Tardive dyskinesia (TD), a potentially irreversible condition that causes involuntary movements associated with dopamine receptor blocking agents, can substantially impair patients’ functioning and diminish their quality of life. While TD was expected to vanish due to more widespread use of second-generation antipsychotics than use of first-generation antipsychotics, in reality, more patients than ever are at risk for developing this condition. Early detection and accurate diagnosis of TD is critical to increasing chances that TD movements will be transient and reversible. Clinicians must be proactive in regularly screening patients for TD, educating the patient and family about risk factors, addressing psychosocial concerns related to the condition, and selecting one of the novel, FDA-approved medications—valbenazine or deutetrabenazine—to treat TD symptoms. Providing a clinical TD diagnosis as early as possible is crucial to implementing treatment strategies that may successfully reduce patients’ TD symptoms.
This CME activity is expired. For more CME activities, visit CMEInstitute.com.
Find more articles on this and other psychiatry and CNS topics:
The Journal of Clinical Psychiatry
The Primary Care Companion for CNS Disorders

CME Background
Articles are selected for credit designation based on an assessment of the educational needs of CME participants, with the purpose of providing readers with a curriculum of CME articles on a variety of topics throughout each volume. Activities are planned using a process that links identified needs with desired results.
To obtain credit, read the article, correctly answer the questions in the Posttest, and complete the Evaluation.
This Academic Highlights section of The Journal of Clinical Psychiatry presents the highlights of the teleconference series “Early Recognition and Treatment of Tardive Dyskinesia in Patients With Mood Disorders and Schizophrenia,” which was held in April, May, and June 2019. This report was prepared and independently developed by the CME Institute of Physicians Postgraduate Press, Inc., and was supported by an educational grant from Neurocrine Biosciences, Inc.
The teleconference was chaired by Joseph P. McEvoy, MD, from Department of Psychiatry and Health Behavior, Medical College of Georgia, Augusta University. The faculty was Daniel E. Kremens, MD, JD, from Department of Neurology, Sidney Kimmel Medical College, Thomas Jefferson University, Philadelphia, Pennsylvania.
CME Objective
After studying this article, you should be able to:
- Recognize early signs of tardive dyskinesia (TD) through regular screening and patient/family education about symptoms
- Address psychosocial concerns related to TD in patients with mood disorders and schizophrenia
- Select FDA-approved medication to treat TD symptoms, considering research on longer-term efficacy and safety
Accreditation Statement
The CME Institute of Physicians Postgraduate Press, Inc., is accredited by the Accreditation Council for Continuing Medical Education to provide continuing medical education for physicians.
Release, Expiration, and Review Dates
This educational activity was published in January 2020 and is eligible for AMA PRA Category 1 Creditâ„¢ through February 28, 2022. The latest review of this material was December 2019.
Financial Disclosure
All individuals in a position to influence the content of this activity were asked to complete a statement regarding all relevant personal financial relationships between themselves or their spouse/partner and any commercial interest. The CME Institute has resolved any conflicts of interest that were identified. In the past year, Marlene P. Freeman, MD, Editor in Chief, has received research funding from JayMac and Sage; has been a member of the advisory boards for Otsuka, Alkermes, and Sunovion; has been a member of the Independent Data Safety and Monitoring Committee for Janssen; has been a member of the Steering Committee for Educational Activities for Medscape; and, as a Massachusetts General Hospital (MGH) employee, works with the MGH National Pregnancy Registry, which is sponsored by Teva, Alkermes, Otsuka, Actavis, and Sunovion, and works with the MGH Clinical Trials Network and Institute, which receives research funding from multiple pharmaceutical companies and the National Institute of Mental Health. No member of the CME Institute staff reported any relevant personal financial relationships. Faculty financial disclosure appears at the end of this activity.
