice about the NIA/
Alzheimer’s Association criteria.
Why Revise the Original
NINCDS/ADRDA Diagnostic Criteria for AD?
Dr McKhann: The original criteria were developed
because we recognized that AD was going to become a
serious problem as the population aged and that we needed consistent, clinically applicable diagnostic criteria. The original criteria were meant to be preliminary but somehow lasted without revision until now.
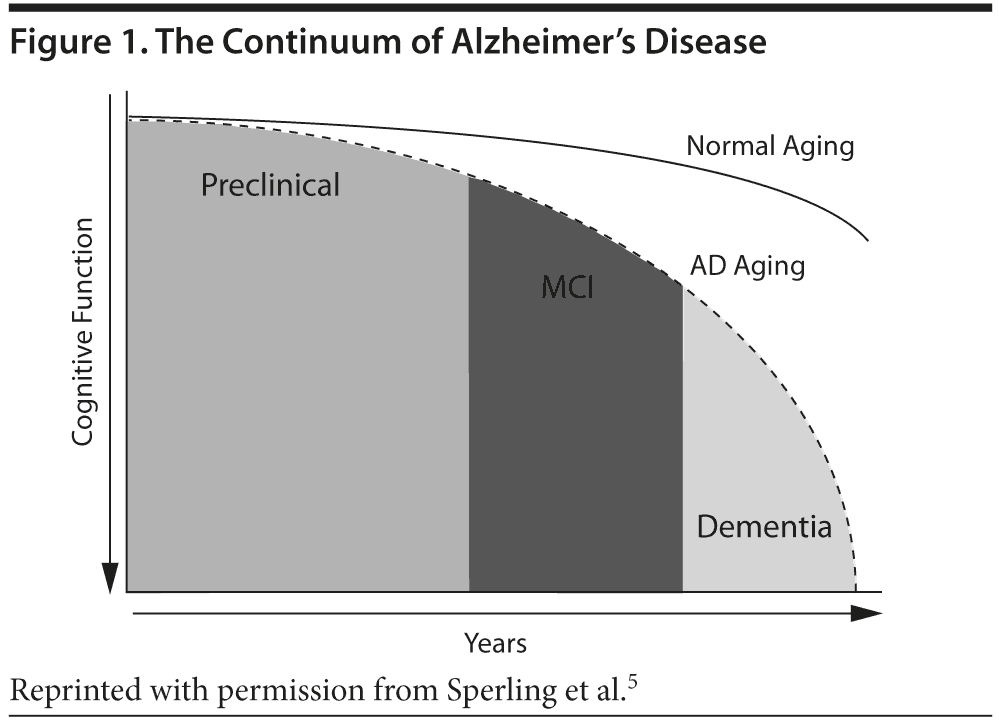
Several limitations of the original criteria existed, which
at the time either were not considered or were unknown. One limitation is the lack of the concept that AD progresses over time and manifests over a continuum (Figure 1).7 The disease starts long before patients present with impairment, possibly a decade or longer. Therefore, we should consider the possibility that AD pathophysiology can be detected preclinically via biomarker evidence, although it is not yet known whether everyone with preclinical biomarker evidence of AD pathophysiology progresses to the clinical phases of the illness. Additionally, most biomarkers did not exist 27 years ago; imaging was primarily used to rule out other diagnostic entities rather than used as a measure of the disease itself. Those are some of the factors that prompted this revision.
Another limitation of the original criteria is the lack of discussion concerning causes of dementia other than AD, such as dementia with Lewy bodies, frontotemporal dementia (FTD), and vascular dementia.
Dr Albert: The reconceptualization of AD as existing on
a continuum was a major advancement, particularly the
concept of MCI due to AD. From a clinical perspective,
patients with mild symptoms who did not have dementia were a critical population to address. Further, the concept of MCI had become widely accepted, largely based on work initiated by Dr Petersen and his colleagues.6,12,13
What Are the Main Take-Home Messages Concerning the Reconceptualization of AD?
