The Association of Disaster-Related Experiences and Self-Reported Recollections of National Trauma With Posttraumatic Stress Disorder Symptoms Following Hurricane Sandy
To the Editor: Hurricane Sandy struck the New York Metropolitan Area on October 29, 2012, leading to massive property damage and more than 100 casualties. The effect on the infrastructure was severe, with more than 8 million New York Metropolitan Area residents suffering from power outages, accompanied by food shortages and mobility restrictions resulting from the widespread flooding. Previous studies show that exposure to natural disasters increased the risk for psychological distress,1-4 while recollections of these events hindered mental health recovery.5,6 Little is known about the association between recollections of national trauma with posttraumatic stress disorder (PTSD) symptoms in the aftermath of natural disaster.
Method. Following approval by the ethics committee of the School of Social Work at Ariel University, we conducted an online survey using Toluna USA, Inc (us.toluna-group.com) of 1,000 people in states affected by Hurricane Sandy 1 month after the hurricane (response rate = 83.3% of a potential 1,200). We used the same method employed in other medical and psychological studies.7,8
We assessed sociodemographic characteristics: age (mean [SD] = 45.16 [14.30] years), gender (n = 655 women; 65.5%), marital status (n = 606 married; 60.6%), and education (n = 455 having college degree or above; 45.5%). We also assessed disaster-related experiences ("Did you lose personal property or belongings during Hurricane Sandy?" with replies on a dichotomous scale of 0 = no and 1 = yes) and self-report recollections of national trauma ("Since Hurricane Sandy, how often do you think of Hurricane Katrina from 2005?" and "Since Hurricane Sandy, how often do you think of the 9/11 World Trade Center [WTC] terror attack?", with replies to both questions made according to a 5-point Likert Scale ranging from 0 = not at all to 4 = very much). PTSD symptoms were assessed by the Impact of Event Scale Revised (IES-R),9 a 22-item scale including PTSD domains of intrusion, avoidance/numbing, and hyperarousal. Scores range from 0 to 88, with a score of 33 or higher indicating elevated risk of clinical levels of PTSD symptoms (Cronbach α = 0.975).9 This instrument has been used widely in other disasters such as the Haiti earthquake in 20103 and the Fukushima earthquake, tsunami, and nuclear disaster in 2011.4
Logistic regression analysis was conducted for the above factors as independent variables while IES-R score of 33 or higher was the dependent variable entered into the model. SPSS version 19.0 (IBM Corporation, Armonk, New York) was used. A 2-sided P < .05 was used to indicate significance. An a priori test showed that the variance inflation factor ranged from 1.021 to 1.400 and tolerance ranged from 0.714 to 0.979, indicating the absence of multicollinearity.10
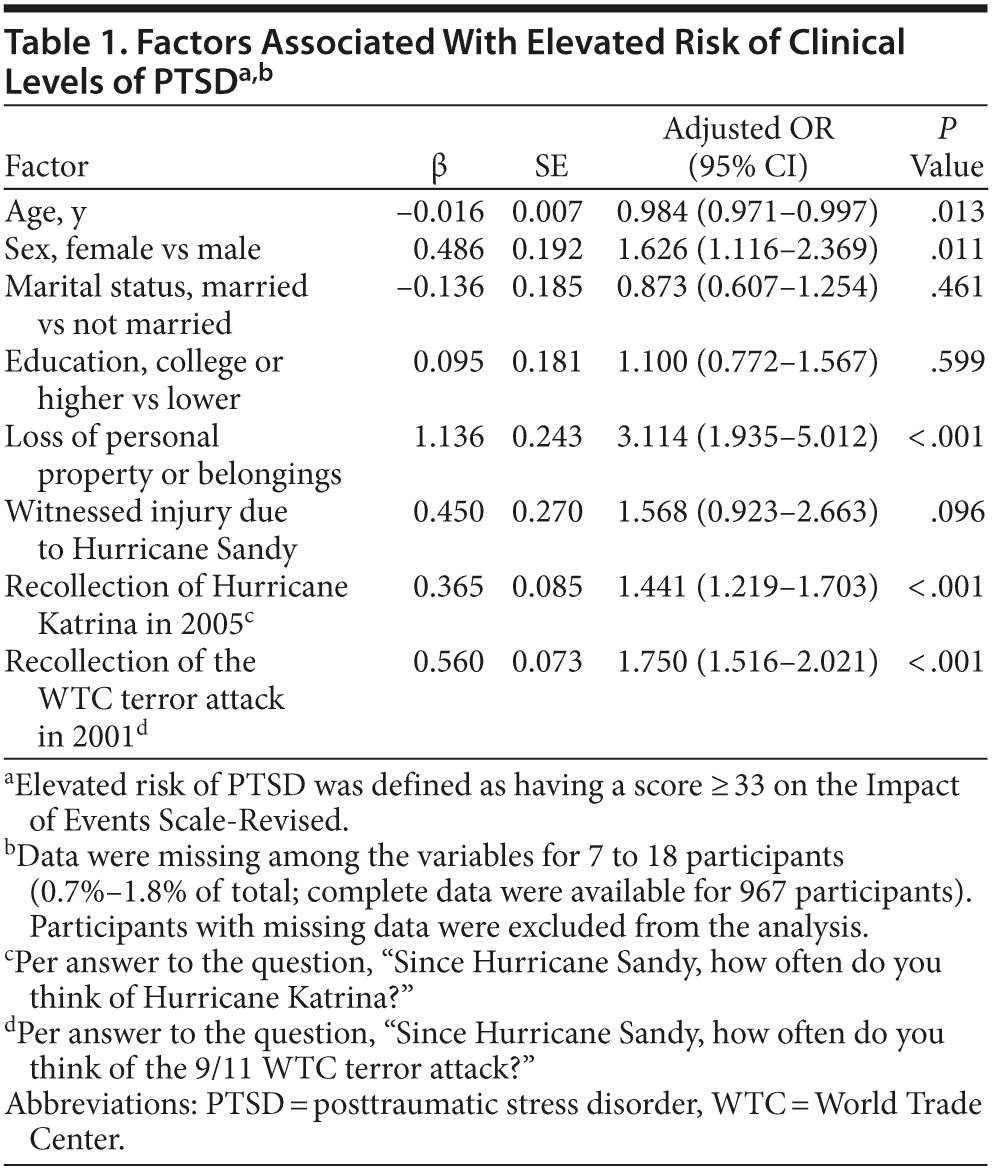
Results. Elevated risk of clinical levels of PTSD symptoms was significantly associated with loss of personal property or belongings (OR = 3.114 [95% CI, 1.935-5.012], P < .001), recollections of Hurricane Katrina (OR = 1.441 [95% CI, 1.219-1.703], P < .001), and recollections of World Trade Center terrorist attacks (OR = 1.750 [95% CI, 1.516-2.021], P < .001). Other significant associations with elevated risk of clinical levels of PTSD were lower age (OR = 0.984 [95% CI, 0.971-0.997], P = .013) and female sex (OR = 1.626 [95% CI, 1.116-2.369], P = .011) (Table 1).