J Clin Psychiatry 2020;81(1):NU18041AH5C
To cite: McEvoy JP, Kremens DE. Early recognition and treatment of tardive dyskinesia in patients with mood disorders and schizophrenia. J Clin Psychiatry. 2020;81(1):NU18041AH5C
To share: https://doi.org/10.4088/JCP.NU18041AH5C
© Copyright 2020 Physicians Postgraduate Press, Inc.
Tardive dyskinesia (TD), a condition of potentially irreversible abnormal involuntary movements that is associated with dopamine receptor blocking agents (DRBAs) such as antipsychotics, can produce substantial impairment of functioning and diminished quality of life for patients.1 Contrary to expectations, TD has not vanished as the use of second-generation antipsychotics (SGAs) has become more widespread than use of first-generation antipsychotics (FGAs). In fact, expanded drug indications and increased off-label prescription of SGAs have placed more patients than ever at risk for TD.
In this Academic Highlights, Drs McEvoy and Kremens discuss best practices for recognizing early signs of TD through regular screening, educating the patient and family about risk factors, addressing psychosocial concerns related to TD, and selecting new FDA-approved medication—valbenazine and deutetrabenazine—to treat TD.
An individual living with TD described the burden the condition places on his life:
Patient Perspectives
“I hate the thought of being like this forever. . . . Most people are understanding, but it’s the odd moments when I’ m in public or a quiet place and the lip smacking becomes noticeable, not to mention the odd sensations in my tongue from constantly rubbing against my bottom teeth.”2
The Importance of Early Recognition and Diagnosis of TD
Accurate diagnosis of TD is crucial for potential reversal of symptoms; however, Dr Kremens noted it can present a clinical challenge due to the insidious onset and fluctuating nature of symptoms. Clinicians may underestimate the risk of TD associated with SGA treatment and should review patients’ risk factors and try to prevent TD.2,3 Dr Kremens emphasized that clinicians should discuss risk factors with patients and caregivers (Table 1).4 Regular screening and patient education are important. If patients develop signs of TD, diagnostic tools and criteria should be used.
Monitoring for TD
Because TD may become persistent and irreversible, Dr Kremens said that prevention (if possible) by the conservative use of antipsychotics is critical.3 If TD does develop, early detection may increase the chances that TD movements will be transient and reversible.
According to the American Psychiatric Association (APA),5 all patients should be examined for signs of TD before initiating DRBA therapy, at least twice a year in patients taking DRBAs, and upon changes in DRBA dose or agent or observation of previously undetected movements. (For more information on APA guidelines and related topics, see the other activities in this series online.)
Screening tools. Monitoring for TD should involve the use of an appropriate tool, such as the Abnormal Involuntary Movement Scale (AIMS).6 A 14-item clinician-administered rating scale, the AIMS has been widely accepted as an objective measure for assessing the severity and extent of TD.7,8 Dr Kremens mentioned that using the full AIMS may be too time consuming for clinicians in a busy office practice, and suggestions have been made to develop a shorter, simpler AIMS or other instrument.7
Diagnostic criteria. While an important tool, the AIMS cannot be used by itself to diagnose TD. The Schooler-Kane criteria9,10 for TD require that a patient have ≥ 3 months of cumulative exposure to neuroleptics, the absence of other conditions that might cause involuntary movements, and at least moderate dyskinetic movements in 1 body area (≥ 3 rated by the AIMS) or mild dyskinetic movements in 2 body areas (≥ 2 rated by the AIMS).
Per the Diagnostic and Statistical Manual of Mental Disorders, Fifth Edition (DSM-5),11 to confirm a diagnosis of TD, symptoms must persist for 1 month after the medication is discontinued. The involuntary movements should be athetoid or choreiform and typically of the tongue, jaw, and extremities.12
According to Dr Kremens, other conditions associated with abnormal movement that may resemble TD must be ruled out, such as Huntington disease, drug-induced dyskinesias, edentulous dyskinesia, Wilson disease and other metabolic disorders, Tourette syndrome, and immune-mediated choreas.12,13
Case Practice Question
Discussion of the best response can be found at the end of the activity.
