ABSTRACT
Comorbidity is common with posttraumatic stress disorder, and alcohol use disorder (AUD) is among the most common co-occurring disorders. When viewed through the lens of avoidance behaviors, AUD can shape an individual’s response to distressing trauma reminders by dulling the emotional response and promoting disengagement from the traumatic memory. Over time, this response strengthens posttraumatic distress by reinforcing the belief that traumatic memories and their emotional responses are themselves dangerous and intolerable. In turn, this belief may impede treatment progress. Concurrent trauma-focused therapy and AUD treatment can serve to establish more adaptive coping strategies. Reducing reliance on alcohol for coping while engaging safely and effectively with trauma memories allows the individual to process the memories, build tolerance to emotional distress, and ultimately reframe maladaptive trauma-related beliefs and decrease the intensity of reactions. This case presents concurrent psychopharmacology and cognitive processing therapy for co-occurring posttraumatic stress disorder and AUD. We explore how alcohol use, and emotional avoidance more broadly, become targets for change.
J Clin Psychiatry 2023;84(1):22ct14636
To cite: Zack Ishikawa R, Steere R, Conteh N, et al. Treating PTSD and alcohol use disorder: concurrent cognitive processing therapy and psychopharmacology. J Clin Psychiatry. 2023;84(1):22ct14636.
To share: https://doi.org/10.4088/JCP.22ct14636
© 2022 Physicians Postgraduate Press, Inc.
aDepartment of Psychiatry, Massachusetts General Hospital, Boston, Massachusetts
bCenter for Women’s Mental Health, Department of Psychiatry, Massachusetts General Hospital, Boston, Massachusetts
cWest End Clinic, Department of Psychiatry, Massachusetts General Hospital, Boston, Massachusetts
dCenter for Anxiety and Traumatic Stress Disorders, Massachusetts General Hospital, Boston, Massachusetts
*Corresponding author: Rachel Zack Ishikawa, PhD, MPH, Massachusetts General Hospital, 55 Fruit St, Boston, MA 02131 ([email protected]).
Presented here is a series that highlights the discussion of a complex case by several expert clinicians, faculty members of Massachusetts General Hospital/Harvard Medical School, from distinct fields of study. Cross Talk demonstrates that clinical challenges can often be improved upon by leveraging more, rather than fewer, clinical perspectives.
Avoidance is a required criterion for diagnosing posttraumatic stress disorder (PTSD). Avoidance can include behavioral avoidance of external reminders of trauma, such as people, places, or situations, or it can refer to cognitive or emotional avoidance of trauma-related memories, thoughts, or feelings.1 In addition to cognitive, emotional, or behavioral avoidance, other avoidance behaviors include social withdrawal, self-harm, disordered eating, and substance/alcohol misuse.2
These behaviors have both short- and long-term consequences. In the short term, they serve a protective function, by distancing the individual from distressing trauma reminders. In the long term, however, avoidance behaviors maintain PTSD by reinforcing the perception that trauma-related thoughts and feelings are themselves dangerous.3 In addition, avoidance behaviors can develop into maladaptive strategies for coping with adversity. In the case of substance use and disordered eating, avoidance behaviors may also develop into their own distinct disorders, with both medical and psychological repercussions. Comorbidity of PTSD and alcohol use disorder (AUD) is high, with 30% lifetime prevalence of AUD among civilians with PTSD.4
The following case illustrates the intersection of PTSD and AUD in a patient with multiple childhood traumas and persistent cognitive and emotional avoidance, due to fears of vulnerability and future trauma. The patient received concurrent psychotherapy and psychopharmacology to reduce her reliance on alcohol and her need for emotional and cognitive avoidance, while also reducing PTSD symptoms and developing new, more adaptive resources for engaging and coping with the sequelae of trauma.
Case History and Treatment Course
Dr Rachel Zack Ishikawa and Dr Rachel Steere: Mary is a 54-year-old Black woman, married to a man and mother to a teenage son and adult daughter. She is a college graduate and works as a human resources administrator for a health insurance company. Mary was referred for trauma-focused therapy by her primary care provider. She was evaluated at the Massachusetts General Hospital (MGH) Center for Anxiety and Traumatic Stress Disorders (CATSD) in August 2021 and diagnosed with PTSD and severe AUD. PTSD index traumas were the traumatic deaths of family members and emotional abuse by her mother. Associated symptoms included nightmares and flashbacks; elevated physiological response to trauma cues marked by intense fear, racing heart, sweating, and muscle tightness; avoidance of trauma-related fears; and emotional and cognitive suppression. She also endorsed self-blame for her family members’ deaths as well as for provoking her mother’s abusive behavior toward her, feelings of guilt, persistent negative emotional state, and detachment from others. Lastly, alterations in arousal included hypervigilance around her children’s safety, exaggerated startle response, and self-destructive behavior, specifically alcohol use. Her initial score on the PTSD Checklist for DSM-5 (PCL-5)5 was 44, above the clinical threshold of 33 for PTSD. Mary also endorsed anxiety, anhedonia, hopelessness, insomnia, fatigue, and passive, transient suicidal ideation without plan or intent.
