Because this piece does not have an abstract, we have provided for your benefit the first 3 sentences of the full text.
To the Editor: Heritability in liability to schizophrenia has been estimated at 81%. Therefore, genetic risk factors play a key role in the complex etiology of schizophrenia, and they are also thought to affect the presentation of schizophrenia symptoms. Consequently, the severity of symptoms should be greater among schizophrenia patients with familial antecedents of psychoses than for nonfamilial or sporadic cases.
This work may not be copied, distributed, displayed, published, reproduced, transmitted, modified, posted, sold, licensed, or used for commercial purposes. By downloading this file, you are agreeing to the publisher’s Terms & Conditions.
Parental Antecedents of Psychosis Are Associated With Severity of Positive and Negative Symptoms in Schizophrenia Patients
To the Editor: Heritability in liability to schizophrenia has been estimated at 81%.1 Therefore, genetic risk factors play a key role in the complex etiology of schizophrenia, and they are also thought to affect the presentation of schizophrenia symptoms. Consequently, the severity of symptoms should be greater among schizophrenia patients with familial antecedents of psychoses than for nonfamilial or sporadic cases. However, few studies have compared the symptoms of familial and nonfamilial schizophrenia, and those that have investigated only small samples.2-4 We compared the symptom severity of patients who had a parent with a diagnosis of schizophrenia to that of patients with no antecedent of either psychotic or affective disorder among their parents or grandparents.
Method. The participants were 211 patients with a diagnosis of schizophrenia according to DSM-IV criteria who had 1 first-degree relative willing to cooperate in the collection of the patient’s familial psychiatric antecedents. Antecedents were assessed using the Family History Research Diagnostic Criteria (FH-RDC),5 as previously described,6 and symptom severity was assessed using the Spanish adaptation of the Positive and Negative Syndrome Scale (PANSS).7,8 We used the classical PANSS subscales described by Kay et al,7 and we also grouped symptoms using the 5-factor model suggested by Wallwork et al.9 We identified 39 (18.5%) familial patients, defined by the presence of 1 parent with schizophrenia (10 fathers and 29 mothers), and 172 (81.5%) sporadic patients, who had no psychotic antecedent among their parents or grandparents. All participants were clinically stable white outpatients, without prominent psychotic symptoms (mean ± SD positive and negative PANSS scores of 12.9 ± 6.2 and 17.7 ± 7.7, respectively), and they were able to understand the purpose of the study. Informed consent was