Case 1. Tom is a 26-year-old white man. He is HIV-positive and acquired HIV through unprotected sex. He has no history of drug or alcohol abuse. He was diagnosed with schizophrenia when he was 21 years old and has been taking an SGA. He responded well and has tolerated his medication without any evidence of extrapyramidal movements at his prior visits. At his visit with you today, you perform an AIMS and notice that he has developed shifting of his jaw, excessive blinking, and movements in his fingers and toes. Which of the following characteristics increases Tom’s risk of developing TD?
a.Younger age
b.HIV positivity
c.Treatment with an SGA
d.Male sex
Psychosocial Implications of TD
Many patients with schizophrenia and some with severe bipolar disorder demonstrate multiple fixed deficits, which can include negative psychopathology, neurologic soft signs, and a lack of insight into their illness, in addition to psychosis and agitation.14-17 Tardive dyskinesia is more common and severe in patients with fixed deficits, and these patients tend to be unaware that they have abnormal involuntary movements.18
An individual living with TD described her lack of awareness of her abnormal movements:
Patient Perspectives
“With the lip movement, I am completely unaware that I am doing it. . . . I only found out when a coworker asked me about it. . . . I had no idea what she was talking about. I asked some other people and they said: ‘ Oh, that thing you do with your lips. Sure, I’ ve seen that.’ “19
Dr McEvoy noted that, in patients with lack of insight into the presence of TD, motivation to treat it is determined primarily by the AIMS results.20 If the movements are disfiguring or interfere with the patient’s basic functioning, clinicians should aggressively treat patients even if they are unaware of the movements or express little distress about them.
Patients with bipolar disorder, especially the milder variants, and patients with recurrent major depression are more likely to achieve sustained remission of their target psychopathology than are patients with schizophrenia.21 These patients have fewer and less severe deficits and are more likely to be aware of and distressed by abnormal movements.22,23
Dr McEvoy shared that even mild movements should be treated if patients are distressed by them, as they can substantially impact psychosocial functioning. In an interview with the Depression and Bipolar Support Alliance (oral communication, March 2019), a patient described not realizing how noticeable her movements were until she saw herself in a video:
Patient Perspectives
