Sudden Cardiac Death in Users of Second-Generation Antipsychotics
To the Editor: First-generation antipsychotics have been linked to sudden cardiac death (SCD),1,2 but information on the relationship between second-generation antipsychotics (SGAs) and this possible adverse effect is limited. However, the latter association was recently strengthened by a retrospective large cohort study in Medicaid enrollees in Tennessee aged 30 to 74 years.3 If the results of that study are generalizable to other populations, a considerable number of individual case safety reports with this problem would probably be found in large international pharmacovigilance data sets. Moreover, with the use of such data, certain characteristics of the affected subjects could be investigated in more detail.
Method. We reviewed international individual case safety reports of suspected adverse drug reactions (ADRs) from the World Health Organization drug safety database, VigiBase, which contains over 4.5 million records from more than 90 countries (as of March 2009).4 Although the data are heterogeneous, at least with respect to origin (country as well as reporter of the ADR) and content (eg, quality and assessment of causality), they have been used to highlight and support emerging drug safety issues.5-7 We analyzed all cases of SCD during SGA treatment that were identified in VigiBase on January 10, 2008. Obvious duplicates and suicides were excluded. Drugs known to prolong the QT interval were defined as drugs generally accepted by the QT Drug Lists Advisory Board of the Arizona Center for Education and Research on Therapeutics to carry a risk, a possible risk, or a conditional risk of causing torsades de pointes.8 A disproportionality measure, the Information Component (IC), was used to identify if SCD was excessively reported for the various SGAs relative to the overall reporting rate in VigiBase.9,10
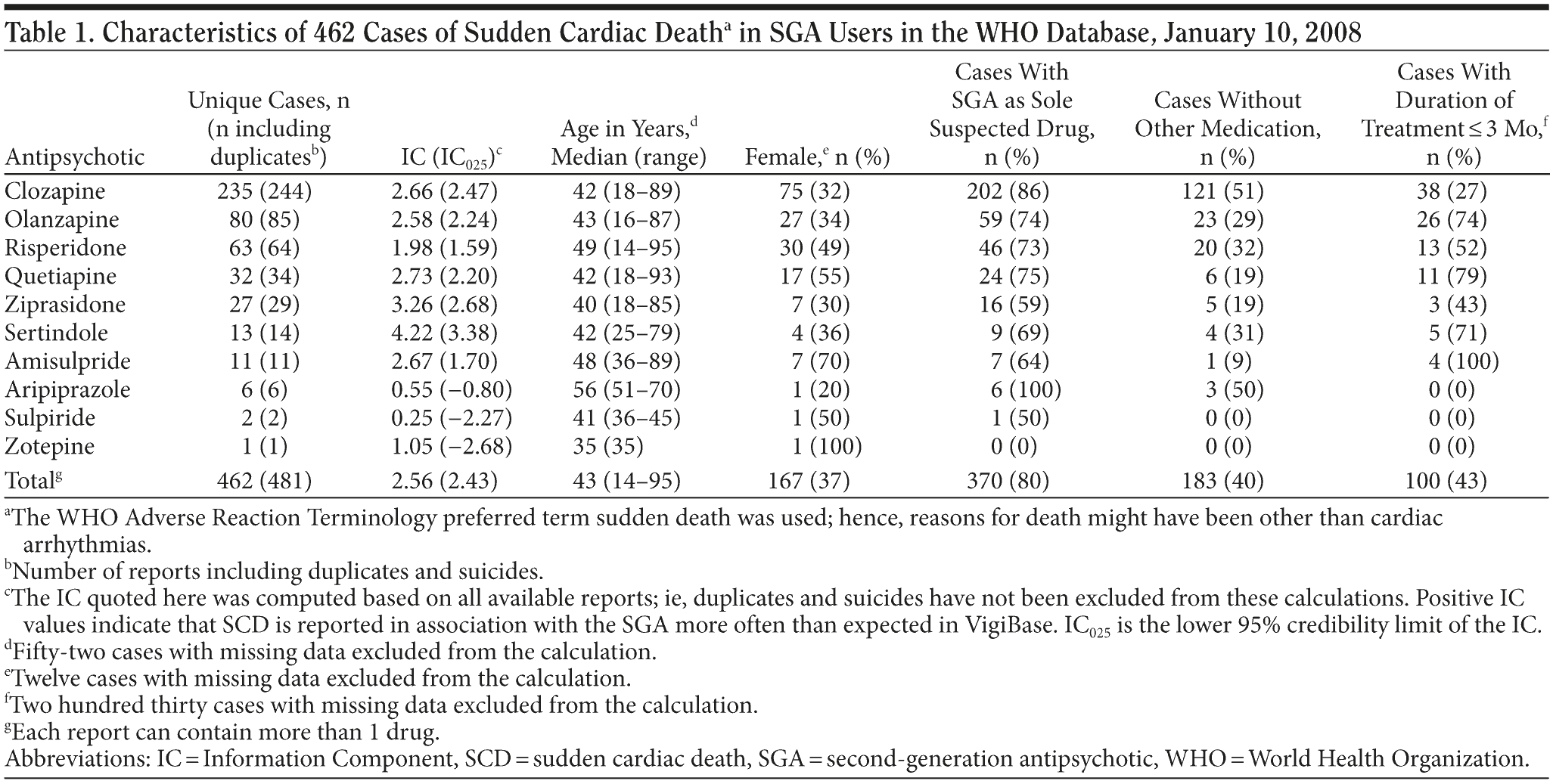
Results. In VigiBase, a total of 462 unique reports of SCD during SGA treatment, from 17 countries, were identified (Table 1). Clozapine was the suspected agent in most reports. Notably, the reports often concerned relatively young patients, the median age being 43 years. In 80% of the reports the SGA was the sole suspect for the reaction, and in 66% of all reports no additional drug known to prolong the QT interval was reported. The duration of treatment was 3 months or less in 43% of the reports. SCD was reported disproportionately more often for SGAs compared to the overall reporting in VigiBase, although the IC value is uncertain for the SGAs with very few reports.