Mary consumed 1 pint of vodka or 1.5 L of wine each night. During brief periods of abstinence from alcohol, she took clonazepam 1 mg nightly, a long-term prescription from her primary care provider, to fall asleep. She endorsed a loss of control around alcohol use, recurrent interpersonal and psychological problems related to drinking, intense cravings, and the development of tolerance to the effects of alcohol. She reported no problems fulfilling her major role obligations at work or at home and denied withdrawal symptoms. She had never received targeted AUD treatment.
Given the 4- to 5-month waitlist for therapy through CATSD, Mary was referred to AUD treatment while she waited for trauma-focused therapy. This included a referral for psychopharmacology and an intensive outpatient program (IOP). She was first seen by psychiatrist Dr Rachel Steere of the MGH West End Clinic (WEC) in August 2021.
August 2021–January 2022
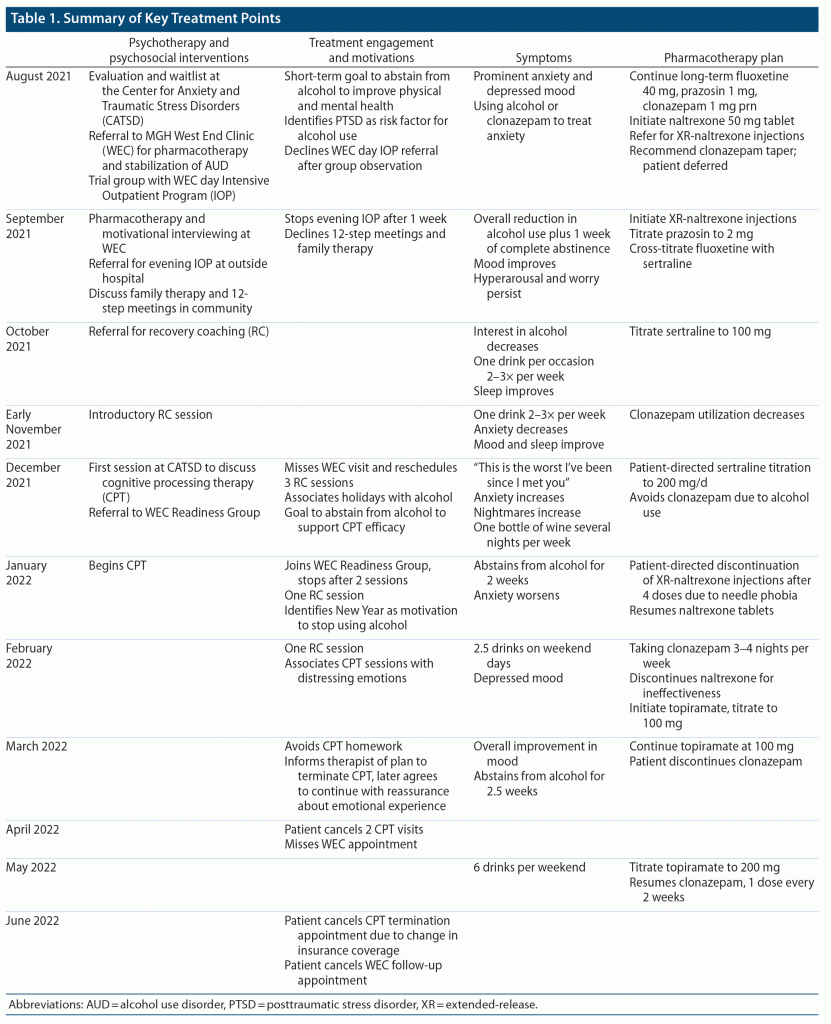
Mary received concurrent treatment for PTSD and AUD from August 2021–March 2022. Table 1 summarizes key treatment points.
At her initial presentation to WEC, Mary’s treatment goal was to reduce her alcohol use from 1 pint of vodka daily to a lower-risk pattern in order to facilitate trauma-focused psychotherapy. She agreed to minimize clonazepam use, which similarly interferes with PTSD treatment. Dr Steere started naltrexone 50 mg daily for AUD, later transitioning to monthly extended-release (XR)-naltrexone injections. Mary’s primary care provider was already prescribing fluoxetine 40 mg daily for a depressive episode occurring several years earlier. Dr Steere added prazosin, titrated to 2 mg nightly, for nightmares.
