CME Background
Articles are selected for credit designation based on an assessment of the educational needs of CME participants, with the purpose of providing readers with a curriculum of CME articles on a variety of topics throughout each volume. Activities are planned using a process that links identified needs with desired results.
To obtain credit, read the article, correctly answer at least 70% of the questions in the Posttest, and complete the Evaluation.
CME Objective
After studying this article, you should be able to:
- Select the most appropriate medication for a patient experiencing bipolar I depression
Accreditation Statement
The CME Institute of Physicians Postgraduate Press, Inc., is accredited by the Accreditation Council for Continuing Medical Education to provide continuing medical education for physicians.
Credit Designation
The CME Institute of Physicians Postgraduate Press, Inc., designates this journal-based CME activity for a maximum of 1 AMA PRA Category 1 Creditâ„¢. Physicians should claim only the credit commensurate with the extent of their participation in the activity.
Note: The American Academy of Physician Assistants (AAPA) accepts certificates of participation for educational activities certified for AMA PRA Category 1 Creditâ„¢ from organizations accredited by ACCME or a recognized state medical society. Physician assistants may receive a maximum of 1 hour of Category I credit for completing this program.
Date of Original Release/Review
This educational activity is eligible for AMA PRA Category 1 Creditâ„¢ through May 31, 2017. The latest review of this material was March 2014.
Financial Disclosure
All individuals in a position to influence the content of this activity were asked to complete a statement regarding all relevant personal financial relationships between themselves or their spouse/partner and any commercial interest. The CME Institute has resolved any conflicts of interest that were identified. In the past year, Alan J. Gelenberg, MD, Editor in Chief, has been a consultant for Allergan, Forest, and Zynx Health; has received grant/research support from Pfizer; and has been a stock shareholder of Healthcare Technology Systems. No member of the CME Institute staff reported any relevant personal financial relationships. Faculty financial disclosure appears with the article.
J Clin Psychiatry 2014;75(5):e413-e416
(doi:10.4088/JCP.12065co3c)
© Copyright 2014 Physicians Postgraduate Press, Inc.
This Commentary section of The Journal of Clinical Psychiatry presents the highlights and outcomes of the CME series “Update on Best Practices for Managing Bipolar Depression,” which was published online in April 2013, and is also based on a teleconference discussion held on December 6, 2013. This report was prepared and independently developed by the CME Institute of Physicians Postgraduate Press, Inc., and was supported by an educational grant from Sunovion Pharmaceuticals, Inc.
The teleconference was chaired by Gary S. Sachs, MD, from the Department of Psychiatry, Harvard Medical School, and the Bipolar Clinic and Research Program, Massachusetts General Hospital, Boston. The faculty was Terence A. Ketter, MD, from the Department of Psychiatry and Behavioral Sciences and the Bipolar Disorders Clinic, Stanford School of Medicine, Stanford, California.
Financial disclosure: Dr Sachs is an employee of Bracket Global; is a consultant for Allergan, Lundbeck, and Otsuka; and is a member of the speakers/advisory boards for Elan, Janssen, Merck, Otsuka, and Sunovion. Dr Ketter is a consultant or member of the advisory boards for Allergan, Forest, Janssen, Sunovion, and Teva/Cephalon; has received grant/research support from Agency for Healthcare Research and Quality, Sunovion, and Teva/Cephalon; has received lecture honoraria from GlaxoSmithKline and Otsuka; and has received royalties from American Psychiatric Publishing, Inc. His spouse/partner is an employee and stock shareholder of Janssen.
The opinions expressed herein are those of the faculty and do not necessarily reflect the opinions of the CME provider and publisher or the commercial supporter.
Although the cardinal diagnostic feature of bipolar disorder is periods of abnormal mood elevation (mania or hypomania), patients spend more time depressed than manic and experience greater disability during depressive episodes. Bipolar depression is a challenge to manage because only 3 approved treatments are available for bipolar I depression and only 1 approved treatment is available for bipolar II depression. Because of the disability associated with bipolar depression, and because treatment options are limited, clinicians wanting to provide personalized care and effective management should be familiar with at least the high quality evidence on approved treatment options, as well as simple formal patient assessment techniques.
This Commentary summarizes an online CME program of 2 activities by Gary S. Sachs, MD, and Terence A. Ketter, MD, which were designed to provide learners with an update on the best practices for managing bipolar depression. This Commentary also presents outcomes from the program and highlights from a discussion between Dr Sachs and Dr Ketter in which they identified areas of continued need in patient assessment and treatment selection.