Dr Albert: I would like to emphasize at least 3 take-home messages: (1) Viewing AD as existing on a spectrum is critical. Alzheimer’s pathophysiologic processes begin in individuals who are cognitively normal, accumulate and are prevalent among those with MCI, and then cause the onset of AD dementia. Therefore, dementia is at the end of the spectrum and does not cover the entire range of individuals with AD pathology. (2) Wide consensus exists concerning the core clinical criteria for AD dementia and for MCI due to Alzheimer’s pathology. (3) The implementation of biomarkers in research can help to elucidate the underlying pathology of clinical symptoms. I stress the research use of biomarkers because they are not yet clinically applicable; however, this research will help to advance the field to the point where biomarkers may be used in clinical care.
How Have Advancements in Biomarker Identification Influenced the Reconceptualization of AD?
Dr Sperling: As Dr Albert explained, the tremendous
advances in the identification of biomarkers have allowed us to link clinical symptoms to the possible underlying etiology of MCI and AD dementia. We can also now detect early neuropathologic evidence of Alzheimer’s pathology in patients who are clinically normal. Although we have identified early AD pathology via autopsies of older, clinically normal adults, biomarkers now allow us to detect this evidence in vivo, which presents an opportunity for longitudinal follow-up, again, to try to link the pathology to the eventual clinical course.
Dr Petersen: Also, patients with clinically diagnosed MCI have biomarkers that consistently fall between normal aging and dementia on the AD spectrum as evidenced in studies using magnetic resonance imaging (MRI), fluorodeoxyglucose positron emission tomography (FDG PET), and CSF assays (Table 2).14–16 These results corroborate the AD continuum concept showing that the pathophysiology is present at the MCI phase of AD, although not as severe as in the dementia phase. Thus, we may be able to detect AD much earlier than we could when the original NINCDS/ADRDA diagnostic criteria were developed.

What Advice Would You Give Clinicians Regarding the Use of Neuroimaging,
CSF Biomarkers, and Genetic Testing
to Assess Patients for Prodromal
AD, MCI, or Dementia?
Dr McKhann: Alzheimer’s dementia and MCI due to AD are clinical entities, and the clinical criteria have not changed much for practicing physicians. A major problem is applying
biomarkers in the diagnosis of MCI and AD. The use of
imaging and other biomarkers is not yet readily available or fiscally feasible in many clinical settings. Additionally, the use of biomarkers for preclinical detection and for clinical diagnosis is in a stage of evolution, and measurement is not yet standardized for practical purposes. Therefore, our recommendation at this time is that AD biomarkers be used primarily in
research settings. Additional data are needed to clarify their role in clinical settings.
Dr Albert: Complete knowledge about biomarkers is still lacking, which is why the work groups reached a consensus that biomarkers be primarily used in research. As Dr McKhann stated, we have not established standardized measurement of biomarkers, which will account for the variability across institutions as well as establish cut-off points for distinguishing a diseased state from a normal state. Additionally, a majority of the research that has been conducted on biomarkers has focused on select populations. We need community studies to determine how using biomarkers will operate in real-world settings and to obtain generalizable and replicable results. So, much more work needs to be done before biomarkers can routinely be used in clinical practices.
Dr Petersen: And yet, some of these tests are available in clinical practice, which may present a conundrum for practitioners. For example, many clinicians would obtain an MRI scan for a patient who presents with memory impairment. Then, without standardization, interpreting the results
becomes an issue.
In the meantime, practicing physicians can become more comfortable with looking at these scans and examining the relevant areas of the brain that may be involved early in the disease process, which may signal whether there is an underlying degenerative process, in addition to recognizing the other exclusionary information the MRI provides. Similarly, CSF tests are commercially available, although their predictive ability for disease progression has not been validated. Some insurance companies do reimburse for the use of FDG PET scans in the differential diagnosis of AD and FTD.
Therefore, becoming familiar with the tools through which biomarkers can be detected is advantageous for clinicians, although actually using those tools in practice at this time is not recommended.
Dr Sperling: To clarify, we are also not recommending neuroimaging or CSF assays for people who are asymptomatic or who are considered clinically normal and are not concerned about their memory.