After 6 weeks, despite a decrease in alcohol use, daytime hyperarousal symptoms and ruminative worry persisted. Fluoxetine was switched to sertraline, a less activating selective serotonin reuptake inhibitor, and this was gradually titrated to 200 mg daily.
Shortly after these changes, Mary reported decreased anxiety symptoms, improvements in sleep, and a reduction in nightmares. She decreased alcohol use to 1 drink 2–3 days per week. She began a virtual IOP and recovery coaching. She took clonazepam only once every 2–3 weeks.
Then, around Thanksgiving, Mary’s anxiety symptoms and nightmares acutely worsened. She worried constantly about her son’s safety and returned to drinking 1 bottle of wine nightly. She shared that she had only attended the IOP for 1 week due to her work schedule. She expressed some guilt about her alcohol use but did not feel ready to change until after the holidays.
January 2022–March 2022
Mary reported complete abstinence from alcohol for the first 2 weeks of January, part of a New Year’s resolution. At that point, she had received 4 doses of XR-naltrexone, but due to a fear of needles, she decided to switch to naltrexone tablets. She also joined a weekly WEC Readiness Group focused on resolving ambivalence and teaching harm reduction strategies. After a few sessions, she stopped attending, citing her work schedule. At her follow-up in February, she reported drinking half a bottle of wine each weekend and was taking clonazepam 3–4 nights per week. She had strong cravings for alcohol despite adherence to naltrexone and was feeling disappointed with its lack of effectiveness. Dr Steere provided information about alternative agents for AUD. Topiramate was chosen for its off-label indications for both AUD and PTSD, with a target dose of 200–300 mg daily.6–8
At the same time, Mary started cognitive processing therapy (CPT) for PTSD with Dr Rachel Zack Ishikawa. CPT, one of the first-line psychotherapies recommended for treating PTSD,9 is a 12- to 15-session, cognitively based treatment that helps patients learn how to challenge and modify unhelpful beliefs related to trauma. The goal of CPT is for patients to create a new understanding and conceptualization of the trauma, thereby reducing the ongoing negative effects of trauma on their current life.
As Mary began to explore trauma-related beliefs, 3 salient themes emerged that would become central to her therapy. The first theme was racial othering. Mary described herself as living between worlds, and not belonging to any of them. She was raised by a young single mother who was professionally successful but began using drugs when Mary was young. Mary lived between her grandmother’s house in Boston and her mother’s house in western Massachusetts. She went to school in the suburbs, through the METCO program, a program for integrating Boston students into neighboring suburban schools. Mary said that she felt like an outsider everywhere, excluded by the neighborhood kids because she went to school in the suburbs and excluded and bullied at school because she was Black.
This history was activated in the present as fear for her teenaged son. Mary feared that as a tall, young, Black man, whom she described as having “effeminate” mannerisms, he would be targeted for both his race and his sexuality. Given legitimate fears about racially motivated violence against young Black men, she felt that her fears for his safety were realistic. Mary relied on frequent check-ins and phone tracking to reassure herself. Their relationship had become strained as a result. Mary worked to parse out the difference between fears related to her prior traumas and fears resulting from current, chronic racial trauma and explored how she might distinguish between realistic precautions and excessive and counterproductive safety behaviors.
The second theme was that of emotional abuse and neglect. Her mother’s volatile and neglectful treatment of Mary while she was using drugs caused Mary to feel unloved and unwanted. Two examples stood out as particularly distressing. On one occasion, when she was between 8–10 years old, her mother forced her to stay in her room for hours because drug activity was going on in the apartment. When she told her mother that she was hungry, her mother threw a bag full of moldy bread and cockroaches onto Mary’s bed, causing the roaches to stream out of the bag and onto her blankets. She described feeling pure horror, and throughout life has had an insect phobia.
On another occasion, she was out with friends and arrived home late. She reported that her mother refused to let her into the apartment. She had to spend the night on the doormat and get on the school bus the next day in the same clothes she had worn the day before. This incident evoked intense shame, confusion, and self-blame about what had made her deserving of such treatment.