I went to a Christmas party for church, and the church was going to make a video of all of us there, singing a song so that they could use that as the invitation for another Christmas party. . . . And so I was singing the song “Joy to the World” and then they sent it out by e-mail to everybody in the church. And I opened it with my husband and I was mortified. I was the only one having movements during the song. My hands were flapping up and down with every single word. My husband said I looked like a chicken that was trying to take flight. . . . You know, he helped me find the funny side of it, but . . . I was very embarrassed as well because I knew every member in my church was going to see this.”
FDA-Approved Medications to Treat TD
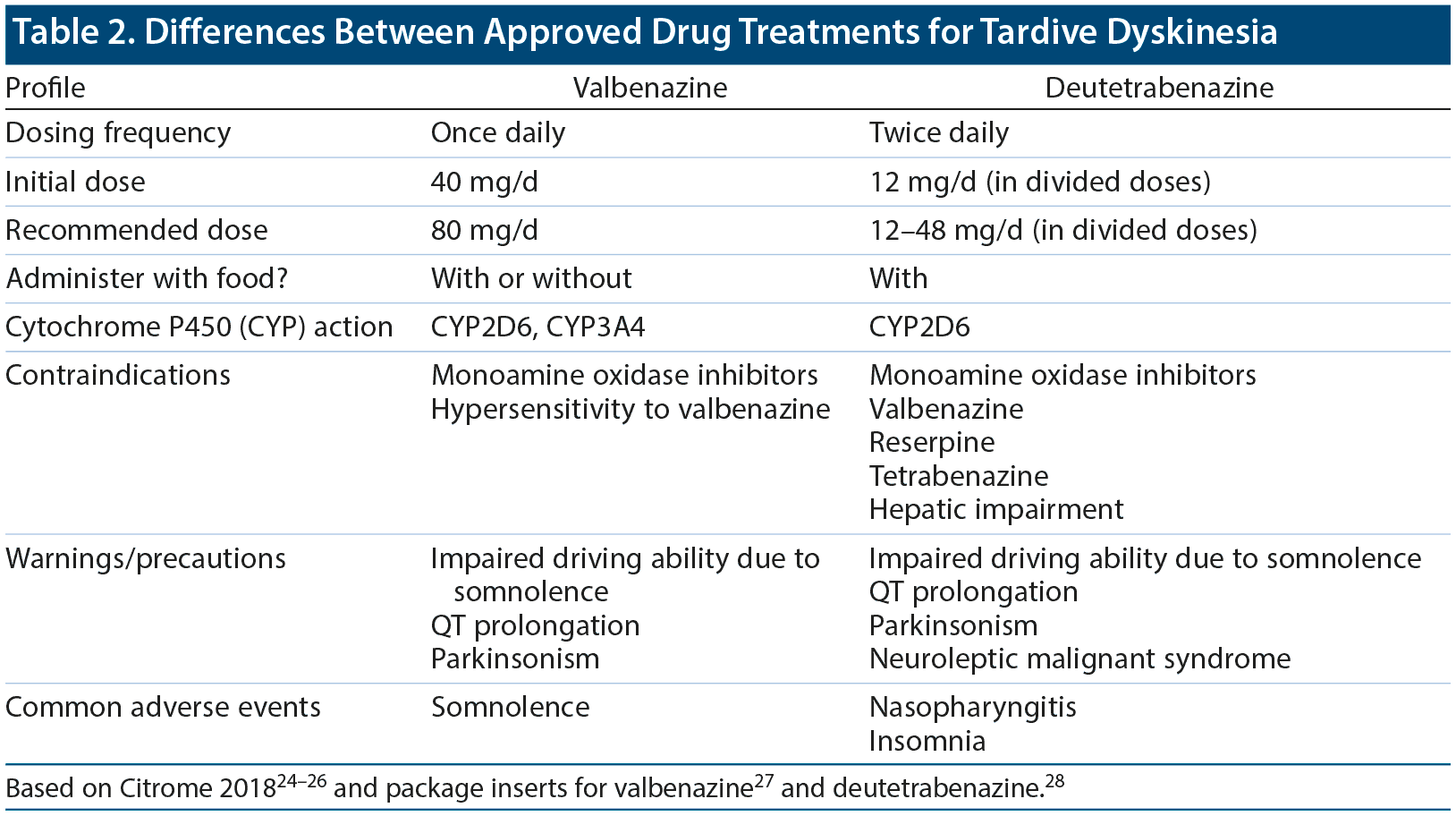
Two treatments for TD, which are both novel vesicular monoamine transporter type 2 (VMAT2) inhibitors, have been approved by the FDA: valbenazine and deutetrabenazine (Table 2).24-28According to Dr McEvoy, these new medications can be life changing for individuals with TD who continue to need antipsychotic treatment despite the side effects.8
Individuals with TD described the difference that treatment made to them:
Patient Perspectives
“[My doctor] started me on some new medications and experimented with decreasing a few of the medications I was already taking to get the right combination to treat my mental disorder and also help my TD symptoms. As a result, my level of distress has decreased tremendously. I am braver now socially.”29
“This new treatment has changed my life in ways I never thought it could. I can go in public without fear of being stared at, I can breathe normally, I feel human again. Antipsychotics changed my life, and I can’ t imagine my life without them, and now that I have the additional medication, I can’ t imagine my life without that either.”30
Valbenazine
Valbenazine received FDA approval for the treatment of TD in 2017 based largely on the positive results of KINECT 3, a phase 3 double-blind randomized controlled trial. In this study,31 participants (N = 225) with schizophrenia, schizoaffective disorder, or a mood disorder who had moderate or severe TD were randomly assigned in a 1:1:1 ratio to once-daily placebo, valbenazine 40 mg/d, or valbenazine 80 mg/d. About 86% of participants were taking antipsychotics. Least-squares mean change in AIMS dyskinesia scores was -3.2 for the 80-mg/d group, -1.9 for the 40-mg/d group, and -0.1 for the placebo group (P < .001 for 80 mg/d vs placebo). The 1-year KINECT 3 extension study32 demonstrated long-term efficacy, safety, and tolerability of valbenazine for the treatment of TD.