Dr Blacker: Right. As Dr Albert pointed out, much research
still needs to be done in community populations.
Dr Petersen: Some people have suggested that the role of genetic testing was underplayed in the new criteria.
Dr McKhann: The work groups for the NIA/Alzheimer’s
Association criteria discussed genetic testing, and we wanted to be very cautious about this topic. Therefore, we included very little about the genetic aspects of AD in the publications.
What Factors Will Influence Your Use
and Interpretation of Amyloid PET Scans (When They Become Available) or
CSF Amyloid and Tau Assays?
Dr Petersen: At least one of the amyloid-labeling ligands may soon be approved for use in PET scans to detect the presence of amyloid plaques in the brain. A negative scan would show that amyloid plaques are not present, which may provide useful information to clinicians. However, once the imaging technique is available, clinicians probably will scan to see if amyloid plaques are present to account for the particular syndrome with which the patient is presenting.
Although it will be interesting to see how amyloid-labeling
ligands are used, I caution that these are still research techniques and their future clinical implications are yet to be determined, particularly regarding the time frame of disease progression. For example, if a patient presents with a certain degree of cognitive impairment and if evidence of the presence of amyloid is found, either by CSF assays or neuroimaging, this result indicates that the disease will probably progress, but at what rate is unknown. Other measures, such as FDG PET, MRI, and CSF tau assays, may provide additional information as to the rate of disease progression for individual patients. Overall, more longitudinal data are needed
before we can appropriately interpret biomarker results.
Dr Sperling: I completely agree and believe that finding negative results may be the greatest utility at this time for PET amyloid scans or CSF assays. Although these tests have limitations and cannot rule out AD, the data thus far suggest that these techniques are fairly sensitive in detecting amyloid plaques. Therefore, if a patient has AD dementia and does not have the presence of amyloid plaques in an imaging scan or spinal tap, then clinicians may need to re-evaluate the AD
diagnosis and perhaps pursue additional tests or patient history. Finding an absence of amyloid plaques may be particularly helpful for patients who have an unusual clinical course or suspected early-onset AD. While nearly one-third of cognitively normal older adults may have a positive amyloid PET scan, more information is needed to determine what happens to these individuals over time. Until we have more information from longitudinal research studies or prevention trials, we do not recommend the clinical use of amyloid
imaging to predict whether or when cognitively normal people might develop symptoms.
How Will the Proposed Criteria Advance
the Scientific Understanding,
Treatment, and Prevention of AD?
Dr Sperling: The new criteria can help us to begin planning and then, hopefully, implementing prevention trials of possible biologically active agents. The work group on preclinical AD developed the criteria around the idea of finding a specific population at risk for MCI due to AD and AD dementia. We could use biomarkers to track disease progression in response to therapy in these individuals and use the emergence of clinical or cognitive impairment as an endpoint. So, my hope is that these criteria will move us to conduct studies of treatment earlier in the disease process.
Dr McKhann: I would like to emphasize the paradigm shift that is coupled with conducting earlier treatment trials. A majority of previous treatment trials have been conducted in AD dementia, most of which have not had promising clinical implications, possibly due to the irreversible neurodegeneration experienced in the late stage of the illness. As Dr Sperling said, we need to shift the emphasis from treating AD dementia to identifying preclinical AD and using therapies that prevent its conversion to MCI and dementia. Pharmaceutical companies and the US Food and Drug Administration (FDA) both appear to be moving in this direction as well.
Dr Petersen: It is incumbent upon the field to demonstrate the validity and utility of biomarkers. Currently, studies are being designed and conducted in the MCI phase of AD using imaging and other biomarkers to determine if the biomarkers correspond as expected with the clinical disease progression. Ideally, patients would respond to treatment at this phase of illness and the biomarkers would respond accordingly, establishing them as potential surrogate markers for the prevention trials described by Dr Sperling. So, I think these criteria are important to lend some credibility to the earlier stages of AD and to the use of biomarkers, either to stratify the populations or eventually as outcomes themselves.