The third theme was that of traumatic loss and Mary’s belief in her own complicity in the deaths of loved ones. At age 11, she dreamt that her grandfather was in a casket and then learned the next day that he had died, following a physical assault. At 14, Mary delayed coming home to meet her mother for the drive back to western Massachusetts. Her mother drove back without her, and the next day Mary learned that she had been killed in a car accident, after being struck by a drunk driver. When Mary was 35, she found herself admiring her grandmother’s bracelet, and wishing she could have it. The next day, her grandmother had a stroke. She was admitted to a nursing home and died within a year. Mary believed that she willed these deaths into existence, and that thinking about future tragedy would cause it to occur.
Despite the adversity she endured, she habitually minimized its significance and criticized her reactions as excessive, saying, “These things are trivial.” As a consequence, she believed she should be able to manage her problems herself, and she felt undeserving of therapy. This disparagement, in turn, eventually led to therapy ambivalence and avoidance.
In the first month of therapy, Mary was engaged in sessions and thoughtfully completed home practice. However, at session 5, in February, she said that said she had been dreading that day’s session. While she said that she had been feeling “great,” she reported she had not done her homework due to elevated emotional distress while working on the worksheets. She had not wanted to spoil her positive mood by refocusing on trauma.
Many patients hesitate at this point in trauma treatment as they confront long-avoided beliefs and emotions. Mary believed that the intensity of CPT could jeopardize the tenuous positive mood she was experiencing. Eventually, she responded to reassurance that her fear was an understandable response to the perception of danger in discussing trauma-related content, and she was able to proceed. This discussion highlighted Mary’s impulse to avoid, as well as her receptivity to validation and her willingness to reconsider avoidance as a coping strategy.
This was the beginning of a pattern of vacillation for Mary. She would first become apprehensive about continuing treatment, either because she was feeling “amazing” and did not see a need to focus on painful memories or because she was overwhelmed by intolerable emotions of sadness, remorse, or fear. Examining her apprehension helped her to feel reassured and supported, and she would then engage thoughtfully with treatment for another several sessions before re-entering the cycle.
For example, in March, after Dr Zack Ishikawa had been away on vacation, Mary said she wanted to stop therapy. She agreed to meet to discuss her decision and for closure. In that session, she said she was feeling considerably better since reducing her alcohol use and that family responsibilities required her full attention. She noted, however, that her husband expressed concern that her decision was driven by avoidance. In discussing this possibility, Mary responded with surprise at hearing that intense emotional responses to trauma are not only expected but acceptable and reasonable. She had never considered that her unwanted emotions not only made sense but were encouraged in treatment. To decrease the intensity of these emotions required engaging with them and with the beliefs that gave rise to them. Ultimately, Mary acknowledged both the pain and the value in continuing to meet, and she committed to proceeding with treatment.
Current Status
Mary’s vacillation in treatment could be understood as a reaction to her fears of confronting the pain of past trauma and of the emotional intensity it elicited. Both alcohol and treatment disengagement became effective ways to block the unwanted emotions. At these times, she would adamantly maintain that she could cope by just pushing through and blocking difficult thoughts. She would say she felt “amazing” or “fantastic.” However, she would eventually recognize the inadequacy of this strategy.
Although CPT is a cognitively based treatment, repeated re-engagement with treatment functioned as an exposure to her emotions. As she began to face and build tolerance to the distress, she recognized that her coping capacity was greater than she had believed. By the completion of CPT, in May 2022, Mary made strides in reducing hypervigilance and self-blame and in increasing flexibility of thinking and engagement with positive emotions.
For example, she came to recognize that constant vigilance about her son both strained their relationship and maintained her fear, rather than relieving it. She no longer checked on him as frequently or demanded that he check in with her. This has led to greater harmony in their relationship. She has reduced all-or-nothing thinking, by simultaneously acknowledging the role of drugs in her mother’s behavior as well as the suffering she endured as a result. She can experience compassion for both herself and her mother, and she can allow herself to feel grief at what she lost. Finally, she acknowledged that the family deaths were not her fault. She regards the perception that she can predict death as a strategy to perceive control where, as a child, chaos was so pervasive.
Overall, Mary reported less worry about the future, less rumination on the past, and more time enjoying family and friends. She remarked, “I never knew I could just feel normal, but I really do.” Her posttreatment PCL-5 score was 8. She also reported a lower level of alcohol use, at 2–3 drinks per week.
This progress appears to be significant, but we remain concerned that avoidance and symptom minimization may continue to limit her ability to benefit fully from treatment. Mary twice no-showed for her final session with Dr Zack Ishikawa, eventually saying she had lost insurance coverage with a job change and could not meet. Regarding her alcohol use, Dr Steere believes that Mary’s eagerness to demonstrate a “correct” response to medication may in fact have contributed to disappointment with medication effectiveness later in treatment. Indeed, after an initial robust response to topiramate 50 mg twice daily, Mary eventually reached a dose of 200 mg daily after strong cravings reemerged, and she returned to 6 drinks over the course of each weekend. As of her last appointment with Dr Steere in May 2022, Mary continued her pattern of 6 drinks each weekend, higher than she reported in therapy. Mary also failed to reschedule a subsequent missed session with Dr Steere.
