Recent reports indicate that the current coronavirus disease 2019 (COVID-19) pandemic is generating substantial increases in the global burden of depression, anxiety, and acute stress disorders.1,2 Potential explanations include fear of contagion, grief for the death of loved ones, social isolation due to confinement measures, and stress due to negative economic consequences in both the short and long terms, among others. One major concern is that this unprecedented health and social crisis will also bring about an increase in the incidence of suicidal behaviors.2-4
The emergency department (ED) is paramount for suicide prevention efforts: most suicidal crises and suicide attempts are evaluated and treated in the ED. Moreover, as up to 50% of suicidal patients experience barriers to follow-up care and disengage from outpatient mental health services,5 the ED often constitutes the only window of opportunity for individual-level suicide prevention.
Methods
We assessed the impact of the COVID-19 outbreak on trends in weekly all-cause psychiatric ED visits and ED visits due to suicidal ideation or suicide attempt (defined as any self-injurious act with at least some intent to die), using triage data from the electronic health care records of a major general hospital in Madrid, Spain (one of the global epicenters of the pandemic), between November 2018 and April 2020. We conducted an interrupted time-series analysis and compared trends before and after the day of the first confirmed COVID-19 case at the ED. Our models used an AR(1) correlation matrix to account for autocorrelated data, and we added robust standard errors. All analyses were conducted using the itsa command with the prais option in Stata v.15 for PC (College Station, Texas; StataCorp; 2017).
Results
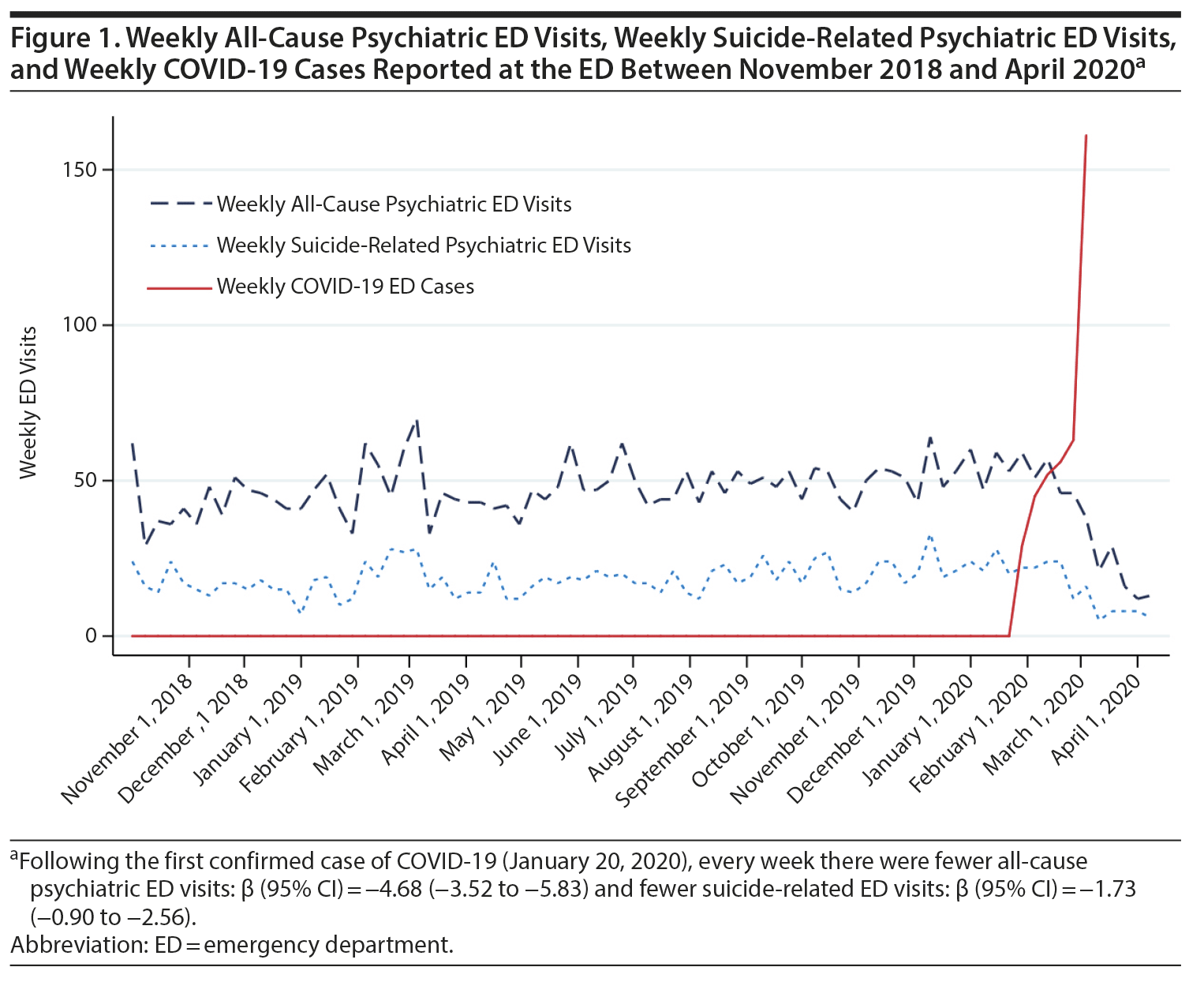
Figure 1 represents the weekly counts of suicide-related and all-cause psychiatric emergency visits, as well as weekly counts of COVID-19 confirmed cases, reported by the ED over the study period. According to our interrupted time-series analysis, every week after the first confirmed case of COVID-19 there were fewer suicide-related ED visits (β = −1.73; 95% confidence interval [CI] = −0.90, −2.56) and fewer all-cause psychiatric ED visits (β = −4.68; 95% CI = −3.52, −5.83).