Dr Kremens noted that the only adverse effect with ≥ 5% incidence for valbenazine and occurring ≥ 2 times than with placebo was somnolence/fatigue/sedation, with rates of 10.9% for valbenazine (both doses) and 4.2% for placebo, resulting in a number needed to harm of 15 (95% CI, 9-52).25 The product label has a precaution against driving until the drug’s sleep effects on the patient are known.27 Besides somnolence, Dr Kremens identified QT prolongation as the other labeled precaution. Other adverse effects include anticholinergic effects, balance problems, headache, gastrointestinal issues, and arthralgia.
Valbenazine is slowly metabolized, allowing for once-daily dosing, with or without food, starting at 40 mg and increasing to 80 mg after 1 week.27
Deutetrabenazine
Deutetrabenazine received FDA approval for the treatment of TD in 2017 on the basis of results from 2 double-blind randomized controlled trials: the phase 2/3 trial ARM-TD and the phase 3 trial AIM-TD.26 In both studies, Dr Kremens noted that patients could continue the use of DRBAs or antidepressants as long as there had been no recent change in these medications.
The ARM-TD study33 examined a flexible dose of deutetrabenazine starting at 12 mg/d (6 mg twice daily) and titrated weekly by 6 mg/d, if required, versus placebo in 117 patients with moderate to severe TD. The mean total daily dose was 38.8 mg/d at the end of the 12-week study period. AIMS scores decreased significantly in the deutetrabenazine group versus the placebo group (-3.0 vs −1.6; P = .019), and the drug was well tolerated.
The AIM-TD fixed-dose study34 randomized 298 patients 1:1:1:1 to receive placebo or deutetrabenazine 12, 24, or 36 mg/d (divided in 2 doses) for 8 weeks after a 4-week titration period. Least-squares mean AIMS scores improved by -3.2 (P = .003) and -3.3 (P = .001) in the groups receiving deutetrabenazine 24 and 36 mg/d, respectively, compared with -1.4 for placebo.
Dr Kremens shared that deutetrabenazine was well tolerated, with low rates of side effects in both ARM-TD and AIM-TD.33,34 The adverse effects that occurred in ≥ 4% of participants taking deutetrabenazine and at a greater rate than with placebo were nasopharyngitis and insomnia,28 with number needed to harm values of 50 (not significant) and 34 (95% CI, 18-725), respectively.26 Depression/dysthymia and akathisia/restlessness also occurred more often than with placebo.28 Prescribing information28 states that the use of deutetrabenazine in combination with other drugs known to prolong QTc may result in clinically significant QT prolongations. For patients requiring deutetrabenazine doses greater than 24 mg/d and who are taking other drugs known to prolong QTc, assess the QTc interval before and after increasing the dose of deutetrabenazine or the other drugs.
Deutetrabenazine is dosed twice daily, is titrated typically over several weeks, and should be taken with food, explained Dr Kremens.28
Case Practice Question
Discussion of the best response can be found at the end of the activity.
