‘ ‹’ ‹
Click to enlarge page
Awareness of the prevalence and impact of bipolar disorder in pediatric patients has grown in recent years. Youths with this disorder are at risk for poor long-term outcomes, but with careful screening, clinicians may be able to detect early signs or subthreshold symptoms and provide a timely diagnosis and effective treatment. Although several pharmacologic options are available for patients aged 10 years and up, they differ in their safety and tolerability profiles. Clinicians should select the agent that best balances benefit and risk—at the lowest efficacious dose—and provide careful monitoring for adverse events throughout treatment.
Johns Hopkins University and the Kennedy Krieger Institute, Baltimore, Maryland. (Dr Findling); Private practice, Menlo Park, California (Dr Chang)
‘ ‹’ ‹’ ‹’ ‹’ ‹’ ‹’ ‹

This Academic Highlights section of The Journal of Clinical Psychiatry presents the highlights of the planning teleconference series “Improving the Diagnosis and Treatment of Adolescent Bipolar Disorder,” which was held in June 2017. This report was prepared and independently developed by the CME Institute of Physicians Postgraduate Press, Inc., and was supported by an educational grant from Sunovion Pharmaceuticals Inc.
The teleconference was chaired by Robert L. Findling, MD, MBA (chair), from Johns Hopkins University and the Kennedy Krieger Institute, Baltimore, Maryland. The faculty was Kiki D. Chang, MD, who is in private practice in Menlo Park, California.
Financial Disclosure: All individuals in a position to influence the content of this activity were asked to complete a statement regarding all relevant personal financial relationships between themselves or their spouse/partner and any commercial interest. The CME Institute has resolved any conflicts of interest that were identified. In the past year, Marlene P. Freeman, MD, Editor in Chief, has received research funding from JayMac and Sage, has been a member of the Independent Data Safety and Monitoring Committee for Janssen, has been medical editor for the Global Organization for EPA and DHA Omega-3s newsletter, and, as a Massachusetts General Hospital (MGH) employee, works with the MGH National Pregnancy Registry, which is sponsored by Alkermes, Otsuka, Actavis, and Sunovion, and works with the MGH Clinical Trials Network and Institute, which receives research funding from multiple pharmaceutical companies and the National Institute of Mental Health. No member of the CME Institute staff reported any relevant personal financial relationships.
J Clin Psychiatry 2018;79(2):su17023ah3c
To cite: Findling RL, Chang KD. Improving the diagnosis and treatment of pediatric bipolar disorder. J Clin Psychiatry. 2018;79(2):su17023ah3c.
To share: https://doi.org/10.4088/JCP.su17023ah3c
© Copyright 2018 Physicians Postgraduate Press, Inc.
Bipolar disorder is a serious mental illness associated with premature mortality and potentially severe disability, and it may affect as much as 6% of the adult population when the full bipolar spectrum is considered.1 Bipolar disorder was previously considered to occur only rarely, if ever, in children and adolescents.2 Yet, over the past 20 years, a body of scientific literature has grown supporting the validity of bipolar diagnoses in this age group,3 and diagnostic rates have increased dramatically.4 These developments have created controversy and generated concerns that pediatric patients are now being overdiagnosed with bipolar disorder. However, between 50% and 66% of adults with well-diagnosed bipolar disorder report onset prior to age 19 years, and 15%-28% experienced onset prior to age 13 years; these data indicate that bipolar disorder may be more common in this population than is generally believed, potentially affecting as many as 2 million children in the United States alone.5
Compared with adult-onset bipolar disorder, pediatric bipolar disorder is associated with a more severe course of illness, greater treatment resistance, an increased risk for substance abuse and suicidality, and poorer psychosocial outcomes.5-7 To mitigate these risks, clinicians must first accurately differentiate bipolar disorder from conditions with similar presentations and then formulate an effective treatment plan for patients. In this Academic Highlights, Drs Robert L. Findling and Kiki D. Chang discuss current evidence on accurately diagnosing and safely and effectively treating bipolar disorder in pediatric patients. Drs Findling and Chang defined pediatric as ages 10 to 17 years.
RECOGNITION AND DIAGNOSIS OF BIPOLAR DISORDER IN PEDIATRIC PATIENTS
The prevalence of and appropriate diagnostic criteria for pediatric bipolar disorder have long been topics of debate due to the often ambiguous nature of bipolar symptoms in this population and because diagnostic rates appear to have increased dramatically in recent years, raising fears of overdiagnosis.2,8 Dr Chang explained that the diagnostic rate of pediatric bipolar disorder increased 40-fold from 1994 to 2003; by comparison, the diagnostic rate in adults increased only one-fold during the same time period.4 However, the overall number of clinical diagnoses in youth remained low, with office-based visits with bipolar disorder diagnosis increasing from only 0.01%-0.44% during that same time period.4
Special Considerations for the Assessment of Pediatric Patients
Because available treatments for pediatric bipolar disorder are associated with considerable risks, young patients must be carefully assessed for signs of and risk factors for this condition, and then formally diagnosed using standardized diagnostic criteria before treatment is initiated.2 Diagnostic interviewing will most likely be the primary method for obtaining evidence of manic symptoms because direct observation of these symptoms in the acute care setting is not always possible. According to Dr Chang, the interview process for pediatric patients differs from that for adults. Information will need to be gathered from multiple sources to build a complete picture of pediatric patient symptomatology because different informants will have different perceptions of observed behaviors.2 Clinicians should interview or collect information from the patient, the patient’s parents, and collateral sources such as teachers. Additionally, parents should always be asked for a family history of psychiatric conditions, but clinicians should be aware that these histories are often underreported. Parents are usually able to provide the most accurate information about symptoms of mania and functional impairment because they tend to be most familiar with the patient’s behavior. Teachers are not typically a reliable source of information about manic symptoms because they are not in a position to observe symptoms like decreased need for sleep and may mistake other symptoms of mania for attention-deficit/hyperactivity disorder (ADHD) or oppositional disorders.9 Patients are also not reliable sources of information about these symptoms because they often lack insight into mania.2 Patients are, however, the most reliable source of information on depressive symptoms because often these symptoms are internalized and frequently not shared with parents or other people.