Discussion
These data suggest that suicide-related ED visits have decreased in Madrid, Spain, during the COVID-19 outbreak. We believe that 2 potential explanations could be considered: (1) there has been a real reduction in suicidal ideation and suicide attempts, or (2) suicidal ideation and suicide attempts have remained unchanged or increased, but patients are not presenting to the ED during suicidal crises. Given that all-cause psychiatric emergencies have also decreased even though most scientific reports indicate that the burden of mental disorders is probably on the rise,1 the second possibility seems more likely. In fact, suicide risk reportedly increased during the 2003 severe acute respiratory syndrome (SARS) epidemic.6
Regardless of the specific reasons underlying patients’ avoidance of the ED during suicidal crises (fear of contagion, lockdown measures, etc), this phenomenon poses a major public health challenge in terms of access to care, especially as a large proportion of suicidal patients receive prevention interventions only during ED visits. Psychiatry departments should place strong emphasis on monitoring patients’ access to emergency care and implementing alternative outreach strategies. For instance, repeated telephone contacts can lower suicide risk because they reduce the sense of social isolation, enhance adherence to treatment, and allow for repeated assessments of immediate suicide risk.7 Also, several evidence-based suicide prevention strategies such as the Safety Planning Intervention8 can be performed on the telephone. The effect of the COVID-19 pandemic on health care systems will be far-reaching and long-lasting, and it is imperative to develop and scale-up strategies that minimize its impact on mental health and suicide risk.
Received: April 21, 2020.
Published online: September 1, 2020.
Potential conflicts of interest: None.
Funding/support: This project was partially funded by a personal training grant awarded by the “La Caixa” Foundation (Dr Mart×nez-Alés; grant number LCF/BQ/AA17/11610021).
Role of the sponsor: “La Caixa” Foundation had no role in any aspect related to the conduct of the study.
REFERENCES
1.Liu S, Yang L, Zhang C, et al. Online mental health services in China during the COVID-19 outbreak. Lancet Psychiatry. 2020;7(4):e17-e18. PubMed CrossRef
2.Courtet P, Olié E, Debien C, et al. Keep socially (but not physically) connected and carry on: preventing suicide in the age of COVID-19. J Clin Psychiatry. 2020;81(3):20com13370. PubMed CrossRef
3.Reger MA, Stanley IH, Joiner TE. Suicide mortality and coronavirus disease 2019: a perfect storm? JAMA Psychiatry. 2020. PubMed CrossRef
4.Gunnell D, Appleby L, Arensman E, et alCOVID-19 Suicide Prevention Research Collaboration. Suicide risk and prevention during the COVID-19 pandemic. Lancet Psychiatry. 2020;7(6):468-471. PubMed CrossRef
5.Lizardi D, Stanley B. Treatment engagement: a neglected aspect in the psychiatric care of suicidal patients. Psychiatr Serv. 2010;61(12):1183-1191. PubMed CrossRef
6.Cheung YT, Chau PH, Yip PS. A revisit on older adults suicides and severe acute respiratory syndrome (SARS) epidemic in Hong Kong. Int J Geriatr Psychiatry. 2008;23(12):1231-1238. PubMed CrossRef
7.Vaiva G, Vaiva G, Ducrocq F, et al. Effect of telephone contact on further suicide attempts in patients discharged from an emergency department: randomised controlled study. BMJ. 2006;332(7552):1241-1245. PubMed CrossRef
8.Stanley B, Brown GK, Brenner LA, et al. Comparison of the Safety Planning Intervention with follow-up vs usual care of suicidal patients treated in the emergency department. JAMA Psychiatry. 2018;75(9):894-900. PubMed CrossRef
aLa Paz University Hospital, Madrid, Spain
bColumbia University Mailman School of Public Health, New York, New York
‡Equal contribution.
*Corresponding author: Gonzalo Mart×nez-Alés, MD, MSc, 722 W 168th St, New York, NY 10032 ([email protected]).
J Clin Psychiatry 2020;81(5):20l13419
To cite: Hernández-Calle D, Mart×nez-Alés G, Mediavilla R, et al. Trends in psychiatric emergency department visits due to suicidal ideation and suicide attempts during the COVID-19 pandemic in Madrid, Spain. J Clin Psychiatry. 2020;81(5):20l13419.
To share: https://doi.org/10.4088/JCP.20l13419
© Copyright 2020 Physicians Postgraduate Press, Inc.
This PDF is free for all visitors!