Because this piece does not have an abstract, we have provided for your benefit the first 3 sentences of the full text.
To the Editor: Lee et al studied the impact of clozapine on the erythroid lineage in a sample of schizophrenic patients and found a high incidence of anemia in the first 2 years following clozapine initiation, with smoking and baseline hemoglobin level shown to be significant protective factors. They concluded that there was a need for further studies of the relationships between schizophrenia, clozapine, and anemia. Following their observations and conclusions, we would like to note the following 2 main points:
First, regarding the known dose-related clozapine toxicity, the presence of a mean plasma clozapine level above the upper limit of the therapeutic range (360-690 ng/mL) among anemic patients should be highlighted.
This work may not be copied, distributed, displayed, published, reproduced, transmitted, modified, posted, sold, licensed, or used for commercial purposes. By downloading this file, you are agreeing to the publisher’s Terms & Conditions.
See reply by Lee and Remington and article by Lee et al
Anemia Among Schizophrenic Patients: Influence of Clozapine and C-Reactive Protein
To the Editor: Lee et al1 studied the impact of clozapine on the erythroid lineage in a sample of schizophrenic patients and found a high incidence of anemia in the first 2 years following clozapine initiation, with smoking and baseline hemoglobin level shown to be significant protective factors. They concluded that there was a need for further studies of the relationships between schizophrenia, clozapine, and anemia. Following their observations and conclusions, we would like to note the following 2 main points:
First, regarding the known dose-related clozapine toxicity, the presence of a mean plasma clozapine level above the upper limit of the therapeutic range (360-690 ng/mL)2 among anemic patients should be highlighted. In fact, the group of anemic patients1 presented a mean value of 771.7 ± 287.1 ng/mL (n = 7), which suggests a potentially toxic outcome, compared with a lower mean value of 575.0 ± 262.8 ng/mL (n = 19) in non-anemic patients, although the difference was not significant because of a lack of sufficient statistical power. In this regard, we know that cytochrome P450 reductase (CYP) 1A2 is the most important route of clozapine metabolism,2 the metabolic activity of which is mediated by smoking, as it is one of most important CYP1A2 inducers. Smoking, which has been shown to have different incidences among anemic and non-anemic patients (22% vs 65%, Z = 3.6; 95% CI, 0.1967-0.6653; P < .001) according to Lee and colleagues’ study,1 is crucial for the presence of toxicity associated with high plasma clozapine levels; further, there is a proven dose-response relation between plasma concentration and the risk of adverse events.3,4 Thus, if Lee et al1 had submitted data on plasma clozapine level and compared smokers with nonsmokers, we would have additional information about the influence of smoking on the plasma levels of clozapine and their toxicity.
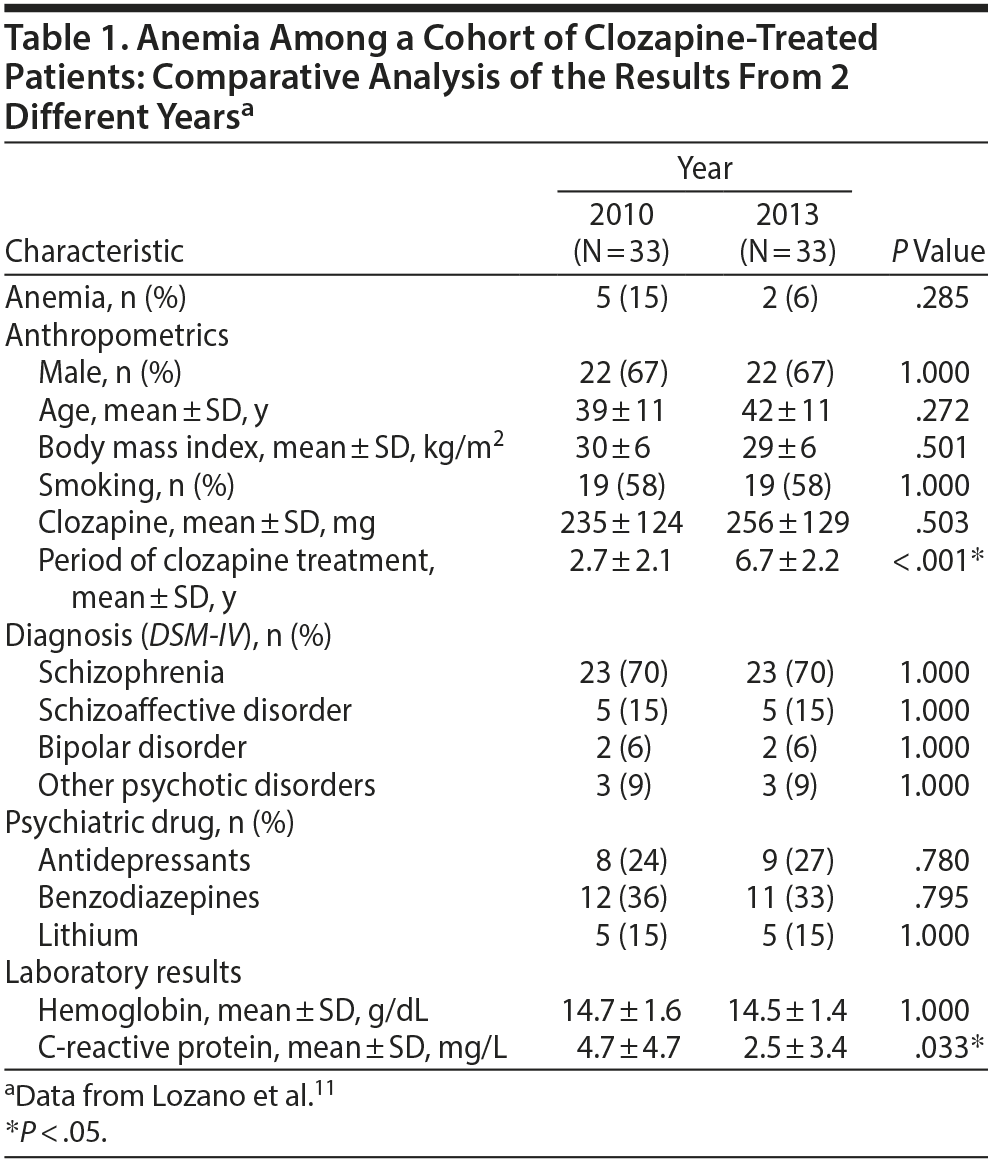