Mary’s vacillating course of therapy has demonstrated how powerful the pull of avoidance can be, and how persuasive the belief that the only viable option to survival is forging ahead while denying posttraumatic distress. At the same time, she demonstrated a remarkable willingness to examine her enactments of traumatic avoidance. In risking vulnerability—with treatment, her relationship with her providers, and the future—she has acknowledged another, more rewarding path forward. This path remains precarious for her, however, and it is our hope that the benefits of engagement ultimately prove more compelling than the relentlessness of avoidance.
Multicultural Perspective
Dr Nkechi Conteh
When delivering therapy in a multicultural context, an awareness of the impact and implications of intergenerational trauma and environmental trauma is essential. Accordingly, this includes being mindful of the possibility that due to past and current discrimination, the patient may subconsciously attempt to (1) educate the psychotherapist on their cultural norms and context or (2) present their best self instead of their authentic self so as to portray their culture or race in the best possible light to protect against further bias. Though well-intentioned, such situations may prevent the development of the necessary milieu in which growth can occur and derail the therapeutic experience.
In the example of Mary, one can observe evidence of intergenerational trauma impacting her self-identity. From an early age, she was encouraged to associate with a specific culture or class of persons. The impact of being molded to crave experiences that may not be authentic to her culture and to put her best foot forward always is reflected in her consistent use of positive adjectives to describe her mood and her inability to attend appointments when she cannot present a self that is less than perfect. As such, it behooves the therapist to learn about the patient’s background/culture from sources other than the patient and to become conversant with these aspects, including religious views and societal expectations, in a nonjudgmental way.
Alleviating mistrust should be another primary goal. Mary’s exposure to the frailty of relationships so early in life combined with the historical and present racial trauma makes this of paramount importance. One should remain mindful of nonverbal cues (expressed on both sides) and understand cultural idioms while abstaining from the liberal use of such phrases. If these phrases are to be used for any reason, permission should always be sought. Another way to ameliorate mistrust is to avoid a “one-size-fits-all approach” and remain aware that patients of the same race may have vastly different experiences or interpretations. Radical honesty about one’s knowledge or lack thereof should be employed when necessary but without placing undue burden on the patient or redirecting the focus of therapy from the patient to the therapist. Overidentification, sometimes in an attempt to build rapport, may also perpetuate mistrust and come across as extremely invalidating of the patient’s experience of racially charged encounters.
Previous encounters with discrimination may also prompt the patient to minimize traumatic experiences as a defense mechanism against further bias. This can be witnessed in Mary’s apparent trivialization of traumatic incidents. There may be a subliminal desire to subscribe to harmful cultural tropes such as the “strong Black woman” stereotype. As such, one must avoid premature validation or overemphasis on resilience as these approaches may have the unintended consequences of positively reinforcing inauthenticity or harmful practices.
Psychodynamic Perspective
Dr Margaret A. Cramer
Mary’s internal life includes a number of unconscious fantasies, a reaction formation, an unconscious identification, and disavowed aggression and grief. She expresses some of her ambivalence about recovery when she asks her doctors to adopt her “nothing to see here” stance, even as she continues to relapse. From a dynamic viewpoint, we know that women often report first use or first use to intoxication in the aftermath of physically or sexually abusive events, so I recommend learning more about the specific circumstances in which Mary first used alcohol. In hearing the story of the first encounter with of the drug of choice, patients often suddenly flush, eyes glow, and voices soften. This is the story of finding the love of their lives, the maternal object that never abandons, abuses, or disappoints and never requires vulnerability to another. Alcoholics often fear for the integrity of their own minds and worry that feelings will make them crazy, so the prospect of acknowledging and expressing them can feel deeply threatening. It is not surprising then that Mary has struggled so mightily to string together even a few weeks of sobriety. It is not just that “these things are trivial,” as she says, but more that these things must be trivial, because if they were not, they would overwhelm with the threat of psychic disorganization.
If “bad thoughts make bad things happen,” then Mary’s positivity can keep people alive and safe and, in a powerful reaction formation, keep her children safe from her own disavowed rage. There is an unconscious identification with the mother here and perhaps the father. Scratch the surface, Mary fears, and you will find her abusive and neglectful mother or abandoning father. The efforts to have more for the self are thus abandoned time and again because the despised child that lives within is unworthy of care.