Case 2. James is a 27-year-old man who was diagnosed with schizophrenia at age 18 years. He has been treated with 5 mg at bedtime of haloperidol for the past 5 years with no relapses and no distressing or intrusive psychotic symptoms. He lives independently with a roommate and has a part-time job stacking shelves. He has gradually developed increasingly apparent spontaneous movements in his face and hands over the past 6 months; you diagnose these as tardive dyskinesia. His roommate and his employer have asked about the movements, and James is concerned that he may lose his job. A trial of pyridoxine 50 mg twice a day has not decreased the movements. The intervention with the greatest likelihood to suppress the movements with the least side effect burden is
a.Increase the haloperidol to 10 mg at bedtime.
b.Add benztropine 2 mg daily.
c.Increase the pyridoxine dose to 200 mg twice a day.
d.Begin treatment with a VMAT2 inhibitor.
Discussion of Case Practice Questions
Case 1: Preferred response is b.
HIV positivity is a risk factor for developing TD. Other risk factors include older age, female sex, longer duration and higher doses of DRBAs, treatment with FGAs, preexisting mood disorder, cognitive disturbance, alcohol or substance abuse, diabetes, early occurrence of extrapyramidal symptoms, and African American ethnicity—none of which apply to Tom.
Case 2: Preferred response is d.
Valbenazine and deutetrabenazine are both novel VMAT2 inhibitors approved by the FDA to treat TD. James continues to need antipsychotic treatment, which has been effective in treating his schizophrenia; therefore, he is an optimal candidate for the approved VMAT2 inhibitors.
Clinical Points
- Discuss risk factors and early signs of TD with patients and caregivers.
- Screen patients for signs of TD during routine appointments.
- Avoid prescribing first-generation antipsychotics.
- Monitor patients taking second-generation antipsychotics for early TD signs.
- Recognize the social and occupational impact of TD symptoms in patients who are aware of and distressed by them.
- Treat patients who have TD with evidence-based agents.
- Differentiate between the 2 FDA-approved agents for TD.
- Follow recommended administration, titration, and monitoring of medications for TD.
Published online: January 28, 2020.
Disclosure of off-label usage: The chair has determined that, to the best of his knowledge, benztropine is not approved by the US Food and Drug Administration for the treatment of tardive dyskinesia.
Credit Designation
The CME Institute of Physicians Postgraduate Press, Inc., designates this journal-based CME activity for a maximum of 1 AMA PRA Category 1 Creditâ„¢. Physicians should claim only the credit commensurate with the extent of their participation in the activity.
Note: The American Academy of Physician Assistants (AAPA) accepts certificates of participation for educational activities certified for AMA PRA Category 1 Creditâ„¢ from organizations accredited by ACCME or a recognized state medical society. Physician assistants may receive a maximum of 1 hour of Category I credit for completing this program.
Financial Disclosure
Dr McEvoy has received grant/research support from Takeda, Alkermes, Boehringer Ingelheim, Teva, Neurocrine, and Otsuka; has received honoraria from Neurocrine; and is a member of the speakers/advisory boards for Merck, Neurocrine, and Alkermes. Dr Kremens is a consultant for Teva, UCB, Sunovion, Impax, Lundbeck, Acadia, USWorldMeds, Adamas, AbbVie, Merz, Allergan, Acorda, Kyowa, Neurocrine, GE Healthcare, and St Jude Medical; is a member of the speakers/advisory boards for Teva, UCB, Impax, Lundbeck, Acadia, USWorldMeds, and Adamas; and has received grant/research support from Acorda and Enterin.
Review Process
The faculty members agreed to provide a balanced and evidence-based presentation and discussed the topics and CME objectives during the planning sessions. The faculty’s submitted content was validated by CME Institute staff, and the activity was evaluated for accuracy, use of evidence, and fair balance by the Chair and a peer reviewer who is without conflict of interest.
The opinions expressed herein are those of the faculty and do not necessarily reflect the opinions of the CME provider and publisher or Neurocrine Biosciences, Inc.