Dr Reiman: While we will never give up on the effort to find demonstrably effective treatments for those patients in the most severe stages of AD, we have an opportunity to evaluate some of the most promising treatments at earlier clinical and preclinical stages when they might have the most profound benefit.
What DSM-5 Terminology and Criteria May Be Anticipated, and How Do They Compare With the NIA/Alzheimer’s Association Criteria?
Dr Petersen: The DSM-5 category of neurocognitive disorders will describe not only the AD spectrum but also other forms of dementia and other causes of cognitive impairment. Nevertheless, the DSM will include criteria corresponding to 2 of the 3 stages of AD articulated in the NIA/Alzheimer’s Association criteria and reflecting an increasingly severe continuum: (1) mild neurocognitive disorder, which is comparable to MCI, and (2) major neurocognitive disorder, which is consistent with dementia. The DSM has not previously included a predementia phase of cognitive impairment, so this development is new. The addition of preclinical AD criteria to the DSM-5 is unlikely, as they have no diagnostic utility at this time. Currently, the proposed DSM-5 criteria are undergoing field trials to test the criteria in various clinical settings. The criteria will then be revised and are slated to be published in 2013.
Dr Blacker: In general, the DSM-5 Neurocognitive Disorders Work Group is trying to harmonize with expert groups on all etiologic subtypes. The work group was aware of the impending release of the NIA/Alzheimer’s Association criteria, and plans to revise its earlier draft of the criteria for major and mild neurocognitive disorder due to AD to harmonize with the NIA/Alzheimer’s Association criteria described here. Although the criteria are similar, the DSM-5 has a broader mandate in terms of being used not only in clinical settings but also in legal and clerical settings. Therefore, the DSM criteria must be clear and concrete. But the
2 sets of criteria will be similar and would be used similarly by clinicians.
What Advice Would You Give
Clinicians Trying to Grapple
With These Various New Criteria?
Dr Petersen: Several criteria are emerging, including those from the NIA/Alzheimer’s Association, the DSM-5, and also one we have not discussed, the International
Working Group for New Research Criteria for the Diagnosis of AD by Dubois et al.11 All of these criteria have a similar conceptual foundation, but some differ regarding the clinical characterization of diagnostic qualification for patients and specifics for using biomarkers and genetic testing.
Dr McKhann: Keep in mind that many of the criteria focused primarily on research purposes, particularly those from the NIA/Alzheimer’s Association and the International Working Group for New Research Criteria for the Diagnosis of AD. Therefore, practicing clinicians will not need to implement a majority of the recommendations.
What Cognitive Tests Can
Clinicians Use to Help Assess MCI?
Dr Petersen: Memory impairment is central to most clinical presentations along the AD spectrum, and clinicians need to be sensitive to some assessment of memory. However, caution should be used for tools that require a minimal amount of recall (eg, 3 words) from patients after only a brief period of time has passed, such as is done with the Mini-Mental State Examination. To truly assess memory, several items should be listed and followed by other cognitive activities and a substantial delay (eg, 10 to 30 minutes) before the patient is asked to recall the listed items. This method would allow patients more time to forget the items, which is a cardinal symptom present early in the development of AD and in mediotemporal lobe impairment. Although not all presentations of MCI with an AD substrate have memory loss, most clinicians would benefit from using an episodic memory assessment tool to evaluate patients.
Dr Albert: In the criteria for MCI due to AD, we recommended several appropriate tests that assess both immediate and delayed recall as well as other cognitive abilities, and they are helpful in identifying patients with MCI who are likely to develop AD dementia (Table 3).6 If formal tests are not available, informal tests may be used; however, informal tests are unlikely to be sensitive to the subtle memory problems seen in patients with early-stage MCI. Because patients are often impaired in several domains, not just in memory, multiple tests may need to be conducted to obtain a thorough and accurate clinical assessment.

What Work Remains to Support
or Further Develop the Research
and Diagnostic Criteria?
Dr Albert: The most pressing work that needs to be done is conducting community studies, establishing a standardization for the use of biomarkers, and verifying the longitudinal course of biomarkers during disease progression.