I recommend a focus on increasing Mary’s tolerance for painful and forbidden affects. The discovery that not all anger is murderous, and all sadness overwhelming, can reduce the central anxiety that keeps her imprisoned in addiction and trauma. Regarding termination, I suggest an active termination phase of treatment that can help Mary have a new experience of loss, one in which goodbye is not a separation catastrophe. This can stand in stark contrast to the traumatic losses of the past. If Mary can learn that not every goodbye is a tragic one then she may be on her way to being able to be sad and angry without the belief that a world has to be shattered in the bargain.
Substance Use and Psychopharmacology Perspectives
Dr Vinod Rao
The clinicians’ discussion demonstrates that this patient meets sufficient criteria for a substance use disorder.10 But, in a patient with such a history of impoverished attachments who may cope in multiple maladaptive ways, why does alcohol use merit such focus?
First, the dynamics may be more complicated than simply alcohol’s role in “self-medicating” symptoms of trauma.11 Many patients describe evolving explanations of their alcohol use over time. What begins as a form of coping may turn into a behavioral habit or may develop into physical dependence.12 As such, interventions targeting the “underlying cause” may no longer impact the habitual drinking. Moreover, there has existed concern in the field that use of substances may interfere with psychotherapies to target trauma13 or may make negative consequences from the therapy more likely.14 Although few studies have specifically examined the role of co-occurring alcohol use during therapy, there exist some data arguing that drinking may be a risk factor for dropout from prolonged exposure therapy.15 It is worth noting that, like alcohol, benzodiazepines potentiate inhibitory activity at GABAA receptors, and benzodiazepines have been identified as problematic in patients with recent or remote experiences of trauma.16
Regarding pharmacology for AUD, topiramate is a sensible choice to target alcohol use. Topiramate has multiple pharmacologic effects, including boosting inhibitory activity through allosteric modulation of GABAA receptors, while diminishing excitatory activity through antagonism of AMPA and kainate glutamatergic receptors.17 Two clinical trials have argued that topiramate’s efficacy is noninferior to the FDA-approved medication naltrexone, at target doses of 200 mg18 or 300 mg19 total daily. For this patient, although she described a remarkable benefit at small doses, this may represent placebo effect, and it was appropriate to continue titration toward at least 200 mg.
As a prescriber, I have a limited number of arrows in my pharmacologic quiver. But there are myriad opportunities to encourage cultivation of what is called recovery capital—the social, environmental, psychological, and financial resources that help people achieve and maintain their recovery goals and build a fulfilling life.20 Recovery capital can include, for example, peer support meetings, seeking employment, housing, connecting with family, and volunteering. While it could prove quite helpful for this patient to pursue, say, a dialectical behavior therapy (DBT) skills group, I would encourage any endeavor the patient chooses that would grow her recovery capital.
Cognitive-Behavioral Therapy Perspective
Dr Susan Sprich
As a practitioner of cognitive-behavioral therapy (CBT), one of the first things that sprang to my mind when hearing about this case was the concept of apparent competence, which is drawn from DBT. DBT was created by Marsha Linehan in 199321 and is considered a “third wave” CBT treatment. Apparent competence refers to a tendency for patients to seem more capable, emotionally put together, and competent than they really are. Because they seem to be okay, others do not realize how much they are suffering and how much help they need. I think it would be helpful to describe the concept of apparent competence to the patient and ask her if she thinks that this might apply to her. If so, the patient and therapist can have a shared language to use to describe what is happening in different clinical interactions.
It is important to encourage the patient to continue working on tolerating uncertainty as uncertainty is an integral part of life. To use another DBT term, it is effective when we “radically accept” uncertainty. I think there is a way to validate the patient’s very real concerns about her son’s safety and point out that there is no way to guarantee anyone’s safety with 100% certainty at any time. As parents, we try to teach our children behaviors that will keep them safe, and it seems that she has done this to the best of her ability. Pointing out that the reassurance-seeking behaviors in which the patient was engaging were counterproductive and not actually contributing to the son’s safety was on target. I might even go a step further and draw a diagram illustrating the relationship between feeling anxious, engaging in a reassurance-seeking behavior (calling or texting son), and anxiety decreasing.
When thinking about how to conduct exposure and response prevention (focusing on reducing behaviors that Mary uses to lessen feelings of uncertainty), there is a delicate balance between wanting to respect the patient’s desire to move slowly and needing to send the message that the therapist does not believe that there is a causal relationship between the patient having thoughts about death and family members becoming ill and/or dying. Of course, we can never force patients to do exposure exercises if they don’t want to do them, but if the therapist agrees that exposure exercises should not be conducted because they are too “dangerous,” we risk validating the idea that thoughts can cause people to die.