Dr Chang pointed out that structured interview techniques are frequently used in research settings to help clinicians gather important assessment information, but in practice, clinicians typically use unstructured interview techniques that may not always reliably uncover manic episodes in pediatric patients. Bipolar disorder could be more accurately diagnosed with the application of structured interviews and screening tools that have been demonstrated to reliably detect manic symptomatology. Examples of these types of instruments include the Schedule for Affective Disorders and Schizophrenia for School-Age Children-Present and Lifetime version (K-SADS-PL),10,11 the Child Mania Rating Scale (CMRS),12 the Parent Young Mania Rating Scale (P-YMRS)13 and the short form of the Parent General Behavior Inventory (P-GBI).14

- Be alert for signs of mania or hypomania in young patients presenting with depression, attention-deficit/hyperactivity disorder, anxiety, or irritability.
- Include reliable informants such as teachers and parents when conducting diagnostic assessments.
- Be familiar with the variable presentations of manic symptoms in different age groups.
- Select treatments that provide the optimal balance of efficacy and tolerability.
- Monitor patients throughout treatment for the development of any medication-related adverse events such as signs of toxicity in patients receiving lithium or weight gain and other metabolic changes in patients receiving atypical antipsychotics.
Early Signs of Potential Bipolar Prodrome
Dr Chang emphasized that the ability to identify initial presentations of bipolar disorder in youth is of the utmost importance for providing an accurate diagnosis and early treatment. Yet, diagnosing bipolar disorder in young patients is challenging because symptom patterns in children and adolescents are not the same as in adults and can change with age and developmental state.15 In some cases, they will present with bipolar symptoms that do not yet meet full criteria for a diagnosis.3
Bipolar disorder is now beginning to be considered a progressive condition with a prodromal period, after which a patient may or may not progress to the full illness. Clinicians, therefore, should be alert for several clinical presentations that can potentially indicate a possible diagnosis of pediatric bipolar disorder, including depression, ADHD, anxiety, and irritability.16,17 However, Dr Chang stated that individually, none of these presentations necessarily indicate bipolar disorder, but when two or more occur together and/or with a family history of mood disorders, clinicians should suspect underlying bipolar disorder and probe further.
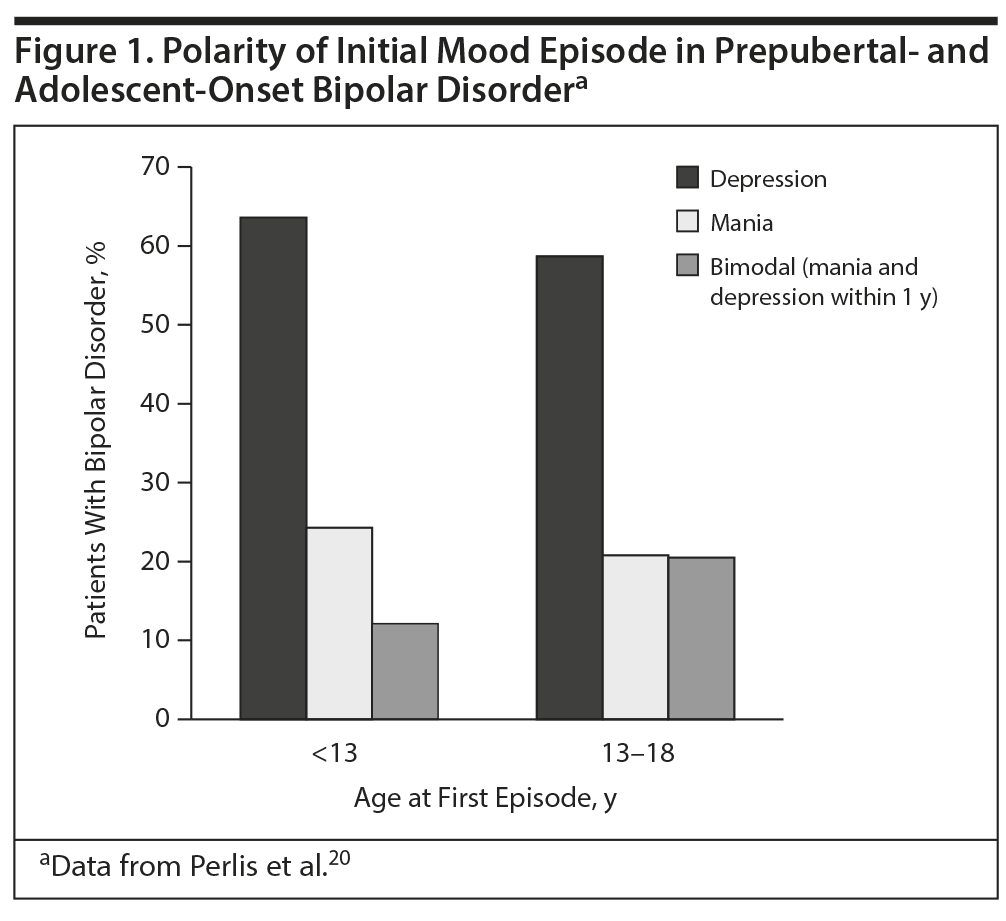
Depression. Depression is one of the most common indicators of pediatric bipolar disorder and is often the first presenting symptom.18 Geller and colleagues19 followed up with a group of adults who had participated in a depression study as children and found that 48.6% had converted to a bipolar disorder diagnosis. Furthermore, Perlis and colleagues20 assessed the illness onset characteristics of the first 1,000 patients enrolled in the Systematic Treatment Enhancement Program for Bipolar Disorder (STEP-BD) and found that among patients who experienced onset prior to age 18 years, more than twice as many experienced depression as an initial episode compared with mania onset (Figure 1).20
When pediatric patients present with depression, certain variables are associated with an increased risk of a bipolar outcome and should prompt clinicians to screen for past manic episodes and monitor for future ones. These variables include a rapid onset of depression, psychomotor retardation, psychosis, pharmacologic hypomania, ADHD with mood instability, mood lability, and family history of mood disorders (especially bipolar disorder).21-24