obtained from both the patients and their relatives, and the investigation was approved by the Ethics Committee of the Hospital Sant Joan de Reus. The general linear model was used to compare the PANSS scores of patients with and without parental antecedents of schizophrenia, with current age as a covariate. Estimated marginal means were calculated instead of average means to adjust the PANSS scores to the current age. The statistical analyses were performed using IBM SPSS Statistics for Windows, Version 19.0 (IBM Corp, Armonk, NY).
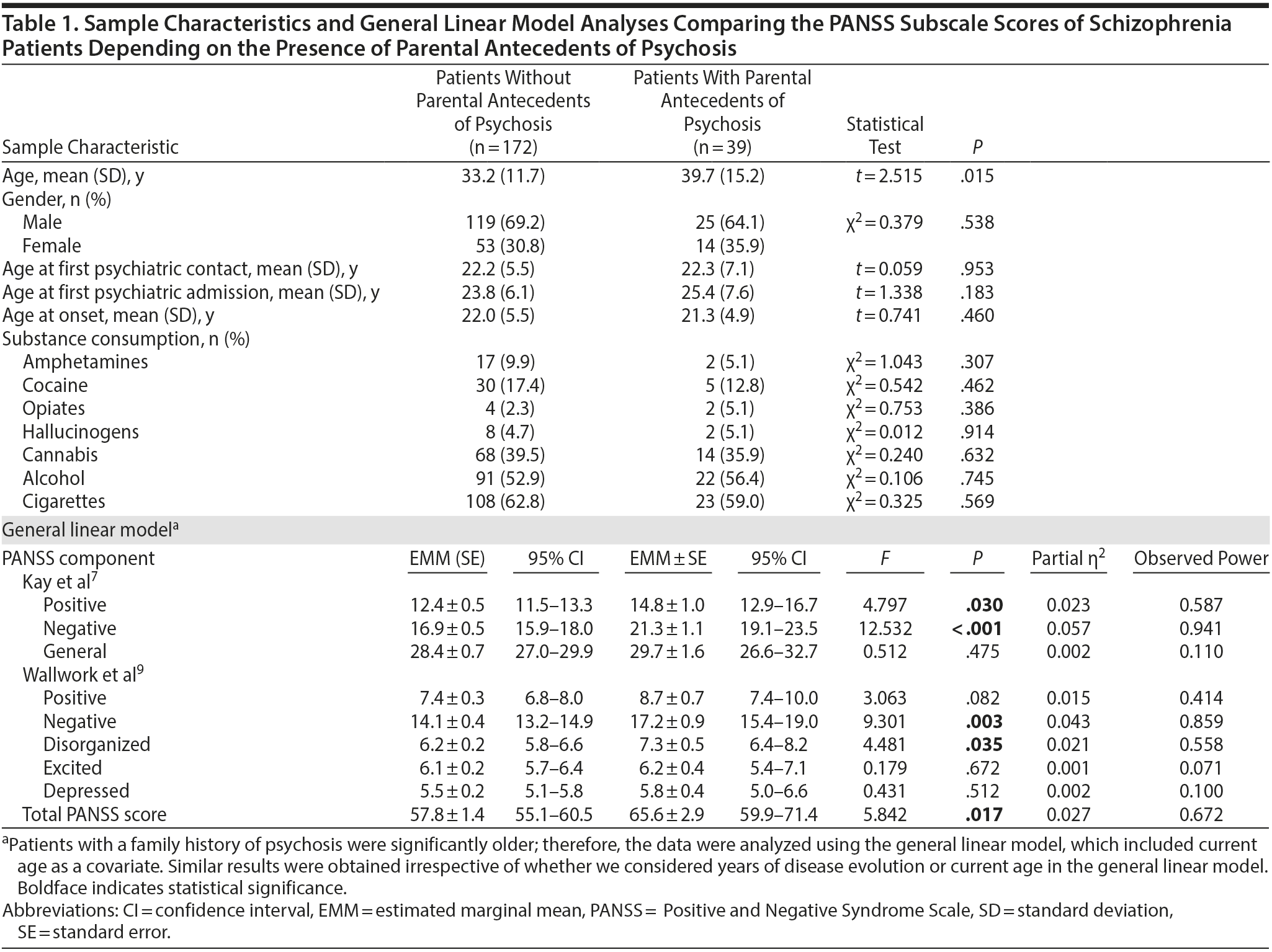
Results. Table 1 shows the sample characteristics and the results of the study. Patients with parental antecedents of schizophrenia presented higher estimated marginal means on all of the PANSS subscales, and statistically significant differences were observed in the positive and negative subscales described by Kay et al7 and in the negative and disorganized subscales described by Wallwork et al.9
The present study found that patients with parental antecedents of schizophrenia presented a more severe phenotype, as measured by the positive and negative PANSS subscales. Patients with antecedents of psychoses in parents presented a more severe phenotype, according to the positive and negative subscales of Kay et al7 and the negative and disorganized dimensions of Wallwork et al.9 Although we were not able to consider the environmental effect of being brought up by a parent with schizophrenia, epidemiologic studies have shown greater effects for genetic factors than for environmental factors.1 Previous studies comparing the symptomatology of familial and nonfamilial cases have associated familial schizophrenia with greater severity of both negative2,3 and positive symptoms,4 though not in the same study. Familial schizophrenia has also been associated with an earlier age at onset, more severe structural brain abnormalities, a higher number of minor physical anomalies, a higher incidence of deficit syndrome, poorer outcomes, and greater impairment of cognitive functions.10 Historically, having a first-degree relative diagnosed with schizophrenia has been identified as the main risk factor for developing the illness, with an odds ratio of 9.8.1 Similar results have recently been found by large population-based studies.11,12 Interestingly, Agerbo et al11 showed that the risk of schizophrenia among individuals with a first-degree relative with the disease was 8.3, similar to the 8.0 value suggested by the Polygenic Risk Score (PRS), a composite score based on associated genetic variants. Agerbo et al noted a significant interaction between the PRS and family history of schizophrenia, which seems to indicate that patients with familial antecedents present higher genetic liability.