REFERENCES
1. Carbon M, Kane JM, Leucht S, et al. Tardive dyskinesia risk with first- and second-generation antipsychotics in comparative randomized controlled trials: a meta-analysis. World Psychiatry. 2018;17(3):330-340. PubMed CrossRef
2. Solmi M, Pigato G, Kane JM, et al. Clinical risk factors for the development of tardive dyskinesia. J Neurol Sci. 2018;389:21-27. PubMed CrossRef
3. Ricciardi L, Pringsheim T, Barnes TRE, et al. Treatment recommendations for tardive dyskinesia. Can J Psychiatry. 2019;64(6):388-399. PubMed CrossRef
4. Jankelowitz SK. Treatment of neurolept-induced tardive dyskinesia. Neuropsychiatr Dis Treat. 2013;9:1371-1380. PubMed CrossRef
5. Lehman AF, Lieberman JA, Dixon LB, et al; American Psychiatric Association; Steering Committee on Practice Guidelines. Practice guideline for the treatment of patients with schizophrenia, second edition. Am J Psychiatry. 2004;161(suppl):1-56. PubMed
6. Guy W. ECDEU Assessment Manual for Psychopharmacology. Revised Edition. Washington, DC: US Department of Health, Education, and Welfare; 1976.
7. Caroff SN. Overcoming barriers to effective management of tardive dyskinesia. Neuropsychiatr Dis Treat. 2019;15:785-794. PubMed CrossRef
8. Niemann N, Jankovic J. Treatment of tardive dyskinesia: a general overview with focus on the vesicular monoamine transporter 2 inhibitors. Drugs. 2018;78(5):525-541. PubMed CrossRef
9. Schooler NR, Kane JM. Research diagnoses for tardive dyskinesia. Arch Gen Psychiatry. 1982;39(4):486-487. PubMed CrossRef
10.Kane JM. Assessing patients for tardive dyskinesia. J Clin Psychiatry. 2017;78(9):e1428. PubMed CrossRef
11.American Psychiatric Association. Diagnostic and Statistical Manual for Mental Disorders. Fifth Edition. Washington, DC: American Psychiatric Association; 2013.
12.Jain R, Correll CU. Tardive dyskinesia: recognition, patient assessment, and differential diagnosis. J Clin Psychiatry. 2018;79(2):NU17034AH1C. PubMed CrossRef
13.Citrome L, Dufresne R, Dyrud JM. Tardive dyskinesia: minimizing risk and improving outcomes in schizophrenia and other disorders. Am J Manag Care. 2007;12(suppl).
14.Feng Y, Wang Z, Lin G, et al. Neurological soft signs and neurocognitive deficits in remitted patients with schizophrenia, their first-degree unaffected relatives, and healthy controls [published online ahead of print May 23, 2019]. Eur Arch Psychiatry Clin Neurosci. PubMed CrossRef
15.Bora E, Binnur Akdede B, Alptekin K. Neurocognitive impairment in deficit and non-deficit schizophrenia: a meta-analysis. Psychol Med. 2017;47(14):2401-2413. PubMed CrossRef
16.Chan RCK, Geng F-L, Lui SSY, et al. Course of neurological soft signs in first-episode schizophrenia: relationship with negative symptoms and cognitive performances. Sci Rep. 2015;5(1):11053. PubMed CrossRef
17.Chrobak AA, Siwek GP, Siuda-Krzywicka K, et al. Neurological and cerebellar soft signs do not discriminate schizophrenia from bipolar disorder patients. Prog Neuropsychopharmacol Biol Psychiatry. 2016;64:96-101. PubMed CrossRef
18.Arango C, Adami H, Sherr JD, et al. Relationship of awareness of dyskinesia in schizophrenia to insight into mental illness. Am J Psychiatry. 1999;156(7):1097-1099. PubMed CrossRef
19.Elib1971. Tardive Dyskinesia: I was diagnosed with TD about a year ago. Drugs.com website. https://www.drugs.com/answers/tardive-dyskinesia-diagnosed-td-year-ago-3123904.html. Published September 11, 2016. Accessed November 8, 2017.