ADHD. In pediatric patients, ADHD may be misdiagnosed as bipolar disorder because symptoms such as restlessness, distractibility, and sleep difficulties overlap. However, clinicians can accurately attribute the symptoms to bipolar disorder if they determine that they occur episodically rather than chronically.25 Clinicians should be aware that ADHD is also frequently comorbid with bipolar disorder, and to complicate matters further, the presence of ADHD alone may antecede the development of bipolar disorder.26 Joshi and Wilens16 found comorbidity rates of ADHD to be 84% in patients with childhood-onset bipolar disorder and 52% in those with adolescent-onset bipolar disorder. Thus, patients who have ADHD plus a family history of bipolar disorder may eventually develop a bipolar disorder.24,27
Anxiety. Dr Chang expressed that anxiety is common in youths and is not necessarily suggestive of underlying mood dysregulation. In the presence of other warning signs, though, such as a family history of bipolar disorder, further investigation is warranted because anxiety and bipolar disorders are frequently comorbid.16,25 Depending on the population studied and the type of anxiety disorder, comorbidity rates with bipolar disorder have ranged from 12.5% to 76%.16
Irritability. According to Dr Chang, irritability and anger are perhaps the most common presenting problems in youths with bipolar disorder. Irritability is common in pediatric bipolar disorder, but when irritability does occur in a child, it is not necessarily due to mania and does not necessarily indicate the presence of bipolar disorder.3,17 Irritability is very common in young people in general and may be due to many factors, including depression, anxiety, pervasive developmental disorders, frustration with attentional deficits associated with ADHD, disruptive mood dysregulation disorder, and oppositional disorders.28,29 Nevertheless, the presence of severe irritability that is episodic in nature and begins or increases in conjunction with other manic symptoms should raise the index of suspicion for underlying bipolar disorder and warrant investigation.3
Diagnostic Criteria for Bipolar Disorder
When pediatric patients present with clear evidence of mania or hypomania that cannot be attributed to the use of a medication, substance use, or another medical condition, they should be assessed for a bipolar diagnosis. The Diagnostic and Statistical Manual for Mental Disorders25 (DSM-5) criteria for bipolar disorders are the same for both adult and pediatric patients. A bipolar I disorder diagnosis requires the occurrence of at least 1 manic episode, and a bipolar II disorder diagnosis requires 1 depressive episode or more and 1 hypomanic episode or more. The DSM-525 also includes a diagnostic category for other specified bipolar and related disorders that is characterized by subthreshold symptoms not meeting diagnostic criteria for bipolar I or II disorder but that still cause distress or impairment and last 2 to 3 days.
Although the diagnostic criteria for adults and children are the same, identifying mania in pediatric patients can be tricky because, in general, children and adolescents have more mood fluctuations and mood lability than adults. Youths naturally have mood states that can change quickly. To qualify for a manic episode, young patients with bipolar disorder need to exhibit an elevated, irritable, or expansive mood lasting for at least 1 week for mania or 4 days for hypomania, with the mood symptoms present for most of each day but not necessarily 24 hours a day.25 Dr Chang added that although bipolar disorder not otherwise specified (NOS) is no longer an official DSM diagnosis, this construct should be considered in pediatric patients who have manic symptoms lasting more than 4 hours per day but less than 4 days in a row. These patients experience considerable impairment and are likely to progress to full mania within a few years. A study by Axelson et al30 of pediatric patients meeting criteria for bipolar disorder NOS found that after 5 years, 36% of the youths with no family history of bipolar disorder and 59% of those with a first- or second-degree relative with bipolar disorder had converted to bipolar I or II disorder.