Rigorous monitoring for agranulocytosis during clozapine treatment could lead to increased reporting of other ADRs as well. This might have contributed to the large proportion of reports with sudden cardiac deaths with clozapine as the suspected agent. Other reporting biases, including variable differential underreporting of suspected ADRs,11 probably exist for these data, and comparisons between drugs should therefore be considered with great caution.
In conclusion, these data suggest that SCD in SGA users is likely to be an international problem and may occur early in treatment and in younger patients. More studies are urgently needed to investigate the association further.
References
1. Sicouri S, Antzelevitch C. Sudden cardiac death secondary to antidepressant and antipsychotic drugs. Expert Opin Drug Saf. 2008;7(2):181-194. PubMed doi:10.1517/14740338.7.2.181
2. Davidson M. Risk of cardiovascular disease and sudden death in schizophrenia. J Clin Psychiatry. 2002;63(suppl 9):5-11. PubMed
3. Ray WA, Chung CP, Murray KT, et al. Atypical antipsychotic drugs and the risk of sudden cardiac death. N Engl J Med. 2009;360(3):225-235. doi:10.1056/NEJMoa0806994
4. Lindquist M. VigiBase, the WHO Global ICSR database system: basic facts. Drug Inf J. 2008;49(5):409-419.
5. Bate A, Lindquist M, Orre R, et al. Data-mining analyses of pharmacovigilance signals in relation to relevant comparison drugs. Eur J Clin Pharmacol. 2002;58(7):483-490. PubMed doi:10.1007/s00228-002-0484-z
6. Coulter DM, Bate A, Meyboom RH, et al. Antipsychotic drugs and heart muscle disorder in international pharmacovigilance: data mining study. BMJ. 2001;322(7296):1207-1209. PubMed doi:10.1136/bmj.322.7296.1207
7. Edwards IR, Bate A, Lindquist M. Abacavir and increased risk of myocardial infarction [letter]. Lancet. 2008;372(9641):805. doi:10.1016/S0140-6736(08)61333-1
8. Torsades list, possible torsades list, and conditional torsades list. Arizona CERT Web site. http://www.azcert.org/medical-pros/drug-lists/bycategory.cfm. Accessed October 27, 2009.
9. Bate A, Lindquist M, Edwards IR, et al. A Bayesian neural network method for adverse drug reaction signal generation. Eur J Clin Pharmacol. 1998;54(4):315-321. PubMed doi:10.1007/s002280050466
10. Norén GN, Bate A, Orre R, et al. Extending the methods used to screen the WHO drug safety database towards analysis of complex associations and improved accuracy for rare events. Stat Med. 2006;25(21):3740-3757. PubMed doi:10.1002/sim.2473
11. Hazell L, Shakir SA. Under-reporting of adverse drug reactions: a systematic review. Drug Saf. 2006;29(5):385-396. PubMed doi:10.2165/00002018-200629050-00003
Author affiliations: Sahlgrenska University Hospital, Göteborg (Mr Karlsson and Drs Wallerstedt and Hפgg); Uppsala Monitoring Centre, WHO Collaborating Centre for International Drug Monitoring, Uppsala (Ms Star and Dr Bate); and University Hospital, Linköping (Dr Hפgg), Sweden. Potential conflicts of interest: Ms Star has a limited number of stocks in AstraZeneca, the manufacturer of quetiapine. Mr Karlsson and Drs Wallerstedt, Bate, and Hפgg report no additional financial or other relationships relevant to the subject of this letter. Funding/support: Funded by the Swedish Foundation for Strategic Research, Swedish Research Council Grant 2006-5172, Stockholm, Sweden; and the County Council of ×–stergötland, Linköping, Sweden, grant LIO-10675. Disclaimer: The opinions and conclusions in this letter are not necessarily those of the various centers, nor of the WHO. Previous presentation: Presented as a poster at the 24th International Conference on Pharmacoepidemiology & Therapeutic Risk Management, Copenhagen, Denmark, August 17-20, 2008. Acknowledgment: The authors are indebted to the national centers that contributed data.
doi:10.4088/JCP.09l05262
© Copyright 2009 Physicians Postgraduate Press, Inc.