The prevalence of elevated risk of clinical levels of PTSD symptoms (IES-R score: 33) 1 month after Hurricane Sandy was 23.6%. After Hurricane Sandy, a large portion of the participants had recollection of Hurricane Katrina (81.7%) and 9/11 WTC terror attacks (61.4%), whereas only a small portion of the participants reported loss of property or personal belongings (18.4%). These results were similar to other studies pertaining to Hurricane Andrew1 and Hurricane Katrina.2 Expanding past research, recollections of previous major national trauma were associated with exacerbation of mental health.5,6
Several limitations warrant discussion. Our report was cross-sectional with oversampling of women and of people who are more likely to be in a less-affected area and who had access to electricity and communication. We obtained neither baseline measures nor long-term outcomes. PTSD symptoms were measured by a self-report questionnaire, and no comparison group was available.
Recall of past events may potentially prime for future psychological distress following disasters. Clinicians can benefit from attending to preexisting anxieties when identifying those likely to present with higher levels of PTSD symptoms.
References
1. David D, Mellman TA, Mendoza LM, et al. Psychiatric morbidity following Hurricane Andrew. J Trauma Stress. 1996;9(3):607-612. PubMed doi:10.1002/jts.2490090316
2. Galea S, Brewin CR, Gruber M, et al. Exposure to hurricane-related stressors and mental illness after Hurricane Katrina. Arch Gen Psychiatry. 2007;64(12):1427-1434. PubMed doi:10.1001/archpsyc.64.12.1427
3. Ben-Ezra M, Soffer CY. Hospital personnel reactions to Haiti’s earthquake: a preliminary matching study. J Clin Psychiatry. 2010;71(12):1700-1701. PubMed doi:10.4088/JCP.10l06205blu
4. Ben-Ezra M, Palgi Y, Hamama-Raz Y, et al. Subjective assessments of threats and their association to posttraumatic stress disorder symptoms: the case of the 2011 Japan earthquake and nuclear disaster. J Clin Psychiatry. 2013;74(3):280. PubMed doi:10.4088/JCP.12l08055
5. Voelker R. Memories of Katrina continue to hinder mental health recovery in New Orleans. JAMA. 2010;304(8):841-843. PubMed doi:10.1001/jama.2010.1193
6. Shambaugh G, Matthew R, Silver RC, et al. Public perceptions of traumatic events and policy preferences during the George W. Bush administration: a portrait of America in turbulent times. Stud Conflict Terrorism. 2010;33(1):55-91. doi:10.1080/10576100903488410
7. Salsman JM, Lai JS, Hendrie HC, et al. Assessing psychological well-being: self-report instruments for the NIH Toolbox [published online ahead of print June 16, 2013]. Qual Life Res. doi:10.1007/s11136-013-0452-3 PubMed
8. Butt Z, Peipert J, Webster K, et al. General population norms for the functional assessment of cancer therapy-Kidney Symptom Index (FKSI). Cancer. 2013;119(2):429-437. PubMed doi:10.1002/cncr.27688
9. Weiss D, Marmar C. The impact of event scale-revised. In: Wilson J, Keane T, eds. Assessing Psychological Trauma and PTSD. New York, NY: Guilford; 1997.
10. O’ brien RM. A caution regarding rules of thumb for variance inflation factors. Qual Quant. 2007;41(5):673-690. doi:10.1007/s11135-006-9018-6
Author affiliations: School of Social Work, Ariel University, Ariel (Prof Ben-Ezra and Dr Hamama-Raz); Department of Gerontology, Faculty of Social Welfare and Health Sciences, University of Haifa, Haifa (Dr Palgi), Israel; Department of Psychological Medicine, King’s College London, London (Dr Rubin); and School of Social Sciences, Brunel University, Uxbridge (Prof Goodwin), United Kingdom.
Potential conflicts of interest: None reported.
Funding/support: This work was supported by an internal researcher grant from the research authority at Ariel University (No. 803590) awarded to Prof Ben-Ezra.
Role of the sponsor: The funding organization had no role in the design and conduct of the study; in the collection, management, analysis, and interpretation of the data; or in the preparation, review, or approval of the manuscript.
J Clin Psychiatry 2013;74(12):1265-1266 (doi:10.4088/JCP.13l08535).
© Copyright 2013 Physicians Postgraduate Press, Inc.