My impression is that CBT tools have already been of help to this patient, and my hope is that CBT and DBT will provide additional tools that the patient can use to help her cope with her symptoms.
Integrative Discussion
Dr Jonah N. Cohen
With current challenges around access to care, treatment in academic psychiatry departments like Mass General’s must be shorter-term. However, this sometimes poses a challenge when clinical presentations are more complex and are characterized by significant symptoms and/or comorbidities. In such cases, I tend to think about an integrative treatment that is symptom-focused but informed by unconscious, characterological, and sociocultural dynamics. Drs Zack Ishikawa and Steere present the case of Mary and the treatment of co-occurring trauma symptoms and alcohol misuse.
Dr Cramer discusses Mary’s relationship to her painful emotions, her unconscious fears, and her relationship to alcohol. Like Dr Cramer, I believe Mary’s inner world might be explained by two interrelated themes: (1) difficulty managing emotional experience and (2) a tendency to experience self, others, and the world in a dichotomous (ie, good/bad) manner. I suspect that Mary’s emotions feel threatening in their capacity to engulf her. As a result, feelings such as guilt, fear, anger, and shame must be avoided, through either alcohol or the minimization of experience. Mary finds herself caught in an unending back-and-forth between compulsive avoidance of overwhelming internal experiences and external traumatic reminders on the one hand and the compulsive urge toward alcohol and minimization on the other. And yet, how might Mary come to learn to better tolerate the emotions that threaten the integrity of her internal world? How does she come to face the racial trauma, traumatic loss, and unfathomable abuse and neglect that threaten her basic trust of others and the world? And how does Mary do this without the need to minimize, turn toward alcohol, or move away from treatment and those who want to help her?
Drs Rao, Conteh, and Sprich provide helpful ideas that address the intrapsychic challenges Dr Cramer identifies. Dr Rao discusses pharmacologic options that might assist in treating Mary’s substance use disorder. Dr Rao also discusses the idea of recovery capital, resources Mary might leverage in supporting her journey. Through peer support, connecting with family, and volunteering, Mary might make relationships that challenge her interpersonal schemas of mistrust. Relatedly, Dr Conteh discusses the crucial role of a multiculturally responsive therapeutic approach. Dr Conteh suggests how learning about Mary’s background and being attuned to the particulars of Mary’s experience rather than using a one-size-fits-all approach may help earn Mary’s trust over time, a potentially significant therapeutic achievement given Mary’s early life experiences. Finally, Dr Sprich identifies Mary’s difficulties tolerating uncertainty and suggests that exposure and response prevention might be a useful intervention. By challenging her feelings that bad things will happen if she is not vigilant, Mary might learn to better tolerate her anxiety and fears around hurting others, eventually increasing her sense of mastery over her emotional world. Overall, effective treatment, particularly in shorter-term care models, requires a team-based approach that puts aside theoretical allegiance in favor of pragmatic clinical care that considers both symptoms and their intrapsychic and sociocultural underpinnings. We owe Mary and Drs Zack Ishikawa and Steere a debt of gratitude for sharing their work with us.
Submitted: August 16, 2022; accepted October 3, 2022.
Published online: November 9, 2022.
Relevant financial relationships: Dr Sprich receives royalties from Springer and Oxford University Press and honoraria from the Association for Behavioral and Cognitive Therapies. Dr Cohen is a board member of the Endowment for the Advancement of Psychotherapy at Massachusetts General Hospital. All other authors report no disclosures/conflicts of interest.
Funding/support: Cross Talk is financially supported by the Endowment for the Advancement of Psychotherapy at Massachusetts General Hospital.
Role of the sponsor: The funding agency had no role in the preparation, review, or approval of the manuscript or the decision to submit the manuscript for publication.
Statement of de-identification and consent: The patient featured in this case provided written consent to have her clinical case history published. The patient’s name has been changed to protect confidentiality.
Clinical Points
- Concurrent trauma-focused treatment and AUD treatment enables positive behavior change while targeting the etiology of alcohol use and the development of alternative adaptive beliefs and coping strategies.
- Recovery from both PTSD and AUD requires the ability to engage with and tolerate distressing emotions. This can be an intensely fear-provoking undertaking for many patients, and progress is usually not linear.
- Pharmacologic agents are important and underutilized tools for the treatment of alcohol use disorder, but ambivalence about medications is common and expected.