The results of the present study emphasize the need to consider the antecedents of psychosis in clinical practice, because having a family history of schizophrenia is associated with a more severe clinical expression of the disease. Additionally, our results contribute new evidence that the stratification of the sample according to the presence of psychosis in the family may reduce the heterogeneity of schizophrenia and could be a valuable variable in clinical and genetic studies intending to elucidate the neurobiological basis of schizophrenia.
References
1. Sullivan PF. The genetics of schizophrenia. PLoS Med. 2005;2(7):e212. PubMed
2. Malaspina D, Goetz RR, Yale S, et al. Relation of familial schizophrenia to negative symptoms but not to the deficit syndrome. Am J Psychiatry. 2000;157(6):994-1003. PubMed doi:10.1176/appi.ajp.157.6.994
3. Mart×n Reyes M, Mendoza Qui×±ónez R, D×az de Villalvilla T, et al. Family transmission of positive and negative symptoms in familial and sporadic schizophrenia [in Spanish]. Actas Esp Psiquiatr. 2004;32(6):353-357. PubMed
4. Sautter FJ, McDermott BE. The short-term course of familial and nonfamilial schizophrenic-spectrum disorder. J Psychiatr Res. 1994;28(1):97-106. PubMed doi:10.1016/0022-3956(94)90038-8
5. Endicott NC, Andreasen RL, Spitzer RL. Family History-Research Diagnostic Criteria (FH-RDC). 3rd ed. New York, NY: New York State Psychiatric Institute; 1978.
6. Verge B, Alonso Y, Miralles C, et al. New evidence for the involvement of mitochondrial inheritance in schizophrenia: results from a cross-sectional study evaluating the risk of illness in relatives of schizophrenia patients. J Clin Psychiatry. 2012;73(5):684-690. PubMed doi:10.4088/JCP.10m06718
7. Kay SR, Fiszbein A, Opler LA. The Positive and Negative Syndrome Scale (PANSS) for schizophrenia. Schizophr Bull. 1987;13(2):261-276. PubMed doi:10.1093/schbul/13.2.261
8. Peralta V, Cuesta MJ. Psychometric properties of the Positive and Negative Syndrome Scale (PANSS) in schizophrenia. Psychiatry Res. 1994;53(1):31-40. PubMed doi:10.1016/0165-1781(94)90093-0
9. Wallwork RS, Fortgang R, Hashimoto R, et al. Searching for a consensus five-factor model of the Positive and Negative Syndrome Scale for schizophrenia. Schizophr Res. 2012;137(1-3):246-250. PubMed doi:10.1016/j.schres.2012.01.031
10. Erol A, Bayram S, Kosger F, et al. Executive functions in patients with familial versus sporadic schizophrenia and their parents. Neuropsychobiology. 2012;66(2):93-99. PubMed doi:10.1159/000337738
11. Agerbo E, Sullivan PF, Vilhjálmsson BJ, et al. Polygenic risk score, parental socioeconomic status, family history of psychiatric disorders, and the risk for schizophrenia: a Danish population-based study and meta-analysis. JAMA Psychiatry. 2015;72(7):635-641. PubMed doi:10.1001/jamapsychiatry.2015.0346
12. Svensson E, Rogvin M, Hultman CM, et al. Schizophrenia susceptibility and age of diagnosis—a frailty approach. Schizophr Res. 2013;147(1):140-146. PubMed doi:10.1016/j.schres.2013.03.004
aHospital Universitari Institut Pere Mata, IISPV, Universitat Rovira i Virgili, CIBERSAM, Reus, Catalonia, Spain
bDepartment of Psychiatry, Corporació Sanit× ria I Universit× ria Parc Taul×, Sabadell, Catalonia, Spain
Submitted: July 16, 2015; accepted December 4, 2015.
Potential conflicts of interest: None.
Funding/support: Supported in part by the Spanish Ministry of Science and Innovation, Instituto de Salud Carlos III, Madrid, Spain, Grant PS09/01052, and ERDF (European Regional Development Fund).
Role of the sponsor: The funding agencies had no role in the design, preparation, or decision to submit this letter for publication.
J Clin Psychiatry 2016;77(9):1201-1202
dx.doi.org/10.4088/JCP.15l10241
© Copyright 2016 Physicians Postgraduate Press, Inc.
This PDF is free for all visitors!