20.Kane JM, Correll CU, Nierenberg AA, et al; Tardive Dyskinesia Assessment Working Group. Revisiting the Abnormal Involuntary Movement Scale: Proceedings from the Tardive Dyskinesia Assessment Workshop. J Clin Psychiatry. 2018;79(3):17cs11959. PubMed CrossRef
21.Spellmann I, Schennach R, Seemüller F, et al. Validity of remission and recovery criteria for schizophrenia and major depression: comparison of the results of two one-year follow-up naturalistic studies. Eur Arch Psychiatry Clin Neurosci. 2017;267(4):303-313. PubMed CrossRef
22.Braw Y, Sitman R, Sela T, et al. Comparison of insight among schizophrenia and bipolar disorder patients in remission of affective and positive symptoms: analysis and critique. Eur Psychiatry. 2012;27(8):612-618. PubMed CrossRef
23.Mishra DK, Alreja S, Sengar KS, et al. Insight and its relationship with stigma in psychiatric patients. Ind Psychiatry J. 2009;18(1):39-42. PubMed CrossRef
24.Citrome L. Tardive dyskinesia: placing vesicular monoamine transporter type 2 (VMAT2) inhibitors into clinical perspective. Expert Rev Neurother. 2018;18(4):323-332. PubMed CrossRef
25.Citrome L. Valbenazine for tardive dyskinesia: a systematic review of the efficacy and safety profile for this newly approved novel medication—what is the number needed to treat, number needed to harm and likelihood to be helped or harmed? Int J Clin Pract. 2017;71(7):ijcp.12964. PubMed CrossRef
26.Citrome L. Deutetrabenazine for tardive dyskinesia: a systematic review of the efficacy and safety profile for this newly approved novel medication—what is the number needed to treat, number needed to harm and likelihood to be helped or harmed? Int J Clin Pract. 2017;71(11):ijcp.13030. PubMed CrossRef
27.Ingrezza (valbenazine): highlights of prescribing information. December 2018. NIH website. https://dailymed.nlm.nih.gov/dailymed/drugInfo.cfm?setid=4c970164-cafb-421f-9eb5-c226ef0a3417. Accessed October 18, 2019.
28.Austedo (deutetrabenazine): highlights of prescribing information. July 2019. NIH website. https://dailymed.nlm.nih.gov/dailymed/drugInfo.cfm?setid=7ea3c60a-45c7-44cc-afc2-d87fa53993c0. Accessed October 18, 2019.
29.Don’ t Let TD Overwhelm You. CME Institute website. https://www.cmeinstitute.com/patients/pages/post5.aspx. Published May 3, 2019. Accessed January 2, 2020.
30.Krueger B. Facing tardive dyskinesia. NAMI: National Alliance on Mental Illness. https://www.nami.org/Personal-Stories/Facing-Tardive-Dyskinesia#. Published 2018. Accessed January 2, 2020.
31.Hauser RA, Factor SA, Marder SR, et al. KINECT 3: a phase 3 randomized, double-blind, placebo-controlled trial of valbenazine for tardive dyskinesia. Am J Psychiatry. 2017;174(5):476-484. PubMed CrossRef
32.Factor SA, Remington G, Comella CL, et al. The effects of valbenazine in participants with tardive dyskinesia: results of the 1-year KINECT 3 extension study. J Clin Psychiatry. 2017;78(9):1344-1350. PubMed CrossRef
33.Fernandez HH, Factor SA, Hauser RA, et al. Randomized controlled trial of deutetrabenazine for tardive dyskinesia: the ARM-TD study. Neurology. 2017;88(21):2003-2010. PubMed CrossRef
34.Anderson KE, Stamler D, Davis MD, et al. Deutetrabenazine for treatment of involuntary movements in patients with tardive dyskinesia (AIM-TD): a double-blind, randomised, placebo-controlled, phase 3 trial. Lancet Psychiatry. 2017;4(8):595-604. PubMed CrossRef
This PDF is free for all visitors!