Because this piece does not have an abstract, we have provided for your benefit the first 3 sentences of the full text.
To the Editor: Drug reaction with eosinophilia and systemic symptoms (DRESS) is a potentially life-threatening, delayed-onset drug reaction that is typically characterized by skin eruption and fever. DRESS can include eosinophilia, atypical lymphocytes, lymphadenopathy, and internal organ involvement. The clinical presentation is variable; patients exhibit a wide array of signs and symptoms that do not always present concurrently. This heterogeneity can result in missing or delaying the diagnosis, with harmful consequences for the patient.
This work may not be copied, distributed, displayed, published, reproduced, transmitted, modified, posted, sold, licensed, or used for commercial purposes. By downloading this file, you are agreeing to the publisher’s Terms & Conditions.
US Food and Drug Administration Warning About the Risk of Drug Reaction with Eosinophilia and Systemic Symptoms With Ziprasidone
To the Editor: Drug reaction with eosinophilia and systemic symptoms (DRESS) is a potentially life-threatening, delayed-onset drug reaction that is typically characterized by skin eruption and fever. DRESS can include eosinophilia, atypical lymphocytes, lymphadenopathy, and internal organ involvement.1-3 The clinical presentation is variable; patients exhibit a wide array of signs and symptoms that do not always present concurrently. This heterogeneity can result in missing or delaying the diagnosis, with harmful consequences for the patient.
Method. The Division of Pharmacovigilance at the US Food and Drug Administration (FDA) recently reviewed postmarketing cases of DRESS reported in association with the use of ziprasidone in the FDA Adverse Event Reporting System (FAERS). FAERS is a database that contains spontaneous adverse event reports submitted to FDA. FAERS supports FDA postmarketing safety surveillance for drug and therapeutic biologic products. It is a passive surveillance system and is therefore subject to substantial underreporting.
On the basis of the Phenotype Standardization Project Drug-Induced Skin Injury criteria,4 we defined a case of DRESS as one that reported an onset of DRESS within 3 months of starting therapy, had evidence of involvement of the skin and/or internal organ system, and included at least 2 of the following: fever, eosinophilia and/or atypical lymphocytes, or lymphadenopathy.
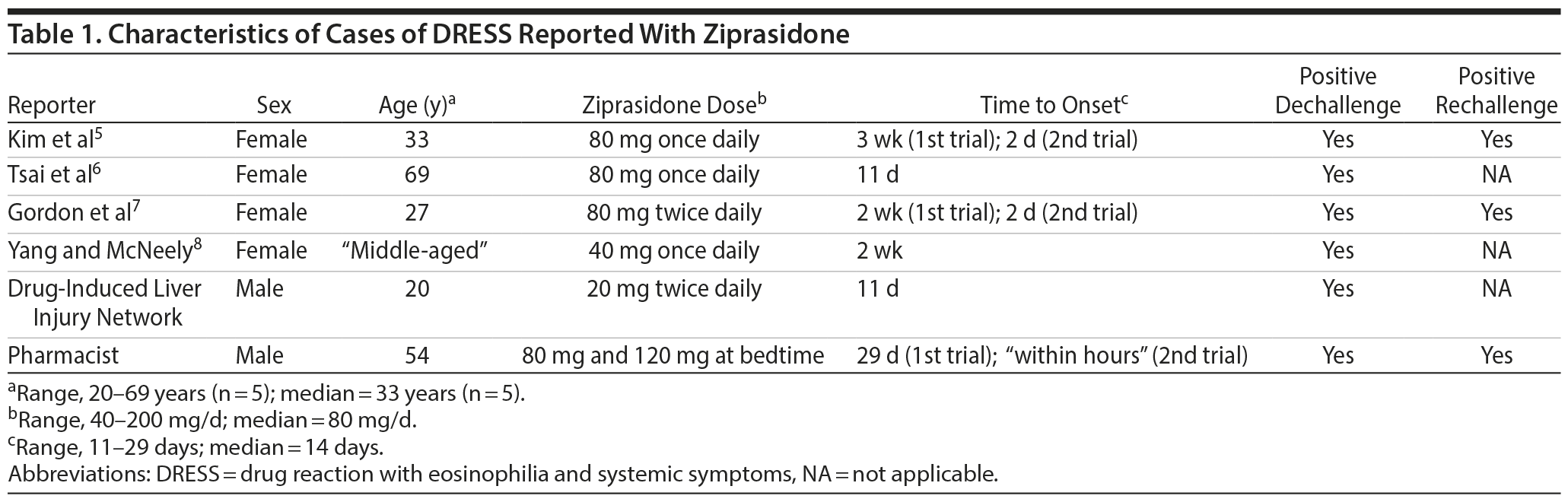
Results. We identified 6 cases in FAERS, 4 of which were already published in the medical literature.5-8 The remaining 2 were reported by health care professionals. Three cases met our case definition for DRESS, and the other 3 provided sufficient clinical information to suspect DRESS. For all cases, the time to onset of DRESS signs and symptoms after the initiation of ziprasidone ranged from 11 days to 1 month, with a median of 14 days. Furthermore, in 3 cases, another episode of DRESS upon reexposure to ziprasidone (positive rechallenge) was reported, with a faster time to onset following rechallenge than with the initial administration of ziprasidone. These features are consistent with the time to onset of DRESS. Table 1 shows more characteristics of the cases.