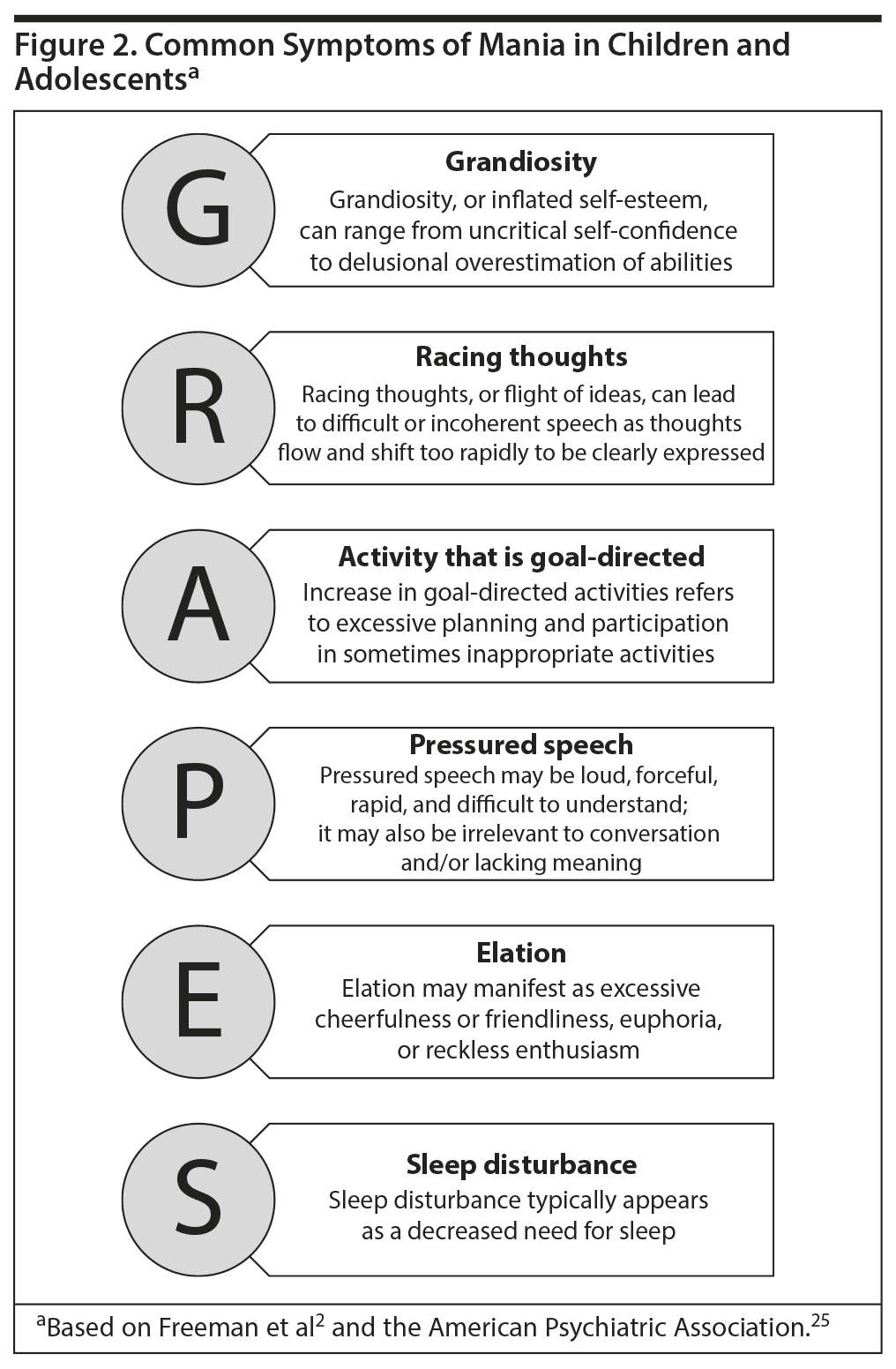
For a DSM diagnosis of bipolar disorder to be present, patients must exhibit not only elevated, expansive, or irritable mood but also 3 or more symptoms of mania if the primary mood is elevated or 4 or more symptoms if the primary mood is irritable.25 Dr Chang suggested using the mnemonic GRAPES to remember the cardinal symptoms of mania: Grandiosity, Racing thoughts, Activity that is goal-directed, Pressured speech, Elation, and Sleep disturbance (Figure 2).2,25 When evaluating pediatric patients for these symptoms, clinicians must know what is developmentally normal for different age groups in different settings so that they can determine when these symptoms are not age-appropriate. For instance, it is normal for a 10-year-old to display an excited, elevated mood at an amusement park, but if this same mood is exhibited in church or repeatedly in the classroom, it may be an indication of mania.31
Disruptive Mood Dysregulation Disorder
Disruptive mood dysregulation disorder (DMDD) is a new diagnosis in the DSM-5 that, as Dr Chang explained, was added to reduce the perceived overdiagnosis of pediatric bipolar disorder. This diagnosis is for young patients who exhibit chronic, severe irritability with temper outbursts but no other symptoms of mania.2,8 The diagnostic criteria require the patient to experience severe and persistent irritability with 3 or more severe temper outbursts per week.25 The anger and irritability must be displayed in multiple settings and must have been present for at least a year, with onset between the ages of 6 and 10 years.25 The diagnosis of DMDD is controversial. Little research exists on this disorder, and, therefore, little is known about the stability of the diagnosis over time, the possibility for remission, or even effective treatments.3,8 At this point, more longitudinal data on prevalence and treatment are needed for the usefulness of the DMDD diagnosis to be determined.3
Case Practice Question
Case 1. Bianca is a 15-year-old girl whose parents forced her to come in for an evaluation regarding her unusual behavior, including wearing revealing clothing, talking back, and staying up late. Who are the most reliable reporters to ask about symptoms of mania?
- Bianca
- Her teachers
- Her parents
- Her siblings
Discussion of Case Practice Question
Preferred response: c. Her parents
Although all of the possible informants may have important information to provide, Bianca’s parents are the most familiar with her behavior. Siblings are usually not as reliable. Bianca is likely to be relatively unreliable because mania often clouds insight and judgment in the patient, and teachers may attribute her behavior to oppositionality rather than mania.
TREATING BIPOLAR DISORDER IN ADOLESCENTS
Dr Findling began his discussion of treatment options for bipolar disorder in adolescents with the important reminder that although the information given here focuses on pharmacotherapy, clinicians should also consider nonpharmacologic treatment approaches. Psychological, school-based, family-based, and peer-based psychosocial treatments may benefit adolescents with bipolar disorder, and support groups and group psychosocial interventions may be helpful for the entire family.15 When planning pharmacologic treatment for adolescent patients with bipolar disorder, clinicians should choose agents on the basis of not only demonstrated efficacy but also on the medication’s adverse event profile.