Summary of CME Activities
In “Unmet Needs in the Assessment and Management of Bipolar I Depression,” Dr Sachs discussed 3 important best practices for managing bipolar I depression. The first is the use of formal assessments to evaluate lifetime and current illness. Formal assessments prevent clinicians from relying on impressionistic assessments for diagnosis. Integration of formal scales in conjunction with routine follow-up visits allow clinicians to track treatment response and inform treatment decisions. To address time constraints, clinicians can ask patients to complete pre-assessments prior to office visits. The Montgomery-Asberg Depression Rating Scale (MADRS), Beck Depression Inventory (BDI), and Young Mania Rating Scale (YMRS), among others, can be completed by patients before a visit and then be reviewed by the doctor fairly quickly.
The second practice addressed by Dr Sachs is the use of an individualized model of care designed to provide long-term care. Most models of care are more appropriate for acute rather than chronic conditions and, therefore, aim to find a cure. Clinicians must educate patients that bipolar disorder is a chronic condition with no cure, and their goal should be to manage the illness guided by the progressive wisdom accumulated as clinicians and patients work together over time. To provide individualized care, clinicians can use their knowledge of bipolar depression as well as individual patient factors to identify 2 to 4 potentially appropriate treatment options to present to the patient. Proven agents with a strong evidence base for efficacy and a favorable side effect profile should be offered first.
Finally, Dr Sachs emphasized the need to provide collaborative care that strengthens the therapeutic alliance by fostering communication and shared decision-making between the doctor and patient. Clinicians may need to negotiate with the patient to establish an agreeable treatment plan and promote adherence. Patients and care partners should be educated and encouraged to be active participants in the treatment plan. Furthermore, Dr Sachs explained that formal assessments should be used throughout treatment, and the results of these assessments should be shared with patients to increase their understanding of the efficacy of treatment strategies.
In “Important Distinctions Between Bipolar I and Bipolar II Depression,” Dr Ketter explained that bipolar II depression is associated with less severe mood elevations than bipolar I and patients spend more time depressed and experience comparable levels of functional impairment and risk of suicide. Only 3 treatments are FDA-approved for the treatment of acute bipolar depression: quetiapine, olanzapine/fluoxetine combination, and lurasidone. Only quetiapine is approved for the treatment of bipolar II depression. Dr Ketter stated that, when selecting pharmacotherapy, clinicians must consider patient preferences as well as the potential risks and benefits of available treatments.