Dr Sperling: The community studies need to be completed in all 3 phases of the illness, particularly the preclinical phase. Compared with the general population, many volunteers for research studies have a higher socioeconomic status and a higher level of education. We need to get a better sense of whether epidemiologically-based community samples will reflect evidence of early AD pathology in the same proportions and at the same rate of progression as shown in the research groups.
Dr Petersen: Also, do the clinical criteria augmented with biomarkers function the same across age groups, eg, individuals aged 60 to 70 years versus individuals aged
80 years and older?
Dr McKhann: And, to emphasize Dr Petersen’s remarks, we do not yet know if the biomarkers will change with
effective treatment of AD. So, we need to know: (1) the progression of biomarkers in relation to disease state, both treated and untreated, and (2) if some neurodegeneration is potentially reversible, which is critical. A separate work group is evaluating pathological criteria in relation to the new clinical criteria.5
Dr Sperling: After the new criteria were published online, I received some criticism from colleagues about how cautious we were with regard to the implementation of biomarkers. From the comments in this discussion, I think that we all recognize that there is much that we still have to learn.
Disclosure of off-label usage: Dr Reiman has determined that, to the
best of his knowledge, no investigational information about pharmaceutical agents that is outside US Food and Drug Administration–approved labeling has been presented in this activity—other than the hopeful but cautious approach the experts expressed as amyloid PET and other AD biomarkers continue to be developed.
Financial disclosure: Dr Reiman has been a consultant for Amnestix, AstraZeneca, Bayer, Eisai, Elan, Eli Lilly, GlaxoSmithKline, Novartis, Siemens, and Takeda; his institution has received research grant support from AstraZeneca and Avid/Eli Lilly; he and his colleagues have proposed an “Alzheimer’s Prevention Initiative” to accelerate the evaluation of preclinical AD treatments; and he was a member of the NIA/Alzheimer’s Association Preclinical AD Work Group. Dr Albert has been a consultant for Eli Lilly and Genentech and has received grant/research support through Johns Hopkins University from GE Healthcare. Dr Petersen has been a consultant for Pfizer (Data Monitoring Committee), Janssen (Alzheimer’s Immunotherapy Data Monitoring Committee), Elan, and GE Healthcare. Dr Sperling has been a consultant for Pfizer, Janssen, Elan, Bristol-Myers Squibb, Bayer, Avid, Link, and Esai; has
received grant/research support from Bristol-Myers Squibb, Janssen,
and Elan; and has received honoraria from Pfizer and Avid (symposia). Drs Blacker and McKhann have no personal affiliations or financial relationships with any commercial interest to disclose relative to the activity.
References
1. Alzheimer’s Association, Thies W, Bleiler L. 2011 Alzheimer’s disease facts and figures. Alzheimers Dement. 2011;7(2):1–63. http://www.alz.org/downloads/Facts_Figures_2011.pdf. Accessed May 13, 2011. PubMed doi:10.1016/S1552-5260(11)00040-9
2. Alzheimer’s Association. Changing the Trajectory of Alzheimer’s
Disease: A National Imperative. Chicago, IL: Alzheimer’s Association; 2010. http://www.alz.org/documents_custom/trajectory.pdf. Accessed May 13, 2011.
3. Alzheimer’s Disease International. World Alzheimer Report 2010: The Global Economic Impact of Dementia. London, United Kingdom: Alzheimer’s Disease International; 2010. http://www.alz.org/documents/national/World_Alzheimer_Report_2010.pdf. Accessed July 5, 2011.