Pharmacotherapy for Acute Manic and Mixed Episodes
As of February 2018, the US Food and Drug Administration (FDA) has approved only lithium and the atypical antipsychotics risperidone, olanzapine, quetiapine, aripiprazole, and asenapine for treating manic and/or mixed states in adolescents with bipolar disorder.32 In addition to these approved agents, other pharmacologic treatments, namely anticonvulsants and additional antipsychotics, have been studied as acute treatments for adolescent manic and mixed states, but definitive evidence of efficacy for these agents is lacking in this population.3,15 Regardless of the regulatory approval status of the agent being used, patient safety and medication tolerability should be closely monitored throughout treatment.
Lithium. Lithium has long been considered a mainstay of treatment for mania in adults. Despite this agent’s historically having FDA approval for use in pediatric mania, rigorous placebo-controlled data were not available in this population until fairly recently.33 The Collaborative Lithium Trials (CoLT)34 were designed to fill this void. In the first double-blind efficacy study33 to be conducted as part of the CoLT initiative, 81 patients aged 7 to 17 years experiencing a bipolar I manic or mixed episode were randomly assigned to receive either lithium or placebo for up to 8 weeks. The study showed that lithium was significantly better than placebo in reducing manic symptoms (P < .05) as measured by the Young Mania Rating Scale (YMRS). Dr Findling noted that the YMRS is a key outcome measure frequently used to assess the effectiveness of mania treatments.35 Another notable finding of the study was that lithium was not associated with weight gain, which is a problem with several other agents used to treat bipolar disorder.33 The most common side effects were gastrointestinal, eg, nausea, diarrhea, and vomiting, but these rarely led to study discontinuation.
Dr Findling explained that blood lithium levels should be monitored in patients to prevent lithium toxicity, and clinicians should be alert for early signs of toxicity including ataxia, motor coordination difficulties, and tremor.36 This agent has a narrow therapeutic window, and the best time to measure lithium levels is 12 hours after the last dose. During lithium treatment, clinicians should also monitor adolescent patients’ renal, thyroid, parathyroid, neurologic, and cardiac function and watch for hematologic changes, such as an increased number of white blood cells.34
Anticonvulsants. Several anticonvulsant therapies have been studied for efficacy in treating bipolar mania, but overall, none of them have definitively demonstrated superiority to placebo and none have been approved to treat bipolar mania in adolescents.
Wagner and colleagues37 conducted a trial of divalproex extended-release for manic and mixed states in 150 adolescent patients. After 4 weeks, the patients receiving the medication had experienced no improvement from baseline YMRS scores compared with placebo.
A trial38 evaluating topiramate in 56 pediatric patients initially looked promising, but the study was discontinued after a concurrent adult study failed to show topiramate superiority over placebo. While patients in the adolescent study appeared to have substantial improvement, the results are inconclusive due to the small sample size coupled with the absence of a statistically significant difference between topiramate and placebo.
A multicenter trial39 of oxcarbazepine also failed to show benefit over placebo in 116 adolescents. Oxcarbazepine-treated patients’ YMRS scores at the end of the trial were not significantly different from those in the placebo group.
Atypical antipsychotics. Unlike anticonvulsants, many atypical antipsychotics have shown significant superiority to placebo in reducing manic symptoms, but the side effect profiles of atypical antipsychotics must be balanced against their effectiveness. The American Academy of Child and Adolescent Psychiatry (AACAP) practice parameters for the use of atypical antipsychotics in children and adolescents40 recommend monitoring patient weight and body mass index, blood glucose and risk of diabetes, lipid profiles, extrapyramidal side effects, and abnormal involuntary movements. Cardiovascular health should also be monitored via regular blood pressure and heart rate screenings, and any significant electrocardiographic changes should be evaluated.
Haas and colleagues41 compared treatment with risperidone at 0.5-2.5 mg/d and 3.0-6.0 mg/d to placebo for 3 weeks in 169 children and adolescents. Patients randomly assigned to the lower- and higher-dose risperidone groups showed similar improvement in YMRS scores, and both groups showed significant improvement over placebo (P < .001 for both doses). Adverse effects included somnolence, headache, and fatigue and were more severe in the higher-dose group than in the lower-dose group. Dr Findling emphasized that although both active treatment groups experienced similar improvement, the group receiving the higher dose also experienced a heavier burden of side effects, which is an excellent illustration of why patients should initially be treated with the minimally effective evidence-based dose in order to minimize side effects.
Tohen and colleagues42 conducted a multicenter study of 161 adolescents experiencing an acute manic or mixed episode to assess the safety and efficacy of olanzapine (2.5-20.0 mg/d) compared with placebo. The investigators found significantly greater improvement in YMRS scores from baseline (P < .001) in the olanzapine group; however, the side effect profile caused concern. In 3 weeks, olanzapine-treated patients gained a mean of 3.7 kg, while placebo-treated patients gained a mean of 0.3 kg. In addition, changes in fasting blood glucose, cholesterol, hepatic enzymes, prolactin, and uric acid were significantly greater with olanzapine than with placebo.
Pathak et al43 conducted a 3-week trial of quetiapine in 277 adolescents with bipolar mania. Patients were randomly assigned to receive either 400 mg/d or 600 mg/d. Both doses were found to be superior to placebo (P < .001). Adverse effects associated with quetiapine were mostly mild to moderate; the most common were somnolence, sedation, dizziness, and headache. In addition, patients in both quetiapine groups experienced weight gain (mean 1.7 kg for both doses versus 0.4 kg for placebo) and greater mean changes in fasting glucose, total cholesterol, low-density lipoprotein cholesterol, triglycerides, insulin, and prolactin.
A 4-week study44 evaluated aripiprazole at 10 mg/d and 30 mg/d in 296 adolescents. The authors found that, as in the case of risperidone, mean YMRS score reductions with both doses of aripiprazole were significantly superior to those with placebo (P < .0001 for both doses). Again, the higher dose of aripiprazole was associated with increased incidence of some adverse effects, such as somnolence and extrapyramidal disorder, compared with the lower dose.