To assess medication efficacy and tolerability, Dr Ketter suggested that clinicians use the number needed to treat (NNT) and the number needed to harm (NNH). The NNT is the number of patients who must be treated with 1 intervention versus another to experience 1 additional positive outcome. The NNH is the number of patients who would need to be treated with 1 intervention versus another to experience 1 additional negative outcome. Treatments with smaller NNTs are more effective, and treatments with higher NNHs are more tolerable. Dr Ketter recommended selecting more effective agents for patients with urgent mood symptoms, and more tolerable agents for patients who are concerned about side effects and have less urgent needs.
Dr Ketter reviewed the efficacy and tolerability data available for bipolar depression treatments, including both approved and off-label treatments, such as antipsychotics, mood stabilizers, stimulant-like drugs, and antidepressants. He concluded that, among approved treatments, only lurasidone is likely to deliver more efficacy without sacrificing tolerability, according to current data.
SUMMARY OF OUTCOMES
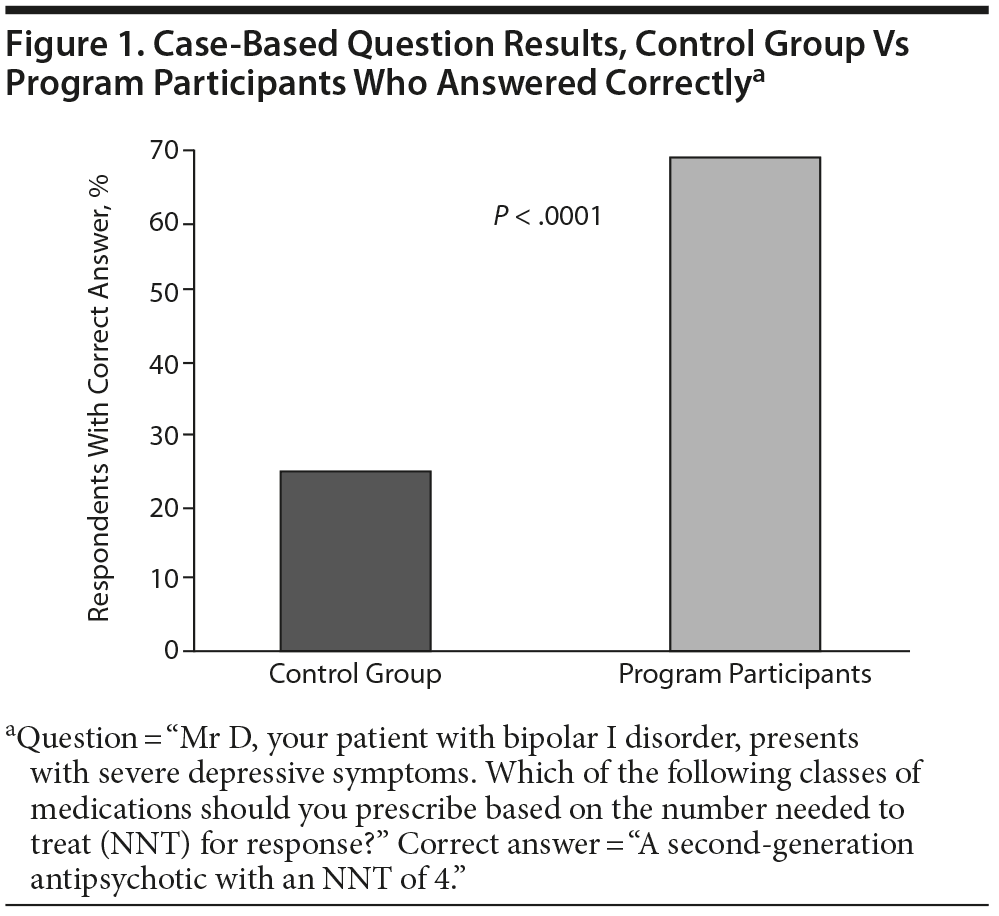
One way in which outcomes data for this CME program were obtained was by comparing the percentage of participants who answered posttest questions correctly with results from a control group of nonparticipants. Participants demonstrated gains in both knowledge and competence compared with the control group, showing that this program succeeded in achieving its educational objectives. For example, compared with a minority (44%) of control group respondents, a majority (69%) of participants were able to correctly answer a question about using NNT to select the most effective treatment for a patient with bipolar I depression, which is a statistically significant difference (P < .0001; Figure 1).
- Select agents based on the greater need, clinical urgency, or greater tolerability.
- Base treatment selection on available data as well as patient factors and preferences.
- Use formal assessments at each patient visit to track trends over time.
Participants were also asked how often they currently used certain clinical strategies (based on the educational objectives; Table 1) and how often they planned to use those strategies after participating in the program. Participants reported greater planned future use of all strategies.
DISCUSSION
After reviewing the outcomes for the program, Drs Sachs and Ketter discussed areas of future educational need related to patient assessment and treatment selection.
The Role of Assessments in Practice
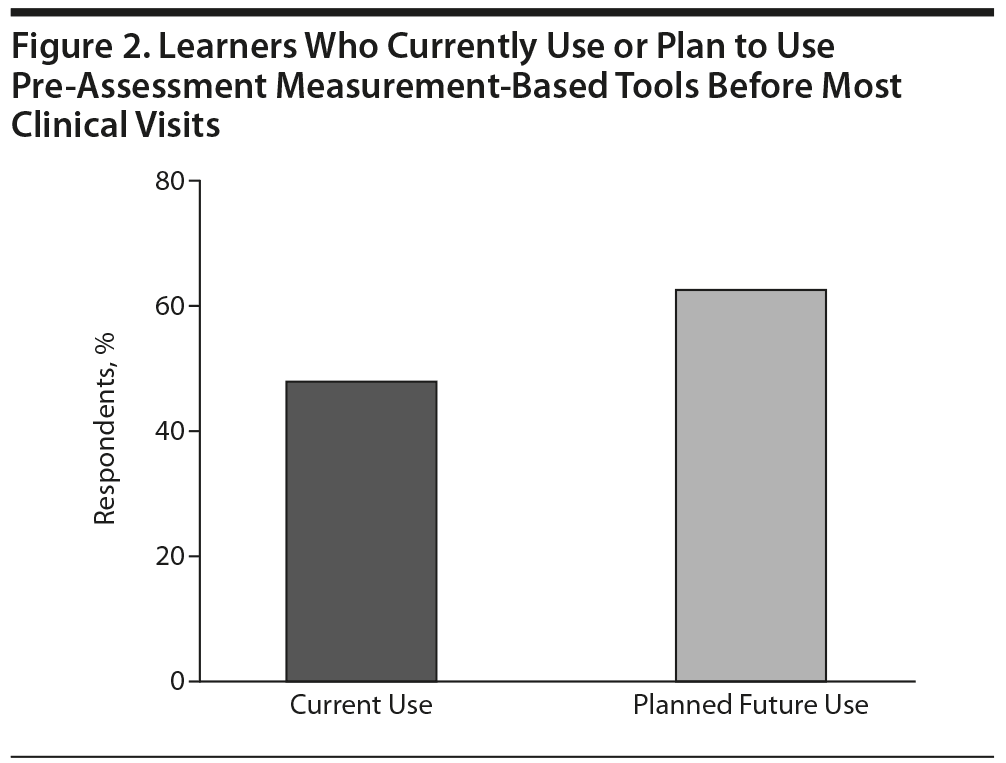
Dr Sachs: In my presentation, I mentioned the value of using pre-assessments. The CME program outcomes data revealed that these types of assessments are currently used sometimes by clinicians, and in the future they plan to use them more but not all of the time (Figure 2). Clinicians may need more information on how to interpret the results of various assessments and what the actual results mean in terms of their cross-sectional reference points. Integrating the use of these assessments into their practice would give clinicians and their patients a definitive knowledge of the outcomes of each treatment trial.