Second, regarding clozapine-related anemia that presents following treatment initiation within the first 2 years, the effect of clozapine on high-sensitivity C-reactive protein (hs-CRP), an acute-phase reactant and marker of inflammation, as a possible confounder for the typing of anemia and, therefore, the attribution of its pathogenesis, should be highlighted. For example, anemia of inflammation is most commonly described as normocytic-normochromic, but it can become microcytic-hypochromic (a typical pattern of iron-deficiency anemia) or resolved in accordance with the development of the inflammatory disorder.5 In fact, we know that clozapine, especially at the beginning, leads to increased hs-CRP unrelated to age, race, or smoking status.6-8 Moreover, hs-CRP level is inversely related to hemoglobin level, which could result in transient anemia through hs-CRP elevation.9,10 In this regard, observations based on post hoc comparative data analysis (2010 vs 2013), from our own previous study,11 showed a decrease in the mean value of hs-CRP (t = 2.1786; 95% CI, 0.183-4.217; P < .05) and anemia prevalence over time (Table 1). Thus, if Lee et al1 had submitted data on hs-CRP among anemic compared with non-anemic patients, we would have additional information about the influence of inflammatory cytokines on clozapine-related anemia.
In conclusion, these data, if supplied, would have provided additional insight into the pathogenesis, diagnosis, and treatment of clozapine-related anemia.
References
1. Lee J, Bies R, Bhaloo A, et al. Clozapine and anemia: a 2-year follow-up study. J Clin Psychiatry. 2015;76(12):1642-1647. PubMed doi:10.4088/JCP.14m09143
2. Olsson E, Edman G, Bertilsson L, et al. Genetic and clinical factors affecting plasma clozapine concentration. Prim Care Companion CNS Disord. 2015;17(1):doi:10.4088/PCC.14m01704 PubMed.
3. Simon V, van Winkel R, De Hert M. Are weight gain and metabolic side effects of atypical antipsychotics dose dependent? a literature review. J Clin Psychiatry. 2009;70(7):1041-1050. PubMed doi:10.4088/JCP.08r04392
4. Melkersson KI, Hulting AL, Brismar KE. Different influences of classical antipsychotics and clozapine on glucose-insulin homeostasis in patients with schizophrenia or related psychoses. J Clin Psychiatry. 1999;60(11):783-791. PubMed doi:10.4088/JCP.v60n1112
5. Cartwright GE, Lauritsen MA, Jones PJ, et al. The anemia of infection, I: hypoferremia, hypercupremia, and alterations in porphyrin metabolism in patients. J Clin Invest. 1946;25(1):65-80. PubMed doi:10.1172/JCI101690
6. Joseph J, Depp C, Martin AS, et al. Associations of high sensitivity C-reactive protein levels in schizophrenia and comparison groups. Schizophr Res. 2015;168(1-2):456-460. PubMed doi:10.1016/j.schres.2015.08.019
7. Hefner G, Shams ME, Unterecker S, et al. Inflammation and psychotropic drugs: the relationship between C-reactive protein and antipsychotic drug levels. Psychopharmacology (Berl). 2015. PubMed doi:10.1007/s00213-015-3976-0
8. Löffler S, Löffler-Ensgraber M, Fehsel K, et al. Clozapine therapy raises serum concentrations of high sensitive C-reactive protein in schizophrenic patients. Int Clin Psychopharmacol. 2010;25(2):101-106. PubMed doi:10.1097/YIC.0b013e32833643fd
9. Breiterman-White R. C-reactive protein and anemia: implications for patients on dialysis. Nephrol Nurs J. 2006;33(5):555-558. PubMed
10. Yang M, Ma N, Fu H, et al. Hematocrit level could reflect inflammatory response and disease activity in patients with systemic lupus erythematosus. Clin Lab. 2015;61(7):801-807. PubMed
11. Lozano R, Mar×n R, Santacruz MJ, et al. Selective immunoglobulin M deficiency among clozapine-treated patients: a nested case-control study. Prim Care Companion CNS Disord. 2015;17(4):doi:10.4088/PCC.15m01782. PubMed
aPharmacy Department, bHematology Department, and cPsychiatry Department, Hospital Real de Nuestra Señora de Gracia, Zaragoza, Spain
Potential conflicts of interest: None.
Funding/support: None.
J Clin Psychiatry 2016;77(4):e467
dx.doi.org/10.4088/JCP.15lr10392
© Copyright 2016 Physicians Postgraduate Press, Inc.
This PDF is free for all visitors!