Asenapine is the most recent antipsychotic to gain FDA approval for treating pediatric mania. A 2015 trial45 compared asenapine with placebo in 403 adolescents at 3 twice-daily doses: 2.5 mg, 5.0 mg, and 10.0 mg. Patients showed more improvement in manic or mixed episodes with asenapine at all doses than with placebo (P < .001). Asenapine had adverse effects similar to those of other atypical antipsychotics, including somnolence, sedation, and increased appetite. Patients also experienced oral paresthesia or hypoesthesia as well as increased weight gain and higher levels of glucose, lipid parameters, and insulin compared with placebo.
Other atypical antipsychotics have been investigated for adolescent mania but not received regulatory approval for its use in this patient population. Dr Findling and colleagues46 conducted a 4-week trial of ziprasidone in which 237 adolescents participated first in a randomized controlled trial (RCT) and then in a 26-week open-label extension study. Ziprasidone was found to be superior to placebo in the RCT (P = .0005), and continued improvement in YMRS scores occurred in the extension. Adverse effects associated with ziprasidone treatment included sedation, somnolence, headache, fatigue, and nausea. Although the results from this study suggested benefit, the FDA did not approve ziprasidone for the treatment of bipolar mania due to concerns about the precision with which the study was executed.
Pharmacotherapy for Bipolar Depression
Treatment of bipolar depression in adolescents must be undertaken cautiously to prevent mood destabilization or a switch to a manic or mixed episode.15 Currently, there are two FDA-approved treatment options for bipolar depression in adolescents—the olanzapine/fluoxetine combination and lurasidone. An 8-week trial47 of the olanzapine/fluoxetine combination in 176 adolescents with bipolar depression found significant superiority to placebo (P < .01). The most common adverse effects were somnolence, weight gain, and increased appetite. Patients taking the olanzapine/fluoxetine combination gained significantly more weight than placebo-treated patients (4.4 kg compared with 0.5 kg, P < .001).
Recently, DelBello et al48 conducted a 6-week study that evaluated the efficacy and safety of lurasidone (20-80 mg/d) in 347 adolescents with bipolar depression. Lurasidone was associated with significantly decreased depressive symptoms compared to placebo (P < .0001). Adverse events with lurasidone were relatively modest; the most common were nausea and somnolence.
Other agents have been studied for adolescent bipolar depression but failed to show benefit. Two separate studies43,49 that investigated quetiapine for pediatric bipolar depression found a nearly identical benefit to that of placebo. Although no difference was found between quetiapine and placebo in these 2 trials, Dr Findling pointed out that patients still experienced benefit whether it was from the treatment or placebo.
Bipolar Maintenance Pharmacotherapy
Although many adolescent patients with bipolar disorder will require ongoing pharmacologic treatment to prevent relapse,15 few placebo-controlled studies of maintenance treatments have been conducted in this population.3 One study50 investigated the efficacy of lamotrigine as adjunctive maintenance treatment for bipolar I disorder in 173 adolescents. Patients started the trial with lamotrigine added to their usual pharmacotherapy; this was followed by randomization to either continue taking lamotrigine or take adjunctive placebo for up to 36 weeks. Time to a bipolar event (ie, depressed, manic/hypomanic, or mixed mood state) was the primary outcome measure. A benefit for adjunctive lamotrigine was not found in patients aged 10 to 12 years; however, older patients (aged 13-17 years) appeared to have benefit in a post hoc analysis. The primary analysis of the overall population did not demonstrate a statistically significant difference between active treatment and placebo (P = .072). Lamotrigine is not approved for the treatment of bipolar disorder in patients aged 10 to 17 years.
Case Practice Question
Case 2. Jill is a 16-year-old girl. She has previously been hospitalized twice for manic episodes and has taken no medication in 3 months. Jill now presents with depressed mood and symptoms consistent with a major depressive episode. Which pharmacologic intervention has the best evidence to support its prescription to Jill?
- Olanzapine/fluoxetine combination
- Quetiapine
- Lithium
Discussion of Case Practice Question
Preferred response: a. Olanzapine/fluoxetine combination
Olanzapine/fluoxetine combination is the first agent FDA-approved to treat episodes of bipolar depression in adolescent patients.
CONCLUSION
Bipolar disorder in children and adolescents is more common than previously thought and carries a considerable risk for poor long-term outcomes, which places a great responsibility on clinicians to accurately recognize this disorder as soon as possible and initiate safe and effective treatment. To accomplish early recognition of bipolar disorder in pediatric patients, clinicians must be aware of early signs of the disorder and then follow up with a full diagnostic evaluation. After diagnosis, clinicians must select from several pharmacologic approaches that have demonstrated efficacy, while also considering the risk for adverse effects. No matter which medication is chosen, patient safety and tolerability should be closely monitored throughout the course of treatment. These evidence-based strategies can enable clinicians to achieve optimal patient outcomes in pediatric bipolar disorder with available treatments.
Find more articles on this and other psychiatry and CNS topics:
The Journal of Clinical Psychiatry
The Primary Care Companion for CNS Disorders
REFERENCES
1. Merikangas KR, Akiskal HS, Angst J, et al. Lifetime and 12-month prevalence of bipolar spectrum disorder in the National Comorbidity Survey replication. Arch Gen Psychiatry. 2007;64(5):543-552. PubMed CrossRef
2. Freeman AJ, Chang K, Youngstrom E. Diagnosing bipolar disorder in children and adolescents. In: Yildiz A, Ruiz P, Nemeroff CB, eds. The Bipolar Book: History, Neurobiology, and Treatment. Oxford, UK: Oxford University Press; 2015:61-87.