Dr Ketter: With measurement-based care, time is an important factor. Clinicians do need to take time to try a medication for a patient, but, if assessments show that it isn’ t very effective after 2 weeks, it likely won’ t be very effective after 6 weeks. This is a complicated issue, and that guideline may need to be modified in certain circumstances. For instance, some drugs need to be titrated up gradually to become effective, so they may need more time for the results to be evaluated. On the other hand, assessments can show that the patient’s depression has not returned over time, but not why. In clinical practice, you do not have the benefit of a control group, so you have to use the test of time, along with formal assessments, to really determine the success of a treatment.
Dr Sachs: Other factors also are relevant to practicing measurement-based care. For example, situations can cause mood symptoms to fluctuate. A worsening mood could be unrelated to the ongoing treatment, such as having a bad week at work. An assessment of a patient at a particular point in time should be put into context. Multiple assessments over time are needed, and clinical interviews should add information. You really need to get a sense of the patient’s mood trend over time to determine if an assessment reflects a durable remission or a clear worsening.
A balance between clinical experience, patient factors, and available evidence is relevant to population versus personalized prescribing. At the beginning of treatment, when you know nothing else about the patient other than what you find out in the first interview, you are informed by the data for the population and your general clinical experience. But, as you go forward and proceed with treatment trials for that patient, you shift into what you know about this particular patient and his or her real response to the treatment (as measured by formal assessments).
Efficacy Vs Tolerability
Dr Sachs: Further information on selecting the most appropriate medication would be helpful. Second-generation antipsychotics are important treatment options, but they do not all have data showing that they work. A lot of clinicians prescribe them, but they may prescribe agents that are not effective for bipolar depression.
Dr Ketter: Learners would also benefit from further information on whether to prioritize efficacy or tolerability based on the urgency of the situation. If a patient is experiencing symptoms that urgently need to be resolved, you must use a drug you know will work. But, if the situation is not urgent and the patient is concerned about side effects, you may be willing to try a less effective drug that will be well-tolerated.
Dr Sachs: Clinicians must recognize when patients are not in an urgent care situation. These situations allow the clinician to pursue sequential care in which patient preferences can be the key drivers.
Dr Ketter: Parameters for clinical urgency include the likelihood of a suicide attempt, a psychiatric hospitalization, or a job or relationship loss. These are some of the possible events that would indicate that the patient’s efficacy needs outweigh tolerability concerns.
Clinicians must also recognize situations in which tolerability issues may not apply. For example, if someone is experiencing depression with horrible insomnia, giving them treatment that may cause drowsiness might not be problematic. Clinicians must consider potential benefits as well as harms when assessing side effects.
Dr Sachs: For one person, a side effect might be a harm, but, for another person, it would be a benefit. We should personalize care based on our understanding of an individual patient. It is really going from population-based prescribing to personal prescribing.
Dr Ketter: When a patient is already overweight or has metabolic issues, then drugs with side effects that would exacerbate those factors should not be under consideration. Many of the longer term issues with treatment relate to the durability of the response and the ongoing tolerability. Does the patient stay well? Is the patient able to stay with this treatment for a long time? Or do serious problems gradually evolve, such as sleep or metabolic disturbances? Some tolerability issues take time to become apparent, and they can escalate over time. Clinicians need to decide at what point they should intervene and try something different.
Disclosure of off-label usage: Dr Sachs has determined that, to the best of his knowledge, no investigational information outside of US Food and Drug Administration-approved labeling has been presented in this article.
Drug names: lurasidone (Latuda), olanzapine/fluoxetine combination (Symbyax and others), quetiapine (Seroquel and others).