The incidence of DRESS in the general population is unknown, but estimates range from 1:1,000 to 1:10,000.1,9 Although there were no fatalities in our case series, DRESS has a mortality rate of up to 10%.1,9 The exact pathogenesis of DRESS is unknown; however, it is thought to be the result of a combination of genetic and immunologic factors. The medical literature provides hypotheses, such as detoxification defects in the drug metabolism pathway, resulting in toxic metabolite formation and an immune response. Reactivation of herpes virus (HHV-6, HHV-7) or Epstein-Barr virus infections may also play a role by inducing or amplifying the immune reaction.1,3,10-12 Although symptoms of DRESS may persist weeks to months after discontinuing the drug, the key to management is early recognition and withdrawal of the offending agent to improve outcomes and prevent fatalities. Management also includes supportive care and systemic steroids in more severe cases.13
Given its clinical severity and the need for prompt discontinuation of the drug, clinicians should be aware of the potential causal relationship between ziprasidone and DRESS. The Warnings and Precautions section of the prescribing information for all ziprasidone products14 has been updated as follows:
Drug reaction with eosinophilia and systemic symptoms (DRESS) has been reported with ziprasidone exposure. DRESS consists of a combination of 3 or more of the following: cutaneous reaction (such as rash or exfoliative dermatitis), eosinophilia, fever, lymphadenopathy and one or more systemic complications such as hepatitis, nephritis, pneumonitis, myocarditis, and pericarditis. DRESS is sometimes fatal. Discontinue ziprasidone if DRESS is suspected.
The FDA-Approved Patient Labeling section has also been updated with lay terms for signs and symptoms of DRESS. Additionally, a Drug Safety Communication was published on December 11, 2014, to inform health care professionals and consumers of the potential risk.15
References
1. Cacoub P, Musette P, Descamps V, et al. The DRESS syndrome: a literature review. Am J Med. 2011;124(7):588-597. PubMed doi:10.1016/j.amjmed.2011.01.017
2. Tas S, Simonart T. Management of drug rash with eosinophilia and systemic symptoms (DRESS syndrome): an update. Dermatology. 2003;206(4):353-356. PubMed doi:10.1159/000069956
3. Bocquet H, Bagot M, Roujeau JC. Drug-induced pseudolymphoma and drug hypersensitivity syndrome (drug rash with eosinophilia and systemic symptoms: DRESS). Semin Cutan Med Surg. 1996;15(4):250-257. PubMed doi:10.1016/S1085-5629(96)80038-1
4. Pirmohamed M, Friedmann PS, Molokhia M, et al. Phenotype standardization for immune-mediated drug-induced skin injury. Clin Pharmacol Ther. 2011;89(6):896-901. PubMed doi:10.1038/clpt.2011.79
5. Kim MS, Kim SW, Han TY, et al. Ziprasidone-induced hypersensitivity syndrome confirmed by reintroduction. Int J Dermatol. 2014;53(4):e267-e268. PubMed doi:10.1111/ijd.12246
6. Tsai CF, Tsai SJ, Hwang JP. Ziprasidone-induced hypersensitivity syndrome in an aged schizophrenia patient. Int J Geriatr Psychiatry. 2005;20(8):797-799. PubMed doi:10.1002/gps.1346
7. Gordon JS, Neyman KM, Wells RD, et al. Drug rash with eosinophilia and systemic symptoms (DRESS syndrome). Cutis. 2012;89(4):180-182. PubMed
8. Yang SH, McNeely MJ. Rhabdomyolysis, pancreatitis, and hyperglycemia with ziprasidone. Am J Psychiatry. 2002;159(8):1435. PubMed doi:10.1176/appi.ajp.159.8.1435
9. RegiSCAR website. http://www.regiscar.org. Accessed April 1, 2015.
10. Walsh SA, Creamer D. Drug reaction with eosinophilia and systemic symptoms (DRESS): a clinical update and review of current thinking. Clin Exp Dermatol. 2011;36(1):6-11. PubMed doi:10.1111/j.1365-2230.2010.03967.x
11. Sullivan JR, Shear NH. The drug hypersensitivity syndrome: what is the pathogenesis? Arch Dermatol. 2001;137(3):357-364. PubMed
12. Shiohara T, Inaoka M, Kano Y. Drug-induced hypersensitivity syndrome (DIHS): a reaction induced by a complex interplay among herpesviruses and antiviral and antidrug immune responses. Allergol Int. 2006;55(1):1-8. PubMed doi:10.2332/allergolint.55.1
13. Husain Z, Reddy BY, Schwartz RA. DRESS syndrome, part 2: management and therapeutics. J Am Acad Dermatol. 2013;68(5):709.e1-709.e9, quiz 718-720. PubMed doi:10.1016/j.jaad.2013.01.032
14. Geodon [package insert]. New York, NY: Roerig; 2014. http://www.accessdata.fda.gov/dr ugsatfda_docs/label/2014/020825s053,020919s040,s021483s013lbl.pdf. Updated December 2014. Accessed December 10, 2014.
15. FDA Drug Safety Communication. FDA reporting mental health drug ziprasidone (Geodon) associated with rare but potentially fatal skin reactions. December 11, 2014. http://www.fda.gov/Drugs/DrugSafety/ucm426391.htm. Accessed December 11, 2014.
Author affiliations: Division of Pharmacovigilance, Center for Drug Evaluation and Research, US Food and Drug Administration, Silver Spring, Maryland.
Potential conflicts of interest: None reported.
Funding/support: None reported.
Disclaimer: The views expressed in this paper are those of the authors and do not necessarily represent those of the US Food and Drug Administration.
J Clin Psychiatry 2015;76(9):e1138-e1139
dx.doi.org/10.4088/JCP.15l09921
© Copyright 2015 Physicians Postgraduate Press, Inc.
This PDF is free for all visitors!