3. Goldstein BI, Birmaher B, Carlson GA, et al. The International Society for Bipolar Disorders Task Force report on pediatric bipolar disorder: knowledge to date and directions for future research. Bipolar Disord. 2017;19(7):524-543. PubMed CrossRef
4. Moreno C, Laje G, Blanco C, et al. National trends in the outpatient diagnosis and treatment of bipolar disorder in youth. Arch Gen Psychiatry. 2007;64(9):1032-1039. PubMed CrossRef
5. Post RM, Kowatch RA. The health care crisis of childhood-onset bipolar illness: some recommendations for its amelioration. J Clin Psychiatry. 2006;67(1):115-125. PubMed CrossRef
6. Leverich GS, Post RM, Keck PE, et al. The poor prognosis of childhood-onset bipolar disorder. J Pediatr. 2007;150(5):485-490. PubMed CrossRef
7. Carter TDC, Mundo E, Parikh SV, et al. Early age at onset as a risk factor for poor outcome of bipolar disorder. J Psychiatr Res. 2003;37(4):297-303. PubMed CrossRef
8. Mason BL, Brown ES, Croarkin PE. Historical underpinnings of bipolar disorder diagnostic criteria. Behav Sci (Basel). 2016;6(3). PubMed CrossRef
9. Youngstrom EA, Birmaher B, Findling RL. Pediatric bipolar disorder: validity, phenomenology, and recommendations for diagnosis. Bipolar Disord. 2008;10(1 pt 2):194-214. PubMed CrossRef
10. Ambrosini PJ. Historical development and present status of the Schedule for Affective Disorders and Schizophrenia for School-Age Children (K-SADS). J Am Acad Child Adolesc Psychiatry. 2000;39(1):49-58. PubMed CrossRef
11. Kaufman J, Birmaher B, Brent D, et al. Schedule for Affective Disorders and Schizophrenia for School-Age Children-Present and Lifetime Version (K-SADS-PL): initial reliability and validity data. J Am Acad Child Adolesc Psychiatry. 1997;36(7):980-988. PubMed CrossRef
12. Pavuluri MN, Henry DB, Devineni B, et al. Child Mania Rating Scale: development, reliability, and validity. J Am Acad Child Adolesc Psychiatry. 2006;45(5):550-560. PubMed CrossRef
13. Marchand WR, Clark SC, Wirth L, et al. Validity of the Parent Young Mania Rating Scale in a community mental health setting. Psychiatry (Edgmont). 2005;2(3):31-35. PubMed
14. Youngstrom EA, Frazier TW, Demeter C, et al. Developing a 10-item mania scale from the Parent General Behavior Inventory for children and adolescents. J Clin Psychiatry. 2008;69(5):831-839. PubMed CrossRef
15. McClellan J, Kowatch R, Findling RL, Work Group on Quality Issues. Practice parameter for the assessment and treatment of children and adolescents with bipolar disorder. J Am Acad Child Adolesc Psychiatry. 2007;46(1):107-125. PubMed CrossRef
16. Joshi G, Wilens T. Comorbidity in pediatric bipolar disorder. Child Adolesc Psychiatr Clin N Am. 2009;18(2):291-319. PubMed CrossRef
17. Van Meter AR, Burke C, Kowatch RA, et al. Ten-year updated meta-analysis of the clinical characteristics of pediatric mania and hypomania. Bipolar Disord. 2016;18(1):19-32. PubMed CrossRef
18. Lish JD, Dime-Meenan S, Whybrow PC, et al. The National Depressive and Manic-depressive Association (DMDA) survey of bipolar members. J Affect Disord. 1994;31(4):281-294. PubMed CrossRef
19. Geller B, Zimerman B, Williams M, et al. Bipolar disorder at prospective follow-up of adults who had prepubertal major depressive disorder. Am J Psychiatry. 2001;158(1):125-127. PubMed CrossRef
20. Perlis RH, Miyahara S, Marangell LB, et al. Long-term implications of early onset in bipolar disorder: data from the first 1000 participants in the Systematic Treatment Enhancement Program for Bipolar Disorder (STEP-BD). Biol Psychiatry. 2004;55(9):875-881. PubMed CrossRef
21. Strober M, Carlson G. Bipolar illness in adolescents with major depression: clinical, genetic, and psychopharmacologic predictors in a three- to four-year prospective follow-up investigation. Arch Gen Psychiatry. 1982;39(5):549-555. PubMed CrossRef
22. Akiskal HS. Developmental pathways to bipolarity: are juvenile-onset depressions pre-bipolar? J Am Acad Child Adolesc Psychiatry. 1995;34(6):754-763. PubMed CrossRef
23. Venkataraman S, Naylor MW, King CA. Mania associated with fluoxetine treatment in adolescents. J Am Acad Child Adolesc Psychiatry. 1992;31(2):276-281. PubMed CrossRef
24. Hauser M, Correll CU. The significance of at-risk or prodromal symptoms for bipolar I disorder in children and adolescents. Can J Psychiatry. 2013;58(1):22-31. PubMed CrossRef
25. American Psychiatric Association. Diagnostic and Statistical Manual for Mental Disorders. Fifth Edition. Washington, DC: American Psychiatric Association; 2013.