4. McKhann G, Drachman D, Folstein M, et al. Clinical diagnosis of Alzheimer’s disease: report of the NINCDS-ADRDA work group
under the auspices of Department of Health and Human Services
Task Force on Alzheimer’s Disease. Neurology. 1984;34(7):939–944. PubMed
5. Jack CR Jr, Albert MS, Knopman DS, et al. Introduction to the recommendations from the National Institute on Aging–Alzheimer’s Association workgroups on diagnostic guidelines for Alzheimer’s disease. Alzheimers Dement. 2011;7(3):257–262. http://download.journals.elsevierhealth.com/pdfs/journals/1552-5260/PIIS1552526011001002.pdf. Accessed August 5, 2011. PubMed doi:10.1016/j.jalz.2011.03.004
6. Grundman M, Petersen RC, Ferris SH, et al, for the Alzheimer’s Disease Cooperative Study. Mild cognitive impairment can be distinguished from Alzheimer disease and normal aging for clinical trials. Arch Neurol. 2004;61(1):59–66. doi:10.1001/archneur.61.1.59 PubMed
7. Sperling RA, Aisen PS, Beckett LA, et al. Toward defining the preclinical stages of Alzheimer’s disease: recommendations from the National Institute on Aging–Alzheimer’s Association workgroups on diagnostic guidelines for Alzheimer’s disease. Alzheimers Dement. 2011;7(3):280–292. http://download.journals.elsevierhealth.com/pdfs/journals/1552-5260/PIIS1552526011000999.pdf. Accessed August 5, 2011. PubMed doi:10.1016/j.jalz.2011.3.003
8. Albert MS, Dekosky ST, Dickson D, et al. The diagnosis of mild cognitive impairment due to Alzheimer’s disease: recommendations from the National Institute on Aging–Alzheimer’s Association workgroups on diagnostic guidelines for Alzheimer’s disease. Alzheimers Dement. 2011;7(3):270–290. http://download.journals.elsevierhealth.com/pdfs/
journals/1552-5260/PIIS155252601100104X.pdf. Accessed
August 5, 2011. PubMed doi:10.1016/j.jalz.2011.03.008
9. McKhann GM, Knopman DS, Chertkow H, et al. The diagnosis of dementia due to Alzheimer’s disease: recommendations from the National Institute on Aging–Alzheimer’s Association workgroups on diagnostic guidelines for Alzheimer’s disease. Alzheimers Dement. 2011;7(3):263–269. http://download.journals.elsevierhealth.com/pdfs/journals/1552-5260/PIIS1552526011001014.pdf. Accessed August 5, 2011. PubMed doi:10.1016/j.jalz.2011.03.005
10. Jeste DV, Blacker D, Blazer D, et al. Neurocognitive disorders: a proposal from the DSM-5 Neurocognitive Disorders Work Group. American Psychiatric Association. http://www.dsm5.org/Proposed%20Revision%20Attachments/APA%20Neurocognitive%20Disorders%20Proposal%20for%20DSM-5.pdf. Published January 7, 2010. Accessed May 10, 2011.
11. Dubois B, Feldman HH, Jacova C, et al. Revising the definition of Alzheimer’s disease: a new lexicon. Lancet Neurol. 2010;9(11):
1118–1127. doi:10.1016/S1474-4422(10)70223-4 PubMed
12. Gauthier S, Reisberg B, Zaudig M, et al, for the International Psychogeriatric Association Expert Conference on mild cognitive
impairment. Mild cognitive impairment. Lancet. 2006;367(9518):
1262–1270. PubMed doi:10.1016/S0140-6736(06)68542-5
13. Petersen RC, O’Brien J. Mild cognitive impairment should be considered for DSM-V. J Geriatr Psychiatry Neurol. 2006;19(3):147–154. doi:10.1177/0891988706291085 PubMed
14. Landau SM, Harvey D, Madison CM, et al, for the Alzheimer’s Disease Neuroimaging Initiative. Comparing predictors of conversion and
decline in mild cognitive impairment. Neurology. 2010;75(3):230–238. PubMed doi:10.1212/WNL.0b013e3181e8e8b8
15. Smith EE, Egorova S, Blacker D, et al. Magnetic resonance imaging white matter hyperintensities and brain volume in the prediction of mild
cognitive impairment and dementia. Arch Neurol. 2008;65(1):94–100. PubMed doi:10.1001/archneurol.2007.23
16. Oghabian MA, Batouli SA, Norouzian M, et al. Using functional Magnetic Resonance Imaging to differentiate between healthy aging subjects, Mild Cognitive Impairment, and Alzheimer’s patients. J Res Med Sci. 2010;15(2):84–93. PubMed