- Collaborative decision-making with patients can foster autonomy and engagement in care. This may be especially important for patients undergoing trauma-focused psychotherapy.
References (21)

- American Psychiatric Association. Diagnostic and Statistical Manual of Mental Disorders. Fifth Edition. American Psychiatric Association; 2013. doi:10.1176/appi.books.9780890425596.
- Resick PA, Monson CM, Chard KM. Cognitive Processing Therapy for PTSD: A Comprehensive Manual. Guilford Press; 2017.
- Hawn SE, Cusack SE, Amstadter AB. A systematic review of the self-medication hypothesis in the context of posttraumatic stress disorder and comorbid problematic alcohol use. J Trauma Stress. 2020;33(5):699–708. PubMed CrossRef
- Blanco C, Xu Y, Brady K, et al. Comorbidity of posttraumatic stress disorder with alcohol dependence among US adults: results from National Epidemiological Survey on Alcohol and Related Conditions. Drug Alcohol Depend. 2013;132(3):630–638. PubMed CrossRef
- Weathers FW, Litz BT, Keane TM, et al. The PTSD Checklist for DSM-5 (PCL-5). National Center for PTSD. Published 2013. https://www.ptsd.va.gov/professional/assessment/adult-sr/ptsd-checklist.asp
- Batki SL, Pennington DL, Lasher B, et al. Topiramate treatment of alcohol use disorder in veterans with posttraumatic stress disorder: a randomized controlled pilot trial. Alcohol Clin Exp Res. 2014;38(8):2169–2177. PubMed CrossRef
- de Moraes Costa G, Zanatta FB, Ziegelmann PK, et al. Pharmacological treatments for adults with post-traumatic stress disorder: a network meta-analysis of comparative efficacy and acceptability. J Psychiatr Res. 2020;130:412–420. PubMed CrossRef
- Jonas DE, Amick HR, Feltner C, et al. Pharmacotherapy for adults with alcohol use disorders in outpatient settings: a systematic review and meta-analysis. JAMA. 2014;311(18):1889–1900. PubMed CrossRef
- American Psychological Association. Clinical Practice Guideline for the Treatment of Posttraumatic Stress Disorder (PTSD) in Adults (2017). American Psychological Association; 2017. doi:10.1037/e501872017-001.
- American Psychiatric Association, American Psychiatric Association, DSM-5 Task Force. Diagnostic and Statistical Manual of Mental Disorders: DSM-5. American Psychiatric Association; 2013.
- Hawn SE, Cusack SE, Amstadter AB. A systematic review of the self-medication hypothesis in the context of posttraumatic stress disorder and comorbid problematic alcohol use. J Trauma Stress. 2020;33(5):699–708. PubMed CrossRef
- Wise RA, Koob GF. The development and maintenance of drug addiction. Neuropsychopharmacology. 2014;39(2):254–262. PubMed CrossRef
- American Psychological Association. Trauma and Substance Abuse: Causes, Consequences, and Treatment of Comorbid Disorders. American Psychological Association; 2003:315. doi:10.1037/10460-000.
- Killeen TK, Back SE, Brady KT. The use of exposure-based treatment among individuals with PTSD and co-occurring substance use disorders: clinical considerations. J Dual Diagn. 2011;7(4):194–206. PubMed CrossRef
- van Minnen A, Arntz A, Keijsers GPJ. Prolonged exposure in patients with chronic PTSD: predictors of treatment outcome and dropout. Behav Res Ther. 2002;40(4):439–457. PubMed CrossRef
- Guina J, Rossetter SR, DeRhode BJ, et al. Benzodiazepines for PTSD: a systematic review and meta-analysis. J Psychiatr Pract. 2015;21(4):281–303. PubMed CrossRef
- Arnone D. Review of the use of topiramate for treatment of psychiatric disorders. Ann Gen Psychiatry. 2005;4(1):5. PubMed CrossRef
- Flórez G, Saiz PA, García-Portilla P, et al. Topiramate for the treatment of alcohol dependence: comparison with naltrexone. Eur Addict Res. 2011;17(1):29–36. PubMed CrossRef
- Baltieri DA, Daró FR, Ribeiro PL, et al. Comparing topiramate with naltrexone in the treatment of alcohol dependence. Addiction. 2008;103(12):2035–2044. PubMed CrossRef
- Granfield R, Cloud W. Social context and “natural recovery”: the role of social capital in the resolution of drug-associated problems. Subst Use Misuse. 2001;36(11):1543–1570. PubMed CrossRef
- Linehan MM. Cognitive-Behavioral Treatment of Borderline Personality Disorder. Guilford Press; 1993.
This PDF is free for all visitors!