26. Axelson D, Goldstein B, Goldstein T, et al. Diagnostic precursors to bipolar disorder in offspring of parents with bipolar disorder: a longitudinal study. Am J Psychiatry. 2015;172(7):638-646. PubMed CrossRef
27. Chang K, Howe M, Gallelli K, et al. Prevention of pediatric bipolar disorder: integration of neurobiological and psychosocial processes. Ann N Y Acad Sci. 2006;1094(1):235-247. PubMed CrossRef
28. Hameed U, Dellasega CA. Irritability in pediatric patients: normal or not? Prim Care Companion CNS Disord. 2016;18(2):doi:10.4088/PCC.15br01893. PubMed CrossRef
29. Wozniak J, Biederman J, Richards JA. Diagnostic and therapeutic dilemmas in the management of pediatric-onset bipolar disorder. J Clin Psychiatry. 2001;62(suppl 14):10-15. PubMed
30. Axelson DA, Birmaher B, Strober MA, et al. Course of subthreshold bipolar disorder in youth: diagnostic progression from bipolar disorder not otherwise specified. J Am Acad Child Adolesc Psychiatry. 2011;50(10):1001-1016.e3. PubMed CrossRef
31. Geller B, Zimerman B, Williams M, et al. Phenomenology of prepubertal and early adolescent bipolar disorder: examples of elated mood, grandiose behaviors, decreased need for sleep, racing thoughts and hypersexuality. J Child Adolesc Psychopharmacol. 2002;12(1):3-9. PubMed CrossRef
32. Stahl SM. Prescriber’s Guide, 6th Edition. Cambridge, UK: Cambridge University Press; 2017.
33. Findling RL, Robb A, McNamara NK, et al. Lithium in the acute treatment of bipolar I disorder: a double-blind, placebo-controlled study. Pediatrics. 2015;136(5):885-894. PubMed CrossRef
34. Findling RL, Frazier JA, Kafantaris V, et al. The Collaborative Lithium Trials (CoLT): specific aims, methods, and implementation. Child Adolesc Psychiatry Ment Health. 2008;2(1):21. PubMed CrossRef
35. Young RC, Biggs JT, Ziegler VE, et al. A rating scale for mania: reliability, validity and sensitivity. Br J Psychiatry. 1978;133(5):429-435. PubMed CrossRef
36. Findling RL, Pavuluri MN. Lithium. In: Geller B, DelBello MP, eds. Treatment of Bipolar Disorder in Children and Adolescents. New York, NY: Guilford Press; 2008:43-68.
37. Wagner KD, Redden L, Kowatch RA, et al. A double-blind, randomized, placebo-controlled trial of divalproex extended-release in the treatment of bipolar disorder in children and adolescents. J Am Acad Child Adolesc Psychiatry. 2009;48(5):519-532. PubMed CrossRef
38. Delbello MP, Findling RL, Kushner S, et al. A pilot controlled trial of topiramate for mania in children and adolescents with bipolar disorder. J Am Acad Child Adolesc Psychiatry. 2005;44(6):539-547. PubMed CrossRef
39. Wagner KD, Kowatch RA, Emslie GJ, et al. A double-blind, randomized, placebo-controlled trial of oxcarbazepine in the treatment of bipolar disorder in children and adolescents. Am J Psychiatry. 2006;163(7):1179-1186. PubMed CrossRef
40. Findling RL, Drury SS, Jensen PS, et al; AACAP Committee on Quality Issues. Practice parameter for the use of atypical antipsychotic medications in children and adolescents. J Am Acad Child Adolesc Psychiatry.
41. Haas M, Delbello MP, Pandina G, et al. Risperidone for the treatment of acute mania in children and adolescents with bipolar disorder: a randomized, double-blind, placebo-controlled study. Bipolar Disord. 2009;11(7):687-700. PubMed CrossRef
42. Tohen M, Kryzhanovskaya L, Carlson G, et al. Olanzapine versus placebo in the treatment of adolescents with bipolar mania. Am J Psychiatry. 2007;164(10):1547-1556. PubMed CrossRef
43. Pathak S, Findling RL, Earley WR, et al. Efficacy and safety of quetiapine in children and adolescents with mania associated with bipolar I disorder: a 3-week, double-blind, placebo-controlled trial. J Clin Psychiatry. 2013;74(1):e100-e109. PubMed CrossRef
44. Findling RL, Nyilas M, Forbes RA, et al. Acute treatment of pediatric bipolar I disorder, manic or mixed episode, with aripiprazole: a randomized, double-blind, placebo-controlled study. J Clin Psychiatry. 2009;70(10):1441-1451. PubMed CrossRef
45. Findling RL, Landbloom RL, Szegedi A, et al. Asenapine for the acute treatment of pediatric manic or mixed episode of bipolar I disorder. J Am Acad Child Adolesc Psychiatry. 2015;54(12):1032-1041. PubMed CrossRef
46. Findling RL, CavuÅŸ I, Pappadopulos E, et al. Efficacy, long-term safety, and tolerability of ziprasidone in children and adolescents with bipolar disorder. J Child Adolesc Psychopharmacol. 2013;23(8):545-557. PubMed CrossRef
47. Detke HC, Delbello MP, Landry J, et al. Olanzapine/fluoxetine combination in children and adolescents with bipolar I depression: a randomized, double-blind, placebo-controlled trial. J Am Acad Child Adolesc Psychiatry. 2015;54(3):217-224. PubMed CrossRef
48. DelBello MP, Goldman R, Phillips D, et al. Efficacy and safety of lurasidone in children and adolescents with bipolar I depression: a double-blind, placebo-controlled study. J Am Acad Child Adolesc Psychiatry. 2017;56(12):1015-1025. PubMed CrossRef
49. DelBello MP, Chang K, Welge JA, et al. A double-blind, placebo-controlled pilot study of quetiapine for depressed adolescents with bipolar disorder. Bipolar Disord. 2009;11(5):483-493. PubMed CrossRef
50. Findling RL, Chang K, Robb A, et al. Adjunctive maintenance lamotrigine for pediatric bipolar I disorder: a placebo-controlled, randomized withdrawal study. J Am Acad Child Adolesc Psychiatry. 2015;54(12):1020-1031.e3. PubMed CrossRef
This PDF is free for all visitors!